Full Question & Answer Text (for Search Engines)
Question 1:
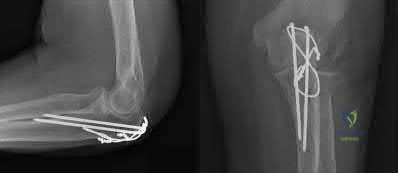
A 5-year-old boy falls from monkey bars and sustains a widely displaced supracondylar humerus fracture. Upon presentation to the emergency department, the hand is pink but the radial pulse is absent. He undergoes prompt closed reduction and percutaneous pinning. Post-operatively in the recovery room, the radial pulse remains absent, but the hand is warm with brisk capillary refill (less than 2 seconds) and normal oxygen saturation on the index finger. Which of the following is the most appropriate next step in management?
Options:
- Immediate return to the operating room for open exploration of the brachial artery
- Removal of the pins and placement of a hyperflexion cast
- Observation with close neurovascular monitoring
- CT angiography of the upper extremity
- Prophylactic forearm fasciotomies
Correct Answer: Observation with close neurovascular monitoring
Explanation:
The patient has a 'pink, pulseless' hand following reduction and pinning of a supracondylar humerus fracture. Current pediatric orthopedic guidelines recommend observation for a well-perfused (pink, warm, brisk capillary refill) but pulseless hand post-reduction. The collateral circulation around the elbow is robust enough to maintain distal viability. Vascular exploration is indicated if the hand is white, cold, and poorly perfused (pulseless and ischemic) after a well-aligned reduction. Arteriography is generally not indicated and delays treatment if the limb is ischemic. Removing pins would destabilize the fracture and risk further neurovascular injury.
Question 2:
A 55-year-old man presents with an insidious onset of dull, aching shoulder pain. Radiographs demonstrate a calcified intramedullary lesion in the proximal humerus with endosteal scalloping involving 80% of the cortical thickness. Biopsy confirms a low-grade chondrosarcoma. What is the most appropriate definitive management?
Options:
- Observation with serial radiographs every 6 months
- Intralesional curettage with phenol adjuvant and bone grafting
- Wide surgical resection with anatomic reconstruction
- Neoadjuvant chemotherapy followed by wide resection
- Primary radiation therapy
Correct Answer: Wide surgical resection with anatomic reconstruction
Explanation:
The clinical and radiographic presentation is classic for a primary central chondrosarcoma. Unlike enchondromas, chondrosarcomas frequently exhibit endosteal scalloping greater than 2/3 of the cortical thickness and present with mechanical or biologic pain. Chondrosarcomas are notoriously resistant to both chemotherapy and radiation therapy. The mainstay of treatment for conventional chondrosarcoma is wide surgical resection. While extended intralesional curettage may be considered for some appendicular atypical cartilaginous tumors (Grade 1), wide resection is the gold standard, especially with significant endosteal scalloping and risk of cortical breakthrough.
Question 3:
A 68-year-old man presents with progressive difficulty buttoning his shirts and a wide-based, unsteady gait. He denies neck pain but notes occasional shock-like sensations radiating down his spine with neck flexion. On physical examination, tapping the distal phalanx of the middle finger results in spontaneous flexion of the thumb and index finger. Which of the following examination findings is considered the most specific for his likely diagnosis?
Options:
- Lhermitte's sign
- Hoffmann reflex
- Inverted brachioradialis reflex
- Sustained ankle clonus
- Babinski sign
Correct Answer: Inverted brachioradialis reflex
Explanation:
The patient's presentation is highly suspicious for cervical spondylotic myelopathy (CSM). He demonstrates a positive Hoffmann reflex and Lhermitte's sign. While the Hoffmann reflex is highly sensitive for upper motor neuron pathology in the cervical spine, it is not highly specific and can be present in asymptomatic individuals. The inverted brachioradialis reflex (striking the brachioradialis tendon produces finger flexion rather than elbow flexion/supination) is highly specific for cervical myelopathy at the C5-C6 level and indicates a combined upper and lower motor neuron lesion at that specific segment.
Question 4:
To reduce wear rates in total hip arthroplasty, highly cross-linked polyethylene (HXLPE) was developed. However, the process of irradiation creates free radicals that can lead to long-term oxidation and material degradation. Which of the following manufacturing processes is specifically utilized to neutralize or eliminate these free radicals without requiring post-irradiation thermal treatment (melting or annealing)?
Options:
- Gamma irradiation in an inert argon environment
- Ethylene oxide gas sterilization
- Blending or diffusing with Vitamin E (alpha-tocopherol)
- Cold drawing of the ultra-high molecular weight polyethylene
- Addition of barium sulfate to the polymer matrix
Correct Answer: Blending or diffusing with Vitamin E (alpha-tocopherol)
Explanation:
Irradiation of UHMWPE creates cross-links that improve wear resistance but also generates free radicals that predispose the material to oxidation. Historically, thermal treatments like remelting or annealing were used to quench these free radicals, but remelting reduces mechanical strength. The addition of Vitamin E (alpha-tocopherol) acts as an antioxidant, quenching free radicals without the need for thermal treatment, thereby preserving the material's mechanical properties while preventing oxidative degradation.
Question 5:
A 22-year-old female soccer player undergoes primary anterior cruciate ligament (ACL) reconstruction. The surgeon discusses autograft choices. Compared to a bone-patellar tendon-bone (BTB) autograft, the use of a multi-stranded hamstring autograft is statistically associated with a higher risk of which of the following postoperative outcomes?
Options:
- Anterior knee pain during kneeling
- Patellar fracture
- Postoperative extension deficit
- Increased laxity on instrumented testing
- Contralateral ACL rupture
Correct Answer: Increased laxity on instrumented testing
Explanation:
Multiple level I studies and meta-analyses comparing BTB and hamstring autografts for ACL reconstruction have shown that hamstring grafts are associated with slightly increased laxity on instrumented testing (e.g., KT-1000) and a higher theoretical risk of graft rupture in young, high-demand female athletes. BTB autografts have higher rates of donor-site morbidity, particularly anterior knee pain, kneeling pain, and a small risk of patellar fracture. Extension deficits are also slightly more common with BTB grafts.
Question 6:
A 35-year-old carpenter lacerates his index finger with a utility knife, sustaining a Zone II injury to the flexor digitorum profundus (FDP) and superficialis (FDS) tendons. A primary multi-strand core suture repair is planned. Which of the following factors is most significantly responsible for increasing the work of flexion and gliding resistance following this repair?
Options:
- Use of a 4-strand repair instead of a 2-strand repair
- Epitendinous suture placement
- Increased cross-sectional bulk of the repair site
- Venting of the A4 pulley
- Excision of one slip of the FDS tendon
Correct Answer: Increased cross-sectional bulk of the repair site
Explanation:
The most significant factor affecting the work of flexion and gliding resistance after flexor tendon repair is the increased cross-sectional bulk (volume) of the repaired tendon. Increased bulk causes friction and impingement as the tendon attempts to glide under the intact annular pulleys (A2 and A4). While multi-strand repairs (4-strand, 6-strand) increase tensile strength, if they are not performed meticulously, they can increase tendon bulk. An epitendinous suture actually reduces gliding resistance by smoothing the repair site. Venting pulleys or excising an FDS slip generally decreases resistance.
Question 7:
A 28-year-old male sustains a low-energy twisting injury to his midfoot. Initial weight-bearing radiographs show a subtle 2 mm widening between the base of the first and second metatarsals. If this Lisfranc injury is missed and goes untreated, which muscle acts as the primary deforming force leading to dorsal displacement of the first metatarsal?
Options:
- Peroneus longus
- Tibialis anterior
- Extensor hallucis longus
- Tibialis posterior
- Peroneus brevis
Correct Answer: Tibialis anterior
Explanation:
In a Lisfranc injury, the critical ligamentous disruption occurs between the medial cuneiform and the base of the second metatarsal. The tibialis anterior inserts onto the medial cuneiform and the base of the first metatarsal. Its unantagonized pull in the setting of instability acts as a primary deforming force, pulling the first metatarsal and medial cuneiform dorsally and medially. The peroneus longus, which inserts plantarly on the lateral aspect of the first metatarsal base and medial cuneiform, exerts a plantar and lateral force.
Question 8:
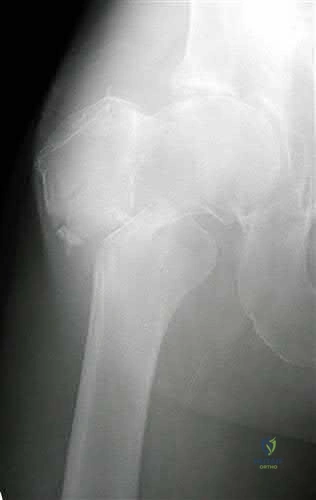
A 13-year-old boy with a BMI in the 95th percentile presents with a 2-month history of vague left knee and thigh pain. On physical examination, he has an obligate external rotation of the left hip with passive hip flexion. Radiographs confirm a slipped capital femoral epiphysis (SCFE). Which of the following best describes the anatomic displacement of the femoral metaphysis relative to the epiphysis in this condition?
Options:
- Metaphysis displaces posterior and inferior
- Metaphysis displaces anterior and superior
- Metaphysis displaces posterior and superior
- Metaphysis displaces anterior and inferior
- Metaphysis displaces directly medial
Correct Answer: Metaphysis displaces anterior and superior
Explanation:
In Slipped Capital Femoral Epiphysis (SCFE), the proximal femoral epiphysis remains relatively secure in the acetabulum while the femoral neck (metaphysis) displaces. Because the mechanical axis of weight-bearing forces acts anteriorly and superiorly on the proximal femur, the metaphysis translates anteriorly and superiorly. Clinically and radiographically, this makes the epiphysis appear to have slipped posteriorly and inferiorly relative to the neck. Therefore, the metaphysis moves anteriorly and superiorly.
Question 9:
A 60-year-old woman undergoes volar locked plating for a comminuted, dorsally angulated distal radius fracture. Six weeks postoperatively, she suddenly loses the ability to actively extend her thumb interphalangeal joint. Rupture of the extensor pollicis longus (EPL) tendon in this scenario is most directly associated with which iatrogenic factor?
Options:
- Plate placement distal to the volar watershed line
- Over-distraction of the radiocarpal joint during reduction
- Prominent screw tips penetrating the dorsal cortex
- Use of a tourniquet for greater than 120 minutes
- Failure to repair the pronator quadratus
Correct Answer: Prominent screw tips penetrating the dorsal cortex
Explanation:
EPL tendon rupture after volar locked plating of a distal radius fracture is most commonly caused by attrition from prominent screw tips penetrating the dorsal cortex. The EPL runs in the 3rd dorsal compartment, closely apposed to the dorsal cortex of the distal radius, making it highly vulnerable to protruding dorsal screws. Conversely, rupture of the flexor pollicis longus (FPL) tendon on the volar side is associated with prominent hardware placed distal to the volar watershed line.
Question 10:
A 62-year-old man who underwent a primary ceramic-on-ceramic total hip arthroplasty two years ago presents with an audible 'squeaking' from his hip during normal ambulation. Radiographs show well-fixed components. Which of the following factors is most highly correlated with the development of squeaking in ceramic-on-ceramic bearings?
Options:
- Acetabular component placed in excessive anteversion and high inclination
- Decreased femoral offset
- Use of a 36-mm head instead of a 28-mm head
- Acetabular retroversion combined with a varus femoral stem
- Micro-motion of the uncemented femoral stem
Correct Answer: Acetabular component placed in excessive anteversion and high inclination
Explanation:
Squeaking in ceramic-on-ceramic total hip arthroplasties is a well-documented phenomenon. It is most strongly associated with component malposition, specifically high acetabular inclination (abduction) and excessive anteversion. This malposition leads to 'edge loading,' where the mechanical contact forces are concentrated on the rim of the ceramic liner. Edge loading disrupts the fluid film lubrication, resulting in stripe wear, increased friction, and the generation of an audible squeak.
Question 11:
You are evaluating a 14-year-old female with Adolescent Idiopathic Scoliosis (AIS) to determine surgical fusion levels. According to the Lenke classification system, a proximal thoracic curve is defined as 'structural' (and thus typically requires inclusion in the fusion construct) if the Cobb angle on side-bending radiographs is at least:
Options:
- 10 degrees
- 15 degrees
- 20 degrees
- 25 degrees
- 30 degrees
Correct Answer: 25 degrees
Explanation:
In the Lenke classification for adolescent idiopathic scoliosis, a minor curve is considered 'structural' if it does not bend out to less than 25 degrees on coronal side-bending radiographs, or if there is kyphosis of at least +20 degrees across the regional segments. Identifying structural minor curves is critical, as the general rule is to include all structural curves in the fusion construct.
Question 12:
A 32-year-old female presents with knee pain. Radiographs reveal an eccentric, expansile, purely lytic lesion in the distal femoral epiphysis extending to the subchondral bone. Biopsy shows multinucleated giant cells interspersed among mononuclear spindle cells. In the pathogenesis of this tumor, the neoplastic mononuclear cells overexpress a specific surface molecule that drives the recruitment and differentiation of the reactive giant cells. Which of the following is that molecule?
Options:
- RANK
- RANKL (Receptor Activator of Nuclear Factor Kappa-B Ligand)
- Osteoprotegerin (OPG)
- Vascular Endothelial Growth Factor (VEGF)
- Fibroblast Growth Factor Receptor 3 (FGFR3)
Correct Answer: RANKL (Receptor Activator of Nuclear Factor Kappa-B Ligand)
Explanation:
The clinical picture describes a Giant Cell Tumor (GCT) of bone. The true neoplastic cells in a GCT are the spindle-shaped mononuclear stromal cells. These cells highly express RANKL (Receptor Activator of Nuclear Factor Kappa-B Ligand). RANKL binds to the RANK receptor found on the surface of normal circulating monocyte/macrophage precursors, driving them to fuse and form the prominent, reactive osteoclast-like multinucleated giant cells that cause the extensive osteolysis. This pathway is the target of the monoclonal antibody Denosumab.
Question 13:
Articular cartilage relies on a highly organized extracellular matrix for its biomechanical properties. In which specific histologic zone of normal hyaline articular cartilage are the collagen fibers oriented primarily perpendicular to the articular surface, and the chondrocytes arranged in distinct vertical columns?
Options:
- Superficial (tangential) zone
- Middle (transitional) zone
- Deep (radial) zone
- Calcified zone
- Tidemark
Correct Answer: Deep (radial) zone
Explanation:
Articular cartilage is divided into four main zones. In the superficial (tangential) zone, collagen fibers are parallel to the joint surface to resist shear forces. In the middle (transitional) zone, collagen fibers are randomly oriented. In the deep (radial) zone, collagen fibers are oriented perpendicular to the joint surface and chondrocytes are arranged in vertical columns, providing high resistance to compressive forces. The tidemark separates the deep zone from the calcified zone.
Question 14:
A 35-year-old man sustains a high-energy Pauwels Type III (vertical shear) femoral neck fracture. To maximize biomechanical stability and minimize the risk of varus collapse during internal fixation, current biomechanical literature suggests which of the following constructs provides the highest resistance to shear forces?
Options:
- Three parallel cancellous screws in an inverted triangle configuration
- Three parallel cancellous screws in a standard triangle configuration
- A sliding hip screw (SHS) construct combined with a partially threaded derotational cancellous screw
- Two parallel fully threaded cortical screws
- A single large-diameter, partially threaded cancellous screw
Correct Answer: A sliding hip screw (SHS) construct combined with a partially threaded derotational cancellous screw
Explanation:
Pauwels Type III femoral neck fractures have a fracture line greater than 50 degrees from the horizontal, subjecting the fracture to extreme shear forces and a high risk of varus collapse, nonunion, and AVN. Biomechanical studies consistently show that a fixed-angle device, such as a sliding hip screw (SHS), combined with a derotational screw, provides superior resistance to vertical shear and varus collapse compared to multiple cancellous screws alone in young adults.
Question 15:
A 45-year-old man presents with numbness in his small and ring fingers and intrinsic muscle weakness. Physical examination reveals a 'claw' posture of the ring and small fingers. Which of the following clinical findings would best differentiate a high ulnar nerve compression (cubital tunnel syndrome) from a low ulnar nerve compression (Guyon's canal syndrome)?
Options:
- A positive Froment's sign
- Weakness of the dorsal interossei
- A positive Wartenberg's sign
- Less pronounced clawing of the ring and small fingers (ulnar paradox)
- Preservation of two-point discrimination on the volar tip of the small finger
Correct Answer: Less pronounced clawing of the ring and small fingers (ulnar paradox)
Explanation:
The 'ulnar paradox' refers to the phenomenon where a higher ulnar nerve lesion (at the elbow) results in a less pronounced claw deformity compared to a lower lesion (at the wrist). This occurs because a high lesion paralyzes the ulnar-innervated half of the flexor digitorum profundus (FDP) to the ring and small fingers, reducing the flexion force at the DIP joints. In a low lesion, the FDP is intact and forcefully flexes the DIP joints against the paralyzed intrinsics, creating a severe claw. Additionally, loss of sensation over the dorsal ulnar aspect of the hand indicates a lesion proximal to the wrist, as the dorsal sensory branch of the ulnar nerve branches off proximal to Guyon's canal.
Question 16:
A 42-year-old recreational basketball player feels a 'pop' in his calf and is diagnosed with an acute Achilles tendon rupture. He is considering non-operative management versus open surgical repair. Based on recent Level I evidence comparing non-operative management utilizing an early functional rehabilitation protocol to surgical repair, non-operative management is associated with:
Options:
- A significantly higher rerupture rate
- A significantly lower rate of return to sports
- Equivalent rerupture rates but a significantly higher risk of sural nerve injury
- Equivalent rerupture rates and a lower rate of soft-tissue and wound complications
- A 50% decrease in peak plantarflexion strength at 2-year follow-up
Correct Answer: Equivalent rerupture rates and a lower rate of soft-tissue and wound complications
Explanation:
Historically, non-operative management of Achilles tendon ruptures with prolonged cast immobilization resulted in higher rerupture rates. However, modern Level I trials (e.g., Willits et al.) utilizing early functional rehabilitation (weight-bearing in a functional brace with early range of motion) demonstrate that non-operative management yields rerupture rates equivalent to surgical repair, while entirely avoiding surgical complications such as wound breakdown, infection, and iatrogenic nerve injury.
Question 17:
A 6-month-old female with Developmental Dysplasia of the Hip (DDH) fails initial Pavlik harness treatment. She undergoes closed reduction and application of a hip spica cast under general anesthesia. To minimize the risk of iatrogenic avascular necrosis (AVN) of the femoral head, the hip should be immobilized in the 'human position'. What specific joint angles correspond to this position?
Options:
- Greater than 110 degrees of flexion and maximal abduction
- 90 to 100 degrees of flexion and less than 60 degrees of abduction
- Neutral flexion/extension and 45 degrees of abduction
- 45 degrees of flexion and maximal external rotation
- 120 degrees of flexion and 90 degrees of abduction
Correct Answer: 90 to 100 degrees of flexion and less than 60 degrees of abduction
Explanation:
The 'human position' for spica casting in DDH entails positioning the hip in approximately 90 to 100 degrees of flexion and moderate abduction (usually 45 to 60 degrees). Immobilizing the hip in extreme, forced abduction (the 'frog-leg' position, >60 degrees abduction) dramatically increases the risk of avascular necrosis (AVN) of the femoral head by compressing the extraosseous epiphyseal vessels against the acetabular margin.
Question 18:
During a posterior-stabilized total knee arthroplasty (TKA), after the bony cuts are made and trial components are placed, the surgeon evaluates the gaps. The knee is stable and symmetric in full extension, but in 90 degrees of flexion, the joint is symmetrically tight, making it difficult to insert the trial polyethylene insert. Utilizing an anterior referencing system, what is the most appropriate next step to balance the knee?
Options:
- Resect 2 mm more of the distal femur
- Upsize the femoral component
- Downsize the femoral component
- Increase the thickness of the tibial polyethylene insert
- Release the superficial medial collateral ligament
Correct Answer: Downsize the femoral component
Explanation:
A knee that is balanced in extension but tight in flexion requires an increase in the flexion gap without altering the extension gap. When using an anterior referencing system, the anterior cut remains flush with the anterior cortex. Downsizing the femoral component reduces the anterior-posterior (AP) dimension, which brings the posterior cut further anteriorly, thereby reducing posterior condylar offset and opening (enlarging) the flexion gap. Resecting more distal femur would increase the extension gap. Upsizing the femur would make it tighter in flexion.
Question 19:
The Lower Extremity Assessment Project (LEAP) study investigated outcomes in patients with severe lower extremity trauma, including high-grade open tibial shaft fractures. The study compared limb salvage versus early amputation. Which of the following factors was found to be the most significant predictor of poor long-term clinical and functional outcomes in these patients?
Options:
- The initial Gustilo-Anderson classification
- The choice between limb salvage versus primary amputation
- The specific type of soft tissue flap used for coverage
- Low socioeconomic status and lack of continuous health insurance
- The delay to definitive bony fixation beyond 48 hours
Correct Answer: Low socioeconomic status and lack of continuous health insurance
Explanation:
A hallmark finding of the landmark LEAP study was that socioeconomic and psychosocial factors, rather than the initial injury severity or the surgical decision (limb salvage vs. amputation), were the strongest predictors of long-term functional outcome. Factors such as low socioeconomic status, lack of continuous health insurance, poor social support, smoking, and lower educational levels correlated highly with poor outcomes and failure to return to work.
Question 20:
A 22-year-old rugby player with recurrent anterior shoulder instability and 25% glenoid bone loss undergoes a Latarjet procedure. This procedure restores stability through a described 'triple-blocking' effect. Which of the following mechanisms is considered the most significant dynamic contributor to anterior stability in the Latarjet procedure?
Options:
- The static bony block extending the glenoid articular arc
- The sling effect of the conjoined tendon reinforcing the inferior capsule and subscapularis when the arm is abducted and externally rotated
- The repair of the native capsule to the coracoacromial ligament stump
- The dynamic tensioning of the long head of the biceps brachii
- The tenodesis of the subscapularis directly to the anterior labrum
Correct Answer: The sling effect of the conjoined tendon reinforcing the inferior capsule and subscapularis when the arm is abducted and externally rotated
Explanation:
The Latarjet procedure provides a 'triple-blocking' effect for anterior shoulder instability. The three components are: 1) The dynamic 'sling' effect of the conjoined tendon across the inferior subscapularis and anterior capsule when the arm is abducted and externally rotated; 2) The static bony effect of the coracoid bone block increasing the glenoid arc; and 3) The capsular repair (capsule sutured to the CA ligament stump). Biomechanical studies have demonstrated that the dynamic sling effect of the conjoined tendon contributes most significantly to the stability provided by the construct, accounting for up to 75% of the stabilizing force.
Question 21:
Which of the following best describes the normal kinematics of the native knee that modern total knee arthroplasty (TKA) designs attempt to replicate?
Options:
- Femoral rollback with internal rotation of the tibia during flexion
- Femoral rollback with external rotation of the tibia during flexion
- Anterior femoral translation with tibial internal rotation during flexion
- Paradoxical anterior sliding of the femur during deep flexion
- Pure hinge motion with a single radius of curvature
Correct Answer: Femoral rollback with internal rotation of the tibia during flexion
Explanation:
Normal knee kinematics involve a 'screw-home' mechanism and 'femoral rollback'. As the knee goes from extension into flexion, the lateral femoral condyle rolls posteriorly more than the medial condyle, causing the femur to externally rotate relative to the tibia (or the tibia to internally rotate relative to the femur). Modern TKA designs, particularly posterior-stabilized or medial-pivot designs, attempt to recreate this native femoral rollback and tibial internal rotation to optimize flexion and patellar tracking.
Question 22:
A 55-year-old active male presents with an audible squeak from his total hip arthroplasty, performed 4 years ago for osteoarthritis. He has a ceramic-on-ceramic bearing. Which of the following factors is most strongly associated with the development of this acoustic phenomenon?
Options:
- Femoral stem retroversion
- Edge loading due to acetabular component malpositioning
- Use of an oxidized zirconium femoral head
- Low body mass index (BMI)
- Polyethylene oxidation
Correct Answer: Edge loading due to acetabular component malpositioning
Explanation:
Squeaking in a ceramic-on-ceramic (CoC) total hip arthroplasty is a well-documented phenomenon. It is most strongly associated with edge loading of the bearing surfaces, which typically occurs due to acetabular cup malpositioning (especially excessive abduction or anteversion). Edge loading leads to stripe wear and loss of fluid-film lubrication, culminating in the acoustic squeak. High BMI and younger, more active patients are also at higher risk, whereas oxidized zirconium and polyethylene are distinct bearing materials not associated with the classic CoC squeak.
Question 23:
A 35-year-old male presents after a high-speed motor vehicle collision. Radiographs show a traumatic spondylolisthesis of the axis with severe angulation and minimal translation. The fracture line is oblique. According to the Levine and Edwards classification (Type IIA), what is the most critical management principle during initial stabilization?
Options:
- Immediate application of heavy cervical traction to reduce angulation
- Avoidance of cervical traction and use of a halo vest with mild compression
- Immediate C1-C2 transarticular screw fixation
- Anterior odontoid screw fixation
- Application of a hard cervical collar alone
Correct Answer: Avoidance of cervical traction and use of a halo vest with mild compression
Explanation:
A Levine and Edwards Type IIA Hangman's fracture is characterized by severe angulation with minimal translation and an oblique fracture line. The mechanism of injury is flexion-distraction. Because the anterior longitudinal ligament and the C2-C3 disc are completely disrupted, applying cervical traction is strictly contraindicated as it will distract the fracture site and worsen the deformity. The correct treatment is gentle reduction in extension with mild compression, followed by immobilization in a halo vest.
Question 24:
A 65-year-old male with type II diabetes presents with progressive stiffness of his thoracic and lumbar spine. Radiographs demonstrate flowing ossification along the anterolateral aspect of four contiguous vertebral bodies. The sacroiliac joints are preserved, and disc heights are relatively normal. What is the most common metabolic abnormality associated with this condition?
Options:
- HLA-B27 positivity
- Elevated serum uric acid
- Hyperinsulinemia
- Hypocalcemia
- Elevated alkaline phosphatase
Correct Answer: Hyperinsulinemia
Explanation:
The clinical and radiographic presentation is classic for Diffuse Idiopathic Skeletal Hyperostosis (DISH), characterized by flowing ossification of at least four contiguous vertebral bodies with preserved disc height and absent sacroiliitis. DISH is strongly associated with metabolic syndrome, type II diabetes mellitus, obesity, and specifically hyperinsulinemia, which is believed to stimulate osteoblast proliferation and bone formation.
Question 25:
During a double-bundle posterior cruciate ligament (PCL) reconstruction, the surgeon aims to accurately recreate the native anatomy. Which of the following accurately describes the tensioning protocol for the two distinct bundles?
Options:
- The anterolateral bundle is tensioned in full extension, while the posteromedial bundle is tensioned in 90 degrees of flexion.
- The anterolateral bundle is tensioned in 90 degrees of flexion, while the posteromedial bundle is tensioned in full extension.
- Both bundles are tensioned simultaneously in 90 degrees of flexion.
- Both bundles are tensioned simultaneously in full extension.
- The anterolateral bundle is tensioned in 45 degrees of flexion, while the posteromedial bundle is tensioned in 90 degrees of flexion.
Correct Answer: The anterolateral bundle is tensioned in 90 degrees of flexion, while the posteromedial bundle is tensioned in full extension.
Explanation:
The native PCL consists of two main bundles: the anterolateral (AL) bundle and the posteromedial (PM) bundle. The AL bundle is larger and provides primary restraint to posterior tibial translation in flexion; thus, it is tensioned and fixed at 90 degrees of flexion. The PM bundle is smaller and is tight in extension; therefore, it is tensioned and fixed at 0 to 30 degrees of flexion (near full extension).
Question 26:
A 22-year-old professional baseball pitcher presents with posterior shoulder pain during the late cocking phase of throwing. Physical examination reveals a loss of internal rotation of 25 degrees compared to the contralateral side. MRI demonstrates articular-sided fraying of the posterior supraspinatus and an intact anterior capsule. What is the primary pathophysiologic mechanism driving this condition?
Options:
- Subcoracoid impingement
- Subacromial abrasion
- Anterior capsular contracture
- Posteroinferior capsular contracture
- Congenital glenoid retroversion
Correct Answer: Posteroinferior capsular contracture
Explanation:
The scenario describes internal impingement of the shoulder, common in overhead athletes. The hallmark is Glenohumeral Internal Rotation Deficit (GIRD). The primary driver is a thickened, contracted posteroinferior capsule resulting from repetitive eccentric loading during the deceleration phase of throwing. This contracture shifts the glenohumeral contact point posterosuperiorly when the arm is in maximum abduction and external rotation (late cocking phase), causing the undersurface of the rotator cuff to impinge between the greater tuberosity and the posterosuperior glenoid labrum.
Question 27:
A 45-year-old male sustains a severe Schatzker VI tibial plateau fracture with a large posteromedial coronal shear fragment. The surgeon plans a dual-incision approach. Which of the following structures lies in closest proximity to the surgical interval utilized for the posteromedial approach to the tibia?
Options:
- Common peroneal nerve
- Saphenous nerve
- Anterior tibial artery
- Popliteal artery
- Sural nerve
Correct Answer: Saphenous nerve
Explanation:
The posteromedial approach to the tibial plateau typically utilizes the internervous interval between the medial border of the tibia/pes anserinus and the medial head of the gastrocnemius. The saphenous nerve and the great saphenous vein run superficially along the medial aspect of the proximal tibia and must be identified and protected during the superficial dissection. The common peroneal nerve is lateral, and the popliteal artery is posterior, protected by the bulk of the gastrocnemius during this specific approach.
Question 28:
In the surgical management of a vertically oriented, displaced femoral neck fracture (Pauwels Type III) in a 30-year-old patient, which of the following internal fixation constructs provides the highest resistance to vertical shear forces and minimizes the risk of varus collapse?
Options:
- Three parallel cancellous screws placed in an inverted triangle
- Three parallel cancellous screws placed in a triangle with apex distal
- A dynamic hip screw (DHS) with an anti-rotation screw
- Two fully threaded 7.3mm screws placed parallel to the calcar
- A single lag screw cephomedullary nail
Correct Answer: A dynamic hip screw (DHS) with an anti-rotation screw
Explanation:
Pauwels Type III femoral neck fractures have a high vertical angle (>50 degrees), creating extreme shear forces across the fracture site. Multiple biomechanical studies have demonstrated that a fixed-angle construct, such as a Dynamic Hip Screw (DHS) combined with an anti-rotation screw, provides superior biomechanical stability and higher resistance to shear forces and varus collapse compared to multiple cancellous screws in young adults with vertically oriented femoral neck fractures.
Question 29:
A 12-year-old obese male presents with left knee pain and an obligate external rotation of the left hip upon flexion. Radiographs confirm a severe, unstable left slipped capital femoral epiphysis (SCFE). Which of the following is an established indication for prophylactic in situ pinning of the contralateral, asymptomatic hip?
Options:
- Patient age > 14 years at presentation
- Presence of an endocrine disorder such as hypothyroidism
- Unstable SCFE on the ipsilateral side regardless of age
- Presentation with a slipped angle > 60 degrees
- Body Mass Index > 30
Correct Answer: Presence of an endocrine disorder such as hypothyroidism
Explanation:
Prophylactic pinning of the contralateral hip in SCFE is controversial but is strongly indicated in certain high-risk populations. These include patients with underlying endocrinopathies (e.g., hypothyroidism, growth hormone deficiency, renal osteodystrophy), metabolic disorders, or those who present at an atypically young age (females < 10 years, males < 12 years). Severe slips or unstable slips alone, or obesity, do not mandate prophylactic pinning without careful consideration of the risks.
Question 30:
A 2-week-old infant is being treated for idiopathic congenital talipes equinovarus using the Ponseti method. According to the CAVE sequence, which deformity is corrected first, and what is the specific manipulation required to achieve this correction?
Options:
- Cavus, corrected by elevating the first ray to supinate the forefoot and align it with the hindfoot.
- Adduction, corrected by stretching the medial column and pushing against the calcaneocuboid joint.
- Varus, corrected by directly everting the calcaneus.
- Equinus, corrected by a percutaneous Achilles tenotomy during the first casting session.
- Cavus, corrected by depressing the first ray to pronate the forefoot.
Correct Answer: Cavus, corrected by elevating the first ray to supinate the forefoot and align it with the hindfoot.
Explanation:
The Ponseti method follows the CAVE sequence: Cavus, Adductus, Varus, Equinus. The cavus deformity is the first to be addressed. It is driven by relative pronation of the forefoot in relation to the hindfoot. Correction is achieved by elevating the first ray, effectively supinating the forefoot to align it with the hindfoot. Subsequent casts correct adductus and varus simultaneously by abducting the foot around the head of the talus, and equinus is corrected last (often requiring a percutaneous Achilles tenotomy).
Question 31:
A 42-year-old construction worker presents with chronic wrist pain. Radiographs reveal a scaphoid nonunion with advanced radioscaphoid and capitolunate arthritis, but the radiolunate articulation is completely preserved. Which of the following surgical interventions is most appropriate for this stage of Scaphoid Nonunion Advanced Collapse (SNAC)?
Options:
- Proximal row carpectomy (PRC)
- Four-corner arthrodesis with scaphoid excision
- Total wrist arthrodesis
- Scaphoid open reduction and internal fixation with vascularized bone grafting
- Radial styloidectomy
Correct Answer: Four-corner arthrodesis with scaphoid excision
Explanation:
This patient has Stage III SNAC wrist (involvement of the radioscaphoid and capitolunate joints). Because the radiolunate joint is preserved (a hallmark of SNAC and SLAC wrists due to the spherical congruency of the lunate fossa), a motion-preserving salvage procedure is indicated. However, Proximal Row Carpectomy (PRC) is contraindicated in Stage III disease because the capitate head is arthritic and would articulate directly with the lunate fossa. Therefore, four-corner arthrodesis with scaphoid excision is the most appropriate treatment.
Question 32:
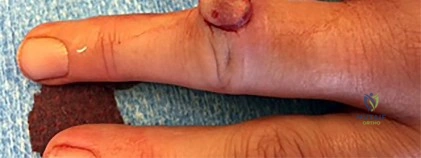
In a complete rupture of the ulnar collateral ligament (UCL) of the thumb metacarpophalangeal joint (Skier's thumb), a Stener lesion prevents non-operative healing. This lesion occurs when the torn ends of the UCL are separated by the aponeurosis of which of the following muscles?
Options:
- Abductor pollicis brevis
- Adductor pollicis
- Flexor pollicis brevis
- Extensor pollicis longus
- First dorsal interosseous
Correct Answer: Adductor pollicis
Explanation:
A Stener lesion occurs when the distal attachment of the ulnar collateral ligament (UCL) is avulsed from the proximal phalanx of the thumb and flips proximally and superficially to the adductor pollicis aponeurosis. The aponeurosis becomes interposed between the torn ends of the ligament, preventing anatomical healing and thus serving as an absolute indication for surgical repair.
Question 33:
A 56-year-old male with poorly controlled diabetes presents with a swollen, erythematous, and warm right foot. Radiographs demonstrate fragmentation, bone debris, and periarticular subluxation at the tarsometatarsal joints. According to the Eichenholtz classification, this patient is in the Development stage (Stage I) of Charcot arthropathy. What is the primary pathophysiological process mediating the acute bone destruction in this phase?
Options:
- Avascular necrosis of the metatarsal heads due to microangiopathy
- Intense osteoclastic resorption mediated by pro-inflammatory cytokines and RANKL
- Dense fibrous tissue proliferation and sclerosis surrounding the joint
- Osteoblastic woven bone formation across the joint spaces
- Subintimal synovial hyperplasia with pannus formation
Correct Answer: Intense osteoclastic resorption mediated by pro-inflammatory cytokines and RANKL
Explanation:
Acute Charcot neuroarthropathy (Eichenholtz Stage I / Development phase) is characterized by an exaggerated inflammatory response. The loss of sympathetic regulation leads to bounding pulses (neurotraumatic theory) and a massive release of pro-inflammatory cytokines (TNF-α, IL-1). These cytokines upregulate the RANKL pathway, leading to intense, uncontrolled osteoclastic bone resorption, which causes the severe fragmentation, osteopenia, and destruction seen on radiographs. Avascular necrosis, fibrous sclerosis, and pannus do not define the acute Charcot phase.
Question 34:
During surgical reconstruction of a subtle Lisfranc injury in a collegiate athlete, the surgeon must address the critical Lisfranc ligament complex. Which of the following accurately describes the anatomic orientation of the proper (intra-osseous) Lisfranc ligament?
Options:
- It connects the medial cuneiform to the base of the first metatarsal.
- It connects the medial cuneiform to the base of the second metatarsal.
- It connects the middle cuneiform to the base of the second metatarsal.
- It connects the lateral cuneiform to the base of the third metatarsal.
- It connects the base of the first metatarsal to the base of the second metatarsal.
Correct Answer: It connects the medial cuneiform to the base of the second metatarsal.
Explanation:
The Lisfranc ligament is an intra-osseous ligament that connects the lateral aspect of the medial cuneiform to the medial base of the second metatarsal. It is the largest and strongest ligament of the Lisfranc complex and is crucial for stabilizing the tarsometatarsal joint, particularly because there is no direct transverse ligament connecting the first and second metatarsal bases.
Question 35:
A 15-year-old male undergoes surgical resection of a conventional osteosarcoma of the distal femur following a 10-week course of neoadjuvant chemotherapy. According to the Huvos grading system, which of the following histologic findings in the resected specimen represents the most significant prognostic factor for long-term survival?
Options:
- Presence of a dense chondroblastic matrix
- Greater than 90% tumor necrosis
- Complete absence of mitotic figures in the remaining viable tumor
- Tumor encapsulation by a thick periosteal shell
- Less than 10% cortical breakthrough
Correct Answer: Greater than 90% tumor necrosis
Explanation:
The most important prognostic factor for overall survival in patients with conventional high-grade osteosarcoma is the histologic response to neoadjuvant chemotherapy. A "good response," defined by the Huvos grading system as greater than 90% tumor necrosis (Grade III or IV), correlates with a significantly improved prognosis and long-term survival.
Question 36:
A 60-year-old male presents with a large, destructive mass in the right ilium. CT scan reveals a lytic lesion with intralesional 'rings and arcs' calcification. Core needle biopsy confirms a Grade II conventional chondrosarcoma. Which of the following is the most appropriate treatment strategy?
Options:
- Wide surgical excision alone
- Intralesional curettage with adjuvant cryotherapy
- Neoadjuvant chemotherapy followed by wide surgical excision
- Wide surgical excision followed by external beam radiation therapy
- Primary radiation therapy
Correct Answer: Wide surgical excision alone
Explanation:
Conventional chondrosarcomas are notoriously resistant to both chemotherapy and radiation therapy due to their poor vascularity, slow growth, and high extracellular matrix content. Intermediate (Grade II) and high-grade (Grade III) chondrosarcomas of the pelvis require wide surgical excision with negative margins as the definitive treatment. Intralesional curettage is reserved for benign or low-grade (Grade I) cartilaginous tumors in the appendicular skeleton.
Question 37:
Articular cartilage relies on a highly organized extracellular matrix to resist compressive and shear forces. In the superficial (tangential) zone of articular cartilage, what is the primary orientation of the Type II collagen fibrils and the relative proteoglycan content compared to the deeper zones?
Options:
- Collagen fibrils are parallel to the joint surface; proteoglycan content is lowest.
- Collagen fibrils are perpendicular to the joint surface; proteoglycan content is lowest.
- Collagen fibrils are parallel to the joint surface; proteoglycan content is highest.
- Collagen fibrils are perpendicular to the joint surface; proteoglycan content is highest.
- Collagen fibrils are randomly oriented; proteoglycan content is uniform throughout.
Correct Answer: Collagen fibrils are parallel to the joint surface; proteoglycan content is lowest.
Explanation:
Articular cartilage is divided into zones. In the superficial (tangential) zone, Type II collagen fibrils are aligned parallel to the joint surface to resist shear forces. This zone has the highest water content but the lowest proteoglycan concentration. Conversely, the deep zone has collagen fibrils aligned perpendicular to the subchondral bone, highest proteoglycan content, and lowest water content, optimizing resistance to compressive loads.
Question 38:
Bone morphogenetic proteins (BMPs), particularly recombinant human BMP-2 and BMP-7, are utilized in orthopedic surgery to promote osteoinduction and bone healing. These signaling molecules exert their cellular effects primarily through which of the following intracellular signaling pathways?
Options:
- Wnt/β-catenin pathway
- JAK/STAT signaling pathway
- MAPK/ERK pathway
- Serine/threonine kinase receptors and Smad proteins
- Tyrosine kinase receptors and the Ras/Raf pathway
Correct Answer: Serine/threonine kinase receptors and Smad proteins
Explanation:
BMPs belong to the Transforming Growth Factor-beta (TGF-β) superfamily. They bind to cell surface type I and type II serine/threonine kinase receptors. Upon activation, these receptors phosphorylate intracellular Smad proteins (specifically R-Smads 1, 5, and 8), which then form a complex with Smad4. This complex translocates to the nucleus to regulate transcription of osteogenic genes (e.g., Runx2, Osterix).
Question 39:
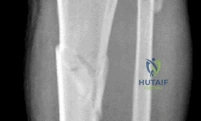
A 28-year-old male is treated with intramedullary nailing for a closed, comminuted midshaft tibial fracture. Twelve hours post-operatively, he complains of severe leg pain out of proportion to the injury, unrelieved by intravenous opioids. Passive stretch of the toes elicits excruciating pain. Compartment pressure monitoring reveals an absolute compartment pressure of 35 mmHg, and his blood pressure is 110/60 mmHg. What is the most appropriate next step in management?
Options:
- Administer a continuous epidural infusion for pain control
- Immediate four-compartment fasciotomy of the leg
- Bivalve the surgical dressing and elevate the leg above the level of the heart
- Continue close observation as the delta pressure is greater than 30 mmHg
- Administer intravenous mannitol
Correct Answer: Immediate four-compartment fasciotomy of the leg
Explanation:
The diagnosis is acute compartment syndrome. The critical threshold for intervention is the delta pressure (Diastolic Blood Pressure - Absolute Compartment Pressure). In this patient, the delta pressure is 60 - 35 = 25 mmHg. A delta pressure of less than 30 mmHg represents inadequate tissue perfusion pressure and is a strict indication for emergent fasciotomy (four-compartment in the leg). Elevating the leg above the level of the heart is contraindicated as it further decreases arterial inflow and worsens tissue ischemia.
Question 40:
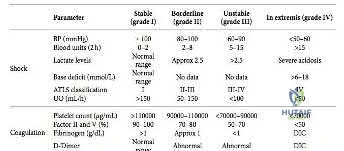
A 35-year-old male is brought to the trauma bay after a motorcycle collision. He is hemodynamically unstable (BP 75/40 mmHg, HR 130 bpm). Pelvic radiographs reveal an Anteroposterior Compression Type III (APC-III) open-book pelvic ring injury with severe symphyseal diastasis. Following the initiation of a massive transfusion protocol, which of the following is the most effective initial mechanical intervention to reduce pelvic volume and control venous hemorrhage?
Options:
- Placement of a supra-acetabular external fixator
- Placement of a pelvic circumferential compression device (binder) centered over the greater trochanters
- Emergent angioembolization of the internal iliac arteries
- Open reduction and internal fixation of the pubic symphysis
- Packing of the preperitoneal space
Correct Answer: Placement of a pelvic circumferential compression device (binder) centered over the greater trochanters
Explanation:
In a hemodynamically unstable patient with an 'open-book' (APC) pelvic ring injury, the initial and most rapid mechanical intervention is the application of a pelvic circumferential compression device (pelvic binder or sheet). It must be centered over the greater trochanters (not the iliac crests) to effectively close the pelvic ring, reduce pelvic volume, and create a tamponade effect for venous bleeding (the most common source of hemorrhage). External fixation, preperitoneal packing, and angioembolization are subsequent steps if the binder and resuscitation fail to stabilize the patient.