Full Question & Answer Text (for Search Engines)
Question 1:
A 34-year-old male presents after a high-speed motorcycle collision. Radiographs demonstrate a displaced scapular body fracture. Which of the following associated injuries is statistically most common in this clinical setting?
Options:
- Rib fractures
- Closed head injury
- Brachial plexus palsy
- Pneumothorax
- Subclavian artery injury
Correct Answer: Rib fractures
Explanation:
Rib fractures are the most common associated injury with scapula fractures, seen in over 50% of cases. Because a massive amount of energy is required to fracture the well-protected scapula, associated injuries to the thorax, including pulmonary contusion and pneumothorax, are highly prevalent, but rib fractures remain the most frequent.
Question 2:
A 62-year-old female who underwent a metal-on-metal total hip arthroplasty 5 years ago presents with new-onset groin pain and a palpable mass. Aspiration yields sterile, cloudy fluid. Histopathological analysis of the periprosthetic tissue is most likely to demonstrate which of the following?
Options:
- Abundant neutrophils and bacterial organisms
- Sheets of lipid-laden macrophages
- Perivascular lymphocytic infiltrate
- Birefringent polymeric wear debris under polarized light
- Extensive caseating granulomas
Correct Answer: Perivascular lymphocytic infiltrate
Explanation:
Adverse local tissue reaction (ALTR) or Aseptic Lymphocytic Vasculitis-Associated Lesions (ALVAL) is a Type IV delayed hypersensitivity reaction to metal ions (cobalt and chromium). Histologically, ALVAL is characterized by extensive perivascular lymphocytic infiltrates. Birefringent wear debris is typical of polyethylene wear, not metal-on-metal.
Question 3:
A 6-year-old boy falls from monkey bars and sustains a completely displaced extension-type supracondylar humerus fracture. Radiographs show the distal fragment is displaced posterolaterally. Based on this displacement pattern, which neurovascular structure is at the greatest risk of injury?
Options:
- Radial nerve
- Ulnar nerve
- Anterior interosseous nerve
- Musculocutaneous nerve
- Axillary nerve
Correct Answer: Anterior interosseous nerve
Explanation:
In extension-type supracondylar fractures, the direction of distal fragment displacement predicts the structure at risk. Posterolateral displacement of the distal fragment results in the proximal fragment being driven anteromedially, stretching the median nerve (specifically the Anterior Interosseous Nerve branch) and brachial artery. Conversely, posteromedial displacement drives the proximal fragment anterolaterally, endangering the radial nerve.
Question 4:
A 45-year-old male presents with right arm pain and weakness. Physical examination reveals weakness in wrist flexion and finger extension, diminished sensation over the dorsal middle finger, and an absent triceps reflex. Which cervical nerve root is most likely compressed?
Options:
Correct Answer: C7
Explanation:
C7 radiculopathy is characterized by weakness in the triceps, wrist flexors (flexor carpi radialis), and finger extensors (extensor digitorum communis). The triceps reflex is diminished or absent, and sensory loss is typically localized over the middle finger. C6 radiculopathy would present with weakness in wrist extension and elbow flexion, a diminished brachioradialis reflex, and sensory loss over the thumb and index finger.
Question 5:
Which of the following Bone Morphogenetic Proteins (BMPs) is an FDA-approved osteoinductive agent for the treatment of acute, open tibial shaft fractures?
Options:
- BMP-2
- BMP-4
- BMP-7
- BMP-9
- BMP-14
Correct Answer: BMP-2
Explanation:
Recombinant human BMP-2 (rhBMP-2) is FDA approved for acute open tibial shaft fractures treated with an intramedullary nail, as well as for anterior lumbar interbody fusion (ALIF). BMPs belong to the TGF-beta superfamily and exert their osteoinductive effects via the Smad 1/5/8 signaling pathways.
Question 6:
A 28-year-old professional cyclist presents with intrinsic muscle weakness in his right hand but normal sensation over the volar and dorsal aspects of the small finger. He is diagnosed with ulnar nerve compression at Guyon's canal. This clinical presentation most likely correlates with compression at which specific zone of Guyon's canal?
Options:
- Zone 1
- Zone 2
- Zone 3
- Zone 4
- Zone 5
Correct Answer: Zone 2
Explanation:
Guyon's canal is divided into three zones. Zone 1 is proximal to the bifurcation; compression here causes mixed motor and sensory deficits. Zone 2 contains only the deep motor branch; compression here (often from a ganglion or hook of hamate fracture) causes isolated motor weakness of ulnar-innervated intrinsic muscles, with normal sensation. Zone 3 contains the superficial sensory branch; compression causes isolated sensory deficits.
Question 7:
During arthroscopic evaluation of a 22-year-old athlete's knee, a longitudinal tear is identified in the peripheral red-red zone of the medial meniscus. Which of the following blood vessels provides the primary vascular supply to this region of the medial meniscus?
Options:
- Middle genicular artery
- Medial inferior genicular artery
- Lateral superior genicular artery
- Descending genicular artery
- Anterior tibial recurrent artery
Correct Answer: Medial inferior genicular artery
Explanation:
The medial and lateral inferior genicular arteries provide the primary blood supply to the peripheral 10-25% (red-red zone) of the menisci via the perimeniscal capillary plexus. The middle genicular artery penetrates the posterior capsule to supply the cruciate ligaments and synovial lining.
Question 8:
A 30-year-old man falls from a height and sustains a talar neck fracture. Six weeks postoperatively, an AP radiograph of the ankle reveals a subchondral radiolucent band extending across the dome of the talus. What is the clinical significance of this radiographic finding?
Options:
- It is an early sign of avascular necrosis of the talar body.
- It indicates an ongoing nonunion at the fracture site.
- It suggests intact vascularity to the talar body.
- It represents a postoperative infection.
- It is pathognomonic for a post-traumatic osteochondral defect.
Correct Answer: It suggests intact vascularity to the talar body.
Explanation:
The finding described is Hawkins sign, which is a subchondral radiolucent band seen in the talar dome 6 to 8 weeks after a talar neck fracture. It represents subchondral osteopenia secondary to hyperemia from disuse. Its presence is a positive prognostic indicator, confirming that the talar body has an intact blood supply and is unlikely to develop avascular necrosis.
Question 9:
A 35-year-old female presents with knee pain. Radiographs reveal an eccentric, lytic epiphyseal lesion extending to the subchondral bone of the distal femur. Biopsy confirms a Giant Cell Tumor (GCT) of bone. Which cellular component of this tumor expresses RANKL, serving as the target for medical therapy?
Options:
- Osteoclast-like multinucleated giant cells
- Neoplastic mononuclear stromal cells
- Reactive osteoblasts
- Endothelial cells
- Chondroid matrix cells
Correct Answer: Neoplastic mononuclear stromal cells
Explanation:
In Giant Cell Tumor of bone, the neoplastic cells are the mononuclear spindle-like stromal cells. These cells express high levels of RANKL. The multinucleated giant cells are reactive osteoclast-like cells that express RANK. Denosumab, a monoclonal antibody against RANKL, targets the neoplastic mononuclear cells' product to prevent the recruitment of the destructive giant cells.
Question 10:
A 55-year-old male who underwent a ceramic-on-ceramic total hip arthroplasty 3 years ago reports a new 'squeaking' noise from his hip during specific movements. He denies pain, and radiographs show no gross loosening. Which of the following component position factors is most strongly associated with the development of squeaking in ceramic-on-ceramic bearings?
Options:
- Decreased femoral offset
- Excessive acetabular cup anteversion
- Insufficient acetabular cup abduction
- Femoral stem retroversion
- Edge loading due to cup malposition
Correct Answer: Edge loading due to cup malposition
Explanation:
Squeaking in ceramic-on-ceramic THA is most strongly associated with edge loading, which often results from cup malposition (such as excessive abduction or extremes of version). Edge loading leads to loss of fluid-film lubrication, stripe wear, and micro-separation during the swing phase, producing the characteristic high-frequency squeak.
Question 11:
A 42-year-old male is brought to the trauma bay after a crush injury. Pelvic radiographs show widening of the pubic symphysis of 3.5 cm and disruption of the anterior sacroiliac ligaments, but intact posterior sacroiliac ligaments. According to the Young-Burgess classification, which type of pelvic ring injury does this represent?
Options:
- APC I
- APC II
- APC III
- LC I
- LC II
Correct Answer: APC II
Explanation:
The Young-Burgess classification divides anteroposterior compression (APC) injuries into three types. APC I: symphysis widening <2.5 cm with intact SI ligaments. APC II: symphysis widening >2.5 cm with disruption of the anterior SI, sacrotuberous, and sacrospinous ligaments, but INTACT posterior SI ligaments (rotationally unstable, vertically stable). APC III involves complete disruption of anterior and posterior SI ligaments.
Question 12:
A 65-year-old female presents with neurogenic claudication and lower back pain. Radiographs reveal a grade I L4-L5 degenerative spondylolisthesis. Which of the following anatomical features is most characteristic of degenerative spondylolisthesis compared to isthmic spondylolisthesis?
Options:
- Defect in the pars interarticularis
- Sagittal orientation of the facet joints
- Association with a high pelvic incidence and sacral slope
- Predilection for the L5-S1 level
- Presentation typically in the second decade of life
Correct Answer: Sagittal orientation of the facet joints
Explanation:
Degenerative spondylolisthesis most commonly occurs at L4-L5 and is associated with a more sagittal orientation of the facet joints, which allows for anterior translation as the disc and joints degenerate without a pars defect. Isthmic spondylolisthesis involves a pars interarticularis defect, most commonly occurs at L5-S1, and is often associated with higher pelvic incidence.
Question 13:
Following a flexor tendon repair in Zone 2, a patient experiences bowstringing of the flexor tendons. During the surgical approach, the surgeon aggressively vented the pulley system. Which two annular pulleys are most critical to preserve to prevent bowstringing and loss of mechanical advantage in the finger?
Options:
- A1 and A3
- A2 and A4
- A1 and A5
- A3 and A5
- A2 and A5
Correct Answer: A2 and A4
Explanation:
The A2 and A4 pulleys are the most crucial biomechanical pulleys in the digital flexor sheath. The A2 pulley arises from the proximal phalanx, and the A4 pulley arises from the middle phalanx. Preserving or reconstructing these pulleys is essential to prevent bowstringing of the flexor tendons, which drastically reduces tendon excursion efficiency and grip strength.
Question 14:
A 6-week-old female infant is diagnosed with developmental dysplasia of the hip (DDH) and placed in a Pavlik harness. During a follow-up visit, the parents report that the infant is no longer actively kicking her left leg, though she cries when the leg is manipulated. Examination shows absent active knee extension on the left. The harness strap positioning is likely causing compression of which structure?
Options:
- Sciatic nerve
- Femoral nerve
- Obturator nerve
- Superior gluteal nerve
- Lateral femoral cutaneous nerve
Correct Answer: Femoral nerve
Explanation:
Femoral nerve palsy is a known complication of the Pavlik harness, typically occurring when the anterior straps are pulled too tight, placing the hips in excessive hyperflexion. The infant presents with decreased active knee extension (decreased kicking). It is usually transient and resolves with temporary removal or adjustment of the harness to decrease hip flexion.
Question 15:
A 24-year-old football player sustains a twisting injury to the knee. On examination, there is a normal posterior sag sign. The dial test demonstrates 15 degrees of increased external rotation compared to the contralateral side at 30 degrees of knee flexion, but symmetrical external rotation at 90 degrees of flexion. What is the most likely diagnosis?
Options:
- Isolated Posterior Cruciate Ligament (PCL) tear
- Isolated Posterolateral Corner (PLC) injury
- Combined PCL and PLC injury
- Isolated Anterior Cruciate Ligament (ACL) tear
- Combined ACL and Posteromedial corner injury
Correct Answer: Isolated Posterolateral Corner (PLC) injury
Explanation:
The dial test evaluates the posterolateral corner (PLC) and the posterior cruciate ligament (PCL). Increased external rotation (>10 degrees compared to the normal side) at 30 degrees of flexion, but symmetric rotation at 90 degrees, indicates an isolated PLC injury. Increased external rotation at both 30 and 90 degrees indicates a combined PCL and PLC injury.
Question 16:
A 40-year-old male sustains a distal femur fracture. CT imaging reveals a coronal plane fracture of the lateral femoral condyle. This specific fracture pattern (Hoffa fracture) is best stabilized with which of the following internal fixation constructs to resist the primary deforming forces?
Options:
- Lateral locking plate only
- Medial and lateral tension band wiring
- Anterior-to-posterior (AP) or posterior-to-anterior (PA) interfragmentary lag screws
- Antegrade intramedullary nail
- External fixation
Correct Answer: Anterior-to-posterior (AP) or posterior-to-anterior (PA) interfragmentary lag screws
Explanation:
A Hoffa fracture is a coronal plane fracture of the femoral condyle (most commonly lateral). Due to its vertical orientation, lateral plating alone often fails to adequately compress the fracture. The gold standard for stabilizing a Hoffa fragment is interfragmentary lag screw fixation directed anterior-to-posterior (AP) or posterior-to-anterior (PA), providing compression perpendicular to the fracture line.
Question 17:
Within articular cartilage, which structural landmark separates the deep uncalcified zone from the calcified cartilage zone and serves as the physical barrier to the transport of nutrients from the subchondral bone?
Options:
- Lamina splendens
- Tidemark
- Cement line
- Physis
- Subchondral bone plate
Correct Answer: Tidemark
Explanation:
The tidemark is the histological boundary that separates the deep zone of true, uncalcified articular cartilage from the calcified zone. It acts as a strict barrier to nutrient diffusion from the subchondral bone, meaning that the uncalcified zones of articular cartilage rely almost entirely on diffusion from synovial fluid for their nutritional demands. The cement line separates the calcified cartilage from the subchondral bone.
Question 18:
A 58-year-old male with poorly controlled type 2 diabetes presents with a swollen, erythematous, and warm left foot. Radiographs reveal fragmentation of the tarsometatarsal joints, periarticular debris, and joint subluxation, but no skin ulceration. According to the Eichenholtz classification, what is the most appropriate initial management for this patient?
Options:
- Immediate open reduction and internal fixation of the midfoot
- Total contact casting and non-weight-bearing
- Intravenous antibiotics for 6 weeks
- Primary arthrodesis of the tarsometatarsal joints
- Below-knee amputation
Correct Answer: Total contact casting and non-weight-bearing
Explanation:
The patient is in Stage 1 (Fragmentation/Developmental phase) of Charcot neuroarthropathy, characterized by a red, hot, swollen foot with radiographic evidence of osteopenia, fragmentation, and subluxation. The gold standard of treatment in the acute phase is immobilization and strict offloading, typically achieved with a total contact cast, to prevent further deformity until the active inflammatory process subsides.
Question 19:
A 14-year-old boy presents with pain and swelling in the mid-shaft of his femur. Radiographs display a permeative, diaphyseal lytic lesion with an 'onion-skin' periosteal reaction. Biopsy reveals small, round, blue cells. Which chromosomal translocation is most characteristically associated with this malignancy?
Options:
- t(11;22)
- t(9;22)
- t(X;18)
- t(2;13)
- t(12;16)
Correct Answer: t(11;22)
Explanation:
Ewing sarcoma is a highly malignant small round blue cell tumor that typically arises in the diaphysis of long bones in children and adolescents. It is strongly associated with the balanced chromosomal translocation t(11;22)(q24;q12), which results in the EWS-FLI1 fusion protein. This unique fusion drives the pathogenesis of the tumor.
Question 20:
A 2-week-old male infant presents with idiopathic congenital talipes equinovarus (clubfoot). The pediatric orthopedist plans to initiate Ponseti serial casting. According to the Ponseti method, what is the correct sequential order of deformity correction?
Options:
- Cavus, Adductus, Varus, Equinus
- Equinus, Varus, Adductus, Cavus
- Adductus, Cavus, Equinus, Varus
- Varus, Equinus, Cavus, Adductus
- Cavus, Varus, Adductus, Equinus
Correct Answer: Cavus, Adductus, Varus, Equinus
Explanation:
The Ponseti method involves sequential correction of the deformities in congenital clubfoot following the mnemonic CAVE: Cavus (corrected first by elevating the first ray), Adductus (corrected by abducting the forefoot around the fixed head of the talus), Varus (which corrects simultaneously with forefoot abduction), and finally Equinus (which often requires a percutaneous Achilles tenotomy as the final step).
Question 21:
An 11-year-old male with a body mass index (BMI) in the 99th percentile presents with left hip pain and an obligatory external rotation during hip flexion. He is diagnosed with a slipped capital femoral epiphysis (SCFE). Which of the following is considered an absolute indication for prophylactic pinning of the contralateral, asymptomatic hip?
Options:
- Obesity with BMI > 95th percentile
- Hypothyroidism
- Age of 11 years
- Male sex
- African American race
Correct Answer: Hypothyroidism
Explanation:
Prophylactic pinning of the contralateral hip in SCFE is controversial but is generally indicated in patients with underlying endocrine disorders (such as hypothyroidism, panhypopituitarism, or renal osteodystrophy), patients undergoing previous radiation therapy, and in very young patients (typically less than 10 years of age for boys). Obesity, while a risk factor for SCFE, is not an absolute indication for prophylactic contralateral pinning.
Question 22:
A 35-year-old male is brought to the trauma bay following a high-speed motorcycle collision. A pelvic binder was placed in the field. Anteroposterior (AP) pelvis radiograph reveals an anterior-posterior compression (APC) injury. His pubic symphysis is widened by 3.5 cm, but the posterior pelvic ring appears grossly intact on initial imaging. In an APC-II pelvic ring injury, which of the following ligamentous structures remains intact?
Options:
- Anterior sacroiliac ligament
- Sacrospinous ligament
- Sacrotuberous ligament
- Posterior sacroiliac ligament
- Pubic symphyseal ligaments
Correct Answer: Posterior sacroiliac ligament
Explanation:
According to the Young-Burgess classification, an APC-II injury is characterized by rupture of the pubic symphysis, anterior sacroiliac ligaments, sacrospinous ligaments, and sacrotuberous ligaments, resulting in an 'open book' pelvis. The posterior sacroiliac ligaments remain intact, providing vertical stability but allowing rotational instability. Rupture of the posterior sacroiliac ligaments would result in an APC-III injury, which is completely unstable both rotationally and vertically.
Question 23:
A 14-year-old boy presents with progressive pain and swelling in his mid-thigh over the last two months. Radiographs reveal a permeative, diaphyseal lytic lesion with an 'onion skin' periosteal reaction. Biopsy demonstrates uniform, small round blue cells. What is the most common chromosomal translocation associated with this patient's diagnosis?
Options:
- t(11;22)
- t(X;18)
- t(12;16)
- t(2;13)
- t(9;22)
Correct Answer: t(11;22)
Explanation:
The clinical presentation and histology are classic for Ewing sarcoma. The most common genetic anomaly associated with Ewing sarcoma is the t(11;22)(q24;q12) translocation, which fuses the EWS gene on chromosome 22 with the FLI1 gene on chromosome 11, occurring in about 85% of cases. t(X;18) is seen in Synovial Sarcoma. t(12;16) is seen in Myxoid Liposarcoma. t(2;13) is seen in Alveolar Rhabdomyosarcoma.
Question 24:
A 55-year-old carpenter presents with a long history of dominant wrist pain. Radiographs demonstrate advanced scapholunate advanced collapse (SLAC). The surgeon is deciding between a four-corner fusion and a proximal row carpectomy (PRC). Which of the following radiographic findings represents an absolute contraindication to performing a proximal row carpectomy?
Options:
- Radioscaphoid arthritis
- Radiolunate arthritis
- Capitolunate arthritis
- Scaphotrapezial arthritis
- Ulnocarpal abutment
Correct Answer: Capitolunate arthritis
Explanation:
A proximal row carpectomy (PRC) involves excising the scaphoid, lunate, and triquetrum, allowing the capitate to articulate within the lunate fossa of the distal radius. Therefore, the articular surfaces of the proximal capitate head and the lunate fossa must be preserved. Capitolunate arthritis (which involves the capitate head) or damage to the lunate fossa are contraindications to PRC, and a four-corner fusion or total wrist arthrodesis should be considered instead.
Question 25:
A 65-year-old female complains of progressive clumsiness in her hands, difficulty buttoning her shirts, and a feeling of unsteadiness when walking. Physical examination reveals hyperreflexia and a positive Hoffmann sign. How is the Hoffmann sign elicited on physical examination?
Options:
- Scraping the lateral plantar aspect of the foot
- Tapping the volar carpal tunnel
- Flicking the distal phalanx of the middle finger
- Tapping the distal biceps tendon
- Rapid, alternating supination and pronation of the forearm
Correct Answer: Flicking the distal phalanx of the middle finger
Explanation:
The Hoffmann sign is an indicator of upper motor neuron dysfunction, commonly seen in cervical spondylotic myelopathy. It is elicited by stabilizing the patient's middle finger and rapidly flicking the distal phalanx downwards (volarward). A positive sign is the reflex flexion of the interphalangeal joint of the thumb and/or index finger. Scraping the plantar foot elicits the Babinski reflex. Tapping the carpal tunnel elicits a Tinel sign.
Question 26:
A 22-year-old male rugby player is evaluated for recurrent anterior shoulder instability. He has had 5 dislocations over the past year. A CT scan of his shoulder indicates 28% anterior glenoid bone loss. What is the most appropriate surgical treatment to minimize his risk of recurrent dislocation?
Options:
- Arthroscopic Bankart repair
- Open Bankart repair
- Latarjet procedure
- Remplissage procedure alone
- Putti-Platt procedure
Correct Answer: Latarjet procedure
Explanation:
Glenoid bone loss is a critical factor in recurrent anterior shoulder instability. Critical bone loss is typically defined as >20-25% of the inferior glenoid width. In the setting of significant anterior glenoid bone loss (>25%), soft tissue stabilization (arthroscopic or open Bankart repair) has unacceptably high failure rates. Bony augmentation procedures, such as the Latarjet procedure (coracoid transfer), are indicated to restore glenoid width and provide a sling effect via the conjoint tendon.
Question 27:
A 60-year-old male who underwent an uncomplicated total hip arthroplasty (THA) 3 years ago presents to the clinic complaining of a high-pitched squeaking noise coming from his hip when he walks or bends over. He denies any pain, instability, or trauma. Based on this presentation, what bearing surface combination was most likely utilized in his THA?
Options:
- Metal-on-polyethylene
- Ceramic-on-ceramic
- Metal-on-metal
- Ceramic-on-polyethylene
- Oxinium-on-polyethylene
Correct Answer: Ceramic-on-ceramic
Explanation:
Squeaking is a known, unique complication associated with ceramic-on-ceramic (CoC) bearing surfaces in total hip arthroplasty, occurring in up to 10% of cases. The exact etiology is multifactorial, potentially involving stripe wear, edge loading, microseparation, or third-body debris. Squeaking typically does not occur with polyethylene or metal-on-metal bearing surfaces.
Question 28:
A 55-year-old male with poorly controlled type 2 diabetes presents with a unilaterally swollen, red, and warm right foot. He denies any ulceration or systemic signs of infection. Radiographs demonstrate fragmentation of the midfoot bones, subchondral debris, and joint subluxation. According to the Eichenholtz classification, the patient is currently in Stage I (Developmental). What is the gold standard initial management?
Options:
- Total contact casting
- Immediate midfoot arthrodesis
- Intravenous antibiotics
- Below-knee amputation
- Calcaneal sliding osteotomy
Correct Answer: Total contact casting
Explanation:
The clinical presentation is highly consistent with acute Charcot arthropathy (Eichenholtz Stage I: Developmental/Fragmentation). The primary goal during the acute phase is to prevent further deformity and allow the inflammatory process to subside. The gold standard treatment is immediate offloading and immobilization using a total contact cast (TCC). Surgery is generally contraindicated during the acute, hyperemic phase due to poor bone quality and high failure rates.
Question 29:
According to Perren's strain theory of bone healing, the process of primary bone healing (direct remodeling by osteonal cutting cones without callus formation) depends heavily on the mechanical environment. For primary bone healing to occur, the interfragmentary strain must remain below which of the following thresholds?
Options:
Correct Answer: 2%
Explanation:
Perren's strain theory postulates that different tissues can tolerate different amounts of deformation (strain) before failure. Granulation tissue tolerates up to 100% strain, cartilage tolerates up to 10%, and bone tolerates only up to 2%. For primary (direct) bone healing to occur, there must be absolute stability with interfragmentary strain less than 2%. Secondary bone healing (callus formation) occurs when strain is between 2% and 10%.
Question 30:
A 2-year-old girl is brought to the pediatric orthopedic clinic by her parents due to worsening bilateral 'bowlegs.' Radiographs reveal a metaphyseal-diaphyseal angle of 18 degrees on the right and 19 degrees on the left, along with medial physeal beaking. She is diagnosed with infantile Blount disease (tibia vara). What is the most appropriate initial management?
Options:
- Observation and reassurance
- Knee-ankle-foot orthoses (KAFOs)
- Proximal tibial valgus osteotomy
- Hemiepiphysiodesis of the lateral proximal tibia
- Guided growth using tension band plates
Correct Answer: Knee-ankle-foot orthoses (KAFOs)
Explanation:
In infantile Blount disease, a metaphyseal-diaphyseal angle (MDA) greater than 16 degrees predicts progression of the deformity, distinguishing it from physiologic bowing. For children under the age of 3 with Langenskiöld Stage I or II and an MDA > 16 degrees, bracing with a knee-ankle-foot orthosis (KAFO) is the recommended initial management. Surgical intervention (osteotomy or guided growth) is indicated if bracing fails, or typically if the child is over 3-4 years old with advanced stages.
Question 31:
A 45-year-old female presents to the emergency department after falling on an outstretched hand. Radiographs show a fracture of the distal radius involving the volar rim, with the carpus subluxated volarly along with the fracture fragment. Which eponymous term correctly describes this injury pattern?
Options:
- Colles fracture
- Smith fracture
- Barton fracture
- Chauffeur fracture
- Die-punch fracture
Correct Answer: Barton fracture
Explanation:
A Barton fracture is a shear fracture of the distal radius articular surface (can be volar or dorsal, though volar is more common) accompanied by subluxation or dislocation of the carpus along with the fractured articular fragment. A Colles fracture is a distally radiused fracture with dorsal displacement. A Smith fracture is a distal radius fracture with volar displacement. A Chauffeur fracture involves the radial styloid. A Die-punch fracture involves the lunate facet.
Question 32:
A 30-year-old female presents with a painful lytic epiphyseal lesion of the distal femur. Biopsy confirms the diagnosis of Giant Cell Tumor of bone. Due to the proximity to the joint space and the large size of the defect, the multidisciplinary tumor board recommends neoadjuvant treatment with Denosumab to downstage the tumor prior to intralesional curettage. What is the precise mechanism of action of Denosumab?
Options:
- Inhibition of osteoclast proton pumps
- Monoclonal antibody against RANK Ligand
- Monoclonal antibody against the RANK receptor
- Inhibition of vascular endothelial growth factor (VEGF)
- Cross-linking of intracellular DNA
Correct Answer: Monoclonal antibody against RANK Ligand
Explanation:
Giant cell tumor of bone (GCTB) is characterized by neoplastic mononuclear stromal cells that express RANKL, which recruits and activates the multinucleated giant cells (osteoclasts) responsible for the osteolysis. Denosumab is a fully human monoclonal antibody that binds directly to RANK Ligand (RANKL), preventing it from interacting with the RANK receptor on osteoclasts and their precursors, thereby inhibiting osteoclast-mediated bone destruction.
Question 33:
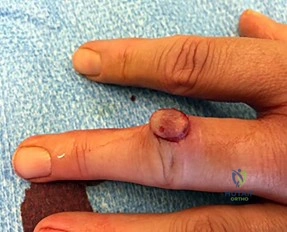
A 25-year-old male rugby player attempts to tackle an opponent by grabbing his jersey. He feels a sudden 'pop' in his right ring finger and presents unable to actively flex the distal interphalangeal (DIP) joint. Radiographs demonstrate a large bony avulsion fragment located volar to the proximal interphalangeal (PIP) joint, failing to retract completely into the palm. According to the Leddy-Packer classification, what type of flexor digitorum profundus (FDP) avulsion injury is this?
Options:
- Type I
- Type II
- Type III
- Type IV
- Type V
Correct Answer: Type II
Explanation:
The Leddy-Packer classification categorizes FDP avulsion injuries ('Jersey finger'). Type I: The tendon retracts all the way into the palm; blood supply is severely compromised, requiring repair within 7-10 days. Type II: The tendon retracts to the level of the PIP joint, caught by the intact vincula; there may be a small fleck of bone. Type III: A large bony avulsion fragment that catches at the A4 pulley, preventing further retraction. The scenario describes a fragment at the PIP joint, which is characteristic of Type II, where it is held by the vincula longum.
Question 34:
A 68-year-old female presents with recurrent posterior dislocations following a primary total hip arthroplasty performed 6 months ago. A recent CT scan evaluating component positioning reveals an acetabular component inclination of 45 degrees and an anteversion of 0 degrees. The femoral stem has 15 degrees of anteversion. What is the most likely underlying cause of her recurrent instability?
Options:
- Acetabular retroversion
- Excessive acetabular anteversion
- Excessive femoral stem anteversion
- Vertical inclination of the acetabular component
- Abductor mechanism deficiency
Correct Answer: Acetabular retroversion
Explanation:
The 'safe zone' for acetabular component placement, historically described by Lewinnek, is 15° ± 10° of anteversion and 40° ± 10° of inclination. An acetabular anteversion of 0 degrees means the cup is placed in relative retroversion compared to normal native anatomy. Acetabular retroversion heavily predisposes a THA patient to posterior dislocation, particularly when the hip is placed in flexion, adduction, and internal rotation.
Question 35:
A 21-year-old collegiate soccer player is undergoing anterior cruciate ligament (ACL) reconstruction. The surgeon discusses various graft options and their respective morbidity profiles. Which of the following complications is most specifically associated with the use of a bone-patellar tendon-bone (BTB) autograft compared to a multi-strand hamstring autograft?
Options:
- Higher graft re-rupture rate
- Increased risk of deep joint infection
- Anterior knee pain
- Symptomatic tunnel widening
- Increased risk of deep vein thrombosis
Correct Answer: Anterior knee pain
Explanation:
Bone-patellar tendon-bone (BTB) autograft is a very reliable graft for ACL reconstruction due to bone-to-bone healing at the tunnels. However, its most common specific donor-site morbidity is anterior knee pain (including pain kneeling), reported in up to 10-30% of patients. Hamstring autografts have less anterior knee pain but are associated with slightly higher rates of tunnel widening and potentially a marginal decrease in deep knee flexion strength.
Question 36:
Articular cartilage depends on a highly organized extracellular matrix to resist compressive loads. Which of the following is the most abundant proteoglycan found in articular cartilage, functioning to provide compressive stiffness through its massive water-binding capacity when complexed with hyaluronic acid?
Options:
- Decorin
- Biglycan
- Aggrecan
- Fibromodulin
- Lumican
Correct Answer: Aggrecan
Explanation:
Aggrecan is the predominant proteoglycan in articular cartilage, constituting up to 90% of the proteoglycan mass. It possesses highly negatively charged glycosaminoglycan (GAG) side chains (chondroitin sulfate and keratan sulfate) that attract water (Donnan osmotic effect). When bound to hyaluronic acid via link proteins, aggrecan forms massive aggregates that become trapped within the Type II collagen meshwork, conferring the cartilage's ability to resist compressive loads.
Question 37:
A 40-year-old male sustains an acute, complete rupture of the Achilles tendon while playing tennis. He opts for non-operative management utilizing functional rehabilitation with early range of motion. Compared to traditional open surgical repair, which of the following best describes the expected outcome of his non-operative approach based on recent prospective trials?
Options:
- Decreased risk of overall complication rate, but an increased risk of sural nerve injury
- Equivalent return to sport rates, but an increased risk of deep infection
- Higher overall complication rate, but equal plantarflexion strength
- Decreased soft-tissue complication rate with a slightly higher risk of re-rupture
- Higher rate of deep vein thrombosis with equivalent re-rupture risk
Correct Answer: Decreased soft-tissue complication rate with a slightly higher risk of re-rupture
Explanation:
Recent high-level evidence (such as the Willits et al. trial) demonstrates that functional rehabilitation (early weight-bearing and ROM) for non-operative management of acute Achilles tendon ruptures yields functional outcomes similar to surgical repair. The non-operative approach avoids surgical complications (infection, wound breakdown, sural nerve injury) but carries a slightly higher re-rupture rate compared to operative management, though this gap has narrowed significantly with modern functional bracing protocols.
Question 38:
A 72-year-old male complains of an insidious onset of bilateral buttock and posterior thigh pain that worsens after walking two blocks or standing for 15 minutes. He notices immediate relief when he sits down on a bench or leans forward onto his grocery shopping cart. What physical examination finding is most characteristic of this patient's underlying condition?
Options:
- Absent bilateral pedal pulses
- Pain alleviation with prolonged standing still
- A relatively normal neurologic examination at rest
- Trophic skin changes and lack of hair on the lower extremities
- A positive seated straight leg raise test
Correct Answer: A relatively normal neurologic examination at rest
Explanation:
This classic presentation represents neurogenic claudication secondary to lumbar spinal stenosis. Symptoms are typically exacerbated by lumbar extension (which decreases canal volume) and relieved by lumbar flexion (sitting, leaning over a cart). Unlike vascular claudication (which is relieved by simply stopping and standing still, and presents with diminished pulses/trophic changes), neurogenic claudication typically presents with a completely normal neurologic exam at rest, as the nerve root ischemia only occurs dynamically during ambulation and extension.
Question 39:
A 28-year-old male is admitted after suffering a closed, highly comminuted tibia fracture from a motor vehicle accident. Twelve hours post-admission, he develops severe, unrelenting leg pain out of proportion to the injury. His systemic blood pressure is 115/70 mmHg. Intracompartmental pressure monitoring of the anterior compartment yields a pressure of 45 mmHg. What is the patient's delta P (ΔP), and what is the most appropriate next step in management?
Options:
- ΔP = 70 mmHg; continue observation
- ΔP = 45 mmHg; administer intravenous pain medication
- ΔP = 25 mmHg; emergent four-compartment fasciotomy
- ΔP = 25 mmHg; bivalve the cast and elevate the leg above the heart
- ΔP = 30 mmHg; emergent four-compartment fasciotomy
Correct Answer: ΔP = 25 mmHg; emergent four-compartment fasciotomy
Explanation:
Acute compartment syndrome is a surgical emergency. The delta P (ΔP) is calculated as the Diastolic Blood Pressure minus the Compartment Pressure. Here, ΔP = 70 mmHg - 45 mmHg = 25 mmHg. A ΔP of less than 30 mmHg is an absolute indication for emergent fasciotomy to release the fascial compartments and restore tissue perfusion. Elevating the leg above the heart actually decreases local arterial perfusion pressure and is contraindicated in suspected compartment syndrome.
Question 40:
A 6-year-old boy presents with a 3-month history of a painless limp. Radiographs demonstrate fragmentation and increased sclerosis of the capital femoral epiphysis, consistent with Legg-Calvé-Perthes disease. The lateral pillar classification (Herring) is widely utilized to determine the prognosis of this condition. This classification system relies on evaluating the height of which specific portion of the capital femoral epiphysis on an anteroposterior (AP) radiograph?
Options:
- The anterior third
- The central third
- The lateral third
- The posterior third
- The medial third
Correct Answer: The lateral third
Explanation:
The Herring Lateral Pillar Classification is assessed on the AP radiograph during the fragmentation stage of Legg-Calvé-Perthes disease. It evaluates the height of the lateral third of the capital femoral epiphysis compared to the contralateral normal side. Group A has no lateral pillar involvement; Group B has >50% lateral pillar height maintained; Group C has <50% of the lateral pillar height maintained. The condition of the lateral pillar is the most significant prognostic factor for late femoral head deformity.
Question 41:
Which Bone Morphogenetic Protein (BMP) is most closely associated with the FDA-approved indication for use in acute, open tibial shaft fractures?
Options:
- BMP-2
- BMP-3
- BMP-4
- BMP-7
- BMP-9
Correct Answer: BMP-2
Explanation:
Recombinant human BMP-2 (rhBMP-2) is FDA approved for the treatment of acute open tibial shaft fractures, typically administered via an absorbable collagen sponge. rhBMP-7 (also known as Osteogenic Protein-1 or OP-1) was previously approved under a humanitarian device exemption for recalcitrant tibial nonunions.
Question 42:
A 45-year-old female presents with sudden onset medial knee pain while squatting. MRI shows a medial meniscus posterior root tear. Biomechanically, what is the consequence of this specific injury on the knee joint?
Options:
- Increased contact area in the medial compartment
- Decreased peak contact pressure during weight-bearing
- Kinematics equivalent to a total medial meniscectomy
- Increased anterior tibial translation during the Lachman test
- Decreased varus laxity in full extension
Correct Answer: Kinematics equivalent to a total medial meniscectomy
Explanation:
A complete posterior root tear of the medial meniscus leads to a complete loss of hoop stresses, resulting in radial extrusion of the meniscus during axial loading. Biomechanically, this is equivalent to a total medial meniscectomy, significantly decreasing the contact area and markedly increasing peak contact pressures, leading to accelerated osteoarthritis.
Question 43:
A 35-year-old male sustains a distal femur fracture. CT scan reveals a coronal plane fracture of the lateral femoral condyle. Which surgical approach is most appropriate for direct visualization and reduction of this specific intra-articular fragment?
Options:
- Medial parapatellar approach
- Direct lateral approach to the distal femur
- Lateral parapatellar approach
- Swashbuckler (extended lateral) approach
- Subvastus approach
Correct Answer: Swashbuckler (extended lateral) approach
Explanation:
A coronal plane fracture of the femoral condyle is a Hoffa fracture (AO 33-B3). The lateral condyle is most commonly affected. The Swashbuckler (extended lateral) approach provides excellent exposure of the distal femur, including the lateral articular surface, for open reduction and internal fixation of distal femur fractures with intra-articular coronal plane components.
Question 44:
During a total knee arthroplasty, the surgeon evaluates the gaps after initial bony resections. The extension gap is symmetric and perfectly balanced, but the flexion gap is tight medially and loose laterally. What is the most appropriate next step to balance the knee?
Options:
- Release the superficial medial collateral ligament
- Release the posterior cruciate ligament
- Externally rotate the femoral component
- Downsize the femoral component
- Resect more distal femur
Correct Answer: Externally rotate the femoral component
Explanation:
A flexion gap that is tight medially and loose laterally indicates relative internal rotation of the femoral component. Externally rotating the femoral component will loosen the medial side in flexion and tighten the lateral side in flexion without affecting the extension gap.
Question 45:
A 42-year-old male presents with severe lower back pain, bilateral sciatica, and new-onset urinary retention (post-void residual greater than 500 mL). MRI confirms a massive L4-L5 central disc herniation. Current literature suggests that surgical decompression is ideally performed within what timeframe to maximize the chance of urologic recovery?
Options:
- 6 hours
- 12 hours
- 24 hours
- 48 hours
- 72 hours
Correct Answer: 48 hours
Explanation:
Cauda equina syndrome is a surgical emergency. Meta-analyses (e.g., Ahn et al.) suggest that decompression within 48 hours provides significantly better outcomes for the return of normal motor, sensory, and urologic function compared to decompression performed after 48 hours.
Question 46:
A 30-year-old female presents with knee pain. Radiographs show an eccentric, lytic epiphyseal lesion of the proximal tibia. Biopsy reveals multinucleated giant cells in a background of mononuclear stromal cells. What is the primary molecular target of the systemic therapy commonly used to treat unresectable cases of this tumor?
Options:
- Vascular Endothelial Growth Factor (VEGF)
- Receptor Activator of Nuclear Factor Kappa-B Ligand (RANKL)
- Platelet-Derived Growth Factor (PDGF)
- Mammalian Target of Rapamycin (mTOR)
- Human Epidermal Growth Factor Receptor 2 (HER2)
Correct Answer: Receptor Activator of Nuclear Factor Kappa-B Ligand (RANKL)
Explanation:
The diagnosis is Giant Cell Tumor of Bone (GCTB). The neoplastic cells are the mononuclear stromal cells, which express high levels of RANKL. This recruits and activates osteoclast-like giant cells. Denosumab, a monoclonal antibody against RANKL, is used for unresectable GCTB or to downstage tumors prior to surgery.
Question 47:
A 13-year-old obese boy presents with left thigh pain and an obligatory external rotation of the left hip during flexion. He is diagnosed with a Slipped Capital Femoral Epiphysis (SCFE). Which of the following is considered an absolute indication for prophylactic pinning of the contralateral asymptomatic hip?
Options:
- Endocrine disorder (e.g., hypothyroidism)
- Age greater than 15 years
- Male gender
- Obesity (BMI greater than 95th percentile)
- Modified Klein line intersection on the normal hip
Correct Answer: Endocrine disorder (e.g., hypothyroidism)
Explanation:
Prophylactic pinning of the contralateral hip in SCFE is controversial but generally recommended in patients with a high risk of developing a contralateral slip. Absolute indications or strong recommendations include the presence of an underlying endocrine disorder (hypothyroidism, panhypopituitarism, renal osteodystrophy) or prior radiation therapy, as these patients have a much higher rate of bilateral involvement.
Question 48:
Which of the following best defines 'stress relaxation' in the context of orthopedic biomechanics and viscoelastic materials?
Options:
- Increasing deformation over time under a constant load
- Decreasing force over time under a constant deformation
- Energy lost as heat during a loading-unloading cycle
- Increased stiffness with an increased rate of loading
- The point at which a material transitions from elastic to plastic deformation
Correct Answer: Decreasing force over time under a constant deformation
Explanation:
Viscoelastic materials exhibit time-dependent properties. 'Stress relaxation' is the decrease in stress (force) over time when the material is held at a constant strain (deformation). 'Creep' is the progressive deformation (strain) over time under a constant load (stress).
Question 49:
A 28-year-old carpenter sustains a laceration to his volar index finger at the level of the proximal phalanx, transecting both the FDS and FDP tendons. This injury corresponds to which flexor tendon zone?
Options:
- Zone I
- Zone II
- Zone III
- Zone IV
- Zone V
Correct Answer: Zone II
Explanation:
Zone II (historically called 'no mans land') extends from the A1 pulley (distal palmar crease) to the FDS insertion (mid-middle phalanx). Lacerations here commonly involve both FDS and FDP and have a high risk of adhesion formation due to the tightly constrained fibro-osseous sheath.
Question 50:
A 45-year-old male is brought to the ED after a motorcycle crash. His pelvis is unstable. Radiographs show symphyseal diastasis of 3.5 cm and widening of the anterior sacroiliac joints, but the posterior SI ligaments remain intact. According to the Young-Burgess classification, what type of injury is this?
Options:
- APC I
- APC II
- APC III
- LC I
- LC II
Correct Answer: APC II
Explanation:
Anterior-Posterior Compression (APC) injuries: APC I is symphysis widening < 2.5 cm with intact posterior ligaments. APC II is symphysis widening > 2.5 cm, torn anterior SI, sacrotuberous, and sacrospinous ligaments, but INTACT posterior SI ligaments (rotationally unstable, vertically stable). APC III involves disruption of both anterior and posterior SI ligaments (rotationally and vertically unstable).
Question 51:
A 55-year-old diabetic male presents with a swollen, erythematous, and warm left foot. Radiographs demonstrate periarticular debris, fragmentation, and joint subluxation at the tarsometatarsal joints. According to the Eichenholtz classification of Charcot arthropathy, what stage does this represent?
Options:
- Stage 0
- Stage 1
- Stage 2
- Stage 3
- Stage 4
Correct Answer: Stage 1
Explanation:
Eichenholtz Stage 1 (Development/Fragmentation) is characterized by clinical erythema, swelling, and warmth, with radiographic features of bone fragmentation, debris, joint subluxation, and fracture. Stage 2 (Coalescence) shows absorption of debris and early fusion. Stage 3 (Reconstruction) shows consolidation and remodeling. Stage 0 is the clinical high-risk foot with no radiographic changes.
Question 52:
You are treating an infant with idiopathic congenital talipes equinovarus using the Ponseti method. What is the correct sequence of deformity correction?
Options:
- Equinus, Varus, Adduction, Cavus
- Cavus, Adduction, Varus, Equinus
- Adduction, Cavus, Varus, Equinus
- Varus, Cavus, Adduction, Equinus
- Cavus, Equinus, Adduction, Varus
Correct Answer: Cavus, Adduction, Varus, Equinus
Explanation:
The Ponseti method corrects clubfoot deformities in the mnemonic order CAVE: Cavus (corrected first by elevating the first ray to supinate the forefoot and align it with the hindfoot), followed by Adduction, Varus, and finally Equinus (which often requires a percutaneous Achilles tenotomy).
Question 53:
A 25-year-old male undergoes an isolated posterior cruciate ligament (PCL) reconstruction using an anterolateral bundle (ALB) single-bundle technique. At what degree of knee flexion should the ALB graft be tensioned and fixed to best replicate native biomechanics?
Options:
- 0 degrees (full extension)
- 30 degrees
- 45 degrees
- 90 degrees
- 120 degrees
Correct Answer: 90 degrees
Explanation:
The native PCL consists of the anterolateral bundle (ALB) and posteromedial bundle (PMB). The ALB is tightest in flexion, and the PMB is tightest in extension. During a single-bundle PCL reconstruction targeting the ALB, the graft is typically tensioned and fixed at 90 degrees of flexion while an anterior drawer force is applied to restore the normal tibial step-off.
Question 54:
Which bearing surface combination in Total Hip Arthroplasty (THA) is associated with the lowest volumetric wear rate in laboratory simulator studies?
Options:
- Cobalt-chrome on highly cross-linked polyethylene
- Ceramic on highly cross-linked polyethylene
- Cobalt-chrome on conventional polyethylene
- Ceramic on ceramic
- Metal on metal
Correct Answer: Ceramic on ceramic
Explanation:
Ceramic-on-ceramic (CoC) bearing surfaces exhibit the lowest volumetric wear rates of any bearing combination (typically < 1 cubic mm/year). However, they carry unique risks, such as squeaking and catastrophic ceramic fracture. Modern highly cross-linked polyethylene also has very low wear and is more commonly used clinically to avoid the risks of CoC.
Question 55:
Articular cartilage has specialized zones with varying structure and function. Which of the following best describes the collagen fiber orientation and primary collagen type in the superficial zone of articular cartilage?
Options:
- Perpendicular to the joint surface, Type I
- Parallel to the joint surface, Type II
- Randomly oriented, Type II
- Perpendicular to the joint surface, Type II
- Parallel to the joint surface, Type I
Correct Answer: Parallel to the joint surface, Type II
Explanation:
The superficial (tangential) zone of articular cartilage makes up 10-20% of the thickness. The collagen fibers (primarily Type II, like the rest of hyaline cartilage) are oriented parallel to the joint surface to resist shear forces. The deep zone fibers are oriented perpendicularly to anchor the cartilage to the subchondral bone.
Question 56:
A 32-year-old female falls from a height and sustains a talar neck fracture with subtalar and tibiotalar joint dislocation, but the talonavicular joint remains intact. What is the Hawkins classification of this fracture and the approximate associated risk of avascular necrosis (AVN)?
Options:
- Hawkins Type II, 20-50% AVN risk
- Hawkins Type III, 50-100% AVN risk
- Hawkins Type IV, 50-100% AVN risk
- Hawkins Type II, 0-10% AVN risk
- Hawkins Type III, 20-50% AVN risk
Correct Answer: Hawkins Type III, 50-100% AVN risk
Explanation:
Hawkins Type I: Nondisplaced (0-10% AVN). Type II: Subtalar dislocation/subluxation (20-50% AVN). Type III: Subtalar and tibiotalar dislocation (50-100% AVN). Type IV: Subtalar, tibiotalar, and talonavicular dislocation (50-100% AVN). The scenario describes a Type III fracture.
Question 57:
A 60-year-old male presents with dorsal midfoot pain and limited dorsiflexion of the great toe. Radiographs demonstrate dorsal osteophytes and joint space narrowing at the first metatarsophalangeal (MTP) joint, consistent with Coughlin and Shurnas Grade 3 hallux rigidus. Conservative management has failed. What is the most reliable surgical treatment for long-term pain relief?
Options:
- Cheilectomy
- Moberg osteotomy
- First MTP joint arthrodesis
- Keller resection arthroplasty
- Synthetic hemiarthroplasty
Correct Answer: First MTP joint arthrodesis
Explanation:
For advanced (Grade 3 or 4) hallux rigidus with severe pain and functional limitation, arthrodesis of the first MTP joint is the gold standard and most reliable surgical procedure for definitive pain relief. Cheilectomy is indicated for earlier grades (Grade 1 and 2) with primarily dorsal impingement pain.
Question 58:
A 72-year-old male with known cervical spondylosis is involved in a hyperextension motor vehicle accident. He presents with bilateral upper extremity weakness (hands worse than arms) and relative sparing of lower extremity strength. What is the classic anatomic explanation for this specific pattern of weakness?
Options:
- Damage to the anterior horn cells in the cervical spine
- Ischemia of the anterior spinal artery
- Selective damage to the central fibers of the corticospinal tract
- Injury to the dorsal columns
- Avulsion of the C8-T1 nerve roots
Correct Answer: Selective damage to the central fibers of the corticospinal tract
Explanation:
Central Cord Syndrome is typically caused by a hyperextension injury in a stenotic cervical spine. The corticospinal tract has a somatotopic organization where the cervical (upper extremity) motor fibers are located more medially (centrally) and the sacral/lumbar (lower extremity) fibers are located more laterally. Therefore, central cord damage disproportionately affects the upper extremities.
Question 59:
De Quervain's tenosynovitis involves inflammation of the first dorsal compartment of the wrist. Which tendons are located within this compartment?
Options:
- Extensor pollicis longus and extensor pollicis brevis
- Abductor pollicis longus and extensor pollicis brevis
- Abductor pollicis longus and abductor pollicis brevis
- Extensor carpi radialis longus and brevis
- Extensor digitorum communis and extensor indicis proprius
Correct Answer: Abductor pollicis longus and extensor pollicis brevis
Explanation:
The first dorsal compartment contains the Abductor Pollicis Longus (APL) and Extensor Pollicis Brevis (EPB). The Extensor Pollicis Longus (EPL) is in the third compartment and routes around Lister's tubercle. De Quervain's is classically diagnosed with a positive Finkelstein's or Eichhoff's test.
Question 60:
A 14-year-old boy presents with a permeative lytic lesion in the diaphysis of the femur with an 'onion skin' periosteal reaction. A biopsy confirms small blue round cells. Which chromosomal translocation is pathognomonic for this tumor?
Options:
- t(11;22)
- t(X;18)
- t(9;22)
- t(2;13)
- t(12;16)
Correct Answer: t(11;22)
Explanation:
The clinical and radiographic presentation is classic for Ewing Sarcoma. The pathognomonic genetic abnormality is a translocation between chromosomes 11 and 22 [t(11;22)(q24;q12)], which leads to the formation of the EWS-FLI1 fusion protein. This occurs in approximately 85% of cases. t(X;18) is Synovial Sarcoma; t(9;22) is myxoid chondrosarcoma (and CML); t(2;13) is Alveolar Rhabdomyosarcoma; t(12;16) is Myxoid Liposarcoma.
Question 61:
A 55-year-old poorly controlled diabetic male presents with a massively swollen, warm, and erythematous right foot. He denies any recent trauma or open wounds. Laboratory studies reveal a normal white blood cell count and normal inflammatory markers. Radiographs demonstrate fragmentation and subluxation at the tarsometatarsal joints. What is the most appropriate initial management for this condition?
Options:
- Intravenous broad-spectrum antibiotics
- Total contact casting and non-weight bearing
- Urgent arthrodesis of the midfoot
- Below-knee amputation
- Magnetic resonance imaging to definitively rule out osteomyelitis
Correct Answer: Total contact casting and non-weight bearing
Explanation:
This patient is presenting with acute Charcot arthropathy (Eichenholtz stage 0 or 1), characterized by a swollen, warm, erythematous foot with radiographic evidence of joint fragmentation, in the setting of normal inflammatory markers. The mainstay of initial treatment for acute Charcot arthropathy is strict immobilization and off-loading, typically achieved with a total contact cast (TCC). This prevents progressive deformity while the acute inflammatory phase resolves. Surgery is contraindicated during the acute inflammatory phase due to the high risk of hardware failure and worsening bone destruction.
Question 62:
A 30-year-old male is involved in a motor vehicle collision. A cervical spine CT reveals bilateral pars interarticularis fractures of C2 with 4 mm of anterior translation and slight angulation of C2 on C3. The presumed mechanism is hyperextension and axial loading followed by severe flexion. According to the Levine-Edwards classification, what type of fracture does this represent?
Options:
- Type I
- Type II
- Type IIA
- Type III
- Type IV
Correct Answer: Type II
Explanation:
This is a Levine-Edwards Type II traumatic spondylolisthesis of the axis (Hangman's fracture). Type I involves <3 mm translation with no angulation (mechanism: hyperextension/axial loading). Type II involves >3 mm translation and significant angulation, caused by hyperextension and axial load followed by severe flexion and compression. Type IIA shows severe angulation with minimal translation (mechanism: flexion/distraction) and typically worsens with traction. Type III involves severe translation/angulation accompanied by bilateral C2-C3 facet dislocations.
Question 63:
A 13-year-old female undergoes in situ percutaneous pinning for a stable slipped capital femoral epiphysis (SCFE). Six months postoperatively, she presents with progressive hip stiffness, pain, and a severely restricted range of motion. Anteroposterior radiographs of the pelvis demonstrate concentric joint space narrowing of the affected hip to less than 3 mm. What is the most likely diagnosis?
Options:
- Avascular necrosis of the femoral head
- Chondrolysis
- Hardware failure
- Femoroacetabular impingement
- Septic arthritis
Correct Answer: Chondrolysis
Explanation:
Chondrolysis is a devastating complication of SCFE, characterized by acute cartilage necrosis resulting in progressive joint space narrowing (typically defined as <3 mm), severe stiffness, and pain. It is strongly associated with unrecognized intra-articular pin penetration during fixation. While avascular necrosis (AVN) is another severe complication, it typically presents with segmental collapse and sclerosis of the femoral head rather than isolated symmetric joint space narrowing.
Question 64:
A 30-year-old female presents with knee pain. Radiographs reveal an eccentric, lytic, epiphyseal lesion in the distal femur that extends to the subchondral bone without a sclerotic margin. Biopsy reveals numerous multinucleated giant cells interspersed in a background of mononuclear stromal cells. Which cell type represents the true neoplastic component of this tumor?
Options:
- Osteoclasts
- Osteoblasts
- Mononuclear stromal cells
- Macrophages
- Chondroblasts
Correct Answer: Mononuclear stromal cells
Explanation:
The diagnosis is Giant Cell Tumor (GCT) of bone. Despite the striking histological presence of multinucleated giant cells (which give the tumor its name), the true neoplastic cells are the mononuclear stromal cells. These spindle-shaped stromal cells express high levels of RANKL (Receptor Activator of Nuclear factor Kappa-B Ligand), which recruits and stimulates normal host macrophages to fuse into the reactive, bone-resorbing multinucleated giant cells.
Question 65:
A 25-year-old male manual laborer complains of persistent dorsal, central wrist pain. Radiographs show sclerosis of the lunate with preservation of its height and architecture. Ulnar variance is determined to be negative 2 mm. What is the most appropriate surgical intervention to halt disease progression?
Options:
- Proximal row carpectomy
- Scaphoid-trapezium-trapezoid (STT) arthrodesis
- Radial shortening osteotomy
- Total wrist arthrodesis
- Lunate excision and silastic arthroplasty
Correct Answer: Radial shortening osteotomy
Explanation:
The patient has Kienbock's disease (avascular necrosis of the lunate), Lichtman Stage II (sclerosis without collapse), in the setting of negative ulnar variance. A joint leveling procedure, such as a radial shortening osteotomy or ulnar lengthening, is the treatment of choice. This mechanically unloads the radiolunate joint, theoretically promoting revascularization of the lunate and halting disease progression before carpal collapse occurs.
Question 66:
A 60-year-old male who underwent a metal-on-metal total hip arthroplasty 8 years ago presents with groin pain and a palpable anterior mass. Serum cobalt and chromium levels are significantly elevated. A MARS MRI shows a thick-walled, cystic mass communicating with the joint. What is the characteristic histological finding associated with this condition?
Options:
- Abundant acute inflammatory infiltrate with neutrophils
- Aseptic Lymphocyte-Dominated Vasculitis-Associated Lesions (ALVAL)
- Monoclonal sheets of plasma cells
- Multinucleated foreign body giant cells containing birefringent polyethylene debris
- Malignant spindle cells with high mitotic activity
Correct Answer: Aseptic Lymphocyte-Dominated Vasculitis-Associated Lesions (ALVAL)
Explanation:
The clinical picture describes an adverse local tissue reaction (ALTR) or 'pseudotumor' associated with metal-on-metal bearing surfaces. Histologically, this immune-mediated delayed-type hypersensitivity response (Type IV) to metal debris is characterized by Aseptic Lymphocyte-Dominated Vasculitis-Associated Lesions (ALVAL), demonstrating a robust perivascular lymphocytic infiltrate and tissue necrosis.
Question 67:
A 22-year-old collegiate athlete undergoes an anterior cruciate ligament (ACL) reconstruction using a bone-patellar tendon-bone autograft. During the biological process of 'ligamentization', at approximately what postoperative time frame does the graft reach its nadir of mechanical strength, placing the patient at highest risk for traumatic rupture?
Options:
- 1-2 weeks
- 3-4 weeks
- 6-12 weeks
- 6-9 months
- 12-18 months
Correct Answer: 6-12 weeks
Explanation:
The 'ligamentization' of a tendon autograft used for ACL reconstruction consists of three phases: necrosis, proliferation/revascularization, and remodeling/maturation. During the proliferation phase, which occurs approximately 6 to 12 weeks postoperatively, there is intense cellular activity, revascularization, and collagen degradation/resynthesis. Because the original collagen architecture is being broken down before the new organized matrix matures, the graft is mechanically at its weakest during this 6 to 12 week window.
Question 68:
A 28-year-old female is involved in a high-speed collision. She sustains a talar neck fracture with complete subluxation of the subtalar joint; however, the tibiotalar (ankle) joint remains congruous. Based on the Hawkins classification, what is the approximate risk of avascular necrosis (AVN) of the talar body?
Options:
- 0-10%
- 20-50%
- 70-100%
- 100%
Correct Answer: 20-50%
Explanation:
The patient has a Hawkins Type II talar neck fracture, defined by subluxation or dislocation of the subtalar joint with an intact ankle joint. The reported risk of AVN for Hawkins Type II fractures is classically between 20% and 50%. Type I (nondisplaced) has a 0-10% risk, Type III (dislocation of both subtalar and ankle joints) has a 70-100% risk, and Type IV (Type III plus talonavicular dislocation) also carries an extraordinarily high risk nearing 100%.
Question 69:
An adult tibia shaft fracture is treated with a statically locked intramedullary nail, creating a biomechanical environment that allows for micromotion at the fracture site. This environment promotes secondary bone healing. What is the correct physiological sequence of secondary bone healing?
Options:
- Inflammation, soft callus, hard callus, remodeling
- Soft callus, hard callus, inflammation, remodeling
- Inflammation, hard callus, soft callus, remodeling
- Inflammation, remodeling, soft callus, hard callus
- Hard callus, soft callus, remodeling, inflammation
Correct Answer: Inflammation, soft callus, hard callus, remodeling
Explanation:
Secondary bone healing occurs when there is relative stability (micromotion) at the fracture site, promoting callus formation. The classic sequential phases are: 1) Inflammation (hematoma formation and cytokine release), 2) Soft callus (fibrocartilage generation via chondrogenesis), 3) Hard callus (conversion of cartilage to woven bone via endochondral ossification), and 4) Remodeling (replacement of woven bone with lamellar bone via osteoclast and osteoblast activity).
Question 70:
A 25-year-old running back sustains a forceful plantarflexion injury to his foot. A weight-bearing AP radiograph reveals a 3 mm diastasis between the base of the first and second metatarsals. He is diagnosed with a Lisfranc injury. Which ligament represents the primary structural stabilizer of this joint complex?
Options:
- Dorsal Lisfranc ligament
- Plantar Lisfranc ligament
- Interosseous Lisfranc ligament
- Spring ligament
- Long plantar ligament
Correct Answer: Interosseous Lisfranc ligament
Explanation:
The Lisfranc ligament complex connects the medial cuneiform to the base of the second metatarsal. It consists of three bands: dorsal, interosseous, and plantar. The interosseous Lisfranc ligament is the thickest, strongest, and primary structural stabilizer of the complex. The plantar band is the second strongest, while the dorsal band is the weakest and often the first to fail during hyperplantarflexion injuries.
Question 71:
A 45-year-old male presents to the emergency department with acute onset of severe bilateral sciatica, saddle anesthesia, and urinary retention with overflow incontinence following heavy lifting. An urgent MRI reveals a massive L4-L5 disc extrusion causing central canal stenosis and compression of the cauda equina. Surgical decompression should ideally be performed within what time frame to maximize the probability of neurological recovery, particularly bladder and bowel function?
Options:
- 12 hours
- 24 to 48 hours
- 72 hours
- 1 week
- 2 weeks
Correct Answer: 24 to 48 hours
Explanation:
Cauda equina syndrome is an absolute surgical emergency. Current literature and clinical guidelines dictate that urgent surgical decompression must be performed, ideally within 24 to 48 hours of symptom onset. Intervening within this critical window provides the best chance for the recovery of bladder, bowel, and sexual function, as well as the resolution of motor and sensory deficits.
Question 72:
When applying the Ponseti casting method for the conservative management of congenital talipes equinovarus (clubfoot), the deformity is corrected in a specific sequential order. Which component of the deformity is corrected LAST?
Options:
- Cavus
- Adductus
- Varus
- Equinus
Correct Answer: Equinus
Explanation:
The Ponseti method utilizes serial casting to gradually stretch contracted tissues. The sequence of correction follows the acronym CAVE: Cavus (corrected first by supinating the forefoot and elevating the first ray to align with the hindfoot), Adductus, Varus, and finally Equinus. Equinus is corrected last to prevent a rocker-bottom deformity, and it frequently requires a percutaneous Achilles tenotomy to achieve adequate dorsiflexion.
Question 73:
A 65-year-old male complains of severe mechanical back pain and profound fatigue. Laboratory tests show anemia, hypercalcemia, and an elevated M-spike on serum protein electrophoresis. Plain radiographs demonstrate multiple 'punched-out' lytic lesions in the skull and spine. What is the current imaging modality of choice to accurately assess the extent of skeletal burden in this disease?
Options:
- Technetium-99m bone scintigraphy
- Whole-body low-dose CT or MRI
- Gallium-67 scan
- Dual-energy x-ray absorptiometry (DEXA)
- Positron emission tomography without CT
Correct Answer: Whole-body low-dose CT or MRI
Explanation:
The diagnosis is Multiple Myeloma. The characteristic bone lesions are purely osteolytic, caused by myeloma cells stimulating osteoclasts (via RANKL) while inhibiting osteoblast activity (via DKK1 and sFRP-2). Because there is little to no reactive osteoblastic bone formation, traditional Technetium-99m bone scans frequently yield false negatives. Therefore, whole-body low-dose CT, whole-body MRI, or PET-CT are the modalities of choice to identify myeloma bone lesions.
Question 74:
A 30-year-old carpenter sustains a volar laceration over the proximal phalanx of his index finger, severing both the flexor digitorum superficialis (FDS) and flexor digitorum profundus (FDP) tendons (Zone II). Following primary surgical repair, the hand therapist initiates a rehabilitation protocol that uses a dorsal blocking splint, allowing for active extension and utilizing rubber band traction attached to the fingernail to achieve passive flexion. Which protocol is being utilized?
Options:
- Kleinert protocol
- Duran protocol
- Early active motion protocol
- Immobilization protocol
- Strickland protocol
Correct Answer: Kleinert protocol
Explanation:
The Kleinert protocol is a dynamic splinting program used after flexor tendon repair. It involves a dorsal blocking splint (which prevents passive extension past a certain angle) combined with rubber bands attached to the patient's fingernails and anchored volarly. This allows the patient to perform active extension against the resistance of the rubber band, while the band passively pulls the finger back into flexion, protecting the repair.
Question 75:
During a primary total knee arthroplasty (TKA), the surgeon determines the rotational alignment of the femoral component. If the surgeon chooses to use the surgical epicondylar axis (SEA) to establish rotation, what specific anatomical landmarks must be connected?
Options:
- The medial epicondylar sulcus and the most prominent point of the lateral epicondyle
- The most prominent point of the medial epicondyle and the most prominent point of the lateral epicondyle
- The center of the trochlear groove and the apex of the intercondylar notch
- The posterior-most aspects of the medial and lateral femoral condyles
- The medial collateral ligament insertion and the fibular head
Correct Answer: The medial epicondylar sulcus and the most prominent point of the lateral epicondyle
Explanation:
Establishing correct femoral rotation is critical for patellar tracking and flexion gap balance in TKA. The Surgical Epicondylar Axis (SEA) connects the sulcus on the medial epicondyle (the origin of the deep MCL) to the most prominent point on the lateral epicondyle. This differs from the Clinical Epicondylar Axis, which connects the most prominent points of both the medial and lateral epicondyles.
Question 76:
A 25-year-old collegiate baseball pitcher presents with vague, deep shoulder pain and mechanical symptoms (clicking) during the late cocking phase of throwing. A magnetic resonance arthrogram demonstrates a tear of the superior labrum with complete detachment of the biceps tendon anchor from the superior glenoid rim. According to the Snyder classification, this represents which type of SLAP lesion?
Options:
- Type I
- Type II
- Type III
- Type IV
- Type V
Correct Answer: Type II
Explanation:
Type II SLAP (Superior Labrum Anterior to Posterior) lesions are the most common and are characterized by detachment of the superior labrum and the long head of the biceps anchor from the superior glenoid. Type I involves degenerative fraying with an intact biceps anchor. Type III is a bucket-handle tear of the labrum with an intact biceps anchor. Type IV is a bucket-handle tear of the labrum that extends directly into the substance of the biceps tendon.
Question 77:
A 40-year-old pedestrian is struck by a motor vehicle, sustaining a severe valgus force to the knee. Computed tomography reveals a pure central depression fracture of the lateral tibial plateau, with the lateral cortical rim remaining intact. According to the Schatzker classification system, how is this fracture pattern classified?
Options:
- Schatzker I
- Schatzker II
- Schatzker III
- Schatzker IV
- Schatzker V
Correct Answer: Schatzker III
Explanation:
Schatzker III fractures are pure central depressions of the lateral tibial plateau without an associated split of the lateral margin. Schatzker I is a pure wedge split of the lateral plateau. Schatzker II is a split-depression of the lateral plateau (most common). Schatzker IV involves the medial plateau. Schatzker V is a bicondylar fracture with intact metaphyseal-diaphyseal continuity. Schatzker VI involves metaphyseal-diaphyseal dissociation.
Question 78:
Parathyroid hormone (PTH) plays a central role in maintaining systemic calcium homeostasis by acting on bone, kidneys, and the intestines. What is the direct mechanism by which continuously elevated PTH levels stimulate bone resorption?
Options:
- Directly binding to receptors on mature osteoclasts to increase their resorptive activity
- Binding to receptors on osteoblasts, causing upregulation of RANKL, which subsequently activates osteoclasts
- Downregulating the expression of RANKL and upregulating osteoprotegerin (OPG)
- Stimulating the release of calcitonin from the thyroid gland
- Inducing rapid apoptosis of osteoblasts
Correct Answer: Binding to receptors on osteoblasts, causing upregulation of RANKL, which subsequently activates osteoclasts
Explanation:
Osteoclasts do not possess receptors for PTH. Instead, continuous PTH binds to PTH receptors (PTH1R) on the surface of osteoblasts. This binding stimulates osteoblasts to upregulate the expression of RANKL (and downregulate OPG). RANKL then binds to the RANK receptor on osteoclast precursors, promoting their differentiation, fusion, and activation into mature bone-resorbing osteoclasts.
Question 79:
A 35-year-old recreational athlete sustains an acute tear of his Achilles tendon during a tennis match. After discussing the risks and benefits, he chooses non-operative management utilizing a modern early functional rehabilitation protocol. Historically, compared to primary open surgical repair, non-operative management carries a significantly higher risk of which of the following complications?
Options:
- Deep vein thrombosis
- Sural nerve entrapment
- Re-rupture of the tendon
- Deep surgical site infection
- Loss of extreme ankle plantarflexion strength
Correct Answer: Re-rupture of the tendon
Explanation:
Historically, non-operative treatment of acute Achilles tendon ruptures was associated with a higher rate of re-rupture compared to surgical repair, while surgery carries higher risks of wound complications, infections, and sural nerve injury. It should be noted, however, that recent high-quality studies using aggressive early functional rehabilitation protocols have demonstrated that the re-rupture rate in non-operative patients approaches that of operative patients.
Question 80:
A 65-year-old male presents with bilateral hand clumsiness, gait instability, and frequent falls. Physical examination reveals hyperreflexia in all four extremities, a positive Hoffman sign bilaterally, and an unsteady, broad-based gait. He requires the use of a cane at all times to ambulate safely, but he is not restricted to a wheelchair. What is his Nurick classification grade for cervical spondylotic myelopathy?
Options:
- Grade 1
- Grade 2
- Grade 3
- Grade 4
- Grade 5
Correct Answer: Grade 4
Explanation:
The Nurick classification assesses gait impairment in cervical spondylotic myelopathy. Grade 0: root symptoms only. Grade 1: signs of cord involvement, normal gait. Grade 2: mild gait involvement, able to be employed. Grade 3: gait abnormality preventing employment, but walks unassisted. Grade 4: requires assistance (e.g., cane, walker, or another person) to ambulate. Grade 5: wheelchair-bound or bedridden. Because this patient requires a cane, he is Nurick Grade 4.
Question 81:
A 35-year-old male presents with a progressive, dull ache in his proximal femur. Radiographs reveal a lytic lesion in the femoral head epiphysis with a sclerotic margin. Biopsy shows tumor cells with abundant clear cytoplasm and central nuclei, interspersed with coarse woven bone and osteoclast-like giant cells. What is the most appropriate treatment?
Options:
- Intralesional curettage and bone grafting.
- Wide surgical resection.
- Preoperative radiation followed by curettage.
- Chemotherapy and limb salvage.
- Radiofrequency ablation.
Correct Answer: Wide surgical resection.
Explanation:
Clear cell chondrosarcoma typically presents in the epiphyses of long bones (most commonly the proximal femur or humerus) in young adults. It is considered a low-grade malignant bone tumor. Standard treatment is wide surgical resection, as intralesional curettage results in an unacceptably high local recurrence rate.
Question 82:
A 28-year-old male is involved in a high-speed MVC and sustains a neck injury. CT scan shows a fracture through the pars interarticularis of C2 bilaterally. There is 4 mm of anterior translation of C2 on C3, and 12 degrees of severe kyphotic angulation. According to the Levine-Edwards classification, what is the injury type and the recommended initial treatment?
Options:
- Type II; application of halo vest and gentle traction.
- Type IIA; application of halo vest with slight compression and extension, strictly avoiding traction.
- Type III; immediate open reduction and internal fixation.
- Type I; rigid cervical collar for 6 weeks.
- Type IIA; anterior cervical discectomy and fusion (ACDF).
Correct Answer: Type IIA; application of halo vest with slight compression and extension, strictly avoiding traction.
Explanation:
The Levine-Edwards classification categorizes traumatic spondylolisthesis of the axis (Hangman's fracture). Type IIA is characterized by minimal translation but severe angulation, signifying severe disruption of the C2-C3 disc and posterior longitudinal ligament. Traction is strictly contraindicated in Type IIA injuries as it can cause over-distraction and neurologic injury. Appropriate treatment is a halo vest applied with gentle compression and extension.
Question 83:
A 24-year-old football player falls forward over his plantar-flexed foot. He complains of severe midfoot pain. Radiographs demonstrate a small avulsion fracture at the base of the second metatarsal. The ligament primarily injured in this pathology originates from which structure and inserts onto which structure?
Options:
- Medial cuneiform to the base of the second metatarsal.
- Lateral cuneiform to the base of the third metatarsal.
- Cuboid to the base of the fourth metatarsal.
- Navicular to the medial cuneiform.
- Base of the first metatarsal to the base of the second metatarsal.
Correct Answer: Medial cuneiform to the base of the second metatarsal.
Explanation:
The Lisfranc ligament is an interosseous ligament connecting the lateral aspect of the medial cuneiform to the medial aspect of the base of the second metatarsal. It is the keystone structure stabilizing the tarsometatarsal joint complex. An avulsion off the base of the 2nd MT (the 'fleck sign') is pathognomonic for a Lisfranc injury.
Question 84:
A 65-year-old female presents with severe base of thumb pain. Radiographs reveal advanced thumb carpometacarpal (CMC) joint arthritis with complete loss of joint space, significant subluxation, and cystic changes. Additionally, there is complete loss of joint space and osteophyte formation at the scaphotrapezial trapezoid (STT) joint. According to the Eaton-Littler classification, what stage is this disease?
Options:
- Stage I
- Stage II
- Stage III
- Stage IV
- Stage V
Correct Answer: Stage IV
Explanation:
The Eaton-Littler classification for thumb CMC arthritis: Stage I (subtle widening, no subluxation), Stage II (slight narrowing, <1/3 subluxation, osteophytes <2mm), Stage III (marked narrowing, >1/3 subluxation, osteophytes >2mm), Stage IV (pantrapezial arthritis, which involves the STT joint in addition to the CMC joint).
Question 85:
A 9-year-old boy with panhypopituitarism and a BMI of 32 presents with right knee pain and a limp. He is diagnosed with a right slipped capital femoral epiphysis (SCFE). Which of the following is the strongest indication for prophylactic in situ pinning of his contralateral asymptomatic left hip?
Options:
- His BMI greater than 30.
- His age at presentation and endocrine disorder.
- The degree of slip on the symptomatic right side.
- The presence of right knee pain instead of hip pain.
- His male gender.
Correct Answer: His age at presentation and endocrine disorder.
Explanation:
Prophylactic pinning of the contralateral hip in SCFE is recommended for patients at very high risk for a subsequent bilateral slip. High-risk factors include underlying endocrine disorders (e.g., hypothyroidism, panhypopituitarism, renal osteodystrophy) and young age at presentation (typically <10 years old for boys or <11 for girls).
Question 86:
Bone Morphogenetic Proteins (BMPs) are used as osteoinductive agents in spine fusions and nonunion surgery. Which of the following BMPs is an FDA-approved recombinant protein utilized in anterior lumbar interbody fusion (ALIF) within a specific carrier?
Options:
- rhBMP-2
- rhBMP-3
- rhBMP-4
- rhBMP-6
- rhBMP-9
Correct Answer: rhBMP-2
Explanation:
rhBMP-2 (recombinant human bone morphogenetic protein-2) is FDA approved for use in single-level anterior lumbar interbody fusions (ALIF) with an absorbable collagen sponge carrier and a specific interbody cage. It acts as an osteoinductive agent by stimulating mesenchymal stem cells to differentiate into osteoblasts.
Question 87:
A 42-year-old male sustains a high-energy distal tibia pilon fracture. An anterolateral surgical approach is planned for open reduction and internal fixation. During this approach, which nerve is at greatest risk of iatrogenic injury as it crosses the operative field?
Options:
- Sural nerve
- Deep peroneal nerve
- Superficial peroneal nerve
- Saphenous nerve
- Tibial nerve
Correct Answer: Superficial peroneal nerve
Explanation:
The anterolateral approach to the distal tibia uses the internervous plane between the superficial peroneal nerve (lateral compartment) and deep peroneal nerve (anterior compartment). The superficial peroneal nerve crosses the surgical field from medial to lateral as it travels distally over the ankle, placing it at high risk of iatrogenic injury.
Question 88:
A 28-year-old athlete undergoes evaluation for a knee injury. MRI confirms an isolated tear of the posterior cruciate ligament (PCL). Which of the following statements regarding the biomechanics of the PCL is correct?
Options:
- The anterolateral bundle is tight in extension and loose in flexion.
- The posteromedial bundle is the primary restraint to posterior tibial translation at 90 degrees of flexion.
- The anterolateral bundle is tight in flexion and loose in extension.
- The PCL provides primary restraint to varus stress at 30 degrees of flexion.
- The posteromedial bundle is tight in flexion and loose in extension.
Correct Answer: The anterolateral bundle is tight in flexion and loose in extension.
Explanation:
The PCL consists of two main bundles: the larger anterolateral (AL) bundle and the smaller posteromedial (PM) bundle. Biomechanically, the AL bundle is tight in flexion and loose in extension, making it the primary restraint to posterior translation at 90 degrees of flexion. The PM bundle is tight in extension and loose in flexion.
Question 89:
A 55-year-old male who underwent a metal-on-metal total hip arthroplasty 6 years ago presents with new-onset groin pain and a palpable mass. Workup reveals an aseptic lymphocyte-dominated vasculitis-associated lesion (ALVAL). Which type of hypersensitivity reaction is the primary driver of this pathology?
Options:
- Type I
- Type II
- Type III
- Type IV
- Type V
Correct Answer: Type IV
Explanation:
ALVAL (aseptic lymphocyte-dominated vasculitis-associated lesion), also known clinically as a pseudotumor in the context of metal-on-metal hip replacements, is primarily mediated by a Type IV (delayed, T-cell mediated) hypersensitivity reaction to metal wear debris (usually cobalt and chromium ions).
Question 90:
A 19-year-old male presents with severe night pain in his right mid-tibia that is predictably relieved by ibuprofen. Imaging shows a 0.8 cm radiolucent nidus surrounded by dense reactive sclerosis. The pain associated with this lesion is mediated by the overproduction of which of the following?
Options:
- Interleukin-6
- Tumor Necrosis Factor-alpha
- Prostaglandin E2
- Substance P
- Bradykinin
Correct Answer: Prostaglandin E2
Explanation:
Osteoid osteoma is a benign bone-forming tumor characterized by a small nidus (<1.5 cm) that produces high levels of Prostaglandin E2 (PGE2) via COX-2 expression. This robust PGE2 production causes intense vasodilation and localized pain, which is characteristically worse at night and dramatically responsive to NSAIDs.
Question 91:
A 32-year-old female falls from a height. CT of the lumbar spine reveals an L1 burst fracture. There is splaying of the spinous processes on the AP radiograph. MRI confirms disruption of the posterior ligamentous complex (PLC). Neurological examination is completely normal. According to the Thoracolumbar Injury Classification and Severity (TLICS) score, what is her total score and the recommended management?
Options:
- Score 2; nonoperative management.
- Score 4; operative or nonoperative management.
- Score 5; operative management.
- Score 7; operative management.
- Score 3; nonoperative management.
Correct Answer: Score 5; operative management.
Explanation:
TLICS scoring involves three categories: Morphology: Burst fracture = 2 points. Neurology: Intact = 0 points. Posterior Ligamentous Complex (PLC): Disrupted = 3 points. Total score = 5 points. A score > 4 indicates operative management is strongly recommended.
Question 92:
A 40-year-old manual laborer presents with central dorsal wrist pain. Radiographs show sclerosis and early collapse of the lunate, without fixed scaphoid rotation or pan-carpal arthritis. Ulnar variance is -3mm. According to the Lichtman classification, this represents Stage IIIa Kienbock's disease. Which of the following is the most appropriate surgical intervention?
Options:
- Proximal row carpectomy (PRC)
- Total wrist arthrodesis
- Radial shortening osteotomy
- Scaphoid-trapezium-trapezoid (STT) fusion
- Lunate excision and silastic replacement
Correct Answer: Radial shortening osteotomy
Explanation:
In Kienbock's disease, ulnar negative variance increases sheer stress on the lunate. For Stage II and Stage IIIa (lunate collapse but preserved carpal height and normal scaphoid alignment), joint leveling procedures like a radial shortening osteotomy are indicated to offload the lunate. Salvage procedures like PRC or intercarpal fusions are reserved for later stages (IIIb or IV).
Question 93:
A 58-year-old patient with poorly controlled diabetes mellitus presents with a swollen, erythematous, and warm right foot. Radiographs reveal extensive periarticular debris, fragmentation of the tarsal bones, and early subluxation at the midfoot. According to the Eichenholtz classification, what stage of Charcot arthropathy is this, and what is the most appropriate initial treatment?
Options:
- Stage 0; urgent open reduction and internal fixation.
- Stage I; total contact casting and strict non-weight bearing.
- Stage II; custom orthotic footwear.
- Stage III; midfoot arthrodesis.
- Stage I; immediate intravenous antibiotics and surgical debridement.
Correct Answer: Stage I; total contact casting and strict non-weight bearing.
Explanation:
Eichenholtz Stage I (Development/Fragmentation) is characterized by acute inflammation, osteopenia, fragmentation, joint subluxation, and debris. Standard initial treatment in this acute phase is strict immobilization with a total contact cast (TCC) and restricted weight-bearing to prevent progressive collapse until the acute inflammation subsides and transitions to Stage II (Coalescence).
Question 94:
In a 7-year-old boy diagnosed with Legg-Calve-Perthes disease (LCPD), AP pelvis radiographs are obtained during the fragmentation phase. The lateral pillar of the femoral head maintains exactly 40% of its normal height. According to the Herring lateral pillar classification, what group does this patient fall into, and what is the general prognosis?
Options:
- Group A; good prognosis without surgical intervention.
- Group B; fair prognosis, may benefit from containment surgery.
- Group C; poor prognosis, high risk of aspherical head and premature arthritis.
- Group B/C border; excellent prognosis.
- Group A; poor prognosis requiring immediate osteotomy.
Correct Answer: Group C; poor prognosis, high risk of aspherical head and premature arthritis.
Explanation:
The Herring lateral pillar classification evaluates the height of the lateral third of the femoral head on an AP radiograph during the fragmentation stage. Group A: no loss of height. Group B: >50% lateral pillar height maintained. Group C: <50% lateral pillar height maintained. Group C patients have a poor prognosis, frequently resulting in an aspherical head and early-onset osteoarthritis.
Question 95:
Articular cartilage is highly specialized to withstand compressive and shear forces. Within the deep (basal) zone of articular cartilage, how is the type II collagen network primarily oriented relative to the articular surface?
Options:
- Parallel
- Randomly oriented
- Perpendicular
- Tangential
- Oblique at 45 degrees
Correct Answer: Perpendicular
Explanation:
The structural arrangement of articular cartilage varies by depth. In the superficial zone, collagen fibers are oriented parallel to the joint surface to resist shear forces. In the transitional (middle) zone, they are randomly oriented. In the deep (basal) zone, collagen fibers run strictly perpendicular to the articular surface, firmly anchoring the cartilage to the underlying calcified zone.
Question 96:
A 38-year-old skier falls and twists her knee. Radiographs and CT show a fracture of the lateral tibial plateau characterized by a split wedge fragment with central articular depression. According to the Schatzker classification, what type of fracture is this?
Options:
- Type I
- Type II
- Type III
- Type IV
- Type V
Correct Answer: Type II
Explanation:
Schatzker classification of tibial plateau fractures: Type I = lateral split wedge. Type II = lateral split with central depression (the most common type overall). Type III = pure lateral depression. Type IV = medial plateau fracture. Type V = bicondylar fracture. Type VI = plateau fracture with metadiaphyseal dissociation.
Question 97:
During a primary total knee arthroplasty (TKA), after making all bone cuts and placing trial components, the surgeon assesses the gaps. The knee is noted to be perfectly balanced and appropriately tensioned in full extension but is excessively tight in 90 degrees of flexion. Which of the following component adjustments is the most appropriate to correct this mismatch?
Options:
- Downsize the femoral component and translate it anteriorly.
- Upsize the femoral component and translate it posteriorly.
- Release the posterior capsule.
- Downsize the femoral component while maintaining the anterior referencing.
- Increase the thickness of the polyethylene tibial insert.
Correct Answer: Downsize the femoral component while maintaining the anterior referencing.
Explanation:
A knee that is balanced in extension but tight in flexion requires an isolated increase in the flexion gap. This is achieved by downsizing the femoral component, which selectively decreases the posterior condylar offset. Anterior referencing must be maintained to avoid notching the anterior femur. Releasing the posterior capsule primarily opens the extension gap.
Question 98:
A 29-year-old female presents with knee pain. Radiographs show an eccentric, lytic lesion in the distal femoral epiphysis extending into the metaphysis. Biopsy confirms a Giant Cell Tumor of bone. Neoadjuvant therapy with denosumab is considered. What is the mechanism of action of this medication?
Options:
- Monoclonal antibody against Vascular Endothelial Growth Factor (VEGF).
- Bisphosphonate that inhibits osteoclast farnesyl pyrophosphate synthase.
- Monoclonal antibody against Receptor Activator of Nuclear factor Kappa-B Ligand (RANKL).
- Tyrosine kinase inhibitor targeting c-kit.
- Selective estrogen receptor modulator.
Correct Answer: Monoclonal antibody against Receptor Activator of Nuclear factor Kappa-B Ligand (RANKL).
Explanation:
Denosumab is a human monoclonal antibody that binds to RANKL. In Giant Cell Tumor of Bone (GCTB), neoplastic mononuclear stromal cells secrete massive amounts of RANKL, recruiting and activating the reactive osteoclast-like multinucleated giant cells that cause bone destruction. Denosumab blocks this interaction, inhibiting osteoclast activity.
Question 99:
A 45-year-old man presents with chronic wrist pain and a history of a scaphoid fracture 10 years ago. Radiographs demonstrate a scaphoid nonunion. There is radioscaphoid arthritis and narrowing of the scaphocapitate joint, but the lunocapitate and radiolunate joints are completely preserved. According to the Scaphoid Nonunion Advanced Collapse (SNAC) classification, what is the stage of his arthritis?
Options:
- Stage I
- Stage II
- Stage III
- Stage IV
- Stage V
Correct Answer: Stage II
Explanation:
SNAC arthritis staging progresses predictably based on altered kinematics. Stage I involves arthritis localized to the radial styloid and the distal scaphoid fragment. Stage II progresses to involve the scaphocapitate joint. Stage III involves the lunocapitate joint. The radiolunate joint is uniquely spared in both SLAC and SNAC wrists due to the spherical congruency of the lunate fossa.
Question 100:
A 45-year-old male feels a 'pop' in his posterior knee while squatting. MRI reveals a radial tear at the attachment site of the posterior horn of the medial meniscus. Biomechanical studies indicate that a complete posterior root tear of the medial meniscus leads to which of the following?
Options:
- Decreased peak contact pressures in the medial compartment.
- A kinematic equivalent of a completely intact meniscus due to the intact meniscofemoral ligaments.
- Biomechanical equivalent of a total medial meniscectomy.
- Increased anterior translation of the tibia in extension.
- Subluxation of the lateral meniscus.
Correct Answer: Biomechanical equivalent of a total medial meniscectomy.
Explanation:
The posterior root firmly anchors the medial meniscus to the tibial plateau, allowing it to convert axial loads into circumferential hoop stresses. A complete root tear severely disrupts these hoop stresses, leading to functional meniscal extrusion. Biomechanically, this failure is equivalent to a total medial meniscectomy, causing drastically increased peak contact pressures.