Full Question & Answer Text (for Search Engines)
Question 1:
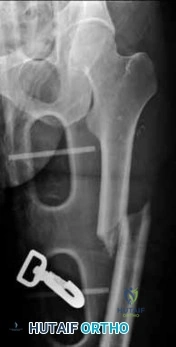
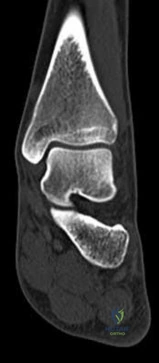
A 12-year-old obese male presents with left thigh pain and a limp. The provided radiograph is shown. He is diagnosed with a Slipped Capital Femoral Epiphysis (SCFE). What is the most widely accepted indication for prophylactic pinning of the contralateral hip?
Options:
- Initial presentation with a severe slip angle > 50 degrees
- Age < 10 for girls or < 12 for boys, or underlying endocrinopathy
- Open triradiate cartilage at the time of presentation
- Positive family history of SCFE in a first-degree relative
- Body Mass Index (BMI) > 99th percentile for age
Correct Answer: Age < 10 for girls or < 12 for boys, or underlying endocrinopathy
Explanation:
Prophylactic pinning of the contralateral hip is generally indicated in patients with metabolic or endocrine disorders (e.g., hypothyroidism, renal osteodystrophy) and in patients presenting at a very young age (girls <10, boys <12) due to a substantially increased risk of a contralateral slip. Recent literature also strongly weights the modified Oxford bone age score.
Question 2:
A 32-year-old male sustains a high-energy trauma. Imaging demonstrates a vertically oriented femoral neck fracture (Pauwels III). Which of the following biomechanical environments is most responsible for the high rate of nonunion and osteonecrosis in this specific fracture pattern?
Options:
- Excessive compressive forces across the fracture site
- High shear stress promoting varus displacement
- Primary distraction at the inferior cortex during weight bearing
- Failure of the implant to allow dynamic sliding
- Interposition of the iliofemoral ligament within the fracture site
Correct Answer: High shear stress promoting varus displacement
Explanation:
Pauwels III femoral neck fractures have a fracture line greater than 50 degrees relative to the horizontal. This vertical orientation changes the physiological loading from compressive forces to high shear forces. This shear stress promotes varus displacement and instability, leading to the known higher risks of nonunion and avascular necrosis in young adults.
Question 3:
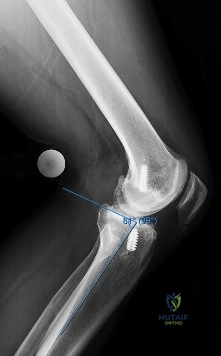
A 15-year-old male presents with worsening knee pain. Radiographs reveal a metaphyseal aggressive bone lesion with a 'sunburst' periosteal reaction and Codman's triangle. Biopsy confirms a high-grade intramedullary osteosarcoma. What is the standard algorithmic approach to treatment for this patient?
Options:
- Wide surgical resection alone
- Neoadjuvant chemotherapy followed by wide surgical resection and adjuvant chemotherapy
- Neoadjuvant radiotherapy followed by wide surgical resection
- Marginal excision followed by adjuvant chemotherapy
- Primary amputation without chemotherapy
Correct Answer: Neoadjuvant chemotherapy followed by wide surgical resection and adjuvant chemotherapy
Explanation:
The standard of care for high-grade classic intramedullary osteosarcoma is neoadjuvant (pre-operative) chemotherapy, followed by wide surgical resection (either limb salvage or amputation), and then adjuvant (post-operative) chemotherapy. The percentage of histologic necrosis seen in the resected specimen after neoadjuvant chemotherapy is one of the strongest prognostic indicators for long-term survival.
Question 4:
In total hip arthroplasty (THA), which of the following bearing surface combinations is known to have the lowest volumetric wear rate, but carries unique risks of catastrophic squeaking and component fracture?
Options:
- Ceramic-on-Ceramic
- Metal-on-Highly Cross-Linked Polyethylene
- Ceramic-on-Highly Cross-Linked Polyethylene
- Metal-on-Metal
- Ceramic-on-Conventional Polyethylene
Correct Answer: Ceramic-on-Ceramic
Explanation:
Ceramic-on-ceramic (CoC) bearings exhibit the lowest volumetric wear rates of any THA bearing surface, often being nearly unmeasurable in vitro. However, CoC bearings are uniquely associated with complications such as squeaking (reported in up to 10% in some series) and the rare but catastrophic fracture of the ceramic components, often due to edge loading, impingement, or material defects.
Question 5:
A 22-year-old female collegiate soccer player requires a revision anterior cruciate ligament (ACL) reconstruction. The surgeon elects to use an irradiated allograft. What irradiation dose threshold is definitively known to significantly alter the biomechanical properties of the allograft, reducing its structural stiffness and maximal load compared to native tissue?
Options:
- 1.0 - 1.2 Mrad
- 1.5 - 1.8 Mrad
- 2.0 - 2.5 Mrad
- Greater than 3.0 Mrad
- Any dose of irradiation regardless of threshold
Correct Answer: Greater than 3.0 Mrad
Explanation:
Irradiation is utilized by tissue banks for terminal sterilization to reduce disease transmission risk (e.g., HIV, Hepatitis). Biomechanical studies show that high-dose irradiation, specifically greater than 3.0 Mrad (megarads), significantly alters the structural and mechanical properties of the graft. Many tissue banks now use low-dose irradiation (1.0-1.5 Mrad) or targeted radioprotectants to minimize these detrimental effects while maintaining sterility.
Question 6:
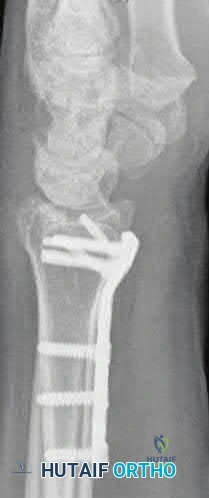
A 45-year-old manual laborer presents with chronic radial-sided wrist pain, recalling a fall on an outstretched hand 5 years ago. Imaging shows a scaphoid nonunion with radioscaphoid and capitolunate arthritis, but the radiolunate joint remains completely preserved. This describes which stage of Scaphoid Nonunion Advanced Collapse (SNAC), and what is a standard surgical option?
Options:
- SNAC Stage 1; Radial styloidectomy
- SNAC Stage 2; Proximal row carpectomy (PRC)
- SNAC Stage 3; Four-corner fusion with scaphoid excision
- SNAC Stage 4; Total wrist arthrodesis
- SNAC Stage 3; Scaphoid open reduction internal fixation with vascularized bone graft
Correct Answer: SNAC Stage 3; Four-corner fusion with scaphoid excision
Explanation:
The progression of SNAC wrist is predictable. Stage 1 involves arthritis at the radial styloid; Stage 2 involves the entire radioscaphoid joint; Stage 3 involves the capitolunate joint; Stage 4 involves the radiolunate and/or entire carpus. Because the radiolunate joint is preserved in Stage 3, a four-corner fusion (capitate, hamate, lunate, triquetrum) with scaphoid excision is the standard salvage procedure. Proximal row carpectomy is contraindicated due to capitolunate arthritis.
Question 7:
A spiral fracture of the tibial shaft is treated with a reamed intramedullary nail, creating an environment of relative stability. During the reparative phase of secondary fracture healing, which of the following anatomic structures is the primary source of the cells that form the massive initial soft callus?
Options:
- Endosteum
- Periosteum
- Bone marrow cavity
- Circulating systemic mesenchymal stem cells
- Haversian canals
Correct Answer: Periosteum
Explanation:
Secondary bone healing occurs in environments with relative stability (e.g., IM nailing, casting, bridge plating) and is characterized by callus formation. The primary source of cells for the initial bridging soft callus is the periosteum, specifically its inner cambium layer, which is highly cellular and rich in osteoprogenitor cells that rapidly proliferate and differentiate into chondrocytes and osteoblasts.
Question 8:
A 65-year-old male presents with classic symptoms of neurogenic claudication. He reports bilateral leg pain and fatigue that worsens with walking but is reliably relieved by leaning forward onto a shopping cart. In the pathogenesis of degenerative lumbar spinal stenosis, which structure is primarily responsible for dynamic central canal compression during spinal extension?
Options:
- Posterior longitudinal ligament
- Ligamentum flavum
- Annulus fibrosus
- Interspinous ligament
- Facet joint capsule
Correct Answer: Ligamentum flavum
Explanation:
In degenerative lumbar spinal stenosis, extension of the spine decreases the sagittal diameter of the canal because the ligamentum flavum buckles inward (shingling), dynamically compressing the thecal sac. Flexion of the spine pulls the ligamentum flavum taut, increasing the available canal space and alleviating neurogenic claudication symptoms. Hypertrophic ligamentum flavum is a major structural contributor to central stenosis.
Question 9:
A 25-year-old male involved in a motorcycle crash sustains an anteroposterior compression (APC) type III pelvic ring injury. He arrives hemodynamically unstable, and a pelvic binder is immediately applied. What is the most common anatomic source of massive retroperitoneal hemorrhage in this fracture pattern?
Options:
- Superior gluteal artery
- Internal pudendal artery
- Presacral and prevesical venous plexus
- External iliac artery
- Corona mortis
Correct Answer: Presacral and prevesical venous plexus
Explanation:
While arterial injuries (such as to the superior gluteal or internal pudendal arteries) can cause rapid and devastating hemorrhage requiring embolization, the vast majority (80-90%) of bleeding in pelvic fractures originates from the presacral and prevesical venous plexuses, as well as the raw cancellous bone edges. The application of a pelvic binder reduces pelvic volume and facilitates the tamponade of this venous bleeding.
Question 10:
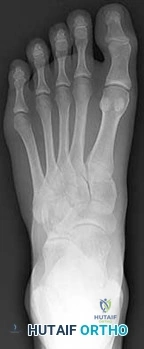
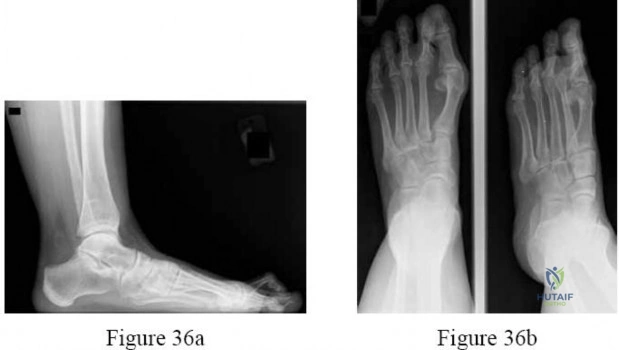
A 30-year-old female sustains a midfoot injury after falling from a horse. Radiographs demonstrate diastasis between the bases of the 1st and 2nd metatarsals. In a normal anatomic state, the native Lisfranc ligament originates and inserts on which two bony structures?
Options:
- Lateral aspect of the medial cuneiform to the medial aspect of the base of the 2nd metatarsal
- Base of the 1st metatarsal directly to the base of the 2nd metatarsal
- Medial aspect of the middle cuneiform to the base of the 2nd metatarsal
- Plantar aspect of the medial cuneiform to the base of the 1st metatarsal
- Lateral cuneiform to the base of the 3rd metatarsal
Correct Answer: Lateral aspect of the medial cuneiform to the medial aspect of the base of the 2nd metatarsal
Explanation:
The Lisfranc ligament is a stout, obliquely oriented intra-articular ligament that acts as the primary stabilizer of the second tarsometatarsal joint complex. It connects the lateral aspect of the medial cuneiform to the medial aspect of the base of the second metatarsal. Importantly, there is no direct ligamentous connection between the bases of the first and second metatarsals.
Question 11:
A 9-year-old boy sustains a distal femur fracture. Radiographs demonstrate a fracture line propagating along the physis and exiting through the metaphysis, producing a small metaphyseal bone fragment (Thurston-Holland fragment). Based on the Salter-Harris classification, what type of fracture is this, and what is the typical expectation regarding growth arrest?
Options:
- Type I; Excellent prognosis, rarely affects growth
- Type II; Most common type, usually does not affect growth, though distal femur location carries a uniquely higher risk
- Type III; Intra-articular fracture with high risk of growth arrest
- Type IV; Crosses the physis, requires anatomic reduction to prevent bar formation
- Type V; Crush injury, universally poor prognosis
Correct Answer: Type II; Most common type, usually does not affect growth, though distal femur location carries a uniquely higher risk
Explanation:
A fracture that propagates through the physis and exits through the metaphysis (creating a Thurston-Holland fragment) is a Salter-Harris Type II fracture. It is the most common physeal fracture pattern. Because the germinal layers of the physis remain attached to the epiphysis, the general prognosis for growth is good. However, one must recognize that Type II fractures of the distal femur inherently carry a high risk of growth arrest (up to 40-50%) compared to other locations.
Question 12:
A 6-year-old girl falls on an outstretched hand and sustains a completely displaced, extension-type supracondylar humerus fracture (Gartland Type III). On physical examination, she cannot actively flex the interphalangeal joint of her thumb or the distal interphalangeal joint of her index finger. Which specific nerve structure is most likely injured?
Options:
- Ulnar nerve
- Radial nerve
- Anterior interosseous nerve (AIN)
- Posterior interosseous nerve (PIN)
- Musculocutaneous nerve
Correct Answer: Anterior interosseous nerve (AIN)
Explanation:
The anterior interosseous nerve (AIN), a motor branch of the median nerve, is the most commonly injured nerve in extension-type pediatric supracondylar humerus fractures (particularly with posterolateral displacement). It innervates the flexor pollicis longus (FPL), the radial half of the flexor digitorum profundus (FDP), and the pronator quadratus. Deficits manifest clinically as the inability to form an 'OK' sign.
Question 13:
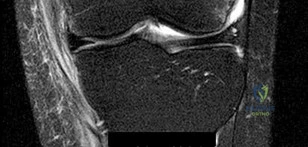
A 68-year-old female is evaluated 6 weeks after an uncomplicated primary total knee arthroplasty (TKA). Despite dedicated daily physical therapy, her range of motion remains stalled at 10 to 70 degrees. Radiographs reveal well-fixed and well-aligned components without signs of loosening. What is the most appropriate next step in her management?
Options:
- Revision TKA with placement of a constrained condylar insert
- Manipulation under anesthesia (MUA)
- Open arthrolysis and polyethylene insert exchange
- Arthroscopic lysis of adhesions
- Discharge from formal PT and encourage continued home stretching
Correct Answer: Manipulation under anesthesia (MUA)
Explanation:
Postoperative stiffness after TKA is a well-recognized complication. The optimal timing for manipulation under anesthesia (MUA) is generally between 6 to 12 weeks postoperatively when conservative measures (aggressive PT) have plateaued or failed. Performing an MUA within this window is highly effective for breaking up immature adhesions. Waiting beyond 12 weeks decreases the success rate due to the maturation of dense intra-articular scar tissue.
Question 14:
During the arthroscopic repair of a massive, retracted, U-shaped posterosuperior rotator cuff tear, the surgeon elects to perform margin convergence prior to tendon-to-bone fixation. Which of the following best explains the primary biomechanical advantage of margin convergence?
Options:
- Side-to-side suturing of the anterior and posterior leaflets reduces strain on the free margin of the tendon at the bone
- Anchoring the medial apex directly to the greater tuberosity provides the strongest single-point fixation
- It converts a U-shaped tear into an L-shaped tear, maximizing the footprint contact area for single-row repair
- It releases the coracohumeral ligament, directly addressing the posterior retraction vector
- It medializes the rotator cuff footprint beyond the articular margin, increasing the resting tension
Correct Answer: Side-to-side suturing of the anterior and posterior leaflets reduces strain on the free margin of the tendon at the bone
Explanation:
Margin convergence is a technique popularized by Burkhart for repairing large, U-shaped rotator cuff tears. Suturing the anterior and posterior limbs of the tear side-to-side (moving laterally toward the footprint) causes the free margin of the tear to converge toward the greater tuberosity. Biomechanically, this significantly decreases the strain (tension) at the critical tendon-to-bone repair site, reducing the likelihood of repair failure.
Question 15:
A 62-year-old female presents with a pathologic subtrochanteric femur fracture. Her laboratory workup reveals hypercalcemia, anemia, and an elevated total serum protein. Serum protein electrophoresis demonstrates a monoclonal spike. Which of the following best describes the underlying pathophysiology responsible for the lytic bone lesions in this condition?
Options:
- Direct mechanical bone resorption by proliferating malignant plasma cells
- Secretion of RANKL and MIP-1alpha by tumor cells stimulating profound osteoclast activity
- Systemic secretion of parathyroid hormone-related peptide (PTHrP) from the primary tumor mass
- Decreased osteoblast function secondary to toxic accumulation of systemic bisphosphonates
- Tumor cell production of high levels of matrix metalloproteinases leading to primary cartilage and matrix destruction
Correct Answer: Secretion of RANKL and MIP-1alpha by tumor cells stimulating profound osteoclast activity
Explanation:
Multiple myeloma, a malignancy of plasma cells, causes characteristic osteolytic bone lesions through an uncoupling of bone remodeling. Myeloma cells upregulate osteoclastogenesis by secreting factors such as Macrophage Inflammatory Protein-1 alpha (MIP-1α) and Receptor Activator of Nuclear factor Kappa-B Ligand (RANKL). Concurrently, they inhibit osteoblast activity (via factors like DKK1 and sclerostin). PTHrP is classically associated with solid metastatic tumors (e.g., breast, lung), not myeloma.
Question 16:
A 72-year-old male is scheduled for an elective total hip arthroplasty. He has a history of non-valvular atrial fibrillation and is currently taking Rivaroxaban. To minimize bleeding risk while avoiding prolonged periods without protection, pharmacokinetic guidelines suggest normal-renal-function patients should stop a direct oral anticoagulant (DOAC) approximately how many half-lives before major surgery?
Options:
- 1 half-life
- 2-3 half-lives
- 4-5 half-lives
- 7-10 half-lives
- 14 half-lives
Correct Answer: 4-5 half-lives
Explanation:
Pharmacokinetically, a drug is considered to have undergone near-complete clinical elimination (approx 94-97% cleared) after 4 to 5 half-lives. For direct oral anticoagulants (DOACs) like Rivaroxaban or Apixaban in a patient with normal renal function, current perioperative guidelines recommend stopping the drug 48 to 72 hours prior to procedures with a high risk of bleeding, which corresponds to roughly 4-5 half-lives.
Question 17:
A 45-year-old male presents with severe right arm pain radiating down to his middle finger. Neurologic examination reveals prominent triceps weakness and an absent triceps deep tendon reflex. His biceps and brachioradialis reflexes are intact. MRI reveals a posterolateral cervical disc herniation. At which cervical spinal level is the pathology most likely located?
Options:
- C4-C5
- C5-C6
- C6-C7
- C7-T1
- T1-T2
Correct Answer: C6-C7
Explanation:
The clinical presentation (triceps weakness, absent triceps reflex, and sensory symptoms radiating to the middle finger) is the classic triad of a C7 radiculopathy. The C7 nerve root exits the cervical spine through the C6-C7 neural foramen, making a C6-C7 posterolateral disc herniation the most likely structural cause.
Question 18:
A 40-year-old skier sustains a highly comminuted Schatzker Type VI tibial plateau fracture. Over the next few hours, he develops tense swelling of the lower leg, paresthesias in the first web space, and pain out of proportion to the injury with passive toe extension. If compartment pressures are measured to confirm acute compartment syndrome, which of the following provides the most reliable threshold for diagnosing the condition?
Options:
- Absolute compartment pressure > 20 mmHg
- Absolute compartment pressure > 25 mmHg
- Delta pressure (Diastolic blood pressure minus compartment pressure) < 30 mmHg
- Delta pressure (Systolic blood pressure minus compartment pressure) < 30 mmHg
- Delta pressure (Mean arterial pressure minus compartment pressure) < 40 mmHg
Correct Answer: Delta pressure (Diastolic blood pressure minus compartment pressure) < 30 mmHg
Explanation:
Acute compartment syndrome is primarily a clinical diagnosis, but pressure measurements are critical in equivocal cases or obtunded patients. The most reliable and widely accepted metric is the delta pressure (ΔP), calculated as the Diastolic Blood Pressure minus the Intracompartmental Pressure. A delta pressure of less than 30 mmHg strongly supports the diagnosis and dictates emergent fasciotomy, as capillary perfusion relies on the gradient with diastolic pressure.
Question 19:
A 42-year-old weekend warrior sustains a sudden "pop" in his posterior calf while lunging for a tennis ball. He is diagnosed with an acute Achilles tendon rupture via a positive Thompson test. He opts for non-operative management utilizing an early functional rehabilitation protocol. Based on modern Level I evidence, how does this approach compare to operative repair?
Options:
- It has a significantly higher rate of deep vein thrombosis
- It carries a significantly higher risk of permanent sural nerve dysfunction
- It demonstrates equivalent rerupture rates while completely avoiding surgical complications like infection
- It results in significantly superior plantar flexion strength and return to play metrics at 2 years
- It demands a much longer period of strict non-weight-bearing cast immobilization
Correct Answer: It demonstrates equivalent rerupture rates while completely avoiding surgical complications like infection
Explanation:
Historically, traditional cast immobilization for Achilles ruptures had higher rerupture rates than surgery. However, modern Level I randomized trials (e.g., Willits et al.) have demonstrated that non-operative management coupled with an *early functional rehabilitation protocol* (early weight-bearing in a functional orthosis and early ROM) yields rerupture rates that are statistically equivalent to operative repair. The primary advantage of the non-operative functional approach is the complete avoidance of surgical complications, such as wound breakdown, deep infection, and iatrogenic sural nerve injury.
Question 20:
A 28-year-old chef accidentally lacerates the volar aspect of his index finger proximal phalanx (Zone II), resulting in a loss of PIP and DIP joint active flexion. He undergoes primary flexor tendon repair. To optimize the biomechanical strength of the tendon repair and minimize gap formation to allow for an early active motion protocol, what is the current gold standard core suture construct?
Options:
- Traditional 2-strand repair with 4-0 nonabsorbable suture
- 4-strand or 6-strand core repair augmented with a peripheral running epitendinous suture
- Barbed suture knotless repair without the need for epitendinous augmentation
- Figure-of-eight 2-strand repair using heavy 2-0 suture
- Multiple superficial horizontal mattress sutures exclusively
Correct Answer: 4-strand or 6-strand core repair augmented with a peripheral running epitendinous suture
Explanation:
In flexor tendon repairs, particularly in Zone II, the goal is to achieve sufficient mechanical strength to withstand early active motion protocols, which are crucial for preventing adhesion formation and optimizing glide. A multi-strand core repair (4-strand or 6-strand) using robust suture (e.g., 3-0 or 4-0) combined with a peripheral running epitendinous suture provides substantially greater tensile strength and resistance to gap formation than a traditional 2-strand repair. The epitendinous suture adds strength and smooths the repair site to facilitate gliding.