Endoscopic Resection of Posterior Ankle Impingement: An Intraoperative Masterclass
Key Takeaway
Master the endoscopic treatment of posterior ankle impingement. This immersive guide details patient selection, comprehensive anatomy, meticulous intraoperative steps for os trigonum resection, and critical neurovascular safeguards. Learn to manage FHL pathology, prevent complications, and guide postoperative recovery for optimal patient outcomes, especially in high-demand athletes.
Introduction and Epidemiology
Posterior ankle impingement syndrome represents a complex clinical disorder characterized by chronic or acute posterior ankle pain exacerbated by forced plantarflexion. Historically managed with open surgical techniques, the evolution of posterior hindfoot endoscopy has revolutionized the treatment paradigm, offering superior visualization, reduced morbidity, and accelerated return to high-demand activities. Synonyms documented in the orthopedic literature include posterior block of the ankle, posterior triangle pain, talar compression syndrome, os trigonum syndrome, os trigonum impingement, posterior tibiotalar impingement syndrome, and nutcracker-type syndrome.
The primary offending osseous structures are typically the os trigonum or an elongated posterolateral process of the talus, commonly referred to as the Stieda process. The os trigonum originates as a secondary ossification center of the talus, which typically mineralizes between the ages of 11 and 13 years in males and 8 and 11 years in females. Under normal physiologic conditions, this ossification center fuses with the posterior body of the talus within one year of its appearance. However, failure of fusion results in an independent ossicle, remaining as a separate entity in 1.7% to 7% of the normal population. The presence of an os trigonum is observed twice as frequently in a unilateral presentation compared to bilateral occurrences.
Epidemiologically, posterior ankle impingement syndrome is disproportionately observed in athletic populations subjected to repetitive, extreme plantarflexion. Classical cohorts include classical ballet dancers (specifically during en pointe and demi-pointe positioning), soccer players executing instep kicks, gymnastics athletes, and fast bowlers in cricket. The pathology may manifest acutely following a severe hyperplantarflexion injury or, more commonly, insidiously due to repetitive microtrauma leading to disruption of the synchondrosis between the os trigonum and the talus.
Surgical Anatomy and Biomechanics
A rigorous understanding of the posterior ankle and hindfoot anatomy is paramount for safe endoscopic navigation, given the dense concentration of critical neurovascular structures in close proximity to the operative field.
Osseous Structures and Variants
The posterior process of the talus is anatomically divided into a smaller posteromedial process and a larger posterolateral process (trigonal process). These two processes flank the sulcus for the flexor hallucis longus (FHL) tendon, serving as a critical pulley system for the tendon as it transitions from the posterior leg into the midfoot.
When an os trigonum is present, it is typically found in direct connection with the posterolateral tubercle.

The os trigonum is completely corticalized and features three distinct anatomical surfaces: anterior, inferior, and posterior. The anterior surface connects to the posterolateral tubercle via a synchondrosis comprised of fibrous, fibrocartilaginous, or hyaline cartilaginous tissue. The inferior surface contributes to the posterior articulation of the talocalcaneal (subtalar) joint.

Soft Tissue and Neurovascular Landmarks
The posterior surface of the os trigonum is nonarticular and serves as an anchor point for multiple ligamentous structures. These include the posterior talofibular ligament (PTFL), the posterior talocalcaneal ligament, the deep layer of the flexor retinaculum, and the talar component of the fibuloastragalocalcaneal ligament of Rouviere and Canela Lazaro.

The deep posterior compartment musculature transitions into tendinous structures at this level. The tibialis posterior tendon, the flexor digitorum longus tendon, and the FHL tendon are situated in distinct fibrous tunnels. The FHL tendon is the most critical intraoperative landmark during posterior endoscopy. It serves as the medial boundary of the safe working zone.

The primary neurovascular bundle is located immediately medial and anterior to the FHL tendon at the level of the ankle joint. The tibial nerve is the most lateral structure within this bundle, placing it at highest risk if dissection strays medial to the FHL tendon.

Anatomical variants must be anticipated. The peroneocalcaneal internus muscle, frequently termed a false FHL, can mimic the true FHL tendon. Misidentification of this anomalous muscle can lead the surgeon medial to the true FHL, resulting in catastrophic neurovascular injury. Furthermore, vascular anomalies are well-documented; the posterior tibial artery may be hypoplastic or completely absent in 0% to 2% of patients, with a dominant peroneal artery traversing across the posterior ankle toward the tarsal tunnel to supply the plantar foot.
Kinematics and Pathogenesis
The pathogenesis of posterior ankle impingement is predominantly driven by the "nutcracker effect."

During forced terminal plantarflexion, the posterior anatomical structures are forcefully compressed between the posterior rim of the tibial plafond and the superior surface of the calcaneus. Repetitive compression leads to chronic inflammation, capsulitis, and tenosynovitis of the FHL.

In cases involving an os trigonum, the nutcracker mechanism induces shear stress across the synchondrosis, leading to microfractures, non-union, and symptomatic instability of the ossicle. Additionally, acute ankle sprains involving hyperdorsiflexion or inversion can cause an avulsion fracture of the posterior talofibular ligament, leading to secondary impingement from hypertrophic scar tissue or a mobile osseous fragment.

Indications and Contraindications
Patient selection is dictated by a combination of pathognomonic clinical findings and confirmatory advanced imaging. The hallmark clinical sign is reproducible pain during the passive forced plantarflexion test (posterior impingement test). Diagnostic intra-articular or extra-articular injections of local anesthetic under ultrasound guidance can confirm the anatomical source of the nociceptive signaling.
| Category | Specific Criteria |
|---|---|
| Operative Indications | Failure of 3-6 months of non-operative management (NSAIDs, immobilization, physical therapy, targeted corticosteroid injections). |
| Symptomatic os trigonum with MRI evidence of synchondrosis disruption and bone marrow edema. | |
| Symptomatic Stieda process causing mechanical block to plantarflexion. | |
| Concomitant FHL tenosynovitis or FHL entrapment requiring tenolysis. | |
| Posterior intra-articular loose bodies or osteochondral lesions of the posterior talar dome. | |
| Absolute Contraindications | Active local or systemic infection. |
| Severe peripheral vascular disease compromising wound healing. | |
| Lack of definitive clinical diagnosis or negative diagnostic injection. | |
| Relative Contraindications | Severe posterior ankle osteoarthritis (may require arthrodesis rather than simple debridement). |
| Prior extensive posterior open surgical approaches (due to altered anatomy and dense scar tissue). | |
| Achilles tendon pathology requiring simultaneous open reconstruction. |
Pre Operative Planning and Patient Positioning
Imaging Modalities
Standard weight-bearing radiographs of the foot and ankle, including a true lateral projection in neutral and maximal plantarflexion, are mandatory. These views evaluate the size and morphology of the os trigonum, the presence of a Stieda process, and the degree of osseous impingement.
Magnetic Resonance Imaging (MRI) is the gold standard for evaluating soft tissue involvement. Sagittal STIR and T2-weighted sequences are highly sensitive for detecting bone marrow edema within the os trigonum and the adjacent posterior talus, indicating active mechanical stress across the synchondrosis. MRI also evaluates the FHL tendon sheath for fluid, stenosis, or low-lying muscle bellies. Computed Tomography (CT) may be utilized for precise preoperative mapping of complex osseous anatomy, particularly in cases of post-traumatic deformity or suspected loose bodies.
Operating Room Setup
The procedure is performed under general or regional anesthesia. The patient is placed in the prone position. Careful padding of all bony prominences, particularly the anterior superior iliac spines and the contralateral knee, is required. The operative lower extremity is positioned with the foot extending just over the edge of the operating table, allowing for unrestricted, full-arc manipulation of the ankle joint during the procedure. A well-padded thigh tourniquet is applied to maintain a bloodless field.

Standard arthroscopic equipment includes a 4.0-mm, 30-degree arthroscope, standard motorized shavers (4.0 mm to 4.5 mm), radiofrequency ablation wands, and arthroscopic burrs. A fluid management system is utilized, typically maintained at a pressure of 30 to 40 mm Hg to prevent excessive fluid extravasation into the posterior leg compartments.
Detailed Surgical Approach and Technique
The two-portal posterior endoscopic approach, popularized by van Dijk, is the standard of care. This technique relies on establishing an extra-articular working space anterior to the Achilles tendon and posterior to the ankle and subtalar joints.
Portal Placement
Accurate portal placement is critical for avoiding iatrogenic neurovascular injury.

The posterolateral portal is established first. A vertical stab incision is made immediately anterior to the lateral border of the Achilles tendon, at or slightly proximal to the level of the tip of the lateral malleolus. A hemostat is introduced and directed anteriorly toward the first web space, passing through the crural fascia.

The arthroscope trochar is then introduced, and the camera is inserted.
The posteromedial portal is created under direct intra-articular (or extra-articular) visualization. A spinal needle is inserted immediately anterior to the medial border of the Achilles tendon at the same horizontal level as the posterolateral portal.

Once the needle is visualized via the arthroscope, a vertical incision is made, and a shaver is introduced.
Endoscopic Dissection and Resection
The initial phase of the procedure involves clearing the pre-Achilles fat pad to establish the working space.

The shaver blade must always face anteriorly, away from the Achilles tendon, to prevent inadvertent tendon injury. As the fibrofatty tissue is cleared, the posterior capsule of the ankle joint and the subtalar joint come into view.
The FHL tendon must be identified early in the dissection. It is located medially within the working space.

The surgeon must observe the excursion of the FHL tendon by passively flexing and extending the great toe. The FHL tendon represents the absolute medial limit of dissection. No instruments should be passed medial to the FHL tendon to avoid injury to the tibial nerve and posterior tibial artery.
Once the FHL is identified, the os trigonum or Stieda process is localized lateral to the tendon.

The posterior talofibular ligament and the posterior talocalcaneal ligament attachments to the os trigonum are carefully released using a radiofrequency wand or an arthroscopic elevator. The synchondrosis between the os trigonum and the talus is identified.

The ossicle is mobilized using an osteotome, curette, or grasper. If the os trigonum is large, it may need to be fragmented with an arthroscopic burr or a strong grasper before extraction through the portal. If a Stieda process is the primary pathology, an arthroscopic burr is utilized to resect the elongated process until it is flush with the posterior border of the talar body.
Flexor Hallucis Longus Tenolysis
Following osseous resection, attention is turned to the FHL tendon. In many cases of posterior ankle impingement, the FHL is tethered by a stenotic retinaculum or tenosynovitis. The fibro-osseous tunnel of the FHL is released proximally and distally using a retrograde knife or arthroscopic scissors.

The tendon is inspected for partial tears or a low-lying muscle belly, which may contribute to the impingement. Dynamic evaluation is performed by plantarflexing the ankle and extending the hallux to ensure free excursion of the tendon without residual impingement.

Once adequate resection and tenolysis are confirmed, the joint is thoroughly irrigated, and the portals are closed with simple non-absorbable sutures.
Complications and Management
While posterior ankle endoscopy is associated with lower morbidity compared to open approaches, the anatomical density of the posterior hindfoot presents unique risks. Meticulous surgical technique and strict adherence to anatomical landmarks are required to mitigate these complications.
| Complication | Estimated Incidence | Etiology and Prevention | Management and Salvage Strategy |
|---|---|---|---|
| Sural Nerve Injury | 1% - 3% | Proximity to the posterolateral portal. Prevent by using superficial skin incisions and blunt subcutaneous dissection. | Observation for transient neuropraxia. Gabapentinoids for painful neuromas. Surgical excision and burying of the nerve stump for refractory neuromas. |
| Tibial Nerve / Vascular Injury | < 1% | Dissection medial to the FHL tendon. Prevent by establishing the FHL as the strict medial boundary. | Immediate vascular surgery consultation if arterial injury is suspected. Direct repair for nerve transection. |
| Achilles Tendon Injury | < 1% | Direct trauma from the shaver blade. Prevent by keeping the shaver blade facing anteriorly at all times. | Conservative management for minor fraying. Open repair for significant iatrogenic ruptures. |
| Incomplete Resection | 2% - 5% | Failure to adequately visualize the lateral extent of the os trigonum or inadequate burring of the Stieda process. | Revision endoscopy. Ensure dynamic intraoperative testing (forced plantarflexion) prior to closure. |
| Infection | < 1% | Standard surgical risk. Prevent with strict sterile technique and preoperative prophylactic antibiotics. | Oral antibiotics for superficial portal infections. Arthroscopic irrigation and debridement for deep space infections. |
Post Operative Rehabilitation Protocols
The postoperative rehabilitation following endoscopic posterior ankle impingement surgery is generally accelerated compared to open procedures, focusing on early restoration of range of motion and prevention of FHL tendon adhesions.
Acute Phase
During the first 0 to 14 days postoperatively, the patient is placed in a bulky compressive dressing or a removable controlled ankle motion (CAM) boot. Weight-bearing as tolerated (WBAT) is typically permitted immediately, utilizing crutches for support as dictated by patient comfort. Strict elevation is mandated to minimize posterior compartment swelling, which can lead to wound healing complications and increased pain.
Active range of motion (ROM) of the toes, specifically the hallux, is initiated on postoperative day one. This is a critical step to ensure FHL tendon gliding and prevent tethering within the retromalleolar groove. Active dorsiflexion and plantarflexion of the ankle are encouraged to the limits of pain.
Intermediate Phase
At two weeks postoperatively, sutures are removed. The patient is transitioned out of the CAM boot and into a standard supportive shoe. Formal physical therapy commences.
The primary goals of this phase (weeks 2 to 6) include the restoration of full, symmetric ankle and subtalar range of motion. Joint mobilization techniques are utilized to address any residual capsular restriction. Strengthening focuses on the intrinsic foot musculature, the deep posterior compartment (tibialis posterior, FHL, FDL), and the peroneal musculature. Proprioceptive training is initiated using balance boards and uneven surfaces.
Return to Sport Phase
Progression to the final phase of rehabilitation (6+ weeks) is contingent upon achieving pain-free, full range of motion and symmetric strength. For classical ballet dancers, this phase involves a gradual, supervised return to demi-pointe and eventually en pointe work. The therapist must ensure that the dancer is not utilizing compensatory mechanisms, such as midfoot breakdown, to achieve terminal plantarflexion.
For field athletes, agility drills, plyometrics, and sport-specific cutting maneuvers are introduced. Return to competitive play is generally achieved between 8 and 12 weeks postoperatively, provided the athlete can perform sport-specific tasks without apprehension or reactive effusion.
Summary of Key Literature and Guidelines
The paradigm shift from open to endoscopic management of posterior ankle impingement syndrome is heavily supported by modern orthopedic literature. The seminal work by van Dijk et al. established the safety and efficacy of the two-portal hindfoot endoscopic approach, demonstrating a steep but manageable learning curve and significantly reduced postoperative morbidity compared to traditional posteromedial or posterolateral open incisions.
Subsequent systematic reviews and meta-analyses have consistently demonstrated that endoscopic resection of the os trigonum yields excellent functional outcomes. Studies report a return to prior level of sport in over 90% of athletes, with an average return-to-play timeline of approximately 8 to 10 weeks. This is a marked improvement over open techniques, which historically required 16 to 24 weeks for a full return to high-demand activities.
Current clinical guidelines strongly recommend the endoscopic approach for isolated posterior impingement pathology. However, surgeons are cautioned to maintain proficiency in open approaches for complex cases involving massive heterotopic ossification, severe anatomical distortion from prior trauma, or concomitant pathologies requiring extensive reconstruction not amenable to endoscopic techniques. Mastery of the posterior endoscopic anatomy remains a critical competency for the modern foot and ankle surgeon managing athletic populations.
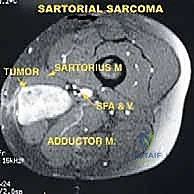
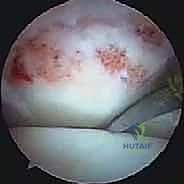
Clinical & Radiographic Imaging


















You Might Also Like