Full Question & Answer Text (for Search Engines)
Question 1:
A 25-year-old male presents after a motor vehicle collision. Imaging reveals a traumatic spondylolisthesis of the axis. Radiographs show a fracture through the pars interarticularis of C2 with severe angulation and minimal translation, without facet dislocation. Applying axial traction causes the fracture gap to widen. Based on the Levine and Edwards classification, what is the most appropriate management?
Options:
- Application of cervical traction followed by halo vest
- Gentle compression in extension followed by halo vest immobilization
- Application of a hard cervical collar for 6 weeks
- Immediate posterior C1-C2 fusion
- Anterior C2-C3 discectomy and fusion
Correct Answer: Gentle compression in extension followed by halo vest immobilization
Explanation:
The patient has a Levine-Edwards Type IIA Hangman's fracture, characterized by severe angulation and minimal translation without facet dislocation. Because the mechanism involves flexion-distraction, applying axial traction is contraindicated as it will widen the fracture gap and potentially cause neurologic injury. The appropriate treatment is gentle compression in extension, followed by placement in a halo vest.
Question 2:
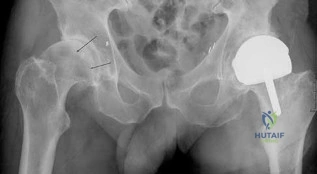
A 32-year-old male is brought to the trauma bay in hemorrhagic shock after a motorcycle crash. An anteroposterior radiograph of the pelvis demonstrates an APC-III injury. A pelvic binder is applied. To maximize reduction of the pelvic volume, at what anatomical landmark should the binder be centered?
Options:
- Anterior superior iliac spines
- Iliac crests
- Greater trochanters
- Symphysis pubis
- Ischial tuberosities
Correct Answer: Greater trochanters
Explanation:
Pelvic binders should be centered over the greater trochanters to effectively close the pelvic ring and reduce pelvic volume. Placement over the iliac crests or ASIS can paradoxically widen the true pelvis or fail to achieve adequate reduction in an open-book pelvic injury.
Question 3:
Teriparatide is utilized in the management of osteoporosis to stimulate bone formation. Intermittent administration of this parathyroid hormone (PTH) analog exerts its primary anabolic effect by binding to receptors on which of the following cell types?
Options:
- Osteoclasts
- Osteoblasts
- Osteocytes
- Macrophages
- Chondrocytes
Correct Answer: Osteoblasts
Explanation:
Intermittent administration of parathyroid hormone (PTH) or its analog (teriparatide) exerts a paradoxical anabolic effect on bone by directly binding to PTH1 receptors on osteoblasts, stimulating their proliferation, increasing their lifespan by preventing apoptosis, and increasing bone formation.
Question 4:
A 12-year-old obese male presents with left thigh pain and an antalgic gait for 4 weeks. He has been entirely unable to bear weight on the left leg for the past 2 days. Radiographs show a slipped capital femoral epiphysis (SCFE) with a slip angle of 60 degrees. What is the most significant risk factor for the development of avascular necrosis (AVN) in this patient?
Options:
- Severity of the slip angle
- Patient's weight
- Duration of symptoms prior to presentation
- Inability to bear weight
- Use of a single screw for fixation
Correct Answer: Inability to bear weight
Explanation:
The clinical inability to bear weight, even with crutches, defines an unstable SCFE according to the Loder classification. Unstable SCFE carries a significantly higher risk of avascular necrosis (AVN), historically up to 50%, compared to stable SCFE where AVN is rare. While a severe slip angle increases the technical difficulty of fixation, stability is the primary predictor of AVN.
Question 5:
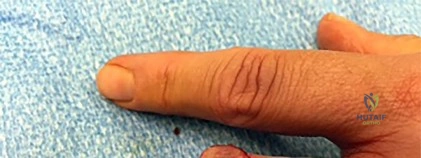
A 28-year-old carpenter sustains a volar laceration to his dominant index finger at the level of the proximal phalanx. He is unable to flex the proximal or distal interphalangeal joints. During surgical exploration, the flexor digitorum profundus (FDP) and flexor digitorum superficialis (FDS) are found to be completely transected in Zone II. What is the most appropriate management?
Options:
- Primary repair of the FDP only and excision of the FDS slips
- Primary repair of both FDP and FDS
- Primary repair of the FDS only and excision of the FDP
- Two-stage tendon reconstruction with a silicone rod
- Excision of the FDP and tenodesis of the distal phalanx
Correct Answer: Primary repair of both FDP and FDS
Explanation:
In Zone II flexor tendon injuries, the standard of care is primary repair of both the FDP and FDS tendons. Repairing both tendons helps preserve the vincula (blood supply), maintains a smooth gliding surface, reduces the risk of postoperative bowstringing, and generally leads to superior functional outcomes compared to isolated FDP repair.
Question 6:
A 72-year-old female undergoes a primary total hip arthroplasty via a posterior approach. Postoperatively, she experiences recurrent posterior dislocations. Radiographic evaluation demonstrates an anteverted cup at 15 degrees and an abduction angle of 40 degrees, with the femoral stem in 5 degrees of retroversion. What is the most likely cause of her instability?
Options:
- Insufficient acetabular component abduction
- Excessive acetabular component anteversion
- Femoral component retroversion
- Impingement of the anterior capsule
- Weakness of the hip abductor musculature
Correct Answer: Femoral component retroversion
Explanation:
Stability in total hip arthroplasty is largely dependent on the combined anteversion of the acetabular and femoral components, which should optimally be between 25 and 35 degrees (Widmer's criteria). In this case, the acetabular cup is anteverted 15 degrees, but the femoral stem is retroverted 5 degrees, resulting in a combined anteversion of only 10 degrees. This relative retroversion significantly increases the risk of posterior dislocation.
Question 7:
A 24-year-old football player sustains a hyperplantarflexion injury to his midfoot. Radiographs demonstrate widening of the space between the base of the first and second metatarsals. Which of the following best describes the anatomy of the primary ligament disrupted in this injury?
Options:
- A dorsal ligament extending from the navicular to the medial cuneiform
- A plantar ligament extending from the calcaneus to the cuboid
- A dorsal ligament extending between the medial cuneiform and second metatarsal
- A plantar ligament extending from the medial cuneiform to the base of the second metatarsal
- An interosseous ligament extending between the bases of the first and second metatarsals
Correct Answer: A plantar ligament extending from the medial cuneiform to the base of the second metatarsal
Explanation:
The Lisfranc ligament is an interosseous ligament located plantarly. It extends from the lateral aspect of the medial cuneiform to the medial aspect of the base of the second metatarsal. It is the largest and strongest of the ligaments supporting the first tarsometatarsal articulation, and its disruption is the hallmark of a Lisfranc injury. There is no direct intermetatarsal ligament between the bases of the first and second metatarsals.
Question 8:
A 14-year-old boy presents with right thigh pain and swelling. Radiographs show a permeative, diaphyseal lesion with an 'onion-skin' periosteal reaction. Biopsy reveals uniform small round blue cells. Cytogenetic analysis of this tumor is most likely to demonstrate which of the following translocations?
Options:
- t(11;22)
- t(X;18)
- t(2;13)
- t(12;16)
- t(9;22)
Correct Answer: t(11;22)
Explanation:
The clinical presentation, radiographic findings ('onion-skin' periostitis), and histology (small round blue cells) are diagnostic of Ewing sarcoma. Over 90% of Ewing sarcomas are characterized by the t(11;22)(q24;q12) chromosomal translocation, which results in the EWS-FLI1 fusion protein. t(X;18) is seen in synovial sarcoma, t(2;13) in alveolar rhabdomyosarcoma, and t(12;16) in myxoid liposarcoma.
Question 9:
Sclerostin is a protein that negatively regulates bone formation. Monoclonal antibodies targeting sclerostin (e.g., romosozumab) are utilized in the treatment of severe osteoporosis. Sclerostin exerts its inhibitory effect on osteoblasts primarily by antagonizing which of the following intracellular signaling pathways?
Options:
- RANK/RANKL pathway
- Wnt/β-catenin pathway
- TGF-β/SMAD pathway
- Bone Morphogenetic Protein (BMP) pathway
- Notch signaling pathway
Correct Answer: Wnt/β-catenin pathway
Explanation:
Sclerostin is secreted by osteocytes and inhibits bone formation by binding to LRP5/6 receptors on osteoblasts. This binding blocks the coreceptor function of LRP5/6, thereby antagonizing the canonical Wnt/β-catenin signaling pathway, which is essential for osteoblast differentiation and survival.
Question 10:
According to recent quantitative anatomical studies utilizing MRI and gadolinium, which of the following vessels provides the principal intraosseous blood supply to the humeral head, challenging historical teachings regarding proximal humerus vascularity?
Options:
- Anterior humeral circumflex artery
- Posterior humeral circumflex artery
- Suprascapular artery
- Thoracoacromial artery
- Circumflex scapular artery
Correct Answer: Posterior humeral circumflex artery
Explanation:
Historically, the anterior humeral circumflex artery (via its arcuate branch) was thought to be the primary blood supply to the humeral head. However, modern quantitative studies (e.g., Hettrich et al.) have demonstrated that the posterior humeral circumflex artery provides the vast majority (approximately 64%) of the intraosseous blood supply to the humeral head.
Question 11:
A 2-week-old infant is undergoing the Ponseti method for the treatment of idiopathic clubfoot. The deformity consists of cavus, adductus, varus, and equinus. In the Ponseti casting technique, the correction of the cavus deformity is achieved first. Which of the following maneuvers is mechanically correct to accomplish this initial step?
Options:
- Pronation of the forefoot and depression of the first ray
- Supination of the forefoot by elevating the first ray
- Eversion of the hindfoot with plantarflexion of the first ray
- Abduction of the forefoot while stabilizing the calcaneus laterally
- Dorsiflexion of the entire foot simultaneously to stretch the Achilles tendon
Correct Answer: Supination of the forefoot by elevating the first ray
Explanation:
The cavus deformity in clubfoot is primarily driven by pronation of the forefoot relative to the hindfoot. The first and most critical step in the Ponseti method is to correct the cavus by elevating the first ray (dorsiflexing the first metatarsal), which effectively supinates the forefoot to align it with the midfoot and hindfoot. Subsequent casts correct the adductus and varus by abducting the supinated foot around the stabilized head of the talus.
Question 12:
A 25-year-old overhead athlete is diagnosed with a superior labrum anterior and posterior (SLAP) tear after failing nonoperative management. During diagnostic arthroscopy, which of the following intraoperative findings specifically defines a Type II SLAP tear according to the Snyder classification?
Options:
- Degenerative fraying of the superior labrum with an intact biceps anchor
- Detachment of the superior labrum and biceps anchor from the superior glenoid tubercle
- A bucket-handle tear of the superior labrum with an intact biceps anchor
- A bucket-handle tear of the superior labrum extending into the long head of the biceps tendon
- An anteroinferior labral tear extending contiguously to the superior labrum
Correct Answer: Detachment of the superior labrum and biceps anchor from the superior glenoid tubercle
Explanation:
In the Snyder classification of SLAP tears: Type I is degenerative fraying of the labrum with an intact biceps anchor. Type II is a frank detachment of the superior labrum and the biceps anchor from the superior glenoid. Type III is a bucket-handle tear of the labrum with an intact biceps anchor. Type IV is a bucket-handle tear of the labrum that extends into the biceps tendon. Type V (an extension of the classification) involves an anteroinferior Bankart lesion extending to the superior labrum.
Question 13:
A 55-year-old female undergoes volar locked plating for a comminuted intra-articular distal radius fracture. Six months postoperatively, she suddenly loses the ability to actively flex the interphalangeal joint of her thumb. What is the most likely pathophysiologic cause of this complication?
Options:
- Attritional rupture of the flexor pollicis longus (FPL) tendon due to prominent hardware distal to the watershed line
- Attritional rupture of the extensor pollicis longus (EPL) tendon due to dorsally prominent screws
- Delayed median nerve palsy due to carpal tunnel syndrome
- Postoperative adhesions tethering the flexor digitorum profundus (FDP) tendons
- Late-onset anterior interosseous nerve (AIN) palsy secondary to scar tissue formation
Correct Answer: Attritional rupture of the flexor pollicis longus (FPL) tendon due to prominent hardware distal to the watershed line
Explanation:
The inability to actively flex the thumb IP joint several months after volar plating of the distal radius is most commonly due to attritional rupture of the flexor pollicis longus (FPL) tendon. This typically occurs when the volar plate is placed too distally, crossing the 'watershed line' of the distal radius, leading to mechanical friction between the plate edge and the FPL tendon during wrist motion.
Question 14:
A 16-year-old gymnast complains of chronic low back pain exacerbated by extension. Radiographs and subsequent MRI show a unilateral pars interarticularis defect at L5 without evidence of spondylolisthesis. She has failed 6 months of structured conservative management including bracing and physical therapy. She strongly wishes to return to competitive gymnastics. What is the most appropriate surgical intervention?
Options:
- L5-S1 anterior lumbar interbody fusion (ALIF)
- L5-S1 posterior lumbar interbody fusion (PLIF)
- Direct surgical repair of the pars interarticularis (e.g., pedicle screw-hook construct)
- Wide lumbar laminectomy at L5
- Microdiscectomy at L5-S1
Correct Answer: Direct surgical repair of the pars interarticularis (e.g., pedicle screw-hook construct)
Explanation:
In young, active patients (like athletes) with symptomatic spondylolysis (pars defect) who fail nonoperative treatment and do not have a significant spondylolisthesis, direct pars repair is the procedure of choice. Techniques include the Buck procedure (direct lag screw), Scott wiring, or a pedicle screw-laminar hook construct. This preserves the motion segment and allows a higher rate of return to sports compared to fusion.
Question 15:
During the flexion arc of a normal native human knee, the center of rotation of the femur relative to the tibia changes dynamically. Which of the following statements best describes the kinematic phenomenon known as 'femoral rollback'?
Options:
- The medial femoral condyle translates posteriorly more than the lateral femoral condyle during deep flexion.
- The lateral femoral condyle translates posteriorly significantly more than the medial femoral condyle during deep flexion.
- Both femoral condyles translate anteriorly symmetrically during deep flexion.
- The tibia internally rotates symmetrically relative to the femur during terminal extension.
- The patella tracks medially during early flexion and laterally during deep flexion.
Correct Answer: The lateral femoral condyle translates posteriorly significantly more than the medial femoral condyle during deep flexion.
Explanation:
Femoral rollback is asymmetrical in the native knee. As the knee flexes, the lateral femoral condyle rolls back (translates posteriorly) significantly on the lateral tibial plateau, while the medial femoral condyle remains relatively stationary, acting as a pivot point. This differential rollback inherently couples knee flexion with internal rotation of the tibia relative to the femur.
Question 16:
A 19-year-old male presents with severe right thigh pain that is classically worse at night and dramatically relieved by NSAIDs. A CT scan reveals a 7 mm radiolucent nidus surrounded by dense reactive sclerosis in the femoral cortex. What is the most definitive and minimally invasive treatment modality for this condition?
Options:
- En bloc surgical resection
- Intralesional curettage and bone grafting
- Radiofrequency ablation (RFA) of the nidus
- External beam radiation therapy
- Long-term intravenous bisphosphonate therapy
Correct Answer: Radiofrequency ablation (RFA) of the nidus
Explanation:
The clinical history of night pain relieved by NSAIDs, combined with the CT finding of a radiolucent nidus with surrounding sclerosis, is diagnostic of an osteoid osteoma. CT-guided radiofrequency ablation (RFA) is the standard of care, offering a highly successful, minimally invasive, and definitive treatment, replacing the historical need for surgical en bloc resection.
Question 17:
A 55-year-old male with long-standing, poorly controlled type 2 diabetes presents with a warm, swollen, and erythematous left foot. He denies any recent trauma, fevers, or systemic signs of infection. Plain radiographs show early fragmentation and subluxation of the tarsometatarsal joints. His inflammatory markers are mildly elevated. What is the most appropriate initial management?
Options:
- Immediate open reduction and internal fixation of the tarsometatarsal joints
- Intravenous antibiotics and emergent surgical debridement
- Total contact casting (TCC) and strict non-weight bearing
- Amputation at the transmalleolar level (Syme amputation)
- Intra-articular corticosteroid injection into the affected midfoot joints
Correct Answer: Total contact casting (TCC) and strict non-weight bearing
Explanation:
This patient is presenting with acute Eichenholtz stage I Charcot neuroarthropathy. The foot is acutely inflamed, and initial radiographs show fragmentation. The mainstay of treatment in the acute fragmentation phase is immobilization and strict offloading, ideally utilizing a total contact cast (TCC), to arrest progression of the deformity until the acute inflammatory phase subsides and the bones coalesce.
Question 18:
Bone morphogenetic proteins (BMPs) are critical members of the TGF-beta superfamily that induce the differentiation of mesenchymal stem cells into osteoblasts. Which of the following recombinant BMPs is FDA-approved specifically for use in anterior lumbar interbody fusion (ALIF) with a metallic interbody cage?
Options:
- rhBMP-2
- rhBMP-3
- rhBMP-4
- rhBMP-7
- rhBMP-9
Correct Answer: rhBMP-2
Explanation:
Recombinant human BMP-2 (rhBMP-2, trade name Infuse) is FDA-approved for use in single-level anterior lumbar interbody fusion (ALIF) when used with an approved interbody fusion device. rhBMP-7 (OP-1) was previously approved for recalcitrant long bone nonunions under an HDE but is generally no longer commercially available in the US.
Question 19:
A 28-year-old male undergoes reamed intramedullary nailing for a closed comminuted tibial shaft fracture. In the recovery room, he complains of severe leg pain out of proportion to the injury, unremitting despite high-dose intravenous opioids. Passive stretch of his toes elicits excruciating pain. Intracompartmental pressure testing yields an anterior compartment pressure of 45 mmHg, and his diastolic blood pressure is 65 mmHg. What is the most appropriate next step in management?
Options:
- Elevate the leg above heart level and apply continuous ice packs
- Administer a continuous epidural anesthetic to manage the pain
- Perform an emergent four-compartment fasciotomy of the leg
- Return to the operating room for removal of the intramedullary nail and conversion to an external fixator
- Obtain a stat arterial duplex ultrasound of the lower extremity
Correct Answer: Perform an emergent four-compartment fasciotomy of the leg
Explanation:
The patient exhibits classic clinical signs of acute compartment syndrome. The objective threshold for emergent fasciotomy is a delta P (diastolic blood pressure minus compartment pressure) of less than 30 mmHg. In this case, delta P is 20 mmHg (65 - 45 = 20), which is an absolute indication for emergent four-compartment fasciotomy. Elevating the leg above the heart is contraindicated as it reduces arterial perfusion pressure and exacerbates ischemia.
Question 20:
A 6-year-old girl falls from monkey bars and sustains a widely displaced extension-type supracondylar fracture of the distal humerus. On physical examination prior to reduction, she is unable to flex the interphalangeal joint of the thumb and the distal interphalangeal joint of the index finger, resulting in an inability to make an 'A-OK' sign. Which nerve is most likely injured?
Options:
- Radial nerve
- Ulnar nerve
- Anterior interosseous nerve (AIN)
- Posterior interosseous nerve (PIN)
- Musculocutaneous nerve
Correct Answer: Anterior interosseous nerve (AIN)
Explanation:
The anterior interosseous nerve (AIN), a motor branch of the median nerve, is the most commonly injured nerve in extension-type supracondylar humerus fractures. It innervates the flexor pollicis longus (FPL) and the flexor digitorum profundus (FDP) to the index and middle fingers. Injury results in the inability to flex the IP joint of the thumb and DIP joint of the index finger, preventing the patient from making an 'OK' sign.
Question 21:
A 58-year-old female presents with groin pain and swelling three years after undergoing a metal-on-metal total hip arthroplasty. Aseptic lymphocyte-dominated vasculitis-associated lesion (ALVAL) is suspected. Which of the following immunologic mechanisms is primarily responsible for the pathogenesis of this condition?
Options:
- Type I Hypersensitivity (IgE-mediated)
- Type II Hypersensitivity (Cytotoxic)
- Type III Hypersensitivity (Immune complex-mediated)
- Type IV Hypersensitivity (Delayed, T-cell mediated)
- Macrophage-induced osteolysis via particulate wear debris
Correct Answer: Type IV Hypersensitivity (Delayed, T-cell mediated)
Explanation:
ALVAL (Aseptic Lymphocyte-dominated Vasculitis-Associated Lesion) is a classic complication of metal-on-metal implants or corrosion at modular junctions (trunnionosis). It is driven by a Type IV (delayed, T-cell mediated) hypersensitivity reaction to metal ions (like cobalt and chromium). Histologically, it is characterized by a perivascular lymphocytic infiltrate. This distinguishes it from classic polyethylene wear debris, which is characterized by a macrophage-mediated foreign body response.
Question 22:
An 8-week-old infant is being treated with a Pavlik harness for developmental dysplasia of the hip (DDH). During the weekly clinical check, the orthopedic surgeon assesses the harness fit to prevent complications. Which of the following strap misadjustments most directly places the infant at risk for avascular necrosis (AVN) of the femoral head?
Options:
- Excessive flexion of the anterior straps
- Inadequate flexion of the anterior straps
- Excessive abduction of the posterior straps
- Excessive adduction of the posterior straps
- Over-tightening of the chest strap
Correct Answer: Excessive abduction of the posterior straps
Explanation:
In the Pavlik harness, excessive abduction (too tight posterior straps) forces the femoral head into rigid abduction, creating high pressure that compresses the epiphyseal blood vessels (primarily branches of the medial circumflex femoral artery), leading to AVN of the femoral head. Conversely, excessive flexion (too tight anterior straps) puts the infant at risk for transient femoral nerve palsy.
Question 23:
A 35-year-old male is involved in a high-speed motor vehicle collision. Lateral cervical spine radiographs and CT reveal a Levine-Edwards Type IIA traumatic spondylolisthesis of the axis (Hangman's fracture). What is the primary mechanism of injury for this specific fracture subtype?
Options:
- Hyperextension and axial loading
- Hyperextension and axial loading followed by severe flexion
- Flexion and distraction
- Flexion and compression
- Pure rotational shear
Correct Answer: Flexion and distraction
Explanation:
The Levine-Edwards classification for Hangman's fractures (traumatic spondylolisthesis of the axis) is based on mechanism. Type I is hyperextension-axial loading. Type II is hyperextension-axial loading followed by severe flexion. Type IIA is flexion-distraction, characterized by minimal translation but severe angulation, and the disc space is often widened posteriorly. Type IIA fractures are unstable in traction, which is a critical clinical pearl; traction will exacerbate the deformity. Type III is flexion-compression.
Question 24:
The posterior cruciate ligament (PCL) is composed of two primary bundles. Which of the following accurately describes the biomechanical behavior of the anterolateral (AL) and posteromedial (PM) bundles during knee range of motion?
Options:
- AL bundle is tight in flexion; PM bundle is tight in extension
- AL bundle is tight in extension; PM bundle is tight in flexion
- Both bundles are maximally tight in flexion
- Both bundles are maximally tight in extension
- AL bundle limits external rotation; PM bundle limits internal rotation
Correct Answer: AL bundle is tight in flexion; PM bundle is tight in extension
Explanation:
The PCL consists of the larger anterolateral (AL) bundle and the smaller posteromedial (PM) bundle. Biomechanically, the AL bundle is tightest in knee flexion and lax in extension. Conversely, the PM bundle is tightest in knee extension and lax in flexion. This reciprocal relationship is vital to understanding PCL reconstruction biomechanics.
Question 25:
A 40-year-old gymnast falls on an outstretched hand, sustaining a 'Terrible Triad' injury of the elbow. According to standard surgical protocols (e.g., Pugh and McKee), which of the following is the generally recommended sequence of surgical reconstruction to restore stability?
Options:
- Lateral collateral ligament (LCL) repair -> Coronoid fixation -> Radial head fixation/replacement -> Medial collateral ligament (MCL) repair
- Radial head fixation/replacement -> Coronoid fixation -> LCL repair -> MCL repair (if needed)
- Coronoid fixation -> Radial head fixation/replacement -> LCL repair -> MCL repair (if needed)
- MCL repair -> Coronoid fixation -> Radial head fixation/replacement -> LCL repair
- Coronoid fixation -> LCL repair -> Radial head fixation/replacement -> MCL repair
Correct Answer: Coronoid fixation -> Radial head fixation/replacement -> LCL repair -> MCL repair (if needed)
Explanation:
The classic 'Terrible Triad' of the elbow includes an elbow dislocation, radial head fracture, and coronoid fracture. The standard inside-out surgical algorithm established by Pugh et al. starts deep/anterior and moves lateral: 1) Fixation or reconstruction of the coronoid process, 2) Fixation or replacement of the radial head, 3) Repair of the lateral collateral ligament (LCL) complex to the lateral epicondyle. If the elbow remains unstable after these steps, 4) Repair of the medial collateral ligament (MCL) or application of a hinged external fixator is indicated.
Question 26:
A 55-year-old male presents with deep thigh pain. Radiographs reveal a permeative radiolucent lesion in the proximal femur with 'popcorn' calcifications. Core needle biopsy demonstrates a hypercellular hyaline cartilage tumor with nuclear atypia and binucleated cells, consistent with Grade II conventional chondrosarcoma. What is the most appropriate management?
Options:
- Intralesional curettage and bone grafting
- Intralesional curettage with adjuvant cryotherapy
- Wide local excision (en bloc resection) alone
- Wide local excision followed by adjuvant chemotherapy
- Neoadjuvant radiation therapy followed by wide local excision
Correct Answer: Wide local excision (en bloc resection) alone
Explanation:
Conventional chondrosarcoma is notably resistant to both chemotherapy and radiation therapy due to its poor vascularity, slow division rate, and extracellular matrix properties. The mainstay of treatment for intermediate-grade (Grade II) and high-grade (Grade III) chondrosarcoma is wide local excision (en bloc resection) with negative margins. Intralesional curettage is only acceptable for Grade I (atypical cartilaginous tumors) in the appendicular skeleton.
Question 27:
A 60-year-old male with poorly controlled diabetes presents with a swollen, warm, and minimally painful foot. Radiographs are obtained to evaluate for Charcot neuroarthropathy. According to the Eichenholtz classification, which of the following clinical and radiographic findings is characteristic of Stage II (Coalescence)?
Options:
- Erythema and soft tissue swelling with normal radiographs
- Periarticular fragmentation, joint subluxation, and copious debris
- Absorption of fine intra-articular debris and early fracture sclerosis/consolidation
- Rounding of bone ends, fixed deformity, and complete joint remodeling
- Acute osteomyelitis with periosteal elevation and gas in the soft tissues
Correct Answer: Absorption of fine intra-articular debris and early fracture sclerosis/consolidation
Explanation:
The Eichenholtz classification of Charcot neuroarthropathy includes: Stage 0 (Pre-radiographic): erythema, swelling, warmth, normal X-rays. Stage I (Development/Fragmentation): joint destruction, subluxation, fragmentation, and debris. Stage II (Coalescence): decreased warmth/swelling, absorption of fine debris, early sclerosis, and fracture healing. Stage III (Remodeling): consolidated fractures, rounded bone ends, osteophyte formation, and fixed residual deformity.
Question 28:
During a primary total knee arthroplasty, trial components are placed, and gap balancing is assessed. The knee is found to be tight in 90 degrees of flexion but perfectly balanced in full extension. Which of the following femoral component adjustments will best correct this specific imbalance?
Options:
- Decrease the thickness of the polyethylene tibial insert
- Increase the distal femoral resection
- Downsize the femoral component (decrease AP dimension)
- Upsize the femoral component (increase AP dimension)
- Decrease the posterior slope of the tibial cut
Correct Answer: Downsize the femoral component (decrease AP dimension)
Explanation:
In TKA gap balancing, the flexion gap is primarily controlled by the anteroposterior (AP) dimension of the femoral component, while the extension gap is controlled by the distal femoral resection. If the knee is tight in flexion but balanced in extension, the flexion gap needs to be increased without affecting the extension gap. Downsizing the femoral component decreases its AP dimension (specifically taking more posterior condyle), which opens up the flexion gap while leaving the extension gap unchanged.
Question 29:
Bone morphogenetic proteins (BMPs) play a critical role in osteoinduction and bone healing. Recombinant human BMP-2 (rhBMP-2) is utilized in various spine and orthopedic trauma procedures. Upon binding to its transmembrane serine/threonine kinase receptor, which intracellular signaling pathway is primarily activated by BMP-2?
Options:
- Smad 2 and 3
- Smad 1, 5, and 8
- Wnt/Beta-catenin
- MAP kinase (MAPK)
- JAK/STAT
Correct Answer: Smad 1, 5, and 8
Explanation:
BMP-2 and BMP-7 act via cell surface receptors that have intrinsic serine/threonine kinase activity. Once activated, these receptors phosphorylate the intracellular R-Smads (Receptor-regulated Smads), specifically Smad 1, Smad 5, and Smad 8. These complex with Co-Smad (Smad 4) to translocate to the nucleus and induce osteogenic gene transcription. Smad 2 and 3 are primarily associated with the TGF-beta signaling pathway, not BMP.
Question 30:
A 45-year-old male is struck by a vehicle and sustains a complex tibial plateau fracture. The injury is classified as a Schatzker Type IV fracture. What is the classic mechanism of injury, and which surgical approach is most commonly required for anatomic reduction and buttressing of this specific pattern?
Options:
- Valgus force with axial loading; Anterolateral approach
- Valgus force with axial loading; Posteromedial approach
- Varus force with axial loading; Anterolateral approach
- Varus force with axial loading; Posteromedial approach
- Pure axial loading; Dual (anterolateral and posteromedial) approach
Correct Answer: Varus force with axial loading; Posteromedial approach
Explanation:
Schatzker Type IV represents a medial tibial plateau fracture, classically caused by a high-energy varus force combined with axial loading. Because the medial plateau is dense and strong, this fracture implies high energy and often subluxation/dislocation of the knee joint. The optimal surgical approach involves buttressing the medial fragment, which is best achieved via a posteromedial approach to place an anti-glide or buttress plate.
Question 31:
An infant is born with idiopathic congenital talipes equinovarus (clubfoot) and is referred for Ponseti serial casting. According to the Ponseti method, what is the first step in the manual manipulation and casting sequence to correct the deformities?
Options:
- Dorsiflexion of the ankle to correct equinus
- Abduction of the midfoot with counter-pressure on the calcaneocuboid joint
- Supination of the forefoot with elevation of the first ray to correct cavus
- Pronation of the forefoot to correct adduction
- Eversion of the hindfoot to correct varus
Correct Answer: Supination of the forefoot with elevation of the first ray to correct cavus
Explanation:
The Ponseti method corrects clubfoot deformities in a specific sequence remembered by the acronym CAVE: Cavus, Adductus, Varus, Equinus. The very first step is to correct the cavus deformity by supinating the forefoot and elevating the first metatarsal (first ray) to align the forefoot with the hindfoot. Abduction of the midfoot with counter-pressure on the head of the talus (not calcaneocuboid joint) then corrects the adductus and varus simultaneously.
Question 32:
A 28-year-old male presents after an unprovoked seizure. He complains of right shoulder pain and is unable to externally rotate his arm. Imaging confirms a posterior shoulder dislocation. Further evaluation reveals an impaction fracture of the humeral head known as a reverse Hill-Sachs lesion. Where is this articular defect classically located?
Options:
- Posterolateral aspect of the humeral head
- Anteromedial aspect of the humeral head
- Posteromedial aspect of the humeral head
- Anterolateral aspect of the humeral head
- Central articular surface of the humeral head
Correct Answer: Anteromedial aspect of the humeral head
Explanation:
A posterior shoulder dislocation commonly results in an impaction fracture of the humeral head as it is driven against the posterior glenoid rim. This defect is known as a reverse Hill-Sachs lesion and is classically located on the anteromedial aspect of the humeral head. In contrast, an anterior dislocation produces a standard Hill-Sachs lesion, which is located on the posterolateral aspect of the humeral head.
Question 33:
A 24-year-old carpenter sustains a volar laceration to the index finger at the level of the proximal phalanx, resulting in a Zone II flexor tendon injury. During primary repair, the surgeon carefully preserves the flexor tendon sheath pulleys. Which two pulleys are most biomechanically critical to prevent bowstringing of the flexor tendons?
Options:
- A1 and A3
- A1 and A5
- A2 and A3
- A2 and A4
- A3 and C1
Correct Answer: A2 and A4
Explanation:
In the flexor tendon pulley system of the fingers, there are 5 annular (A) and 3 cruciform (C) pulleys. The A2 pulley (located over the proximal phalanx) and the A4 pulley (located over the middle phalanx) are the major mechanical pulleys. Preservation or reconstruction of the A2 and A4 pulleys is absolutely critical to prevent bowstringing of the flexor tendons, which would cause significant loss of mechanical advantage and active range of motion.
Question 34:
A 45-year-old male presents with severe, radiating leg pain. An MRI of the lumbar spine is obtained. Imaging demonstrates a 'far lateral' (extraforaminal) disc herniation at the L4-L5 level. Which nerve root is most likely to be directly compressed by this specific type of herniation?
Options:
- L3 nerve root
- L4 nerve root
- L5 nerve root
- S1 nerve root
- Both L4 and L5 nerve roots equally
Correct Answer: L4 nerve root
Explanation:
In the lumbar spine, a classic posterolateral (paracentral) disc herniation affects the traversing nerve root (e.g., L4-L5 disc affects the L5 root). However, a 'far lateral' or extraforaminal disc herniation affects the exiting nerve root at that same level. Therefore, a far lateral disc herniation at L4-L5 will compress the exiting L4 nerve root, causing weakness in knee extension and anterior thigh pain.
Question 35:
During normal human gait, the muscles of the lower extremity exhibit highly coordinated, phased activity. Peak concentric contraction and maximal electromyographic (EMG) activity of the gastrocnemius-soleus complex occurs during which specific phase of the gait cycle?
Options:
- Initial contact (Heel strike)
- Loading response (Foot flat)
- Mid stance
- Terminal stance (Heel off)
- Pre-swing (Toe off)
Correct Answer: Terminal stance (Heel off)
Explanation:
The gastrocnemius-soleus complex is crucial for ankle plantarflexion. During mid stance, the triceps surae contracts eccentrically to control the forward progression of the tibia over the fixed foot (controlling ankle dorsiflexion). Its peak electrical activity and maximal concentric contraction occur during terminal stance (heel off) to provide the active push-off required for forward propulsion, right before pre-swing.
Question 36:
A 22-year-old male is brought to the trauma bay after a motorcycle accident. Pelvic radiographs demonstrate significant widening of the pubic symphysis, indicative of an anteroposterior compression (APC) injury. To classify this as an APC Type III injury (Young-Burgess classification), which of the following combinations of posterior pelvic ring ligaments must be completely disrupted?
Options:
- Anterior sacroiliac ligaments only
- Sacrospinous and sacrotuberous ligaments only
- Anterior sacroiliac, sacrospinous, and sacrotuberous ligaments (posterior sacroiliac ligaments intact)
- Anterior sacroiliac, posterior sacroiliac, sacrospinous, and sacrotuberous ligaments
- Posterior sacroiliac ligaments only
Correct Answer: Anterior sacroiliac, posterior sacroiliac, sacrospinous, and sacrotuberous ligaments
Explanation:
In the Young-Burgess classification, APC I involves symphysis widening <2.5 cm with intact posterior ligaments. APC II involves symphysis widening >2.5 cm, disruption of the anterior sacroiliac, sacrospinous, and sacrotuberous ligaments, but the critical posterior sacroiliac (SI) ligaments remain intact (rotationally unstable, vertically stable). APC III indicates complete disruption of the anterior SI, sacrospinous, sacrotuberous, AND the posterior SI ligaments, resulting in a completely unstable hemipelvis (both rotationally and vertically).
Question 37:
A 35-year-old recreational athlete undergoes percutaneous repair of an acute Achilles tendon rupture. During passage of the proximal transverse sutures, a nerve is inadvertently entrapped. Which nerve is at greatest risk during this procedure, and what is its normal anatomic relationship to the Achilles tendon insertion?
Options:
- Saphenous nerve; crosses medial to the tendon 10 cm proximal to the insertion
- Tibial nerve; runs strictly anterior to the tendon throughout its course
- Sural nerve; crosses the lateral border of the tendon approximately 10 cm proximal to the insertion
- Sural nerve; crosses the medial border of the tendon approximately 5 cm proximal to the insertion
- Superficial peroneal nerve; crosses the lateral border of the tendon 15 cm proximal to the insertion
Correct Answer: Sural nerve; crosses the lateral border of the tendon approximately 10 cm proximal to the insertion
Explanation:
The sural nerve is at the greatest risk of iatrogenic injury during percutaneous or minimally invasive Achilles tendon repair, particularly during the placement of proximal, lateral sutures. Anatomically, the sural nerve travels distally in the posterior calf and classically crosses the lateral border of the Achilles tendon from medial to lateral at an average of 9.8 cm (approximately 10 cm) proximal to the calcaneal insertion.
Question 38:
A 16-year-old male presents with a persistent, dull ache in his right tibia that is significantly worse at night. The pain is rapidly and completely relieved by ibuprofen. Imaging demonstrates a cortical thickening with a small (<1.5 cm) radiolucent nidus. What is the primary biochemical mechanism driving this patient's nocturnal pain?
Options:
- Release of substance P from surrounding reactive periosteum
- Elevated production of prostaglandin E2 (PGE2) by osteoblasts within the nidus
- High concentrations of interleukin-1 (IL-1) and TNF-alpha triggering osteoclasts
- Direct mechanical expansion of the medullary cavity by a growing cyst
- Histamine release from mast cells infiltrating the lytic lesion
Correct Answer: Elevated production of prostaglandin E2 (PGE2) by osteoblasts within the nidus
Explanation:
The clinical presentation is classic for an osteoid osteoma. The pathognomonic symptom is severe, unrelenting night pain that is exquisitely responsive to nonsteroidal anti-inflammatory drugs (NSAIDs) or salicylates. This is because the cells within the nidus (active osteoblasts) contain very high levels of cyclooxygenase-2 (COX-2) and produce massive amounts of prostaglandin E2 (PGE2). PGE2 induces intense local vasodilation and directly stimulates local nerve endings.
Question 39:
A 65-year-old patient complains of an audible "squeaking" sound from her total hip arthroplasty, which utilizes a ceramic-on-ceramic bearing surface. What surgical or mechanical factor is most strongly associated with the initiation of squeaking in modern ceramic-on-ceramic hips?
Options:
- Excessive femoral head size (>36 mm)
- Use of a highly cross-linked polyethylene liner
- Component malpositioning leading to micro-separation and edge-loading
- Deep periprosthetic joint infection (PJI)
- Galvanic corrosion at the modular head-neck junction
Correct Answer: Component malpositioning leading to micro-separation and edge-loading
Explanation:
Squeaking is a known complication unique to hard-on-hard bearing surfaces, most notably alumina ceramic-on-ceramic THA. The primary mechanical etiology is stripe wear caused by micro-separation during the swing phase of gait, leading to edge-loading when the head re-engages the rim of the cup. This is strongly associated with component malpositioning (particularly excessive cup anteversion or high inclination angles) that disrupts fluid film lubrication.
Question 40:
A healthy, highly active 40-year-old male falls from a ladder and sustains a displaced intracapsular fracture of the femoral neck (Garden IV). He is brought to the emergency department within 4 hours of the injury. What is the most appropriate surgical management for this specific patient?
Options:
- Urgent hemiarthroplasty of the hip
- Urgent total hip arthroplasty (THA)
- Closed or open reduction and internal fixation (CRIF/ORIF) as soon as possible
- Application of skeletal traction followed by delayed ORIF at 1 week
- Core decompression with fibular strut allografting
Correct Answer: Closed or open reduction and internal fixation (CRIF/ORIF) as soon as possible
Explanation:
In a young, physiologically active patient (generally <60-65 years old), a displaced femoral neck fracture is an orthopedic urgency. The goal is head preservation despite the high risk of avascular necrosis (AVN) and nonunion. The standard of care is urgent closed or open reduction and internal fixation (using cannulated screws or a sliding hip screw device) to restore the native anatomy. Arthroplasty (hemi or THA) is reserved for older, lower-demand patients or cases of delayed presentation where head salvage is impossible.
Question 41:
A 72-year-old male presents with recurrent posterior dislocations following a right total hip arthroplasty performed 2 months ago via a posterior approach. Radiographs show a well-fixed femoral stem and an acetabular component with 10 degrees of anteversion and 45 degrees of abduction. During revision surgery, the acetabular component is found to be solidly ingrown. Which of the following is the most appropriate surgical intervention to prevent further posterior dislocations?
Options:
- Increase femoral offset by changing to a longer femoral head.
- Revise the acetabular shell to increase anteversion.
- Apply a constrained acetabular liner into the existing shell.
- Revise the femoral stem to increase anteversion.
- Prescribe an abduction orthosis for 6 weeks.
Correct Answer: Revise the acetabular shell to increase anteversion.
Explanation:
The ideal acetabular cup position in total hip arthroplasty is generally considered to be 15 to 20 degrees of anteversion and 40 to 45 degrees of abduction. An anteversion of 10 degrees is relatively retroverted, especially when a posterior approach is used, predisposing the patient to posterior instability. Since the cup is malpositioned, the most appropriate treatment is revision of the acetabular shell to correct the anteversion.
Question 42:
A 45-year-old male sustains a Schatzker IV tibial plateau fracture with a large posteromedial shear fragment. He is scheduled for open reduction and internal fixation. A posteromedial surgical approach is planned. To safely access the fracture fragment, the surgical interval is developed between which of the following structures?
Options:
- Medial head of the gastrocnemius and the pes anserinus
- Semimembranosus and semitendinosus
- Popliteus and soleus
- Tibialis posterior and flexor digitorum longus
- Anterior tibialis and extensor hallucis longus
Correct Answer: Medial head of the gastrocnemius and the pes anserinus
Explanation:
The posteromedial approach to the tibial plateau utilizes the interval between the medial head of the gastrocnemius (which is retracted laterally/posteriorly) and the pes anserinus tendons (which are retracted anteriorly/medially). This provides excellent direct access to posteromedial shear fragments for buttress plating.
Question 43:
A 68-year-old male presents with progressive hand clumsiness and gait imbalance over the past year. Examination reveals a positive Hoffmann sign bilaterally and hyperreflexia in the lower extremities. MRI of the cervical spine demonstrates severe spinal canal stenosis at C4-C5 and C5-C6. Which of the following specific MRI findings in the spinal cord is most strongly associated with a poor prognosis for neurologic recovery following surgical decompression?
Options:
- Focal T2 hyperintensity alone
- T1 hypointensity combined with T2 hyperintensity
- Diffuse T2 hyperintensity across multiple levels
- T1 hyperintensity
- Loss of the subarachnoid space without intrinsic cord signal changes
Correct Answer: T1 hypointensity combined with T2 hyperintensity
Explanation:
In cervical spondylotic myelopathy, the presence of T1 hypointensity combined with T2 hyperintensity in the spinal cord indicates myelomalacia (permanent cystic necrosis/gliosis of the cord). This finding is strongly correlated with a poor prognosis for neurologic recovery even after adequate surgical decompression. T2 hyperintensity alone may indicate reversible edema.
Question 44:
A 24-year-old man sustains a proximal pole scaphoid fracture after a fall on an outstretched hand. He is counseled regarding the high risk of nonunion and avascular necrosis associated with this specific fracture pattern. Which of the following accurately describes the primary blood supply to the proximal pole of the scaphoid?
Options:
- Retrograde blood flow from the dorsal carpal branch of the radial artery
- Antegrade blood flow from the superficial palmar arch
- Direct branches from the anterior interosseous artery
- Retrograde blood flow from the ulnar artery via the deep palmar arch
- Antegrade blood flow from the volar carpal branch of the radial artery
Correct Answer: Retrograde blood flow from the dorsal carpal branch of the radial artery
Explanation:
The scaphoid receives its primary blood supply from the dorsal carpal branch of the radial artery, which enters the bone distally and provides retrograde blood flow to the proximal pole. This retrograde supply makes proximal pole fractures particularly vulnerable to avascular necrosis and nonunion.
Question 45:
A 12-year-old boy with a BMI of 32 presents with a 4-week history of vague left knee pain and an antalgic gait. Radiographs reveal a mild, stable slipped capital femoral epiphysis (SCFE) of the left hip. He is taken to the operating room for in situ pinning. To minimize the risk of joint penetration and adequately stabilize the epiphysis, the starting point for the screw should be located on the:
Options:
- Posterior aspect of the femoral neck
- Anterior aspect of the femoral neck
- Direct lateral aspect of the greater trochanter
- Inferior aspect of the femoral neck
- Superior aspect of the femoral neck
Correct Answer: Anterior aspect of the femoral neck
Explanation:
In a slipped capital femoral epiphysis, the epiphysis displaces posteriorly and inferiorly relative to the femoral neck. To correctly trajectory a single screw perpendicular to the physis and into the center of the displaced epiphysis without violating the posterior cortex of the femoral neck, an anterior and superior starting point on the metaphysis/neck is required.
Question 46:
A 35-year-old male sustains a transverse midshaft radius fracture. He undergoes open reduction and internal fixation with a 3.5 mm dynamic compression plate placed in absolute stability. Which of the following best describes the predominant mechanism of bone healing expected in this scenario?
Options:
- Endochondral ossification with a cartilaginous intermediate
- Primary bone healing characterized by osteoclast-led cutting cones followed by osteoblasts
- Intramembranous ossification with robust callus formation
- Chondroid metaplasia within the fracture hematoma
- Secondary bone healing driven by micromotion at the fracture site
Correct Answer: Primary bone healing characterized by osteoclast-led cutting cones followed by osteoblasts
Explanation:
Absolute stability (rigid fixation with anatomic reduction and no gap) eliminates interfragmentary strain, bypassing callus formation. It leads to primary (direct) bone healing, which occurs via Haversian remodeling driven by osteoclast-led cutting cones followed immediately by osteoblasts laying down new bone.
Question 47:
A 42-year-old recreational athlete sustains an acute, complete rupture of the Achilles tendon. He opts for non-operative management and is enrolled in a functional rehabilitation protocol featuring early weight-bearing in a functional brace. Compared to traditional management involving prolonged non-weight-bearing cast immobilization, functional rehabilitation is associated with:
Options:
- A significantly higher rate of tendon rerupture
- A significantly lower rate of tendon rerupture
- A higher incidence of deep vein thrombosis
- Similar rerupture rates but improved early functional outcomes and faster return to work
- Inferior plantarflexion strength at 1 year
Correct Answer: Similar rerupture rates but improved early functional outcomes and faster return to work
Explanation:
Recent high-level evidence demonstrates that for acute Achilles tendon ruptures, non-operative management utilizing an early functional rehabilitation protocol (early weight-bearing and controlled range of motion in a brace) provides similar rerupture rates to surgical repair and traditional casting, while improving early functional outcomes, reducing DVT risk, and expediting return to work compared to prolonged immobilization.
Question 48:
A 20-year-old collegiate female basketball player undergoes an anterior cruciate ligament reconstruction using a bone-patellar tendon-bone (BTB) autograft. She successfully completes rehabilitation and returns to play at 9 months. Which of the following is the most commonly reported complication specifically associated with this choice of graft compared to hamstring autograft?
Options:
- Increased incidence of deep surgical site infection
- Higher rate of graft rupture upon return to sport
- Anterior knee pain, particularly with kneeling
- Persistent saphenous nerve neuropathy
- Hamstring weakness and delayed sprint speed recovery
Correct Answer: Anterior knee pain, particularly with kneeling
Explanation:
The most common and specific complication associated with the use of a bone-patellar tendon-bone (BTB) autograft is donor site morbidity, manifesting primarily as anterior knee pain and pain with kneeling. Saphenous nerve injury and hamstring weakness are more commonly associated with hamstring autografts.
Question 49:
A 14-year-old boy presents with worsening knee pain and swelling. Radiographs demonstrate a mixed lytic and sclerotic lesion in the distal femoral metaphysis with a 'sunburst' periosteal reaction. Biopsy confirms a high-grade intramedullary osteosarcoma. Which of the following represents the standard, most appropriate treatment algorithm for this patient?
Options:
- Immediate wide surgical resection followed by adjuvant radiation therapy
- Neoadjuvant chemotherapy, wide surgical resection, and adjuvant chemotherapy
- Neoadjuvant radiation therapy, wide surgical resection, and adjuvant chemotherapy
- Isolated wide surgical resection with negative margins
- Intralesional curettage, cementation, and adjuvant chemotherapy
Correct Answer: Neoadjuvant chemotherapy, wide surgical resection, and adjuvant chemotherapy
Explanation:
The standard of care for high-grade conventional intramedullary osteosarcoma is multi-agent neoadjuvant chemotherapy, followed by definitive surgical local control (limb-salvage wide resection or amputation), and concluding with adjuvant chemotherapy. Osteosarcoma is generally considered radioresistant, so radiation therapy is not a primary modality unless the tumor is unresectable.
Question 50:
A 28-year-old motorcyclist is involved in a high-speed collision and sustains an anterior-posterior compression (APC) type III pelvic ring injury. According to the Young-Burgess classification, this injury pattern is characterized by the complete disruption of the symphysis pubis and which of the following posterior ligamentous complexes?
Options:
- Anterior sacroiliac, sacrospinous, and sacrotuberous ligaments only
- Anterior sacroiliac, sacrospinous, sacrotuberous, and posterior sacroiliac ligaments
- Posterior sacroiliac ligaments only
- Iliolumbar ligaments only
- Sacrospinous and sacrotuberous ligaments only
Correct Answer: Anterior sacroiliac, sacrospinous, sacrotuberous, and posterior sacroiliac ligaments
Explanation:
An APC III pelvic injury involves complete disruption of both the anterior and posterior pelvic rings. This includes the symphysis pubis anteriorly, and all of the posterior ligamentous structures: the anterior sacroiliac ligaments, the pelvic floor ligaments (sacrospinous and sacrotuberous), and the strong posterior sacroiliac ligaments, leading to complete global instability of the hemipelvis.
Question 51:
A 58-year-old male with a history of a metal-on-metal total hip arthroplasty performed 8 years ago presents with progressive groin pain and swelling. Laboratory evaluation reveals significantly elevated serum cobalt and chromium ion levels. MRI demonstrates a large, thick-walled fluid collection. Histologic analysis of the periprosthetic tissue is most likely to show an adverse local tissue reaction (ALVAL) characterized by:
Options:
- Abundant neutrophils and intracellular gram-positive cocci
- A dense perivascular infiltrate of lymphocytes, indicative of a Type IV delayed hypersensitivity reaction
- Extensive sheets of foamy macrophages containing polyethylene debris
- A predominant eosinophilic infiltrate consistent with a Type I IgE-mediated allergy
- Myxoid degeneration and chondroid metaplasia
Correct Answer: A dense perivascular infiltrate of lymphocytes, indicative of a Type IV delayed hypersensitivity reaction
Explanation:
Adverse Local Tissue Reaction (ALTR) or Aseptic Lymphocyte-Dominated Vasculitis-Associated Lesion (ALVAL) in response to metal wear debris from metal-on-metal implants is histologically characterized by a dense perivascular lymphocytic infiltrate. This represents a Type IV (cell-mediated) delayed hypersensitivity reaction to metal ions.
Question 52:
A 30-year-old carpenter sustains a laceration to his dominant index finger, resulting in a Zone II injury of both the flexor digitorum superficialis (FDS) and flexor digitorum profundus (FDP). Postoperatively, the hand therapist initiates an early active motion rehabilitation protocol. The primary rationale for utilizing early active motion over prolonged immobilization in this specific scenario is to:
Options:
- Increase the tensile strength of the tendon faster than immobilization
- Promote primary tendon healing without a cellular phase
- Prevent the formation of restrictive peritendinous adhesions while minimizing the risk of rupture
- Allow early return to heavy manual labor within 3 weeks
- Prevent contracture of the lumbrical muscles
Correct Answer: Prevent the formation of restrictive peritendinous adhesions while minimizing the risk of rupture
Explanation:
Early active or passive motion protocols following flexor tendon repair in Zone II are critical to facilitate intrinsic tendon healing and promote tendon glide. This movement helps prevent the formation of restrictive peritendinous adhesions (which limit excursion) while providing enough controlled stress to stimulate healing without rupturing the repair.
Question 53:
A 75-year-old male with severe neurogenic claudication secondary to multilevel lumbar spinal stenosis is considering surgical intervention after failing 6 months of conservative treatment. Which of the following preoperative clinical features is most predictive of a highly successful outcome following a lumbar laminectomy and decompression?
Options:
- Predominance of axial low back pain over radicular leg symptoms
- Presence of profound bilateral foot drop
- Symptom relief with lumbar extension
- Predominance of radicular leg pain and claudication over axial back pain
- Concomitant severe diabetic peripheral neuropathy
Correct Answer: Predominance of radicular leg pain and claudication over axial back pain
Explanation:
In patients with lumbar spinal stenosis, decompression surgery (laminectomy) is highly effective at relieving radicular leg pain and neurogenic claudication. Patients whose primary complaint is axial back pain often have poorer outcomes, as decompression alone does not address back pain reliably.
Question 54:
A 7-month-old female infant is evaluated for developmental dysplasia of the hip (DDH). She was initially treated with a Pavlik harness starting at 6 weeks of age, but the hip remained irreducible. Subsequent attempts at weaning and re-application have failed. Radiographs show a persistently dislocated left hip with acetabular dysplasia. What is the most appropriate next step in management?
Options:
- Re-application of the Pavlik harness for an additional 6 weeks
- Application of an abduction orthosis (e.g., Ilfeld splint)
- Closed reduction under general anesthesia and spica casting
- Open reduction, pelvic osteotomy, and femoral shortening osteotomy
- Observation until skeletal maturity, followed by total hip arthroplasty
Correct Answer: Closed reduction under general anesthesia and spica casting
Explanation:
If Pavlik harness treatment fails to achieve or maintain a reduction in an infant with DDH, the harness should be discontinued to avoid 'Pavlik harness disease' (damage to the posterior acetabular wall) and AVN. The next definitive step in management for a child typically between 6 and 18 months of age is closed reduction under general anesthesia followed by spica casting.
Question 55:
A 25-year-old athlete sustains a midfoot injury after a forceful plantarflexion mechanism. Radiographs demonstrate widening of the space between the base of the first and second metatarsals. MRI confirms a complete rupture of the Lisfranc ligament. Anatomically, the Lisfranc ligament is an interosseous ligament that connects the:
Options:
- Medial cuneiform to the base of the second metatarsal
- Intermediate cuneiform to the base of the second metatarsal
- Lateral cuneiform to the base of the third metatarsal
- Medial cuneiform to the base of the first metatarsal
- Navicular to the base of the first metatarsal
Correct Answer: Medial cuneiform to the base of the second metatarsal
Explanation:
The Lisfranc ligament is a strong interosseous ligament that originates from the lateral aspect of the medial cuneiform and inserts onto the medial aspect of the base of the second metatarsal. It is a critical stabilizer of the tarsometatarsal joint complex.
Question 56:
Articular cartilage is a highly specialized tissue designed to withstand significant compressive loads. The mechanical properties of cartilage vary across its depth. Which of the following correctly describes the biochemical composition of the deep zone of articular cartilage?
Options:
- Highest concentration of water and highest concentration of proteoglycans
- Highest concentration of water and lowest concentration of proteoglycans
- Lowest concentration of water and highest concentration of proteoglycans
- Lowest concentration of water and lowest concentration of proteoglycans
- Highest concentration of Type I collagen
Correct Answer: Lowest concentration of water and highest concentration of proteoglycans
Explanation:
Articular cartilage composition varies by zone. The superficial zone has the highest water content and lowest proteoglycan content. In contrast, the deep zone has the lowest water content and the highest concentration of proteoglycans, allowing it to provide maximal resistance to compressive forces.
Question 57:
A 22-year-old male undergoes arthroscopic evaluation of the knee for a medial meniscus tear. The surgeon must decide between meniscal repair and partial meniscectomy. The potential for meniscal healing is primarily dictated by its vascular supply. Which area of the meniscus possesses the greatest intrinsic potential for healing following surgical repair?
Options:
- The inner third (white-white zone)
- The middle third (red-white zone)
- The peripheral third (red-red zone)
- The anterior horn exclusively
- The posterior root exclusively
Correct Answer: The peripheral third (red-red zone)
Explanation:
The vascular supply to the meniscus originates from the perimeniscal capillary plexus, which supplies only the peripheral 10% to 30% of the meniscus. Tears in this peripheral third (the 'red-red' zone) have robust blood supply and the highest potential for healing following surgical repair.
Question 58:
A 32-year-old female presents with a 3-month history of progressive left knee pain. Radiographs reveal an expansile, purely lytic lesion in the epiphysis of the proximal tibia, extending to the subchondral bone. A biopsy confirms the diagnosis of a Giant Cell Tumor (GCT) of bone. Staging workup is negative for metastases. Which of the following is the most appropriate primary surgical treatment?
Options:
- Marginal excision with a 1 cm margin
- Intralesional curettage alone
- Extended intralesional curettage with high-speed burring, local adjuvants, and defect filling
- Wide en bloc resection and endoprosthetic reconstruction
- Above-knee amputation
Correct Answer: Extended intralesional curettage with high-speed burring, local adjuvants, and defect filling
Explanation:
Giant cell tumors of bone are locally aggressive benign tumors. The standard treatment to minimize the risk of local recurrence while preserving joint function is extended intralesional curettage (using a high-speed burr), followed by the application of local adjuvants (such as phenol, argon beam, or hydrogen peroxide) to kill remaining microscopic disease, and filling the defect with bone graft or PMMA cement.
Question 59:
A 26-year-old male is admitted after sustaining a severely comminuted, closed fracture of the tibial shaft. He develops escalating leg pain out of proportion to his injury. Examination reveals tense compartments and pain with passive stretch of the toes. Intracompartmental pressure testing is performed. Which of the following pressure measurements (Delta P = Diastolic Blood Pressure - Compartment Pressure) is widely considered the absolute indication for emergent fasciotomy?
Options:
- Delta P greater than 45 mmHg
- Delta P less than 30 mmHg
- Absolute compartment pressure greater than 15 mmHg
- Absolute compartment pressure greater than 20 mmHg
- Delta P less than 10 mmHg
Correct Answer: Delta P less than 30 mmHg
Explanation:
The diagnosis of acute compartment syndrome is primarily clinical, but when objective measurements are needed, the 'Delta P' is used. A Delta P (diastolic blood pressure minus intracompartmental pressure) of less than 30 mmHg indicates inadequate tissue perfusion and is a universally accepted absolute indication for emergent fasciotomy.
Question 60:
A 68-year-old female is undergoing a primary posterior-stabilized total knee arthroplasty. During trialing, the surgeon notes that the knee is perfectly balanced in full extension, but the flexion gap is unacceptably tight, limiting flexion to 80 degrees and causing posterior lift-off of the tibial tray. Which of the following surgical adjustments is the most appropriate maneuver to balance the knee?
Options:
- Resect more distal femur
- Decrease the posterior slope of the tibial cut
- Upsize the femoral component
- Downsize the femoral component using an anterior referencing guide
- Release the posterior capsule
Correct Answer: Downsize the femoral component using an anterior referencing guide
Explanation:
A tight flexion gap with a balanced extension gap means the AP dimension of the femoral component is too large, or the posterior tibial slope is inadequate. Downsizing the femoral component (when using an anterior referencing system) reduces the posterior condylar offset, thereby specifically opening the flexion gap without affecting the extension gap. Increasing (not decreasing) the posterior tibial slope would also be an option.
Question 61:
A 65-year-old male is undergoing a total hip arthroplasty via the direct anterior approach. Which of the following best describes the deep internervous plane utilized during this approach?
Options:
- Between sartorius and tensor fasciae latae
- Between rectus femoris and gluteus medius
- Between gluteus medius and minimus
- Between tensor fasciae latae and gluteus medius
- Between pectineus and psoas
Correct Answer: Between rectus femoris and gluteus medius
Explanation:
The direct anterior (Smith-Petersen) approach to the hip utilizes a superficial and a deep internervous plane. The superficial plane is between the sartorius (innervated by the femoral nerve) and the tensor fasciae latae (innervated by the superior gluteal nerve). The deep interval is between the rectus femoris (femoral nerve) and the gluteus medius (superior gluteal nerve).
Question 62:
A 45-year-old male sustains a complex tibial plateau fracture involving a displaced posteromedial fragment. The surgeon elects to use a posteromedial approach for open reduction and internal fixation. This approach utilizes an interval between which of the following structures?
Options:
- Medial head of the gastrocnemius and the soleus
- Medial head of the gastrocnemius and the pes anserinus
- Semimembranosus and semitendinosus
- Popliteus and medial head of the gastrocnemius
- Tibialis posterior and flexor digitorum longus
Correct Answer: Medial head of the gastrocnemius and the pes anserinus
Explanation:
The posteromedial approach to the proximal tibia is the standard approach for addressing posteromedial shear fragments in tibial plateau fractures. The surgical interval exploits the space between the medial head of the gastrocnemius (which is retracted laterally) and the pes anserinus tendons (which are retracted medially and anteriorly).
Question 63:
Bone morphogenetic proteins (BMPs) are members of the TGF-beta superfamily. Recombinant human BMP-2 (rhBMP-2) has been approved by the FDA for specific clinical applications. Which of the following is an FDA-approved indication for the use of rhBMP-2?
Options:
- Acute open tibial shaft fractures
- Recalcitrant nonunion of the humeral shaft
- Posterolateral lumbar fusion
- Treatment of unicameral bone cysts
- Acute closed femoral shaft fractures
Correct Answer: Acute open tibial shaft fractures
Explanation:
rhBMP-2 (Infuse) is FDA-approved for the treatment of acute, open tibial shaft fractures stabilized with an intramedullary nail within 14 days of injury, as well as for anterior lumbar interbody fusion (ALIF). Recombinant human BMP-7 (OP-1) was historically approved for long bone nonunions and revision posterolateral lumbar fusion, though its availability has changed.
Question 64:
A 9-year-old boy presents with right hip pain and a limp. Radiographs confirm a slipped capital femoral epiphysis (SCFE). His weight is in the 40th percentile for his age. In addition to in situ pinning of the right hip, which of the following is the most appropriate next step in management?
Options:
- Prophylactic pinning of the contralateral hip
- Closed reduction and spica casting
- Endocrine evaluation including TSH, free T4, BUN, and creatinine
- MRI of the bilateral hips
- Open reduction and surgical subluxation
Correct Answer: Endocrine evaluation including TSH, free T4, BUN, and creatinine
Explanation:
SCFE typically affects obese adolescents between the ages of 10 and 16. Atypical presentations include patients younger than 10 or older than 16, those with a weight less than the 50th percentile, and those with bilateral involvement at presentation. These atypical presentations strongly warrant an endocrine and metabolic workup to rule out underlying disorders such as hypothyroidism or renal osteodystrophy.
Question 65:
A 24-year-old man falls onto an outstretched hand and sustains an acute, minimally displaced fracture of the proximal pole of the scaphoid. Because of the specific vascular anatomy of the scaphoid, which of the following is the most widely recommended treatment for this injury?
Options:
- Short arm thumb spica cast for 6 weeks
- Long arm thumb spica cast for 12 weeks
- Percutaneous or open screw fixation
- Proximal row carpectomy
- Scaphoid excision and four-corner fusion
Correct Answer: Percutaneous or open screw fixation
Explanation:
The blood supply to the scaphoid enters distally via branches of the radial artery and flows retrograde to the proximal pole. Because of this tenuous vascular supply, proximal pole fractures have a very high rate of nonunion and avascular necrosis. Operative fixation (percutaneous or open) is recommended even for non-displaced proximal pole fractures to optimize the biomechanical environment for healing.
Question 66:
Following an anterior cruciate ligament (ACL) reconstruction using a bone-patellar tendon-bone autograft, a patient exhibits a lack of full knee flexion but achieves full extension. The physical examination reveals a tight graft in flexion. Which of the following technical errors during graft placement most likely accounts for this finding?
Options:
- Femoral tunnel placed too anteriorly
- Femoral tunnel placed too posteriorly
- Tibial tunnel placed too anteriorly
- Tibial tunnel placed too posteriorly
- Graft tensioned in full flexion
Correct Answer: Femoral tunnel placed too anteriorly
Explanation:
Placement of the femoral tunnel in ACL reconstruction is critical for graft isometry. If the femoral tunnel is placed too anteriorly, the distance between the femoral and tibial origins increases as the knee flexes. This results in a graft that is tight in flexion (causing loss of flexion) and lax in extension.
Question 67:
A 16-year-old female with a diagnosis of Charcot-Marie-Tooth disease presents with a progressive, symptomatic cavovarus foot deformity. During clinical evaluation, her first ray is noted to be rigidly plantarflexed. This specific component of her deformity is primarily driven by the unopposed action of which muscle?
Options:
- Tibialis anterior
- Tibialis posterior
- Peroneus brevis
- Peroneus longus
- Extensor hallucis longus
Correct Answer: Peroneus longus
Explanation:
In Charcot-Marie-Tooth (CMT) disease, the classic cavovarus foot deformity is driven by specific muscle imbalances. The tibialis anterior and peroneus brevis weaken early. The relatively preserved strength of the peroneus longus, which is unopposed by the weak tibialis anterior, powerfully plantarflexes the first ray, causing the forefoot-driven cavus deformity.
Question 68:
A 65-year-old male presents with deteriorating hand dexterity and gait imbalance. On physical examination, tapping the distal brachioradialis tendon results in diminished reflex elbow flexion, but elicits spontaneous flexion of the ipsilateral fingers. This physical exam finding localizes the spinal cord pathology to which of the following levels?
Options:
- C3-C4
- C4-C5
- C5-C6
- C6-C7
- C7-T1
Correct Answer: C5-C6
Explanation:
The inverted brachioradialis reflex is a specific clinical sign for cervical spondylotic myelopathy. It consists of an absent or diminished brachioradialis reflex (a lower motor neuron finding at C5-C6) coupled with hyperactive finger flexion (an upper motor neuron finding for levels below C6). This combination localizes the primary compressive pathology to the C5-C6 level.
Question 69:
A 14-year-old boy presents with progressive knee pain and swelling. Radiographs reveal a poorly marginated, bone-forming lesion in the distal femoral metaphysis with elevation of the periosteum forming a Codman's triangle. A biopsy confirms conventional osteosarcoma. Mutations in which of the following pairs of tumor suppressor genes are most commonly implicated in the pathogenesis of this condition?
Options:
- BRCA1 and PTEN
- RB1 and TP53
- APC and MLH1
- NF1 and NF2
- VHL and WT1
Correct Answer: RB1 and TP53
Explanation:
Conventional osteosarcoma is highly malignant and characterized by the production of osteoid by tumor cells. The pathogenesis is strongly associated with mutations in the RB1 (retinoblastoma) and TP53 (p53) tumor suppressor genes. Patients with hereditary retinoblastoma or Li-Fraumeni syndrome (germline TP53 mutation) have a significantly increased risk of developing osteosarcoma.
Question 70:
In the context of wear mechanisms in total joint arthroplasty, the generation of wear debris between the non-articulating backside of a polyethylene acetabular liner and the inner surface of a metallic acetabular shell is classified as which of the following?
Options:
- Mode I wear
- Mode II wear
- Mode III wear
- Mode IV wear
- Adhesive wear
Correct Answer: Mode IV wear
Explanation:
Wear in total joint arthroplasty is categorized into four modes. Mode I occurs between two intended bearing surfaces (e.g., femoral head and polyethylene liner). Mode II occurs when a primary bearing surface rubs against a non-intended secondary surface (e.g., femoral head against metallic shell after liner wear-through). Mode III is third-body wear caused by loose particles. Mode IV wear occurs between two non-primary bearing surfaces rubbing against each other, such as backside wear between the polyethylene liner and the metallic acetabular shell.
Question 71:
A trauma surgeon is performing an ilioinguinal approach to the anterior pelvis for the fixation of an anterior column acetabular fracture. During dissection over the superior pubic ramus, brisk arterial bleeding is encountered. This bleeding is most likely originating from an anastomosis between the obturator vessels and branches of which of the following?
Options:
- Internal iliac artery
- External iliac or inferior epigastric artery
- Superior gluteal artery
- Internal pudendal artery
- Deep circumflex iliac artery
Correct Answer: External iliac or inferior epigastric artery
Explanation:
The 'corona mortis' (crown of death) is an important vascular anastomosis located over the posterior aspect of the superior pubic ramus, approximately 5-6 cm lateral to the pubic symphysis. It connects the obturator system (internal iliac system) with the external iliac or inferior epigastric vessels. It is vulnerable to injury during anterior pelvic approaches and can cause significant hemorrhage.
Question 72:
A 2-week-old infant is brought to the clinic for management of a rigid idiopathic clubfoot using the Ponseti method. What is the essential first maneuver performed during the application of the initial corrective cast?
Options:
- Dorsiflexion of the ankle to correct equinus
- Pronation of the forefoot to correct forefoot adduction
- Supination of the forefoot with elevation of the first ray to correct the cavus
- Eversion of the calcaneus to correct hindfoot varus
- External rotation of the foot while blocking the calcaneus
Correct Answer: Supination of the forefoot with elevation of the first ray to correct the cavus
Explanation:
The Ponseti method addresses clubfoot deformity in a specific sequence (CAVE: Cavus, Adductus, Varus, Equinus). The first step is to correct the cavus deformity. This is achieved by supinating the forefoot (specifically elevating the first ray) to align the forefoot with the already pronated hindfoot. Subsequent casts correct adductus and varus by laterally directing the forefoot against the talar head, and equinus is corrected last (often requiring a percutaneous Achilles tenotomy).
Question 73:
The 'glenoid track' concept is utilized to evaluate bipolar bone loss in anterior shoulder instability. A Hill-Sachs lesion is considered 'off-track' and at risk for engaging the anterior glenoid rim if its medial margin is located where?
Options:
- Lateral to the medial margin of the glenoid track
- Medial to the medial margin of the glenoid track
- Superior to the superior margin of the glenoid track
- Inferior to the inferior margin of the glenoid track
- Exactly on the greater tuberosity footprint
Correct Answer: Medial to the medial margin of the glenoid track
Explanation:
The glenoid track represents the contact zone of the glenoid on the humeral head during shoulder abduction and external rotation. Its width is determined by the native glenoid width minus the anterior glenoid bone loss. A Hill-Sachs lesion is 'off-track' (meaning it will engage the anterior glenoid rim, leading to dislocation) if the medial margin of the lesion extends medial to the medial margin of the calculated glenoid track.
Question 74:
A 32-year-old mechanic sustains a volar laceration to his middle finger at the level of the proximal phalanx, resulting in a loss of active flexion at both the proximal and distal interphalangeal joints. This injury is located within which flexor tendon zone?
Options:
- Zone I
- Zone II
- Zone III
- Zone IV
- Zone V
Correct Answer: Zone II
Explanation:
Verdan's flexor tendon zones classify the anatomical locations of flexor tendon injuries. Zone II (historically called 'no man's land' due to historically poor surgical outcomes) extends from the proximal aspect of the A1 pulley (distal palmar crease) to the insertion of the flexor digitorum superficialis (FDS) on the middle phalanx. Lacerations here frequently involve both the FDS and flexor digitorum profundus (FDP) tendons within the tight fibro-osseous sheath.
Question 75:
The Lisfranc ligament is a critical stabilizing structure of the tarsometatarsal joint complex. Which of the following best describes its anatomic origin and insertion?
Options:
- Medial aspect of the medial cuneiform to the medial aspect of the first metatarsal base
- Lateral aspect of the medial cuneiform to the medial aspect of the second metatarsal base
- Medial aspect of the middle cuneiform to the lateral aspect of the second metatarsal base
- Lateral aspect of the medial cuneiform to the base of the third metatarsal
- Distal aspect of the navicular to the base of the second metatarsal
Correct Answer: Lateral aspect of the medial cuneiform to the medial aspect of the second metatarsal base
Explanation:
The Lisfranc ligament is an intra-articular interosseous ligament that provides vital stability to the midfoot. It originates from the lateral aspect of the medial cuneiform and inserts onto the medial aspect of the base of the second metatarsal. Notably, there is no direct intermetatarsal ligament connecting the bases of the first and second metatarsals, making this link crucial for structural integrity.
Question 76:
In a posterior-stabilized total knee arthroplasty (TKA), the posterior cruciate ligament is resected. Which specific design feature of the implant is intended to substitute for the function of the posterior cruciate ligament by facilitating femoral rollback during knee flexion?
Options:
- The symmetric conformity of the polyethylene insert
- The posterior slope built into the tibial baseplate
- The interaction between the femoral cam and the polyethylene tibial post
- The extension of the anterior femoral flange
- The deep trochlear groove
Correct Answer: The interaction between the femoral cam and the polyethylene tibial post
Explanation:
In a posterior-stabilized (PS) TKA, the native posterior cruciate ligament (PCL) is excised. To replicate its biomechanical role, the implant incorporates a central polyethylene post on the tibial insert and a metallic cam on the femoral component. As the knee flexes, the femoral cam engages the tibial post, forcibly driving the femur posteriorly (femoral rollback). This increases knee flexion clearance and improves the lever arm of the extensor mechanism.
Question 77:
A 28-year-old male falls from a height and sustains a thoracolumbar spinal fracture. A CT scan confirms a burst fracture at L1. According to the Denis three-column theory of spinal stability, a burst fracture is characterized by the biomechanical failure of which columns under an axial load?
Options:
- Anterior column only
- Anterior and middle columns
- Middle and posterior columns
- Anterior and posterior columns
- Anterior, middle, and posterior columns
Correct Answer: Anterior and middle columns
Explanation:
According to the Denis classification system, spinal stability is assessed using a three-column model. The anterior column consists of the anterior longitudinal ligament and the anterior half of the vertebral body/disc. The middle column comprises the posterior half of the body/disc and the posterior longitudinal ligament. The posterior column includes the pedicles, facets, and posterior ligamentous complex. A burst fracture, resulting from axial loading, involves failure of both the anterior and middle columns, potentially retropulsing bone fragments into the spinal canal.
Question 78:
A 5-year-old girl falls off monkey bars and presents with a Gartland type III extension-type supracondylar humerus fracture. The hand is pink, well-perfused, but she is unable to flex the interphalangeal joint of her thumb and the distal interphalangeal joint of her index finger. Which of the following nerve structures has most likely been injured?
Options:
- Radial nerve
- Ulnar nerve
- Anterior interosseous nerve
- Musculocutaneous nerve
- Recurrent motor branch of the median nerve
Correct Answer: Anterior interosseous nerve
Explanation:
The anterior interosseous nerve (AIN), a motor branch of the median nerve, is the most commonly injured nerve in extension-type supracondylar humerus fractures. It innervates the flexor pollicis longus, the lateral half of the flexor digitorum profundus (index and middle fingers), and the pronator quadratus. Clinically, AIN function is assessed by having the patient form an 'OK' sign. Failure to do so (resulting in a flattened pinch mechanism) indicates an AIN palsy.
Question 79:
Articular cartilage is a complex tissue structured into distinct zones. Which zone contains chondrocytes arranged in vertical columns, has collagen fibers oriented perpendicular to the joint surface, and possesses the highest concentration of proteoglycans?
Options:
- Superficial tangential zone
- Middle (transitional) zone
- Deep (radial) zone
- Calcified cartilage zone
- Tidemark
Correct Answer: Deep (radial) zone
Explanation:
Articular cartilage consists of four structural zones. The deep (or radial) zone contains chondrocytes organized in vertical columns parallel to the collagen fibers, which are themselves oriented perpendicular to the articular surface. This architecture provides maximum resistance to compressive forces. The deep zone also contains the highest concentration of proteoglycans and the lowest water content of the uncalcified layers.
Question 80:
A 15-year-old boy presents with localized pain and swelling in his left mid-thigh, accompanied by a low-grade fever. Radiographs display a permeative, destructive diaphyseal lesion of the femur with a lamellated 'onion-skin' periosteal reaction. Histology shows sheets of uniform, small round blue cells. The most characteristic cytogenetic abnormality associated with this tumor is:
Options:
- t(11;22)(q24;q12)
- t(9;22)(q34;q11)
- t(X;18)(p11;q11)
- t(12;16)(q13;p11)
- t(2;13)(q35;q14)
Correct Answer: t(11;22)(q24;q12)
Explanation:
The clinical presentation, radiographic findings (diaphyseal lesion, onion-skin periosteal reaction), and histology (small round blue cells) are diagnostic for Ewing sarcoma. The hallmark cytogenetic abnormality is the t(11;22)(q24;q12) chromosomal translocation, which is present in over 85% of cases and results in the formation of the EWS-FLI1 fusion transcript.
Question 81:
Review the clinical image. What is the earliest radiographic change expected in the natural progression of Scaphoid Nonunion Advanced Collapse (SNAC) if left untreated?
Options:
- Radioscaphoid joint arthritis (radial styloid)
- Capitolunate joint arthritis
- Scaphotrapezial joint arthritis
- Radiolunate joint arthritis
- Ulnocarpal arthritis
Correct Answer: Radioscaphoid joint arthritis (radial styloid)
Explanation:
Scaphoid Nonunion Advanced Collapse (SNAC) follows a predictable pattern of degenerative changes. Stage I involves arthritis isolated to the articulation between the scaphoid and the radial styloid. Stage II progresses to involve the entire radioscaphoid joint. Stage III involves the capitolunate joint. The radiolunate joint is characteristically spared because the lunate fossa cartilage remains concentric with the lunate.
Question 82:
A 65-year-old female undergoes a posterior approach total hip arthroplasty as shown in the postoperative radiograph. She suffers a posterior dislocation 3 weeks postoperatively while rising from a low chair. Which of the following component positions increases the risk of posterior dislocation?
Options:
- Increased acetabular anteversion
- Decreased acetabular anteversion
- Increased acetabular inclination
- Increased femoral offset
- Increased femoral anteversion
Correct Answer: Decreased acetabular anteversion
Explanation:
Posterior instability in total hip arthroplasty is exacerbated by positions of flexion, internal rotation, and adduction. Component malpositions that predispose to posterior dislocation include decreased acetabular anteversion (retroversion), decreased femoral anteversion, and insufficient femoral offset.
Question 83:
An 11-year-old boy presents with a painful mass on his thigh and fever. Radiographs show a permeative diaphyseal lesion with an 'onion skin' periosteal reaction. Biopsy reveals small round blue cells. Which chromosomal translocation is most characteristic of this tumor?
Options:
- t(11;22)
- t(9;22)
- t(X;18)
- t(12;16)
- t(2;13)
Correct Answer: t(11;22)
Explanation:
Ewing sarcoma is characterized by small, round, blue cells and classically presents in the diaphysis of long bones with an 'onion skin' periosteal reaction. It is associated with the t(11;22)(q24;q12) translocation, resulting in the EWS-FLI1 fusion protein in approximately 85% of cases.
Question 84:
According to the 2018 International Consensus Meeting (ICM) criteria for periprosthetic joint infection (PJI), which of the following is considered a major criterion?
Options:
- Elevated serum CRP > 10 mg/L
- Positive leukocyte esterase strip test
- Two positive periprosthetic tissue cultures with identical organisms
- Synovial fluid WBC > 3000 cells/uL
- Elevated serum D-dimer
Correct Answer: Two positive periprosthetic tissue cultures with identical organisms
Explanation:
The ICM criteria state that the presence of either a sinus tract communicating with the joint or two positive periprosthetic tissue/fluid cultures with phenotypically identical organisms serves as definitive (major) evidence of PJI. The other options are considered minor criteria.
Question 85:
A 35-year-old male sustains a severe pelvic injury in an MVA. A spur sign, which is pathognomonic for a both-column acetabular fracture, is identified. This sign is best visualized on which of the following radiographic views?
Options:
- AP pelvis
- Iliac oblique
- Obturator oblique
- Inlet view
- Outlet view
Correct Answer: Obturator oblique
Explanation:
The spur sign represents the inferior portion of the intact superior ilium that has been left behind when the articular segment is displaced medially. It is pathognomonic for a both-column fracture of the acetabulum and is best visualized on the obturator oblique radiograph of the Judet series.
Question 86:
A 24-year-old pitcher undergoes arthroscopic repair of a type II SLAP lesion. Postoperatively, he notes significant weakness with external rotation and a vague, aching pain in the posterior shoulder. Physical examination reveals atrophy of the infraspinatus. Which of the following is the most likely cause?
Options:
- Suprascapular nerve entrapment at the spinoglenoid notch
- Axillary nerve injury
- Musculocutaneous nerve injury
- Suprascapular nerve entrapment at the suprascapular notch
- Radial nerve injury
Correct Answer: Suprascapular nerve entrapment at the spinoglenoid notch
Explanation:
Repair of SLAP lesions, specifically when placing posterior anchors or passing sutures at the posterosuperior labrum, places the suprascapular nerve at risk as it passes through the spinoglenoid notch. Injury here predominantly causes isolated denervation and atrophy of the infraspinatus, sparing the supraspinatus.
Question 87:
Which zone of articular cartilage has the highest concentration of proteoglycans and the lowest concentration of water?
Options:
- Superficial (tangential) zone
- Middle (transitional) zone
- Deep (radial) zone
- Calcified cartilage zone
- Subchondral bone
Correct Answer: Deep (radial) zone
Explanation:
The deep (radial) zone of articular cartilage contains the lowest water content, highest proteoglycan concentration, and the largest diameter collagen fibrils which are oriented perpendicular to the joint surface to resist compressive forces.
Question 88:
During surgical decompression of the ulnar nerve at the elbow, an anatomical release is planned. What is the most proximal potential site of ulnar nerve compression that must be evaluated?
Options:
- Arcade of Struthers
- Medial intermuscular septum
- Osborne's ligament
- Aponeurosis of the flexor carpi ulnaris
- Deep flexor pronator aponeurosis
Correct Answer: Arcade of Struthers
Explanation:
The potential sites of ulnar nerve compression around the elbow from proximal to distal include: the Arcade of Struthers (about 8 cm proximal to the medial epicondyle), the medial intermuscular septum, the medial epicondyle itself, Osborne's ligament (cubital tunnel), and the deep aponeurosis of the FCU.
Question 89:
A 55-year-old diabetic male presents with back pain, fever, and progressive bilateral lower extremity weakness. MRI reveals a spinal epidural abscess compressing the thoracic spinal cord. What is the most common causative organism?
Options:
- Pseudomonas aeruginosa
- Escherichia coli
- Staphylococcus aureus
- Mycobacterium tuberculosis
- Streptococcus pneumoniae
Correct Answer: Staphylococcus aureus
Explanation:
Staphylococcus aureus is the most common organism isolated in spinal epidural abscesses, accounting for more than 60% of cases. Immediate surgical decompression and targeted intravenous antibiotics are standard of care, especially when neurological deficits are present.
Question 90:
A 14-year-old boy presents with rigid flat feet and lateral ankle pain. Radiographs demonstrate a 'C sign'. This finding is most strongly indicative of which of the following conditions?
Options:
- Calcaneonavicular coalition
- Talocalcaneal coalition
- Talonavicular coalition
- Cubonavicular coalition
- Accessory navicular
Correct Answer: Talocalcaneal coalition
Explanation:
The 'C sign' on a lateral radiograph of the foot is formed by the continuous outline of the medial talar dome and the inferior sustentaculum tali. It indicates the presence of a talocalcaneal (subtalar) coalition. Calcaneonavicular coalition is typically identified by the 'anteater nose' sign on an oblique view.
Question 91:
Denosumab is an effective pharmacological agent used in the management of osteoporosis. What is its specific mechanism of action?
Options:
- Binds to RANKL and inhibits osteoclast activation
- Directly induces osteoclast apoptosis
- Stimulates osteoblast activity via PTH receptor
- Inhibits farnesyl pyrophosphate synthase
- Binds to sclerostin to promote bone formation
Correct Answer: Binds to RANKL and inhibits osteoclast activation
Explanation:
Denosumab is a fully human monoclonal antibody that binds to RANKL (Receptor Activator of Nuclear factor Kappa-B Ligand), preventing it from interacting with RANK on osteoclasts and their precursors. This inhibits osteoclast formation, function, and survival. Bisphosphonates inhibit farnesyl pyrophosphate synthase.
Question 92:
When performing a reverse total shoulder arthroplasty for rotator cuff tear arthropathy, moving the center of rotation medially and inferiorly relative to the native anatomy accomplishes which of the following mechanical advantages?
Options:
- Decreases the deltoid moment arm and increases tension
- Increases the deltoid moment arm and increases inferior subluxation risk
- Increases the deltoid moment arm and decreases torque on the glenoid component
- Decreases the deltoid moment arm and increases torque on the glenoid component
- Increases the tension of the remaining rotator cuff muscles only
Correct Answer: Increases the deltoid moment arm and decreases torque on the glenoid component
Explanation:
Grammont's principles for reverse total shoulder arthroplasty involve distalizing the humerus (to tension the deltoid) and medializing the center of rotation. Medialization increases the deltoid moment arm, improving its mechanical efficiency, and simultaneously reduces shear forces (torque) on the glenosphere, reducing the risk of aseptic loosening.
Question 93:
When performing an anatomic single-bundle anterior cruciate ligament (ACL) reconstruction, improper tunnel placement can lead to graft failure. Positioning the femoral tunnel too anterior (shallow in the notch) will result in a graft that is:
Options:
- Tight in flexion and loose in extension
- Loose in flexion and tight in extension
- Tight in both flexion and extension
- Loose in both flexion and extension
- Associated with increased risk of posterior cruciate ligament impingement
Correct Answer: Tight in flexion and loose in extension
Explanation:
In ACL reconstruction, if the femoral tunnel is placed too anteriorly (high in the notch with the knee flexed), the distance between the femoral and tibial attachments will increase as the knee goes into flexion. This causes the graft to be inappropriately tight in flexion and excessively loose in extension.
Question 94:
A patient presents with an acute monoarticular swelling of the first metatarsophalangeal joint. Joint aspiration is performed. Under polarized light microscopy, the synovial fluid is expected to demonstrate:
Options:
- Positively birefringent rhomboid-shaped crystals
- Positively birefringent needle-shaped crystals
- Negatively birefringent needle-shaped crystals
- Negatively birefringent rhomboid-shaped crystals
- Non-birefringent envelope-shaped crystals
Correct Answer: Negatively birefringent needle-shaped crystals
Explanation:
The patient is presenting with podagra, classic for gout. Gout is caused by monosodium urate crystals, which appear as negatively birefringent, needle-shaped crystals under polarized light microscopy. Pseudogout (CPPD) presents with weakly positively birefringent, rhomboid-shaped crystals.
Question 95:
A 4-month-old female is being treated for developmental dysplasia of the hip (DDH) using a Pavlik harness. What is the most common nerve palsy associated with excessive hyperflexion of the hips in this device?
Options:
- Sciatic nerve
- Obturator nerve
- Femoral nerve
- Lateral femoral cutaneous nerve
- Superior gluteal nerve
Correct Answer: Femoral nerve
Explanation:
Excessive flexion of the hips in a Pavlik harness can cause impingement of the femoral nerve against the inguinal ligament, leading to a femoral nerve palsy (typically presenting as decreased active knee extension). Excessive abduction, conversely, increases the risk of avascular necrosis of the femoral head.
Question 96:
During evaluation of an ankle fracture, a syndesmotic injury is suspected. On standard mortise radiographs of a normal ankle, the tibiofibular clear space should measure:
Options:
- Less than 2 mm
- Less than 4 mm
- Less than 6 mm
- Greater than 6 mm
- Less than 10 mm
Correct Answer: Less than 6 mm
Explanation:
The tibiofibular clear space is measured 1 cm proximal to the tibial plafond. On both AP and mortise views, it should be less than 6 mm in a normal ankle. A measurement greater than 6 mm suggests a syndesmotic injury. Tibiofibular overlap should be >1 mm on the mortise view.
Question 97:
A 32-year-old female falls on an outstretched hand and sustains a 'terrible triad' injury of the elbow. This injury pattern classically includes an elbow dislocation, a radial head fracture, and a fracture of which of the following structures?
Options:
- Olecranon
- Capitellum
- Coronoid process
- Lateral epicondyle
- Medial epicondyle
Correct Answer: Coronoid process
Explanation:
The 'terrible triad' of the elbow is defined by the presence of a posterior or posterolateral elbow dislocation, a radial head fracture, and a fracture of the coronoid process. It is highly unstable and typically requires surgical intervention to restore the bony stabilizers (coronoid, radial head) and lateral collateral ligament complex.
Question 98:
A patient presents with a midshaft humerus fracture and a concomitant complete radial nerve palsy. The fracture is closed and treated nonoperatively in a functional brace. At 12 weeks, there is no clinical or electromyographic (EMG) evidence of radial nerve recovery, and the fracture is healing well. What is the most appropriate next step in management?
Options:
- Continued observation for another 3 months
- Tendon transfers
- Surgical exploration of the radial nerve
- Magnetic resonance imaging of the cervical spine
- Ultrasound-guided nerve block
Correct Answer: Surgical exploration of the radial nerve
Explanation:
Radial nerve palsy associated with a closed humeral shaft fracture is initially managed expectantly. If there are no clinical or electromyographic signs of spontaneous recovery by 3 to 4 months post-injury, surgical exploration of the radial nerve is indicated.
Question 99:
Osteogenesis imperfecta (OI) type I is a connective tissue disorder characterized by brittle bones and blue sclerae. It is most commonly caused by a mutation in which of the following genes?
Options:
- FGFR3
- COMP
- COL1A1 or COL1A2
- COL2A1
- RUNX2
Correct Answer: COL1A1 or COL1A2
Explanation:
Osteogenesis imperfecta is primarily caused by autosomal dominant mutations in the COL1A1 or COL1A2 genes, which encode the alpha-1 and alpha-2 chains of type I collagen. FGFR3 mutations cause achondroplasia. COMP mutations are seen in pseudoachondroplasia and multiple epiphyseal dysplasia. COL2A1 mutations cause type II collagenopathies (e.g., Kniest dysplasia). RUNX2 mutations cause cleidocranial dysplasia.
Question 100:
A 72-year-old female who has been taking a medication for osteoporosis for 8 years presents with a low-energy fracture of the femoral shaft. What is the primary mechanism by which bisphosphonates increase the risk of these atypical femur fractures?
Options:
- Inhibition of osteoblast differentiation
- Disruption of the vascular supply to the diaphysis
- Direct toxicity to osteocytes
- Suppression of bone turnover leading to accumulation of microdamage
- Stimulation of parathyroid hormone secretion
Correct Answer: Suppression of bone turnover leading to accumulation of microdamage
Explanation:
Long-term bisphosphonate therapy heavily suppresses osteoclast activity, which severely blunts normal targeted bone remodeling. Over time, normal physiological microdamage in the cortical bone is not repaired and accumulates. This leads to altered biomechanical properties and eventually the propagation of microcracks into a stress fracture and completed atypical femur fracture.