Masterclass: Open Reduction and Internal Fixation of Tibial Tuberosity Fractures
Key Takeaway
This masterclass guides fellows through open reduction and internal fixation of tibial tuberosity fractures. We cover essential anatomy, preoperative planning, precise intraoperative steps, instrument use, and critical decision-making. Learn to manage neurovascular risks, achieve anatomical reduction, and select appropriate hardware. We also discuss pearls, pitfalls, and comprehensive postoperative rehabilitation protocols for optimal patient outcomes.
Introduction and Epidemiology
Tibial tuberosity fractures represent a rare and unique subset of pediatric and adolescent orthopedic injuries, accounting for less than 3% of all epiphyseal fractures and approximately 1% of all pediatric fractures. These injuries predominantly occur in the later stages of skeletal growth, typically between the ages of 12 and 15 years, immediately preceding the physiological closure of the proximal tibial physis.
Demographically, tibial tuberosity avulsion fractures demonstrate a strong male predilection. While cases in females are documented, the overwhelming majority occur in adolescent boys. This discrepancy is largely attributed to the later onset of physeal closure in males combined with the higher baseline generation of quadriceps force during explosive athletic activities. The quintessential mechanism of injury involves jumping sports, with basketball and track and field being the most frequently cited activities.

A significant proportion of patients presenting with acute tibial tuberosity fractures possess a clinical or radiographic history of Osgood-Schlatter disease (tibial tuberosity apophysitis). The chronic traction apophysitis alters the structural integrity of the developing secondary ossification center, creating a localized stress riser. The microtrauma associated with Osgood-Schlatter disease leads to fibrocartilaginous proliferation and disorganized ossification, which ultimately weakens the apophyseal-epiphyseal junction, predisposing the adolescent athlete to an acute avulsion failure under maximal load.
Surgical Anatomy and Biomechanics
Developmental Stages of the Tibial Tubercle
Understanding the embryological and postnatal development of the tibial tubercle is paramount for accurate radiographic interpretation and surgical planning. The tubercle develops through four distinct histological and radiographic stages:
- Cartilaginous Stage: In early childhood, the tibial tubercle is composed entirely of hyaline cartilage before any secondary center of ossification forms.
- Apophyseal Stage: Occurring between ages 8 to 12 years in girls and 9 to 14 years in boys, a secondary center of ossification emerges within the distal portion of the cartilaginous anlage. During this phase, the apophysis is distinct and not yet osseously connected to the primary epiphysis of the proximal tibia.
- Epiphyseal Stage: The "tongue" of the apophysis coalesces with the epiphyseal bone, creating a continuous cartilaginous physis. This stage typically spans ages 10 to 15 years for girls and 11 to 17 years for boys. This transitional period is the most vulnerable window for avulsion injuries.
- Bony Stage: The physis undergoes complete physiological fusion, progressing from posterior to anterior and proximal to distal, ultimately resulting in a mature, solid bony continuum.

Extensor Mechanism Biomechanics
The patellar ligament inserts into the proximal portion of the tibial apophysis, with a broad, fan-like extension continuing distally into the anterior tibial periosteum. Anatomically, this insertion is slightly lateral to the mechanical midline of the tibia. Consequently, the avulsed fracture fragment is typically centered lateral to the midline and hinges medially. This lateral eccentricity dictates the surgical approach, as anterolateral visualization is often required to fully assess the fracture bed and any intra-articular extension.
Vascular Anatomy and Compartment Syndrome Risk
A critical anatomical relationship is the proximity of the anterior tibial recurrent artery. This vessel originates from the anterior tibial artery immediately after it passes through the interosseous membrane. It courses superiorly over the anterior surface of the lateral tibial condyle. In the event of a displaced tibial tuberosity fracture, the anterior tibial recurrent artery or its proximal branches can be lacerated by the sharp osseous fragments.

Following laceration, the artery frequently retracts into the tight fascial confines of the anterolateral compartment. Unrecognized arterial hemorrhage into this non-distensible space is the primary pathophysiological driver for acute anterior compartment syndrome, a devastating complication uniquely associated with this specific fracture pattern.
Pathogenesis of Failure
The primary mechanism of injury is a violent, eccentric contraction of the quadriceps muscle complex against a fixed, planted foot. The force generated by the adolescent quadriceps can exceed the tensile strength of the maturing epiphyseal-apophyseal junction and its surrounding periosteal sleeve. A secondary mechanism involves sudden, forceful passive flexion of the knee while the quadriceps is maximally contracted, such as a gymnast landing short on a dismount. Patients sustaining these fractures frequently demonstrate quadriceps hypertrophy and strength profiles that exceed those of their age-matched peers.
Indications and Contraindications
The decision algorithm for managing tibial tuberosity fractures hinges on the degree of displacement, the integrity of the extensor mechanism, and the presence of intra-articular extension. The Ogden classification heavily influences the treatment paradigm.

| Variable | Operative Management | Non Operative Management |
|---|---|---|
| Fracture Displacement | > 2 mm displacement of the fracture fragment | < 2 mm displacement (minimally displaced) |
| Extensor Mechanism | Inability to actively extend the knee against gravity | Intact active straight leg raise |
| Articular Involvement | Ogden Type III (intra-articular extension) | Ogden Type I or II (extra-articular) |
| Soft Tissue Status | Impending or acute compartment syndrome | Benign soft tissue envelope |
| Associated Injuries | Concomitant meniscal tear or ligamentous avulsion | Isolated injury |
| Patient Factors | High-demand athlete requiring anatomical restoration | Low-demand patient or medical comorbidities precluding surgery |
Contraindications to immediate open reduction and internal fixation (ORIF) include active local soft tissue infection, severe medical instability, or massive soft tissue compromise (e.g., severe blistering) that precludes a safe surgical incision. In the setting of acute compartment syndrome, emergent fasciotomy supersedes fracture fixation, though simultaneous fixation is typically performed during the fasciotomy procedure.
Pre Operative Planning and Patient Positioning
Clinical Evaluation
The patient typically presents with acute, severe pain, marked swelling over the anterior proximal tibia, and an inability to bear weight. Differentiating this acute event from a flare of Osgood-Schlatter disease relies on the suddenness of symptom onset and the profound loss of function.
Physical examination reveals a prominent, tender mass over the tibial tubercle. In displaced fractures (Ogden Types II, III, and IV), the patient will exhibit an extensor lag or a complete inability to perform an active straight leg raise. Patella alta may be palpable or visible due to the proximal migration of the avulsed fragment.
A meticulous neurovascular examination is mandatory. The surgeon must maintain a high index of suspicion for anterior compartment syndrome. Pain out of proportion to the injury, pain with passive stretch of the extensor hallucis longus (EHL) or tibialis anterior, and tense anterior compartments necessitate immediate intra-compartmental pressure monitoring or emergent surgical release.

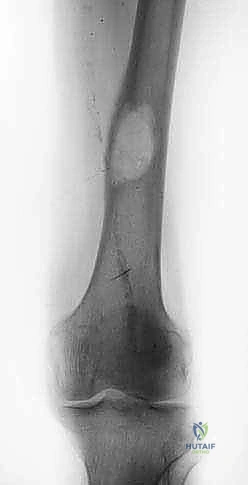
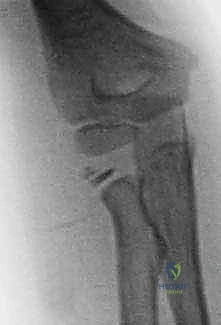
Radiographic Evaluation and Classification
Standard anteroposterior (AP) and lateral radiographs of the knee are the initial diagnostic modalities. The lateral radiograph is the most critical view for assessing the degree of proximal migration and the specific fracture pattern. If the fracture is non-displaced or subtle, bilateral comparison radiographs can differentiate an acute fracture from a fragmented, un-fused apophysis secondary to Osgood-Schlatter disease.
The Ogden classification, a modification of the Watson-Jones system, dictates the morphological description:
* Type I: Fracture propagates transversely through the apophysis, distal to the epiphyseal-apophyseal junction.
* Type II: Fracture propagates proximally, exiting between the primary epiphysis and the apophysis.
* Type III: Fracture propagates proximally through the primary epiphysis, entering the anterior articular surface of the knee joint.
* Type IV (Ryu and Debenham): Avulsion of the entire proximal tibial epiphysis along with the tuberosity.
* Type V (McKoy and Stanitski): A "Y" type fracture with both anterior and posterior intra-articular extension.

Advanced imaging is frequently indicated. Computed Tomography (CT) is highly recommended for all Ogden Type III fractures to precisely define the articular step-off and assist in preoperative screw trajectory planning. Magnetic Resonance Imaging (MRI) is utilized if concomitant soft tissue injuries (meniscal tears, anterior cruciate ligament avulsions, or quadriceps tendon ruptures) are suspected, which are reported in up to 10% of cases.
Patient Positioning and Setup
The patient is positioned supine on a radiolucent operating table. A small bump is placed under the ipsilateral hip to correct natural external rotation, bringing the patella and tibial tubercle facing directly anterior. A non-sterile pneumatic tourniquet is applied to the proximal thigh.
The contralateral limb is secured, and the fluoroscopy unit (C-arm) is positioned on the contralateral side, draped sterilely, and brought in perpendicular to the operative field. The surgeon must ensure that perfect AP and lateral fluoroscopic images can be obtained without obstruction before prepping and draping. Prophylactic intravenous antibiotics are administered prior to tourniquet inflation.
Detailed Surgical Approach and Technique
Incision and Superficial Dissection
Surgical access is achieved via a longitudinal anterior midline or slightly anterolateral incision. The incision typically begins at the inferior pole of the patella and extends distally over the tibial tubercle to approximately 2-3 cm distal to the fracture site.

Careful subcutaneous dissection is performed. The surgeon must be vigilant to identify and protect the infrapatellar branch of the saphenous nerve, which typically crosses the proximal tibia from medial to lateral. Retraction of this nerve minimizes the risk of postoperative anterior knee numbness or painful neuroma formation.
Deep Dissection and Fracture Exposure
The deep fascia is incised in line with the skin incision. The fracture hematoma is encountered immediately and must be thoroughly irrigated and evacuated. At this stage, the surgeon must inspect the anterolateral muscular interval for any active arterial bleeding from the anterior tibial recurrent artery. If bleeding is identified, it must be meticulously cauterized or ligated to prevent postoperative compartment syndrome.
The avulsed tibial tubercle fragment is typically retracted proximally by the resting tone of the quadriceps. The periosteum is frequently torn extensively on the medial and lateral aspects of the tubercle. This periosteal sleeve must be carefully elevated and preserved, as a robust periosteal repair is critical for the final biomechanical construct.

Joint Inspection and Management of Articular Extension
For Ogden Type III fractures, direct visualization of the articular surface is mandatory. This can be achieved through a limited submeniscal arthrotomy or via concurrent knee arthroscopy. The anterior horns of the medial and lateral menisci must be probed. In cases where the fracture line extends through the meniscal attachments, the meniscus may be incarcerated within the fracture site. Any interposed meniscal tissue must be extricated to allow for anatomical reduction of the articular block. Concomitant meniscal tears should be repaired using standard inside-out or all-inside techniques prior to definitive fracture fixation.
Fracture Reduction Techniques
The fracture bed on the proximal tibia is debrided of interposed organized hematoma, periosteum, and loose cartilaginous debris using a curette or a Freer elevator.
Reduction is achieved by extending the knee to relax the extensor mechanism. A towel clip or a pointed reduction clamp is placed with one tine on the proximal aspect of the avulsed fragment (or the distal patellar tendon insertion) and the other tine on the intact tibial shaft distal to the fracture. Distal traction is applied to pull the fragment into its anatomical bed.

Because the patellar tendon inserts slightly lateral to the midline, the fragment tends to rotate. The surgeon must ensure rotational alignment is perfectly restored. Temporary provisional fixation is achieved using two 1.6 mm or 2.0 mm Kirschner wires (K-wires) driven from anterior to posterior. Fluoroscopy is utilized to confirm anatomical reduction on both AP and lateral planes. For Ogden Type III fractures, articular congruity must be perfectly restored with zero step-off.
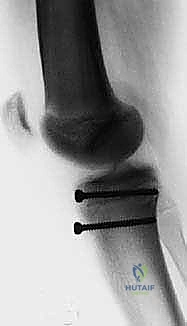
Internal Fixation Strategy
Definitive fixation is most commonly achieved using cannulated cancellous screws. The choice between 4.0 mm, 4.5 mm, or 5.0 mm screws depends on the size of the patient and the fragment.
Guide pins for the cannulated screws are placed over the provisional K-wires. The trajectory of the screws is critical. They should be directed from anterior to posterior, and slightly proximal to distal, perpendicular to the fracture plane. In patients nearing skeletal maturity, traversing the closing physis with the screws is acceptable and necessary for stable fixation.

Typically, two screws are utilized to control rotational forces. The screws can be partially threaded to achieve interfragmentary compression. Washers may be utilized if the anterior cortex of the avulsed fragment is comminuted or soft, preventing the screw head from penetrating the cortical shell.
In cases of severe comminution or purely tendinous avulsions (sleeve fractures), suture anchors or a transosseous suture technique using heavy non-absorbable sutures (#2 or #5) may be required to augment the osseous fixation. A tension band wiring construct is rarely indicated in the modern era due to hardware prominence but remains a salvage option for highly comminuted fragments.

Soft Tissue and Periosteal Repair
Following rigid osseous fixation, the torn medial and lateral retinaculum and the robust anterior periosteal sleeve must be meticulously repaired. This step is not merely cosmetic; it significantly reinforces the fixation construct against the massive tensile forces of the quadriceps. Absorbable sutures (e.g., #1 or 0 Vicryl) are used in an interrupted fashion to close the periosteal envelope over the hardware. The tourniquet is deflated prior to skin closure to ensure meticulous hemostasis, again mitigating the risk of postoperative compartment syndrome.
Complications and Management
Despite generally favorable outcomes following ORIF, tibial tuberosity fractures carry a unique profile of potential complications. Anticipation and early recognition are vital for joint preservation and limb salvage.

| Complication | Incidence | Etiology / Risk Factors | Salvage Strategy |
|---|---|---|---|
| Anterior Compartment Syndrome | 2% - 5% | Laceration of anterior tibial recurrent artery; failure to evacuate hematoma. | Emergent four-compartment lower leg fasciotomy. Delayed wound closure and skin grafting. |
| Genu Recurvatum | Rare (< 2%) | Premature localized arrest of the anterior proximal tibial physis with continued posterior growth. | Proximal tibial opening wedge osteotomy to correct sagittal plane deformity once skeletal maturity is reached. |
| Prominent Hardware / Bursitis | 30% - 50% | Subcutaneous nature of the anterior tibia; use of large screw heads or washers. | Elective hardware removal after radiographic union (typically 6-12 months post-op). |
| Loss of Reduction / Extensor Lag | < 5% | Patient non-compliance with weight-bearing restrictions; inadequate initial fixation. | Revision ORIF with augmented fixation (suture anchors, tension band) and prolonged immobilization. |
| Nonunion / Malunion | < 1% | Poor biological environment; unrecognized interposition of periosteum. | Debridement, autologous bone grafting, and rigid revision internal fixation. |
| Knee Stiffness / Arthrofibrosis | 5% - 10% | Prolonged postoperative immobilization; lack of early guided physical therapy. | Aggressive physical therapy; arthroscopic lysis of adhesions and manipulation under anesthesia if refractory. |
Focus on Compartment Syndrome
The most devastating acute complication is anterior compartment syndrome. The fascial boundaries of the anterior compartment are rigid. If the anterior tibial recurrent artery bleeds into this space, intracompartmental pressures rapidly exceed capillary perfusion pressure, leading to muscle and nerve ischemia. Surgeons must never apply a circumferential cast in the acute postoperative setting. If compartment syndrome develops, emergent fasciotomy is the only definitive treatment; failure to perform this within the ischemic window (typically 6 hours) results in irreversible muscle necrosis, foot drop, and severe permanent disability.
Post Operative Rehabilitation Protocols
The postoperative rehabilitation protocol must balance the need to protect the fixation construct against the massive forces of the quadriceps with the goal of preventing arthrofibrosis and restoring normal joint kinematics.
Phase 1: Maximum Protection (Weeks 0 to 4)
Immediately postoperatively, the limb is placed in a hinged knee brace locked in full extension.
* Weight Bearing: The patient is typically restricted to toe-touch weight-bearing (TTWB) or non-weight-bearing (NWB) with crutches.
* Range of Motion (ROM): Active extension is strictly prohibited to prevent tension on the repair. Passive range of motion (PROM) may be initiated early (0-30 degrees) depending on the absolute rigidity of the fixation, though many surgeons prefer to maintain strict extension for the first 2-3 weeks, particularly in highly comminuted patterns.
* Strengthening: Isometric quadriceps sets and straight leg raises (in the locked brace) are initiated to prevent profound muscle atrophy.
Phase 2: Controlled Mobilization (Weeks 4 to 8)
Radiographs are obtained at 4 weeks to confirm maintenance of reduction and early callus formation.
* Weight Bearing: Progression to weight-bearing as tolerated (WBAT) with the brace locked in extension.
* Range of Motion: The brace is unlocked to allow progressive active-assisted and passive flexion. The goal is to achieve 90 degrees of flexion by week 6 and full flexion by week 8.
* Strengthening: Active extension is gradually introduced, focusing on terminal extension control. Closed kinetic chain exercises (e.g., mini-squats, leg presses) are initiated with light resistance.
Phase 3: Strengthening and Return to Sport (Weeks 8 to 16+)
Once clinical and radiographic union is achieved (typically 8-12 weeks), the brace is discontinued.
* Strengthening: Aggressive open and closed kinetic chain quadriceps strengthening. Eccentric loading is introduced cautiously.
* Return to Sport: Clearance for explosive jumping sports requires full, painless ROM, radiographic union, and isokinetic quadriceps strength that is at least 90% of the contralateral, uninjured limb. This typically occurs between 4 and 6 months postoperatively.
Summary of Key Literature and Guidelines
The academic foundation for the management of tibial tuberosity fractures is built upon several seminal works.
Ogden (1980) revolutionized the understanding of these injuries by correlating the fracture patterns with the histological stages of apophyseal development. His classification system (Types I, II, and III) remains the universal language for describing these fractures and directly guides the operative threshold based on articular extension.
Ryu and Debenham (1985) and later McKoy and Stanitski (2003) expanded the classification to include Type IV (avulsion of the entire proximal epiphysis) and Type V (biplanar intra-articular fractures), respectively. These additions highlight the complex, high-energy variants that require extensive preoperative planning and advanced imaging.
Recent literature, including comprehensive reviews by Sink et al., emphasizes the critical, under-recognized risk of anterior compartment syndrome. Modern guidelines strongly advocate for meticulous hemostasis of the anterior tibial recurrent artery, avoidance of acute circumferential casting, and a low threshold for intracompartmental pressure monitoring.
Furthermore, contemporary surgical guidelines mandate the use of preoperative CT scanning for all Ogden Type III fractures to quantify articular step-off, and recommend concurrent arthroscopy or arthrotomy to address the high incidence (up to 10%) of concomitant meniscal incarcerations or tears, ensuring a comprehensive restoration of joint mechanics.
Clinical & Radiographic Imaging












You Might Also Like