Full Question & Answer Text (for Search Engines)
Question 1:
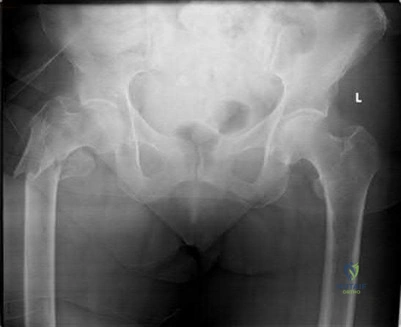
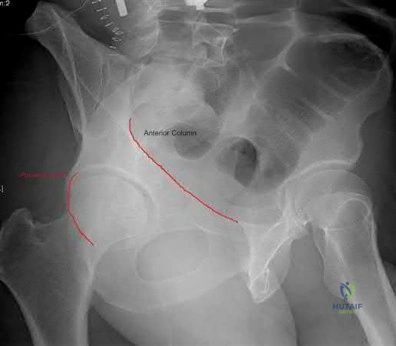
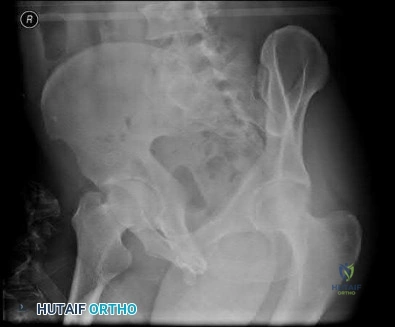
A 35-year-old male is brought to the trauma bay after a severe fall from height. He is hypotensive and tachycardic. An AP pelvis radiograph demonstrates a vertically displaced left hemipelvis with severe disruption of the posterior sacroiliac complex and symphysis pubis. If active arterial hemorrhage is identified on angiography, which vessel is most likely injured in this specific injury pattern?
Options:
- Obturator artery
- Internal pudendal artery
- Superior gluteal artery
- Corona mortis
- Inferior epigastric artery
Correct Answer: Superior gluteal artery
Explanation:
Vertical shear pelvic fractures involve massive disruption of the posterior pelvic ring, including the sacrotuberous and sacrospinous ligaments. The superior gluteal artery exits the pelvis through the greater sciatic notch in close proximity to the sacroiliac joint and is the most commonly injured artery in vertical shear pelvic fractures. In contrast, APC (Anteroposterior Compression) injuries are more typically associated with injuries to the internal pudendal and obturator arteries.
Question 2:
A 45-year-old manual laborer presents with chronic wrist pain and stiffness. Radiographs demonstrate Scaphoid Nonunion Advanced Collapse (SNAC) Stage III. Which of the following joint involvement patterns correctly describes SNAC Stage III, making Proximal Row Carpectomy (PRC) contraindicated?
Options:
- Isolated radioscaphoid arthritis
- Capitolunate arthritis
- Scaphocapitate arthritis
- Pancarpal arthritis
- Radiolunate arthritis
Correct Answer: Capitolunate arthritis
Explanation:
SNAC staging progresses as follows: Stage I involves the radioscaphoid joint (specifically the radial styloid); Stage II involves the scaphocapitate joint; Stage III involves the capitolunate joint; and Stage IV is pancarpal arthritis. Proximal row carpectomy (PRC) relies on a preserved proximal capitate head articulating with the lunate fossa of the radius. Because SNAC III involves degenerative changes at the capitolunate joint (including the capitate head), PRC is contraindicated, and a four-corner arthrodesis is the preferred motion-preserving salvage procedure.
Question 3:
A 6-year-old child presents after a fall from monkey bars with a widely displaced extension-type Gartland III supracondylar humerus fracture. On initial examination, the hand is pink but the radial pulse is not palpable. After emergent closed reduction and percutaneous pinning in the operating room, the radial pulse remains absent, but the hand remains warm and pink with a capillary refill of less than 2 seconds. What is the most appropriate next step in management?
Options:
- Immediate exploration of the brachial artery
- CT angiography of the upper extremity
- Observation and hospital admission for serial neurovascular checks
- Administration of intra-arterial vasodilators
- Prophylactic volar forearm fasciotomy
Correct Answer: Observation and hospital admission for serial neurovascular checks
Explanation:
The management of a 'pink, pulseless' hand following reduction and pinning of a pediatric supracondylar humerus fracture is observation. Collateral circulation in children is typically excellent and sufficient to maintain viability of the limb. Arterial exploration is indicated only if the hand is 'white and pulseless' (dysvascular) after a successful reduction.
Question 4:
A 12-year-old obese male presents with a stable slipped capital femoral epiphysis (SCFE) of the left hip. Which of the following factors is the strongest indication for prophylactic in situ pinning of the asymptomatic contralateral right hip?
Options:
- Body Mass Index greater than the 95th percentile
- Slip angle greater than 50 degrees on the affected side
- Age greater than 14 years at presentation
- Presence of an underlying endocrine disorder (e.g., hypothyroidism)
- Male gender
Correct Answer: Presence of an underlying endocrine disorder (e.g., hypothyroidism)
Explanation:
Prophylactic pinning of the contralateral hip in SCFE is controversial but is strongly indicated in patients with a high risk of bilateral involvement. Risk factors predicting contralateral slip include an underlying endocrine disorder (such as hypothyroidism, panhypopituitarism, or renal osteodystrophy), prior radiation therapy, or age of presentation less than 10 years (or low modified Oxford bone age score).
Question 5:
A 15-year-old boy presents with progressive distal femur pain. Imaging and subsequent biopsy confirm conventional high-grade osteosarcoma. Following neoadjuvant chemotherapy, the tumor is resected. Which of the following histologic findings in the resection specimen is the most critical prognostic indicator of overall survival?
Options:
- Presence of MDM2 amplification
- Degree of tumor necrosis less than 90%
- Predominance of chondroblastic over osteoblastic matrix
- Intralesional hemorrhage and cystic changes
- Identification of multinucleated giant cells
Correct Answer: Degree of tumor necrosis less than 90%
Explanation:
The most important prognostic factor for conventional high-grade osteosarcoma following neoadjuvant chemotherapy is the histologic response to the chemotherapy. A good response is defined as greater than 90% tumor necrosis in the resection specimen. Less than 90% tumor necrosis (a poor response) is associated with lower overall survival and a higher risk of systemic metastasis.
Question 6:
A 4-month-old female with developmental dysplasia of the hip (DDH) has been treated with a Pavlik harness for 4 weeks. Clinical and ultrasonographic evaluations confirm that the left hip remains persistently dislocated. What is the most appropriate next step in management?
Options:
- Continue Pavlik harness treatment for an additional 4 weeks
- Transition to a rigid abduction orthosis (e.g., Ilfeld or Rhino brace)
- Perform an immediate open reduction and spica casting
- Perform a proximal femoral varus derotational osteotomy
- Perform a pelvic (Salter) osteotomy
Correct Answer: Transition to a rigid abduction orthosis (e.g., Ilfeld or Rhino brace)
Explanation:
If a Pavlik harness fails to achieve reduction within 3 to 4 weeks, its use should be discontinued to prevent complications such as 'Pavlik harness disease' (erosion of the posterior acetabular lip) and avascular necrosis. The AAOS guidelines recommend transitioning to a rigid or semi-rigid abduction orthosis as the next step before considering closed or open surgical reduction.
Question 7:
A 65-year-old male undergoes MRI of the shoulder for chronic weakness and pain. The radiologist notes a positive 'tangent sign' on the sagittal oblique T1-weighted images. What does this radiographic finding specifically indicate regarding the supraspinatus muscle?
Options:
- Intramuscular fatty infiltration of Goutallier Stage 1
- Retraction of the tendon medial to the glenoid rim
- Complete tearing of the anterior cable of the rotator cuff
- Severe muscle atrophy signifying a likely irreparable tear
- Concomitant injury to the suprascapular nerve
Correct Answer: Severe muscle atrophy signifying a likely irreparable tear
Explanation:
The 'tangent sign' is assessed on a sagittal oblique MRI slice (Y-view). A line is drawn connecting the superior border of the coracoid process to the superior border of the scapular spine. If the supraspinatus muscle belly falls below this line, the tangent sign is positive. This indicates severe muscle atrophy and is strongly predictive of an irreparable rotator cuff tear and poor functional outcomes following attempted repair.
Question 8:
A 40-year-old male sustains a high-energy Pilon fracture. Initial treatment consists of a spanning external fixator across the ankle joint. Which of the following clinical findings best indicates that the soft tissue envelope has recovered sufficiently to permit definitive open reduction and internal fixation (ORIF)?
Options:
- Return of the 'wrinkle sign' on the anterior ankle skin
- Epithelialization of serous fracture blisters within 48 hours
- Resolution of the dependent rubor when the leg is elevated
- A palpable dorsalis pedis pulse overriding the external fixator
- Normalization of the erythrocyte sedimentation rate (ESR)
Correct Answer: Return of the 'wrinkle sign' on the anterior ankle skin
Explanation:
In the staged management of high-energy Pilon fractures, definitive ORIF must be delayed until the soft tissue envelope has adequately healed to minimize the risk of wound complications and infection. The return of skin wrinkles (the 'wrinkle sign') indicates a significant reduction in interstitial edema and is the widely accepted clinical milestone for proceeding with definitive fixation, typically 10 to 21 days post-injury.
Question 9:
Which of the following synovial fluid biomarkers is an antimicrobial peptide released primarily by neutrophils and has demonstrated both high sensitivity and high specificity for diagnosing periprosthetic joint infection (PJI)?
Options:
- C-reactive protein (CRP)
- Interleukin-6 (IL-6)
- Alpha-defensin
- Leukocyte esterase
- Procalcitonin
Correct Answer: Alpha-defensin
Explanation:
Alpha-defensin is a biomarker released by host neutrophils in response to pathogens. It is highly accurate for diagnosing periprosthetic joint infection (PJI). Studies have shown it maintains high sensitivity and specificity even in scenarios where other inflammatory markers may be equivocal (such as concurrent systemic inflammatory diseases or prior antibiotic administration).
Question 10:
A 50-year-old male presents with a large, expansile lesion in the proximal femur showing endosteal scalloping and 'popcorn' calcifications on radiographs. Biopsy confirms a grade II chondrosarcoma. What is the most appropriate definitive management?
Options:
- Neoadjuvant chemotherapy followed by wide surgical excision
- Wide surgical excision alone
- Intralesional curettage, adjuvant phenol, and cementation
- Primary external beam radiation therapy
- Denosumab therapy followed by resection
Correct Answer: Wide surgical excision alone
Explanation:
Chondrosarcomas are generally highly resistant to both chemotherapy and radiation therapy due to their poor vascularity and dense extracellular matrix. For intermediate-to-high grade (Grade II and III) chondrosarcomas, the standard of care is definitive wide surgical excision alone. Intralesional curettage is reserved for benign cartilaginous lesions (enchondromas) or select well-differentiated (Grade I) chondrosarcomas in the appendicular skeleton.
Question 11:
A 60-year-old female undergoes open reduction and internal fixation of a distal radius fracture with a volar locking plate. Three months postoperatively, she suddenly loses the ability to actively flex the interphalangeal joint of her thumb. Which technical error during the initial surgery is the most likely cause of this complication?
Options:
- Placement of the plate prominent to the volar watershed line
- Penetration of a dorsal screw into the third extensor compartment
- Failure to release the brachioradialis tendon
- Over-reduction of the volar tilt leading to median nerve compression
- Placement of a screw excessively deep into the distal radioulnar joint
Correct Answer: Placement of the plate prominent to the volar watershed line
Explanation:
Attritional rupture of the flexor pollicis longus (FPL) tendon is a well-documented complication of volar locking plate fixation for distal radius fractures. It most commonly occurs when the plate is placed distal to the 'watershed line' (Soong Grade 2), causing the FPL tendon to rub directly against the prominent distal edge of the plate during wrist motion.
Question 12:
A 17-year-old female high school soccer player sustains an isolated anterior cruciate ligament (ACL) tear. She undergoes primary ACL reconstruction. Which of the following graft choices is associated with the highest rate of re-rupture in this specific demographic?
Options:
- Bone-patellar tendon-bone (BPTB) autograft
- Quadrupled hamstring autograft
- Quadriceps tendon autograft
- Bone-patellar tendon-bone (BPTB) allograft
- Hamstring allograft augmented with suture tape
Correct Answer: Bone-patellar tendon-bone (BPTB) allograft
Explanation:
In young, active patients (particularly those under 25 years of age returning to high-impact pivoting sports like soccer), allografts (such as BPTB allograft) have a significantly higher clinical failure and re-rupture rate compared to autografts. Autografts (BPTB, hamstring, or quadriceps) are the gold standard for this patient demographic.
Question 13:
A 45-year-old male presents to the emergency department with severe low back pain and bilateral radicular leg pain. Which of the following clinical findings is the most sensitive early indicator of Cauda Equina Syndrome?
Options:
- Saddle anesthesia (S4-S5 dermatomal sensory loss)
- Bilateral loss of Achilles reflexes
- Urinary retention with elevated post-void residual volume
- Loss of rectal sphincter tone on digital exam
- Profound bilateral foot drop
Correct Answer: Urinary retention with elevated post-void residual volume
Explanation:
Urinary retention is the most sensitive symptom/finding in suspected Cauda Equina Syndrome (CES). A normal post-void residual volume (typically < 100-200 mL) makes CES highly unlikely. While saddle anesthesia and decreased rectal tone are classic, specific signs, they may present later or be absent in early incomplete CES.
Question 14:
A 14-year-old female gymnast complains of chronic, activity-related low back pain. Radiographs reveal a Grade II spondylolisthesis at L5-S1. If this is an isthmic spondylolisthesis, what is the primary anatomic etiology of the slippage?
Options:
- Congenital dysplasia of the L5-S1 facet joints
- A bilateral defect or stress fracture in the pars interarticularis
- Degenerative hypertrophy of the ligamentum flavum
- A previous iatrogenic destabilization from laminectomy
- Microinstability related to a generalized connective tissue disorder
Correct Answer: A bilateral defect or stress fracture in the pars interarticularis
Explanation:
Isthmic spondylolisthesis (Wiltse Type II) is caused by a defect (spondylolysis), elongation, or acute fracture in the pars interarticularis. This is common in adolescent athletes involved in repetitive lumbar hyperextension (e.g., gymnasts, fast bowlers). Dysplastic spondylolisthesis (Wiltse Type I) is due to congenital anomalies of the upper sacrum or the arch of L5 (facet joint dysplasia).
Question 15:
A 65-year-old male with a metal-on-metal total hip arthroplasty placed 10 years ago presents with persistent groin pain. MRI reveals a large, solid-cystic mass communicating with the joint. Biopsy of the periprosthetic tissue is most likely to demonstrate which of the following histopathological hallmarks characteristic of Aseptic Lymphocytic Vasculitis-Associated Lesions (ALVAL)?
Options:
- Abundant multinucleated foreign body giant cells containing polyethylene particles
- Acute neutrophilic exudate extending to the bone-cement interface
- Extensive spindle cell proliferation with high mitotic activity
- Sheet-like infiltration of foamy macrophages with cholesterol clefts
- Extensive perivascular lymphocytic infiltrates
Correct Answer: Extensive perivascular lymphocytic infiltrates
Explanation:
ALVAL (Aseptic Lymphocytic Vasculitis-Associated Lesions) is an adverse local tissue reaction (ALTR) specifically associated with metal-on-metal implants or mechanically assisted crevice corrosion (trunnionosis). Histologically, it is a delayed-type (Type IV) hypersensitivity reaction characterized by an extensive perivascular infiltrate of lymphocytes (mostly T-cells), macrophages, and tissue necrosis. Polyethylene wear causes a different reaction dominated by macrophages and foreign body giant cells.
Question 16:
The Ponseti method is the gold standard for the treatment of idiopathic clubfoot (talipes equinovarus). To avoid a 'rocker-bottom' deformity, in what precise order must the components of the clubfoot deformity be corrected?
Options:
- Equinus, Varus, Adductus, Cavus
- Varus, Cavus, Equinus, Adductus
- Adductus, Cavus, Varus, Equinus
- Cavus, Adductus, Varus, Equinus
- Equinus, Adductus, Cavus, Varus
Correct Answer: Cavus, Adductus, Varus, Equinus
Explanation:
The components of clubfoot are corrected sequentially according to the mnemonic CAVE: Cavus (by elevating the first ray to supinate the forefoot), Adductus, Varus, and lastly Equinus. Attempting to correct equinus too early, before the calcaneus is fully abducted, leads to a midfoot breach and a rocker-bottom foot deformity. Equinus is often addressed at the end with an Achilles tenotomy.
Question 17:
A newborn delivered via forceps-assisted vaginal delivery presents with the right upper extremity held in adduction, internal rotation, and extension at the elbow, with the wrist flexed ('waiter's tip' posture). Which nerve roots are predominantly injured in this condition?
Options:
- C8 and T1
- C7, C8, and T1
- C5 and C6
- C5, C6, and C7
- Isolated C7
Correct Answer: C5 and C6
Explanation:
The 'waiter's tip' posture is characteristic of Erb's palsy, which is an upper trunk brachial plexus injury involving the C5 and C6 nerve roots. This causes paralysis of the deltoid and supraspinatus (loss of abduction), infraspinatus and teres minor (loss of external rotation), and biceps and brachialis (loss of elbow flexion). Injury to C8 and T1 results in Klumpke's palsy, affecting the intrinsic muscles of the hand (claw hand).
Question 18:
A 45-year-old male sustains a severe high-energy knee injury. Radiographs show a depressed, split fracture of the medial tibial plateau with extension into the intercondylar eminence (Schatzker Type IV). Which surgical approach is generally most critical to anatomically reduce and buttress the primary fracture fragment?
Options:
- Anterolateral approach
- Posteromedial approach
- Direct anterior parapatellar approach
- Posterolateral approach
- Direct medial approach
Correct Answer: Posteromedial approach
Explanation:
Schatzker IV fractures involve the medial tibial plateau. The primary fracture fragment in medial plateau injuries typically displaces posteromedially due to the pull of the semimembranosus and the medial femoral condyle's biomechanics. A posteromedial surgical approach is required to properly visualize, reduce, and place an anti-glide buttress plate on the posteromedial apex of the fragment. An anterolateral approach is utilized for Schatzker I, II, and III (lateral plateau) fractures.
Question 19:
A 50-year-old female presents with sudden onset medial knee pain without mechanical locking. MRI demonstrates a medial meniscus posterior root tear with 4 mm of meniscal extrusion. Biomechanically, untreated meniscal root tears have been shown to be equivalent to which of the following?
Options:
- Total meniscectomy
- Partial meniscectomy
- Anterior cruciate ligament deficiency
- Medial collateral ligament sprain
- Posterior cruciate ligament deficiency
Correct Answer: Total meniscectomy
Explanation:
Meniscal root tears completely disrupt the circumferential hoop stresses of the meniscus. Without these intact roots anchoring the meniscus to the tibial plateau, axial loading simply pushes the meniscus out of the joint (extrusion). Biomechanical studies have demonstrated that an untreated meniscal root tear leads to peak contact pressures identical to a total meniscectomy, resulting in rapid joint degeneration.
Question 20:
Denosumab is widely utilized as a neoadjuvant or definitive therapy for unresectable Giant Cell Tumor of Bone. By what mechanism does denosumab arrest the progression of this lesion?
Options:
- It induces apoptosis of the neoplastic mononuclear stromal cells directly via p53 activation
- It cross-links DNA via alkylation, preventing mitosis in highly proliferative cells
- It competitively inhibits vascular endothelial growth factor (VEGF), leading to tumor ischemia
- It stimulates osteoblastic activity by agonizing the Wnt/beta-catenin pathway
- It acts as a monoclonal antibody against RANKL, preventing osteoclast-like giant cell formation
Correct Answer: It acts as a monoclonal antibody against RANKL, preventing osteoclast-like giant cell formation
Explanation:
Giant Cell Tumor of Bone consists of neoplastic mononuclear stromal cells that overexpress RANKL (Receptor Activator of Nuclear factor Kappa-B Ligand). This overproduction recruits and activates reactive multinucleated osteoclast-like giant cells, which cause massive localized bone destruction. Denosumab is a fully human monoclonal antibody that binds directly to RANKL, inhibiting the formation, function, and survival of these giant cells, thereby arresting osteolysis and allowing the bone to re-ossify.
Question 21:
A 32-year-old female presents with a painless, slowly enlarging mass behind her knee. The radiograph is shown. Biopsy confirms a low-grade, bone-forming tumor on the surface of the posterior distal femur with a 'string sign' representing radiolucency between the tumor and the cortex. Which of the following genetic alterations is most classically associated with this diagnosis?
Options:
- t(11;22) chromosomal translocation
- t(X;18) chromosomal translocation
- GNAS gene mutation
- EXT1 gene mutation
- MDM2 and CDK4 gene amplification
Correct Answer: MDM2 and CDK4 gene amplification
Explanation:
The clinical scenario and imaging description represent parosteal osteosarcoma, a low-grade surface osteosarcoma typically found on the posterior aspect of the distal femur. It is characterized molecularly by ring chromosomes and amplification of the 12q13-15 region, which includes the MDM2 and CDK4 genes. t(11;22) is associated with Ewing sarcoma. t(X;18) is seen in synovial sarcoma. GNAS mutations are found in fibrous dysplasia. EXT1 mutations are associated with hereditary multiple exostoses.
Question 22:
During an ilioinguinal approach to the acetabulum, massive bleeding occurs while dissecting over the superior pubic ramus near the symphysis. The injured vessel, commonly referred to as the 'corona mortis,' typically represents an anastomosis between the obturator artery and which of the following?
Options:
- Internal pudendal artery
- Superior gluteal artery
- Inferior epigastric or external iliac artery
- Femoral artery
- Deep circumflex iliac artery
Correct Answer: Inferior epigastric or external iliac artery
Explanation:
The 'corona mortis' (crown of death) is an anatomical variant describing an anastomosis between the obturator system and the external iliac or inferior epigastric system. It is located on the posterior aspect of the superior pubic ramus. Injury to this vessel during pelvic or acetabular surgery (like the ilioinguinal or Stoppa approaches) can lead to severe, difficult-to-control hemorrhage.
Question 23:
A 16-year-old female athlete undergoes primary anterior cruciate ligament (ACL) reconstruction using a soft-tissue hamstring autograft. Which of the following factors has been shown to be most strongly associated with an increased risk of early graft failure in this population?
Options:
- Use of suspensory fixation on the femur
- Graft diameter less than 8 mm
- Concomitant partial medial meniscectomy
- Use of interference screw fixation on the tibia
- Timing of surgery within 3 weeks of injury
Correct Answer: Graft diameter less than 8 mm
Explanation:
In adolescent and young adult patients, utilizing a hamstring autograft with a diameter of less than 8 mm has been significantly associated with higher rates of graft failure. Surgeons often consider augmenting the graft or choosing an alternative graft source (like bone-patellar tendon-bone) if the intraoperative hamstring size is inadequate.
Question 24:
A 55-year-old man of East Asian descent presents with progressive clumsiness in his hands, difficulty with fine motor tasks, and a wide-based gait. Imaging of his cervical spine is shown. What is the underlying pathophysiology most likely responsible for his myelopathic symptoms?
Options:
- Hypertrophy of the ligamentum flavum
- Ectopic bone formation within the posterior longitudinal ligament
- Disc herniation leading to cord contusion
- Congenital fusion of the cervical vertebrae
- Destructive granulomatous infection of the vertebral body
Correct Answer: Ectopic bone formation within the posterior longitudinal ligament
Explanation:
The scenario describes cervical myelopathy secondary to Ossification of the Posterior Longitudinal Ligament (OPLL). This condition is characterized by ectopic bone formation within the posterior longitudinal ligament and is particularly prevalent in East Asian populations. It causes progressive anterior compression of the spinal cord, leading to myelopathic symptoms such as clumsiness in the hands (loss of fine motor skills) and a spastic, wide-based gait.
Question 25:
In total hip arthroplasty (THA), the adoption of highly cross-linked polyethylene (HXLPE) has significantly reduced wear rates compared to conventional polyethylene. However, the high-dose irradiation process alters the mechanical properties of the material. Which mechanical property is most significantly decreased as a direct result of irradiation for cross-linking?
Options:
- Modulus of elasticity
- Wear resistance
- Fatigue crack propagation resistance
- Coefficient of friction
- Oxidation resistance prior to remelting
Correct Answer: Fatigue crack propagation resistance
Explanation:
While high-dose irradiation creates cross-links that greatly improve wear resistance, it also makes the polyethylene more brittle. This results in a decrease in ductility, ultimate tensile strength, and most notably, fatigue crack propagation resistance (fracture toughness). This is why highly cross-linked polyethylene is generally avoided in unicompartmental knees or very thin tibial inserts where high stress concentrations might lead to component fracture.
Question 26:
A 13-year-old obese boy presents with non-traumatic knee pain and is noted to have an obligate external rotation of his hip when it is passively flexed. Radiographs confirm the diagnosis. He is unable to bear weight on the affected extremity. What is the primary complication associated with this presentation compared to a patient who is able to bear weight?
Options:
- Chondrolysis
- Avascular necrosis (AVN) of the femoral head
- Femoroacetabular impingement (FAI)
- Slipped capital femoral epiphysis on the contralateral side
- Leg length discrepancy
Correct Answer: Avascular necrosis (AVN) of the femoral head
Explanation:
The patient has an unstable slipped capital femoral epiphysis (SCFE), defined by Loder criteria as the inability to bear weight even with crutches. Unstable SCFE has a significantly higher rate of avascular necrosis (up to nearly 50% in some series) compared to stable SCFE (which has an AVN rate near 0%). Both stable and unstable SCFEs can lead to impingement or contralateral slips, but AVN is the critical distinguishing risk factor of an unstable slip.
Question 27:
In a patient with a high radial nerve palsy following a mid-shaft humerus fracture, tendon transfers are planned to restore function. Which of the following tendon transfers is the classic and most commonly utilized choice to restore wrist extension?
Options:
- Flexor carpi ulnaris (FCU) to Extensor digitorum communis (EDC)
- Flexor carpi radialis (FCR) to Extensor pollicis longus (EPL)
- Pronator teres (PT) to Extensor carpi radialis brevis (ECRB)
- Palmaris longus (PL) to Extensor carpi radialis longus (ECRL)
- Flexor digitorum superficialis (FDS) to Extensor carpi ulnaris (ECU)
Correct Answer: Pronator teres (PT) to Extensor carpi radialis brevis (ECRB)
Explanation:
The classic transfer to restore wrist extension in a radial nerve palsy is the Pronator Teres (PT) transferred to the Extensor Carpi Radialis Brevis (ECRB). The ECRB is chosen over the ECRL because its central location on the wrist provides a more balanced extension without excessive radial deviation.
Question 28:
A 42-year-old recreational basketball player sustains an acute Achilles tendon rupture. He opts for nonoperative management. Based on current high-level evidence, which of the following statements best describes the outcomes of functional rehabilitation compared to surgical repair?
Options:
- Surgical repair results in significantly superior functional scores at 1 year.
- Traditional cast immobilization yields similar re-rupture rates as surgical repair.
- Early functional weight-bearing protocols have re-rupture rates equivalent to surgical repair.
- Surgical repair has a lower rate of iatrogenic nerve injury than nonoperative management.
- Nonoperative management has a higher rate of deep vein thrombosis.
Correct Answer: Early functional weight-bearing protocols have re-rupture rates equivalent to surgical repair.
Explanation:
Recent randomized controlled trials and meta-analyses have demonstrated that when nonoperative management employs early functional rehabilitation and early weight-bearing (functional bracing), the re-rupture rates are equivalent to those of surgical repair, while avoiding the risks of wound complications and surgical site infections.
Question 29:
Titanium alloy (Ti-6Al-4V) is frequently utilized in orthopedic implants, including fracture plates and intramedullary nails. Compared to stainless steel (316L) and cobalt-chrome (Co-Cr) alloys, which of the following is a primary biomechanical advantage of titanium?
Options:
- Higher modulus of elasticity leading to better load sharing
- Lower modulus of elasticity resulting in decreased stress shielding
- Superior resistance to galvanic corrosion when mixed with other metals
- Higher density providing increased implant weight and stability
- Greater resistance to wear and scratching in articulating surfaces
Correct Answer: Lower modulus of elasticity resulting in decreased stress shielding
Explanation:
Titanium has a significantly lower modulus of elasticity (closer to that of cortical bone) compared to stainless steel and cobalt-chrome. This allows for more load sharing with the host bone, thereby decreasing the phenomenon of stress shielding (which can lead to bone resorption around the implant). Titanium is famously poor for wear resistance on articulating surfaces.
Question 30:
A 68-year-old osteoporotic female sustains a proximal humerus fracture. The AP radiograph is shown. According to the Hertel criteria, which of the following radiographic features is the most reliable predictor of humeral head ischemia?
Options:
- Anatomical neck fracture pattern
- Greater tuberosity displacement > 1 cm
- Metaphyseal head extension (calcar segment) less than 8 mm
- Varus angulation greater than 20 degrees
- Disruption of the medial periosteal hinge > 2 mm
Correct Answer: Metaphyseal head extension (calcar segment) less than 8 mm
Explanation:
Hertel et al. described radiographic criteria predictive of humeral head ischemia. The most reliable predictors include a metaphyseal head extension (calcar segment) of less than 8 mm, disruption of the medial hinge (>2 mm), and an anatomic neck fracture. Among the choices, the calcar segment length < 8 mm represents a highly predictive sign that the primary blood supply (the ascending branch of the anterior humeral circumflex artery and intraosseous vessels) has been severely compromised.
Question 31:
A posterior medial meniscal root tear severely compromises normal knee biomechanics. Which of the following statements regarding the biomechanical consequence of a complete posterior medial root tear is most accurate?
Options:
- It results in increased tension on the anterior cruciate ligament but does not alter contact pressures.
- Peak contact pressures in the medial compartment are equivalent to those seen after a total medial meniscectomy.
- The tear increases hoop stresses but maintains normal tibiofemoral kinematics.
- It primarily increases lateral compartment contact pressures due to a varus shift.
- Biomechanical forces remain unchanged if the meniscofemoral ligament of Wrisberg is intact.
Correct Answer: Peak contact pressures in the medial compartment are equivalent to those seen after a total medial meniscectomy.
Explanation:
A complete tear of the posterior medial meniscal root disrupts the meniscal ring, abolishing its ability to convert axial loads into hoop stresses. Biomechanical studies have shown that this effectively renders the meniscus non-functional, resulting in peak contact pressures in the medial compartment that are equivalent to those measured after a total medial meniscectomy.
Question 32:
During a primary posterior-stabilized (PS) total knee arthroplasty, using a measured resection technique, the surgeon evaluates the gaps. The knee is perfectly balanced and symmetrical in extension, but it is too tight in flexion bilaterally. Which of the following is the most appropriate step to balance the knee?
Options:
- Resect more distal femur
- Release the posterior capsule
- Downsize the femoral component and use anterior referencing
- Upsize the femoral component
- Insert a thinner tibial polyethylene liner
Correct Answer: Downsize the femoral component and use anterior referencing
Explanation:
When the knee is tight in flexion but balanced in extension, the flexion gap needs to be increased without affecting the extension gap. Downsizing the femoral component (using anterior referencing to take more bone off the posterior condyles) will increase the flexion gap without altering the extension space. Resecting more distal femur only increases the extension gap. A thinner liner would make the extension gap loose.
Question 33:
A 72-year-old male complains of bilateral calf, thigh, and buttock pain that worsens with walking. He is being evaluated to differentiate between neurogenic claudication (lumbar spinal stenosis) and vascular claudication. Which of the following findings is most specific for neurogenic claudication?
Options:
- Pain relief occurs promptly with standing still.
- Pain is brought on by riding a stationary bicycle.
- Diminished posterior tibial pulses.
- Pain relief when walking uphill or leaning over a shopping cart.
- Skin changes including loss of hair on the lower extremities.
Correct Answer: Pain relief when walking uphill or leaning over a shopping cart.
Explanation:
Pain relief with lumbar flexion (e.g., walking uphill, pushing a shopping cart, or sitting) is a hallmark of neurogenic claudication due to lumbar spinal stenosis. Flexion of the lumbar spine increases the cross-sectional area of the spinal canal and neural foramina, relieving compression on the nerve roots. Vascular claudication typically worsens with walking uphill due to increased metabolic demand, and relieves simply by standing still.
Question 34:
A 28-year-old male presents with knee pain. Radiographs reveal an eccentric, purely lytic epiphyseal lesion extending to the subchondral bone of the proximal tibia. Biopsy histology is shown. Multinucleated giant cells in a background of mononuclear stromal cells are seen. Which systemic medication is specifically designed to target the pathophysiology of this lesion?
Options:
- Methotrexate
- Doxorubicin
- Imatinib
- Denosumab
- Bisphosphonates
Correct Answer: Denosumab
Explanation:
The patient has a Giant Cell Tumor (GCT) of bone. The neoplastic mononuclear stromal cells in GCT express high levels of RANKL, which stimulates the recruitment and differentiation of non-neoplastic multinucleated giant cells that cause the osteolysis. Denosumab is a monoclonal antibody that inhibits RANKL, effectively halting this process and promoting ossification of the lytic defect. It is utilized for unresectable tumors or to facilitate joint salvage.
Question 35:
A 22-year-old male falls onto an extended wrist and sustains a displaced fracture of the proximal pole of the scaphoid. What anatomical feature dictates the precarious blood supply and high risk of avascular necrosis (AVN) in this specific fracture?
Options:
- The proximal pole is supplied exclusively by the anterior interosseous artery.
- Blood supply runs retrograde, with vessels entering the distal half and dorsal ridge before supplying the proximal pole.
- The proximal pole receives its blood supply from a single volar branch of the ulnar artery.
- Blood supply depends entirely on the scapholunate interosseous ligament.
- The scaphoid relies on diffusion from synovial fluid for its entire nutrient supply.
Correct Answer: Blood supply runs retrograde, with vessels entering the distal half and dorsal ridge before supplying the proximal pole.
Explanation:
The major blood supply to the scaphoid comes from branches of the radial artery that enter the bone distally, primarily along the dorsal ridge, and flow in a retrograde direction to perfuse the proximal pole. Fractures through the waist or proximal pole disrupt this retrograde flow, leading to a high incidence of nonunion and avascular necrosis of the proximal fragment.
Question 36:
A 5-year-old child falls on an outstretched hand and sustains the elbow injury shown. The fracture is displaced 4 mm. If left untreated or mismanaged as a simple sprain, what is the most likely long-term clinical complication?
Options:
- Cubitus varus and tardy radial nerve palsy
- Cubitus valgus and tardy ulnar nerve palsy
- Myositis ossificans of the brachialis
- Premature closure of the olecranon apophysis
- Volkmann's ischemic contracture
Correct Answer: Cubitus valgus and tardy ulnar nerve palsy
Explanation:
The scenario describes a lateral condyle fracture of the pediatric humerus. Because the lateral condyle provides the lateral buttress of the elbow and is intra-articular, nonunion (due to inadequate immobilization or failure to fix a displaced fracture) commonly leads to a progressive cubitus valgus deformity. Over time, the increased carrying angle stretches the ulnar nerve behind the medial epicondyle, resulting in a tardy ulnar nerve palsy.
Question 37:
A 24-year-old football player sustains a high-energy hyperplantarflexion midfoot injury. Weight-bearing radiographs show a 2.5 mm widening between the base of the first and second metatarsals. An avulsion fracture ('Fleck sign') is seen. The structure avulsed normally attaches to which two bones?
Options:
- Medial cuneiform and base of the first metatarsal
- Middle cuneiform and base of the second metatarsal
- Medial cuneiform and base of the second metatarsal
- Lateral cuneiform and cuboid
- Navicular and medial cuneiform
Correct Answer: Medial cuneiform and base of the second metatarsal
Explanation:
The 'Fleck sign' represents an avulsion of the Lisfranc ligament. This critical, stout ligament originates on the lateral aspect of the medial cuneiform and inserts on the medial aspect of the base of the second metatarsal. It is the primary stabilizer of the midfoot, as there is no direct ligamentous connection between the first and second metatarsal bases.
Question 38:
In the treatment of unstable intertrochanteric femur fractures with a cephalomedullary nail, achieving correct lag screw placement is critical. According to the original study by Baumgaertner et al., what is the ideal tip-apex distance (TAD) recommended to minimize the risk of lag screw cut-out?
Options:
- Less than 10 mm
- Less than 15 mm
- Less than 25 mm
- Less than 35 mm
- Greater than 25 mm
Correct Answer: Less than 25 mm
Explanation:
Baumgaertner et al. defined the tip-apex distance (TAD) as the sum of the distance from the tip of the lag screw to the apex of the femoral head on both AP and lateral radiographs, after correcting for magnification. A TAD of less than 25 mm was shown to significantly correlate with a minimal risk of lag screw cut-out in the treatment of intertrochanteric fractures.
Question 39:
Normal articular cartilage is divided into distinct zones. In which zone is the concentration of water and collagen the highest, with chondrocytes characteristically flattened and arranged parallel to the joint surface?
Options:
- Superficial (tangential) zone
- Middle (transitional) zone
- Deep (radial) zone
- Tidemark
- Calcified cartilage zone
Correct Answer: Superficial (tangential) zone
Explanation:
The superficial (tangential) zone of articular cartilage contains the highest concentration of water (approximately 80%) and the highest concentration of collagen (primarily Type II). The collagen fibrils and flattened chondrocytes are aligned parallel to the articular surface to resist shear forces.
Question 40:
A 22-year-old rugby player has a history of recurrent anterior shoulder instability. A 3D reconstructed pre-operative CT scan is shown. The imaging demonstrates an inverted pear-shaped glenoid with a calculated anterior-inferior bone loss of 27%. What is the most appropriate surgical management to minimize his recurrence risk?
Options:
- Arthroscopic Bankart repair with capsular plication
- Arthroscopic remplissage alone
- Open inferior capsular shift
- Latarjet procedure (coracoid transfer)
- Thermal capsulorrhaphy
Correct Answer: Latarjet procedure (coracoid transfer)
Explanation:
In patients with anterior shoulder instability and significant glenoid bone loss (>20-25%, often creating an 'inverted pear' appearance), soft tissue procedures alone (like an arthroscopic Bankart repair) have unacceptably high recurrence rates. A bony augmentation procedure, most commonly the Latarjet procedure (transfer of the coracoid process with the attached conjoint tendon to the anterior glenoid neck), is the gold standard treatment.