Full Question & Answer Text (for Search Engines)
Question 1:
How does highly cross-linked ultra-high-molecular-weight polyethylene (UHMWPE) differ from conventional polyethylene in total joint arthroplasty?
Options:
- Increased wear resistance and decreased fracture toughness
- Increased wear resistance and increased yield strength
- Decreased wear resistance and increased ultimate tensile strength
- Decreased wear resistance and decreased fracture toughness
- Increased wear resistance with no change in mechanical properties
Correct Answer: Increased wear resistance and decreased fracture toughness
Explanation:
Highly cross-linked polyethylene is manufactured by exposing the material to radiation, which forms covalent bonds between the polymer chains. This process significantly decreases adhesive and abrasive wear. However, the cross-linking process and subsequent thermal treatment (melting or annealing) to extinguish free radicals also alter its mechanical properties, resulting in decreased yield strength, ultimate tensile strength, and fracture toughness.
Question 2:
A 12-year-old male with a BMI > 95th percentile presents with hip pain and is diagnosed with a Slipped Capital Femoral Epiphysis (SCFE). Which of the following is the strongest indication for prophylactic in situ pinning of the asymptomatic contralateral hip?
Options:
- Age greater than 14 years at presentation
- Presence of a moderate slip angle (30-50 degrees) on the affected side
- Underlying endocrinopathy, such as hypothyroidism
- Male sex and African American descent
- History of prior hip trauma
Correct Answer: Underlying endocrinopathy, such as hypothyroidism
Explanation:
Prophylactic pinning of the contralateral hip in SCFE is controversial but is strongly indicated in patients with underlying endocrinopathies (e.g., hypothyroidism, growth hormone deficiency) or renal osteodystrophy. These conditions dramatically increase the risk of bilateral involvement. Other indications include inability to follow up, radiation therapy, and open triradiate cartilage (though age and triradiate status are debated, endocrinopathy is universally agreed upon).
Question 3:
A 30-year-old male presents with a comminuted intra-articular fracture of the first metacarpal base. What are the primary deforming forces acting on the metacarpal shaft in this injury?
Options:
- Extensor pollicis longus and flexor pollicis longus
- Abductor pollicis longus and adductor pollicis
- Extensor pollicis brevis and abductor pollicis brevis
- Opponens pollicis and first dorsal interosseous
- Flexor pollicis brevis and adductor pollicis
Correct Answer: Abductor pollicis longus and adductor pollicis
Explanation:
In intra-articular fractures of the thumb metacarpal base (Bennett and Rolando fractures), the palmar ulnar fragment remains attached to the anterior oblique ligament (beak ligament). The metacarpal shaft is pulled proximally, dorsally, and radially by the abductor pollicis longus (APL), while the adductor pollicis (AP) pulls the metacarpal head into the palm, resulting in the classic supination and adduction deformity.
Question 4:
A 65-year-old female presents with neurogenic claudication. Radiographs demonstrate degenerative spondylolisthesis. What is the most common level of involvement and the corresponding nerve root most likely compressed in the lateral recess?
Options:
- L3-L4 level; L3 nerve root
- L3-L4 level; L4 nerve root
- L4-L5 level; L4 nerve root
- L4-L5 level; L5 nerve root
- L5-S1 level; L5 nerve root
Correct Answer: L4-L5 level; L5 nerve root
Explanation:
Degenerative spondylolisthesis most commonly occurs at the L4-L5 level. It is characterized by an intact pars interarticularis, facet hypertrophy, and ligamentum flavum buckling, leading to central and lateral recess stenosis. The L5 nerve root (traversing root) is most commonly compressed in the lateral recess at the L4-L5 level.
Question 5:
Which bundle of the posterior cruciate ligament (PCL) is the primary restraint to posterior tibial translation at 90 degrees of knee flexion?
Options:
- Posterolateral bundle
- Anteromedial bundle
- Anterolateral bundle
- Posteromedial bundle
- Meniscofemoral ligament of Wrisberg
Correct Answer: Anterolateral bundle
Explanation:
The PCL has two main bundles: the anterolateral (AL) and posterolateral (PL) bundles. The AL bundle is larger, tighter in flexion, and acts as the primary restraint to posterior tibial translation at 90 degrees of knee flexion. The PL bundle is tighter in extension. Reconstructing the AL bundle is the primary goal in single-bundle PCL reconstruction.
Question 6:
A 15-year-old male is diagnosed with high-grade osteosarcoma of the distal femur without evidence of metastatic disease. What is the single most important prognostic factor for his long-term survival?
Options:
- Histologic response to neoadjuvant chemotherapy
- Surgical margins achieved during resection
- Anatomic location of the tumor
- Serum alkaline phosphatase levels at presentation
- Subtype of osteosarcoma (e.g., osteoblastic vs. chondroblastic)
Correct Answer: Histologic response to neoadjuvant chemotherapy
Explanation:
In non-metastatic high-grade osteosarcoma, the extent of tumor necrosis following neoadjuvant chemotherapy is the single most important prognostic indicator. A good response is defined as >90% necrosis (Huvos grade III or IV) and correlates highly with increased overall and disease-free survival.
Question 7:
A 55-year-old active female who underwent a ceramic-on-ceramic total hip arthroplasty 2 years ago presents with a loud, audible squeaking during hip flexion. Which of the following is most strongly associated with this complication?
Options:
- Use of a larger diameter femoral head
- Femoral stem anteversion of 15 degrees
- Acetabular component retroversion and edge loading
- Failure to use a ceramic liner with a metal rim
- Post-operative heterotopic ossification
Correct Answer: Acetabular component retroversion and edge loading
Explanation:
Squeaking in ceramic-on-ceramic THA is a well-documented phenomenon. It is most strongly associated with component malposition—specifically, excessive acetabular cup abduction or retroversion, which leads to edge loading, stripe wear, and microseparation. Patient factors such as high BMI and younger, more active lifestyles also contribute.
Question 8:
A 22-year-old football player sustains a midfoot injury. To accurately assess the integrity of the Lisfranc complex, the surgeon must understand its anatomy. Which of the following accurately describes the attachments of the primary Lisfranc ligament?
Options:
- Medial cuneiform to the base of the first metatarsal
- Middle cuneiform to the base of the second metatarsal
- Lateral cuneiform to the base of the third metatarsal
- Medial cuneiform to the base of the second metatarsal
- Middle cuneiform to the base of the first metatarsal
Correct Answer: Medial cuneiform to the base of the second metatarsal
Explanation:
The Lisfranc ligament is an intra-articular interosseous ligament that connects the lateral aspect of the medial cuneiform to the medial aspect of the base of the second metatarsal. It is the strongest and most crucial ligament for the stability of the tarsometatarsal joint complex. There is notably no intermetatarsal ligament between the first and second metatarsal bases.
Question 9:
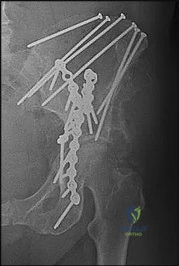
A 72-year-old female on prolonged bisphosphonate therapy presents with thigh pain. Radiographs show a fracture of the femoral shaft. Which of the following radiographic features is most characteristic of an atypical femur fracture associated with bisphosphonate use?
Options:
- Spiral fracture pattern with medial comminution
- Transverse or short oblique fracture line originating at the lateral cortex with localized periosteal thickening (beaking)
- High-energy comminuted fracture with extensive soft tissue damage
- Pathologic fracture through a geographic lytic lesion
- Subtrochanteric fracture with significant medial cortical thickening
Correct Answer: Transverse or short oblique fracture line originating at the lateral cortex with localized periosteal thickening (beaking)
Explanation:
Atypical femur fractures (AFFs) associated with prolonged bisphosphonate therapy have specific major criteria defined by the ASBMR. These include a location anywhere from just distal to the lesser trochanter to just proximal to the supracondylar flare, transverse or short oblique orientation, non-comminuted (or minimally comminuted), and originating at the lateral cortex with localized periosteal or endosteal thickening ('beaking').
Question 10:
A patient presents with numbness in the small and ring fingers. Which of the following clinical findings best differentiates ulnar nerve compression at the cubital tunnel from compression at Guyon's canal?
Options:
- Weakness of the adductor pollicis
- Decreased sensation over the dorsal ulnar aspect of the hand
- Positive Froment's sign
- Wasting of the first dorsal interosseous muscle
- Clawing of the small and ring fingers
Correct Answer: Decreased sensation over the dorsal ulnar aspect of the hand
Explanation:
The dorsal ulnar cutaneous nerve (DUCN) branches off the ulnar nerve approximately 5-8 cm proximal to the wrist and supplies sensation to the dorsal ulnar aspect of the hand. A lesion at Guyon's canal (at the wrist) spares the DUCN, meaning dorsal sensation will be intact. A lesion at the elbow (cubital tunnel) affects the entire ulnar nerve, including the DUCN, resulting in decreased sensation over the dorsal ulnar hand.
Question 11:
A 25-year-old restrained driver involved in a high-speed motor vehicle collision sustains a flexion-distraction injury of the lumbar spine. Which of the following associated injuries has the highest incidence in this patient profile?
Options:
- Aortic transection
- Diaphragmatic rupture
- Hollow viscus injury (e.g., bowel perforation)
- Renal artery avulsion
- Splenic laceration
Correct Answer: Hollow viscus injury (e.g., bowel perforation)
Explanation:
Flexion-distraction injuries of the spine (Chance fractures) often occur from lap-belt injuries in motor vehicle accidents. The fulcrum of flexion is anterior to the spine (at the abdominal wall), causing tension failure of the posterior and middle columns. This mechanism is highly associated with intra-abdominal injuries, particularly hollow viscus injuries (e.g., small bowel perforations), which occur in up to 40-50% of cases.
Question 12:
Which of the following describes the correct vascular anatomy and blood supply of the scaphoid, predisposing its proximal pole to avascular necrosis following fracture?
Options:
- The primary blood supply enters at the dorsal ridge and supplies the proximal pole via retrograde flow.
- The primary blood supply enters the proximal pole directly from the anterior interosseous artery.
- The primary blood supply enters the volar tubercle and supplies the bone via antegrade flow.
- The ulnar artery provides the dominant supply to the proximal pole via the deep palmar arch.
- The dorsal carpal branch of the radial artery enters the proximal pole directly.
Correct Answer: The primary blood supply enters at the dorsal ridge and supplies the proximal pole via retrograde flow.
Explanation:
The major blood supply to the scaphoid (70-80%) comes from branches of the radial artery that enter the bone via the dorsal ridge (near the waist) and perfuse the proximal pole in a retrograde fashion. Because of this retrograde flow, fractures at the waist or proximal pole can disrupt the blood supply to the proximal fragment, greatly increasing the risk of avascular necrosis and nonunion.
Question 13:
A 7-year-old boy sustains a displaced lateral condyle fracture of the humerus. The family refuses surgery, and the fracture goes on to a nonunion. Years later, which of the following is the most likely late complication to develop?
Options:
- Median nerve palsy
- Anterior interosseous nerve syndrome
- Radial nerve palsy
- Tardy ulnar nerve palsy
- Posterior interosseous nerve entrapment
Correct Answer: Tardy ulnar nerve palsy
Explanation:
A nonunion of a lateral condyle fracture typically leads to a progressive cubitus valgus deformity due to the failure of the lateral column of the distal humerus to support the elbow joint properly. Over time, this valgus deformity stretches the ulnar nerve behind the medial epicondyle, resulting in a tardy ulnar nerve palsy years or even decades after the initial injury.
Question 14:
During a posterior-stabilized total knee arthroplasty, the surgeon assesses the flexion and extension gaps. The extension gap is symmetric and perfectly balanced, but the flexion gap is excessively tight. Which of the following is the most appropriate surgical adjustment?
Options:
- Resect more proximal tibia
- Downsize the femoral component to decrease the anteroposterior dimension
- Release the posterior cruciate ligament (PCL)
- Release the posterior capsule
- Increase the distal femoral resection
Correct Answer: Downsize the femoral component to decrease the anteroposterior dimension
Explanation:
When the extension gap is balanced but the flexion gap is tight, the goal is to increase the flexion gap without altering the extension gap. This can be achieved by decreasing the anteroposterior (AP) size of the femoral component, translating the femoral component anteriorly, or recessing the PCL (if retaining it, though this is a PS knee so PCL is already gone). Resecting more proximal tibia affects both gaps. Downsizing the AP femur size uniquely increases the flexion gap.
Question 15:
A 22-year-old collegiate baseball pitcher is diagnosed with a Type II SLAP (Superior Labrum Anterior and Posterior) lesion. The 'peel-back' mechanism is thought to be the primary cause of this injury. During which phase of the throwing motion does this mechanism generate the maximum torsional force on the biceps anchor?
Options:
- Wind-up
- Early cocking
- Late cocking
- Acceleration
- Follow-through
Correct Answer: Late cocking
Explanation:
The 'peel-back' mechanism occurs during the late cocking phase of throwing, when the shoulder is in maximal abduction and external rotation. In this position, the biceps vector shifts posteriorly, creating a torsional force that twists the biceps root and peels the superior labrum off the glenoid rim.
Question 16:
In the Young-Burgess classification, an Anteroposterior Compression Type II (APC-II) pelvic ring injury is characterized by a "symphyseal diastasis or longitudinal rami fractures" and widening of the sacroiliac joint. Which of the following best describes the status of the posterior pelvic ligaments in an APC-II injury?
Options:
- Both anterior and posterior sacroiliac ligaments are ruptured
- Anterior sacroiliac ligaments are ruptured, while the posterior sacroiliac ligaments remain intact
- Both anterior and posterior sacroiliac ligaments are intact
- Sacrospinous ligaments are intact, but sacrotuberous ligaments are ruptured
- Posterior sacroiliac ligaments are ruptured, while the anterior sacroiliac ligaments remain intact
Correct Answer: Anterior sacroiliac ligaments are ruptured, while the posterior sacroiliac ligaments remain intact
Explanation:
An APC-II injury involves disruption of the symphysis pubis (or vertical rami fractures) along with widening of the anterior sacroiliac joint. This anterior widening signifies rupture of the anterior sacroiliac ligaments and the sacrotuberous/sacrospinous ligaments, but the posterior sacroiliac ligaments remain intact. Because the strong posterior SI ligaments are intact, the pelvis is rotationally unstable but vertically stable. An APC-III injury occurs when the posterior SI ligaments also rupture, leading to global instability.
Question 17:
Which bone morphogenetic protein (BMP) is FDA-approved as an alternative to autograft for the treatment of acute, open tibial shaft fractures stabilized with an intramedullary nail?
Options:
- rhBMP-2
- rhBMP-7 (OP-1)
- rhBMP-3
- rhBMP-4
- rhBMP-9
Correct Answer: rhBMP-2
Explanation:
Recombinant human Bone Morphogenetic Protein-2 (rhBMP-2) is FDA approved for use in acute, open tibial shaft fractures stabilized with an intramedullary nail. rhBMP-7 (Osteogenic Protein-1 or OP-1) previously had a Humanitarian Device Exemption (HDE) for recalcitrant long bone nonunions but is no longer commercially available in the US for this indication.
Question 18:
A 58-year-old male with long-standing poorly controlled type 2 diabetes presents with a unilaterally swollen, red, and warm foot without skin ulceration. Radiographs reveal fragmentation and subluxation at the tarsometatarsal joints. Which imaging modality is most sensitive and specific for differentiating acute Charcot neuroarthropathy from underlying osteomyelitis in this scenario?
Options:
- Technetium-99m bone scan
- Three-phase bone scan
- Gallium-67 scan
- Non-contrast MRI
- Indium-111 labeled leukocyte scan combined with Technetium-99m sulfur colloid marrow scan
Correct Answer: Indium-111 labeled leukocyte scan combined with Technetium-99m sulfur colloid marrow scan
Explanation:
Differentiating Charcot arthropathy from osteomyelitis can be difficult, as both show increased uptake on a standard bone scan and marrow edema on MRI. The combination of an Indium-111 labeled leukocyte (WBC) scan and a Technetium-99m sulfur colloid marrow scan is the most highly specific test. In osteomyelitis, there is discordant uptake (increased WBC uptake, decreased sulfur colloid uptake due to marrow replacement by infection). In Charcot arthropathy, there is concordant uptake.
Question 19:
A patient suffers a knife laceration to the volar aspect of the hand, resulting in an inability to flex the proximal and distal interphalangeal joints of the middle finger. The injury is classified as a Zone II flexor tendon injury. What are the precise anatomic boundaries of flexor tendon Zone II?
Options:
- From the carpal tunnel to the A1 pulley
- From the A1 pulley to the insertion of the flexor digitorum superficialis (FDS)
- From the insertion of the FDS to the insertion of the flexor digitorum profundus (FDP)
- From the musculotendinous junction to the distal wrist crease
- From the A2 pulley to the A4 pulley
Correct Answer: From the A1 pulley to the insertion of the flexor digitorum superficialis (FDS)
Explanation:
Verdan's classification divides the flexor tendons into five zones. Zone II, historically known as "no man's land" due to historically poor surgical outcomes, extends from the proximal edge of the A1 pulley (distal palmar crease) to the insertion of the flexor digitorum superficialis (FDS) tendon on the middle phalanx. In this zone, both the FDS and FDP tendons travel together in a tight fibro-osseous sheath.
Question 20:
A 12-year-old premenarchal female is evaluated for Adolescent Idiopathic Scoliosis (AIS). She has a right thoracic curve. Her Risser stage is 0. Based on SRS (Scoliosis Research Society) guidelines, which of the following is the primary indication for initiating full-time bracing treatment?
Options:
- Curve magnitude of 15 to 20 degrees with documented progression of 5 degrees
- Any curve greater than 45 degrees regardless of progression
- Curve magnitude of 20 to 25 degrees at initial presentation
- Curve magnitude of 25 to 45 degrees with documented progression, or initial curve 30 to 39 degrees
- Curve magnitude of 10 degrees combined with a positive family history
Correct Answer: Curve magnitude of 25 to 45 degrees with documented progression, or initial curve 30 to 39 degrees
Explanation:
The SRS guidelines for bracing in AIS include patients who are skeletally immature (Risser 0-2, premenarchal) with a curve of 25 to 29 degrees that has documented progression of 5 degrees or more, or an initial presentation with a curve between 30 and 39 degrees. Curves > 45-50 degrees are generally indications for surgery, while curves < 25 degrees without documented progression are observed.
Question 21:
A 68-year-old male presents with insidious onset of anterior thigh pain five years after a primary total hip arthroplasty using a dual-taper modular femoral stem and a cobalt-chromium head. Radiographs are unremarkable. Aseptic joint aspiration reveals cloudy fluid with a normal nucleated cell count but elevated cobalt and chromium ions. During revision surgery, black necrotic debris is noted exclusively around the head-neck junction. What is the primary underlying electrochemical mechanism responsible for this finding?
Options:
- Fretting wear leading to third-body abrasion
- Galvanic corrosion driven by mixed-metal implantation
- Mechanically assisted crevice corrosion (MACC)
- Type IV hypersensitivity reaction to nickel
- Osteolysis secondary to polyethylene particulate debris
Correct Answer: Mechanically assisted crevice corrosion (MACC)
Explanation:
The clinical scenario and finding of black debris at the modular head-neck taper (trunnion) strongly suggest trunnionosis. The primary mechanism is mechanically assisted crevice corrosion (MACC). Micromotion at the modular interface (fretting) disrupts the protective passive oxide layer on the metal (usually titanium or cobalt-chromium). Once the oxide layer is breached, the crevice environment allows for a local drop in pH and oxygen depletion, accelerating the electrochemical corrosion process. This releases metal ions and debris, leading to adverse local tissue reactions (ALTR).
Question 22:
A 24-year-old male sustains a high-energy pelvic ring injury after a motor vehicle collision. CT imaging demonstrates a displaced crescent fracture of the ilium extending into the posterior aspect of the sacroiliac joint, consistent with a Day Type II lateral compression injury. What is the most biomechanically stable method of surgical fixation for this specific posterior ring injury?
Options:
- Anterior symphyseal plating alone
- Closed reduction and percutaneous iliosacral screw fixation alone
- Open reduction and internal fixation with a posterior iliac plate alone
- Combined iliosacral screw fixation for the sacroiliac component and lateral plating for the iliac wing fracture
- External fixation of the anterior ring
Correct Answer: Combined iliosacral screw fixation for the sacroiliac component and lateral plating for the iliac wing fracture
Explanation:
Day Type II crescent fractures involve a major fracture line exiting the iliac wing, but a substantial portion of the posterior ilium remains attached to the sacrum via the posterior SI ligaments. Biomechanical studies have demonstrated that for Day Type II fractures (where the fracture extends into the SI joint), combining an iliosacral screw to stabilize the SI joint component with an orthopedic plate for the iliac wing fracture provides the most stable construct, superior to either method alone.
Question 23:
A 32-year-old collegiate football player sustains a purely ligamentous Lisfranc injury. Weight-bearing radiographs demonstrate 3 mm of widening between the medial cuneiform and the base of the second metatarsal. According to recent prospective randomized trials, which treatment modality yields the best long-term functional outcome and lowest rate of reoperation for this specific injury pattern?
Options:
- Closed reduction and percutaneous Kirschner wire fixation
- Open reduction and internal fixation with transarticular screws
- Open reduction and internal fixation with dorsal bridge plating
- Primary arthrodesis of the first, second, and third tarsometatarsal joints
- Conservative management with a non-weight-bearing cast for 6 weeks
Correct Answer: Primary arthrodesis of the first, second, and third tarsometatarsal joints
Explanation:
In the setting of purely ligamentous Lisfranc injuries, multiple studies (including classic randomized controlled trials by Ly and Coetzee) have demonstrated that primary arthrodesis of the medial column (1st, 2nd, and 3rd TMT joints) yields superior functional outcomes, faster return to pre-injury activity levels, and significantly lower reoperation rates compared to ORIF with transarticular screws. Hardware removal and post-traumatic arthritis are significant complications associated with ORIF in purely ligamentous injuries.
Question 24:
A 16-year-old male presents with knee pain. Radiographs and a subsequent MRI reveal a high-grade conventional osteosarcoma of the distal femur. He undergoes neoadjuvant chemotherapy followed by wide surgical resection. Pathologic evaluation of the resected specimen is performed. Which of the following is the most significant independent prognostic factor for long-term overall survival in this patient?
Options:
- The specific chemotherapeutic agents used in the neoadjuvant regimen
- Histologic evidence of >90% tumor necrosis in the resection specimen
- The anatomic size of the tumor (volume > 200 mL)
- The degree of soft tissue extension outside the bony cortex
- Alkaline phosphatase levels at the time of initial diagnosis
Correct Answer: Histologic evidence of >90% tumor necrosis in the resection specimen
Explanation:
The degree of tumor necrosis following neoadjuvant chemotherapy is the single most important prognostic factor for overall survival in patients with localized high-grade osteosarcoma. A 'good response' is defined as >90% tumor necrosis (Huvos grade III or IV) and is associated with significantly higher 5-year survival rates compared to poor responders (<90% necrosis). While tumor size and initial lab markers have prognostic value, histologic response is the most highly predictive metric.
Question 25:
A patient undergoes a metal-on-metal total hip arthroplasty. Four years later, they present with pain and a large cystic pseudo-tumor. Histological analysis of the peri-articular tissue reveals aseptic lymphocytic vasculitis-associated lesions (ALVAL). What is the primary immunologic mechanism driving this specific histological response?
Options:
- IgE-mediated mast cell degranulation (Type I hypersensitivity)
- Cytotoxic antibody-mediated complement activation (Type II hypersensitivity)
- Immune complex deposition in the microvasculature (Type III hypersensitivity)
- T-cell mediated delayed hypersensitivity (Type IV hypersensitivity)
- Macrophage-driven foreign body granulomatous reaction without lymphocytic involvement
Correct Answer: T-cell mediated delayed hypersensitivity (Type IV hypersensitivity)
Explanation:
ALVAL (Aseptic Lymphocytic Vasculitis-Associated Lesions) is characteristic of adverse local tissue reactions (ALTR) in metal-on-metal hip implants. It is driven by a Type IV (delayed) hypersensitivity reaction to metal ions (like cobalt and chromium). This cell-mediated response involves the activation of CD4+ Th1 cells and is characterized histologically by a dense perivascular lymphocytic infiltrate, tissue necrosis, and the formation of pseudotumors, distinguishing it from the simple macrophage-mediated foreign body response seen with conventional polyethylene wear debris.
Question 26:
A 25-year-old elite overhead pitcher undergoes shoulder arthroscopy for chronic shoulder pain and mechanical symptoms. A Type II SLAP tear is identified. When evaluating the normal anatomy of the biceps-labral complex in preparation for repair, what is the typical anatomical origin of the long head of the biceps tendon?
Options:
- 100% from the superior glenoid tubercle
- 100% from the superior labrum
- Approximately 50% from the supraglenoid tubercle and 50% from the superior labrum
- Primarily from the coracoid process with expansions to the superior labrum
- Primarily from the intra-articular aspect of the greater tuberosity
Correct Answer: Approximately 50% from the supraglenoid tubercle and 50% from the superior labrum
Explanation:
The long head of the biceps tendon originates in a bifurcated manner. Anatomical studies show that approximately 50% of the tendon fibers attach directly to the supraglenoid tubercle of the scapula, and the remaining 50% blend into the superior aspect of the glenoid labrum. This structural relationship is critical to understand when diagnosing and repairing SLAP (Superior Labrum Anterior to Posterior) lesions, as tension on the biceps directly forces the superior labrum away from the glenoid.
Question 27:
A 13-year-old overweight male presents with an acute exacerbation of chronic right groin and knee pain. He walks with an externally rotated gait. Radiographs confirm a severe Slipped Capital Femoral Epiphysis (SCFE). Pathophysiologically, the slippage in SCFE occurs primarily through which specific histological zone of the proximal femoral physis?
Options:
- Reserve zone
- Proliferative zone
- Zone of hypertrophy
- Zone of provisional calcification
- Primary spongiosa
Correct Answer: Zone of hypertrophy
Explanation:
Slipped Capital Femoral Epiphysis (SCFE) typically occurs due to mechanical shear forces across a weakened physis during the adolescent growth spurt. Histologically and biomechanically, the weakest layer of the growth plate is the zone of hypertrophy. The slippage classically occurs through this layer because the chondrocytes are enlarged, and the extracellular matrix is sparse compared to the reserve or proliferative zones, making it highly susceptible to shear stress.
Question 28:
A 55-year-old female presents with a progressive flatfoot deformity, lateral hindfoot pain, and inability to perform a single-leg heel rise. Clinical exam shows a flexible hindfoot valgus and forefoot abduction. Radiographs show >40% uncoverage of the talonavicular joint. Diagnosis of Stage IIB Posterior Tibial Tendon Dysfunction (PTTD) is made. Which of the following surgical interventions is most critical to correct the specific forefoot abduction deformity in this stage?
Options:
- Medial displacement calcaneal osteotomy (MDCO)
- Flexor digitorum longus (FDL) transfer to the navicular
- Lateral column lengthening (Evans osteotomy)
- Spring ligament reconstruction
- Triple arthrodesis
Correct Answer: Lateral column lengthening (Evans osteotomy)
Explanation:
Stage IIB PTTD is characterized by a flexible flatfoot with significant forefoot abduction (>40% talonavicular uncoverage). While an FDL transfer replaces the function of the diseased posterior tibial tendon, and a medial displacement calcaneal osteotomy (MDCO) corrects hindfoot valgus, the lateral column lengthening (Evans osteotomy) is specifically required to correct the forefoot abduction deformity by lengthening the lateral column and pivoting the navicular back over the talar head.
Question 29:
A 28-year-old male sustains a severe closed crush injury to his left leg. Over the next 4 hours, his pain becomes disproportionate to the injury, and he experiences extreme pain with passive stretch of his toes. Compartment pressure monitoring is initiated. Which of the following thresholds represents the most widely accepted absolute indication for a four-compartment fasciotomy?
Options:
- Absolute compartment pressure > 20 mmHg
- Absolute compartment pressure > 30 mmHg
- Delta P (Mean Arterial Pressure - Compartment Pressure) < 30 mmHg
- Delta P (Diastolic Blood Pressure - Compartment Pressure) < 30 mmHg
- Delta P (Systolic Blood Pressure - Compartment Pressure) < 40 mmHg
Correct Answer: Delta P (Diastolic Blood Pressure - Compartment Pressure) < 30 mmHg
Explanation:
The diagnosis of acute compartment syndrome is primarily clinical, but when using intracompartmental pressure monitoring, the 'Delta P' is the most reliable metric. Delta P is calculated as the Diastolic Blood Pressure minus the Compartment Pressure. A Delta P of less than 30 mmHg indicates inadequate tissue perfusion pressure and is the universally accepted threshold indicating the need for emergent fasciotomy. Using absolute compartment pressures alone (e.g., >30 mmHg) can lead to unnecessary surgeries, especially in hypertensive patients.
Question 30:
A 68-year-old female presents with persistent anterior knee pain three years following a primary Posterior Stabilized (PS) Total Knee Arthroplasty. She reports a distinct 'catching' and 'popping' sensation as her knee extends from roughly 40 degrees of flexion to full extension. What is the most likely pathophysiological cause of this phenomenon?
Options:
- Aseptic loosening of the tibial baseplate
- Patellar clunk syndrome due to a fibrosynovial nodule engaging the intercondylar box
- Oversizing of the femoral component leading to excessive retinacular tension
- Polyethylene wear of the post-cam mechanism
- Global instability due to secondary medial collateral ligament attenuation
Correct Answer: Patellar clunk syndrome due to a fibrosynovial nodule engaging the intercondylar box
Explanation:
The classic presentation of a painless or painful 'pop' or 'clunk' as the knee moves from flexion into extension (typically around 30-45 degrees) in a Posterior Stabilized (PS) TKA is Patellar Clunk Syndrome. It is caused by the formation of a fibrosynovial nodule on the undersurface of the distal quadriceps tendon just superior to the patella. During flexion, this nodule drops into the intercondylar box of the PS femoral component. As the knee extends, the nodule catches on the superior edge of the box and then abruptly pops out, causing the 'clunk'.
Question 31:
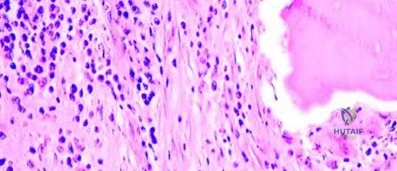
A 35-year-old female presents with a lytic lesion in the distal femur. Biopsy confirms Giant Cell Tumor (GCT) of bone. Due to the proximity to the joint and tumor size, the multidisciplinary tumor board recommends neoadjuvant treatment with denosumab prior to curettage. What is the specific molecular mechanism of action of denosumab in treating GCT?
Options:
- Direct induction of apoptosis in the neoplastic mononuclear cells
- Inhibition of vascular endothelial growth factor (VEGF) to reduce tumor angiogenesis
- Binding to RANK Ligand (RANKL), preventing activation of the RANK receptor on osteoclast-like giant cells
- Irreversible binding to hydroxyapatite crystals, inhibiting osteoclastic acid secretion
- Stimulation of osteoprotegerin (OPG) synthesis by osteoblasts
Correct Answer: Binding to RANK Ligand (RANKL), preventing activation of the RANK receptor on osteoclast-like giant cells
Explanation:
Giant Cell Tumor of bone consists of neoplastic mononuclear cells that express high levels of RANK Ligand (RANKL), which recruits and activates reactive multi-nucleated osteoclast-like giant cells that cause the extensive bone destruction. Denosumab is a fully human monoclonal antibody that binds directly to RANKL. By neutralizing RANKL, denosumab prevents the interaction with the RANK receptor on the surface of osteoclast precursors and giant cells, thereby profoundly inhibiting osteolysis and allowing the tumor bed to ossify.
Question 32:
A 62-year-old male with severe cervical spondylotic myelopathy undergoes an MRI of the cervical spine. Which specific MRI signal characteristic in the spinal cord is most strongly correlated with irreversible neurological deficit and poor postoperative functional recovery following decompression?
Options:
- Hyperintensity on T2-weighted images alone
- Hypointensity on T1-weighted images accompanied by T2 hyperintensity
- Loss of the normal cervical lordosis on T1-weighted sagittal images
- Hypertrophy of the ligamentum flavum appearing hypointense on T2 images
- Gadolinium enhancement within the central gray matter
Correct Answer: Hypointensity on T1-weighted images accompanied by T2 hyperintensity
Explanation:
In the setting of cervical spondylotic myelopathy, intrinsic spinal cord signal changes carry significant prognostic value. T2 hyperintensity is a common finding and often represents reversible edema or gliosis. However, the presence of hypointensity on T1-weighted images (which is typically accompanied by focal T2 hyperintensity) indicates cystic necrosis, cavitation, or permanent myelomalacia of the spinal cord. This specific finding is an independent predictor of poor neurological recovery following decompressive surgery.
Question 33:
A 40-year-old female sustains a fall onto an outstretched hand, resulting in a 'terrible triad' injury of the elbow. She is taken to the operating room for open reduction and internal fixation. To systematically restore elbow stability, which of the following sequences of repair is most structurally appropriate and currently recommended?
Options:
- Radial head fixation/replacement → Lateral collateral ligament repair → Coronoid fixation
- Coronoid fixation → Radial head fixation/replacement → Lateral collateral ligament repair
- Lateral collateral ligament repair → Coronoid fixation → Radial head fixation/replacement
- Medial collateral ligament repair → Radial head fixation/replacement → Lateral collateral ligament repair
- Radial head fixation/replacement → Coronoid fixation → Medial collateral ligament repair
Correct Answer: Coronoid fixation → Radial head fixation/replacement → Lateral collateral ligament repair
Explanation:
The terrible triad of the elbow consists of an elbow dislocation, a radial head fracture, and a coronoid fracture. The standard surgical protocol for restoring stability is an 'inside-out' or 'deep-to-superficial' approach. The coronoid (or anterior capsule) is repaired first to restore the anterior buttress. Next, the radial head is fixed or replaced to restore the anterior and valgus buttress. Finally, the lateral collateral ligament (LCL) complex is repaired to the lateral epicondyle to restore posterolateral rotatory stability. The MCL is typically only explored/repaired if the elbow remains unstable after these three steps.
Question 34:
A 14-year-old female gymnast presents with chronic, progressive low back pain exacerbated by extension. Lateral radiographs demonstrate an isthmic spondylolisthesis at L5-S1. In assessing her risk for continued slip progression, which spinopelvic parameter is considered the most predictive intrinsic biomechanical risk factor?
Options:
- A low Pelvic Incidence (PI)
- A high Pelvic Incidence (PI)
- A low Sacral Slope (SS)
- A high Pelvic Tilt (PT) with a low Sacral Slope (SS)
- Lumbar hyperlordosis unrelated to sacral morphology
Correct Answer: A high Pelvic Incidence (PI)
Explanation:
Pelvic incidence (PI) is a fixed morphological parameter unique to each individual (PI = Sacral Slope + Pelvic Tilt). A high pelvic incidence correlates with a more vertical orientation of the sacrum relative to the pelvis, which inherently increases the shear forces at the lumbosacral junction. Consequently, a high pelvic incidence is the most significant spinopelvic parameter predicting the risk of progression in pediatric and adolescent isthmic spondylolisthesis.
Question 35:
An 82-year-old frail female with osteopenia sustains a fall and presents with neck pain. CT scan reveals a displaced Type II odontoid fracture. Conservative management with a hard cervical collar is considered but has a known high nonunion rate. If surgical intervention is elected, what is the preferred technique given her age and bone quality?
Options:
- Anterior single odontoid screw fixation
- Anterior dual odontoid screw fixation
- Posterior C1-C2 instrumented fusion
- Occipitocervical fusion
- Halo vest immobilization
Correct Answer: Posterior C1-C2 instrumented fusion
Explanation:
Type II odontoid fractures in the elderly (>70-80 years) present a significant challenge. While a rigid collar is often used, nonunion rates are very high. Halo vest immobilization is contraindicated in this demographic due to unacceptably high morbidity and mortality (e.g., respiratory complications, falls). If surgery is indicated, anterior odontoid screw fixation relies on good bone quality (which is lacking in osteopenia) and an intact transverse ligament. Therefore, posterior C1-C2 instrumented fusion (e.g., Harms technique) provides the highest union rates and biomechanical stability for elderly osteopenic patients with displaced Type II fractures.
Question 36:
A surgeon is planning to harvest an autologous structural bone graft for a complex nonunion reconstruction. When utilizing a cortical autograft, the graft undergoes incorporation via 'creeping substitution'. What is the initial cellular phase of creeping substitution in cortical bone, and how does it affect the graft biomechanically?
Options:
- Initial osteoblastic apposition, which temporarily increases the mechanical strength of the graft
- Initial osteoclastic resorption, which temporarily decreases the mechanical strength of the graft
- Initial chondrocytic proliferation, forming a cartilaginous intermediate that maintains strength
- Initial vascular ingrowth causing immediate rigid calcification
- Simultaneous osteoclastic and osteoblastic activity maintaining a steady-state mechanical profile
Correct Answer: Initial osteoclastic resorption, which temporarily decreases the mechanical strength of the graft
Explanation:
The incorporation of cortical bone grafts occurs via creeping substitution, which strictly begins with an osteoclastic resorptive phase. Osteoclasts must bore cutting cones into the dense cortical bone to allow subsequent vascular ingrowth and osteoblast activity. Because resorption precedes formation, cortical grafts become significantly weaker and more porous during the first 6 to 12 months before structural integrity is eventually restored. In contrast, cancellous grafts undergo initial osteoblastic apposition, leading to early strengthening.
Question 37:
A 28-year-old carpenter sustains a complete laceration of his index finger flexor digitorum profundus (FDP) and superficialis (FDS) in Zone II. During the primary repair of the FDP tendon, the surgeon places a 4-strand core suture and adds a peripheral running epitendinous suture. What is the primary biomechanical advantage of adding the epitendinous suture?
Options:
- It prevents immediate adhesion formation to the flexor sheath
- It provides the primary resistance against cyclic loading fatigue
- It decreases the cross-sectional area of the tendon, facilitating glide
- It increases the tensile strength of the repair by up to 50% and decreases gap formation
- It replaces the need for a multi-strand core suture configuration
Correct Answer: It increases the tensile strength of the repair by up to 50% and decreases gap formation
Explanation:
In flexor tendon repair, while the core suture provides the bulk of the initial tensile strength, the addition of a peripheral epitendinous suture is crucial. Biomechanical studies have consistently demonstrated that a well-placed epitendinous suture increases the overall ultimate tensile strength of the repair by 10% to 50%, smooths the repair site to improve gliding, and, critically, decreases the incidence of gap formation at the repair site during early active motion protocols.
Question 38:
When evaluating the ultrastructure of articular cartilage, distinct biomechanical properties are conferred by the zonal arrangement of collagen and proteoglycans. Which of the following statements most accurately describes the superficial (tangential) zone of articular cartilage?
Options:
- It has the highest concentration of proteoglycans and lowest water content
- Collagen fibers are oriented perpendicular to the articular surface to resist compressive loads
- It contains the highest concentration of water and collagen fibers oriented parallel to the joint surface
- It is primarily composed of Type X collagen indicating endochondral ossification
- It is physically separated from the middle zone by the 'tidemark'
Correct Answer: It contains the highest concentration of water and collagen fibers oriented parallel to the joint surface
Explanation:
Articular cartilage is structurally divided into zones. The superficial (tangential) zone has the highest water content, the lowest proteoglycan content, and densely packed Type II collagen fibers that are oriented strictly parallel to the articular surface. This parallel alignment provides the cartilage with its maximal tensile stiffness and resistance to shear forces. The deep zone has perpendicular fibers and highest proteoglycans to resist compression. The 'tidemark' separates the deep zone from the calcified cartilage zone, not the superficial from the middle.
Question 39:
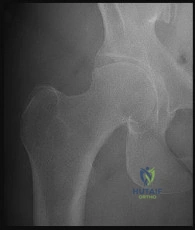
A 38-year-old male presents with right hip pain. He has a history of long-term corticosteroid use for severe asthma. Radiographs demonstrate an area of sclerosis and subchondral radiolucency (crescent sign) in the anterosuperior aspect of the femoral head, consistent with osteonecrosis. According to the modified Ficat and Arlet classification, the presence of a structural subchondral collapse (crescent sign) without narrowing of the hip joint space places him in which stage?
Options:
- Stage I
- Stage II
- Stage III
- Stage IV
- Stage V
Correct Answer: Stage III
Explanation:
The Ficat and Arlet classification is classically used to stage osteonecrosis of the femoral head based on standard radiographs. Stage I has normal radiographs (but positive MRI). Stage II shows cystic/sclerotic changes without subchondral collapse. Stage III is defined by subchondral collapse, which is classically visualized as the 'crescent sign' (subchondral radiolucency indicating mechanical failure of the trabecular bone), but the joint space remains preserved. Stage IV involves secondary osteoarthritis with joint space narrowing and acetabular changes.
Question 40:
A 22-year-old male sustains a severe inversion injury to his ankle. He complains of pain over the lateral aspect of the foot. On examination, he has focal tenderness over the dorsal cuboid. Radiographs reveal a 'nutcracker' fracture of the cuboid. What is the classic mechanism of injury for this specific fracture pattern?
Options:
- Extreme dorsiflexion and axial loading of the midfoot
- Direct crush injury to the dorsum of the foot
- Forceful plantarflexion and inversion causing avulsion of the calcaneocuboid ligament
- Forced plantarflexion and severe abduction, crushing the cuboid between the calcaneus and the 4th/5th metatarsals
- Isolated extreme pronation of the forefoot relative to the hindfoot
Correct Answer: Forced plantarflexion and severe abduction, crushing the cuboid between the calcaneus and the 4th/5th metatarsals
Explanation:
The 'nutcracker' fracture of the cuboid is a classic compression fracture. The mechanism is severe forced abduction of the forefoot with the foot in a plantarflexed position. This forceful movement mechanically compresses (or 'crushes') the cuboid between the anterior articular surface of the calcaneus and the bases of the 4th and 5th metatarsals. This leads to shortening of the lateral column of the foot, which must often be corrected surgically to prevent long-term abduction deformity and painful nonunion/malunion.
Question 41:
A ligament is stretched to a fixed length during a biomechanical study, and the force required to maintain that specific length gradually decreases over time. What intrinsic viscoelastic property of the ligament does this phenomenon describe?
Options:
- Creep
- Stress relaxation
- Hysteresis
- Fatigue failure
- Isotropic elasticity
Correct Answer: Stress relaxation
Explanation:
Stress relaxation is the decrease in stress (force) over time when a viscoelastic material is held at a constant strain (length). In contrast, creep is the increase in strain (deformation) over time when the material is held at a constant stress (load). Hysteresis is the energy lost as heat during the loading and unloading cycle.
Question 42:
A 79-year-old male presents to the emergency department after a ground-level fall. He complains of upper neck pain. He has a history of severe COPD, congestive heart failure, and osteoporosis. CT imaging of the cervical spine shows a Type II odontoid fracture with 2mm of posterior displacement. What is the most appropriate management for this patient?
Options:
- Anterior odontoid screw fixation
- C1-C2 posterior spinal fusion
- Rigid cervical collar
- Halo vest immobilization
- C1-C2 transarticular screw fixation
Correct Answer: Rigid cervical collar
Explanation:
In elderly patients with significant comorbidities (e.g., severe COPD, osteoporosis), non-operative management with a rigid cervical collar is favored for Type II odontoid fractures. While the nonunion rate is high with collar therapy, fibrous nonunion is often well-tolerated, and the morbidity and mortality associated with surgery or a halo vest in frail elderly populations are prohibitively high.
Question 43:
During an anatomical reconstruction of the posterolateral corner (PLC) of the knee, the surgeon is carefully defining the insertions on the proximal fibula. Which of the following structures inserts slightly anterior and distal to the tip (styloid) on the lateral aspect of the fibular head?
Options:
- Biceps femoris
- Popliteofibular ligament
- Fibular collateral ligament (FCL)
- Arcuate ligament
- Fabellofibular ligament
Correct Answer: Fibular collateral ligament (FCL)
Explanation:
The fibular collateral ligament (FCL) inserts on the lateral aspect of the fibular head, approximately 8.2 mm posterior to the anterior margin of the fibular head and 28.4 mm distal to the tip of the fibular styloid. The popliteofibular ligament (PFL) inserts on the posteromedial aspect of the fibular styloid.
Question 44:
A 28-year-old female presents with progressive knee pain. Radiographs show an eccentric, purely lytic lesion in the distal femoral epiphysis extending to the subchondral bone without a sclerotic rim. Biopsy reveals multinucleated giant cells in a background of mononuclear stromal cells. Which systemic therapy specifically targets the primary pathophysiology of this lesion?
Options:
- Denosumab
- Imatinib
- Doxorubicin
- Methotrexate
- Zoledronic acid
Correct Answer: Denosumab
Explanation:
Giant Cell Tumor of Bone (GCTB) is characterized by neoplastic mononuclear stromal cells that express RANKL, which recruits and activates the reactive multinucleated osteoclast-like giant cells causing osteolysis. Denosumab is a monoclonal antibody against RANKL and is highly effective in the treatment of advanced, recurrent, or unresectable GCTB.
Question 45:
A patient sustains a deep glass laceration over the volar aspect of the proximal phalanx of the ring finger, completely transecting both the Flexor Digitorum Superficialis (FDS) and Flexor Digitorum Profundus (FDP) tendons. This anatomical location corresponds to which flexor tendon zone?
Options:
- Zone I
- Zone II
- Zone III
- Zone IV
- Zone V
Correct Answer: Zone II
Explanation:
Zone II (historically known as Bunnell's 'no man\'s land') extends from the distal palmar crease (the proximal edge of the A1 pulley) to the insertion of the FDS tendon on the middle phalanx. It contains both the FDS and FDP tendons within a tight fibro-osseous sheath, making repair challenging and prone to adhesions.
Question 46:
A 32-year-old male sustains a Hawkins Type III talar neck fracture following a high-speed motor vehicle collision. Which of the following accurately describes the displacement pattern and the approximate historical risk of avascular necrosis (AVN) for this specific injury type?
Options:
- Displaced talar neck fracture with subtalar dislocation; 20-50% risk of AVN.
- Displaced talar neck fracture with subtalar and tibiotalar dislocation; nearly 100% risk of AVN.
- Displaced talar neck fracture with subtalar, tibiotalar, and talonavicular dislocation; 100% risk of AVN.
- Nondisplaced talar neck fracture; 0-10% risk of AVN.
- Displaced talar neck fracture with talonavicular dislocation only; 50% risk of AVN.
Correct Answer: Displaced talar neck fracture with subtalar and tibiotalar dislocation; nearly 100% risk of AVN.
Explanation:
Hawkins Type III is a displaced talar neck fracture with dislocation of both the subtalar and tibiotalar joints. The risk of AVN in Type III fractures is exceptionally high, historically reported as up to 100% (though modern series may show ~85-90%). Type I is nondisplaced (~0-15% AVN). Type II has subtalar dislocation (~20-50% AVN). Type IV involves the talonavicular joint in addition to the subtalar and tibiotalar joints.
Question 47:
In the context of total hip arthroplasty (THA), the phenomenon of 'stripe wear' is a localized area of increased wear and surface roughness caused by edge loading during transient microseparation. This is most characteristic of which bearing surface combination?
Options:
- Ceramic-on-ceramic
- Metal-on-metal
- Highly cross-linked polyethylene-on-metal
- Ceramic-on-polyethylene
- Metal-on-conventional polyethylene
Correct Answer: Ceramic-on-ceramic
Explanation:
'Stripe wear' is specifically associated with ceramic-on-ceramic bearings. It occurs when the ceramic femoral head transiently subluxates (microseparation) during the swing phase of gait and contacts the hard rim of the ceramic liner, resulting in a narrow stripe of wear and roughening on the femoral head.
Question 48:
A 12-year-old obese male presents with left knee pain and a limp. Physical examination demonstrates obligate external rotation of the left hip during passive flexion. He is diagnosed with a stable Slipped Capital Femoral Epiphysis (SCFE) and undergoes in situ pinning with a single cannulated screw. What is the most common long-term complication of this treated condition?
Options:
- Avascular necrosis (AVN)
- Chondrolysis
- Femoral-acetabular impingement (FAI)
- Slipped contralateral epiphysis
- Subtrochanteric fracture
Correct Answer: Femoral-acetabular impingement (FAI)
Explanation:
Femoral-acetabular impingement (FAI), specifically cam-type impingement, is the most common complication after in situ pinning of a SCFE. The prominent anterior metaphysis created by the posterior slip abuts the acetabular rim during flexion and internal rotation. AVN is a dreaded complication but is much more common in unstable SCFE. Chondrolysis is associated with unrecognized joint penetration by the hardware.
Question 49:
A 45-year-old female presents in hemorrhagic shock after a severe crush injury. Pelvic radiographs show an APC-III pelvic ring injury (diastasis of the symphysis pubis and bilateral SI joint disruption). A pelvic binder is applied and fluid resuscitation initiated, but she remains hemodynamically unstable. In this clinical scenario, what is the most statistically likely source of her pelvic hemorrhage?
Options:
- Superior gluteal artery
- Obturator artery
- Internal pudendal artery
- Presacral venous plexus
- External iliac artery
Correct Answer: Presacral venous plexus
Explanation:
Venous bleeding accounts for 80-90% of all pelvic hemorrhage in pelvic ring injuries. The presacral venous plexus and prevesical veins are the most common sources. While arterial bleeding (from the superior gluteal, pudendal, or obturator arteries) can be severe, brisk, and often requires angioembolization, the venous plexus is overwhelmingly the most likely overall source of bleeding.
Question 50:
Bone Morphogenetic Protein 2 (BMP-2) signals primarily through which intracellular cascade to stimulate osteoblastic differentiation and endochondral ossification?
Options:
- Wnt/beta-catenin pathway
- Smad 1/5/8 pathway
- JAK/STAT pathway
- Notch/Hes1 pathway
- MAP kinase pathway
Correct Answer: Smad 1/5/8 pathway
Explanation:
BMPs bind to serine/threonine kinase receptors on the cell membrane, leading to the phosphorylation of receptor-regulated Smads (specifically Smad 1, 5, and 8). These phosphorylated Smads form a complex with Smad 4 (co-Smad) and translocate to the nucleus, where they regulate the transcription of osteogenic genes such as Runx2.
Question 51:
A 24-year-old male sustains a severe traction injury to his brachial plexus, resulting in a C5-C6 root avulsion. An Oberlin transfer is planned to restore active elbow flexion. Which donor nerve fascicle is classically utilized in this procedure to transfer to the biceps motor branch of the musculocutaneous nerve?
Options:
- A redundant fascicle from the ulnar nerve
- The thoracodorsal nerve
- The medial pectoral nerve
- A fascicle from the median nerve (FCR branch)
- The intercostobrachial nerve
Correct Answer: A redundant fascicle from the ulnar nerve
Explanation:
The classic Oberlin transfer utilizes a redundant fascicle from the ulnar nerve (usually one supplying the flexor carpi ulnaris) and transfers it directly to the motor branch of the biceps (part of the musculocutaneous nerve) to restore elbow flexion in patients with upper trunk (C5-C6) brachial plexus injuries.
Question 52:
During a primary total knee arthroplasty (TKA), the surgeon inadvertently places the femoral component in internal rotation relative to the surgical epicondylar axis. This specific technical error is most likely to result in which of the following postoperative issues?
Options:
- Lateral patellar tracking and patellofemoral instability
- Medial patellar tracking
- Symmetrical extension space tightness
- Increased lateral compartment laxity in extension
- Excessive lateral compartment tightness in flexion
Correct Answer: Lateral patellar tracking and patellofemoral instability
Explanation:
Internal rotation of the femoral component in TKA shifts the trochlear groove medially relative to the extensor mechanism. This effectively increases the Q-angle, predisposing the patient to lateral patellar subluxation, tracking abnormalities, and patellofemoral instability. It also causes tightness in the medial flexion gap.
Question 53:
A 55-year-old male presents with deep, aching pain in his proximal humerus. Radiographs demonstrate a large, permeative lytic lesion with intralesional 'popcorn' calcifications and significant endosteal scalloping. Core needle biopsy confirms a Grade II (intermediate grade) chondrosarcoma. What is the standard treatment of choice for this lesion?
Options:
- Intralesional curettage and cryotherapy
- Neoadjuvant chemotherapy followed by wide excision
- Wide surgical excision alone
- Radiation therapy followed by wide excision
- Intralesional curettage, phenol, and cementation
Correct Answer: Wide surgical excision alone
Explanation:
Conventional chondrosarcomas are generally resistant to both chemotherapy and radiation therapy. The standard of care for Grade II and Grade III chondrosarcomas is wide, en bloc surgical excision. Extended intralesional curettage with local adjuvants is generally reserved for low-grade (Grade I/atypical cartilaginous tumors) in the appendicular skeleton.
Question 54:
A 68-year-old male presents with bilateral leg heaviness and pain that worsens with standing and walking but improves when leaning forward on a shopping cart. MRI shows severe central canal stenosis at L4-L5. Which of the following anatomical structures bounds the central spinal canal posteriorly and contributes significantly to the stenosis when hypertrophied?
Options:
- The posterior longitudinal ligament
- The pedicles
- The ligamentum flavum and laminae
- The superior articular process
- The intervertebral disc
Correct Answer: The ligamentum flavum and laminae
Explanation:
The central spinal canal is bordered anteriorly by the posterior vertebral body and the intervertebral disc (covered by the PLL), laterally by the pedicles, and posteriorly by the laminae and the ligamentum flavum. Hypertrophy and buckling of the ligamentum flavum, along with facet arthropathy, are primary drivers of acquired central lumbar spinal stenosis.
Question 55:
A 22-year-old collegiate wrestler undergoes an MRI arthrogram after sustaining a traumatic anterior shoulder dislocation. The imaging reveals that the anterior labrum is torn and displaced medially along the glenoid neck, but the anterior periosteum remains intact, forming a sleeve. What is the specific eponym for this lesion?
Options:
- Bankart lesion
- ALPSA lesion
- Perthes lesion
- GLAD lesion
- HAGL lesion
Correct Answer: ALPSA lesion
Explanation:
An ALPSA (Anterior Labroligamentous Periosteal Sleeve Avulsion) lesion occurs when the anterior labrum is torn and rolls medially along the glenoid neck while the periosteum remains intact. A Bankart lesion is a frank detachment of both the labrum and periosteum. A Perthes lesion has an intact periosteum with a non-displaced torn labrum. GLAD is Glenolabral Articular Disruption (involving cartilage). HAGL is Humeral Avulsion of the Glenohumeral Ligament.
Question 56:
A 35-year-old patient with Charcot-Marie-Tooth disease presents with a bilateral cavovarus foot deformity. On examination, the clinician performs a Coleman block test. When the lateral aspect of the foot rests on the block and the first ray is allowed to drop off into a recess, the hindfoot varus corrects completely to neutral. What does this specific finding indicate?
Options:
- Tibialis posterior overactivity is driving the hindfoot varus.
- Weakness of the peroneus brevis is the primary deforming force.
- The hindfoot varus is flexible and primarily driven by a plantarflexed first ray.
- There is a fixed Achilles tendon contracture causing varus.
- The patient has advanced, rigid subtalar joint arthritis.
Correct Answer: The hindfoot varus is flexible and primarily driven by a plantarflexed first ray.
Explanation:
The Coleman block test evaluates the flexibility of the hindfoot in a cavovarus foot. If the hindfoot varus corrects to neutral when the first ray drops off the block, it indicates that the hindfoot deformity is flexible and is secondarily driven by the fixed forefoot pronation (specifically, a plantarflexed first ray). If the hindfoot remains in varus, the hindfoot deformity is rigid/fixed.
Question 57:
A 41-year-old female develops a widespread eczematous skin rash overlying her forearm three weeks after open reduction and internal fixation of a distal radius fracture utilizing a standard 316L stainless steel volar locking plate. Dermatology consultation confirms a metal allergy via patch testing. Which specific element within the stainless steel alloy is most commonly responsible for this type IV hypersensitivity reaction?
Options:
- Titanium
- Cobalt
- Chromium
- Nickel
- Molybdenum
Correct Answer: Nickel
Explanation:
Nickel is the most common metal sensitizer in the general population, accounting for the vast majority of Type IV hypersensitivity (allergic contact dermatitis) reactions to metallic orthopedic implants. Medical-grade 316L stainless steel contains approximately 10-14% nickel, making it a frequent culprit in sensitive individuals, often necessitating hardware removal or revision to a titanium implant.
Question 58:
A 10-year-old boy presents with a painful, rigid flatfoot and a history of recurrent ankle sprains. Examination shows a profound limitation of subtalar motion. Lateral weight-bearing radiographs of the foot demonstrate the 'C-sign'. Which of the following is the most likely diagnosis?
Options:
- Calcaneonavicular coalition
- Talocalcaneal coalition
- Cubonavicular coalition
- Accessory navicular
- Congenital vertical talus
Correct Answer: Talocalcaneal coalition
Explanation:
The 'C-sign' on a lateral radiograph is a continuous C-shaped arc formed by the medial outline of the talar dome and the posterior outline of the sustentaculum tali. It is highly indicative of a talocalcaneal (subtalar) coalition. Calcaneonavicular coalition is typically seen on a 45-degree internal oblique radiograph as the 'anteater nose' sign.
Question 59:
A 28-year-old male sustains a severe crush injury to his right leg and undergoes emergent four-compartment fasciotomies. Postoperatively, the anterior compartment muscles are found to be completely necrotic and require radical debridement. Which of the following physical deficits will this patient inevitably exhibit as a direct result?
Options:
- Inability to actively plantarflex the ankle
- Profound weakness in active foot eversion
- Loss of active ankle dorsiflexion
- Inability to actively flex the toes
- Sensory loss over the entire plantar aspect of the foot
Correct Answer: Loss of active ankle dorsiflexion
Explanation:
The anterior compartment of the leg contains the tibialis anterior, extensor hallucis longus, extensor digitorum longus, and peroneus tertius muscles. The primary function of these muscles is dorsiflexion of the ankle and extension of the toes. Complete necrosis and debridement of this compartment will result in foot drop (loss of active ankle dorsiflexion). Eversion is lateral compartment; plantarflexion/toe flexion is posterior compartment.
Question 60:
A 15-year-old boy complains of intense, unrelenting right thigh pain that is noticeably worse at night and dramatically relieved within 30 minutes of taking ibuprofen. A CT scan reveals a 7mm radiolucent nidus surrounded by dense, reactive cortical sclerosis in the proximal femur. Which of the following factors produced within the nidus is most directly responsible for this characteristic pain pattern?
Options:
- High concentration of interleukins
- Extensive infiltration of eosinophils
- Elevated levels of prostaglandins
- Accumulation of lactic acid
- Overexpression of RANK ligand
Correct Answer: Elevated levels of prostaglandins
Explanation:
The nidus of an osteoid osteoma produces extraordinarily high levels of prostaglandins (particularly Prostaglandin E2, or PGE2) due to high expression of cyclooxygenase (COX) enzymes. This localized prostaglandin production causes profound vasodilation and is the direct cause of the intense, nocturnal pain that is classically and rapidly relieved by NSAIDs or salicylates.