Full Question & Answer Text (for Search Engines)
Question 1:
A 28-year-old male presents after a diving accident. He is awake and alert, complaining of severe neck pain. Neurological exam reveals 4/5 strength in right elbow flexion and wrist extension, with numbness extending into the thumb. Radiographs are obtained showing a unilateral facet dislocation. If an awake closed reduction is attempted but fails, what is the most appropriate next step in management?
Options:
- Immediate anterior cervical discectomy and fusion
- Immediate posterior cervical fusion with instrumentation
- Obtain an MRI of the cervical spine
- Application of a halo vest and observation
- High-dose intravenous methylprednisolone
Correct Answer: Obtain an MRI of the cervical spine
Explanation:
In an awake, cooperative patient with a cervical facet dislocation, closed reduction via cranial traction may be attempted prior to MRI. However, if closed reduction fails, an MRI MUST be obtained prior to any open reduction to evaluate for a herniated nucleus pulposus. If a herniated disc is present, an anterior approach is necessary to decompress the spinal cord before the facet joint is reduced, mitigating the risk of devastating iatrogenic spinal cord injury.
Question 2:
A 45-year-old manual laborer complains of chronic radial-sided wrist pain. He recalls a severe 'sprain' 10 years ago. Radiographs demonstrate scapholunate dissociation with advanced radioscaphoid arthritis. MRI confirms the radiolunate joint is spared, but the proximal capitate shows severe, full-thickness chondral wear. Which of the following procedures is most appropriate to provide durable pain relief while preserving motion?
Options:
- Proximal row carpectomy (PRC)
- Scaphoid excision and four-corner fusion
- Total wrist arthroplasty
- Scapholunate ligament reconstruction using a tendon graft
- Radial styloidectomy and posterior interosseous nerve neurectomy
Correct Answer: Scaphoid excision and four-corner fusion
Explanation:
The patient has Scapholunate Advanced Collapse (SLAC) pattern of the wrist. Stage III SLAC involves the capitolunate joint, while the radiolunate joint characteristically remains spared. Because the capitate head is severely arthritic, Proximal Row Carpectomy (PRC) is contraindicated, as it relies on a healthy cartilage interface between the capitate and the lunate fossa. Scaphoid excision with four-corner fusion (capitate, hamate, lunate, triquetrum) is the procedure of choice.
Question 3:
A 13-year-old obese male presents with left hip pain and an obligatory external rotation of the left hip when it is passively flexed. Radiographs confirm a severe left slipped capital femoral epiphysis (SCFE). Which of the following patient characteristics is an absolute indication for prophylactic pinning of the contralateral asymptomatic right hip?
Options:
- Patient age greater than 14 years at presentation
- Presence of a diagnosed endocrine disorder
- Severe slip angle (>50 degrees) on the symptomatic side
- Male gender with a BMI > 95th percentile
- Inability to ambulate on the affected limb
Correct Answer: Presence of a diagnosed endocrine disorder
Explanation:
Prophylactic pinning of the contralateral asymptomatic hip in a patient with a unilateral SCFE is controversial for standard cases, but it is unequivocally recommended for patients with underlying endocrine disorders (such as hypothyroidism, panhypopituitarism, and renal osteodystrophy). These patients have an exceptionally high incidence of bilateral involvement. Other factors like young age (<10 years) or open triradiate cartilage may also sway a surgeon toward prophylactic pinning.
Question 4:
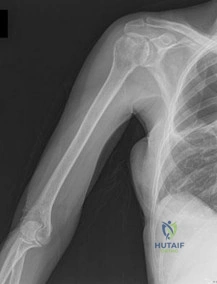
A 65-year-old male who underwent a cementless total hip arthroplasty (THA) 15 years ago presents with new-onset thigh pain. Radiographs reveal eccentric positioning of the femoral head within the acetabular shell and large retroacetabular and proximal femoral radiolucencies. What is the primary biological mediator released by macrophages that directly stimulates osteoclastogenesis and is responsible for the observed bone loss?
Options:
- Interleukin-10 (IL-10)
- Transforming growth factor beta (TGF-B)
- Tumor necrosis factor alpha (TNF-a)
- Interferon gamma (IFN-y)
- Interleukin-4 (IL-4)
Correct Answer: Tumor necrosis factor alpha (TNF-a)
Explanation:
The radiograph demonstrates particle-induced osteolysis, secondary to polyethylene wear debris. When macrophages phagocytose these particles, they release pro-inflammatory cytokines, most notably TNF-a, IL-1, and IL-6. These cytokines stimulate the RANK/RANKL pathway, activating osteoclasts and leading to significant periprosthetic bone loss. IL-10 and IL-4 are anti-inflammatory cytokines, while IFN-y actually inhibits osteoclastogenesis.
Question 5:
A 42-year-old female sustains a high-energy trauma resulting in a complex bicondylar tibial plateau fracture. When planning a standard dual-incision approach (anterolateral and posteromedial) for open reduction and internal fixation, what neurovascular structure is most directly at risk during the superficial dissection of the posteromedial approach?
Options:
- Common peroneal nerve
- Popliteal artery
- Saphenous nerve
- Anterior tibial artery
- Sural nerve
Correct Answer: Saphenous nerve
Explanation:
The posteromedial approach to the proximal tibia utilizes the interval between the pes anserinus (retracted anteriorly) and the medial head of the gastrocnemius (retracted posteriorly). During the superficial dissection, the saphenous nerve and the great saphenous vein are directly at risk and must be carefully mobilized and protected. The common peroneal nerve is at risk laterally. The popliteal artery is posterior to the popliteus and is typically protected by the gastrocnemius during this approach.
Question 6:
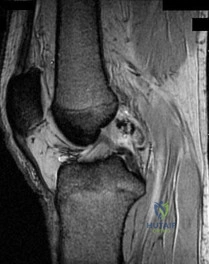
A 22-year-old soccer player sustains a twisting injury to the knee resulting in a rapid effusion. MRI demonstrates a complete midsubstance rupture of the anterior cruciate ligament (ACL). Which of the following concomitant meniscal injuries is statistically most commonly associated with an acute ACL rupture?
Options:
- Medial meniscus bucket-handle tear
- Lateral meniscus posterior horn tear
- Medial meniscus root tear
- Lateral meniscus anterior horn tear
- Discoid lateral meniscus tear
Correct Answer: Lateral meniscus posterior horn tear
Explanation:
In the setting of an acute ACL tear, tears of the lateral meniscus (particularly the posterior horn) are the most common concomitant meniscal injury, seen in roughly 50-70% of acute cases. Conversely, in the chronic ACL-deficient knee, medial meniscus tears become much more common due to the long-term altered kinematics and repeated anterior translation of the tibia, which puts the posterior horn of the medial meniscus under chronic shear stress.
Question 7:
A 30-year-old male sustains an axial load to a plantarflexed foot. On physical examination, there is pronounced plantar ecchymosis and localized pain with passive pronation and abduction of the forefoot. The primary stabilizing ligament of the disrupted joint complex connects which two osseous structures?
Options:
- Medial cuneiform and second metatarsal base
- Middle cuneiform and second metatarsal base
- Medial cuneiform and first metatarsal base
- Cuboid and fourth metatarsal base
- Navicular and medial cuneiform
Correct Answer: Medial cuneiform and second metatarsal base
Explanation:
Plantar ecchymosis in the midfoot is the pathognomonic sign of a Lisfranc injury. The Lisfranc ligament is an interosseous ligament that represents the strongest and most critical stabilizer of the tarsometatarsal complex. It runs obliquely from the lateral aspect of the medial cuneiform to the medial base of the second metatarsal. There is notably no direct transverse ligamentous connection between the bases of the first and second metatarsals.
Question 8:
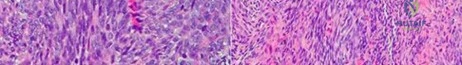
A 15-year-old male presents with deep knee pain awakening him at night. Radiographs show a permeative destructive lesion in the distal femoral metaphysis with a 'sunburst' periosteal reaction and Codman's triangle. Biopsy confirms high-grade conventional osteosarcoma. What is the most critical prognostic factor for long-term overall survival in this patient?
Options:
- Tumor volume at initial presentation
- Histologic subtype (e.g., osteoblastic vs. chondroblastic)
- Presence of skip metastases on initial MRI
- Percentage of tumor necrosis following neoadjuvant chemotherapy
- Patient age and gender at diagnosis
Correct Answer: Percentage of tumor necrosis following neoadjuvant chemotherapy
Explanation:
For localized high-grade osteosarcoma, the most important prognostic indicator is the histologic response to neoadjuvant chemotherapy. This is evaluated during the definitive resection. A 'good response' is typically defined as greater than 90% or 99% tumor necrosis. Patients who achieve this level of necrosis have a significantly improved disease-free and overall survival rate compared to 'poor responders' who have extensive viable tumor cells remaining.
Question 9:
During secondary fracture healing in the setting of relative stability, the fracture callus progresses through an endochondral ossification pathway. Which of the following transcription factors is fundamentally essential for the differentiation of mesenchymal stem cells into chondrocytes to form the initial soft callus?
Options:
- Runx2
- Sox9
- Osterix (Sp7)
- NFATc1
- Beta-catenin
Correct Answer: Sox9
Explanation:
Secondary fracture healing relies heavily on endochondral ossification, beginning with a cartilaginous soft callus. Sox9 is the master transcription factor required for chondrocyte differentiation. Runx2 and Osterix are key transcription factors for osteoblast differentiation (membranous ossification and hard callus formation). NFATc1 is critical for osteoclastogenesis. Beta-catenin is a key component of the Wnt signaling pathway, which promotes osteoblastogenesis while actually suppressing chondrogenesis.
Question 10:
A 72-year-old female presents with chronic right hip pain beginning 2 years following an uncomplicated total hip arthroplasty. Her ESR is 45 mm/hr and CRP is 2.5 mg/dL. A fluoroscopically guided hip aspiration yields synovial fluid with a white blood cell count of 4,500 cells/µL with 85% polymorphonuclear neutrophils. An alpha-defensin immunoassay is positive. According to the MSIS/ICM criteria, what is the most appropriate next surgical step in management?
Options:
- Prescribe a 6-week course of oral antibiotics and reassess
- Perform an open biopsy and wait for final culture results before intervening
- Perform an open irrigation and debridement with modular part exchange (DAIR)
- Perform a two-stage revision arthroplasty
- Proceed with a single-stage exchange arthroplasty without delay
Correct Answer: Perform a two-stage revision arthroplasty
Explanation:
This patient meets the major and minor criteria for a chronic Periprosthetic Joint Infection (PJI) (elevated ESR/CRP, high synovial WBC and PMN%, positive alpha-defensin). Because the symptoms and the index procedure are chronic (>4 weeks), a debridement, antibiotics, and implant retention (DAIR) procedure is contraindicated due to mature biofilm formation. The gold standard treatment for chronic PJI in North America is a two-stage exchange revision arthroplasty.
Question 11:
A 4-month-old infant is being treated with a Pavlik harness for a completely dislocated left hip (Developmental Dysplasia of the Hip). After 3 weeks of strict harness wear, a dynamic ultrasound demonstrates that the left hip remains persistently dislocated. What is the most appropriate next step in management?
Options:
- Continue the Pavlik harness for an additional 3 to 4 weeks
- Adjust the anterior straps to increase hip flexion past 120 degrees
- Transition to a rigid abduction orthosis or perform a closed reduction and spica casting
- Perform an immediate open reduction and Dega pelvic osteotomy
- Discontinue the harness and delay further intervention until the child is walking
Correct Answer: Transition to a rigid abduction orthosis or perform a closed reduction and spica casting
Explanation:
If a hip remains dislocated after 3 to 4 weeks of compliant Pavlik harness use, it is considered a failure, and the harness must be abandoned to prevent 'Pavlik harness disease' (posterior acetabular wear and worsening of the dysplasia). Increasing flexion past 110-120 degrees places the child at high risk for femoral nerve palsy. The next appropriate step is either transitioning to a rigid abduction orthosis (like an Ilfeld splint) or performing a closed reduction under anesthesia followed by spica casting.
Question 12:
A 13-year-old elite baseball pitcher presents with vague, insidious onset shoulder pain that is worst during the deceleration phase of throwing. He denies any acute pop or trauma. Radiographs reveal widening and lateral fragmentation of the proximal humeral physis compared to the contralateral shoulder. What is the most appropriate initial management?
Options:
- Corticosteroid injection into the subacromial space
- Immediate surgical epiphyseodesis to prevent slippage
- Complete cessation of throwing for 3 months followed by a structured return-to-throw program
- Continuation of throwing with a strict pitch count limit
- Arthroscopic labral repair and capsular plication
Correct Answer: Complete cessation of throwing for 3 months followed by a structured return-to-throw program
Explanation:
The patient is presenting with 'Little League Shoulder,' which is proximal humeral epiphysiolysis. It is an overuse injury caused by repetitive rotational stress on the open physis during the throwing motion. The mainstay of treatment is absolute rest from throwing, typically for 3 months, or until the patient is completely pain-free and radiographs show healing of the physis. Once healed, a gradual return-to-throw program focusing on pitching mechanics is initiated.
Question 13:
A 78-year-old male presents after a fall from standing. CT of the cervical spine demonstrates a displaced Type II odontoid fracture. Which of the following factors has been shown in the literature to be the strongest predictor of nonunion if this patient is treated non-operatively in a cervical collar?
Options:
- Initial fracture displacement greater than 5 mm
- Anterior angulation of the dens less than 10 degrees
- Female gender
- Concomitant anterior arch fracture of C1
- The use of a rigid cervical collar instead of a halo vest
Correct Answer: Initial fracture displacement greater than 5 mm
Explanation:
Type II odontoid fractures have a high rate of nonunion, particularly in the elderly. Risk factors for nonunion include patient age >50 years, initial fracture displacement >5 mm, posterior displacement of the dens, and initial angulation >10 degrees. While halo vests provide stiffer immobilization than collars, they carry significant morbidity in the elderly. The degree of initial displacement (>5 mm) remains one of the most critical intrinsic fracture characteristics predicting failure of non-operative management.
Question 14:
A 55-year-old patient with poorly controlled type II diabetes presents with a red, hot, swollen right foot. Inflammatory markers are normal and an MRI confirms no osteomyelitis. Radiographs reveal prominent periarticular osseous debris, fragmentation of the navicular and cuneiforms, and subluxation of the tarsometatarsal joints. According to the Eichenholtz classification of Charcot arthropathy, what stage does this clinical and radiographic picture represent?
Options:
- Stage 0
- Stage I
- Stage II
- Stage III
- Stage IV
Correct Answer: Stage I
Explanation:
The Eichenholtz classification describes the natural history of Charcot arthropathy. Stage 0 is the acute inflammatory stage without radiographic changes. Stage I (Development/Fragmentation) is characterized clinically by a hot, swollen foot and radiographically by osteopenia, periarticular fragmentation, bony debris, and subluxation/dislocation. Stage II (Coalescence) shows absorption of fine debris, fusion of larger fragments, and early sclerosis. Stage III (Consolidation) shows remodeling, rounding of bone ends, and stable deformity.
Question 15:
A 28-year-old rugby player presents unable to actively flex the distal interphalangeal (DIP) joint of his ring finger after grabbing an opponent's jersey. Radiographs reveal a small bony avulsion fragment located at the level of the proximal interphalangeal (PIP) joint. According to the Leddy and Packer classification, what type of injury is this?
Options:
- Type I
- Type II
- Type III
- Type IV
- Type V
Correct Answer: Type II
Explanation:
Jersey finger represents an avulsion of the flexor digitorum profundus (FDP) tendon. Leddy and Packer classification: Type I involves retraction to the palm, both vincula ruptured (high risk of ischemia, requires urgent repair). Type II involves retraction to the PIP joint level, where it is held by the intact vinculum longus; a small bony fragment may be seen at this level. Type III involves a large bony avulsion that is caught at the A4 pulley (DIP joint level). This patient has a Type II injury.
Question 16:
A 32-year-old male develops extreme pain out of proportion, pain with passive stretch, and tense compartments following a closed tibial shaft fracture. Which of the following best describes the fundamental pathophysiologic mechanism leading to cellular hypoxia and tissue death in acute compartment syndrome?
Options:
- Arterial occlusion from mechanical compression of the primary nutrient artery
- Decreased local arteriovenous (AV) pressure gradient leading to capillary collapse
- Massive venodilation causing pooling of blood and stasis within the muscle
- Direct traumatic disruption of the microvasculature preventing collateral flow
- Reperfusion injury mediated by oxygen free radicals upon cast bivalving
Correct Answer: Decreased local arteriovenous (AV) pressure gradient leading to capillary collapse
Explanation:
The pathophysiology of compartment syndrome is driven by an increase in interstitial tissue pressure within a closed non-yielding fascial space. As tissue pressure rises, it quickly surpasses the low capillary venous pressure, severely impairing venous outflow. This leads to a decreased arteriovenous (AV) pressure gradient, resulting in diminished local capillary blood flow, capillary collapse, ischemia, and subsequent muscle/nerve necrosis. Arterial inflow is typically maintained until very late, which is why pulses are usually palpable even in established compartment syndrome.
Question 17:
A 35-year-old female is diagnosed with a locally aggressive giant cell tumor of the distal radius. Preoperative administration of Denosumab is planned to facilitate downstaging and joint-salvage surgery. What is the exact mechanism of action of Denosumab in this context?
Options:
- Monoclonal antibody that binds directly to the RANK receptor on the surface of osteoclasts
- Monoclonal antibody that binds to RANK Ligand (RANKL) preventing its interaction with RANK
- Small molecule inhibitor of the tyrosine kinase VEGF receptor preventing angiogenesis
- Bisphosphonate that induces osteoclast apoptosis by inhibiting farnesyl pyrophosphate synthase
- Selective estrogen receptor modulator (SERM) that enhances systemic osteoprotegerin (OPG) production
Correct Answer: Monoclonal antibody that binds to RANK Ligand (RANKL) preventing its interaction with RANK
Explanation:
Denosumab is a fully human monoclonal antibody that specifically binds to RANKL (Receptor Activator of Nuclear factor Kappa-B Ligand). By binding to RANKL, it prevents it from interacting with the RANK receptor on the surface of osteoclasts and osteoclast precursors. In Giant Cell Tumor of bone, the neoplastic mononuclear stromal cells express high levels of RANKL, which aggressively recruits and activates the reactive multinucleated giant cells (osteoclasts) that cause bone destruction.
Question 18:
A 60-year-old male presents with isolated medial compartment knee osteoarthritis and is being evaluated for a unicompartmental knee arthroplasty (UKA). According to classical indications (Kozinn and Scott), which of the following is considered an absolute contraindication to a fixed-bearing UKA?
Options:
- Patient age greater than 55 years
- Presence of a flexible 10-degree varus deformity
- Complete deficiency of the anterior cruciate ligament (ACL)
- Radiographic evidence of asymptomatic patellofemoral osteophytes
- Patient weight of 85 kg
Correct Answer: Complete deficiency of the anterior cruciate ligament (ACL)
Explanation:
Classical criteria for unicompartmental knee arthroplasty (UKA) include an intact anterior cruciate ligament (ACL). ACL deficiency leads to altered knee kinematics, specifically paradoxical anterior translation of the tibia during flexion, which results in accelerated posterior polyethylene wear and early failure of a fixed-bearing UKA. While some modern surgeons perform UKA in ACL-deficient knees using mobile-bearing designs or concurrent ACL reconstruction, an absent ACL remains a classic board-tested contraindication for standard UKA.
Question 19:
A 40-year-old carpenter presents with the inability to form an 'OK' sign with his thumb and index finger; instead, he forms a flat pinch. Sensation in the hand, fingers, and forearm is completely normal. Which of the following muscles is most likely affected by this isolated nerve lesion?
Options:
- Flexor digitorum superficialis to the index finger
- Flexor pollicis brevis
- Flexor digitorum profundus to the index finger
- Abductor pollicis brevis
- Opponens pollicis
Correct Answer: Flexor digitorum profundus to the index finger
Explanation:
The patient is exhibiting the classic 'OK sign' deficit, which is pathognomonic for Anterior Interosseous Nerve (AIN) syndrome. The AIN is a pure motor branch of the median nerve (hence the normal sensation) that innervates the Flexor Pollicis Longus (FPL), the Flexor Digitorum Profundus (FDP) to the index and middle fingers, and the Pronator Quadratus. The inability to flex the DIP joint of the index finger (FDP) and the IP joint of the thumb (FPL) results in a flat pinch rather than a rounded 'OK' sign.
Question 20:
A neonate is diagnosed with achondroplasia, the most common form of short-limb dwarfism. This condition is primarily characterized by a defect in the proliferation and hypertrophy of chondrocytes in the physis. Which specific genetic mutation and inheritance pattern is most commonly responsible for this disorder?
Options:
- COL1A1 gene mutation, Autosomal Dominant
- COMP gene mutation, Autosomal Dominant
- FGFR3 gene mutation, Autosomal Dominant
- FGFR3 gene mutation, Autosomal Recessive
- SOX9 gene mutation, X-linked Dominant
Correct Answer: FGFR3 gene mutation, Autosomal Dominant
Explanation:
Achondroplasia is caused by an activating point mutation in the Fibroblast Growth Factor Receptor 3 (FGFR3) gene. The inheritance pattern is Autosomal Dominant, although approximately 80% of cases occur as sporadic de novo mutations, which are strongly associated with advanced paternal age. The mutant FGFR3 is constitutively active and functions as an abnormal inhibitor of chondrocyte proliferation in the proliferative zone of the physis, leading to diminished endochondral ossification.