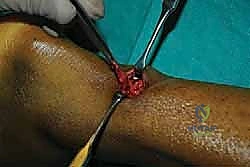
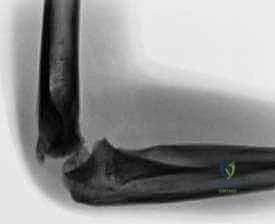
Masterclass: Open Reduction and Internal Fixation of Bicondylar Tibial Plateau Fractures
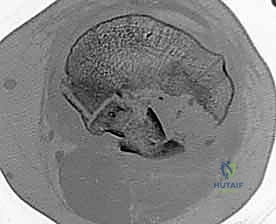
Key Takeaway
This masterclass guides fellows through open reduction and internal fixation of bicondylar tibial plateau fractures. We cover essential surgical anatomy, meticulous preoperative planning, and a granular, real-time intraoperative execution from the surgeon's perspective. Learn precise dissection, reduction techniques, hardware application, and critical pearls to optimize outcomes and manage potential complications for these complex injuries.
Introduction and Epidemiology
Bicondylar tibial plateau fractures represent a severe and complex subset of periarticular knee injuries, typically classified under the AO/OTA system as 41-C (complete articular, multifragmentary) fractures. These injuries inherently involve both the medial and lateral tibial plateaus, disrupting the primary weight-bearing surface of the proximal tibia and compromising the mechanical axis of the lower extremity.

Schatzker type 5 fractures involve both condyles without complete dissociation from the tibial diaphysis. In these patterns, a portion of the articular joint remains in continuity with the shaft, providing a critical keystone for reduction. These are usually amenable to medial and lateral buttress plate fixation. Conversely, Schatzker type 6 fractures involve both condyles with complete metadiaphyseal dissociation of the articular segment from the shaft. This complete uncoupling presents a profound biomechanical challenge, requiring meticulous restoration of the mechanical axis and robust bridging fixation.

Lateral fractures with associated posteromedial fragments must be distinguished from other bicondylar types. The posteromedial fragment is often a coronal shear injury that escapes capture by standard lateral locked plating. It frequently requires independent posteromedial buttress fixation and may be representative of a high-energy fracture-dislocation variant.

Bicondylar tibial plateau fractures are typically caused by a high-energy mechanism, such as motor vehicle collisions or falls from significant height, leading to profound associated injury to the surrounding soft tissue envelope. The mechanism responsible for injury is primarily a severe axial force, which may be coupled with a varus or valgus moment. With a valgus force, the lateral femoral condyle is driven wedge-like into the underlying lateral tibial plateau, causing central depression and lateral blowout. The size and comminution of the fracture fragments depend on multiple factors, including localization of the impact, the magnitude of the axial force, subchondral bone density, and the position of the knee joint at the moment of trauma.

Joint incongruity can predispose to rapid-onset arthrosis. Inadequate fracture stability can lead to catastrophic hardware failure, progressive varus or valgus collapse, and accelerated post-traumatic osteoarthritis. Furthermore, ligamentous injuries have been found to occur in 20% to 77% of tibial plateau fractures. The role of acute repair of ligament injuries at the time of fracture fixation remains controversial. Some advocate concurrent ligamentous repair, while the prevailing consensus suggests that if the bony architecture can be anatomically reduced and stabilized, early ligamentous repair is often unnecessary, allowing the ligaments to heal in an isometric position.
Surgical Anatomy and Biomechanics
A profound understanding of proximal tibial anatomy is non-negotiable for successful surgical reconstruction. In the loaded knee, the medial plateau bears approximately 60% to 75% of the physiological load. Consequently, stronger, denser subchondral bone is found on the medial side to accommodate this increased load transmission.

Morphologically, the medial plateau is larger and concave, acting in concert with the medial femoral condyle to provide inherent osseous stability. The lateral plateau is convex and sits anatomically higher than the medial plateau. The medial proximal tibial angle (MPTA) is 87 degrees relative to the anatomic axis of the tibia (normal range 85 to 90 degrees). The proximal posterior tibial angle (PPTA), representing the physiological posterior slope, is 81 degrees relative to the anatomic axis of the tibia (normal range 77 to 84 degrees). Restoration of both the MPTA and PPTA is critical to prevent abnormal kinematics and premature wear.

Ligamentous and Meniscal Anatomy
The soft tissue attachments dictate the deforming forces on fracture fragments. The iliotibial band inserts on the tubercle of Gerdy on the anterolateral tibia, often serving as a landmark for anterolateral surgical approaches.

The anterior cruciate ligament (ACL) attaches adjacent and medial to the tibial eminence. It acts to resist anterior translation of the tibia relative to the femur. Recognizing a fracture fragment that contains this attachment (often an avulsion of the tibial spine) is vital, as stabilizing this fragment is necessary to re-establish sagittal plane stability to the knee.

The posterior cruciate ligament (PCL) attaches about 1 cm below the joint line on the posterior ridge of the tibial plateau and a few millimeters lateral to the midline. The function of the PCL is to resist posterior tibial translation relative to the femur, acting as the central kinematic pivot of the knee.

The collateral ligaments provide coronal stability. The medial collateral ligament (MCL) resists valgus force, originating on the medial femoral epicondyle and inserting distally on the medial tibial metaphysis. The lateral collateral ligament (LCL) resists varus force and external rotation of the femur, originating on the lateral epicondyle and attaching to the fibular head.

The menisci are crescent-shaped fibrocartilaginous structures that act to dissipate load, deepen the articular surfaces, and provide joint lubrication and nutrition. The medial meniscus is more C-shaped and firmly attached, whereas the lateral meniscus is more circular and mobile. Peripheral meniscal detachments are exceedingly common in bicondylar fractures and must be addressed via submeniscal arthrotomy and subsequent repair during fixation.

Indications and Contraindications
The management of bicondylar tibial plateau fractures is dictated by the degree of articular displacement, metaphyseal comminution, and the integrity of the soft tissue envelope. Operative intervention is the gold standard for displaced bicondylar patterns to restore joint congruity, mechanical alignment, and permit early range of motion.

Operative vs Non Operative Management Parameters
| Management Strategy | Indications | Contraindications |
|---|---|---|
| Operative Fixation (ORIF/Ex-Fix) | Articular step-off > 2-3 mm; Condylar widening > 5 mm; Varus/Valgus instability > 5 degrees; All Schatzker V and VI fractures; Open fractures; Associated compartment syndrome. | Active local infection; Non-ambulatory patient; Severe medical comorbidities precluding anesthesia; Uncorrectable coagulopathy. |
| Non-Operative (Cast/Brace) | Non-displaced or minimally displaced fractures; Medically unstable patients; Severe baseline dementia or non-ambulatory status. | Displaced articular fragments; Mechanical axis deviation; Open fractures; Compartment syndrome. |

In cases of severe soft tissue compromise (e.g., fracture blisters, massive edema), definitive internal fixation is contraindicated acutely. The standard of care shifts to "Damage Control Orthopedics," utilizing a knee-spanning external fixator to restore length, alignment, and rotation while allowing the soft tissue envelope to recover over 10 to 21 days.

Pre Operative Planning and Patient Positioning
Thorough preoperative planning is paramount for executing a complex bicondylar reconstruction. Standard orthogonal radiographs (AP and Lateral) provide an initial assessment of the fracture pattern and metaphyseal extension. However, a fine-cut Computed Tomography (CT) scan with 2D multiplanar reconstructions and 3D surface rendering is mandatory.

CT imaging allows the surgeon to map the articular surface, identify central depression that may be hidden behind an intact cortical rim, and accurately conceptualize the fracture according to the "Three-Column Concept" (medial, lateral, and posterior columns). Identifying a posteromedial or posterolateral shear fragment is critical, as these dictate the surgical approaches required.

Optimizing Patient Positioning
Positioning depends entirely on the planned surgical approaches.
1. Supine Position: Standard for anterolateral and limited medial approaches. A bump is placed under the ipsilateral hip to internally rotate the leg to neutral. A radiolucent triangle or ramp is utilized to allow variable knee flexion, which relaxes the deforming pull of the gastrocnemius.
2. Prone Position: Indicated when isolated posterior approaches (posteromedial or posterolateral) are required for primary posterior shear fractures.
3. Floppy Lateral / Floating Supine: Allows access to both the posteromedial and anterolateral aspects of the knee by externally and internally rotating the hip, respectively.

A sterile tourniquet is typically applied to the proximal thigh to provide a bloodless field during the critical articular reduction phases, though its use should be minimized to reduce ischemic time and postoperative pain.

Detailed Surgical Approach and Technique
The surgical management of Schatzker V and VI fractures generally necessitates a dual-incision technique. Attempting to reduce and fix a bicondylar fracture through a single anterior midline incision with extensive medial and lateral stripping is historically associated with catastrophic wound necrosis and deep infection, and is now largely abandoned.

The Posteromedial Approach
The posteromedial approach is typically executed first to stabilize the medial column, restoring the anatomical length and mechanical axis of the tibia.
1. Incision: A longitudinal incision is made along the posteromedial border of the tibia, starting at the joint line and extending distally.
2. Internervous Plane: There is no true internervous plane; dissection occurs between the medial gastrocnemius (tibial nerve) and the pes anserinus tendons (femoral and obturator nerves).
3. Deep Dissection: The medial gastrocnemius is retracted posteriorly and laterally, protecting the neurovascular bundle. The popliteus muscle may be partially elevated to expose the posterior articular fracture lines.
4. Reduction: The posteromedial fragment is typically reduced via hyperextension and direct manipulation with a ball-spike pusher or dental pick.
5. Fixation: An under-contoured posteromedial buttress plate (often a 3.5mm T-plate or specific posteromedial plate) is applied in an anti-glide fashion to counteract the vertical shear forces.

By stabilizing the medial column first, the surgeon converts a complex Schatzker VI fracture into a simpler Schatzker III or II, providing a stable foundation against which the lateral plateau can be reconstructed.

The Anterolateral Approach
Following medial stabilization, attention is turned to the lateral articular depression and widening.
1. Incision: A curvilinear incision is made centered over Gerdy's tubercle, resembling a hockey stick.
2. Superficial Dissection: The iliotibial band is incised in line with its fibers.
3. Submeniscal Arthrotomy: The coronary ligament is incised to elevate the lateral meniscus, providing direct visualization of the lateral articular surface. Stay sutures are placed in the meniscus for later repair.
4. Articular Reduction: A cortical window is created in the anterolateral metaphysis. Using a bone tamp, the depressed articular segments are elevated en masse to restore the joint line.
5. Void Filling: The resulting metaphyseal void is grafted with autograft, allograft, or synthetic bone substitutes (e.g., calcium phosphate) to support the elevated articular surface.
6. Fixation: A pre-contoured lateral locking plate (typically 3.5mm or 4.5mm system) is applied. Subchondral raft screws are placed as close to the articular surface as possible to prevent secondary subsidence.

Throughout the procedure, orthogonal fluoroscopy must be utilized to confirm articular reduction, restoration of the MPTA and PPTA, and appropriate hardware trajectory, ensuring no screws penetrate the joint space.

Alternative Fixation Strategies
In cases of extreme metaphyseal comminution or compromised soft tissues where extensive plating is perilous, fine wire circular external fixation (Ilizarov or Taylor Spatial Frame) presents a powerful alternative. This technique relies on tensioned wires for periarticular capture and allows for immediate weight-bearing in some protocols, while completely bypassing the zone of soft tissue injury.


Regardless of the modality, the absolute goals remain constant: anatomic articular reduction, restoration of mechanical alignment, and stable fixation permitting early mobilization.

Complications and Management
Bicondylar tibial plateau fractures carry a high complication profile due to the severity of the initial trauma and the complexity of the required surgical interventions.

Summary of Common Complications
| Complication | Incidence | Etiology and Pathogenesis | Prevention and Salvage Strategies |
|---|---|---|---|
| Compartment Syndrome | 10-20% | High-energy axial load causing massive intramuscular edema and bleeding within rigid fascial compartments. | Vigilant clinical monitoring; avoid early definitive fixation in swollen limbs. Salvage: Emergent four-compartment fasciotomy. |
| Deep Infection | 5-15% | Extensive soft tissue stripping; compromised vascularity; prolonged operative time. | Delay definitive fixation until soft tissues wrinkle; utilize dual incisions with wide skin bridges (>7 cm). Salvage: Hardware removal, radical debridement, antibiotic spacers, flap coverage. |
| Post-Traumatic Osteoarthritis | 20-40% | Residual articular step-off > 2mm; mechanical axis malalignment; initial cartilage cell death at impact. | Anatomic articular reduction; subchondral rafting; restoration of normal MPTA. Salvage: Total knee arthroplasty (TKA). |
| Hardware Failure / Subsidence | 5-10% | Inadequate buttressing of the posteromedial fragment; insufficient structural bone grafting of metaphyseal voids. | Recognize and independently plate coronal shear fragments; utilize robust bone void fillers. Salvage: Revision ORIF with structural grafting or conversion to TKA. |

Post-traumatic osteoarthritis (PTOA) is the most frequent long-term complication. The rate of PTOA correlates strongly with the quality of the articular reduction and the restoration of the mechanical axis. However, even with perfect radiographic reconstruction, the initial impact causes irreversible chondrocyte apoptosis, making some degree of arthrosis inevitable in high-energy patterns.

Post Operative Rehabilitation Protocols
The postoperative rehabilitation phase is as critical as the surgical execution. The primary goals are to prevent joint stiffness, protect the articular reconstruction from premature loading, and mitigate the risk of deep vein thrombosis (DVT).

Early Mobilization Phase
Continuous Passive Motion (CPM) or early active-assisted range of motion is initiated within the first 24 to 48 hours post
Clinical & Radiographic Imaging































You Might Also Like