Mini-Open Achilles Tendon Repair: An Intraoperative Masterclass
Key Takeaway
This masterclass details mini-open Achilles tendon repair, focusing on meticulous anatomy, patient positioning, and step-by-step intraoperative execution. Learn precise techniques for suture placement, tensioning, and closure. We cover critical pearls, potential pitfalls, and comprehensive postoperative management, ensuring optimal functional recovery for patients with acute Achilles ruptures.
Introduction and Epidemiology
Spontaneous Achilles tendon ruptures represent a significant orthopaedic challenge and are defined as a partial or complete loss of continuity of the distal tendinous portions of the gastrocnemius and soleus muscles. This catastrophic structural failure results in the consequent loss of physiologic equinus of the ankle and a profound deficit in plantarflexion power. Acute ruptures typically occur in the third to fifth decades of life, predominantly affecting male patients, often during episodic athletic activities. The classic demographic profile is the recreational athlete participating in sports requiring explosive acceleration, sudden changes in direction, or repetitive jumping.

The pathogenesis of Achilles tendon ruptures is multifactorial, driven by two primary competing but often overlapping paradigms, specifically the degenerative theory and the mechanical theory. In the mechanical theory, the tendon suffers acute strain that exceeds its ultimate tensile limit, leading to subsequent failure of the collagen fibrils. Conversely, the degenerative theory posits that chronic, subclinical degeneration of the tendon architecture leads to rupture under normal physiologic loads. Degenerative tendinopathy is present in the vast majority of histologic samples retrieved from spontaneous tendon ruptures. It is widely accepted that degenerated tendons possess diminished tensile strength and are highly susceptible to rupture under physiologic forces.
Histologic analysis demonstrates that ruptured tendons exhibit more advanced intratendinous changes compared to intact tendinopathic tendons. These degenerative alterations are characterized by hypoxic, mucoid, tendolipomatous, and calcific changes. Such pathologic transformations are observed in merely a minority of control tendons. The exact origin of this tendinopathy remains a subject of academic debate, though the overload theory is the most widely accepted. Repeated loading of the musculotendinous unit results in microstructural weakening and, ultimately, failure of the tendon tissue. If the overload persists and the tendon is unable to mount an adequate healing response over time, this weakening propagates, compromising a higher percentage of the total cross sectional area. This failed healing response is modulated by numerous intrinsic factors, including genetics, advancing age, and male gender.
Extrinsic factors and drug related effects also play a critical role in the pathogenesis of Achilles ruptures. Corticosteroids, whether administered locally via injection or systemically, are well documented risk factors for tendon ruptures due to their inhibitory effect on collagen synthesis and fibroblast proliferation. Furthermore, the use of fluoroquinolone antibiotics represents a significant pharmacologic risk factor. Systemic inflammatory conditions, inherent collagen abnormalities, infectious diseases, and hyperlipidemia have similarly been associated with an increased incidence of tendon ruptures.
When left untreated, Achilles ruptures progress to chronic ruptures. The natural history of a neglected rupture involves profound difficulty with ankle plantarflexion, severe atrophy of the gastrocnemius soleus muscle belly, and progressive thickening and scarring of the tendon sheath, which vastly complicates delayed surgical reconstruction.
Surgical Anatomy and Biomechanics
A rigorous understanding of the relevant anatomy is paramount for executing a successful mini open repair. The gastrocnemius muscle merges with the underlying soleus muscle to form the Achilles tendon, which subsequently inserts onto the posterior calcaneal tuberosity. The gastrocnemius muscle is the most superficial muscle of the posterior superficial compartment of the leg. As a biarticular muscle crossing both the knee and the ankle, it is primarily responsible for powerful plantarflexion of the ankle and propelling the body forward during the toe off phase of the gait cycle. In contrast, the soleus muscle is a uniarticular postural muscle with no action on the knee joint, as it originates strictly from the tibia and fibula. The soleus also functions critically as a peripheral vascular pump, facilitating venous return from the lower extremity.

The Achilles tendon is approximately 15 cm in length. It is flattened at both its proximal musculotendinous junction and its distal calcaneal insertion but assumes a rounded morphology in its middle portion. On its anterior surface, the tendon receives muscular fibers from the soleus muscle extending distally almost to its insertion. As the tendon descends, the fibers undergo a variable degree of external rotation, typically 90 degrees, such that the gastrocnemius fibers insert laterally and the soleus fibers insert medially on the calcaneus.
Unlike tendons equipped with a true synovial sheath, the Achilles tendon is enclosed by a paratenon. This structure is a thin, highly vascularized gliding membrane that is continuous proximally with the deep fascia overlying the posterior calf muscles and distally continuous with the periosteum of the calcaneus. The paratenon is the most critical anatomical structure regarding the extrinsic blood supply to the middle portion of the tendon. The majority of the supplying blood vessels arise from the anterior aspect of the paratenon, entering the tendon via the mesotenon. This anterior vascular network is also the primary site where neovascularization occurs in patients suffering from chronic tendinopathy.

Despite the paratenon vascularity, a relatively avascular watershed area exists approximately 2 to 6 cm proximal to the calcaneal insertion. Regarding overall vascular density, the middle portion of the tendon possesses significantly lesser density compared to its proximal musculotendinous or distal insertional parts, predisposing this specific zone to degenerative changes and subsequent rupture.
Biomechanically, the Achilles tendon transmits all the tension generated by the gastrocnemius soleus complex directly to the calcaneus. The tendon is highly elastic and possesses the capability of deforming and recovering its original resting length provided the applied strain does not exceed 4 percent. If the applied strain falls between 4 percent and 8 percent, microscopic failure occurs, and the collagen fibers begin to sustain irreversible damage. At a strain level of approximately 8 percent, macroscopic failure ensues, and the Achilles tendon ruptures.
A critical anatomical consideration during the mini open approach is the sural nerve. The sural nerve courses distally down the posterior calf, typically crossing the lateral border of the Achilles tendon approximately 9.8 cm proximal to the calcaneal insertion. It then runs parallel to the lateral border of the tendon. The proximity of the sural nerve to the lateral aspect of the tendon makes it highly vulnerable to iatrogenic injury during percutaneous or mini open suture passage, necessitating meticulous surgical technique to avoid entrapment.
Indications and Contraindications
The management of acute Achilles tendon ruptures remains a highly debated topic within orthopaedic surgery, with treatment algorithms broadly divided into non operative functional rehabilitation and operative repair. The advent of the mini open technique has shifted the paradigm, offering the biomechanical strength of an open repair while significantly mitigating the wound complication risks associated with traditional extensile open approaches.

Mini open repair is generally indicated for acute, spontaneous ruptures presenting within 2 to 3 weeks of the initial injury. Beyond this timeframe, tendon retraction and muscle atrophy often necessitate a formal open approach, potentially requiring V-Y fascial advancement, turndown flaps, or flexor hallucis longus transfer. The ideal candidate for a mini open repair is a young to middle aged, active patient with a palpable gap located in the classic watershed region 2 to 6 cm proximal to the insertion.
Contraindications to the mini open technique include chronic or neglected ruptures with gap defects exceeding 3 cm after maximal plantarflexion, insertional avulsions requiring suture anchor fixation, and previous local soft tissue compromise that precludes safe percutaneous instrumentation. Systemic contraindications include severe peripheral vascular disease, uncontrolled diabetes mellitus with profound neuropathy, and active local or systemic infection.
| Management Strategy | Primary Indications | Relative Contraindications |
|---|---|---|
| Operative Mini Open Repair | Acute rupture less than 3 weeks old, active lifestyle, high demand athlete, palpable gap in watershed area, delayed presentation with minimal retraction. | Chronic ruptures greater than 4 weeks, gap greater than 3 cm in equinus, severe peripheral vascular disease, active local skin infection, insertional ruptures. |
| Operative Traditional Open Repair | Chronic neglected ruptures, large gap defects requiring augmentation, insertional ruptures requiring anchor fixation, revision Achilles repair. | Poor soft tissue envelope, severe medical comorbidities precluding anesthesia, strictly sedentary lifestyle. |
| Non Operative Functional Rehab | Sedentary patients, elderly patients with low functional demands, high surgical risk patients, acute ruptures with excellent apposition in equinus on ultrasound. | High demand athletes, delayed presentation with wide gap in equinus, non compliant patients unable to adhere to strict bracing protocols. |
Pre Operative Planning and Patient Positioning
Thorough preoperative clinical evaluation is the cornerstone of successful surgical planning. The diagnosis of an acute Achilles tendon rupture is primarily clinical. The pathognomonic physical examination findings include a positive Thompson test, where squeezing the calf muscle belly fails to elicit passive ankle plantarflexion. Additionally, the Matles test will demonstrate a loss of normal resting tension, characterized by increased ankle dorsiflexion of the affected limb when the patient is positioned prone with the knees flexed to 90 degrees. A palpable defect in the substance of the tendon is usually present, though this may be obscured by acute hematoma and localized edema if the examination is delayed.

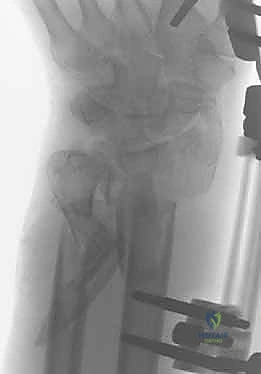
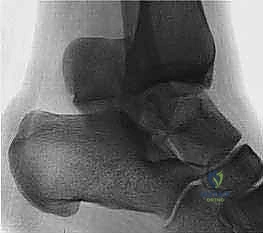
While the diagnosis is clinical, imaging modalities are frequently employed to confirm the diagnosis, characterize the rupture morphology, and assist in surgical planning. Dynamic ultrasonography is highly sensitive and specific, allowing for real time assessment of tendon apposition during passive plantarflexion. Magnetic Resonance Imaging is generally reserved for equivocal cases, delayed presentations to assess the degree of tendon retraction and muscle atrophy, or to evaluate for concomitant pathology.
For the surgical procedure, the patient is typically placed in the prone position on a standard radiolucent operating table. General anesthesia or regional neuraxial anesthesia is utilized based on patient comorbidities and anesthesiologist preference. A well padded thigh tourniquet is applied to the operative extremity to ensure a bloodless surgical field, which is critical for identifying the paratenon and protecting the sural nerve. The operative leg is prepped and draped in a standard sterile fashion, ensuring the entire foot and ankle are exposed to allow for intraoperative manipulation and assessment of resting equinus tension. A bolster is placed under the distal tibia to allow the foot to hang freely, facilitating dynamic assessment of the repair.
Detailed Surgical Approach and Technique
The mini open technique aims to achieve robust mechanical apposition of the ruptured tendon ends while minimizing the disruption of the delicate soft tissue envelope and the critical paratenon blood supply. Various proprietary percutaneous targeting jigs and suture passing devices are available, but the fundamental principles of the technique remain consistent across platforms.
Incision and Superficial Dissection
After exsanguination and tourniquet inflation, the palpable defect is identified. A small transverse or longitudinal incision, typically 2 to 3 cm in length, is centered directly over the palpable gap. A transverse incision is often preferred by some surgeons as it follows Langer lines and may yield a superior cosmetic result, while a longitudinal incision allows for easier proximal or distal extension if the rupture morphology is more complex than anticipated.

Sharp dissection is carried through the epidermis and dermis. The subcutaneous fat is meticulously spread using blunt dissection to avoid injury to the superficial venous plexus and the lesser saphenous vein. The crural fascia is identified and incised longitudinally. Deep to the crural fascia lies the paratenon.
Deep Dissection and Hematoma Evacuation
The paratenon must be handled with utmost care. It is incised longitudinally over the rupture site and carefully retracted. Preservation of the paratenon is a critical step, as it must be closed meticulously at the conclusion of the procedure to restore the gliding mechanism and the anterior vascular supply to the tendon.

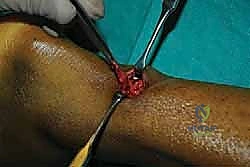
Once the paratenon is opened, the fracture hematoma is encountered. This hematoma is thoroughly evacuated using a combination of suction and blunt curettage. The ruptured tendon ends are typically characterized by a mop end appearance, consisting of frayed, disorganized collagen bundles. The organized, healthy tendon proximal and distal to the rupture zone is identified. Minimal debridement of the tendon ends is performed to preserve length, removing only the most devitalized and avascular tissue.
Suture Device Insertion and Tendon Capture
With the rupture site prepared, the selected percutaneous suture passing device is introduced into the paratenon sheath. For the proximal stump, the jig is inserted deep to the paratenon and advanced proximally. The inner arms of the jig capture the proximal tendon substance. It is imperative to ensure that the jig is seated centrally over the tendon to prevent eccentric suture placement.

High tensile strength, non absorbable multifilament sutures are then passed transversely through the targeting holes of the jig, piercing the skin, paratenon, and tendon substance. To mitigate the risk of sural nerve entrapment, a meticulous technique is required. When passing the lateral needles, the skin should be incised slightly with a scalpel, and a hemostat used to spread the subcutaneous tissues down to the jig prior to advancing the needle. This blunt dissection creates a safe window, pushing the sural nerve away from the trajectory of the needle.
Once the proximal sutures are passed, the device is carefully withdrawn distally, pulling the suture strands out through the central mini open incision. This process yields a robust grasping configuration, often resembling a modified Krackow or locking stitch, securely anchored within the proximal tendon stump. The identical procedure is then repeated for the distal calcaneal stump, ensuring the device is inserted deep to the paratenon and advanced distally toward the calcaneal insertion.
Tendon Approximation and Fixation
With both the proximal and distal tendon stumps secured by the heavy non absorbable sutures, the ankle is placed into maximal plantarflexion. This maneuver approximates the tendon ends and relieves tension on the repair site. The sutures from the proximal stump are tied to the corresponding sutures of the distal stump.
The knot tying sequence must be performed under direct visualization through the mini open incision. The surgeon must ensure that the mop ends of the tendon are intimately apposed and invaginated, preventing any soft tissue interposition. The tension of the repair is verified by comparing the resting equinus of the operative ankle to the contralateral side. The resting tension should ideally match or be slightly tighter than the uninjured side to account for the inevitable physiologic stretching of the construct during the postoperative healing phase.
Paratenon and Wound Closure
Following rigid internal fixation of the tendon, the surgical site is copiously irrigated with sterile saline. The paratenon is then meticulously approximated over the repair site using fine absorbable sutures, such as 3-0 or 4-0 Vicryl. Closure of the paratenon is non negotiable, as it provides a vital biological barrier that prevents adherence of the tendon to the overlying subcutaneous tissue and skin, while simultaneously restoring the extrinsic vascular supply necessary for cellular healing.
The crural fascia and subcutaneous layers are subsequently closed in a layered fashion to eliminate dead space. Finally, the skin is reapproximated using non absorbable nylon sutures or a running subcuticular closure, depending on surgeon preference and the integrity of the skin edges. A sterile, non adherent dressing is applied, and the extremity is immobilized in a well padded short leg splint or a functional controlled ankle motion boot locked in 20 to 30 degrees of plantarflexion.
Complications and Management
While the mini open technique significantly reduces the incidence of catastrophic wound complications compared to traditional open repair, it is not without inherent risks. A thorough understanding of potential complications and their respective salvage strategies is essential for the operating surgeon.

The most unique and concerning complication associated with percutaneous and mini open techniques is iatrogenic injury to the sural nerve. The nerve is particularly vulnerable during the passage of the proximal lateral sutures. Entrapment of the nerve within the suture loop can result in severe neuropathic pain, hyperesthesia, and a positive Tinel sign along the lateral border of the foot. If sural nerve entrapment is suspected postoperatively, early surgical exploration and suture release are mandated to prevent permanent axonal damage and neuroma formation.
Infection, while significantly less common than in traditional open approaches, remains a devastating complication. Superficial surgical site infections can often be managed with targeted oral antibiotic therapy and local wound care. However, deep infections involving the tendon repair or the paratenon require aggressive intervention, including prompt surgical debridement, copious irrigation, and prolonged intravenous antibiotic therapy. In severe cases of deep infection leading to construct failure and tissue necrosis, the infected tendon must be excised, followed by delayed complex reconstruction once the infection is definitively eradicated.
Re-rupture is a risk shared by all treatment modalities for Achilles tendon injuries. The re-rupture rate for mini open repairs is generally comparable to that of traditional open repairs and superior to non operative management. Re-ruptures typically occur within the first three months postoperatively, often secondary to a premature return to weight bearing, a sudden dorsiflexion force, or patient non compliance with the rehabilitation protocol. Management of a re-rupture usually necessitates a formal open revision surgery, frequently requiring augmentation with a flexor hallucis longus transfer or a gastrocnemius fascial turndown flap due to the compromised local tissue quality.
| Complication | Estimated Incidence | Etiology and Risk Factors | Management and Salvage Strategy |
|---|---|---|---|
| Sural Nerve Injury | 2% to 5% | Suture entrapment during lateral pass, direct needle laceration. | Prevention via blunt spreading to the jig. Early exploration and suture release if entrapment is suspected. Neuroma excision for chronic cases. |
| Superficial Infection | 1% to 3% | Poor skin envelope, diabetes, smoking, inadequate paratenon closure. | Local wound care, culture directed oral antibiotics. Close monitoring to prevent deep space extension. |
| Deep Infection | Less than 1% | Contamination, hematoma formation, progression of superficial infection. | Urgent operative debridement, implant removal if necessary, infectious disease consultation, IV antibiotics, delayed reconstruction. |
| Re-Rupture | 2% to 4% | Non compliance, premature aggressive stretching, early unprotected weight bearing. | Formal open revision surgery with V-Y advancement or FHL transfer augmentation. |
| Deep Vein Thrombosis | 1% to 5% | Immobilization, hypercoagulable state, tourniquet use. | Chemical prophylaxis in high risk patients. Therapeutic anticoagulation upon diagnosis. |
Post Operative Rehabilitation Protocols
The evolution of postoperative rehabilitation has mirrored the advancements in surgical technique, shifting from prolonged rigid immobilization to early functional rehabilitation. Early weight bearing and controlled mobilization have been shown to stimulate collagen synthesis, improve collagen fiber alignment, and reduce the incidence of deep vein thrombosis without increasing the risk of re-rupture.

Immediately postoperatively, the patient is placed in a splint or a functional boot locked in significant equinus, typically 20 to 30 degrees. For the first two weeks, patients are generally instructed to remain non weight bearing to allow the initial inflammatory phase of healing to subside and the surgical incisions to seal.
At the two week postoperative mark, assuming uncomplicated wound healing, the sutures are removed. The patient is transitioned to a functional rehabilitation protocol. Weight bearing is progressively initiated in the boot, utilizing heel wedges to maintain the equinus position and protect the repair from excessive dorsiflexion strain. Active plantarflexion and controlled active dorsiflexion to neutral are typically initiated under the guidance of a physical therapist.
Over the subsequent four to six weeks, the heel wedges are sequentially removed, gradually bringing the ankle from equinus to a neutral position. By postoperative week eight, patients are usually transitioned out of the boot into regular footwear with a small heel lift. Strengthening exercises are advanced, focusing on concentric and eccentric loading of the gastrocnemius soleus complex. Return to high impact sports and explosive activities is generally delayed until six to nine months postoperatively, contingent upon the recovery of symmetric muscle strength, endurance, and proprioceptive control.
Summary of Key Literature and Guidelines
The academic discourse surrounding the optimal management of acute Achilles tendon ruptures is vast and continually evolving. High level evidence, including randomized controlled trials and comprehensive meta analyses, heavily influences contemporary clinical practice guidelines.
The landmark randomized controlled trial by Willits et al. demonstrated that when an accelerated functional rehabilitation protocol is employed, there is no statistically significant difference in re-rupture rates between operative and non operative management. However, this study primarily utilized traditional open surgical techniques, which carry a higher inherent risk of wound complications.
Subsequent meta analyses, such as the comprehensive review by Soroceanu et al., have clarified the nuances of surgical intervention. These analyses suggest that while functional rehabilitation narrows the gap in re-rupture rates, operative repair still provides a statistically significant reduction in re-ruptures, particularly in younger, high demand cohorts. Furthermore, operative repair is associated with a higher likelihood of returning to pre injury levels of athletic performance and a lower incidence of profound calf atrophy.
The introduction of the mini open technique represents a critical synthesis of these findings. By combining the robust mechanical fixation of an open repair with the minimal soft tissue disruption of percutaneous techniques, the mini open approach effectively minimizes the wound complication rates that historically detracted from the appeal of surgical intervention. The American Academy of Orthopaedic Surgeons clinical practice guidelines reflect this nuanced understanding, offering moderate recommendations for operative repair in active patients while emphasizing the critical importance of early functional rehabilitation regardless of the chosen treatment modality. The mini open technique, therefore, stands as a highly efficacious, evidence based surgical option for the management of acute Achilles tendon ruptures in appropriately selected patients.
Clinical & Radiographic Imaging










You Might Also Like