Full Question & Answer Text (for Search Engines)
Question 1:
Wnt/beta-catenin pathway activation in mesenchymal stem cells directly promotes differentiation into which of the following cell lineages?
Options:
- Chondrocytes
- Osteoblasts
- Osteoclasts
- Adipocytes
- Fibroblasts
Correct Answer: Osteoblasts
Explanation:
Activation of the Wnt/beta-catenin signaling pathway in multipotent mesenchymal stem cells strongly directs them toward the osteoblastic lineage while simultaneously inhibiting chondrogenic and adipogenic differentiation. Beta-catenin translocates to the nucleus and interacts with TCF/LEF transcription factors to upregulate genes such as Runx2.
Question 2:
A 45-year-old male presents with a high-energy knee injury. Representative radiographs and CT cuts are shown. Based on the principles of treating a bi-condylar tibial plateau fracture with a posteromedial shear fragment, which surgical approach is most appropriately utilized first to stabilize the medial column?
Options:
- Anterolateral
- Direct medial
- Posteromedial
- Posterior (Carlson)
- Anterior midline
Correct Answer: Posteromedial
Explanation:
A posteromedial shear fragment in a bicondylar tibial plateau fracture (Schatzker VI or Moore Type I) requires a posteromedial approach for optimal buttress plating. Stabilizing the medial column first via a posteromedial approach converts the complex fracture into a lateral plateau fracture, which can then be addressed via a standard anterolateral approach.
Question 3:
Prophylactic pinning of the contralateral hip in a patient with a Slipped Capital Femoral Epiphysis (SCFE) is most strongly indicated in which of the following scenarios?
Options:
- 12-year-old male with idiopathic SCFE
- 14-year-old female with obesity
- 10-year-old male with hypothyroidism
- 15-year-old male with acute-on-chronic SCFE
- 13-year-old female with a positive Klein's line intersection
Correct Answer: 10-year-old male with hypothyroidism
Explanation:
Prophylactic pinning of the contralateral hip is generally indicated in patients at high risk for bilateral disease. Risk factors for bilateral SCFE include young age at presentation (< 10 years for girls, < 11 years for boys), endocrine disorders (e.g., hypothyroidism, growth hormone deficiency, renal osteodystrophy), and previous radiation therapy. Thus, the 10-year-old male with hypothyroidism represents the highest risk among the choices.
Question 4:
In total hip arthroplasty, the use of highly cross-linked polyethylene (HXLPE) compared to conventional ultra-high-molecular-weight polyethylene (UHMWPE) is associated with which of the following material property changes?
Options:
- Increased yield strength
- Decreased wear resistance
- Decreased fatigue crack propagation resistance
- Increased ductility
- Increased ultimate tensile strength
Correct Answer: Decreased fatigue crack propagation resistance
Explanation:
Cross-linking of polyethylene significantly improves its wear resistance, which is highly beneficial for the longevity of THA bearings. However, this process alters the mechanical properties of the material, leading to decreased fatigue crack propagation resistance, reduced ductility, decreased ultimate tensile strength, and decreased yield strength.
Question 5:
A 65-year-old man presents with progressive hand clumsiness and gait imbalance. MRI is shown. Examination reveals a positive Hoffman's sign. Which physical exam finding would most specifically suggest concomitant lumbar spinal stenosis (tandem stenosis)?
Options:
- Hyperreflexia in the lower extremities
- Absent ankle reflexes with an upgoing Babinski sign
- Sustained clonus at the ankle
- Positive Lhermitte's sign
- Preservation of lower extremity proprioception
Correct Answer: Absent ankle reflexes with an upgoing Babinski sign
Explanation:
The presence of cervical myelopathy typically causes upper motor neuron (UMN) signs in the lower extremities (hyperreflexia, clonus, positive Babinski). However, in 'tandem stenosis' (concurrent cervical myelopathy and lumbar stenosis), the lower motor neuron (LMN) signs from the lumbar compression can mask the UMN signs in the legs. Thus, absent ankle reflexes (LMN sign) coupled with an upgoing Babinski (UMN sign) is a classic presentation of tandem stenosis.
Question 6:
Biomechanical studies of the flexor tendon pulley system of the fingers indicate that which combination of pulleys is absolutely essential to prevent bowstringing and preserve full digital flexion?
Options:
- A1 and A2
- A2 and A3
- A2 and A4
- A3 and A5
- A1 and A5
Correct Answer: A2 and A4
Explanation:
The A2 and A4 pulleys are the major biomechanical components of the flexor tendon sheath in the digits. They arise from the periosteum of the proximal and middle phalanges, respectively. Loss of both the A2 and A4 pulleys leads to significant bowstringing, reduced excursion efficiency, and loss of full digital flexion.
Question 7:
An 18-year-old male presents with knee pain. A biopsy of a distal femoral lesion is performed. Histology is shown. The definitive diagnosis of osteosarcoma requires the presence of which of the following histologic features?
Options:
- Chondroid matrix production
- Small blue round cells with CD99 positivity
- Malignant cells directly producing osteoid
- Spindle cells arranged in a herringbone pattern
- Multinucleated giant cells in a background of mononuclear cells
Correct Answer: Malignant cells directly producing osteoid
Explanation:
The defining histologic characteristic of osteosarcoma is the production of osteoid directly by malignant mesenchymal cells. While cartilage or fibrous tissue may be present (in chondroblastic or fibroblastic variants), malignant osteoid must be identified for the diagnosis. Small blue round cells correspond to Ewing sarcoma, a herringbone pattern corresponds to fibrosarcoma, and giant cells suggest giant cell tumor of bone.
Question 8:
When comparing bone-patellar tendon-bone (BPTB) autografts to quadrupled hamstring autografts for primary anterior cruciate ligament (ACL) reconstruction, BPTB grafts are associated with a higher incidence of:
Options:
- Graft rupture
- Contralateral ACL tear
- Anterior knee pain
- Hamstring weakness
- Deep surgical site infection
Correct Answer: Anterior knee pain
Explanation:
Bone-patellar tendon-bone (BPTB) autografts are historically considered the 'gold standard' for ACL reconstruction due to excellent bone-to-bone healing and stability. However, the most commonly cited morbidity specific to BPTB autografts, compared to hamstring autografts, is a higher incidence of anterior knee pain and kneeling pain at the donor site.
Question 9:
According to the Young-Burgess classification, an Antero-Posterior Compression (APC) Type II pelvic ring injury is characterized by:
Options:
- Symphysis widening < 2.5 cm with intact posterior ligaments
- Symphysis widening > 2.5 cm with disruption of anterior sacroiliac and sacrotuberous ligaments but intact posterior sacroiliac ligaments
- Disruption of both anterior and posterior sacroiliac ligaments resulting in global instability
- Vertical translation of the hemipelvis
- A transforaminal sacral fracture on the affected side
Correct Answer: Symphysis widening > 2.5 cm with disruption of anterior sacroiliac and sacrotuberous ligaments but intact posterior sacroiliac ligaments
Explanation:
In the Young-Burgess classification, APC I involves symphyseal diastasis < 2.5 cm with intact posterior elements. APC II involves diastasis > 2.5 cm with disruption of the anterior sacroiliac, sacrotuberous, and sacrospinous ligaments, but the posterior sacroiliac ligaments remain intact, causing rotational but not vertical instability. APC III involves complete disruption of both anterior and posterior sacroiliac ligaments, leading to complete spinopelvic dissociation.
Question 10:
A 55-year-old woman presents with a symptomatic hallux valgus deformity. Weight-bearing radiographs demonstrate a hallux valgus angle (HVA) of 42 degrees, an intermetatarsal angle (IMA) of 16 degrees, and clinical hypermobility of the first tarsometatarsal (TMT) joint. What is the most appropriate surgical intervention?
Options:
- Distal chevron osteotomy
- Proximal crescentic osteotomy
- First TMT joint arthrodesis (Lapidus procedure)
- Metatarsophalangeal (MTP) joint arthrodesis
- Akin osteotomy alone
Correct Answer: First TMT joint arthrodesis (Lapidus procedure)
Explanation:
A first tarsometatarsal (TMT) joint arthrodesis, also known as a Lapidus procedure, is indicated for moderate to severe hallux valgus deformities (IMA > 15 degrees) that are accompanied by hypermobility of the first ray. It corrects the deformity at the apex (the TMT joint) and provides stability. A distal chevron is for mild deformities without hypermobility.
Question 11:
Which of the following antibiotics is NOT typically mixed with polymethylmethacrylate (PMMA) bone cement due to its thermolability and inability to withstand the exothermic curing process?
Options:
- Vancomycin
- Tobramycin
- Gentamicin
- Erythromycin
- Tetracycline
Correct Answer: Tetracycline
Explanation:
Antibiotics added to PMMA must be heat-stable because the polymerization of PMMA is highly exothermic (reaching temperatures > 80-100°C). Aminoglycosides (tobramycin, gentamicin), vancomycin, and erythromycin are heat-stable and commonly used. Tetracyclines and most beta-lactams are heat-labile and will be inactivated by the curing process.
Question 12:
A 6-month-old female is evaluated for developmental dysplasia of the hip (DDH). Radiographs are obtained. Which radiographic line is drawn vertically downwards from the lateral edge of the acetabulum to assess hip subluxation?
Options:
- Hilgenreiner's line
- Perkin's line
- Shenton's line
- Klein's line
- Southwick's angle
Correct Answer: Perkin's line
Explanation:
Perkin's line is a vertical line drawn downward from the lateral margin of the acetabulum, perpendicular to Hilgenreiner's line (which is drawn horizontally through the triradiate cartilages). In a normal hip, the ossific nucleus of the femoral head should sit in the lower medial quadrant created by the intersection of these two lines.
Question 13:
A 72-year-old female sustains a distal radius fracture. She undergoes volar locking plate fixation. Three months postoperatively, she suddenly cannot flex the interphalangeal joint of her thumb. Which tendon is most likely injured?
Options:
- Flexor carpi radialis
- Extensor pollicis longus
- Flexor pollicis longus
- Flexor digitorum profundus to the index finger
- Abductor pollicis longus
Correct Answer: Flexor pollicis longus
Explanation:
Attrition rupture of the Flexor Pollicis Longus (FPL) tendon is a known complication of volar plating of the distal radius. It typically occurs due to plate prominence distal to the watershed line, which leads to friction against the FPL tendon during thumb motion.
Question 14:
In kinematic alignment for Total Knee Arthroplasty (TKA), the primary objective is to align the components to the:
Options:
- Mechanical axis of the lower extremity
- Anatomic axis of the femur
- Epicondylar axis for femoral rotation
- Pre-arthritic natural joint lines of the femur and tibia
- Whiteside's anteroposterior line
Correct Answer: Pre-arthritic natural joint lines of the femur and tibia
Explanation:
The goal of kinematic alignment in TKA is to restore the patient's pre-arthritic constitutional alignment and joint line, matching the components to the native flexion and extension axes of the knee. This contrasts with mechanical alignment, which aims to cut the femur and tibia perpendicular to their mechanical axes to achieve a neutral overall limb axis.
Question 15:
The retrograde blood supply to the proximal pole of the scaphoid, which places it at high risk for avascular necrosis following fracture, is primarily derived from branches of which artery?
Options:
- Ulnar artery
- Anterior interosseous artery
- Superficial palmar arch
- Radial artery
- Deep palmar arch
Correct Answer: Radial artery
Explanation:
The primary blood supply to the scaphoid is derived from the radial artery, specifically via its dorsal carpal branch. The vessels enter the scaphoid at the distal pole and along the dorsal ridge, traveling retrogradely to supply the proximal pole. Thus, a proximal pole fracture often disrupts this blood supply, leading to avascular necrosis.
Question 16:
In the Meyerding classification of spondylolisthesis, a Grade III slip corresponds to a vertebral body displacement of:
Options:
- Less than 25%
- 25% to 50%
- 51% to 75%
- 76% to 100%
- Spondyloptosis (>100%)
Correct Answer: 51% to 75%
Explanation:
The Meyerding classification grades the severity of spondylolisthesis based on the percentage of forward translation of the superior vertebral body over the inferior one. Grade I is 1-25%; Grade II is 26-50%; Grade III is 51-75%; Grade IV is 76-100%; Grade V (spondyloptosis) is >100%.
Question 17:
In the context of orthopedic biomechanics, which of the following accurately defines the 'Young's modulus' of a material?
Options:
- The point at which the material permanently deforms
- The area under the stress-strain curve representing toughness
- The slope of the stress-strain curve in the elastic region
- The maximum stress a material can withstand before failure
- The point of total structural failure
Correct Answer: The slope of the stress-strain curve in the elastic region
Explanation:
Young's modulus (or elastic modulus) is a measure of the stiffness of a solid material. It is defined mathematically as the slope of the linear, elastic portion of the stress-strain curve. The higher the Young's modulus, the stiffer the material.
Question 18:
A 30-year-old female presents with pain in her distal radius. Imaging reveals an eccentric, lytic epiphyseal lesion. Biopsy shows characteristic multinucleated giant cells. Which targeted biologic therapy is FDA-approved for unresectable or recurrent cases of this specific bone tumor?
Options:
- Imatinib
- Denosumab
- Rituximab
- Doxorubicin
- Methotrexate
Correct Answer: Denosumab
Explanation:
The presentation and histology describe a Giant Cell Tumor (GCT) of bone. The neoplastic stromal cells in GCT express high levels of RANKL, which recruits and activates the reactive multinucleated giant cells (osteoclast-like cells). Denosumab is a monoclonal antibody against RANKL and is an effective targeted therapy for locally advanced, unresectable, or recurrent GCTs.
Question 19:
During an arthroscopic rotator cuff repair, the 'margin convergence' technique is most biomechanically appropriate and effective for which specific tear pattern?
Options:
- Crescent-shaped tear
- U-shaped tear
- L-shaped tear
- Reverse L-shaped tear
- Partial-thickness articular-sided tear
Correct Answer: U-shaped tear
Explanation:
Margin convergence is an arthroscopic technique popularized by Burkhart, used primarily for large U-shaped rotator cuff tears. By suturing the anterior and posterior leaves of the tear together side-to-side, the free margin of the cuff is brought closer to the greater tuberosity, significantly decreasing the strain required to fix the remaining tendon to the bone bed.
Question 20:
What is considered the most sensitive early clinical sign of acute compartment syndrome in an awake, alert patient?
Options:
- Absent distal pulses
- Pallor of the distal extremity
- Pain out of proportion to the injury with passive stretch
- Motor paralysis
- Decreased capillary refill
Correct Answer: Pain out of proportion to the injury with passive stretch
Explanation:
Pain out of proportion to the apparent injury, specifically exacerbated by passive stretch of the muscles within the involved compartment, is widely regarded as the earliest and most sensitive clinical finding of acute compartment syndrome. The '5 Ps' (pallor, pulselessness, paresthesia, paralysis) are typically late signs indicating irreversible nerve and muscle damage.
Question 21:
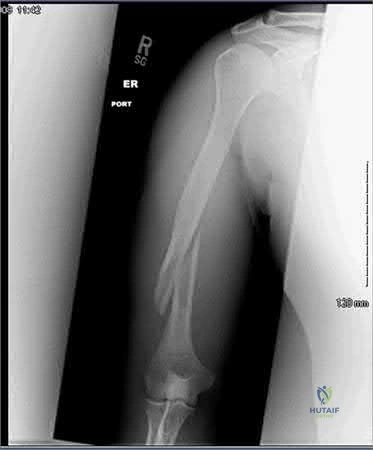
A 45-year-old male presents with a dull ache in his proximal humerus. Radiographs reveal a 6-cm intramedullary lytic lesion with rings and arcs of calcification. MRI demonstrates endosteal scalloping involving 75% of the cortical thickness. Biopsy confirms a grade II chondrosarcoma. Which of the following is the most appropriate surgical management?
Options:
- Intralesional curettage, phenol adjuvant, and bone grafting
- Wide local excision with margins
- Neoadjuvant chemotherapy followed by wide local excision
- Radiation therapy followed by intralesional excision
- Observation with serial radiographs every 6 months
Correct Answer: Wide local excision with margins
Explanation:
This patient has a Grade II (intermediate grade) chondrosarcoma of the proximal humerus. Chondrosarcomas are largely resistant to traditional chemotherapy and radiation therapy. High-grade (Grade II and III) chondrosarcomas, as well as those in the pelvis or proximal appendicular skeleton, require wide local excision with negative margins to minimize local recurrence. Intralesional curettage is reserved for benign enchondromas or selected Grade I (low-grade) chondrosarcomas in the appendicular skeleton.
Question 22:
A 28-year-old female is brought to the trauma bay after a high-speed motor vehicle collision. She is hypotensive and tachycardic. A pelvic radiograph is obtained. It demonstrates a symphyseal diastasis of 3.5 cm and widening of the anterior sacroiliac joints bilaterally. Which of the following describes the status of the posterior pelvic ligaments in this specific injury pattern?
Options:
- Both the anterior and posterior sacroiliac ligaments are disrupted.
- The anterior sacroiliac ligaments are disrupted, but the posterior sacroiliac ligaments remain intact.
- The posterior sacroiliac ligaments are disrupted, but the sacrotuberous ligaments remain intact.
- The iliolumbar ligaments are disrupted, but the sacrospinous ligaments remain intact.
- All sacroiliac and pelvic floor ligaments are disrupted.
Correct Answer: The anterior sacroiliac ligaments are disrupted, but the posterior sacroiliac ligaments remain intact.
Explanation:
The clinical scenario describes an Anteroposterior Compression Type II (APC-II) pelvic ring injury. By definition, an APC-II injury involves disruption of the pubic symphysis (typically >2.5 cm) along with tearing of the anterior sacroiliac, sacrotuberous, and sacrospinous ligaments. The critical distinguishing factor of an APC-II injury from an APC-III injury is that the strong posterior sacroiliac ligaments remain intact, providing vertical stability while allowing rotational instability.
Question 23:
A 30-year-old male sustains a traumatic knee dislocation (Schenck KD-III) after a severe hyperextension injury. Upon presentation, his knee is grossly reduced but extremely unstable. The Ankle-Brachial Index (ABI) is 0.85 in the affected limb and 1.1 in the contralateral limb. What is the most appropriate next step in management?
Options:
- Immediate closed reduction and application of a spanning external fixator
- Observation and serial Doppler examinations every 4 hours
- CT angiography of the lower extremity
- Immediate surgical exploration of the popliteal artery
- MRI of the knee to evaluate ligamentous injury
Correct Answer: CT angiography of the lower extremity
Explanation:
In the setting of a knee dislocation, vascular assessment is paramount. An Ankle-Brachial Index (ABI) less than 0.90 is highly sensitive for an arterial injury (such as a popliteal artery intimal tear or occlusion) and mandates advanced imaging, typically a CT angiogram, or immediate vascular surgery consultation. While immediate surgical exploration is indicated for hard signs of vascular injury (e.g., active hemorrhage, expanding hematoma, pulselessness), an asymmetric ABI <0.9 without hard signs is a firm indication for a CT angiogram.
Question 24:
A 40-year-old male is involved in a motor vehicle collision. A lateral cervical radiograph is obtained. Imaging reveals a traumatic spondylolisthesis of the axis (Hangman's fracture) with 15 degrees of angulation but minimal (< 1 mm) translation. According to the Levine and Edwards classification, which of the following is strictly contraindicated in the initial management of this specific fracture pattern?
Options:
- Rigid cervical collar
- Cervical traction
- Halo vest immobilization
- Immediate anterior cervical discectomy and fusion
- Posterior C1-C2 transarticular screw fixation
Correct Answer: Cervical traction
Explanation:
This describes a Type IIA Hangman's fracture (severe angulation with minimal translation). The proposed mechanism is flexion-distraction. Because of the distraction component and severe instability of the C2-C3 disc space, cervical traction is strictly contraindicated as it can cause catastrophic over-distraction and neurologic injury. The recommended treatment for Type IIA fractures is gentle compression and extension in a halo vest.
Question 25:
A 13-year-old obese male presents to the emergency department with severe acute groin and thigh pain after a minor slip. He is unable to bear weight on the affected limb, even with the assistance of crutches. Radiographs confirm a severe Slipped Capital Femoral Epiphysis (SCFE). Which of the following complications is most specifically associated with this patient's clinical presentation compared to a patient who can bear weight?
Options:
- Chondrolysis
- Avascular necrosis (AVN) of the femoral head
- Premature physeal closure
- Femoroacetabular impingement (FAI)
- Leg length discrepancy
Correct Answer: Avascular necrosis (AVN) of the femoral head
Explanation:
The inability to bear weight with or without crutches defines an 'unstable' SCFE according to the Loder classification. Unstable SCFE has a significantly higher rate of avascular necrosis (AVN) of the femoral head, with rates historically reported between 20% and 50%. Stable SCFE (where the patient can bear weight) has a very low risk of AVN (<10%).
Question 26:
A 68-year-old female presents with recurrent posterior dislocations following a primary Total Hip Arthroplasty performed via a posterior approach. Intraoperative evaluation during revision surgery reveals a well-fixed femoral component with appropriate version and offset. The acetabular component is well-fixed and positioned in 45 degrees of inclination and 5 degrees of retroversion. Which of the following is the most appropriate surgical intervention?
Options:
- Exchange the acetabular liner to a constrained liner without revising the shell
- Revise the femoral component to increase anteversion
- Revise the acetabular component to increase anteversion to approximately 20 degrees
- Advance the greater trochanter to increase abductor tension
- Apply a hip spica cast for 6 weeks
Correct Answer: Revise the acetabular component to increase anteversion to approximately 20 degrees
Explanation:
The patient's recurrent posterior dislocations are primarily due to acetabular malposition (5 degrees of retroversion). The normal 'safe zone' for acetabular anteversion is 15 to 20 degrees (Lewinnek safe zone: 15 ± 10 degrees). Because the underlying issue is structural malposition of the cup leading to posterior impingement and instability, the definitive treatment is to revise the acetabular shell to appropriate anteversion. Simply placing a constrained liner in a malpositioned shell increases the risk of liner failure or aseptic loosening.
Question 27:
A 45-year-old male presents with chronic radial-sided wrist pain. He reports a history of a 'sprained wrist' 10 years ago that was never treated. A radiograph is obtained. It shows a scaphoid nonunion with radioscaphoid arthritis localized to the radial styloid. The midcarpal joint and capitolunate articulation are preserved. Which of the following is the most appropriate surgical treatment?
Options:
- Proximal row carpectomy (PRC)
- Four-corner arthrodesis
- Total wrist arthrodesis
- Radial styloidectomy with scaphoid nonunion takedown and bone grafting
- Scaphoid excision and intercarpal ligament reconstruction
Correct Answer: Radial styloidectomy with scaphoid nonunion takedown and bone grafting
Explanation:
This describes Scaphoid Nonunion Advanced Collapse (SNAC) Stage I, characterized by arthritis limited to the articulation between the distal pole of the scaphoid and the radial styloid. The recommended treatment for SNAC Stage I is radial styloidectomy combined with scaphoid fixation and bone grafting. PRC or four-corner fusion would be indicated for more advanced stages (Stage II or III) where the midcarpal or radiocarpal joint (beyond the styloid) is involved.
Question 28:
A 55-year-old diabetic male presents with a swollen, erythematous, and warm right foot without open ulcerations. He is afebrile with a normal WBC count. Radiographs reveal fragmentation, periarticular debris, and subluxation at the tarsometatarsal joints. According to the Eichenholtz classification, what is the best initial management?
Options:
- Intravenous antibiotics and emergent irrigation and debridement
- Total contact casting and restricted weight-bearing
- Primary midfoot arthrodesis with robust internal fixation
- Surgical exostectomy of prominent bone to prevent ulceration
- Below-knee amputation
Correct Answer: Total contact casting and restricted weight-bearing
Explanation:
This patient is in the acute fragmentation phase (Stage 1) of Eichenholtz Charcot arthropathy. The classic presentation mimics infection (red, hot, swollen), but the absence of systemic signs and an intact skin envelope point toward Charcot. The mainstay of treatment in the acute fragmentation stage is immobilization and offloading, typically achieved via a total contact cast (TCC). Surgery during the acute inflammatory phase carries a high risk of failure and is generally contraindicated unless severe instability threatens the soft tissue envelope.
Question 29:
A 25-year-old male sustains a comminuted fracture of the tibial shaft. Twelve hours post-admission, he develops severe pain out of proportion to the injury, significantly exacerbated by passive stretch of the toes. Compartment syndrome is suspected. Which of the following best describes the primary pathophysiologic mechanism leading to muscle ischemia in this condition?
Options:
- Direct arterial spasm resulting from the initial trauma
- Decreased local arteriovenous pressure gradient due to increased interstitial fluid pressure
- Primary venous thrombosis leading to retrograde cellular death
- Release of oxygen free radicals causing direct myocyte apoptosis
- Systemic hypotension causing selective distal extremity hypoperfusion
Correct Answer: Decreased local arteriovenous pressure gradient due to increased interstitial fluid pressure
Explanation:
Acute compartment syndrome occurs when elevated intracompartmental pressure leads to decreased local blood flow. The primary pathophysiologic event is an increase in tissue fluid pressure that eventually surpasses venous pressure, causing venous outflow obstruction. This leads to a collapse of the local arteriovenous pressure gradient. Without a sufficient AV gradient, capillary perfusion ceases, leading to microvascular compromise and subsequent tissue ischemia. Arterial pulses often remain palpable because the pressure required to occlude a major artery is much higher than that required to arrest capillary flow.
Question 30:
A 30-year-old female undergoes biopsy of an eccentric, lytic lesion in the distal femoral epiphysis. Histology reveals numerous multinucleated giant cells in a background of mononuclear stromal cells. She is initiated on denosumab therapy prior to planned surgical intervention. What is the specific mechanism of action of denosumab in treating this lesion?
Options:
- It binds to the RANK receptor on osteoclasts, preventing activation.
- It binds directly to RANKL, preventing it from interacting with RANK on osteoclasts.
- It serves as a recombinant analog of osteoprotegerin (OPG), directly destroying neoplastic cells.
- It inhibits Vascular Endothelial Growth Factor (VEGF), leading to tumor necrosis.
- It induces apoptosis primarily in the multinucleated giant cells.
Correct Answer: It binds directly to RANKL, preventing it from interacting with RANK on osteoclasts.
Explanation:
Giant cell tumor of bone (GCTB) is characterized by neoplastic mononuclear stromal cells that express high levels of Receptor Activator of Nuclear Factor Kappa-B Ligand (RANKL). This RANKL binds to the RANK receptor on osteoclast precursors, leading to the recruitment of the numerous, non-neoplastic multinucleated giant cells that cause massive bone resorption. Denosumab is a humanized monoclonal antibody that binds directly to RANKL (not the RANK receptor), preventing it from binding to RANK, thereby inhibiting osteoclast-mediated bone destruction.
Question 31:
A 70-year-old male complains of bilateral leg and buttock pain that worsens after walking two blocks. He notes significant relief when he pushes a shopping cart. Physical examination reveals normal lower extremity pulses. Which of the following historical or physical examination findings is most specific for differentiating neurogenic claudication from vascular claudication?
Options:
- Pain relief upon standing still
- Exacerbation of pain while walking downhill
- Presence of 'stocking-glove' sensory deficit
- Diminished ankle reflexes
- Cramping pain strictly localized to the calf
Correct Answer: Exacerbation of pain while walking downhill
Explanation:
Differentiating neurogenic claudication (lumbar spinal stenosis) from vascular claudication relies on postural changes. Neurogenic claudication is exacerbated by lumbar extension, which decreases the cross-sectional area of the spinal canal and neural foramina. Walking downhill requires lumbar extension, thus exacerbating neurogenic claudication. Conversely, walking uphill or leaning forward (shopping cart sign) induces lumbar flexion, opening the canal and providing relief. Vascular claudication is typically relieved simply by standing still, regardless of spine posture, and is reliably reproduced by a specific distance of walking.
Question 32:
A 22-year-old collegiate baseball pitcher presents with vague, deep shoulder pain and a 'dead arm' sensation. During physical examination, the O'Brien test (Active Compression Test) is performed. Which of the following findings during the O'Brien test is considered a classic positive result for a Superior Labrum Anterior Posterior (SLAP) tear?
Options:
- Pain with the arm fully internally rotated that is not relieved by external rotation
- Pain deep in the shoulder with the arm internally rotated that is relieved by external rotation
- Pain strictly localized to the acromioclavicular joint with the arm internally rotated
- Apprehension without pain when the arm is brought into external rotation and abduction
- Inability to actively elevate the arm above 90 degrees due to weakness
Correct Answer: Pain deep in the shoulder with the arm internally rotated that is relieved by external rotation
Explanation:
The O'Brien (Active Compression) test is performed with the shoulder in 90 degrees of forward flexion and 10-15 degrees of adduction. The patient resists a downward force with the arm fully internally rotated (thumb pointing down), and then the test is repeated with the arm fully externally rotated (palm up). A positive test for a SLAP tear is pain located deep within the shoulder during internal rotation that is diminished or eliminated during external rotation. Pain localized superficially to the AC joint during the internal rotation phase suggests AC joint pathology, not a SLAP tear.
Question 33:
A 2-week-old infant with idiopathic clubfoot (talipes equinovarus) is brought to the clinic to begin the Ponseti method of serial casting. According to the Ponseti principles, what is the proper sequence of correcting the components of the clubfoot deformity?
Options:
- Varus, then Cavus, then Adductus, then Equinus
- Adductus, then Varus, then Cavus, then Equinus
- Cavus, then Adductus, then Varus, then Equinus
- Equinus, then Cavus, then Adductus, then Varus
- Cavus, then Varus, then Adductus, then Equinus
Correct Answer: Cavus, then Adductus, then Varus, then Equinus
Explanation:
The Ponseti method strictly follows a specific sequence of correction, remembered by the acronym CAVE: Cavus, Adductus, Varus, Equinus. The first step is to correct the cavus by elevating the first ray, which aligns the forefoot with the hindfoot. Next, the forefoot is abducted (supinated) around the head of the talus, which simultaneously corrects the adductus and the hindfoot varus. Finally, once the foot is fully abducted, the equinus is addressed, typically requiring a percutaneous Achilles tenotomy.
Question 34:
During a primary Total Knee Arthroplasty (TKA), after the preliminary bony cuts have been made and trial components are placed, the surgeon evaluates the joint spaces. The surgeon finds that the extension gap is excessively tight, while the flexion gap is perfectly balanced and stable. Which of the following is the most appropriate next step to balance the knee?
Options:
- Resect an additional 2 mm of the proximal tibia
- Upsize the femoral component
- Resect an additional 2 mm of the distal femur
- Translate the femoral component anteriorly
- Release the anterior aspect of the superficial medial collateral ligament
Correct Answer: Resect an additional 2 mm of the distal femur
Explanation:
In TKA gap balancing, modifications to the femoral side affect only one gap, while modifications to the tibial side affect both gaps. A tight extension gap with a balanced flexion gap requires addressing structures that only affect extension. Resecting more distal femur increases the extension gap without changing the flexion gap. Releasing the posterior capsule and removing posterior femoral osteophytes are also valid soft-tissue interventions for a tight extension gap. Modifying the proximal tibia would inappropriately widen the already balanced flexion gap.
Question 35:
A 28-year-old female sustains a volar laceration to her left index finger over the proximal phalanx, resulting in severing of both the flexor digitorum profundus (FDP) and flexor digitorum superficialis (FDS) tendons in Zone II. During surgical repair, preserving or reconstructing the flexor pulley system is essential. Which two pulleys are considered mechanically critical to prevent bowstringing of the flexor tendons?
Options:
- A1 and A3
- A2 and A4
- A1 and C1
- A3 and A5
- C2 and C3
Correct Answer: A2 and A4
Explanation:
The flexor tendon pulley system of the fingers consists of five annular (A) and three cruciate (C) pulleys. The A2 and A4 pulleys are the major biomechanical workhorses that keep the flexor tendons closely apposed to the phalanges during flexion. Loss or incompetence of the A2 and A4 pulleys leads to bowstringing, significantly reducing the mechanical advantage and excursion of the tendons, leading to a profound loss of active digital flexion.
Question 36:
A 24-year-old football player sustains a hyperplantarflexion injury to his midfoot. Physical examination reveals plantar ecchymosis. Radiographs show a 3 mm diastasis between the base of the first and second metatarsals. Which of the following anatomically describes the Lisfranc ligament, which is presumed to be injured?
Options:
- It connects the medial cuneiform to the base of the first metatarsal.
- It connects the lateral aspect of the medial cuneiform to the medial base of the second metatarsal.
- It connects the intermediate cuneiform to the base of the second metatarsal.
- It connects the plantar aspect of the first metatarsal to the plantar aspect of the second metatarsal.
- It connects the navicular to the medial cuneiform.
Correct Answer: It connects the lateral aspect of the medial cuneiform to the medial base of the second metatarsal.
Explanation:
The Lisfranc ligament is a large, oblique interosseous ligament that is crucial for the stability of the midfoot. It originates on the lateral aspect of the medial cuneiform and inserts onto the medial base of the second metatarsal. Notably, there is no direct ligamentous connection between the bases of the first and second metatarsals, which makes the Lisfranc ligament the critical stabilizing structure uniting the medial column with the central column.
Question 37:
A 35-year-old male is recovering from a closed diaphyseal tibial fracture treated with a cast. Secondary bone healing is occurring via endochondral ossification, progressing through the soft callus stage. Which of the following is the predominant collagen type synthesized in the soft callus phase of fracture healing?
Options:
- Type I collagen
- Type II collagen
- Type III collagen
- Type IV collagen
- Type X collagen
Correct Answer: Type II collagen
Explanation:
Secondary bone healing involves formation of a callus. The soft callus phase is characterized by the formation of cartilaginous tissue bridging the fracture site, which stabilizes the fracture and acts as a scaffold. Because this tissue is essentially fibrocartilage and hyaline cartilage, Type II collagen is the predominant collagen type. Type X collagen is produced later by hypertrophic chondrocytes during endochondral ossification. Type I collagen predominates in mature bone (the hard callus phase).
Question 38:
A 60-year-old female presents with sudden inability to actively flex the interphalangeal (IP) joint of her thumb. She underwent open reduction and internal fixation of a distal radius fracture with a volar locking plate 8 months ago. Radiographs show the plate is well-fixed but positioned distally on the radius. What anatomical landmark was most likely violated, leading to this specific complication?
Options:
- The sigmoid notch
- Lister's tubercle
- The watershed line
- The pronator quadratus insertion
- The radial styloid groove
Correct Answer: The watershed line
Explanation:
This patient has suffered a rupture of the Flexor Pollicis Longus (FPL) tendon, which is the most common tendon rupture following volar plate fixation of the distal radius. The primary risk factor is placing the plate distal to the 'watershed line' (the bony ridge at the distal margin of the pronator fossa). When the plate sits anterior to this line, it acts as a prominent friction point against the flexor tendons, particularly the FPL, leading to attritional wear and delayed rupture.
Question 39:
A 15-year-old male undergoes wide resection of a conventional high-grade osteosarcoma of the distal femur after completing 10 weeks of neoadjuvant chemotherapy (methotrexate, doxorubicin, and cisplatin). Pathological analysis of the resected specimen is evaluated using the Huvos grading system. What percentage of tumor necrosis is required to be classified as a 'good response' (Grade III or IV), which correlates with a significantly better prognosis?
Options:
- Greater than 50%
- Greater than 75%
- Greater than 90%
- Greater than 95%
- 100% necrosis only
Correct Answer: Greater than 90%
Explanation:
The histologic response to neoadjuvant chemotherapy is one of the most important prognostic factors for patients with osteosarcoma. The Huvos grading system categorizes response based on the percentage of tumor necrosis. A 'good response', defined as Huvos Grade III (>90% but <100% necrosis) or Grade IV (100% necrosis), is strongly correlated with improved long-term disease-free and overall survival. Anything less than 90% necrosis is considered a poor response.
Question 40:
A 6-week-old female infant is undergoing treatment for Developmental Dysplasia of the Hip (DDH) with a Pavlik harness. During a routine follow-up, her mother notes that the baby has stopped kicking her right leg. On examination, there is an absence of active knee extension on the right side, but ankle and toe movements are intact. What is the most appropriate management step to address this complication?
Options:
- Adjust the posterior straps to decrease hip abduction
- Adjust the anterior straps to decrease hip flexion
- Immediately abandon the Pavlik harness and transition to a hip spica cast
- Obtain an urgent MRI of the lumbar spine
- Reassure the mother and continue the current harness settings
Correct Answer: Adjust the anterior straps to decrease hip flexion
Explanation:
The infant is presenting with a femoral nerve palsy, a known complication of Pavlik harness treatment. It is caused by excessive flexion of the hip, which compresses the femoral nerve against the inguinal ligament or pelvic brim. The immediate management is to adjust the anterior straps to slightly decrease the amount of hip flexion. The condition is usually transient and resolves once the hyperflexion is corrected. Adjusting the posterior straps addresses abduction (excessive abduction risks AVN, not femoral nerve palsy).
Question 41:
A 68-year-old female presents with atraumatic thigh pain. She has been taking oral alendronate for 8 years. Radiographs reveal cortical thickening of the lateral cortex of the subtrochanteric femur and a transverse fracture. Which of the following best describes the pathomechanism of this injury?
Options:
- Overactivity of osteoblasts
- Accumulation of microdamage due to suppressed targeted remodeling
- Inadequate mineralization of osteoid
- Increased osteoclastic resorption leading to weakened woven bone
- Mutation in COL1A1 gene
Correct Answer: Accumulation of microdamage due to suppressed targeted remodeling
Explanation:
Bisphosphonates are potent inhibitors of osteoclast-mediated bone resorption. Long-term use severely suppresses bone turnover, preventing the targeted remodeling of normal microdamage. This accumulation of microdamage leads to atypical femoral fractures, classically presenting with lateral cortical thickening and a transverse or short oblique fracture pattern.
Question 42:
During an anterior cruciate ligament (ACL) reconstruction, the surgeon chooses to drill the femoral tunnel independently using an anteromedial (AM) portal rather than a transtibial technique. Which of the following is an advantage of the AM portal technique?
Options:
- It decreases the risk of posterior wall blowout
- It allows for more anatomic placement of the femoral tunnel in the native footprint
- It prevents divergence of the interference screw
- It requires less knee hyperflexion during drilling
- It creates a more vertical femoral tunnel
Correct Answer: It allows for more anatomic placement of the femoral tunnel in the native footprint
Explanation:
Independent drilling of the femoral tunnel through an anteromedial portal allows the surgeon to place the tunnel more anatomically within the native ACL footprint, independent of the tibial tunnel trajectory. Transtibial drilling often results in a more vertical, non-anatomic femoral tunnel. Disadvantages of the AM portal technique include the need for knee hyperflexion during drilling and a potentially shorter femoral tunnel.
Question 43:
A 45-year-old male laborer presents with chronic right wrist pain. Radiographs reveal a scapholunate advance collapse (SLAC) pattern. Which joint is classically spared in the progression of SLAC wrist arthritis?
Options:
- Radioscaphoid joint
- Radiolunate joint
- Capitolunate joint
- Scapho-trapezio-trapezoidal (STT) joint
- Scaphocapitate joint
Correct Answer: Radiolunate joint
Explanation:
In the typical progression of a SLAC wrist, the radiolunate joint is characteristically spared due to the congruent, spherical nature of the articulation, which distributes contact stresses evenly despite carpal collapse. The progression of arthritis in SLAC wrist follows a predictable pattern: Stage I involves the radial styloid-scaphoid articulation; Stage II involves the entire radioscaphoid fossa; Stage III involves the capitolunate joint.
Question 44:
An 82-year-old male sustains a fall from standing and presents with neck pain. Computed tomography reveals a Type II odontoid fracture with 2 mm of posterior displacement. He is neurologically intact. What is the most appropriate management, considering his age and fracture pattern?
Options:
- Halo vest immobilization
- Anterior odontoid screw fixation
- Posterior C1-C2 fusion
- Rigid cervical collar
- Soft cervical collar
Correct Answer: Rigid cervical collar
Explanation:
Management of Type II odontoid fractures in the elderly is controversial. However, recent evidence suggests that rigid cervical collar immobilization is the preferred initial treatment for stable or minimally displaced Type II odontoid fractures in patients over 80 years old, as it provides a lower complication rate and lower 1-year mortality compared to surgical intervention or halo vest immobilization. Halo immobilization in the elderly is associated with high morbidity and mortality (up to 40%).
Question 45:
A 13-year-old obese male presents to the emergency department unable to bear weight on his left leg after a minor twisting injury. Radiographs show a slipped capital femoral epiphysis (SCFE). According to the Loder classification, what is the most significant risk associated with this patient's injury type?
Options:
- Chondrolysis
- Avascular necrosis (AVN) of the femoral head
- Coxa magna
- Femoroacetabular impingement (FAI)
- Premature physeal closure
Correct Answer: Avascular necrosis (AVN) of the femoral head
Explanation:
The Loder classification divides SCFE into stable (patient can bear weight with or without crutches) and unstable (patient is unable to bear weight even with crutches). Unstable SCFE has a high rate of avascular necrosis (AVN), ranging from 20% to 50%, whereas stable SCFE has an AVN rate of nearly zero.
Question 46:
A 16-year-old male undergoes wide surgical resection for a conventional high-grade osteosarcoma of the distal femur after completing 10 weeks of neoadjuvant multi-agent chemotherapy. Histologic analysis of the resected specimen is performed. Which of the following findings is the most significant independent predictor of long-term survival?
Options:
- Surgical margins > 5 cm
- Presence of a skip metastasis
- > 90% tumor necrosis in the resection specimen
- Predominance of chondroblastic subtype
- High levels of alkaline phosphatase post-resection
Correct Answer: > 90% tumor necrosis in the resection specimen
Explanation:
In high-grade non-metastatic osteosarcoma, the histologic response to neoadjuvant chemotherapy (percentage of tumor necrosis) is the single most important prognostic factor. A 'good responder' is typically defined as having ≥90% tumor necrosis in the resected specimen, which correlates with significantly improved disease-free and overall survival.
Question 47:
A 65-year-old male presents with groin pain and swelling 5 years after an uncomplicated total hip arthroplasty utilizing a dual-taper modular titanium stem and a large diameter cobalt-chromium femoral head. Aspiration yields cloudy fluid with negative cultures. Blood work shows elevated serum cobalt levels with normal chromium levels. What is the primary mechanism of failure?
Options:
- Adhesive wear at the bearing surface
- Mechanically assisted crevice corrosion at the head-neck junction
- Galvanic corrosion at the stem-cement interface
- Fatigue fracture of the modular neck
- Aseptic loosening secondary to polyethylene wear debris
Correct Answer: Mechanically assisted crevice corrosion at the head-neck junction
Explanation:
The clinical scenario describes trunnionosis, which is mechanically assisted crevice corrosion (MACC) at the modular head-neck junction (trunnion). It is increasingly recognized in THA when large diameter cobalt-chromium heads are paired with titanium alloy stems. The friction and micromotion at the taper junction disrupt the passive oxide layer (fretting), exposing the underlying metal to the fluid environment, leading to crevice corrosion. This classically presents with elevated serum cobalt levels disproportionate to chromium.
Question 48:
A 55-year-old male with long-standing poorly controlled type 2 diabetes presents with a red, hot, swollen, and painless left foot. He has a small, superficial, uninfected ulcer on the plantar surface. Radiographs show soft tissue swelling but no bony destruction. MRI demonstrates bone marrow edema in the midfoot without discrete fluid collections. What is the most appropriate initial management?
Options:
- Intravenous antibiotics and observation
- Incision and drainage
- Total contact casting and non-weight bearing
- Below-knee amputation
- Arthrodesis of the midfoot joints
Correct Answer: Total contact casting and non-weight bearing
Explanation:
The patient is presenting with acute Stage 0 (Eichenholtz) Charcot arthropathy. In the acute phase (characterized by erythema, edema, and warmth), the goal is to prevent structural deformity. The gold standard for initial management of an acute Charcot foot is strict offloading and immobilization, most effectively achieved with a total contact cast (TCC). Antibiotics are not indicated unless there is a confirmed superimposed infection.
Question 49:
A 40-year-old male presents with an acutely swollen and painful knee. Arthrocentesis yields cloudy yellow fluid. Fluid analysis reveals a white blood cell count of 65,000 cells/µL with 85% polymorphonuclear leukocytes (PMNs). Gram stain is negative. Which of the following is the most likely diagnosis?
Options:
- Osteoarthritis
- Traumatic hemarthrosis
- Septic arthritis
- Lyme arthritis
- Gout
Correct Answer: Septic arthritis
Explanation:
Synovial fluid analysis is critical for distinguishing joint pathologies. Fluid with >50,000 WBC/µL and >75% PMNs is highly suspicious for septic arthritis. Although crystalline arthropathies (gout, pseudogout) and severe inflammatory arthropathies can occasionally produce counts this high, septic arthritis must be the presumed diagnosis until proven otherwise. Note: Lyme arthritis can also present with very high WBC counts (averaging 60,000 cells/µL), but septic arthritis remains the most urgent and likely diagnosis in an acutely swollen, hot joint without a specific tick exposure history.
Question 50:
Which of the following combinations of injuries strictly defines a "floating shoulder"?
Options:
- Fracture of the anatomical neck of the humerus and clavicle shaft fracture
- Displaced fracture of the scapular neck and an ipsilateral clavicle shaft fracture
- Acromioclavicular joint dislocation and coracoid process fracture
- Glenohumeral dislocation and a displaced fracture of the acromion
- Scapular body fracture and a sternoclavicular joint dislocation
Correct Answer: Displaced fracture of the scapular neck and an ipsilateral clavicle shaft fracture
Explanation:
A "floating shoulder" refers to a double disruption of the superior shoulder suspensory complex (SSSC). Classically, it is defined as an ipsilateral fracture of the clavicle shaft and the surgical neck of the scapula. This injury can lead to instability of the shoulder girdle, and surgical fixation of one or both fractures may be indicated depending on the degree of displacement (e.g., >2 cm medial translation, altered glenoid polar angle).
Question 51:
During an ulnar collateral ligament (UCL) reconstruction in a professional baseball pitcher, the surgeon aims to reconstruct the primary restraint to valgus stress at the elbow. Which specific band or bundle is the most critical to reconstruct?
Options:
- Posterior bundle
- Transverse ligament
- Anterior band of the anterior bundle
- Posterior band of the anterior bundle
- Radial collateral ligament
Correct Answer: Anterior band of the anterior bundle
Explanation:
The ulnar collateral ligament (UCL) complex consists of the anterior bundle, posterior bundle, and transverse ligament. The anterior bundle is the primary restraint to valgus stress at the elbow from 30 to 120 degrees of flexion. The anterior bundle is further divided into an anterior band (tight in extension to 60 degrees of flexion) and a posterior band (tight in flexion >60 degrees). The anterior band is the most isometric and critical component reconstructed during surgery.
Question 52:
A 70-year-old female presents with bilateral leg pain and cramping that worsens with walking and is relieved by sitting or leaning forward over a shopping cart. Magnetic resonance imaging (MRI) reveals severe central canal stenosis at L4-L5. Hypertrophy of which of the following structures is a primary contributor to her central stenosis?
Options:
- Posterior longitudinal ligament
- Anterior longitudinal ligament
- Ligamentum flavum
- Interspinous ligament
- Iliolumbar ligament
Correct Answer: Ligamentum flavum
Explanation:
The patient has neurogenic claudication secondary to lumbar spinal stenosis. The classic shopping cart sign indicates relief with lumbar flexion, which increases the cross-sectional area of the spinal canal. The primary degenerative contributors to central canal stenosis are intervertebral disc bulging/herniation, facet joint hypertrophy, and hypertrophy/buckling of the ligamentum flavum.
Question 53:
In total hip arthroplasty, highly cross-linked ultra-high molecular weight polyethylene (UHMWPE) is commonly used to reduce wear. Which of the following mechanical properties is significantly decreased as a direct result of the irradiation used to create highly cross-linked polyethylene?
Options:
- Abrasive wear resistance
- Oxidation resistance
- Fatigue strength
- Elastic modulus
- Hardness
Correct Answer: Fatigue strength
Explanation:
Irradiation is used to cross-link UHMWPE chains, which significantly improves its adhesive and abrasive wear resistance. However, cross-linking decreases certain mechanical properties, particularly fatigue strength, yield strength, ultimate tensile strength, and ductility. To prevent oxidation from free radicals generated during irradiation, the material is typically remelted, annealed, or blended with an antioxidant like vitamin E.
Question 54:
In evaluating a patient with suspected carpal tunnel syndrome, which of the following clinical tests is considered the most sensitive for detecting early sensory nerve dysfunction?
Options:
- Tinel's sign
- Phalen's maneuver
- Semmes-Weinstein monofilament testing
- Two-point discrimination test
- Durkan's carpal compression test
Correct Answer: Semmes-Weinstein monofilament testing
Explanation:
Semmes-Weinstein monofilament testing is considered the most sensitive objective clinical test for detecting early sensory nerve dysfunction in carpal tunnel syndrome. It tests threshold sensibility, which is lost earlier than innervation density (tested by two-point discrimination). Durkan's test is the most sensitive provocative maneuver, but for measuring nerve function directly, monofilament testing is superior.
Question 55:
A 6-year-old child sustains a displaced extension-type supracondylar humerus fracture. On presentation, the radial pulse is absent, but the hand is warm and well-perfused (pink). Closed reduction and percutaneous pinning are performed. Post-operatively, the hand remains warm and pink, but the radial pulse is still absent on palpation and Doppler. What is the most appropriate next step in management?
Options:
- Immediate exploration of the brachial artery
- CT angiography of the upper extremity
- Arteriography in the operating room
- Close clinical observation
- Administration of intravenous heparin
Correct Answer: Close clinical observation
Explanation:
The management of a 'pulseless, pink' hand after reduction and pinning of a supracondylar humerus fracture is close clinical observation. As long as the hand remains well-perfused (warm, pink, capillary refill < 2 seconds), there is adequate collateral circulation, and surgical exploration is not indicated. Most pulses will return within days to weeks. If the hand were pulseless and pale (ischemic), urgent exploration of the brachial artery would be required.
Question 56:
A 28-year-old male sustains a Hawkins Type II talar neck fracture. Radiographs taken 8 weeks post-operatively demonstrate a subchondral radiolucent band in the dome of the talus on the AP view (Hawkins sign). What does this finding indicate regarding the talus?
Options:
- Impending avascular necrosis
- Nonunion of the fracture
- Intact vascularity to the talar body
- Post-traumatic arthritis
- Osteochondral defect
Correct Answer: Intact vascularity to the talar body
Explanation:
The Hawkins sign is a subchondral radiolucent band seen in the talar dome on an AP radiograph 6 to 8 weeks after a talar neck fracture. It represents subchondral disuse osteopenia. The process of bone resorption requires an active blood supply; therefore, the presence of a Hawkins sign is a highly reliable indicator that the vascularity to the talar body is intact and avascular necrosis (AVN) is unlikely.
Question 57:
A 12-year-old female presents with pain and swelling in her mid-thigh. Radiographs reveal a permeative, destructive diaphyseal lesion with an "onion-skin" periosteal reaction. Biopsy demonstrates small, round, blue cells. Which of the following cytogenetic abnormalities is most characteristically associated with this tumor?
Options:
- t(11;22)
- t(9;22)
- t(X;18)
- t(12;16)
- t(2;13)
Correct Answer: t(11;22)
Explanation:
The clinical and radiographic presentation describes Ewing sarcoma. The hallmark cytogenetic abnormality of Ewing sarcoma is a balanced translocation between chromosomes 11 and 22, t(11;22)(q24;q12), which results in the fusion of the EWS gene with the FLI1 gene. The tumor cells strongly express CD99 on immunohistochemistry.
Question 58:
According to Perren's strain theory of fracture healing, which type of tissue is expected to form within a fracture gap if the mechanical strain environment is maintained between 2% and 10%?
Options:
- Primary osteonal bone
- Granulation tissue
- Hyaline cartilage
- Lamellar bone
- Woven bone and cartilage (Callus)
Correct Answer: Woven bone and cartilage (Callus)
Explanation:
Perren's strain theory dictates the type of tissue that can survive and differentiate in a fracture gap based on deformation (strain).
- Strain < 2%: Allows for primary bone healing (lamellar bone formation) without a callus.
- Strain between 2% and 10%: Tolerated by cartilage and woven bone, leading to secondary bone healing via endochondral ossification (callus formation).
- Strain > 10%: Tissues tear, and only granulation tissue can survive, leading to nonunion if not stabilized.
Question 59:
A 35-year-old male sustains a femoral neck fracture in a motor vehicle accident. The fracture line is oriented 75 degrees relative to the horizontal (Pauwels Type III). What is the predominant biomechanical force acting on this fracture pattern, making it highly unstable?
Options:
- Compressive force
- Tensile force
- Torsional force
- Shear force
- Bending force
Correct Answer: Shear force
Explanation:
The Pauwels classification for femoral neck fractures in young adults is based on the angle of the fracture line relative to the horizontal.
- Type I: < 30 degrees (predominantly compressive forces, stable).
- Type II: 30-50 degrees.
- Type III: > 50 degrees (predominantly shear forces, highly unstable).
The high shear forces in vertical fracture patterns (Pauwels III) increase the risk of varus collapse and nonunion.
Question 60:
During knee arthroscopy for a suspected meniscal tear, the surgeon identifies a longitudinal tear 2 mm from the meniscocapsular junction. This tear is considered highly amenable to repair. Which of the following vascular structures provides the primary blood supply to this peripheral "red-red" zone of the meniscus?
Options:
- Middle geniculate artery
- Medial and lateral superior geniculate arteries
- Medial and lateral inferior geniculate arteries
- Popliteal artery branches directly
- Descending genicular artery
Correct Answer: Medial and lateral inferior geniculate arteries
Explanation:
The blood supply to the menisci originates primarily from the medial and lateral inferior geniculate arteries, and to a lesser extent, the superior geniculate arteries. These vessels form a perimeniscal capillary plexus within the synovial and capsular tissues. The peripheral 10% to 30% of the meniscus (the "red-red" zone) is well-vascularized and has excellent healing potential following repair. The central portions rely on diffusion from synovial fluid.