Full Question & Answer Text (for Search Engines)
Question 1:
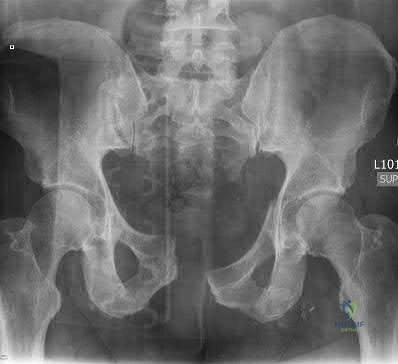
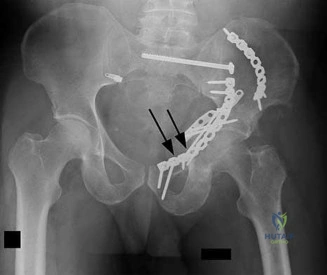
A 45-year-old male sustains an anterior-posterior compression (APC) type III pelvic ring injury following a crush injury. He is hemodynamically unstable upon arrival. If an arterial source of bleeding is identified on pelvic angiography, which of the following arteries is most likely to be injured based on the fracture pattern?
Options:
- Superior gluteal artery
- Inferior gluteal artery
- Internal pudendal artery
- External iliac artery
- Iliolumbar artery
Correct Answer: Internal pudendal artery
Explanation:
In anterior-posterior compression (APC) injuries, the internal pudendal and obturator arteries are the most commonly injured arterial branches due to disruption of the anterior ring. Conversely, in lateral compression injuries and fractures extending through the greater sciatic notch, the superior gluteal artery is the most frequently injured.
Question 2:
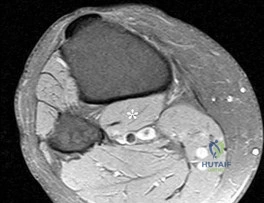
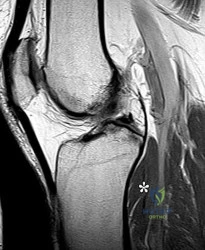
A 22-year-old elite soccer player undergoes an anterior cruciate ligament (ACL) reconstruction. Preoperatively, she demonstrated a high-grade pivot shift test. The surgeon decides to perform an anterolateral ligament (ALL) reconstruction concurrently to improve rotational stability. Which of the following is true regarding the anatomy and biomechanics of the ALL?
Options:
- Its femoral origin is proximal and anterior to the fibular collateral ligament (FCL) attachment.
- It acts as a primary restraint to varus opening at 30 degrees of flexion.
- Its femoral origin is posterior and proximal to the lateral epicondyle.
- It inserts directly onto the fibular head.
- It is primarily responsible for preventing posterior tibial translation.
Correct Answer: Its femoral origin is posterior and proximal to the lateral epicondyle.
Explanation:
The anterolateral ligament (ALL) originates posterior and proximal to the lateral femoral epicondyle and inserts on the proximal tibia midway between Gerdy's tubercle and the fibular head. It acts as a secondary restraint to internal tibial rotation and the pivot shift phenomenon.
Question 3:
A 65-year-old highly active male is undergoing a total hip arthroplasty (THA). The surgeon is discussing bearing surface options with him. Which of the following is a recognized biomechanical or clinical characteristic of ceramic-on-ceramic (CoC) bearings compared to metal-on-polyethylene (MoP) bearings?
Options:
- Higher linear and volumetric wear rates
- Elimination of squeaking risk postoperatively
- Reduced risk of volumetric wear and subsequent osteolysis
- Increased susceptibility to third-body wear damage
- Increased systemic metal ion levels requiring annual monitoring
Correct Answer: Reduced risk of volumetric wear and subsequent osteolysis
Explanation:
Ceramic-on-ceramic (CoC) bearings possess excellent scratch resistance and have the lowest linear and volumetric wear rates among the available bearing surfaces, significantly reducing the incidence of wear particle-induced osteolysis. However, they carry a unique risk of squeaking and catastrophic ceramic component fracture.
Question 4:
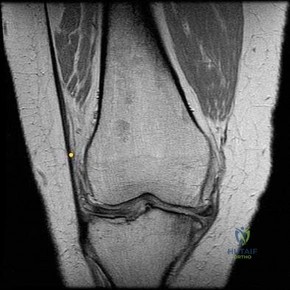
A 60-year-old male presents with progressively worsening manual dexterity and balance issues over the past 8 months. Examination reveals a positive Hoffmann's sign and hyperreflexia. MRI shows multi-level cervical stenosis with cord signal changes. Which of the following MRI findings most strongly predicts a poor neurologic recovery following surgical decompression?
Options:
- Presence of T2 hyperintensity confined to a single level
- Duration of symptoms strictly less than 6 months
- Transverse area of the spinal cord of 50 mm^2 at the level of maximum compression
- Multilevel spondylosis without foraminal stenosis
- Presence of T1 hypointensity within the spinal cord
Correct Answer: Presence of T1 hypointensity within the spinal cord
Explanation:
In the setting of cervical spondylotic myelopathy, T1 hypointensity on MRI represents permanent structural damage to the spinal cord (myelomalacia, necrosis, or cavitation) and is a strong independent predictor of poor clinical outcomes and limited neurologic recovery following decompression. T2 hyperintensity alone can represent reversible edema.
Question 5:
A 12-year-old boy presents with left thigh pain and an antalgic gait for 4 weeks. Radiographs confirm a stable left slipped capital femoral epiphysis (SCFE). Prophylactic in situ pinning of the contralateral asymptomatic right hip is most strongly indicated if the patient has which of the following concomitant conditions?
Options:
- A chronologic age of 14 years at presentation
- A body mass index (BMI) tracking in the 50th percentile
- A diagnosis of hypothyroidism or panhypopituitarism
- A slip angle of 20 degrees on the symptomatic left side
- A modified Oxford bone age score of 22
Correct Answer: A diagnosis of hypothyroidism or panhypopituitarism
Explanation:
Patients with endocrine disorders (such as hypothyroidism, growth hormone deficiency) or renal osteodystrophy are at a significantly elevated risk for bilateral slipped capital femoral epiphysis (SCFE). In these populations, prophylactic pinning of the contralateral hip is highly recommended, regardless of their chronological age.
Question 6:
A 45-year-old manual laborer presents with chronic, progressive dorsal wrist pain and weakness. Radiographs demonstrate scapholunate advanced collapse (SLAC) stage II. Which of the following best describes the anatomical distribution of arthritis and an appropriate salvage procedure for this stage?
Options:
- Arthritis confined to the radioscaphoid joint; treatable with scaphoid excision and four-corner fusion.
- Arthritis involving the radioscaphoid and capitolunate joints; treatable with proximal row carpectomy (PRC).
- Arthritis involving the radiolunate joint; requiring total wrist arthrodesis.
- Arthritis confined to the radial styloid; treatable with isolated radial styloidectomy.
- Arthritis involving the pisotriquetral joint; treatable with isolated pisiform excision.
Correct Answer: Arthritis confined to the radioscaphoid joint; treatable with scaphoid excision and four-corner fusion.
Explanation:
SLAC Stage I involves the radial styloid and distal scaphoid. Stage II involves the entire radioscaphoid joint. Stage III involves the capitolunate joint. The radiolunate joint is typically spared in SLAC wrists. Proximal row carpectomy (PRC) or four-corner fusion with scaphoid excision are appropriate for Stage II, but PRC is contraindicated in Stage III due to capitolunate arthritis.
Question 7:
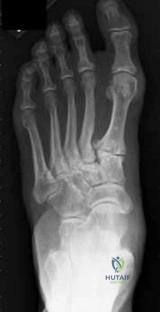
A 55-year-old male with poorly controlled diabetes mellitus and severe peripheral neuropathy presents with a globally swollen, erythematous, and warm left foot. He denies any inciting trauma. Radiographs show periarticular debris and subtle fragmentation at the tarsometatarsal joints. Which of the following is the most appropriate initial management?
Options:
- Immediate open reduction and internal fixation to restore arch alignment
- Total contact casting and strict non-weight-bearing precautions
- Admission for intravenous antibiotics and surgical debridement of the joints
- Corticosteroid injection into the affected tarsometatarsal joints to reduce inflammation
- Guillotine amputation at the transmalleolar level to prevent sepsis
Correct Answer: Total contact casting and strict non-weight-bearing precautions
Explanation:
The patient is presenting with acute Charcot arthropathy (Eichenholtz stage 0 or 1). The clinical picture mimics infection, but the lack of an ulcer or systemic signs points to Charcot. The mainstay of initial treatment during the acute inflammatory phase is immobilization (usually via total contact casting) and non-weight-bearing to arrest the destructive process and prevent further deformity.
Question 8:
A 30-year-old male presents with a slow-growing, deep-seated, painful soft tissue mass in his left foot near the ankle joint. Imaging reveals a heterogeneous mass with stippled calcifications. Biopsy demonstrates a biphasic pattern consisting of spindle cells and epithelial cells. Which of the following cytogenetic abnormalities is classically associated with this tumor?
Options:
- t(11;22)(q24;q12)
- t(x;18)(p11;q11)
- t(9;22)(q22;q12)
- t(12;16)(q13;p11)
- t(2;13)(q35;q14)
Correct Answer: t(x;18)(p11;q11)
Explanation:
The clinical, radiographic, and histologic descriptions are classic for synovial sarcoma. Synovial sarcoma is characterized by the specific chromosomal translocation t(X;18)(p11;q11), which results in the SYT-SSX fusion gene. This molecular marker is highly sensitive and specific for confirming the diagnosis.
Question 9:
In the manufacturing of modern orthopedic implants, titanium alloys are frequently utilized due to their excellent biocompatibility and mechanical profile. Which of the following best explains the primary mechanism underlying titanium's exceptional corrosion resistance in vivo?
Options:
- Galvanic coupling with surrounding soft tissues and bone
- Spontaneous formation of a passive, inert titanium dioxide (TiO2) layer on its surface
- Its extremely high modulus of elasticity closely matching cortical bone
- Constant release of osteoinductive titanium ions inhibiting macrophage activation
- A low coefficient of friction when articulating against ultra-high-molecular-weight polyethylene
Correct Answer: Spontaneous formation of a passive, inert titanium dioxide (TiO2) layer on its surface
Explanation:
Titanium and its alloys owe their high biocompatibility and excellent corrosion resistance to the spontaneous formation of a thin, passive, adherent oxide layer (primarily titanium dioxide, TiO2) on their surface when exposed to air or bodily fluids. This inert layer prevents further oxidation and interaction with the surrounding biological environment.
Question 10:
A 75-year-old female sustains a displaced femoral neck fracture. Prior to the injury, she was highly active, living independently, and ambulating without assistive devices. She undergoes a total hip arthroplasty (THA). Compared to a bipolar hemiarthroplasty, what is a known long-term clinical advantage of THA for this specific patient profile?
Options:
- Significantly lower dislocation rate
- Lower intraoperative surgical blood loss
- Shorter mean operative time
- Lower risk of long-term reoperation for any reason
- Reduced postoperative risk of deep vein thrombosis
Correct Answer: Lower risk of long-term reoperation for any reason
Explanation:
In active, independent older adults with displaced femoral neck fractures, total hip arthroplasty (THA) is associated with better functional outcomes, less long-term groin pain (no acetabular cartilage wear), and lower long-term reoperation rates compared to hemiarthroplasty. This comes at the expense of a higher initial risk of dislocation, longer surgical times, and increased blood loss.
Question 11:
A 50-year-old male undergoes arthroscopic rotator cuff repair for a massive, retracted tear. To improve lateral excursion of the supraspinatus tendon, the surgeon releases the coracohumeral ligament (CHL). Which of the following is true regarding the physiological function of the intact CHL?
Options:
- It primarily originates on the acromion and inserts on the greater tuberosity.
- It acts as a primary restraint to external rotation when the arm is adducted.
- It seamlessly blends with the inferior glenohumeral ligament complex.
- It acts as a dynamic active stabilizer of the long head of the biceps tendon.
- It limits internal rotation when the arm is abducted to 90 degrees.
Correct Answer: It acts as a primary restraint to external rotation when the arm is adducted.
Explanation:
The coracohumeral ligament (CHL) originates on the base of the coracoid process and blends into the rotator interval, inserting onto the greater and lesser tuberosities. It is a primary static restraint to inferior translation and external rotation of the humerus when the shoulder is in an adducted position.
Question 12:
During a primary posterior-stabilized (PS) total knee arthroplasty, the surgeon notices that the knee has symmetric extension and flexion gaps at 90 degrees, but exhibits a sudden 'cam jump' phenomenon when the knee is passively flexed past 110 degrees. Which of the following intraoperative variables is the most likely cause of this kinematic abnormality?
Options:
- A pathologically loose flexion gap relative to the size of the components
- An excessively tight extension gap due to inadequate distal femoral resection
- Use of an oversized femoral component causing patellofemoral overstuffing
- The tibial component being placed with excessive anterior slope
- Significant joint line elevation from extensive distal femoral cuts
Correct Answer: A pathologically loose flexion gap relative to the size of the components
Explanation:
In a posterior-stabilized (PS) TKA, 'cam jump' or dislocation of the cam-post mechanism typically occurs in deep flexion. The primary cause of this phenomenon is a loose flexion gap (often combined with insufficient posterior tibial slope or a small femoral component). This laxity allows the femur to translate anteriorly relative to the tibia in deep flexion, clearing the post.
Question 13:
A 35-year-old male presents following a high-speed motor vehicle accident. CT scan shows a T12 burst fracture with 40% canal compromise. His neurologic exam reveals 3/5 strength in bilateral hip flexors and knee extensors, with preserved perineal sensation. According to the Thoracolumbar Injury Classification and Severity Score (TLICS), how many points are assigned specifically for his neurologic status, and what is the overall treatment implication?
Options:
- 2 points; favoring nonoperative treatment
- 3 points; favoring operative treatment
- 3 points; favoring nonoperative treatment
- 2 points; favoring operative treatment
- 4 points; favoring operative treatment
Correct Answer: 3 points; favoring operative treatment
Explanation:
The TLICS system allocates points based on morphology, neurologic status, and posterior ligamentous complex (PLC) integrity. For neurologic status: intact = 0, nerve root = 2, complete cord injury = 2, incomplete cord injury/cauda equina = 3. This patient has an incomplete deficit (3 points). With morphology being a burst fracture (2 points), the score is at least 5, which strongly favors operative intervention.
Question 14:
An 8-week-old infant with rigid, idiopathic clubfoot is undergoing serial casting using the Ponseti method. To achieve a plantigrade, functional foot, the deformity must be systematically corrected in a specific sequence. Which of the following accurately represents the correct sequence of correction?
Options:
- Equinus, varus, adductus, cavus
- Cavus, adductus, varus, equinus
- Adductus, varus, cavus, equinus
- Varus, cavus, adductus, equinus
- Cavus, varus, adductus, equinus
Correct Answer: Cavus, adductus, varus, equinus
Explanation:
The Ponseti method dictates that clubfoot deformities should be corrected in the specific order summarized by the mnemonic CAVE: Cavus (corrected first by elevating the first ray to supinate the forefoot), Adductus, Varus, and finally Equinus (which often requires a percutaneous Achilles tenotomy as the final step).
Question 15:
A 55-year-old female with long-standing type 2 diabetes presents with a painful, catching ring finger that locks in flexion. She is diagnosed with stenosing tenosynovitis (trigger finger). Which annular pulley is primarily implicated in the pathogenesis of this condition, and what is its anatomic relationship to the corresponding joint?
Options:
- A1 pulley; located at the level of the proximal interphalangeal (PIP) joint
- A2 pulley; located over the mid-portion of the proximal phalanx
- A1 pulley; located at the level of the metacarpophalangeal (MCP) joint
- C1 pulley; located immediately distal to the A1 pulley
- A3 pulley; located at the level of the PIP joint
Correct Answer: A1 pulley; located at the level of the metacarpophalangeal (MCP) joint
Explanation:
Trigger finger is caused by a size mismatch between the flexor tendon (often with a reactive nodule) and the retinacular sheath, primarily at the A1 pulley. The A1 pulley is located palmar to the metacarpophalangeal (MCP) joint. The A2 pulley is over the proximal phalanx, and the A3 pulley is over the PIP joint.
Question 16:
A 40-year-old female presents with a symptomatic hallux valgus deformity that has failed conservative shoe wear modification. Weight-bearing radiographs reveal a hallux valgus angle (HVA) of 35 degrees and a 1-2 intermetatarsal angle (IMA) of 16 degrees. Clinical exam shows a stable first tarsometatarsal (TMT) joint without hypermobility. Which of the following surgical procedures is most biomechanically appropriate?
Options:
- Distal chevron osteotomy
- Proximal metatarsal osteotomy combined with distal soft tissue reconstruction
- First TMT joint arthrodesis (Lapidus procedure)
- First metatarsophalangeal (MTP) joint arthrodesis
- Keller resection arthroplasty
Correct Answer: Proximal metatarsal osteotomy combined with distal soft tissue reconstruction
Explanation:
An intermetatarsal angle (IMA) greater than 13-15 degrees represents a moderate-to-severe deformity. A proximal osteotomy (e.g., Ludloff, crescentic, or proximal chevron) combined with a distal soft tissue release provides superior corrective power for larger IMAs. Distal osteotomies are reserved for mild deformities (IMA < 13 degrees). A Lapidus is indicated if first ray hypermobility is present.
Question 17:
A 15-year-old boy presents with severe nocturnal thigh pain that awakens him from sleep but is dramatically relieved by NSAIDs. Radiographs show dense cortical thickening in the proximal femoral diaphysis. CT scan reveals a 6 mm radiolucent nidus surrounded by intense reactive sclerosis. Which of the following is true regarding the pathophysiology of this specific lesion?
Options:
- It produces high local levels of prostaglandins, particularly PGE2.
- It is characterized by germline mutations in the EXT1 or EXT2 genes.
- It carries a significant risk (approximately 5%) of malignant transformation.
- The radiolucent nidus must typically exceed 2 cm in diameter to cause pain.
- The classic night pain is mediated by histamine release from mast cells within the nidus.
Correct Answer: It produces high local levels of prostaglandins, particularly PGE2.
Explanation:
Osteoid osteoma is a benign bone-forming tumor characterized by a radiolucent nidus usually less than 1.5-2 cm in diameter. The cells within the nidus produce very high levels of prostaglandins, particularly PGE2. This causes profound local vasodilation and severe pain, explaining the classic symptom of night pain that is rapidly and dramatically relieved by NSAIDs or aspirin.
Question 18:
During secondary fracture healing in a long bone, the repair process transitions through several highly coordinated phases. Which type of collagen is predominantly synthesized during the soft callus phase, and which cell type is primarily responsible for its production?
Options:
- Type I collagen; osteoblasts
- Type II collagen; chondrocytes
- Type III collagen; fibroblasts
- Type X collagen; hypertrophic chondrocytes
- Type I collagen; chondroblasts
Correct Answer: Type II collagen; chondrocytes
Explanation:
Secondary fracture healing involves endochondral ossification. During the soft callus phase, the hematoma is replaced by fibrocartilage, predominantly composed of Type II collagen synthesized by proliferating chondrocytes. This cartilaginous template is later calcified (involving Type X collagen) and finally replaced by woven bone (Type I collagen produced by osteoblasts) during the hard callus phase.
Question 19:
A 28-year-old male undergoes reamed intramedullary nailing for a closed, high-energy midshaft tibia fracture. In the PACU, he develops severe, unrelenting leg pain out of proportion to the injury, exacerbated by passive stretch of the hallux. Intracompartmental pressures confirm compartment syndrome. If a four-compartment fasciotomy is performed via a standard two-incision technique, the lateral incision provides direct access to which compartments?
Options:
- Anterior and deep posterior
- Anterior and lateral
- Lateral and superficial posterior
- Superficial posterior and deep posterior
- Anterior and superficial posterior
Correct Answer: Anterior and lateral
Explanation:
The standard two-incision technique for lower leg fasciotomy involves an anterolateral incision and a posteromedial incision. The anterolateral incision is placed between the tibial crest and the fibula, providing access to release the anterior and lateral compartments. The posteromedial incision allows for release of the superficial and deep posterior compartments.
Question 20:
A 16-year-old female athlete experiences her first acute lateral patellar dislocation. Physical exam reveals a positive J-sign and severe apprehension. MRI demonstrates a complete mid-substance tear of the medial patellofemoral ligament (MPFL). If reconstruction is planned, the surgeon must identify the precise femoral attachment of the MPFL. Where is this anatomic landmark located?
Options:
- Anterior and proximal to the medial femoral epicondyle
- Posterior and proximal to the medial femoral epicondyle
- Distal to the medial femoral epicondyle, near the joint line
- Directly at the apex of the adductor tubercle
- In a saddle-shaped depression between the medial epicondyle and adductor tubercle
Correct Answer: In a saddle-shaped depression between the medial epicondyle and adductor tubercle
Explanation:
The femoral origin of the medial patellofemoral ligament (MPFL) is a critical landmark for anatomic reconstruction (often referenced radiographically as Schöttle's point). Anatomically, it is located in a saddle-shaped depression between the medial epicondyle (distal/anterior) and the adductor tubercle (proximal/posterior).
Question 21:
A 45-year-old cyclist presents with numbness in his small and ring fingers, and weakness of finger abduction. Sensation to the dorsal ulnar aspect of the hand is preserved. At which zone of Guyon's canal is the compression most likely located, and what structures are involved?
Options:
- Zone 1; motor and sensory branches
- Zone 2; motor branch only
- Zone 3; sensory branch only
- Zone 1; motor branch only
- Cubital tunnel; motor and sensory branches
Correct Answer: Zone 1; motor and sensory branches
Explanation:
Preservation of dorsal ulnar sensation indicates the compression is distal to the dorsal ulnar sensory branch (which arises proximal to the wrist), localizing the lesion to Guyon's canal. Guyon's canal is divided into three zones: Zone 1 is proximal to the bifurcation and contains both motor and sensory fibers; Zone 2 contains only the deep motor branch; Zone 3 contains only the superficial sensory branch. Mixed motor and sensory deficits localize to Zone 1.
Question 22:
Bone Morphogenetic Proteins (BMPs) initiate intracellular signaling through which of the following receptor types?
Options:
- Tyrosine kinase receptors
- Serine/threonine kinase receptors
- G-protein coupled receptors
- Intracellular nuclear receptors
- Ion channel-linked receptors
Correct Answer: Serine/threonine kinase receptors
Explanation:
BMPs are members of the TGF-beta superfamily. They initiate intracellular signaling cascades by binding to specific Type I and Type II transmembrane serine/threonine kinase receptors, which leads to the phosphorylation and activation of intracellular Smad proteins.
Question 23:
A 32-year-old female presents with a distal femur lytic lesion that is diagnosed as a Giant Cell Tumor of Bone. She is started on Denosumab prior to surgery to help downstage the tumor. What is the mechanism of action of this medication?
Options:
- Direct cytotoxicity to neoplastic osteoblasts
- Monoclonal antibody against RANKL, inhibiting osteoclast formation
- Bisphosphonate that inhibits farnesyl pyrophosphate synthase
- VEGF inhibitor blocking tumor angiogenesis
- Monoclonal antibody against the RANK receptor directly
Correct Answer: Monoclonal antibody against RANKL, inhibiting osteoclast formation
Explanation:
Denosumab is a fully human monoclonal antibody that binds to RANKL (Receptor Activator of Nuclear factor Kappa-B Ligand). By binding RANKL, it prevents it from interacting with the RANK receptor on osteoclasts and osteoclast precursors, thereby profoundly inhibiting osteoclast formation, function, and survival.
Question 24:
A 6-week-old infant is being treated with a Pavlik harness for developmental dysplasia of the hip. At the 2-week follow-up, the mother notes the child is no longer actively extending the knee on the treated side. What is the most likely cause, and what is the appropriate management?
Options:
- Obturator nerve palsy; continue harness
- Femoral nerve palsy; temporarily discontinue the harness
- Sciatic nerve palsy; adjust the posterior strap
- Femoral nerve palsy; adjust the anterior strap to increase flexion
- Dislocated hip; proceed to closed reduction
Correct Answer: Femoral nerve palsy; temporarily discontinue the harness
Explanation:
Hyperflexion in a Pavlik harness can lead to femoral nerve palsy, presenting as decreased active knee extension. The standard initial management for a clinically evident femoral nerve palsy in this setting is to temporarily remove the harness to allow for neurologic recovery, rather than continuing or tightening the straps.
Question 25:
Trunnionosis in total hip arthroplasty is a phenomenon of mechanically assisted crevice corrosion. It is historically most strongly associated with which of the following combinations of head and stem materials?
Options:
- Cobalt-chrome head on titanium stem
- Ceramic head on titanium stem
- Ceramic head on cobalt-chrome stem
- Oxidized zirconium head on titanium stem
- Cobalt-chrome head on cobalt-chrome stem
Correct Answer: Cobalt-chrome head on titanium stem
Explanation:
Trunnionosis, or mechanically assisted crevice corrosion at the modular head-neck junction, has been most commonly observed in combinations utilizing a large cobalt-chrome (CoCr) femoral head on a titanium alloy stem due to galvanic and fretting corrosion mechanics.
Question 26:
Which of the following best describes the functional anatomy and biomechanics of the posterior cruciate ligament (PCL)?
Options:
- The anterolateral bundle is tight in flexion and lax in extension
- The anterolateral bundle is tight in extension and lax in flexion
- The posteromedial bundle is tight in flexion and lax in extension
- The meniscofemoral ligaments are present in less than 20% of knees
- It is the primary restraint to anterior tibial translation
Correct Answer: The anterolateral bundle is tight in flexion and lax in extension
Explanation:
The PCL consists of two main bundles: the anterolateral (AL) bundle and the posteromedial (PM) bundle. The AL bundle is the larger of the two and is tight in flexion and lax in extension. Conversely, the smaller PM bundle is tight in extension and lax in flexion.
Question 27:
The strongest and most important ligamentous stabilizer of the distal tibiofibular syndesmosis is the:
Options:
- Anterior inferior tibiofibular ligament (AITFL)
- Posterior inferior tibiofibular ligament (PITFL)
- Interosseous ligament
- Deltoid ligament
- Transverse tibiofibular ligament
Correct Answer: Posterior inferior tibiofibular ligament (PITFL)
Explanation:
While the anterior inferior tibiofibular ligament (AITFL) is typically the first to tear in a syndesmotic injury, biomechanical studies demonstrate that the posterior inferior tibiofibular ligament (PITFL) provides the greatest proportion of strength (approximately 42%) to the syndesmosis, making it the strongest stabilizer.
Question 28:
In a hemodynamically unstable patient with an anteroposterior compression (APC) type III pelvic ring injury, what is the anatomical target for the optimal placement of a circumferential pelvic sheet or binder?
Options:
- Iliac crests
- Anterior superior iliac spines
- Greater trochanters
- Mid-femur
- Level of the umbilicus
Correct Answer: Greater trochanters
Explanation:
Optimal placement of a pelvic binder is centered directly over the greater trochanters. Placing the binder too high (e.g., iliac crests or ASIS) reduces its biomechanical efficacy in closing the pelvic volume and can paradoxically open the true pelvis further.
Question 29:
A 14-year-old gymnast presents with chronic low back pain exacerbated by extension. Radiographs show a grade II isthmic spondylolisthesis at L5-S1. What is the most common neurological finding associated with this condition if radiculopathy is present?
Options:
- Weakness in ankle dorsiflexion
- Decreased patellar reflex
- Weakness in ankle plantar flexion
- Numbness in the medial aspect of the lower leg
- Radicular pain in the L5 distribution
Correct Answer: Radicular pain in the L5 distribution
Explanation:
In L5-S1 isthmic spondylolisthesis, the exiting L5 nerve root is most commonly compressed within the neural foramen by fibrocartilaginous tissue of the pars defect, resulting in L5 radiculopathy (pain, weakness in EHL, and sensory changes in the first dorsal web space).
Question 30:
A 45-year-old man presents with wrist pain 10 years after an untreated scaphoid fracture. Radiographs show arthritis involving the entire radioscaphoid joint, but the capitolunate joint is completely preserved. What stage of Scaphoid Nonunion Advanced Collapse (SNAC) is this, and what is a recommended salvage procedure?
Options:
- SNAC Stage I; Radial styloidectomy and scaphoid fixation
- SNAC Stage II; Proximal row carpectomy or four-corner fusion
- SNAC Stage III; Total wrist arthrodesis
- SNAC Stage I; Proximal row carpectomy
- SNAC Stage II; Total wrist arthroplasty
Correct Answer: SNAC Stage II; Proximal row carpectomy or four-corner fusion
Explanation:
SNAC staging: Stage I involves the radial styloid and distal scaphoid. Stage II involves the entire radioscaphoid fossa. Stage III involves the capitolunate (midcarpal) joint. Because the entire radioscaphoid joint is arthritic but midcarpal is spared, this is Stage II. Proximal row carpectomy (PRC) or four-corner fusion are standard recommended treatments.
Question 31:
In Legg-Calvé-Perthes disease, which of the following is considered a 'head-at-risk' radiographic sign of Catterall?
Options:
- Medial subluxation of the femoral head
- Vertical physis
- Gage's sign
- Acetabular dysplasia
- Premature closure of the triradiate cartilage
Correct Answer: Gage's sign
Explanation:
Catterall's 'head-at-risk' signs include: Gage's sign (a V-shaped radiolucency in the lateral portion of the epiphysis/metaphysis), calcification lateral to the epiphysis, lateral subluxation of the femoral head, a horizontal physis, and metaphyseal cysts.
Question 32:
During a posterior-stabilized total knee arthroplasty utilizing an anterior referencing guide, the surgeon notes that the knee is tight in flexion and well-balanced in extension. Which of the following is the most appropriate intraoperative step to balance the knee?
Options:
- Recut the distal femur to remove more bone
- Decrease the size of the femoral component
- Decrease the posterior slope of the tibial cut
- Recut the proximal tibia to remove more bone
- Release the posterior cruciate ligament
Correct Answer: Decrease the size of the femoral component
Explanation:
A knee that is tight in flexion but balanced in extension requires a maneuver that exclusively increases the flexion gap. When using an anterior referencing system, decreasing the femoral component size selectively decreases the posterior condylar offset (thinner posterior cut), which enlarges the flexion space without altering the extension space.
Question 33:
In normal articular cartilage, the superficial (tangential) zone is functionally and structurally characterized by which of the following properties?
Options:
- Highest concentration of proteoglycans
- Collagen fibers oriented perpendicular to the joint surface
- Highest concentration of water and collagen fibers oriented parallel to the joint surface
- Chondrocytes arranged in columns
- Highest compressive strength
Correct Answer: Highest concentration of water and collagen fibers oriented parallel to the joint surface
Explanation:
The superficial zone of articular cartilage is characterized by the highest water content, lowest proteoglycan content, and densely packed collagen fibers that are oriented parallel to the joint surface to resist sheer stress.
Question 34:
Which of the following injury patterns classically defines a 'floating shoulder'?
Options:
- Clavicle shaft fracture and acromioclavicular joint separation
- Scapular body fracture and sternoclavicular dislocation
- Humeral head fracture and glenoid fracture
- Glenoid neck fracture and ipsilateral clavicle shaft fracture
- Coracoid base fracture and acromion fracture
Correct Answer: Glenoid neck fracture and ipsilateral clavicle shaft fracture
Explanation:
A 'floating shoulder' refers to a double disruption of the superior shoulder suspensory complex, most classically represented by an ipsilateral fracture of the glenoid neck and a fracture of the clavicle shaft, thereby functionally isolating the glenohumeral joint from the axial skeleton.
Question 35:
A 65-year-old male undergoes arthroscopic rotator cuff repair and is noted to have a highly degenerate long head of the biceps tendon. A biceps tenotomy is performed. Compared to biceps tenodesis, simple tenotomy is associated with a statistically higher rate of:
Options:
- Postoperative stiffness
- Cosmetic deformity (Popeye sign)
- Deep infection
- Chronic regional pain syndrome
- Need for revision surgery
Correct Answer: Cosmetic deformity (Popeye sign)
Explanation:
While both biceps tenotomy and tenodesis yield similarly good outcomes regarding pain relief and function, simple tenotomy has a significantly higher rate of cosmetic deformity (the 'Popeye' muscle bulge) and occasional cramping, compared to tenodesis.
Question 36:
In the evaluation of a suspected Lisfranc injury, which radiographic finding on a weight-bearing AP view of the foot is considered a primary indicator of disruption?
Options:
- Medial displacement of the second metatarsal base relative to the middle cuneiform
- Malalignment of the medial border of the second metatarsal with the medial border of the middle cuneiform
- Widening of the 1st and 2nd intermetatarsal space greater than 2 mm
- Plantar gapping at the tarsometatarsal joint on the lateral view
- Avulsion fracture of the navicular tuberosity
Correct Answer: Malalignment of the medial border of the second metatarsal with the medial border of the middle cuneiform
Explanation:
A classic and pathognomonic finding of a Lisfranc injury on an AP radiograph is any step-off or malalignment of the medial border of the second metatarsal base with the medial border of the middle cuneiform. They should form a perfectly continuous line in a normal foot.
Question 37:
A 16-year-old male presents with severe nocturnal thigh pain that is rapidly relieved by NSAIDs. Radiographs demonstrate a small radiolucent nidus surrounded by dense sclerotic reactive bone in the proximal femur. After failing medical management, which of the following is the most appropriate initial definitive treatment?
Options:
- Open intralesional curettage and bone grafting
- En bloc wide resection
- Radiofrequency ablation (RFA)
- External beam radiation therapy
- Observation with serial radiographs
Correct Answer: Radiofrequency ablation (RFA)
Explanation:
The classic presentation of an osteoid osteoma is night pain relieved by NSAIDs, characterized radiographically by a radiolucent nidus with surrounding sclerosis. Radiofrequency ablation (RFA) is the standard of care for definitive minimally invasive treatment when medical management fails.
Question 38:
The Stener lesion, which prevents non-operative healing of a complete ulnar collateral ligament (UCL) tear of the thumb, involves the interposition of which structure between the torn ends of the UCL?
Options:
- Abductor pollicis brevis aponeurosis
- Adductor pollicis aponeurosis
- Extensor pollicis longus tendon
- Flexor pollicis longus tendon
- Volar plate
Correct Answer: Adductor pollicis aponeurosis
Explanation:
A Stener lesion occurs when the distal attachment of the thumb ulnar collateral ligament (UCL) completely avulses and retracts proximally, becoming displaced superficial to the adductor pollicis aponeurosis. This aponeurosis interposes between the torn UCL ends, preventing native healing and necessitating surgical repair.
Question 39:
A 22-year-old restrained passenger is involved in a high-speed motor vehicle collision. CT of the lumbar spine reveals a flexion-distraction injury (Chance fracture) at L2. Which of the following associated injuries has the highest incidence in this patient population?
Options:
- Aortic transection
- Intra-abdominal visceral injury
- Spinal cord complete transection
- Renal artery thrombosis
- Pelvic ring disruption
Correct Answer: Intra-abdominal visceral injury
Explanation:
Chance fractures (flexion-distraction injuries of the spine) are highly associated with lap-belt use in motor vehicle accidents. They carry a very high rate (up to 40-50%) of concomitant intra-abdominal visceral injuries, particularly to hollow viscous organs like the small bowel.
Question 40:
Tranexamic acid (TXA) is widely used in orthopedic surgery to reduce perioperative blood loss. What is its primary biochemical mechanism of action?
Options:
- Activates the extrinsic coagulation cascade via Factor VII
- Promotes platelet aggregation by binding to von Willebrand factor
- Directly inhibits Factor Xa
- Inhibits the breakdown of fibrin by competitively blocking plasminogen activation
- Enhances the activity of antithrombin III
Correct Answer: Inhibits the breakdown of fibrin by competitively blocking plasminogen activation
Explanation:
Tranexamic acid (TXA) is a synthetic analog of the amino acid lysine. It acts as an antifibrinolytic agent by reversibly binding four to five lysine receptor sites on plasminogen, which prevents plasmin from binding to and degrading fibrin, thereby stabilizing the blood clot.