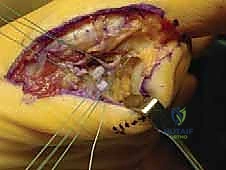
Masterclass: Surgical Management of Femoral Metastatic Bone Disease – Proximal and Diaphyseal Lesions
Key Takeaway
This masterclass guides fellows through the surgical management of metastatic bone disease in the proximal and diaphyseal femur. We meticulously cover comprehensive anatomy, detailed preoperative planning, and granular intraoperative execution, including curettage, cement augmentation, and internal fixation with intramedullary nails or endoprostheses. Critical pearls, potential pitfalls, and essential postoperative care are emphasized to ensure durable reconstruction and optimal patient outcomes.
Introduction and Epidemiology
The femur represents the most common site within the appendicular skeleton for metastatic bone disease requiring surgical intervention. As the primary weight-bearing axis of the lower extremity, the femur is subjected to immense biomechanical forces during standard ambulation. Consequently, metastatic infiltration in this region presents a profound risk for structural failure. The operative management of femoral metastases leaves minimal margin for surgical error; procedures must be rigorously planned and meticulously executed with the primary objective of achieving durable, immediate mechanical reconstruction. Metastatic lesions predominantly affect the proximal third of the femur, a phenomenon directly correlated with the high concentration of persistent hematopoietic red marrow and the robust vascular supply characteristic of the proximal metaphysis and diaphysis.
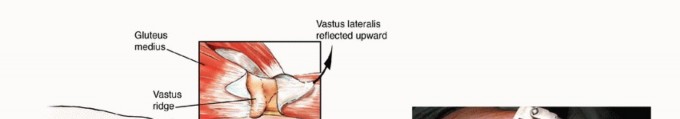
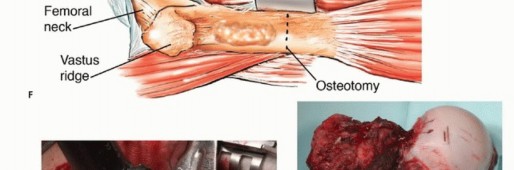
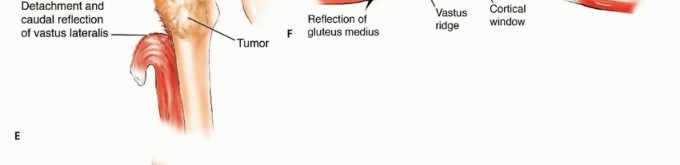
Unlike primary bone and soft tissue sarcomas of the extremity, metastatic carcinomas typically exhibit a relatively confined soft tissue component, even in the presence of extensive cortical osteolysis and medullary canal obliteration. This distinctive oncologic characteristic is surgically advantageous, allowing the orthopedic oncologist to spare vital extracortical structures. Preservation of the joint capsule, overlying musculature, and tendinous attachments is paramount for post-reconstruction functional recovery. Specifically, the meticulous handling and preservation of the rectus femoris and the vastus muscle complex are critical determinants of postoperative extensor mechanism integrity and ambulatory capacity.
The epidemiology of femoral metastases is a direct reflection of the overall prevalence of systemic carcinomas. Five primary malignancies—breast, prostate, lung, renal cell, and thyroid carcinomas—account for approximately eighty percent of all skeletal metastases. It is imperative to recognize that the primary goal of orthopedic oncology in the metastatic setting is generally palliative, not curative. The surgical mandate focuses on immediate and durable pain relief, restoration of mechanical stability, and the facilitation of immediate full weight-bearing to maximize the patient's functional independence and remaining quality of life.
Pathophysiology of Bone Metastases
Tumor cells disseminate to the femur primarily via hematogenous routes, exploiting the slow venous flow within the red marrow sinusoids. Once lodged within the medullary cavity, these metastatic cells manipulate the local bone microenvironment. Osteolytic metastases, classic in breast, lung, and renal cell carcinomas, secrete cytokines and growth factors, most notably Parathyroid Hormone related Protein, Interleukin 6, and Tumor Necrosis Factor alpha. These factors stimulate osteoblasts to upregulate Receptor Activator of Nuclear Factor Kappa B Ligand. The binding of this ligand to its receptor on osteoclast precursors drives massive osteoclastogenesis and subsequent osteolytic destruction.
Conversely, osteoblastic or sclerotic metastases, most frequently observed in prostate cancer and certain breast cancer phenotypes, stimulate aberrant bone formation via the secretion of endothelin 1, bone morphogenetic proteins, and Wnt signaling pathway modulators. Regardless of the morphologic subtype, whether lytic, blastic, or mixed, the normal lamellar architecture of the femur is replaced by woven bone or tumor tissue, severely compromising structural integrity and necessitating rigorous biomechanical evaluation.
Oncologic Characteristics and Systemic Burden
The systemic burden of metastatic disease dictates the overall survival and directly influences surgical decision-making. Patients presenting with femoral metastases frequently possess concurrent visceral metastases, hypercalcemia of malignancy, and profound cancer-induced cachexia. The vicious cycle of bone metastasis not only destroys local osseous architecture but also releases sequestered transforming growth factor beta and insulin-like growth factors from the bone matrix, which in turn fuel further tumor proliferation.
Advancements in targeted immunotherapies, bisphosphonates, and RANKL inhibitors such as denosumab have significantly prolonged the life expectancy of patients with stage IV carcinomas. This epidemiological shift has resulted in a higher prevalence of patients living long enough to develop impending or actual pathologic fractures of the femur. Consequently, orthopedic surgeons must design reconstructions that outlive the patient, accounting for the fact that irradiated, tumor-laden bone possesses virtually no capacity for biological fracture healing or implant osteointegration.
Surgical Anatomy and Biomechanics
Osseous Architecture of the Proximal Femur
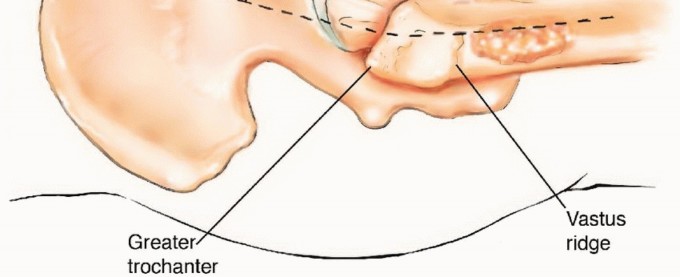
The proximal femur is an intricate biomechanical construct designed to transfer the entire weight of the axial skeleton to the lower extremity. The trabecular architecture is highly organized into distinct compressive and tensile systems. The principal compressive group extends from the superior femoral head down to the medial calcar, resisting the massive vertical loads of ambulation. The principal tensile group arcs from the inferior fovea across the femoral neck to the lateral cortex, countering the bending moments imparted by the abductor musculature.
Metastatic deposits frequently obliterate Ward's triangle, a naturally occurring area of sparse trabecular bone situated between these principal groups. When osteolysis disrupts the medial calcar, the femur loses its primary buttress against varus collapse. Conversely, destruction of the lateral cortex predisposes the femur to catastrophic tension failure. Understanding these distinct failure modalities is critical when selecting between cephalomedullary nailing and endoprosthetic reconstruction.
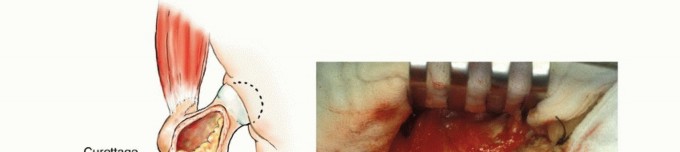
Musculotendinous Attachments and Extensor Mechanism
The functional outcomes following femoral reconstruction are inextricably linked to the preservation of the extensor mechanism, primarily the quadriceps femoris. The rectus femoris, possessing a direct head originating from the anterior inferior iliac spine and an indirect head from the superior acetabular rim, spans two joints and is crucial for dynamic hip flexion and knee extension. Deep to the rectus femoris lies the vastus intermedius, which envelopes the anterior and lateral aspects of the femoral shaft.
The vastus lateralis, the largest component of the quadriceps, originates from the greater trochanter and the lateral lip of the linea aspera. During surgical approaches to the femur, particularly the direct lateral or anterolateral approaches, the vastus lateralis must be meticulously managed. Indiscriminate splitting or devascularization of the vastus musculature leads to profound postoperative extensor lag, massive hematoma formation, and debilitating fibrosis. The orthopedic surgeon must prioritize subperiosteal elevation or precise internervous dissection to maintain the functional excursion of these muscle bellies.
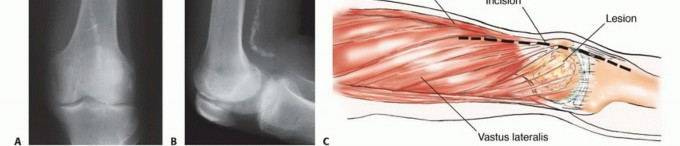
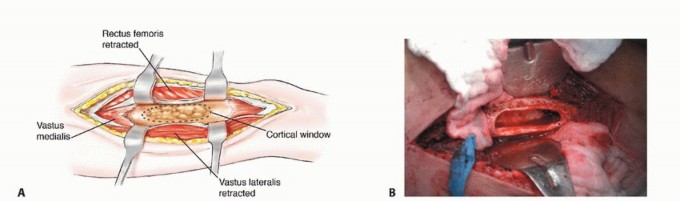
Biomechanical Forces and Structural Failure Risk
The femur is subjected to a complex array of forces including axial compression, bending moments, and torsional shear. During the single-leg stance phase of the gait cycle, the joint reaction force across the femoral head can exceed three to four times body weight. This force creates a massive bending moment across the subtrochanteric region, which is the zone of highest mechanical stress in the human skeleton.
When a metastatic lesion occupies more than fifty percent of the cortical diameter, the torsional strength of the femur is reduced by over seventy percent. The stress riser effect created by a lytic defect concentrates forces at the periphery of the tumor, making spiral or oblique fractures imminent under minimal physiological loads. Surgical implants must therefore bypass the zone of pathology by a minimum of two cortical diameters both proximally and distally to adequately neutralize these forces. In the setting of extensive diaphyseal involvement, full-length intramedullary devices are mandatory to protect the entire bone from subsequent metastatic deposits and mechanical failure.

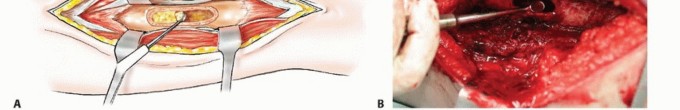
Indications and Contraindications
The decision to proceed with operative intervention in the setting of femoral metastases requires a multidisciplinary assessment involving orthopedic oncology, medical oncology, and radiation oncology. The primary objective is to differentiate between lesions that can be managed non-operatively with radiation and systemic agents versus those that require prophylactic stabilization or definitive resection.
Criteria for Prophylactic Fixation
Prophylactic fixation is indicated for impending pathologic fractures. The Mirels classification remains the most widely cited clinical tool for assessing fracture risk, evaluating four parameters: site of the lesion, nature of the lesion, size of the lesion, and pain characteristics. A Mirels score of nine or greater strongly indicates prophylactic fixation, while a score of eight represents a clinical gray area requiring individualized judgment.
Beyond the Mirels criteria, modern indications for prophylactic surgery include cortical destruction exceeding fifty percent of the bone circumference, an axial cortical lesion greater than three centimeters, or persistent mechanical pain despite appropriate radiotherapy. Prophylactic fixation is inherently superior to post-fracture stabilization, as it is associated with lower intraoperative blood loss, reduced operative time, shorter hospital stays, and significantly improved functional outcomes.
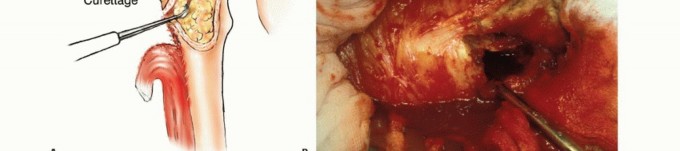
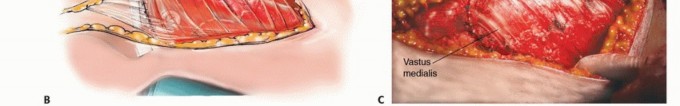
Criteria for Resection and Reconstruction
While intramedullary nailing is the workhorse for diaphyseal lesions, extensive destruction of the femoral head, neck, or intertrochanteric region frequently necessitates tumor resection and endoprosthetic reconstruction. Proximal femoral replacement is indicated when there is insufficient native bone stock to support internal fixation, massive osteolysis of the medial calcar, or failed previous osteosynthesis.
Additionally, solitary bone metastases from favorable primary histologies, such as renal cell carcinoma or breast carcinoma, may warrant wide en bloc resection to achieve local disease control and potentially improve overall survival. In these highly selected cases, the oncologic principles of margin-negative resection supersede the palliative goals of standard stabilization.

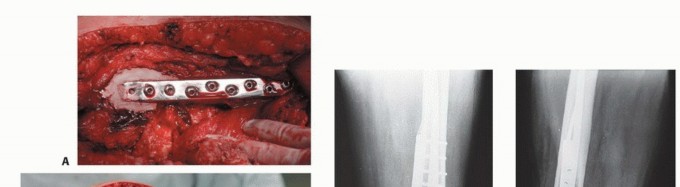
Absolute and Relative Contraindications
Surgical intervention is not universally appropriate. Absolute contraindications include patients with an estimated life expectancy of less than four to six weeks, as the physiological insult of major orthopedic surgery outweighs any potential palliative benefit. Severe, uncorrectable coagulopathy and profound cardiopulmonary instability are also absolute contraindications.
Relative contraindications include widespread, uncontrolled polymicrobial sepsis or localized active infection over the proposed surgical site. In patients with highly radiosensitive tumors, such as multiple myeloma or lymphoma, without an immediate biomechanical threat of fracture, radiation therapy combined with bracing may be trialed before committing to surgical fixation.
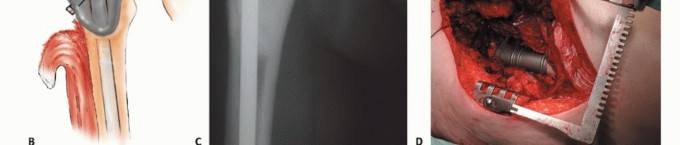
| Clinical Scenario | Operative Indication | Non-Operative Indication |
|---|---|---|
| Mirels Score | Score ≥ 9 (High fracture risk) | Score ≤ 7 (Low fracture risk) |
| Cortical Involvement | > 50% diameter destruction | < 50% diameter destruction |
| Pain Profile | Mechanical, weight-bearing pain | Biologic pain, responsive to RT |
| Life Expectancy | > 6 weeks (Ideally > 3 months) | < 4 to 6 weeks |
| Tumor Histology | Radioresistant (RCC, Thyroid, GI) | Radiosensitive (Myeloma, Lymphoma) |
| Fracture Status | Actual or impending fracture | Incidental finding, structurally sound |
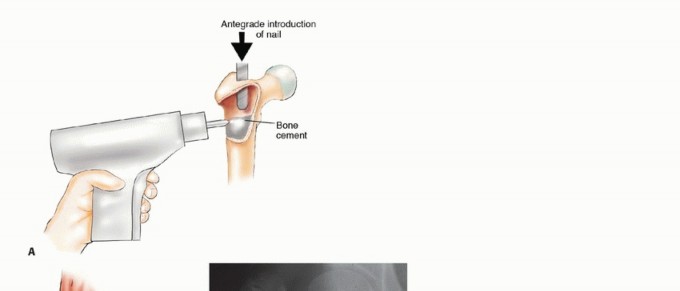
Pre Operative Planning and Patient Positioning
Advanced Imaging and Templating
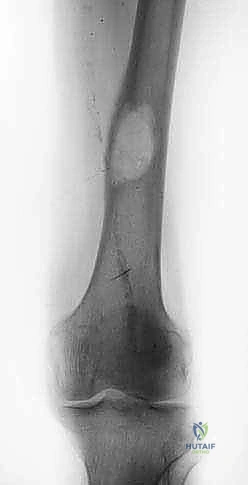
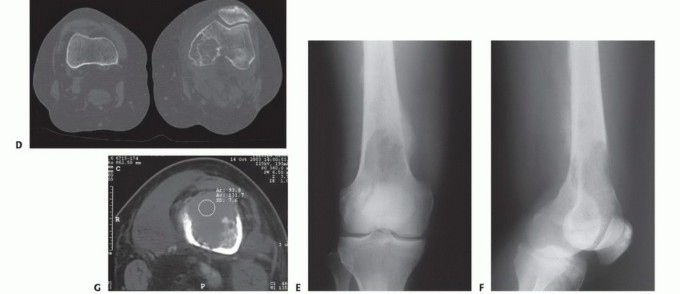
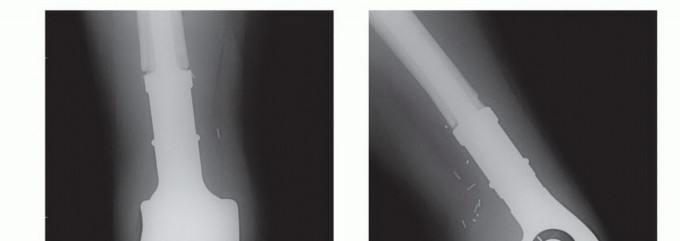
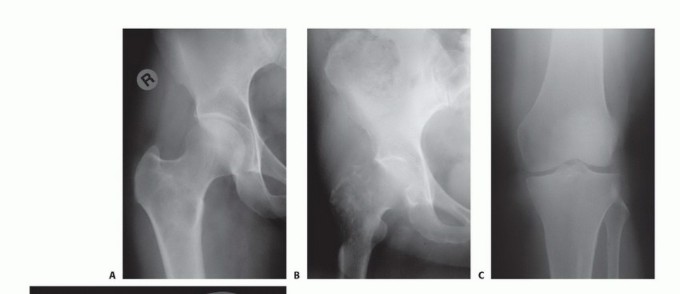
Meticulous preoperative planning is the cornerstone of successful oncologic reconstruction. Standard orthogonal radiographs of the entire femur are mandatory to assess the primary lesion and to rule out synchronous skip metastases within the diaphysis. Computed tomography provides superior resolution of cortical integrity, accurately quantifying the degree of osteolysis and identifying subtle infractions that may alter the surgical approach.
Magnetic resonance imaging of the entire femur is invaluable for delineating the extent of intramedullary tumor propagation and evaluating extracortical soft tissue extension. The T1-weighted sagittal and coronal sequences are particularly sensitive for identifying the border between tumor-infiltrated marrow and normal hematopoietic marrow.
For hypervascular tumors, specifically metastatic renal cell carcinoma and thyroid carcinoma, preoperative angiography and transarterial embolization within twenty-four to forty-eight hours of surgery are critical. Failure to embolize these lesions can result in catastrophic, life-threatening intraoperative hemorrhage during canal reaming or tumor curettage.
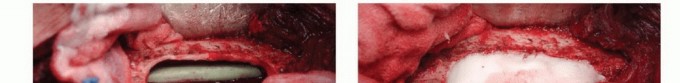
Patient Positioning and Operating Room Setup
Patient positioning dictates the ease of surgical exposure and the accuracy of implant trajectory. For intramedullary nailing of diaphyseal or subtrochanteric lesions, the patient is typically positioned supine on a radiolucent fracture table or a flat Jackson table. The flat table approach, utilizing manual traction, is increasingly preferred in the metastatic setting to avoid the massive torsional forces generated by traction boots, which can inadvertently cause iatrogenic fractures in osteoporotic or tumor-laden bone.
For proximal femoral replacements or extensive open curettage procedures, the lateral decubitus position is optimal. This position allows for an unhindered direct lateral or posterior approach to the hip, facilitating wide exposure of the proximal femur, acetabulum, and the entire vastus-rectus interval. The surgical field must be draped to allow for full manipulation of the extremity, and fluoroscopy must be positioned to easily obtain true anteroposterior and lateral projections of the entire femur without compromising the sterile field.
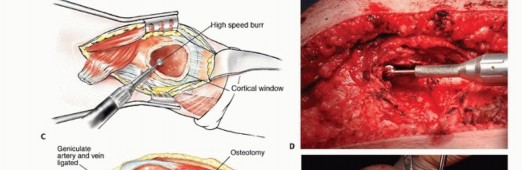
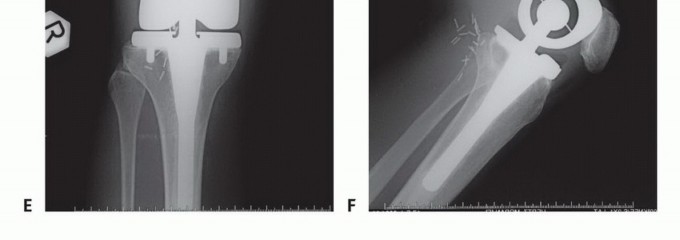
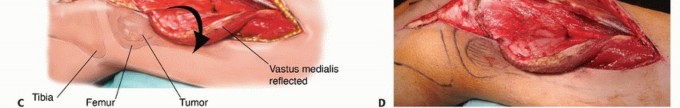
Detailed Surgical Approach and Technique
Anterolateral Approach and Internervous Planes
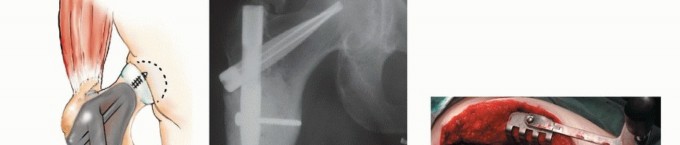
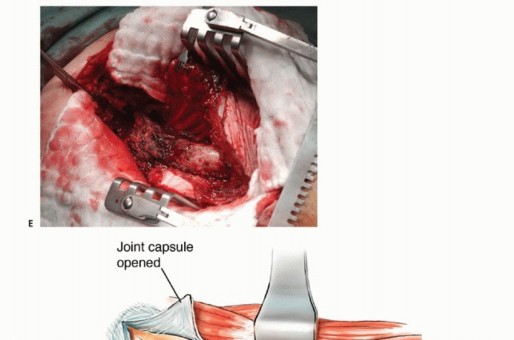
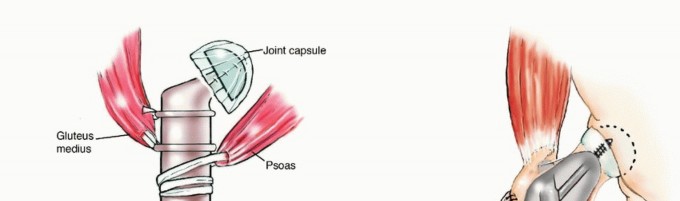
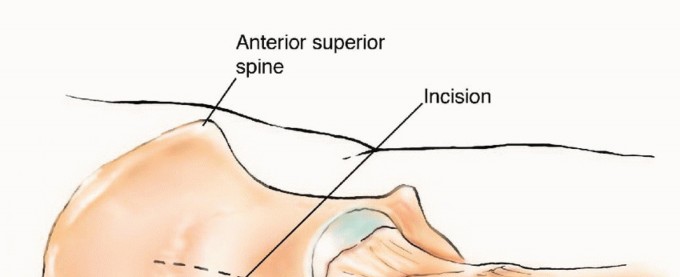
When open intervention is required for proximal femoral lesions, the anterolateral approach, or Watson-Jones approach, provides excellent exposure while capitalizing on a true internervous plane. The superficial dissection exploits the interval between the tensor fasciae latae, innervated by the superior gluteal nerve, and the sartorius, innervated by the femoral nerve.
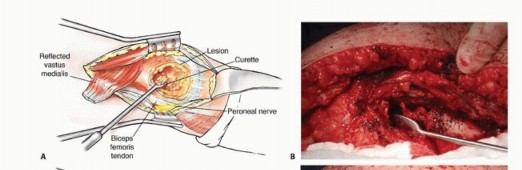
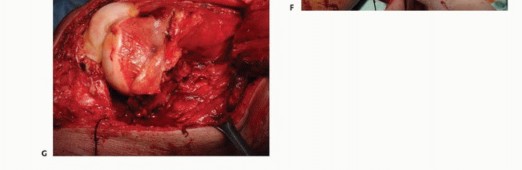
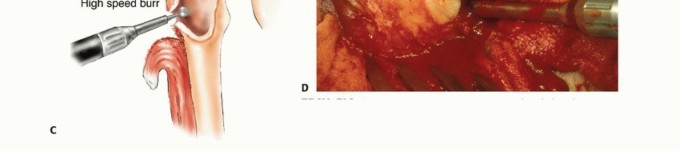
Deep dissection proceeds between the gluteus medius and the rectus femoris. Retracting the rectus femoris medially protects its structural integrity and neurovascular pedicle. The ascending branches of the lateral femoral circumflex artery are consistently encountered in this interval and must be systematically identified and ligated to prevent postoperative hematoma. This approach grants direct access to the anterior hip capsule, the femoral neck, and the intertrochanteric line, making it ideal for intralesional curettage or proximal femoral resections.
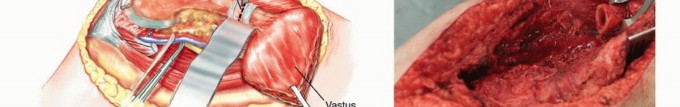
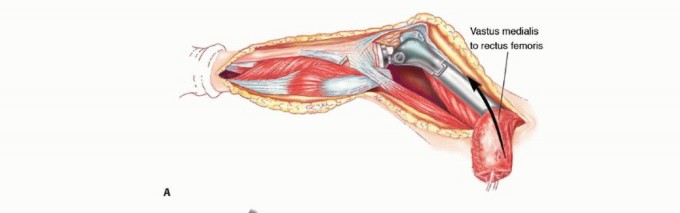
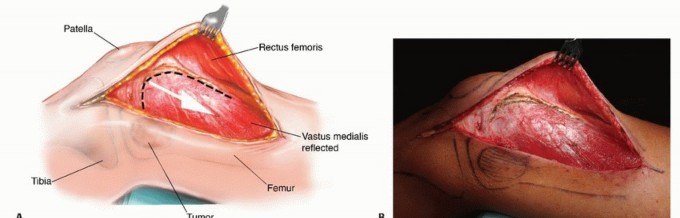
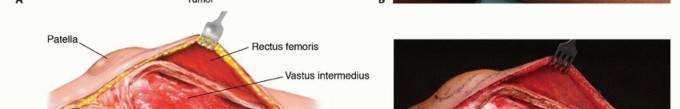
Management of the Rectus Femoris and Vastus Intermedius
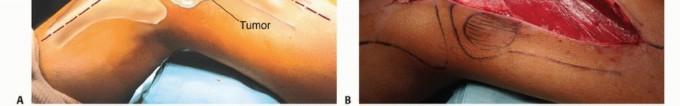
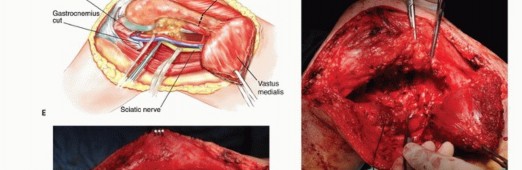
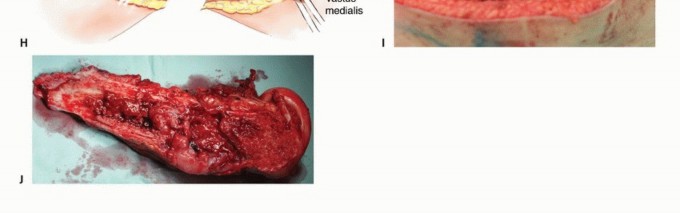
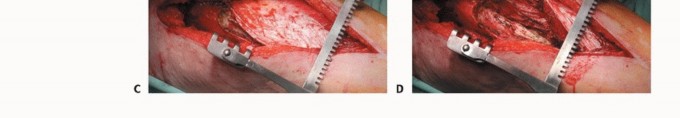
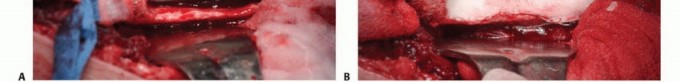
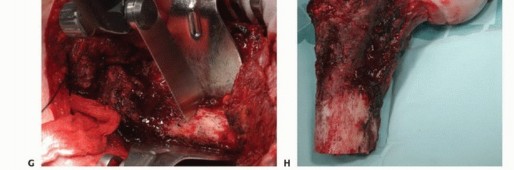
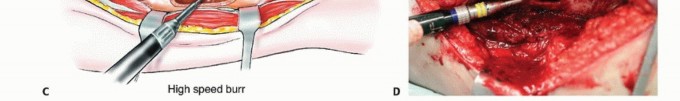
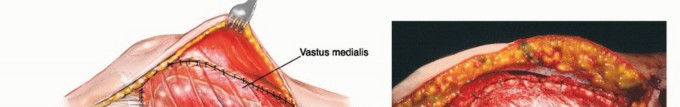
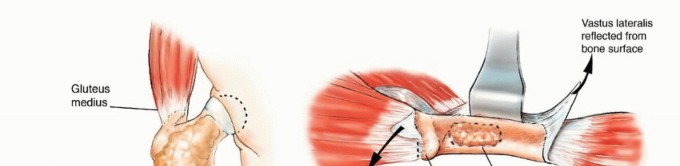
For extensive diaphyseal exposure, the direct lateral approach is frequently utilized. The iliotibial band is incised longitudinally. The critical step involves the management of the vastus lateralis and vastus intermedius. Rather than splitting the muscle belly of the vastus lateralis, which denervates the anterior portion and leads to significant hemorrhage, the muscle should be elevated subperiosteally from posterior to anterior along the linea aspera.
The perforating branches of the profunda femoris artery must be meticulously cauterized or ligated as they pierce the lateral intermuscular septum. By elevating the vastus lateralis and intermedius as a single continuous sleeve, the surgeon preserves the extensor mechanism's continuity. Upon closure, this muscular envelope is repaired back to the lateral intermuscular septum, ensuring that the rectus femoris and vastus complex retain their dynamic tension and gliding capability over the reconstructed femur.
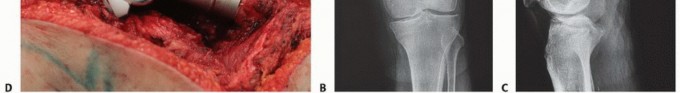








You Might Also Like