Full Question & Answer Text (for Search Engines)
Question 1:
During an anterior intrapelvic (modified Stoppa) approach for the fixation of an acetabular fracture, the surgeon encounters significant bleeding from a vascular anastomosis situated over the superior pubic ramus. What two main vessels typically form this specific anastomosis (Corona Mortis)?
Options:
- Obturator artery and internal iliac artery
- Superior gluteal artery and external iliac artery
- Inferior epigastric artery and obturator artery
- Internal pudendal artery and inferior gluteal artery
- External pudendal artery and medial circumflex femoral artery
Correct Answer: Inferior epigastric artery and obturator artery
Explanation:
The corona mortis ('crown of death') is a vascular anastomosis between the external iliac and internal iliac vascular systems. Specifically, it connects the inferior epigastric artery or vein (from the external iliac system) to the obturator artery or vein (from the internal iliac system). It is located on the posterior aspect of the superior pubic ramus, approximately 4-7 cm from the pubic symphysis, and is at high risk of iatrogenic injury during the modified Stoppa or ilioinguinal approaches.
Question 2:
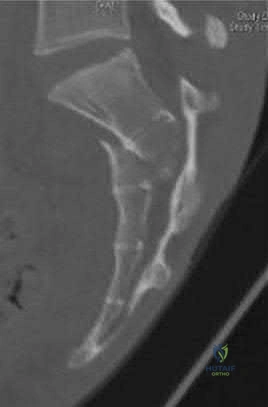
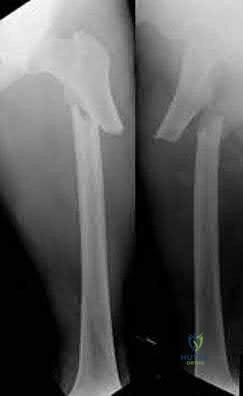
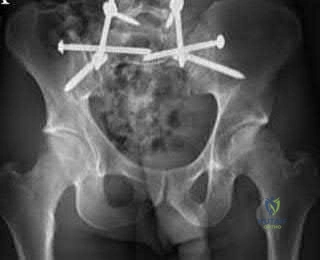
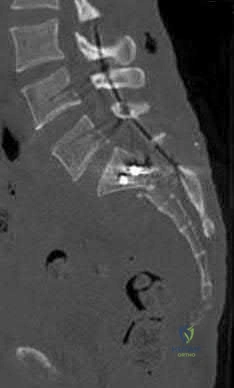
A 12-year-old boy presents with left thigh pain, an antalgic gait, and an externally rotated left lower extremity. Radiographs demonstrate the pathology shown. Which of the following is considered an absolute indication for prophylactic pinning of the asymptomatic, contralateral hip in a patient presenting with Slipped Capital Femoral Epiphysis (SCFE)?
Options:
- Obesity (BMI > 95th percentile)
- Male gender
- Underlying endocrine disorder (e.g., hypothyroidism)
- Age greater than 14 years at presentation
- Black race
Correct Answer: Underlying endocrine disorder (e.g., hypothyroidism)
Explanation:
SCFE is characterized by a displacement of the proximal femoral epiphysis. Prophylactic pinning of the contralateral hip is somewhat controversial but generally recommended in patients with a high risk of subsequent contralateral slip. Absolute indications or highly strong recommendations for prophylactic contralateral pinning include an underlying endocrine disorder (such as hypothyroidism or growth hormone deficiency), renal osteodystrophy, previous radiation therapy, and presentation at a very young age (e.g., < 10 years). Endocrine disorders dramatically increase the risk of bilateral involvement, often occurring simultaneously or sequentially.
Question 3:
A 55-year-old male undergoes excision of a large cartilaginous tumor of the proximal femur. Molecular analysis of the tumor reveals a mutation in the isocitrate dehydrogenase 1 (IDH1) gene. This mutation is a hallmark of and most frequently associated with which of the following conditions?
Options:
- Ollier disease
- Multiple Hereditary Exostoses
- Neurofibromatosis type 1
- Familial Adenomatous Polyposis
- McCune-Albright syndrome
Correct Answer: Ollier disease
Explanation:
Mutations in the IDH1 and IDH2 genes are heavily implicated in the pathogenesis of cartilaginous tumors. Somatic mosaic mutations in these genes are found in over 80% of patients with Ollier disease and Maffucci syndrome, both of which are forms of enchondromatosis. Multiple Hereditary Exostoses is associated with EXT1/EXT2 mutations. McCune-Albright is associated with GNAS mutations. NF1 is associated with the neurofibromin gene.
Question 4:
A 28-year-old sustains a laceration to the volar aspect of the digit in Zone II, requiring surgical exploration and flexor tendon repair. To prevent tendon bowstringing and maximize biomechanical excursion efficiency, which two annular pulleys are the most critical to preserve or reconstruct?
Options:
- A1 and A3
- A2 and A4
- A3 and A5
- A1 and A5
- A2 and A3
Correct Answer: A2 and A4
Explanation:
The flexor tendon sheath mechanism comprises five annular (A1-A5) and three cruciform (C1-C3) pulleys. The A2 and A4 pulleys are the major pulleys responsible for preventing bowstringing of the flexor tendons. The A2 pulley arises from the proximal phalanx, and the A4 arises from the middle phalanx. Biomechanical studies have shown that preserving or reconstructing A2 and A4 is critical to maintaining normal digital kinematics and work of flexion.
Question 5:
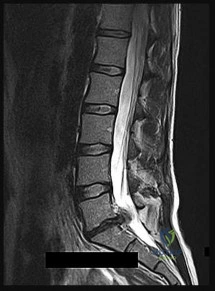
A 32-year-old male is involved in a high-speed motor vehicle collision and arrives with a unilateral C6-C7 facet dislocation and a dense C6 radiculopathy. Closed reduction with cranial tongs is attempted in the awake patient but is unsuccessful. What is the most appropriate next step in management?
Options:
- Perform immediate posterior open reduction without further imaging
- Discharge the patient with a halo-vest orthosis for non-operative management
- Obtain an urgent MRI of the cervical spine followed by surgical intervention
- Perform an immediate anterior cervical discectomy and fusion (ACDF)
- Re-attempt closed reduction under general anesthesia
Correct Answer: Obtain an urgent MRI of the cervical spine followed by surgical intervention
Explanation:
In cases of cervical facet dislocation where awake closed reduction fails, or in a patient who cannot be examined (e.g., obtunded), an MRI of the cervical spine is the standard of care before proceeding to open reduction. The MRI is essential to identify the presence of a herniated intervertebral disc. If an anterior disc herniation is present, a posterior-only open reduction poses a significant risk of extruding the disc further into the spinal canal, potentially causing a catastrophic spinal cord injury. Therefore, MRI dictates whether an anterior approach (to remove the disc before reduction) is required.
Question 6:
During a primary posterior-stabilized total knee arthroplasty, the surgeon assesses the flexion and extension gaps. The knee is found to be tight in both extension and flexion. Which of the following surgical adjustments is the most appropriate next step?
Options:
- Resect more distal femur
- Resect more proximal tibia
- Upsize the femoral component
- Downsize the femoral component
- Release the posterior cruciate ligament
Correct Answer: Resect more proximal tibia
Explanation:
In gap balancing for total knee arthroplasty, the proximal tibial cut affects both the flexion and extension gaps equally. If the knee is symmetrically tight in both flexion and extension, resecting more proximal tibia (or using a thinner tibial polyethylene insert) will increase both gaps equally. Resecting more distal femur would only loosen the extension gap. Changing the femoral size primarily affects the flexion gap (downsizing loosens flexion; upsizing tightens flexion).
Question 7:
A 45-year-old trauma patient sustains an intra-articular distal femur fracture. Advanced imaging identifies a coronal plane fracture of the lateral femoral condyle (Hoffa fragment). Biomechanical studies suggest which of the following screw orientations provides the most rigid fixation for this specific fracture pattern?
Options:
- Medial to lateral lag screws
- Posteroanterior oriented lag screws
- Anteroposterior oriented lag screws
- Distal to proximal lag screws
- Lateral to medial lag screws
Correct Answer: Posteroanterior oriented lag screws
Explanation:
A Hoffa fracture is a coronal plane fracture of the femoral condyle, more commonly affecting the lateral condyle. Biomechanical studies have demonstrated that posteroanterior (PA) directed lag screws provide superior stability and higher load to failure compared to anteroposterior (AP) directed screws. While AP screws are often used clinically due to ease of placement via an anterior approach, PA screws are biomechanically advantageous because they enter through thicker cortical bone posteriorly and are directed perpendicular to the fracture plane.
Question 8:
Romosozumab is a monoclonal antibody utilized in the treatment of severe osteoporosis. It functions by inhibiting sclerostin, thereby promoting bone formation. Sclerostin normally inhibits osteoblastogenesis by antagonizing which of the following signaling pathways?
Options:
- RANK/RANKL pathway
- Wnt/beta-catenin pathway via LRP5/6 receptors
- Transforming Growth Factor-beta (TGF-b) pathway
- Bone Morphogenetic Protein-2 (BMP-2) pathway
- Fibroblast Growth Factor (FGF) pathway
Correct Answer: Wnt/beta-catenin pathway via LRP5/6 receptors
Explanation:
Sclerostin is a glycoprotein secreted primarily by osteocytes. It acts as a negative regulator of bone formation by binding to the LRP5/6 coreceptors on osteoblasts, thereby inhibiting the canonical Wnt/beta-catenin signaling pathway. By blocking sclerostin, medications like romosozumab allow Wnt signaling to proceed, leading to increased osteoblast activity and bone formation.
Question 9:
A 24-year-old professional football player sustains a high-energy axial load injury to a plantarflexed foot. Radiographs demonstrate widening of the midfoot spaces. The critical interosseous Lisfranc ligament connects which of the following two osseous structures?
Options:
- Medial cuneiform to the base of the first metatarsal
- Medial cuneiform to the base of the second metatarsal
- Intermediate cuneiform to the base of the second metatarsal
- Lateral cuneiform to the cuboid
- Navicular to the medial cuneiform
Correct Answer: Medial cuneiform to the base of the second metatarsal
Explanation:
The Lisfranc ligament is a strong interosseous ligament critical for the stability of the tarsometatarsal joint complex. It originates from the lateral aspect of the medial cuneiform and inserts onto the medial aspect of the base of the second metatarsal. There is no direct ligamentous connection between the bases of the first and second metatarsals, making the Lisfranc ligament the primary restraint to lateral displacement of the lesser metatarsals.
Question 10:
During an anterior cruciate ligament (ACL) reconstruction, improper tunnel placement can lead to graft failure or loss of motion. If the femoral tunnel is placed too far anteriorly (shallow) in the intercondylar notch, which of the following graft tension patterns will result?
Options:
- Tight in extension and tight in flexion
- Tight in flexion and lax in extension
- Lax in flexion and tight in extension
- Lax in both extension and flexion
- Isotropic tension throughout the entire range of motion
Correct Answer: Tight in flexion and lax in extension
Explanation:
Proper femoral tunnel placement is critical for ACL graft isometry. If the femoral tunnel is placed too far anteriorly (shallow, moving away from the anatomic footprint towards the anterior cortex), the distance between the femoral and tibial attachments increases as the knee flexes. This results in the graft being overly tight in flexion (often restricting flexion or leading to graft stretch/failure) and lax in extension. Conversely, placement too far posteriorly leads to a graft that is tight in extension and lax in flexion.
Question 11:
A 6-week-old female infant is treated with a Pavlik harness for Developmental Dysplasia of the Hip (DDH). At the second weekly follow-up, the parents report the infant is no longer moving her right lower extremity. Clinical examination reveals an absence of active knee extension on the right. What is the most likely iatrogenic cause of this finding?
Options:
- Avascular necrosis of the femoral head
- Femoral nerve palsy due to excessive hyperflexion
- Obturator nerve palsy due to excessive abduction
- Sciatic nerve palsy due to hyperflexion
- Common peroneal nerve palsy from the posterior foot strap
Correct Answer: Femoral nerve palsy due to excessive hyperflexion
Explanation:
Femoral nerve palsy is the most common nerve palsy associated with Pavlik harness treatment and is typically caused by excessive flexion of the hips. Hyperflexion compresses the femoral nerve against the inguinal ligament, leading to decreased quadriceps function (loss of active knee extension). The treatment is to temporarily adjust or remove the harness; the palsy typically resolves spontaneously within days to weeks.
Question 12:
When executing a posteromedial approach to the knee for open reduction and internal fixation of a posteromedial tibial plateau fracture, the surgeon must develop a plane. The optimal inter-nervous/inter-muscular interval is primarily developed by retracting the medial head of the gastrocnemius laterally and which structure medially?
Options:
- Semimembranosus
- Popliteus
- Soleus
- Tibialis posterior
- Pes anserinus
Correct Answer: Pes anserinus
Explanation:
The posteromedial approach to the tibial plateau typically utilizes the interval between the medial head of the gastrocnemius (which is retracted laterally, protecting the neurovascular bundle in the popliteal fossa) and the pes anserinus (sartorius, gracilis, semitendinosus), which is retracted medially/anteriorly. The semimembranosus can also be retracted medially. The pes anserinus forms the medial boundary of this superficial dissection window.
Question 13:
A 14-year-old patient with high-grade conventional osteosarcoma is undergoing a neo-adjuvant chemotherapy regimen (MAP: Methotrexate, Doxorubicin, Cisplatin). Which of the following is the most significant, dose-limiting toxicity specific to Doxorubicin?
Options:
- Nephrotoxicity
- Ototoxicity
- Cardiomyopathy
- Peripheral neuropathy
- Hemorrhagic cystitis
Correct Answer: Cardiomyopathy
Explanation:
Doxorubicin (Adriamycin) is an anthracycline whose primary, irreversible dose-limiting toxicity is dilated cardiomyopathy, which is dependent on the cumulative lifetime dose. A baseline echocardiogram is mandatory before administration. Cisplatin is known for ototoxicity and nephrotoxicity. High-dose methotrexate requires leucovorin rescue and can cause mucositis, hepatotoxicity, and renal toxicity.
Question 14:
A 68-year-old male presents with new-onset groin pain 6 years after a total hip arthroplasty using a dual-taper modular femoral stem with a cobalt-chromium head and highly cross-linked polyethylene liner. Serum cobalt levels are significantly elevated out of proportion to chromium. Aspirational fluid demonstrates a high macrophage count with black, metallic particulate debris but no organisms. What is the primary mechanism of failure?
Options:
- Polyethylene wear-induced osteolysis
- Mechanically assisted crevice corrosion (Trunnionosis)
- Aseptic loosening of the femoral stem secondary to stress shielding
- Unrecognized periprosthetic joint infection
- Metallosis due to recurrent component impingement
Correct Answer: Mechanically assisted crevice corrosion (Trunnionosis)
Explanation:
The patient's presentation describes an adverse local tissue reaction (ALTR) secondary to trunnionosis. Trunnionosis (mechanically assisted crevice corrosion or MACC) occurs at the modular head-neck junction (trunnion). It is characterized by elevated serum cobalt levels (often disproportionately higher than chromium) and a characteristic local inflammatory response to the fretting and corrosion of the metallic debris. The absence of an alternative metal-on-metal articulation rules out classic bearing-surface metallosis.
Question 15:
During a carpal tunnel release, the surgeon must be meticulously aware of the anatomical variations of the recurrent motor branch of the median nerve. According to the Lanz classification, what is the most common anatomical course of the recurrent motor branch?
Options:
- Extraligamentous with a recurrent course
- Subligamentous with a recurrent course
- Transligamentous through the transverse carpal ligament
- Ulnar branching from the main median nerve trunk
- Branching proximal to the carpal tunnel
Correct Answer: Extraligamentous with a recurrent course
Explanation:
The Lanz classification describes the anatomical variations of the recurrent motor branch of the median nerve. The most common configuration (Lanz Group I, occurring in ~46-90% of individuals depending on the series) is an extraligamentous branch that arises from the radial side of the median nerve just distal to the transverse carpal ligament and then takes a recurrent course to innervate the thenar musculature. The transligamentous course is a well-known variation that places the nerve at high risk during transverse carpal ligament release.
Question 16:
A 70-year-old male complains of bilateral lower extremity pain and cramping when walking a distance of two blocks. Which of the following clinical features most strongly distinguishes neurogenic claudication (due to lumbar spinal stenosis) from vascular claudication?
Options:
- Pain relief when standing completely stationary
- Palliative effect of walking uphill compared to walking downhill
- Diminished pedal pulses and shiny skin
- Exacerbation of pain with spinal flexion
- Distal to proximal progression of symptoms
Correct Answer: Palliative effect of walking uphill compared to walking downhill
Explanation:
Neurogenic claudication, characteristic of lumbar spinal stenosis, is typically relieved by lumbar flexion (which increases the cross-sectional area of the spinal canal and neural foramina). Therefore, patients often experience relief when sitting, leaning on a shopping cart, or walking uphill (which necessitates a flexed posture). Conversely, vascular claudication is strictly tied to the metabolic demand of the muscles; patients have pain with walking any incline (uphill worsens vascular demand) and find relief simply by standing still. Neurogenic claudication is typically aggravated by standing still in extension.
Question 17:
Articular cartilage is a highly specialized connective tissue. The primary structural proteoglycan of articular cartilage is aggrecan. Which of the following is the most abundant glycosaminoglycan (GAG) attached to the aggrecan core protein?
Options:
- Type I collagen
- Chondroitin sulfate
- Fibronectin
- Elastin
- Hydroxyapatite
Correct Answer: Chondroitin sulfate
Explanation:
Aggrecan is the major proteoglycan in articular cartilage and provides the osmotic properties necessary to resist compressive loads. It consists of a core protein with numerous covalently attached glycosaminoglycan (GAG) side chains. The two primary GAGs on aggrecan are chondroitin sulfate and keratan sulfate, with chondroitin sulfate being the most abundant. Type I collagen is primarily found in bone and tendon; articular cartilage is predominantly Type II collagen.
Question 18:
A 35-year-old farmer sustains an open midshaft tibia fracture when a tractor rolls over his leg. The wound is 12 cm long with significant contamination, including soil and manure. According to standard orthopedic trauma guidelines, what is the most appropriate prophylactic intravenous antibiotic regimen?
Options:
- First-generation cephalosporin alone
- First-generation cephalosporin and an aminoglycoside
- First-generation cephalosporin, an aminoglycoside, and high-dose penicillin
- Fluoroquinolone alone
- Third-generation cephalosporin alone
Correct Answer: First-generation cephalosporin, an aminoglycoside, and high-dose penicillin
Explanation:
This is a Gustilo-Anderson Type III open fracture occurring in a farming environment. The standard antibiotic protocol for a Type III open fracture includes a first-generation cephalosporin (for Gram-positive coverage) and an aminoglycoside (for Gram-negative coverage). However, when the wound is heavily contaminated with soil, manure, or standing water (e.g., farm injuries), the addition of high-dose penicillin is indicated to provide coverage against anaerobic organisms, particularly Clostridium species, to prevent gas gangrene.
Question 19:
In the surgical management of recurrent anterior shoulder instability, a 'remplissage' procedure is occasionally performed as an adjunct to arthroscopic Bankart repair. The remplissage procedure addresses a large Hill-Sachs lesion by tenodesing which of the following structures into the defect?
Options:
- Subscapularis
- Long head of the biceps brachii
- Infraspinatus
- Teres minor
- Supraspinatus
Correct Answer: Infraspinatus
Explanation:
The term 'remplissage' translates to 'filling' in French. It is an arthroscopic procedure used to treat engaging or off-track Hill-Sachs lesions (posterosuperior humeral head impaction fractures). It involves the capsulotenodesis of the posterior capsule and the infraspinatus tendon into the humeral head defect, thereby converting an intra-articular defect into an extra-articular one and preventing it from engaging the anterior glenoid rim during abduction and external rotation.
Question 20:
A 58-year-old male with long-standing, poorly controlled diabetes presents with a unilaterally swollen, warm, and erythematous foot without ulceration. Radiographs reveal osseous fragmentation, debris, and joint subluxation in the midfoot, but no significant sclerosis or osteophyte formation. According to the Eichenholtz classification of Charcot neuroarthropathy, what stage does this represent?
Options:
- Stage 0 (Prodromal)
- Stage 1 (Development/Fragmentation)
- Stage 2 (Coalescence)
- Stage 3 (Reconstruction/Consolidation)
- Stage 4 (Late Deformity)
Correct Answer: Stage 1 (Development/Fragmentation)
Explanation:
The Eichenholtz classification describes the radiographic progression of Charcot neuroarthropathy. Stage 0 is clinically swollen and warm with normal radiographs. Stage 1 (Development/Fragmentation) features bony debris, fragmentation, joint subluxation/dislocation, and loss of joint space. Stage 2 (Coalescence) is marked by absorption of fine debris, early fusion of fragments, and sclerosis. Stage 3 (Reconstruction) shows consolidation of fractures, remodeling, and mature osteophyte formation.