Full Question & Answer Text (for Search Engines)
Question 1:
A 35-year-old male is involved in a high-speed motor vehicle collision and sustains the pelvic ring injury shown below. In an Anteroposterior Compression Type III (APC-III) injury, which ligamentous complex is completely disrupted resulting in global pelvic instability?
Options:
- Anterior sacroiliac ligaments only
- Anterior sacroiliac and sacrospinous ligaments only
- Anterior sacroiliac, sacrospinous, sacrotuberous, and posterior sacroiliac ligaments
- Sacrotuberous ligaments only
- Iliolumbar ligaments only
Correct Answer: Anterior sacroiliac, sacrospinous, sacrotuberous, and posterior sacroiliac ligaments
Explanation:
An APC-III injury represents a complete disruption of both the anterior and posterior pelvic rings. The symphysis is widened, and there is complete disruption of the anterior sacroiliac (SI), sacrospinous, sacrotuberous, and posterior SI ligaments. This results in global instability (both rotational and vertical). APC-II injuries typically spare the posterior SI ligaments.
Question 2:
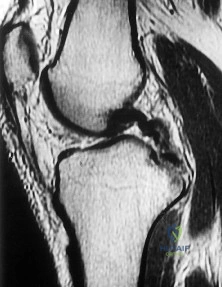
A 42-year-old manual laborer presents with chronic progressive wrist pain and weakness. In the predictable progression of Scapholunate Advanced Collapse (SLAC), which articulation is characteristically spared due to its concentric spherical anatomy?
Options:
- Radioscaphoid
- Capitolunate
- Radiolunate
- Scaphocapitate
- Trapeziometacarpal
Correct Answer: Radiolunate
Explanation:
In SLAC wrist, the radiolunate articulation is characteristically spared, even in late stages. This is due to the concentric, spherical shape of the radiolunate joint, which distributes forces evenly and avoids the abnormal shear forces that cause early degeneration in the radioscaphoid (Stage I/II) and capitolunate (Stage III) joints.
Question 3:
A 72-year-old female undergoes a reverse total shoulder arthroplasty (rTSA) for massive, irreparable cuff tear arthropathy. By medializing and distalizing the center of rotation (COR), which of the following primary biomechanical advantages is achieved?
Options:
- Decreased deltoid moment arm
- Increased shear forces at the glenosphere-baseplate interface
- Increased deltoid moment arm and recruitment of anterior/posterior deltoid fibers
- Restoration of the normal anatomic center of rotation
- Increased tension on the remaining superior rotator cuff
Correct Answer: Increased deltoid moment arm and recruitment of anterior/posterior deltoid fibers
Explanation:
Reverse total shoulder arthroplasty alters the biomechanics of the shoulder by medializing and distalizing the center of rotation. This significantly increases the moment arm of the deltoid, improving its mechanical advantage, and recruits more of the anterior and posterior deltoid fibers to assist with elevation in the absence of a functional rotator cuff.
Question 4:
A 12-year-old obese male presents with a 3-week history of groin pain and an obligatory external rotation of the hip during flexion. What is the primary pathoanatomic mechanical failure occurring in the proximal femur?
Options:
- Failure through the zone of resting cartilage
- Failure through the zone of proliferation
- Failure through the zone of hypertrophy
- Failure through the zone of provisional calcification
- Failure of the labral suction seal
Correct Answer: Failure through the zone of hypertrophy
Explanation:
Slipped Capital Femoral Epiphysis (SCFE) occurs due to shear failure through the physis. Histologically, this failure specifically occurs through the zone of hypertrophy, which is the weakest zone of the growth plate due to an increased matrix-to-cell ratio and decreased structural integrity.
Question 5:
You are reviewing basic science concepts regarding articular cartilage. Which structural zone of articular cartilage contains the highest concentration of water and features collagen fibers oriented parallel to the articular surface to resist shear forces?
Options:
- Superficial (tangential) zone
- Middle (transitional) zone
- Deep (radial) zone
- Tidemark
- Calcified cartilage zone
Correct Answer: Superficial (tangential) zone
Explanation:
The superficial (tangential) zone of articular cartilage makes up 10-20% of articular cartilage thickness. It has the highest water content, lowest proteoglycan content, and densely packed collagen fibers oriented parallel to the joint surface to primarily resist shear forces.
Question 6:
A 45-year-old male is involved in a diving accident resulting in a cervical spine injury. He presents awake, alert, and cooperative, but examination reveals a complete C5 ASIA A spinal cord injury. What is the most appropriate initial management for this bilateral facet dislocation?
Options:
- Immediate MRI to rule out disc herniation prior to any reduction attempts
- Urgent closed awake cervical traction and reduction
- Emergent open posterior reduction and fusion
- Emergent open anterior reduction and fusion
- High-dose intravenous methylprednisolone administration over 24 hours
Correct Answer: Urgent closed awake cervical traction and reduction
Explanation:
In an awake, alert, and cooperative patient with a cervical facet dislocation and a neurologic deficit, urgent closed reduction via skeletal traction is the standard of care. An MRI is not mandatory before attempting closed reduction in an examinable patient, as rapid decompression of the spinal cord is paramount.
Question 7:
A 15-year-old male presents with distal femoral pain. Biopsy confirms conventional high-grade osteosarcoma. He undergoes 10 weeks of neoadjuvant chemotherapy. Following wide surgical resection, histopathologic analysis is performed. Which of the following findings defines a 'good response' to chemotherapy, serving as the strongest prognostic indicator for overall survival?
Options:
- Greater than 90% tumor necrosis
- Greater than 99% tumor necrosis
- High presence of intralesional CD8+ lymphocytes
- Decrease in overall tumor volume by greater than 50%
- Complete ossification of the tumor matrix
Correct Answer: Greater than 90% tumor necrosis
Explanation:
The histologic response to neoadjuvant chemotherapy is the most important prognostic factor in osteosarcoma. A 'good response' is traditionally defined by the Huvos grading system as >90% tumor necrosis (Grade III is 91-99%, Grade IV is 100% necrosis). Patients with a good response have significantly improved long-term survival.
Question 8:
A 28-year-old male sustains a high-energy basicervical femoral neck fracture. He undergoes closed reduction and percutaneous pinning with three cannulated screws. Which of the following screw configurations provides the most biomechanically stable construct?
Options:
- Inverted triangle configuration with screws placed adjacent to the anterior, posterior, and inferior cortices
- Triangle configuration with apex superior, centrally located in the femoral neck
- Two parallel screws placed centrally
- Three divergent screws originating from the lateral cortex
- Four parallel screws clustered centrally
Correct Answer: Inverted triangle configuration with screws placed adjacent to the anterior, posterior, and inferior cortices
Explanation:
For cannulated screw fixation of femoral neck fractures, the most biomechanically stable construct is an inverted triangle configuration. The screws should be placed as far apart as possible, immediately adjacent to the inferior calcar, anterior, and posterior cortices to maximize the spread and leverage, increasing resistance to bending and torsional forces.
Question 9:
A 30-year-old athlete sustains a hyperplantarflexion injury to his midfoot. Weight-bearing radiographs show 3mm of widening between the medial and middle cuneiforms. What is the primary stabilizing structure of the Lisfranc joint complex?
Options:
- Dorsal tarsometatarsal ligament
- Plantar ligament connecting the medial cuneiform to the base of the second metatarsal
- Peroneus longus tendon
- Plantar fascia
- Interosseous ligament between the first and second metatarsals
Correct Answer: Plantar ligament connecting the medial cuneiform to the base of the second metatarsal
Explanation:
The Lisfranc ligament is an intra-articular ligament that connects the lateral aspect of the medial cuneiform to the medial base of the second metatarsal. It is the strongest and primary stabilizer of the Lisfranc joint complex. The dorsal ligaments are relatively weak, predisposing the joint to dorsal dislocation during hyperplantarflexion.
Question 10:
During a posterolateral approach for a total hip arthroplasty, the short external rotators are detached. The primary blood supply to the native femoral head is the medial femoral circumflex artery (MFCA). Where is the main branch of the MFCA located relative to the short external rotators?
Options:
- Anterior to the obturator externus
- Superior to the piriformis tendon
- Between the piriformis and superior gemellus
- Superior to the upper border of the quadratus femoris and deep to the obturator externus
- Superficial to the gluteus maximus
Correct Answer: Superior to the upper border of the quadratus femoris and deep to the obturator externus
Explanation:
The main branch of the medial femoral circumflex artery (MFCA) consistently runs superior to the upper border of the quadratus femoris and deep (anterior) to the obturator externus tendon. During the posterolateral approach, leaving the obturator externus intact or avoiding dissection inferior to the quadratus femoris protects the MFCA.
Question 11:
A 4-month-old female with Developmental Dysplasia of the Hip (DDH) is being treated with a Pavlik harness. Two weeks into treatment, examination reveals absent active knee extension on the affected side. What is the most likely iatrogenic cause?
Options:
- Obturator nerve palsy from excessive abduction
- Femoral nerve palsy from excessive hyperflexion
- Sciatic nerve palsy from excessive extension
- Development of a septic hip joint
- Avascular necrosis of the femoral head
Correct Answer: Femoral nerve palsy from excessive hyperflexion
Explanation:
Femoral nerve palsy is a known complication of the Pavlik harness, typically caused by excessive hip hyperflexion which compresses the femoral nerve against the inguinal ligament. It manifests as decreased spontaneous leg movement and absent active knee extension. The harness should be adjusted to reduce flexion or temporarily removed.
Question 12:
In orthopedic surgery, preoperative antibiotics are routinely administered. Which of the following prophylactic antibiotics functions primarily by inhibiting bacterial cell wall synthesis via binding to the D-alanyl-D-alanine termini of the peptidoglycan precursor?
Options:
- Cefazolin
- Gentamicin
- Vancomycin
- Clindamycin
- Ciprofloxacin
Correct Answer: Vancomycin
Explanation:
Vancomycin is a glycopeptide antibiotic that inhibits cell wall synthesis by binding tightly to the D-alanyl-D-alanine terminus of the cell wall precursor units, preventing peptidoglycan polymerization. Cefazolin (a cephalosporin) also inhibits cell wall synthesis but does so by binding to penicillin-binding proteins (PBPs).
Question 13:
A 65-year-old male undergoes an L4-L5 decompression and pedicle screw fixation. During pedicle preparation, an instrument breaches the inferior cortical wall of the L4 pedicle. Which neural structure is most directly at risk for iatrogenic injury?
Options:
- L3 exiting nerve root
- L4 exiting nerve root
- L5 traversing nerve root
- S1 traversing nerve root
- Thecal sac
Correct Answer: L4 exiting nerve root
Explanation:
In the lumbar spine, the exiting nerve root travels inferior to the pedicle of its corresponding numbered vertebra (e.g., the L4 nerve root exits through the L4-L5 foramen, traveling immediately inferior to the L4 pedicle). An inferior breach of the L4 pedicle puts the L4 exiting nerve root directly at risk. A medial breach puts the dural sac and traversing L5 root at risk.
Question 14:
During an anatomic double-bundle Anterior Cruciate Ligament (ACL) reconstruction, the surgeon aims to replicate native knee kinematics. Which of the following accurately describes the tensioning pattern of the native ACL bundles during knee range of motion?
Options:
- The AM bundle is tightest in extension and the PL bundle in flexion
- The AM bundle is tightest in flexion and the PL bundle is tightest in extension
- Both bundles are tightest in deep flexion
- Both bundles are tightest in full extension
- The PL bundle controls purely valgus stability
Correct Answer: The AM bundle is tightest in flexion and the PL bundle is tightest in extension
Explanation:
The native ACL consists of two primary bundles: the anteromedial (AM) bundle and the posterolateral (PL) bundle. Biomechanically, the AM bundle is tightest in flexion (providing primary anterior stability at 90 degrees), while the PL bundle is tightest in extension (providing primary rotatory stability near full extension).
Question 15:
A 24-year-old carpenter sustains a volar laceration over the proximal phalanx of his index finger, severing both the Flexor Digitorum Superficialis (FDS) and Flexor Digitorum Profundus (FDP) tendons. This injury corresponds to which flexor tendon zone?
Options:
- Zone I
- Zone II
- Zone III
- Zone IV
- Zone V
Correct Answer: Zone II
Explanation:
Zone II (historically called 'No Man\'s Land') extends from the A1 pulley (distal palmar crease) to the insertion of the FDS on the middle phalanx. Injuries here typically involve both the FDS and FDP tendons within the narrow fibro-osseous sheath, making surgical repair challenging due to a high risk of postoperative adhesions.
Question 16:
A 40-year-old skier sustains a Schatzker Type II (split-depressed) fracture of the lateral tibial plateau. Which of the following is the most commonly associated soft tissue injury that must be evaluated and potentially addressed?
Options:
- Popliteal artery intimal tear
- Common peroneal nerve neuropraxia
- Lateral meniscus tear
- Posterior cruciate ligament rupture
- Medial collateral ligament avulsion
Correct Answer: Lateral meniscus tear
Explanation:
Schatzker Type II fractures (split-depressed fractures of the lateral tibial plateau) are highly associated with lateral meniscal tears, which can become trapped in the fracture site. Schatzker IV (medial plateau) and higher-energy variants have a higher association with neurovascular (popliteal artery, peroneal nerve) injuries.
Question 17:
Receptor Activator of Nuclear factor Kappa-B Ligand (RANKL) is critical for osteoclast differentiation, activation, and survival. Which cell type is the primary endogenous source of RANKL in the bone microenvironment?
Options:
- Osteoclasts
- Osteoblasts
- Macrophages
- Chondrocytes
- Hematopoietic stem cells
Correct Answer: Osteoblasts
Explanation:
Osteoblasts (and bone marrow stromal cells) are the primary source of RANKL. RANKL binds to the RANK receptor on osteoclast precursors (macrophage lineage), driving their differentiation and activation. Osteoprotegerin (OPG), also secreted by osteoblasts, acts as a decoy receptor to inhibit this process.
Question 18:
When applying the Ponseti method for the serial casting of idiopathic clubfoot (talipes equinovarus), the deformity must be corrected in a specific sequence to unlock the subtalar joint. What is the correct order of deformity correction?
Options:
- Cavus, Adductus, Varus, Equinus
- Varus, Adductus, Cavus, Equinus
- Equinus, Cavus, Adductus, Varus
- Adductus, Varus, Cavus, Equinus
- Cavus, Varus, Adductus, Equinus
Correct Answer: Cavus, Adductus, Varus, Equinus
Explanation:
The Ponseti method dictates sequential correction following the CAVE acronym: Cavus (by elevating the first ray), Adductus, Varus, and finally Equinus (often requiring a percutaneous Achilles tenotomy). Correcting the cavus first aligns the forefoot with the hindfoot, allowing the talonavicular joint to be reduced.
Question 19:
A 10-year-old boy presents with severe, unrelenting thigh pain. Radiographs reveal a permeative diaphyseal lesion in the femur with a multilamellated 'onion-skin' periosteal reaction. Genetic testing reveals a t(11;22) chromosomal translocation. Which fusion protein is characteristic of this tumor?
Options:
- SYT-SSX1
- EWS-FLI1
- TLS-CHOP
- PAX3-FKHR
- MYC amplification
Correct Answer: EWS-FLI1
Explanation:
The clinical presentation and 'onion-skin' periosteal reaction suggest Ewing Sarcoma. The hallmark of Ewing Sarcoma is the t(11;22)(q24;q12) translocation, which results in the EWS-FLI1 fusion protein. SYT-SSX is seen in synovial sarcoma, TLS-CHOP in myxoid liposarcoma, and PAX3-FKHR in alveolar rhabdomyosarcoma.
Question 20:
A 22-year-old collegiate hockey player presents with chronic groin pain exacerbated by hip flexion, adduction, and internal rotation. Imaging demonstrates a lack of femoral head-neck offset, presenting as a 'pistol grip' deformity. This Cam-type impingement primarily damages which structure initially?
Options:
- Ligamentum teres
- Acetabular labrum at the posteroinferior quadrant
- Articular cartilage of the anterosuperior acetabulum via shear forces
- Femoral head articular cartilage via direct impaction
- Iliopsoas tendon at the pelvic brim
Correct Answer: Articular cartilage of the anterosuperior acetabulum via shear forces
Explanation:
Cam impingement (aspherical femoral head/reduced offset) forces a non-spherical portion of the femoral head into the acetabulum during flexion. This primarily causes outside-in shear forces, leading to delamination of the anterosuperior acetabular articular cartilage, often with secondary separation of the adjacent labrum. Pincer impingement, conversely, causes direct linear compression of the labrum.
Question 21:
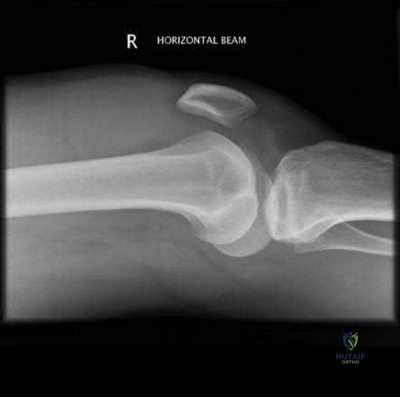
A 12-year-old obese boy presents with left hip pain and an obligate external rotation of the hip during flexion. A radiograph is shown below. What is the most appropriate initial management for the condition demonstrated?
Options:
- Non-weight bearing and urgent in-situ percutaneous pinning
- Closed reduction and hip spica casting
- Open reduction and surgical dislocation (Dunn procedure)
- Protected weight-bearing and serial observation
- Proximal femoral intertrochanteric osteotomy
Correct Answer: Non-weight bearing and urgent in-situ percutaneous pinning
Explanation:
The clinical presentation and radiograph represent a stable Slipped Capital Femoral Epiphysis (SCFE). The gold standard for initial management of a stable SCFE is in-situ pinning, typically utilizing a single partially threaded cannulated screw placed in the center-center position of the epiphysis to prevent further slip and promote physeal closure.
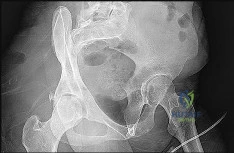
Question 22:
A 35-year-old man is involved in a high-speed motor vehicle collision. Judet views demonstrate a both-column acetabular fracture. Based on the fracture characteristics, which of the following features most strongly indicates the need for an anterior ilioinguinal approach rather than a posterior Kocher-Langenbeck approach?
Options:
- Medial displacement of the quadrilateral plate
- Severe posterior wall comminution
- Presence of a complete sciatic nerve palsy
- Transverse fracture pattern crossing the tectum
- Anterior column displacement predominating over posterior displacement
Correct Answer: Anterior column displacement predominating over posterior displacement
Explanation:
The choice of surgical approach in acetabular fractures is largely dictated by the column with the maximal displacement. An anterior ilioinguinal approach is classically indicated for anterior column, anterior wall, and associated anterior-predominant fractures. A Kocher-Langenbeck approach is chosen when posterior wall/column displacement predominates.
Question 23:
A 16-year-old boy presents with progressive knee pain. Radiographs demonstrate a destructive distal femoral lesion with a 'sunburst' periosteal reaction as shown below. Biopsy confirms high-grade intramedullary osteosarcoma. Following neoadjuvant therapy and surgical resection, what is the single most important prognostic factor for long-term survival?
Options:
- Anatomic location of the tumor
- Histologic tumor necrosis response to neoadjuvant chemotherapy
- Preoperative serum alkaline phosphatase level
- Absolute tumor volume prior to resection
- Extent of soft tissue intramedullary extension
Correct Answer: Histologic tumor necrosis response to neoadjuvant chemotherapy
Explanation:
The image and presentation are classic for a conventional high-grade osteosarcoma. While factors like tumor size and alkaline phosphatase have prognostic value, the most critical prognostic indicator for overall survival is the degree of histologic necrosis (typically aiming for >90% necrosis) following neoadjuvant chemotherapy.
Question 24:
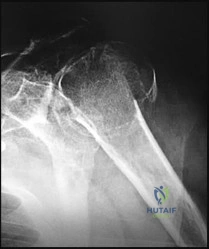
A 72-year-old woman with chronic pseudoparalysis of the shoulder undergoes the procedure shown in the radiograph below. Which of the following is the most commonly reported radiographic complication specifically associated with this biomechanical implant design?
Options:
- Scapular notching
- Glenoid component aseptic loosening
- Acromial stress fracture
- Greater tuberosity nonunion
- Humeral stem subsidence
Correct Answer: Scapular notching
Explanation:
The image depicts a reverse total shoulder arthroplasty (RTSA). Scapular notching, caused by mechanical impingement of the medial humeral metaphysis against the inferior scapular neck during adduction, is the most common radiographic complication. It is historically highest with medialized glenosphere and inlay humerus implant designs.
Question 25:
A 25-year-old football player presents with severe midfoot pain after an axial load was applied to his plantarflexed foot. Weight-bearing radiographs demonstrate widening between the medial and middle cuneiforms without associated fractures. What is the most appropriate surgical management for this purely ligamentous injury variant?
Options:
- Primary arthrodesis of the first, second, and third tarsometatarsal joints
- Closed reduction and prolonged non-weight bearing cast immobilization
- Open reduction and internal fixation with dorsal bridge plating
- Open reduction and internal fixation with transarticular screws
- Percutaneous Kirschner wire fixation
Correct Answer: Primary arthrodesis of the first, second, and third tarsometatarsal joints
Explanation:
The scenario describes a purely ligamentous Lisfranc injury. Multiple studies have shown that primary arthrodesis of the medial column (1st, 2nd, and 3rd TMT joints) for purely ligamentous Lisfranc injuries yields superior patient-reported functional outcomes and lower revision rates compared to traditional ORIF.
Question 26:
A 40-year-old man presents after a diving accident. He is awake, alert, and cooperative, but demonstrates bilateral upper and lower extremity weakness (incomplete tetraplegia). The lateral cervical radiograph shows a bilateral facet dislocation. What is the most appropriate next step in acute management to decompress the spinal cord?
Options:
- Stat MRI of the cervical spine
- Awake closed traction reduction with Gardner-Wells tongs
- Immediate anterior cervical discectomy and fusion
- Immediate posterior cervical laminectomy and fusion
- Administration of the NASCIS-III high-dose methylprednisolone protocol
Correct Answer: Awake closed traction reduction with Gardner-Wells tongs
Explanation:
In an awake, alert, and examinable patient with a cervical facet dislocation and a neurologic deficit, urgent awake closed reduction via cranial traction is the standard of care to rapidly decompress the spinal cord. An MRI is required prior to closed reduction ONLY if the patient is unexaminable (e.g., obtunded, intubated) or fails closed reduction, to rule out a large anterior disc herniation that could be dragged into the canal during reduction.
Question 27:
A 28-year-old carpenter sustains a laceration to the volar aspect of his index finger, resulting in a Zone II flexor digitorum profundus (FDP) transection. He undergoes an immediate primary 4-strand core repair with an epitendinous suture. During his postoperative rehabilitation, at what time point is the healing tendon repair biomechanically at its weakest?
Options:
- Days 1-3
- Days 5-21
- Days 28-35
- Days 42-49
- Days 60-90
Correct Answer: Days 5-21
Explanation:
Following primary flexor tendon repair, the tendon strength initially decreases due to the inflammatory response and softening of the tendon ends. The repair is biomechanically at its weakest point between days 5 and 21 (early fibroblastic phase) before substantial collagen cross-linking restores tensile strength.
Question 28:
Bone graft substitutes are frequently used in orthopedic surgery to augment fusion masses and treat osseous defects. Which of the following bone graft substitutes functions primarily as an osteoinductive agent rather than being purely osteoconductive?
Options:
- Medical-grade calcium sulfate
- Beta-tricalcium phosphate
- Demineralized bone matrix (DBM)
- Cancellous freeze-dried allograft
- Porous hydroxyapatite
Correct Answer: Demineralized bone matrix (DBM)
Explanation:
Demineralized bone matrix (DBM) is processed to remove the mineral component of bone, leaving behind the organic matrix which contains varying levels of bone morphogenetic proteins (BMPs). These proteins make DBM an osteoinductive agent. Calcium sulfate, tricalcium phosphate, and hydroxyapatite are purely osteoconductive.
Question 29:
A 35-year-old construction worker falls 15 feet, sustaining a high-energy distal tibia fracture extending into the plafond with significant soft tissue swelling and fracture blisters. Which of the following surgical strategies is most widely accepted as the standard of care to minimize soft tissue complications in this specific injury pattern?
Options:
- Immediate single-stage open reduction and internal fixation of the tibia and fibula
- Primary arthrodesis of the tibiotalar joint
- Immediate spanning external fixation with delayed definitive internal fixation of the tibia
- Immediate reamed intramedullary nailing of the tibia with percutaneous articular screws
- Immediate circular fine-wire frame application as definitive single-stage treatment
Correct Answer: Immediate spanning external fixation with delayed definitive internal fixation of the tibia
Explanation:
High-energy pilon fractures are notorious for severe soft-tissue compromise. The standard of care to minimize devastating wound complications (such as dehiscence and deep infection) is a staged protocol: initial spanning external fixation to restore length and alignment, allowing the soft-tissue envelope to recover (e.g., return of skin wrinkles), followed by delayed definitive ORIF 1-3 weeks later.
Question 30:
A 25-year-old male sustains a severe knee dislocation resulting in an injury to the anterior cruciate ligament (ACL), posterior cruciate ligament (PCL), and posterolateral corner (PLC). Following acute multiligament reconstruction, including the PLC, which of the following post-operative rehabilitation parameters is most critical to protect the PLC repair?
Options:
- Immediate full weight-bearing on the operative leg
- Avoiding active isolated knee flexion against gravity for 6 weeks
- Avoiding active open-chain knee extension for 6 weeks
- Immobilization strictly in 90 degrees of flexion
- Continuous passive motion stressing the limb in varus
Correct Answer: Avoiding active isolated knee flexion against gravity for 6 weeks
Explanation:
Active knee flexion against gravity isolates and activates the hamstrings. Hamstring contraction exerts a posterior and external rotatory force on the proximal tibia, placing severe stress on the newly reconstructed posterolateral corner (and PCL). Therefore, active hamstring contraction/knee flexion is typically avoided for the first 6 weeks postoperatively.
Question 31:
In the Ponseti method for the conservative management of idiopathic clubfoot, the sequence of deformity correction is strictly ordered to avoid creating a midfoot break. What is the correct sequence of correction?
Options:
- Cavus, Adductus, Varus, Equinus
- Equinus, Varus, Adductus, Cavus
- Cavus, Varus, Adductus, Equinus
- Adductus, Varus, Cavus, Equinus
- Equinus, Adductus, Varus, Cavus
Correct Answer: Cavus, Adductus, Varus, Equinus
Explanation:
The Ponseti method systematically corrects clubfoot deformities following the acronym CAVE: Cavus (corrected first by supinating the forefoot to align it with the hindfoot), followed simultaneously by Adductus and Varus (by abducting the foot around the head of the talus), and finally Equinus (often requiring a percutaneous Achilles tenotomy).
Question 32:
A 30-year-old female presents with knee pain. Radiographs reveal an eccentric, lytic lesion in the distal femoral epiphysis without a sclerotic margin. Biopsy shows multinucleated giant cells in a background of mononuclear stromal cells. The patient is treated with Denosumab prior to curettage. What is the mechanism of action of this medication?
Options:
- Inhibits RANK ligand (RANKL)
- Directly induces apoptosis of multinucleated giant cells
- Inhibits vascular endothelial growth factor (VEGF)
- Binds directly to the RANK receptor on osteoclast precursors
- Inhibits matrix metalloproteinases (MMPs) in the stroma
Correct Answer: Inhibits RANK ligand (RANKL)
Explanation:
Denosumab is a human monoclonal antibody that specifically binds to and inhibits Receptor Activator of Nuclear factor Kappa-B Ligand (RANKL). In Giant Cell Tumor of bone, the neoplastic mononuclear stromal cells secrete excessive RANKL, which recruits and activates the reactive, bone-resorbing multinucleated giant cells. By blocking RANKL, Denosumab halts this process.
Question 33:
In total hip arthroplasty, the choice of bearing surface can impact the long-term survivorship of the implant. Which of the following bearing surface combinations exhibits the lowest in vitro volumetric wear rate?
Options:
- Cobalt-chrome on highly cross-linked polyethylene
- Ceramic on ceramic
- Ceramic on highly cross-linked polyethylene
- Cobalt-chrome on conventional polyethylene
- Oxinium on highly cross-linked polyethylene
Correct Answer: Ceramic on ceramic
Explanation:
Ceramic-on-ceramic (CoC) bearing surfaces have the lowest volumetric wear rate and produce the smallest, least biologically active wear particles among all conventional THA bearing combinations. They are extremely hard and scratch-resistant, though they carry a unique risk of squeaking and catastrophic component fracture.
Question 34:
A 42-year-old man sustains a closed spiral fracture of the middle third of the humeral shaft (Holstein-Lewis type). He has an immediate complete radial nerve palsy on presentation. He is treated non-operatively in a functional fracture brace. At 12 weeks post-injury, there is no clinical recovery, and an electromyogram (EMG) shows no signs of reinnervation. What is the most appropriate next step in management?
Options:
- Continue bracing and repeat EMG in 3 months
- Surgical exploration of the radial nerve
- Immediate tendon transfers for wrist and finger extension
- Open reduction and internal fixation of the humerus
- Ultrasound-guided corticosteroid injection around the radial nerve
Correct Answer: Surgical exploration of the radial nerve
Explanation:
Primary radial nerve palsy in the setting of a closed humerus fracture is usually a neuropraxia and observed initially. However, if there are no clinical or electromyographic (EMG) signs of recovery by 12-16 weeks, surgical exploration of the nerve is indicated to assess for transection, entrapment, or severe neuroma requiring grafting/repair.
Question 35:
In the radiographic evaluation of adult spinal deformity, pelvic parameters are critical for restoring sagittal balance. Which of the following equations accurately defines the geometric relationship between pelvic incidence (PI), pelvic tilt (PT), and sacral slope (SS)?
Options:
- PI = PT + SS
- PI = PT - SS
- PT = PI + SS
- SS = PI x PT
- PI = (PT + SS) / 2
Correct Answer: PI = PT + SS
Explanation:
Pelvic incidence (PI) is a fixed anatomical morphological parameter unique to each individual after skeletal maturity. It dictates the orientation of the pelvis and is geometrically equal to the sum of the pelvic tilt (PT) and the sacral slope (SS): PI = PT + SS. A patient's required lumbar lordosis is typically matched to their PI (LL = PI ± 9 degrees).
Question 36:
A 28-year-old male sustains a vertically oriented, displaced basicervical femoral neck fracture (Pauwels Type III). He undergoes open reduction and internal fixation. Which of the following biomechanical forces across the fracture site is the primary cause of fixation failure and nonunion in this specific fracture pattern?
Options:
- Axial compression
- Anterior translation
- Shear stress
- Tension on the medial calcar
- Rotational torque
Correct Answer: Shear stress
Explanation:
Pauwels Type III fractures are characterized by a highly vertical fracture line (angle > 50 degrees to the horizontal). This vertical orientation converts joint reactive forces primarily into extreme shear forces at the fracture site, which promotes varus displacement and nonunion, making it biomechanically the most challenging femoral neck fracture to stabilize.
Question 37:
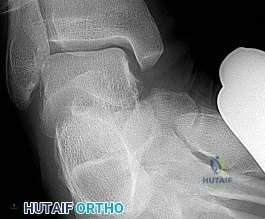
A 55-year-old male with poorly controlled diabetes mellitus presents with a unilaterally swollen, erythematous, and warm foot without open ulcerations. Radiographs show early periarticular fragmentation and joint subluxation at the tarsometatarsal joints. Inflammatory markers (WBC, CRP, ESR) are normal. What is the most appropriate initial management for this condition?
Options:
- Urgent surgical debridement and extensive arthrodesis
- Intravenous empiric antibiotics
- Total contact casting and strict non-weight bearing
- Prescription of a custom orthotic depth shoe
- Intra-articular corticosteroid injection
Correct Answer: Total contact casting and strict non-weight bearing
Explanation:
The clinical picture describes acute Eichenholtz Stage 1 (fragmentation) Charcot neuroarthropathy. With normal inflammatory markers and no ulcer, the primary differential is active Charcot versus infection; the diagnosis is Charcot. The gold standard for initial management of acute Charcot is offloading and immobilization, most effectively achieved with a Total Contact Cast (TCC) until the extremity progresses to the coalescence/consolidation phases.
Question 38:
Articular cartilage relies on the precise biochemical composition and structural orientation of its extracellular matrix for compressive and tensile strength. Which histological zone of articular cartilage is characterized by the highest concentration of water and the lowest concentration of proteoglycans?
Options:
- Superficial (tangential) zone
- Middle (transitional) zone
- Deep (radial) zone
- Calcified zone
- The tidemark
Correct Answer: Superficial (tangential) zone
Explanation:
The superficial (tangential) zone of articular cartilage contains the highest water content (approximately 80%), the lowest concentration of proteoglycans, and collagen fibrils that are oriented parallel to the joint surface to maximally resist shear stresses.
Question 39:
A 22-year-old rugby player grasps an opponent's jersey and forcefully extends his forcefully flexing ring finger, sustaining an avulsion of the flexor digitorum profundus (FDP) tendon. The avulsed tendon retracts proximally into the palm (Zone II/III). According to the Leddy and Packer classification, what type of injury is this, and what is the recommended timeframe for surgical repair?
Options:
- Type I; repair within 7-10 days
- Type II; repair within 3-4 weeks
- Type III; repair anytime within 3 months
- Type I; delayed reconstruction after 6 weeks
- Type IV; immediate primary arthrodesis of the DIP joint
Correct Answer: Type I; repair within 7-10 days
Explanation:
This describes a Leddy and Packer Type I Jersey finger injury, where the FDP tendon retracts into the palm. This proximal retraction completely disrupts the vincula (the tendon's blood supply). To prevent tendon necrosis and irreversible myostatic contracture, early primary repair within 7-10 days is strictly recommended.
Question 40:
A 32-year-old male undergoes reamed intramedullary nailing for a closed tibial shaft fracture. In the recovery room, he complains of severe, escalating pain out of proportion to the injury. The clinical exam is equivocal due to a regional block. Compartment pressures are measured. Which of the following parameter thresholds is the most reliable indicator for acute compartment syndrome?
Options:
- Absolute compartment pressure > 20 mmHg
- Diastolic blood pressure minus compartment pressure ≤ 30 mmHg
- Mean arterial pressure minus compartment pressure ≤ 45 mmHg
- Absolute compartment pressure > 25 mmHg
- Systolic blood pressure minus compartment pressure ≤ 30 mmHg
Correct Answer: Diastolic blood pressure minus compartment pressure ≤ 30 mmHg
Explanation:
The diagnosis of acute compartment syndrome relies on the perfusion pressure of the limb. A delta pressure (Diastolic Blood Pressure minus Compartment Pressure) of less than or equal to 30 mmHg is the most reliable and widely accepted diagnostic threshold for acute compartment syndrome, as it accounts for patient-specific hemodynamic variations better than an absolute pressure cutoff.