Full Question & Answer Text (for Search Engines)
Question 1:
What is the primary purpose of infusing highly cross-linked ultra-high molecular weight polyethylene (UHMWPE) with Vitamin E in total joint arthroplasty?
Options:
- Increase the ultimate yield strength of the polyethylene
- Quench free radicals without the need for post-irradiation melting
- Increase the elastic modulus to match that of cortical bone
- Reduce the incidence of metal allergy postoperatively
- Inhibit bacterial biofilm formation on the articular surface
Correct Answer: Quench free radicals without the need for post-irradiation melting
Explanation:
Highly cross-linked UHMWPE is treated with radiation to increase cross-linking, which dramatically reduces wear rates. However, radiation generates free radicals that can lead to oxidative degradation over time. Traditionally, the polyethylene was melted to eliminate these free radicals, but melting reduces the mechanical properties (such as fatigue strength) of the material. By infusing the polyethylene with Vitamin E (alpha-tocopherol), a potent antioxidant, free radicals are quenched without the need for melting, thereby preserving the material's mechanical strength while preventing oxidative degradation.
Question 2:
During a total hip arthroplasty via a posterior approach, the surgeon decides to use a high-offset femoral stem rather than a standard-offset stem. Assuming neck angle and leg length remain constant, what is the primary biomechanical effect of this change?
Options:
- Increased abductor tension and decreased joint reactive force
- Decreased abductor tension and increased joint reactive force
- Increased risk of sciatic nerve palsy due to soft tissue stretch
- Decreased femoral component anteversion
- Increased global offset leading to impingement
Correct Answer: Increased abductor tension and decreased joint reactive force
Explanation:
Increasing the femoral offset lateralizes the proximal femur. This increases the lever arm (moment arm) of the abductor musculature. Because the abductors have a mechanical advantage, they require less force to balance the pelvis during single-leg stance. A reduction in abductor muscle force proportionally decreases the overall joint reactive force across the hip.
Question 3:
A 45-year-old male presents after a motorcycle collision with a radiographically confirmed anteroposterior compression type II (APC II) pelvic ring injury. Which of the following ligamentous structures is typically intact in this specific injury pattern?
Options:
- Symphyseal ligaments
- Anterior sacroiliac ligaments
- Sacrospinous ligaments
- Sacrotuberous ligaments
- Posterior sacroiliac ligaments
Correct Answer: Posterior sacroiliac ligaments
Explanation:
In the Young-Burgess classification, an APC II pelvic ring injury involves diastasis of the pubic symphysis (rupture of symphyseal ligaments) and 'opening of the book' at the SI joint. This mechanism ruptures the anterior sacroiliac, sacrospinous, and sacrotuberous ligaments. However, the stout posterior sacroiliac ligaments remain intact, acting as a hinge. Complete disruption of the posterior SI ligaments would convert this to a completely unstable APC III injury.
Question 4:
A 12-year-old boy presents with a left-sided stable slipped capital femoral epiphysis (SCFE). Which of the following is the strongest indication for prophylactic in situ pinning of the contralateral asymptomatic right hip?
Options:
- Patient age greater than 14 years
- Presence of an underlying endocrine disorder
- Male gender
- Body mass index greater than 35
- Slipped angle greater than 50 degrees on the affected side
Correct Answer: Presence of an underlying endocrine disorder
Explanation:
The risk of developing a contralateral SCFE is significantly elevated in patients with underlying endocrinopathies (such as hypothyroidism, panhypopituitarism, or renal osteodystrophy). In idiopathic cases, contralateral slip occurs in about 20-40% of patients. However, in patients with endocrine or metabolic disorders, the risk of a bilateral slip approaches 100%. Therefore, an underlying endocrine disorder is an absolute indication for prophylactic pinning of the contralateral hip.
Question 5:
When comparing bone-patellar tendon-bone (BPTB) autograft to quadrupled hamstring autograft for anterior cruciate ligament (ACL) reconstruction, BPTB autograft is generally associated with a higher incidence of which of the following postoperative complications?
Options:
- Hardware prominence requiring removal
- Graft rupture within the first year
- Anterior knee pain and kneeling pain
- Deep vein thrombosis
- Loss of deep flexion strength
Correct Answer: Anterior knee pain and kneeling pain
Explanation:
Both BPTB and hamstring autografts are excellent choices for ACL reconstruction with comparable long-term knee stability and graft survival rates. However, harvest site morbidity differs. BPTB autograft is notoriously associated with a higher incidence of anterior knee pain and discomfort while kneeling, largely due to the harvest of the central third of the patellar tendon and the creation of bone defects in the patella and tibial tubercle. Hamstring harvest may result in temporary or mild permanent loss of deep flexion strength, but anterior knee pain is specifically a hallmark risk of BPTB.
Question 6:
A 24-year-old male sustains a proximal pole scaphoid fracture. The high risk of avascular necrosis in this region is primarily due to the retrograde blood supply originating from branches of which artery?
Options:
- Radial artery
- Ulnar artery
- Anterior interosseous artery
- Posterior interosseous artery
- Deep palmar arch
Correct Answer: Radial artery
Explanation:
The scaphoid is predominantly supplied by the radial artery. The major vascular supply enters the scaphoid distally (at the dorsal ridge) and flows in a retrograde fashion toward the proximal pole. Because of this tenuous retrograde blood supply, fractures at the waist or proximal pole of the scaphoid disrupt the vascular flow, leaving the proximal fragment at a very high risk of nonunion and avascular necrosis.
Question 7:
A 15-year-old boy presents with a painful mass around his distal femur. Biopsy reveals a high-grade pleomorphic spindle cell neoplasm producing malignant osteoid. Mutations in which of the following tumor suppressor genes are most strongly implicated in the pathogenesis of this disease, particularly in familial syndromes like Li-Fraumeni?
Options:
Correct Answer: TP53
Explanation:
The patient has osteosarcoma, the most common primary malignant bone tumor in youths, characterized by the production of malignant osteoid. The tumor suppressor genes most commonly implicated in the pathogenesis of osteosarcoma are TP53 and RB1. Li-Fraumeni syndrome is caused by a germline mutation in the TP53 gene and is associated with a markedly increased risk of developing osteosarcoma, breast cancer, brain tumors, and leukemias.
Question 8:
A 30-year-old football player sustains a foot injury characterized by plantar ecchymosis and pain with pronation/abduction of the forefoot. A subtle widening is noted between the medial and middle cuneiforms. The primary stabilizing ligament injured in this scenario originates from the:
Options:
- Plantar aspect of the medial cuneiform and inserts on the base of the second metatarsal.
- Plantar aspect of the middle cuneiform and inserts on the base of the first metatarsal.
- Dorsal aspect of the medial cuneiform and inserts on the base of the second metatarsal.
- Cuboid and inserts on the base of the fourth metatarsal.
- Navicular and inserts on the base of the first metatarsal.
Correct Answer: Plantar aspect of the medial cuneiform and inserts on the base of the second metatarsal.
Explanation:
The clinical picture (plantar ecchymosis) is pathognomonic for a Lisfranc injury. The Lisfranc ligament is the critical stabilizing structure of the midfoot. It is a stout interosseous ligament that runs obliquely from the lateral plantar aspect of the medial cuneiform to the medial plantar aspect of the base of the second metatarsal. There is no direct ligamentous connection between the first and second metatarsal bases, making the Lisfranc ligament essential for stability.
Question 9:
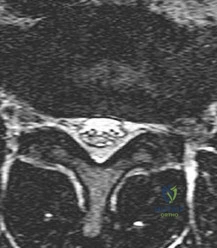
A 65-year-old male presents with worsening hand clumsiness and gait instability. Physical examination reveals a positive Hoffmann sign bilaterally and hyperreflexia in the lower extremities. Which of the following is the most sensitive imaging modality to evaluate the exact extent of the likely underlying pathology?
Options:
- Upright dynamic radiographs of the cervical spine
- Non-contrast computed tomography (CT) of the cervical spine
- Magnetic resonance imaging (MRI) of the cervical spine
- Electromyography (EMG) and nerve conduction studies (NCS)
- Somatosensory evoked potentials (SSEP)
Correct Answer: Magnetic resonance imaging (MRI) of the cervical spine
Explanation:
The patient's symptoms (hand clumsiness, gait instability) and signs (Hoffmann sign, hyperreflexia) are classic for cervical spondylotic myelopathy (CSM), an upper motor neuron lesion caused by spinal cord compression. MRI of the cervical spine is the gold standard and most sensitive imaging modality to evaluate soft tissue structures, the intervertebral discs, and the degree of spinal cord compression or intrinsic cord signal changes (myelomalacia).
Question 10:
Absolute stability constructs (e.g., lag screws and compression plates) in fracture fixation bypass the formation of a soft callus. Which of the following cell types plays the leading role in the 'cutting cone' phase of this specific type of bone healing?
Options:
- Chondrocytes
- Osteoclasts
- Fibroblasts
- Mesenchymal stem cells
- Macrophages
Correct Answer: Osteoclasts
Explanation:
Absolute stability promotes primary (direct) bone healing, which occurs without the formation of a cartilaginous soft callus intermediate. This process relies on Haversian remodeling across the fracture site. The leading edge of this remodeling process is the 'cutting cone,' which is spearheaded by osteoclasts that bore through the dead cortical bone. They are followed closely by trailing osteoblasts that lay down new lamellar bone to bridge the gap.
Question 11:
A 28-year-old male sustains a closed comminuted tibial shaft fracture. Twelve hours post-injury, he complains of excruciating pain out of proportion to the injury, not relieved by intravenous opioids. His foot is warm with palpable dorsalis pedis and posterior tibial pulses. Which of the following physical exam findings is the most sensitive early clinical indicator of acute compartment syndrome?
Options:
- Loss of palpable pedal pulses
- Pallor of the distal extremity
- Pain with passive stretch of the toes
- Motor paralysis of the extensor hallucis longus
- Capillary refill time greater than 3 seconds
Correct Answer: Pain with passive stretch of the toes
Explanation:
Acute compartment syndrome is a surgical emergency characterized by tissue pressure exceeding capillary perfusion pressure. The classic '6 Ps' are pain, pallor, paresthesia, pulselessness, paralysis, and poikilothermia. However, pain out of proportion to the injury and pain with passive stretch of the muscles within the affected compartment are the earliest and most sensitive clinical signs. Pulselessness and paralysis are very late findings and indicate irreversible ischemic damage; pulses often remain intact until very late because arterial pressure is much higher than compartment pressure.
Question 12:
When treating a rigid idiopathic clubfoot using the Ponseti method of serial casting, which component of the deformity must be corrected first?
Options:
- Equinus of the ankle
- Varus of the hindfoot
- Adductus of the forefoot
- Cavus of the midfoot
- Tibial torsion
Correct Answer: Cavus of the midfoot
Explanation:
The Ponseti method follows a strict sequence of correction summarized by the mnemonic CAVE: Cavus, Adductus, Varus, and Equinus. The very first step involves elevating the first ray to correct the cavus deformity of the midfoot, bringing the forefoot into alignment with the hindfoot. Once cavus is corrected, the foot is sequentially abducted to correct adductus and varus, while counter-pressure is held over the lateral aspect of the head of the talus. Finally, equinus is addressed, often requiring a percutaneous Achilles tenotomy.
Question 13:
A 35-year-old carpenter suffers a laceration to the volar aspect of his index finger at the level of the proximal phalanx. He is unable to flex the distal interphalangeal joint. This injury is located in a flexor tendon zone historically referred to as 'no man's land' due to poor outcomes. Which zone is this?
Options:
- Zone I
- Zone II
- Zone III
- Zone IV
- Zone V
Correct Answer: Zone II
Explanation:
Flexor tendon Zone II extends from the distal palmar crease (A1 pulley) to the insertion of the flexor digitorum superficialis (FDS) tendon on the middle phalanx. In this zone, both the FDS and flexor digitorum profundus (FDP) tendons run tightly together within the fibro-osseous digital sheath. Historically, it was called 'no man's land' by Bunnell because primary repairs in this area often failed due to adhesions between the tendons and the sheath. Advances in surgical technique and early active rehabilitation have significantly improved outcomes.
Question 14:
A 72-year-old female presents with a painful total knee arthroplasty 3 years post-operatively. Synovial fluid analysis is performed to rule out periprosthetic joint infection (PJI). Which of the following biomarkers, released by neutrophils in response to pathogens, is highly specific for PJI and can be tested via a synovial fluid immunoassay?
Options:
- C-reactive protein (CRP)
- Interleukin-6 (IL-6)
- Alpha-defensin
- Procalcitonin
- Erythrocyte sedimentation rate (ESR)
Correct Answer: Alpha-defensin
Explanation:
Alpha-defensin is an antimicrobial peptide released by neutrophils in response to pathogens. It has been shown to be highly sensitive and specific for diagnosing periprosthetic joint infection (PJI) when measured in synovial fluid. While serum CRP and ESR are excellent screening tools, and synovial fluid white blood cell counts are standard, alpha-defensin testing provides an excellent diagnostic adjunct, particularly when standard tests are equivocal.
Question 15:
A 22-year-old collegiate baseball pitcher presents with vague, deep shoulder pain and clicking during the late cocking phase of throwing. Magnetic resonance arthrography demonstrates a superior labral tear from anterior to posterior (SLAP tear) with detachment of the biceps anchor from the superior glenoid tubercle. This represents which type of SLAP tear?
Options:
- Type I
- Type II
- Type III
- Type IV
- Type V
Correct Answer: Type II
Explanation:
According to the Snyder classification of SLAP tears: Type I involves fraying of the superior labrum but the biceps anchor is intact. Type II (the most common type, especially in throwers) involves detachment of the superior labrum and the origin of the long head of the biceps tendon from the glenoid. Type III is a bucket-handle tear of the superior labrum with an intact biceps anchor. Type IV is a bucket-handle tear that extends into the biceps tendon. Therefore, a detached biceps anchor signifies a Type II SLAP lesion.
Question 16:
A 55-year-old female falls on an outstretched hand and sustains a distal radius fracture. Radiographs show a fracture of the volar rim of the distal radius with volar subluxation of the carpus alongside the fracture fragment. This fracture pattern is best classified as:
Options:
- Colles fracture
- Smith fracture
- Volar Barton fracture
- Chauffeur's fracture
- Die-punch fracture
Correct Answer: Volar Barton fracture
Explanation:
A volar Barton fracture is an intra-articular fracture of the distal radius involving the volar rim, accompanied by volar subluxation or dislocation of the carpus. It represents a radiocarpal fracture-dislocation. A Colles fracture is an extra-articular fracture with dorsal angulation/displacement, while a Smith fracture is an extra-articular fracture with volar angulation. A Chauffeur's fracture involves the radial styloid, and a die-punch fracture is an intra-articular fracture of the lunate fossa.
Question 17:
A 32-year-old female presents with progressive knee pain. Radiographs reveal an eccentric, lytic, epiphyseal-metaphyseal lesion in the proximal tibia with a 'soap bubble' appearance extending to the subchondral bone. Biopsy shows multinucleated giant cells in a background of mononuclear stromal cells. Which of the following targeted medical therapies is most appropriate for a surgically unresectable lesion of this type?
Options:
- Imatinib
- Denosumab
- Methotrexate
- Bisphosphonates
- Rituximab
Correct Answer: Denosumab
Explanation:
The clinical and radiographic presentation is classic for a Giant Cell Tumor (GCT) of bone. The neoplastic cells in GCT are the mononuclear stromal cells, which express RANK-L (Receptor Activator of Nuclear factor Kappa-B Ligand). This expression recruits and activates the reactive multinucleated giant cells, which are essentially osteoclasts, leading to massive bone lysis. Denosumab is a monoclonal antibody that targets and inhibits RANK-L, thereby cutting off the signal to osteoclasts. It is the medical treatment of choice for unresectable, recurrent, or metastatic giant cell tumors.
Question 18:
A 40-year-old construction worker falls from a scaffolding, sustaining an L1 burst fracture. He is neurologically intact. According to the Thoracolumbar Injury Classification and Severity (TLICS) score, which of the following findings would unequivocally push his score to 5 or higher, thereby strongly favoring operative intervention?
Options:
- 20% loss of anterior vertebral body height
- 30% canal compromise by retropulsed bone fragments
- Disruption of the posterior ligamentous complex (PLC)
- Interpedicular widening on the AP radiograph
- Concomitant transverse process fractures
Correct Answer: Disruption of the posterior ligamentous complex (PLC)
Explanation:
The TLICS scoring system aids in deciding whether a thoracolumbar fracture requires surgery. It is based on three categories: injury morphology, neurological status, and integrity of the posterior ligamentous complex (PLC). A burst fracture (morphology) gives 2 points. Intact neuro status gives 0 points. A confirmed disruption of the PLC adds 3 points. Thus, 2 + 0 + 3 = 5 points. A score of 4 can be treated conservatively or operatively (surgeon's choice), while a score greater than 4 strongly dictates operative intervention. Neither loss of height alone nor the degree of canal compromise automatically mandates surgery without neuro deficits or PLC injury.
Question 19:
The remarkable ability of articular cartilage to resist compressive loads is primarily attributed to the osmotic swelling pressure created by which of the following molecular components?
Options:
- Type II collagen fibrils
- Aggrecan molecules containing chondroitin and keratan sulfate
- Hyaluronic acid backbone without attached side chains
- Lubricin (PRG4) in the superficial zone
- Type X collagen in the calcified zone
Correct Answer: Aggrecan molecules containing chondroitin and keratan sulfate
Explanation:
Articular cartilage consists predominantly of a hydrated extracellular matrix. The structural integrity and compressive resistance rely on the interaction between Type II collagen and proteoglycans. Aggrecan is the most abundant proteoglycan in cartilage. The highly negatively charged glycosaminoglycan (GAG) side chains (chondroitin sulfate and keratan sulfate) attached to aggrecan repel each other and draw water into the tissue via Donnan osmotic pressure. This swelling pressure is constrained by the tensile strength of the Type II collagen network, providing cartilage with its unique ability to resist tremendous compressive loads.
Question 20:
A 45-year-old weekend warrior sustains an acute Achilles tendon rupture while playing tennis. He opts for non-operative management with a functional rehabilitation protocol. Compared to acute operative repair, current literature suggests this management approach is associated with:
Options:
- A significantly higher risk of sural nerve injury
- A higher rate of deep surgical site infections
- An equivalent re-rupture rate when early functional rehabilitation is employed
- A faster return to high-impact sports
- Greater ultimate plantar flexion strength
Correct Answer: An equivalent re-rupture rate when early functional rehabilitation is employed
Explanation:
Historically, non-operative treatment of Achilles tendon ruptures was associated with higher re-rupture rates compared to surgery. However, modern high-quality randomized controlled trials (such as the Willits study) have demonstrated that when non-operative treatment is combined with an early dynamic functional rehabilitation protocol (weight-bearing in an orthosis), the re-rupture rates are equivalent to those of operative repair. Non-operative management eliminates surgical risks like infection, wound breakdown, and iatrogenic sural nerve injury, though some patients may have slightly reduced peak plantar flexion strength compared to the surgical cohort.
Question 21:
A 30-year-old female presents with a slow-growing, painful soft tissue mass in the posterior aspect of her knee. An MRI demonstrates a well-circumscribed mass adjacent to the joint capsule. Biopsy reveals a biphasic pattern consisting of both epithelial-like and spindle cells. Which of the following cytogenetic abnormalities is most characteristic of this lesion?
Options:
- t(11;22)(q24;q12)
- t(X;18)(p11;q11)
- t(12;16)(q13;p11)
- t(2;13)(q35;q14)
- t(9;22)(q22;q12)
Correct Answer: t(X;18)(p11;q11)
Explanation:
The clinical and histological presentation describes a synovial sarcoma, which characteristically features a biphasic microscopic pattern (epithelial and spindle cells). The hallmark cytogenetic translocation for synovial sarcoma is t(X;18)(p11;q11), leading to the SYT-SSX fusion gene. t(11;22) is seen in Ewing sarcoma; t(12;16) in myxoid liposarcoma; t(2;13) in alveolar rhabdomyosarcoma; and t(9;22) in extraskeletal myxoid chondrosarcoma.
Question 22:
A 65-year-old male sustains a proximal humerus fracture after a fall. According to the Hertel criteria, which of the following radiographic features is the most reliable predictor of humeral head ischemia?
Options:
- Metaphyseal head extension > 5 mm
- Calcar length < 8 mm
- Intact medial hinge
- Varus angulation > 20 degrees
- Greater tuberosity displacement > 1 cm
Correct Answer: Calcar length < 8 mm
Explanation:
Hertel et al. described radiographic predictors of humeral head ischemia. The best predictors are a short calcar segment attached to the articular surface (calcar length < 8 mm), disrupted medial hinge, and a basicervical fracture line. A metaphyseal extension > 8 mm (not 5 mm) attached to the head actually predicts a BETTER blood supply (lower risk of ischemia), whereas a shorter segment (< 8 mm) indicates higher risk of ischemia.
Question 23:
In the evaluation of a traumatic spine injury using the Thoracolumbar Injury Classification and Severity (TLICS) score, which of the following mechanisms of injury is assigned the highest number of points?
Options:
- Compression
- Burst
- Translation/Rotation
- Distraction
- Lateral compression
Correct Answer: Distraction
Explanation:
The TLICS score assigns points based on morphology/mechanism: Compression (1 point), Burst (2 points), Translation/Rotation (3 points), and Distraction (4 points). Therefore, a distraction mechanism yields the highest point value in this category, reflecting the severe instability typical of these injuries (e.g., flexion-distraction/Chance fractures).
Question 24:
A 12-year-old obese boy presents with acute on chronic Slipped Capital Femoral Epiphysis (SCFE) of the left hip. In considering treatment options for the asymptomatic contralateral right hip, which of the following is considered the strongest indication for prophylactic in situ pinning?
Options:
- Age > 14 years
- Female gender
- Presence of an underlying endocrine disorder
- Severe initial slip > 50 degrees on the affected side
- Body Mass Index in the 90th percentile
Correct Answer: Presence of an underlying endocrine disorder
Explanation:
Prophylactic pinning of the contralateral asymptomatic hip in SCFE is highly recommended in patients with an underlying endocrine disorder (e.g., hypothyroidism, growth hormone deficiency, renal osteodystrophy) due to an exceedingly high rate of bilateral involvement (up to 100% in some series). Other relative indications include age < 10 years and inability to ensure reliable follow-up.
Question 25:
A 35-year-old recreational boxer presents with pain over the third metacarpophalangeal (MCP) joint. On physical examination, when he makes a fist, the extensor digitorum communis (EDC) tendon visibly subluxates into the ulnar gutter. Which stabilizing structure is most likely disrupted?
Options:
- Radial sagittal band
- Ulnar sagittal band
- Radial collateral ligament
- Central slip
- Terminal extensor tendon
Correct Answer: Radial sagittal band
Explanation:
This is a classic presentation of "Boxer's knuckle," which involves a rupture of the sagittal band at the MCP joint. The EDC tendon subluxates in the direction opposite to the tear. Because the tendon subluxates ulnarly, the radial sagittal band is torn. The middle finger is most commonly affected.
Question 26:
During arthroscopic posterior cruciate ligament (PCL) reconstruction, a surgeon is preparing the tibial tunnel. To prevent iatrogenic injury to the popliteal artery, it is critical to understand its anatomical relationship to the PCL. Where is the popliteal artery located in relation to the PCL tibial footprint?
Options:
- Directly anterior to the PCL tibial attachment
- Medial to the medial meniscus posterior horn
- Lateral to the fibular head
- Directly posterior to the PCL tibial attachment
- Anterolateral to the lateral collateral ligament
Correct Answer: Directly posterior to the PCL tibial attachment
Explanation:
The popliteal artery is at significant risk during tibial tunnel drilling for PCL reconstruction. It is located directly posterior to the PCL tibial attachment (the "facies poplitea"), separated only by the posterior capsule. Studies have shown the distance from the posterior capsule to the artery can be as little as 5 to 10 mm.
Question 27:
According to Perren's Strain Theory of bone healing, different tissues tolerate different amounts of interfragmentary strain before mechanical failure. Which of the following tissues can tolerate the highest percentage of strain?
Options:
- Lamellar bone
- Woven bone
- Fibrocartilage
- Granulation tissue
- Hyaline cartilage
Correct Answer: Granulation tissue
Explanation:
Perren's strain theory dictates that a tissue cannot form if the local strain exceeds its tolerance. Granulation tissue tolerates the highest strain (up to 100%). Fibrocartilage tolerates roughly 10-15%, woven bone 2%, and lamellar bone only 1-2%. Initially, a fracture gap with high strain is filled with granulation tissue, which subsequently decreases the strain, allowing sequential formation of cartilage and ultimately bone.
Question 28:
A surgeon is performing a total knee arthroplasty on a severe valgus knee. While balancing the knee in extension, the lateral compartment remains significantly tight. According to classic lateral release sequences (e.g., Krackow or Ranawat), which structure is typically released first for a tight extension gap?
Options:
- Popliteus tendon
- Lateral collateral ligament (LCL)
- Iliotibial (IT) band
- Posterolateral capsule
- Biceps femoris
Correct Answer: Iliotibial (IT) band
Explanation:
In balancing a valgus knee, the sequence of release depends on whether the knee is tight in extension, flexion, or both. For a tight extension gap, the Iliotibial (IT) band is typically released first (often via "pie-crusting" from the inside out). The popliteus tendon is primarily a flexion stabilizer and is released if the flexion gap is disproportionately tight. The LCL is released if both are tight after initial releases.
Question 29:
A 55-year-old male with long-standing, poorly controlled type 2 diabetes presents with a unilateral red, hot, and swollen foot. There are no open ulcers or signs of systemic toxicity. Radiographs show periarticular fragmentation and joint subluxation at the midfoot. What is the most appropriate initial management?
Options:
- Incision and drainage
- Excision of fragmented bone
- Primary midfoot arthrodesis
- Total contact casting
- Intravenous broad-spectrum antibiotics
Correct Answer: Total contact casting
Explanation:
The patient is presenting with acute Charcot arthropathy (Eichenholtz Stage I: Fragmentation). The hallmark clinical presentation mimics infection (red, hot, swollen), but without an open ulcer, an acute Charcot process is the primary diagnosis. The gold standard initial treatment for an acute Charcot foot is strict immobilization and offloading, optimally achieved with a total contact cast (TCC), until the inflammatory phase resolves (Stage II: Coalescence).
Question 30:
During an anterolateral approach to the distal tibia for open reduction and internal fixation of a pilon fracture, the superficial dissection puts a specific nerve at significant risk. Which nerve crosses the operative field from lateral to medial and must be carefully identified and protected?
Options:
- Deep peroneal nerve
- Superficial peroneal nerve
- Sural nerve
- Saphenous nerve
- Tibial nerve
Correct Answer: Superficial peroneal nerve
Explanation:
The superficial peroneal nerve provides sensation to the dorsum of the foot. In the distal third of the leg, it emerges from the lateral compartment, pierces the crural fascia, and courses anteriorly over the fibula and distal tibia, putting it at direct risk during the superficial dissection of the anterolateral approach to the pilon/distal tibia.
Question 31:
A 28-year-old carpenter amputates his index finger with a table saw. The digit is recovered at the scene but is inadvertently kept at room temperature instead of being cooled. What is the maximum generally accepted warm ischemia time beyond which replantation of a digit is contraindicated?
Options:
- 2 hours
- 6 hours
- 12 hours
- 24 hours
- 36 hours
Correct Answer: 12 hours
Explanation:
For digits (which contain very little muscle mass), the maximum accepted warm ischemia time is approximately 12 hours, and cold ischemia time can be up to 24 hours. This contrasts with proximal major limb replantations (containing significant skeletal muscle), where warm ischemia time > 6 hours is a strict contraindication due to irreversible muscle necrosis and the risk of potentially fatal reperfusion syndrome.
Question 32:
A 40-year-old male is involved in a motor vehicle accident and sustains a traumatic spondylolisthesis of the axis (Hangman's fracture). Radiographs show significant translation of C2 on C3 with severe angulation, classified as a Levine-Edwards Type II fracture. What is the characteristic mechanism of injury for this specific fracture pattern?
Options:
- Pure axial loading resulting in burst morphology
- Hyperextension and axial loading followed by severe flexion
- Pure distraction with associated spinal cord transaction
- Rotational shear leading to unilateral facet dislocation
- Lateral bending causing a compression fracture
Correct Answer: Hyperextension and axial loading followed by severe flexion
Explanation:
Levine-Edwards classification of Hangman's fractures: Type I is caused by hyperextension and axial load (minimal displacement). Type II is characterized by initial hyperextension/axial loading causing the fracture, followed by severe rebound flexion causing displacement and angulation (disruption of the C2-C3 disc). Type IIA is flexion-distraction. Type III involves facet dislocation.
Question 33:
A 19-year-old overhead athlete with multidirectional instability (MDI) of the shoulder has failed a 6-month trial of physical therapy. He undergoes an open inferior capsular shift procedure. During the release of the inferior capsule from the humeral neck, which neurological structure is at greatest risk of iatrogenic injury?
Options:
- Musculocutaneous nerve
- Radial nerve
- Median nerve
- Axillary nerve
- Suprascapular nerve
Correct Answer: Axillary nerve
Explanation:
The axillary nerve runs inferior to the glenohumeral joint capsule as it passes through the quadrangular space. During an inferior capsular shift, release of the capsule from the humeral neck (particularly inferiorly) places the axillary nerve at significant risk. It must be carefully identified and protected, often by leaving a small cuff of capsule on the humerus.
Question 34:
A 3-year-old child presents with progressive bowing of the legs and is diagnosed with infantile Blount's disease (Langenskiöld stage II). Which of the following best describes the primary histological defect in this condition?
Options:
- Abnormal endochondral ossification of the medial proximal tibial physis
- Defective intramembranous ossification of the tibial diaphysis
- Avascular necrosis of the medial tibial epiphysis
- Premature fusion of the lateral distal femoral physis
- Hypertrophy of the zone of provisional calcification secondary to rickets
Correct Answer: Abnormal endochondral ossification of the medial proximal tibial physis
Explanation:
Blount's disease is an osteochondrosis that involves abnormal endochondral ossification at the medial aspect of the proximal tibial physis. Increased compressive forces across the medial knee lead to suppression of physeal growth (Heuter-Volkmann principle). Histologically, there is a disordered, hypercellular zone of hypertrophy and delayed ossification in the medial physis.
Question 35:
A 65-year-old female who underwent a metal-on-metal (MoM) total hip arthroplasty 5 years ago presents with new-onset groin pain and swelling. A MARS MRI reveals a solid-cystic pseudotumor. Histological examination of the periarticular tissue demonstrates Aseptic Lymphocyte-Dominated Vasculitis-Associated Lesion (ALVAL). This pathological process is mediated by which type of immune response?
Options:
- Type I immediate hypersensitivity
- Type II antibody-dependent cytotoxicity
- Type III immune complex-mediated hypersensitivity
- Type IV delayed hypersensitivity
- Type V stimulatory hypersensitivity
Correct Answer: Type IV delayed hypersensitivity
Explanation:
Adverse local tissue reactions (ALTR) in metal-on-metal implants frequently manifest as ALVAL. The histological presence of a dense perivascular lymphocytic infiltrate (predominantly T-cells) characterizes a Type IV delayed hypersensitivity reaction to metal wear debris (typically cobalt and chromium ions).
Question 36:
A 25-year-old elite collegiate football player sustains a purely ligamentous Lisfranc injury to his right foot. Based on level 1 evidence (prospective randomized trials such as those by Coetzee and Ly), which of the following surgical treatments offers the best clinical outcomes and lowest reoperation rates for this specific injury pattern?
Options:
- Closed reduction and percutaneous pinning
- Open reduction and internal fixation (ORIF) with transarticular screws
- Primary arthrodesis of the first, second, and third tarsometatarsal joints
- Primary arthrodesis of all five tarsometatarsal joints
- Flexible fixation utilizing suture buttons alone
Correct Answer: Primary arthrodesis of the first, second, and third tarsometatarsal joints
Explanation:
For purely ligamentous Lisfranc injuries, level 1 evidence (Ly and Coetzee, JBJS 2006) demonstrates that primary arthrodesis of the medial column (1st, 2nd, and 3rd TMT joints) yields significantly better clinical outcomes and lower reoperation rates compared to ORIF. ORIF is associated with high rates of hardware failure and subsequent post-traumatic arthritis necessitating late arthrodesis in purely ligamentous injuries.
Question 37:
A 60-year-old male with a history of lung cancer presents with thigh pain. Radiographs reveal a metastatic lesion in the femur. You apply Mirels' criteria to determine if prophylactic fixation is indicated. Which of the following specific findings yields a maximum score of 3 points in its respective category within Mirels' system?
Options:
- Location in the upper extremity
- Blastic nature of the lesion
- Mild degree of pain
- Size of the lesion occupying 1/3 to 2/3 of the cortex
- Peritrochanteric location
Correct Answer: Peritrochanteric location
Explanation:
Mirels' criteria uses four categories to predict pathologic fracture risk: Site, Pain, Lesion type, and Size. Site scores are: Upper limb (1), Lower limb (2), Peritrochanteric (3). Pain: Mild (1), Moderate (2), Functional/Severe (3). Lesion type: Blastic (1), Mixed (2), Lytic (3). Size: <1/3 (1), 1/3-2/3 (2), >2/3 (3). Thus, a peritrochanteric location yields 3 points.
Question 38:
Articular cartilage is composed of multiple distinct histologic zones, each with unique biochemical properties. Which zone of articular cartilage contains the highest concentration of proteoglycans and the lowest concentration of water?
Options:
- Superficial (tangential) zone
- Middle (transitional) zone
- Deep (radial) zone
- Calcified zone
- Subchondral bone plate
Correct Answer: Deep (radial) zone
Explanation:
The deep (radial) zone of articular cartilage is characterized by the highest concentration of proteoglycans (which provide compressive resistance), the lowest concentration of water, and the thickest collagen fibrils oriented perpendicular to the joint surface. The superficial zone has the highest water content and collagen fibrils parallel to the surface.
Question 39:
A 28-year-old male sustains a high-energy Pauwels type III femoral neck fracture. If this fracture is treated with three parallel cancellous lag screws alone, what biomechanical force is the primary reason for a high rate of fixation failure?
Options:
- High tensile forces along the inferior neck
- High vertical shear forces
- Torsional instability during swing phase
- Distraction forces from the abductor musculature
- Implant pullout secondary to focal osteopenia
Correct Answer: High vertical shear forces
Explanation:
Pauwels classification of femoral neck fractures is based on the angle of the fracture line relative to the horizontal plane. A Pauwels type III fracture is characterized by an angle > 50 degrees (a more vertically oriented fracture line). This orientation converts compressive forces into very high vertical shear forces across the fracture site, which frequently leads to displacement and failure if treated with parallel cancellous screws alone. Fixed-angle constructs (like a sliding hip screw) are favored to resist these shear forces.
Question 40:
A 32-year-old female falls from a height and sustains a Denis Zone 3 sacral fracture. Based on this specific anatomical classification, she is at highest risk for which of the following neurological deficits?
Options:
- Foot drop (L5 nerve root palsy)
- Quadriceps weakness (L4 nerve root palsy)
- Bowel and bladder dysfunction (S2-S4 root injury)
- Isolated loss of the Achilles tendon reflex (S1 root palsy)
- Lateral thigh paresthesia (Lateral femoral cutaneous nerve palsy)
Correct Answer: Bowel and bladder dysfunction (S2-S4 root injury)
Explanation:
The Denis classification of sacral fractures divides the sacrum into three zones. Zone 1 involves the sacral ala (lateral to the foramina) and can involve L5. Zone 2 involves the sacral foramina (risk of sciatica). Zone 3 is central, involving the sacral canal. Zone 3 fractures carry the highest risk (over 50%) of cauda equina syndrome, manifesting as bowel, bladder, and sexual dysfunction due to injury to the S2-S4 nerve roots.