Full Question & Answer Text (for Search Engines)
Question 1:
A 45-year-old male presents after a motor vehicle accident with neck pain. Imaging shows a unilateral facet dislocation at C5-C6. What is the most common neurologic deficit associated with this injury if a radiculopathy is present?
Options:
- C4 radiculopathy
- C5 radiculopathy
- C6 radiculopathy
- C7 radiculopathy
- C8 radiculopathy
Correct Answer: C6 radiculopathy
Explanation:
In a unilateral facet dislocation at C5-C6, the exiting nerve root at that level is C6. The C6 root exits between C5 and C6 in the cervical spine. It is the most commonly injured nerve root in this specific dislocation.
Question 2:
Which of the following surgical approaches is most appropriate for a posteromedial tibial plateau fracture?
Options:
- Anterolateral approach
- Medial approach
- Posteromedial approach
- Posterolateral approach
- Anterior mid-line approach
Correct Answer: Posteromedial approach
Explanation:
Posteromedial shear fractures of the tibial plateau require buttress plating on the posteromedial surface. A posteromedial approach interval is between the medial head of the gastrocnemius and the pes anserinus.
Question 3:
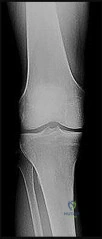
A 13-year-old boy presents with left knee pain and a limp for 3 weeks. Examination reveals obligatory external rotation of the left hip with passive hip flexion. Radiographs demonstrate a mild slip. He is scheduled for in situ pinning. What is the primary goal of this procedure?
Options:
- To anatomically reduce the slip
- To prevent further slippage
- To restore normal hip biomechanics
- To prevent avascular necrosis
- To delay the onset of chondrolysis
Correct Answer: To prevent further slippage
Explanation:
The primary goal of in situ pinning for SCFE is to stabilize the physis and prevent further slippage, allowing the physis to close. Attempting to reduce a chronic slip increases the risk of avascular necrosis.
Question 4:
A 68-year-old female undergoes a primary THA via a posterior approach. Postoperatively, she suffers a posterior dislocation. Which of the following component malpositions most likely contributed to this complication?
Options:
- Excessive acetabular anteversion
- Decreased femoral offset
- Excessive acetabular abduction
- Acetabular retroversion
- Excessive femoral anteversion
Correct Answer: Acetabular retroversion
Explanation:
Posterior dislocation following THA is most commonly associated with acetabular retroversion or insufficient femoral anteversion. Excessive acetabular anteversion typically leads to anterior dislocation.
Question 5:
When performing an anterior cruciate ligament (ACL) reconstruction using a bone-patellar tendon-bone autograft, placement of the femoral tunnel too anteriorly (shallow) will most likely result in:
Options:
- Increased laxity in extension and tightness in flexion
- Tightness in extension and laxity in flexion
- Tightness in both flexion and extension
- Laxity in both flexion and extension
- Patellar tendon rupture
Correct Answer: Increased laxity in extension and tightness in flexion
Explanation:
If the femoral tunnel is placed too anteriorly, the graft will be tight in flexion and loose in extension. Conversely, if it is placed too posteriorly (deep), it will be tight in extension and loose in flexion.
Question 6:
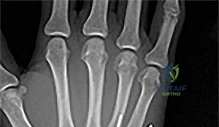
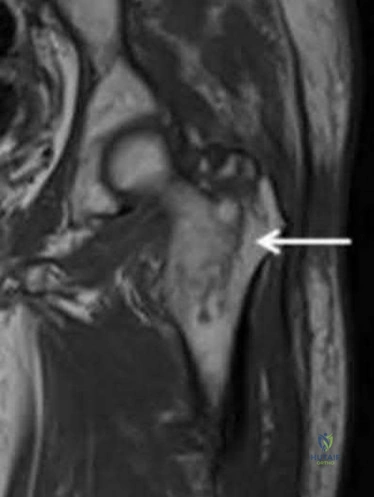
A 25-year-old carpenter lacerates his index finger volar surface at the level of the proximal phalanx base (Zone II). Both the FDS and FDP are lacerated. What is the optimal timing and treatment?
Options:
- Primary repair within 24 hours using a 2-strand core suture
- Primary repair within 1-2 weeks using a 4-strand or 6-strand core suture
- Delayed primary repair at 4 weeks
- Tendon graft at 6 weeks
- Two-stage tendon reconstruction
Correct Answer: Primary repair within 1-2 weeks using a 4-strand or 6-strand core suture
Explanation:
Zone II flexor tendon injuries are best treated with primary repair, ideally within the first 1-2 weeks. Multi-strand core sutures (4 or 6 strands) provide sufficient strength to allow for early active motion protocols, which improve outcomes.
Question 7:
A 40-year-old weekend warrior sustains an acute Achilles tendon rupture. Nonoperative management is chosen. Which of the following protocols has been shown to result in outcomes similar to surgical repair regarding re-rupture rates?
Options:
- Prolonged cast immobilization in equinus for 12 weeks
- Early functional rehabilitation with weight-bearing in a functional brace
- Non-weight-bearing in a neutral cast for 8 weeks
- Immediate full weight-bearing without a brace
- Immobilization in a boot with the ankle in dorsiflexion
Correct Answer: Early functional rehabilitation with weight-bearing in a functional brace
Explanation:
Recent literature shows that early functional rehabilitation protocols (early weight-bearing in a functional brace with a heel lift) for acute Achilles tendon ruptures result in re-rupture rates comparable to operative treatment, while avoiding surgical complications.
Question 8:
Which phase of fracture healing is most dependent on the inflammatory cascade initiated by macrophages and platelets?
Options:
- Hard callus formation
- Soft callus formation
- Hematoma formation and inflammation
- Remodeling
- Woven bone deposition
Correct Answer: Hematoma formation and inflammation
Explanation:
The initial phase of fracture healing is the hematoma formation and inflammatory phase. Platelets and macrophages release cytokines (e.g., PDGF, TGF-beta) that recruit mesenchymal stem cells and initiate the healing process.
Question 9:
A 15-year-old male presents with deep knee pain. Radiographs reveal a mixed lytic and sclerotic lesion in the distal femur metaphysis with a "sunburst" periosteal reaction. Biopsy confirms high-grade conventional osteosarcoma. What is the most appropriate next step in management?
Options:
- Wide surgical resection followed by radiation
- Neoadjuvant chemotherapy followed by wide surgical resection and adjuvant chemotherapy
- Primary amputation
- Curettage and bone grafting
- Radiation therapy alone
Correct Answer: Neoadjuvant chemotherapy followed by wide surgical resection and adjuvant chemotherapy
Explanation:
The standard of care for high-grade conventional osteosarcoma is neoadjuvant (preoperative) chemotherapy, followed by wide surgical resection (limb-sparing surgery if feasible), and then adjuvant (postoperative) chemotherapy.
Question 10:
A 35-year-old male sustains a vertically oriented (Pauwels type III) basicervical femoral neck fracture. Which of the following fixation constructs offers the highest biomechanical stability for this specific fracture pattern?
Options:
- Three parallel cancellous screws
- Sliding hip screw (SHS) alone
- Sliding hip screw with an anti-rotation screw
- Cephalomedullary nail
- Dynamic condylar screw
Correct Answer: Sliding hip screw with an anti-rotation screw
Explanation:
Vertical fracture patterns (Pauwels III) experience high shear forces. A sliding hip screw (SHS) provides better resistance to vertical shear compared to cancellous screws. The addition of an anti-rotation (derotational) screw superior to the SHS provides optimal stability.
Question 11:
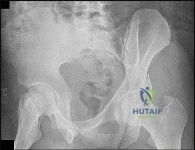
An 18-month-old girl presents with a painless limp and leg length discrepancy. Radiographs show a dislocated left hip with a pseudoacetabulum. What is the most appropriate treatment?
Options:
- Pavlik harness
- Closed reduction and spica casting
- Open reduction, pelvic osteotomy, and femoral shortening osteotomy
- Observation
- Physical therapy
Correct Answer: Open reduction, pelvic osteotomy, and femoral shortening osteotomy
Explanation:
In a walking child over 18 months of age with a completely dislocated hip, open reduction is almost always required. A femoral shortening osteotomy reduces pressure on the cartilage to prevent AVN, and a pelvic osteotomy (e.g., Salter or Pemberton) is usually needed to correct acetabular dysplasia.
Question 12:
Following a primary total knee arthroplasty, a patient experiences isolated patellar clunk syndrome. Which of the following implant designs or technical factors is most closely associated with this phenomenon?
Options:
- Cruciate-retaining (CR) femoral component
- Posterior-stabilized (PS) femoral component with a high intercondylar box
- Medial pivot design
- Patella baja
- Oversized tibial component
Correct Answer: Posterior-stabilized (PS) femoral component with a high intercondylar box
Explanation:
Patellar clunk syndrome occurs in posterior-stabilized TKA when a fibrotic nodule forms at the superior pole of the patella. During extension, this nodule catches in the intercondylar box of the femoral component and "clunks" out as the knee reaches full extension.
Question 13:
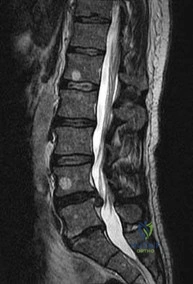
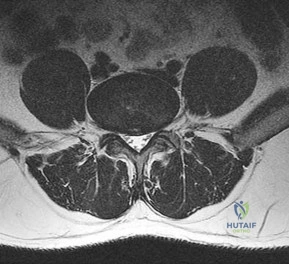
A 65-year-old male presents with neurogenic claudication. He reports pain radiating down both legs when walking, which is relieved by leaning forward on a shopping cart. MRI shows severe spinal stenosis at L4-L5. Which ligament thickens and contributes significantly to the dorsal compression of the thecal sac in this condition?
Options:
- Anterior longitudinal ligament
- Posterior longitudinal ligament
- Ligamentum flavum
- Interspinous ligament
- Supraspinous ligament
Correct Answer: Ligamentum flavum
Explanation:
In degenerative lumbar spinal stenosis, hypertrophy and buckling of the ligamentum flavum commonly cause dorsal compression of the thecal sac.
Question 14:
A 22-year-old football player sustains a recurrent anterior shoulder dislocation. An MRI arthrogram reveals a Bankart tear and a large Hill-Sachs lesion that engages the anterior glenoid rim. What is the best surgical option to address the engaging Hill-Sachs lesion?
Options:
- Isolated arthroscopic Bankart repair
- Remplissage procedure with Bankart repair
- SLAP repair
- Coracoid transfer to the lesser tuberosity
- Subscapularis advancement
Correct Answer: Remplissage procedure with Bankart repair
Explanation:
An engaging Hill-Sachs lesion is a defect on the posterolateral humeral head that engages the anterior glenoid during abduction and external rotation, predisposing to recurrent dislocation. The Remplissage procedure (infilling the defect with the infraspinatus tendon and capsule) combined with a Bankart repair is an effective treatment.
Question 15:
A 45-year-old typist complains of numbness and tingling in the small and ring fingers of her right hand. Examination reveals a positive Tinel's sign at the elbow and weakness of the dorsal interossei. The flexor carpi ulnaris (FCU) strength is normal. Where is the most likely site of compression?
Options:
- Between the two heads of the FCU (Cubital tunnel)
- Guyon's canal
- Ligament of Struthers
- Arcade of Frohse
- Pronator teres syndrome
Correct Answer: Between the two heads of the FCU (Cubital tunnel)
Explanation:
The symptoms indicate ulnar nerve compression. While FCU strength is often preserved due to its proximal innervation (branches sometimes arise proximal to the compression), compression typically occurs at the cubital tunnel (Osborne's ligament/between the heads of FCU). Guyon's canal compression would not cause Tinel's at the elbow.
Question 16:
Which of the following sterilization methods for ultra-high molecular weight polyethylene (UHMWPE) components in total joint arthroplasty promotes cross-linking but also generates free radicals that can lead to oxidation and degradation if not properly treated?
Options:
- Ethylene oxide gas
- Gamma irradiation in air
- Autoclaving
- Gas plasma
- Dry heat
Correct Answer: Gamma irradiation in air
Explanation:
Gamma irradiation induces cross-linking, which improves wear resistance. However, if performed in air, it generates free radicals that react with oxygen, leading to oxidation, chain scission, and subsequent degradation of the polyethylene. Modern techniques involve irradiation in an inert environment (e.g., argon or vacuum) and subsequent melting or annealing to quench free radicals.
Question 17:
A 25-year-old male injures his midfoot when falling from a horse with his foot caught in the stirrup. Radiographs show a widening of the space between the base of the 1st and 2nd metatarsals. Which ligament is primarily ruptured in a classical Lisfranc injury?
Options:
- Ligament connecting the 1st metatarsal to the medial cuneiform
- Ligament connecting the 2nd metatarsal base to the medial cuneiform
- Ligament connecting the 2nd metatarsal base to the intermediate cuneiform
- Plantar fascia
- Spring ligament
Correct Answer: Ligament connecting the 2nd metatarsal base to the medial cuneiform
Explanation:
The Lisfranc ligament connects the medial cuneiform to the base of the second metatarsal. It is a critical stabilizing structure of the midfoot, and its rupture leads to instability.
Question 18:
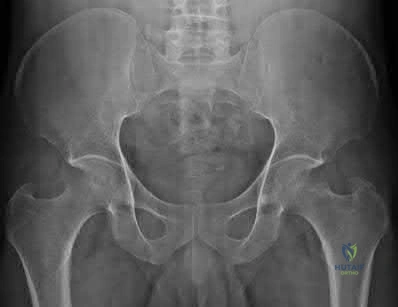
In an anteroposterior compression (APC) type III pelvic ring injury, the symphysis pubis is widely disrupted, and the hemipelvis is completely unstable. Which of the following posterior ligamentous structures is completely disrupted in an APC III injury but intact in an APC II injury?
Options:
- Anterior sacroiliac ligaments
- Sacrospinous ligaments
- Sacrotuberous ligaments
- Posterior sacroiliac ligaments
- Iliolumbar ligaments
Correct Answer: Posterior sacroiliac ligaments
Explanation:
APC II injuries involve disruption of the symphysis pubis, anterior sacroiliac ligaments, and the sacrospinous and sacrotuberous ligaments, but the posterior sacroiliac ligaments remain intact (opening book). In APC III, there is complete disruption of the anterior and posterior sacroiliac ligaments, leading to a completely unstable hemipelvis.
Question 19:
A 10-year-old boy incidentally undergoes an x-ray for a minor ankle sprain, revealing a cortically based, radiolucent lesion surrounded by a thick rim of reactive sclerosis in the distal tibial diaphysis. He describes severe pain at night that is dramatically relieved by NSAIDs. What is the most likely diagnosis?
Options:
- Osteoid osteoma
- Osteoblastoma
- Non-ossifying fibroma
- Chondroblastoma
- Eosinophilic granuloma
Correct Answer: Osteoid osteoma
Explanation:
Osteoid osteoma classically presents in children/young adults with night pain relieved by NSAIDs. Radiographically, it appears as a small radiolucent nidus (<1.5 cm) surrounded by dense reactive sclerosis, typically in the cortex of long bones.
Question 20:
The Ponseti method for the treatment of congenital idiopathic clubfoot (talipes equinovarus) dictates a specific sequence of deformity correction. Which of the following represents the correct sequence of correction?
Options:
- Equinus, varus, adductus, cavus
- Cavus, adductus, varus, equinus
- Adductus, varus, cavus, equinus
- Cavus, varus, equinus, adductus
- Varus, cavus, adductus, equinus
Correct Answer: Cavus, adductus, varus, equinus
Explanation:
The acronym CAVE is used to remember the sequence of correction in the Ponseti method: Cavus (by elevating the first ray), Adductus, Varus, and finally Equinus (often requiring a percutaneous Achilles tenotomy).