Masterclass: Open Reduction and Internal Fixation of Lateral Tibial Plateau Fractures
Key Takeaway
Welcome, fellows, to an immersive intraoperative masterclass on lateral tibial plateau fracture ORIF. We'll meticulously cover comprehensive anatomy, preoperative planning, and precise, real-time surgical execution. Learn critical techniques for reduction, bone grafting, meniscal repair, and optimal hardware placement. Understand potential pitfalls and strategies for effective postoperative rehabilitation and complication management to ensure superior patient outcomes.
Introduction and Epidemiology
Lateral tibial plateau fractures represent a significant portion of intra-articular fractures of the lower extremity, frequently resulting in malalignment of the articular surface and bearing a high risk of subsequent post-traumatic osteoarthritis. These injuries exhibit a bimodal distribution. In younger demographics, they typically occur secondary to high-energy trauma, such as motor vehicle collisions or falls from a significant height, often resulting in complex fracture patterns with substantial soft tissue compromise. Conversely, in the elderly population, lateral plateau fractures frequently manifest as low-energy injuries, predominantly depression-type fractures occurring in osteoporotic bone that is less capable of withstanding axial compression.

The lateral tibial plateau is disproportionately affected compared to the medial plateau. Twisting injuries account for approximately 5 to 10 percent of tibial plateau fractures and are most commonly associated with athletic activities such as skiing. The mechanism of injury dictates the fracture morphology; split or wedge fractures (Schatzker Type I) predominantly occur in younger patients with dense cancellous bone, whereas pure depression fractures (Schatzker Type II and III) occur more frequently in older patients. Understanding the precise epidemiology and energy transfer mechanisms is fundamental for orthopedic surgeons when anticipating associated soft tissue injuries, meniscal pathology, and ligamentous disruption.
Surgical Anatomy and Biomechanics
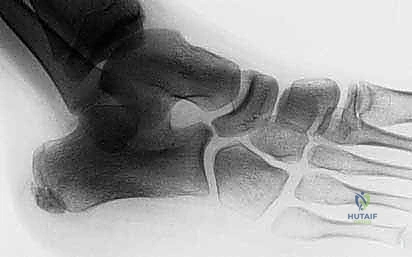
The proximal tibia consists of three primary osseous structures: the lateral plateau, the medial plateau, and the intercondylar eminence. The lateral plateau is smaller, convex, and sits slightly higher than the medial joint surface, forming an angle of approximately 3 degrees of varus with respect to the tibial shaft. This distinct anatomical orientation is a critical landmark for identifying the lateral plateau on orthogonal lateral radiographs.

Both plateaus are covered by a meniscus, which serves as a vital shock absorber and improves the congruency of the femorotibial joint. The asymmetric weight-bearing biomechanics of the knee dictate an eccentric load distribution, wherein the lateral plateau bears approximately 40 percent of the knee load during standard ambulation. This asymmetric weight-bearing results in increased medial subchondral bone formation, rendering the medial plateau stronger and denser, while the lateral plateau remains relatively softer and more susceptible to deformation under valgus and axial loads.

Ligamentous and Soft Tissue Attachments
The intermediate, nonarticular intercondylar eminence serves as the tibial attachment site for the anterior and posterior cruciate ligaments. The stability of the knee joint is intrinsically reliant on these cruciate ligaments, the collateral ligaments, and the joint capsule. The tibial tuberosity and the tubercle of Gerdy are prominent bony landmarks located in the subcondylar region, serving as the insertion points for the patellar tendon and the iliotibial tract, respectively. These landmarks are essential for planning surgical incisions and understanding the deforming forces acting upon fracture fragments.

Several anatomic factors contribute to the higher incidence of lateral versus medial plateau fractures. The relative softness of the subchondral bone of the lateral plateau, the physiologic valgus axis of the lower extremity, and the susceptibility of the leg to medially directed forces all predispose the lateral plateau to failure. The most frequent mechanism causing a lateral plateau fracture involves direct trauma to the proximal tibia, inducing a valgus force that drives the lateral femoral condyle into the softer lateral tibial plateau.
Indications and Contraindications
The natural history of lateral tibial plateau fractures depends heavily on the degree of articular depression, condylar widening, and overall knee stability. Knee instability may result directly from the bony fracture but is frequently exacerbated by accompanying soft tissue injuries, including meniscal tears or ruptures of the cruciate and collateral ligaments. Meniscal injuries have been reported in up to 50 percent of tibial plateau fractures and act as a major determinant of long-term prognosis, as meniscal integrity is paramount for joint stability and load distribution.

For non-displaced or minimally displaced fractures without associated ligamentous instability, the prognosis with conservative management is generally favorable. However, displaced fractures, particularly those resulting in mechanical axis deviation or significant articular incongruity, typically mandate surgical intervention to mitigate the risk of early post-traumatic arthritis.
Operative Versus Non Operative Management Parameters
| Clinical Parameter | Operative Indications | Non Operative Indications |
|---|---|---|
| Articular Step Off | Greater than 2 to 3 mm | Less than 2 mm |
| Condylar Widening | Greater than 5 mm | Minimal to none |
| Mechanical Axis | Varus or valgus malalignment | Preserved mechanical axis |
| Joint Stability | Instability at 20 degrees of flexion | Stable through full range of motion |
| Patient Status | Ambulatory patient with functional demands | Non ambulatory or severe medical comorbidities |
| Soft Tissue Envelope | Resolving swelling positive wrinkle sign | Severe compromise requiring delayed fixation |
Contraindications to immediate definitive internal fixation primarily revolve around the condition of the soft tissue envelope. The marginal soft tissue coverage of the proximal tibia predisposes the region to severe complications, including wound dehiscence, deep infection, and tissue necrosis. In the presence of fracture blisters, massive edema, or an impending compartment syndrome, definitive plating is strictly contraindicated. In such scenarios, damage control orthopedics utilizing joint-spanning external fixation is the standard of care until soft tissue homeostasis is achieved.
Pre Operative Planning and Patient Positioning
A thorough physical examination must always include an exhaustive assessment of the soft tissue envelope. Severe soft tissue injury may preclude primary plating, necessitating temporizing external fixation. Furthermore, clinicians must maintain a high index of suspicion for compartment syndrome, which may result from continuous hemorrhage through the metaphysis into the area of the anterior, lateral, or deep posterior tibial compartments.

Imaging Modalities and Templating
Standard orthogonal radiographs (anteroposterior and lateral views) are the initial imaging modalities of choice. However, two-dimensional plain radiography often underestimates the degree of articular depression and the complexity of the fracture lines. Therefore, a fine-cut computed tomography scan with coronal, sagittal, and three-dimensional reconstructions is considered mandatory for adequate preoperative planning. The CT scan allows the surgeon to map the fracture fragments, identify the location of the primary articular depression, and select the appropriate trajectory for raft screws and buttress plates.

Preoperative templating should be performed to anticipate hardware requirements, including the length and contour of the lateral proximal tibial plate, the volume of bone graft or bone substitute required to fill the metaphyseal void, and the potential need for independent lag screws.
Operating Room Setup
The patient is typically positioned supine on a radiolucent operating table to facilitate unimpeded fluoroscopic imaging. A bump is placed beneath the ipsilateral hip to correct natural external rotation, ensuring the patella faces directly anteriorly. A non-sterile tourniquet is applied to the proximal thigh to optimize visualization during the critical phases of articular reduction. The contralateral leg must be protected and positioned to allow the C-arm to enter from the unaffected side, providing clear orthogonal views of the proximal tibia without obstruction.

Detailed Surgical Approach and Technique
The anterolateral approach is the workhorse for addressing lateral tibial plateau fractures. It provides excellent access to the lateral articular surface, the lateral metaphysis, and the anterior aspect of the lateral condyle.
Incision and Superficial Dissection
An S-shaped or gently curved incision is made, beginning 3 to 5 centimeters proximal to the joint line, centered over Gerdy's tubercle, and extending distally along the anterolateral aspect of the tibial shaft. Full-thickness fasciocutaneous flaps are elevated to preserve the tenuous blood supply to the skin. The iliotibial band is identified, and an incision is made in line with its fibers or slightly anterior to it, entering the internervous plane between the iliotibial band and the tibialis anterior muscle.

The anterior tibial muscle origin is carefully elevated off the proximal lateral tibia. Care must be taken not to dissect too far posteriorly or distally to avoid injury to the anterior tibial artery as it passes through the interosseous membrane, as well as the common peroneal nerve winding around the fibular neck.
Submeniscal Arthrotomy and Joint Visualization
To achieve anatomic reduction of the articular surface, direct visualization is paramount. A submeniscal arthrotomy is performed by incising the coronary ligaments attaching the anterior horn and body of the lateral meniscus to the tibial plateau. Stay sutures are placed in the meniscus, allowing it to be retracted proximally. This maneuver exposes the entire lateral articular surface. A femoral distractor or varus stress applied to the knee can further open the lateral compartment, providing a clear view of the depressed articular fragments.

Articular Reduction and Void Management
Once the fracture is exposed, the split fragment (if present) is hinged open like a book to reveal the central area of articular depression. Using a bone tamp introduced through the metaphyseal fracture line or a dedicated cortical window, the depressed articular segments are carefully elevated from distal to proximal. The elevation must be performed meticulously to avoid over-distracting or fragmenting the chondral surface.

Elevation of the articular surface inevitably creates a metaphyseal bone void. This defect must be filled to provide structural support and prevent late subsidence of the articular surface. Options for void fillers include autologous bone graft (typically harvested from the iliac crest), allograft cancellous chips, or synthetic calcium phosphate cements. Calcium phosphate is highly favored in modern practice due to its high compressive strength, which exceeds that of cancellous bone, allowing for earlier mobilization.
Definitive Fixation Strategy
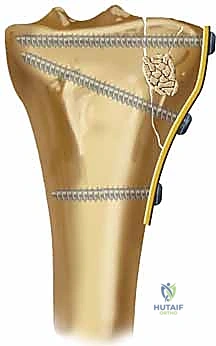
Following articular reduction and grafting, the lateral split fragment is reduced and provisionally held with pointed reduction forceps. Kirschner wires are placed subchondrally to maintain the articular reduction. Definitive fixation is achieved using a pre-contoured lateral proximal tibial locking plate. The plate functions as a buttress against the lateral cortex to resist the valgus deforming forces.

Subchondral raft screws (typically 3.5 mm) are inserted through the proximal holes of the plate, positioned immediately beneath the subchondral bone to support the elevated articular fragments. Distal fixation in the diaphysis is achieved with a combination of cortical and locking screws, depending on bone quality. Fluoroscopy is utilized throughout the procedure to confirm anatomic articular reduction, restoration of the mechanical axis, and appropriate hardware placement without intra-articular penetration.
Finally, the lateral meniscus must be meticulously repaired back to the joint capsule using the previously placed stay sutures to restore its hoop stresses and shock-absorbing capabilities.
Complications and Management
Surgical management of lateral tibial plateau fractures is fraught with potential complications, largely due to the high-energy nature of the trauma and the precarious soft tissue envelope surrounding the proximal tibia.

Early recognition and aggressive management of these complications are critical for preserving limb function. Post-traumatic osteoarthritis remains the most common long-term complication, directly correlating with the severity of the initial cartilage damage, residual articular step-off, and the status of the meniscus.
Common Complications and Salvage Strategies
| Complication | Estimated Incidence | Etiology and Risk Factors | Management and Salvage Strategy |
|---|---|---|---|
| Compartment Syndrome | 5 to 10 percent | High energy trauma continuous metaphyseal hemorrhage | Emergent four compartment fasciotomy delayed fracture fixation |
| Deep Surgical Site Infection | 2 to 8 percent | Poor soft tissue envelope early surgical intervention | Aggressive serial debridement hardware retention if stable appropriate IV antibiotics |
| Loss of Reduction | 5 to 15 percent | Osteoporotic bone inadequate void filling premature weight bearing | Revision open reduction and internal fixation augmentation with cement or longer plate |
| Post Traumatic Osteoarthritis | 20 to 40 percent | Articular incongruity meniscal loss cartilage necrosis | Conservative management initially total knee arthroplasty for end stage disease |
| Common Peroneal Nerve Palsy | 1 to 3 percent | Traction injury during varus stress or retractor placement | Observation baseline EMG at 6 weeks ankle foot orthosis for foot drop |
| Arthrofibrosis | 10 to 15 percent | Prolonged immobilization severe intra articular scarring | Aggressive physical therapy manipulation under anesthesia arthroscopic lysis of adhesions |
Infection management in the presence of hardware requires a nuanced approach. If the fixation remains absolutely stable, the hardware should be retained while the patient undergoes serial irrigation and debridement procedures coupled with culture-directed antibiotic therapy. If the hardware is loose or the fracture has united, hardware removal is indicated.
Post Operative Rehabilitation Protocols
The primary goals of postoperative rehabilitation are to restore full knee range of motion, prevent arthrofibrosis, and protect the articular reduction until bony union is achieved. The rehabilitation protocol must be tailored to the specific fracture pattern, the security of the fixation, and the presence of concomitant soft tissue repairs, such as meniscal suturing.
Immediately postoperatively, the knee is typically placed in a hinged knee brace. Continuous passive motion machines or early active-assisted range of motion exercises are initiated within the first 24 to 48 hours to promote cartilage nutrition and prevent capsular contractures.
Weight-bearing restrictions are strict. Patients are generally restricted to non-weight-bearing or toe-touch weight-bearing status for 8 to 12 weeks. The exact duration depends on radiographic evidence of callus formation and the consolidation of the metaphyseal void filler. Premature weight-bearing is a primary driver of articular subsidence and hardware failure. Progressive weight-bearing is initiated only after clinical and radiographic signs of healing are confirmed, usually transitioning to full weight-bearing by 12 to 16 weeks postoperatively. Strengthening of the quadriceps and hamstring musculature is emphasized throughout the recovery phase to restore dynamic joint stability.
Summary of Key Literature and Guidelines
The academic understanding and surgical approach to lateral tibial plateau fractures have evolved significantly, guided by landmark literature and advanced imaging techniques. The traditional Schatzker classification remains a fundamental communication tool among orthopedic surgeons. However, modern literature emphasizes the importance of three-dimensional column concepts for complex fracture patterns.
Luo and colleagues introduced the three-column concept utilizing axial CT imaging, dividing the tibial plateau into lateral, medial, and posterior columns. This classification highlights the frequently overlooked posterolateral shear fragments that are poorly visualized on standard radiographs and inadequately addressed through a standard anterolateral approach.
Furthermore, Kfuri and Schatzker published a revised classification system in 2018 that integrates 3D CT mapping into the original Schatzker framework, providing a more comprehensive understanding of the principal fracture planes. Their work underscores that lateral plateau fractures (Schatzker I, II, and III) frequently involve the posterior articular segments, necessitating specific positioning and potentially altered surgical approaches, such as a posterolateral approach with fibular osteotomy, to achieve direct buttressing of the posterior cortex.
The management of meniscal injuries in the setting of plateau fractures has also been extensively studied. Literature demonstrates that repairing peripheral meniscal tears concurrently with fracture fixation significantly improves long-term functional outcomes and delays the onset of post-traumatic osteoarthritis. The consensus within the orthopedic community strongly advocates for meniscal preservation whenever technically feasible, reinforcing the necessity of the submeniscal arthrotomy technique for both visualization and subsequent repair.
Clinical & Radiographic Imaging













You Might Also Like