Masterclass: Precision Syme and Boyd Amputations for Congenital Fibular Deficiency
Key Takeaway
This masterclass guides fellows through Syme and Boyd amputations for congenital fibular deficiency. We cover comprehensive anatomy, meticulous preoperative planning, and granular intraoperative execution, emphasizing critical steps like heel pad preservation and neurovascular protection. Learn to manage unique challenges, prevent complications, and optimize functional outcomes for these complex pediatric limb salvage procedures.
Introduction and Epidemiology
Fibular deficiency, historically referred to as fibular hemimelia or paraxial longitudinal deficiency of the fibula, represents the most common congenital long bone deficiency. The condition is characterized by a partial or complete absence of the fibula, but the nomenclature "fibular deficiency" is preferred as it more accurately reflects the pan-limb nature of the dysplasia. The embryological insult occurs between the fourth and seventh weeks of gestation, likely secondary to an anomaly in the apical ectodermal ridge or the zone of polarizing activity, leading to a cascade of developmental failures along the postaxial border of the lower limb.

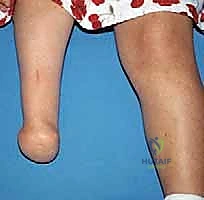
Epidemiologically, fibular deficiency occurs in approximately 1 in 40,000 live births. It is typically sporadic, though rare familial cases with autosomal dominant inheritance patterns have been reported, occasionally associated with broader genetic syndromes. The clinical presentation exists on a wide spectrum, ranging from mild limb length discrepancy with a completely stable, plantigrade foot to severe shortening with complete absence of the fibula, an unstable ankle, and severe equinovalgus deformity with absent lateral rays.

The Achterman and Kalamchi classification is widely utilized to categorize the severity of the deficiency. Type I represents a hypoplastic fibula, further subdivided into Type IA (proximal fibular epiphysis is distal to the tibial physis, and distal fibular epiphysis is proximal to the distal tibial physis) and Type IB (partial absence of the fibula, typically the proximal half). Type II represents complete absence of the fibula and is the most common presentation.

The primary dilemma in managing fibular deficiency revolves around the decision between limb lengthening and early amputation. A critical tenet of pediatric orthopedic surgery is that delayed amputation should be avoided whenever possible. The consensus dictates that if amputation is indicated, it should ideally be performed between 10 and 18 months of age. This timing coincides with the child’s natural neuromotor development as they begin to pull to a stand. Performing the amputation at this stage facilitates rapid psychosocial adjustment, seamless integration of the prosthesis into the child's body schema, and optimal motor skill acquisition. A common pitfall among consulting physicians and parents is the reluctance to commit to a definitive path, leading to the ill-advised strategy of attempting lengthening with amputation as a fallback. This approach severely compromises the child's psychosocial development and subjects them to unnecessary surgical morbidity.
Surgical Anatomy and Biomechanics
Fibular deficiency is not an isolated osseous anomaly; it is a complex, multi-segmental limb deformity. The extent of the fibular absence does not reliably correlate with the severity of the overall limb length inequality or the functional capacity of the foot. Surgical decision-making requires a comprehensive understanding of the pathoanatomy affecting the entire lower extremity.

Proximal to the primary defect, the femur frequently exhibits mild to moderate shortening, femoral retroversion, and lateral femoral condyle hypoplasia. The knee joint is often dysplastic, characterized by cruciate ligament deficiency (frequently an absent anterior cruciate ligament), valgus alignment, and patellofemoral instability. The tibia is universally shortened and typically presents with a characteristic anteromedial diaphyseal bow, often marked by a cutaneous dimple at the apex of the deformity.

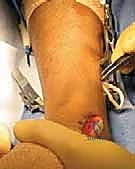
At the level of the ankle and foot, the structural anomalies dictate the feasibility of limb salvage. The ankle typically demonstrates severe valgus secondary to the absent lateral malleolus, and the tibiotalar articulation often assumes a ball-and-socket configuration. The foot frequently exhibits tarsal coalitions, absence of one or more lateral rays, and a rigid equinovalgus posture.

Understanding the vascular and neural anatomy of the hindfoot is paramount for both Syme and Boyd amputations. The viability of the heel pad—the critical weight-bearing structure in these procedures—depends entirely on the posterior tibial neurovascular bundle. The posterior tibial artery and nerve course posterior to the medial malleolus before bifurcating into the medial and lateral plantar branches. In fibular deficiency, vascular anomalies are common, including the hypoplasia or absence of the anterior tibial artery, making the limb heavily reliant on the posterior tibial or peroneal vessels. Strict protection of the posterior tibial bundle during the medial dissection is non-negotiable to maintain heel pad perfusion and sensation.

Biomechanically, the Syme and Boyd amputations offer distinct advantages over standard transtibial (below-knee) amputations. The Syme amputation is an ankle disarticulation that preserves the heel pad, anchoring it to the distal tibia. This provides a robust, end-bearing stump that allows for energy-efficient ambulation and the ability to bear weight over short distances without a prosthesis (e.g., walking to the bathroom at night). Furthermore, by preserving the distal tibial articular cartilage (or the entire distal tibial physis in children), the Syme procedure effectively prevents terminal bony overgrowth, a common and problematic complication in pediatric diaphyseal amputations.
The Boyd amputation modifies the ankle disarticulation by preserving the calcaneus (or a portion thereof) and fusing it to the distal tibia. This tibiocalcaneal arthrodesis creates a rigid, bony block that definitively prevents posterior or lateral migration of the heel pad—a known complication of the Syme procedure. The Boyd amputation provides exceptional end-bearing capacity and maintains slightly more limb length, though the technical execution of the arthrodesis in a dysplastic limb can be demanding.
Indications and Contraindications
The decision matrix for treating fibular deficiency relies heavily on the predicted leg length discrepancy (LLD) at skeletal maturity and the functional status of the foot. The predicted LLD can be calculated using the Paley multiplier method or the Green-Anderson growth remaining charts.

Amputation (Syme or Boyd) is definitively indicated when the predicted LLD exceeds 30% of the contralateral limb length, or when the foot is severely dysplastic, rigid, and nonfunctional (e.g., severe equinovalgus, less than three rays). In these scenarios, achieving a plantigrade, functional foot through reconstruction is highly improbable, and the magnitude of lengthening required would necessitate multiple, high-morbidity procedures with a high risk of failure and joint contracture.
Conversely, limb lengthening and reconstruction are indicated for patients with a predicted LLD of less than 10%, a stable ankle joint, and a functional, plantigrade foot.
The most challenging clinical scenarios fall within the "gray zone" of 10% to 30% predicted LLD. In this cohort, both amputation and multiple lengthenings have demonstrated excellent functional outcomes in the literature. Care must be highly individualized, taking into account the family's psychosocial support system, access to specialized orthopedic and prosthetic care, and the specific anatomical nuances of the knee and ankle stability.

| Clinical Parameter | Indications for Amputation (Syme/Boyd) | Indications for Limb Lengthening |
|---|---|---|
| Predicted LLD at Maturity | > 30% | < 10% (10-30% is individualized) |
| Foot Function | Nonfunctional, rigid, severe ray deficiency | Functional, plantigrade, > 3 rays |
| Ankle Stability | Unstable, severe valgus, absent lateral support | Stable, mild/correctable valgus |
| Knee Status | Severe instability or contracture | Stable, functional ROM |
| Psychosocial Factors | Preference for definitive, single-stage surgery | Strong family support for multiple surgeries |
| Vascular Anatomy | Adequate posterior tibial perfusion to heel pad | Adequate perfusion for distraction osteogenesis |
Contraindications for Syme or Boyd amputations include inadequate perfusion to the heel pad, rendering it non-viable for weight-bearing. Additionally, severe proximal deformities (e.g., proximal focal femoral deficiency) that would preclude the fitting of a standard prosthesis may necessitate alternative surgical strategies, such as rotationplasty or more proximal amputations.
Pre Operative Planning and Patient Positioning
Preoperative planning begins with a meticulous clinical examination, assessing the entire kinetic chain from the hip to the toes. Range of motion of the hip and knee, the presence of fixed contractures, and the stability of the knee ligaments must be documented. The foot must be evaluated for flexibility, ray count, and vascular status.

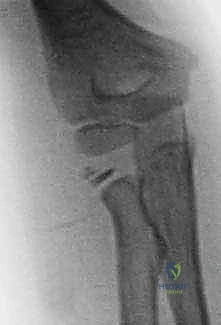
Radiographic evaluation requires weight-bearing anteroposterior and lateral radiographs of the entire lower extremity, ideally using a long-leg cassette. A scanogram or orthoroentgenogram is utilized to accurately measure the current segment lengths to calculate the predicted LLD at skeletal maturity. Advanced imaging, such as MRI, is rarely necessary unless there is a specific concern regarding tethered cord or concurrent spinal anomalies, which can occasionally present with lower extremity dysplasia.

Vascular assessment is critical. Palpation of pulses may be insufficient in the dysplastic limb. Doppler ultrasound should be routinely employed to confirm the presence and robust flow of the posterior tibial artery, as the viability of the Syme or Boyd flap depends entirely on this vessel. If the posterior tibial artery is absent or severely hypoplastic, a standard Syme or Boyd amputation may be contraindicated, and a transtibial amputation utilizing alternative flap designs may be required.

Patient positioning is supine on a standard radiolucent operating table to allow for intraoperative fluoroscopy, which is particularly crucial during the Boyd amputation for assessing the tibiocalcaneal arthrodesis and hardware placement. A bump is placed under the ipsilateral hip to correct the external rotation posture commonly associated with fibular deficiency, ensuring the patella is pointing directly toward the ceiling. A pneumatic tourniquet is applied to the proximal thigh to provide a bloodless surgical field, facilitating meticulous dissection of the neurovascular structures.

Detailed Surgical Approach and Technique
The Syme Amputation Technique
The Syme amputation relies on the meticulous subperiosteal excision of the talus and calcaneus while preserving the integrity of the heel pad and its neurovascular supply.

Incision: The classic fish-mouth incision is utilized. The anterior limb of the incision begins slightly distal to the tip of the medial malleolus, courses straight across the anterior aspect of the ankle joint, and terminates at the tip of the lateral malleolus (or the equivalent anatomical landmark if the fibula is absent). The plantar limb connects these two points, passing vertically across the plantar aspect of the heel. It is critical that the plantar incision is angled slightly anteriorly to ensure an adequate volume of heel pad is captured in the flap.

Dissection and Capsulotomy: The anterior incision is deepened through the subcutaneous tissue to the extensor retinaculum. The anterior tibial neurovascular bundle is identified, ligated, and divided. The extensor tendons are transected under tension so they retract proximally. An anterior capsulotomy of the ankle joint is performed, and the medial and lateral collateral ligaments are divided from inside the joint to allow plantarflexion of the talus.

Talocalcaneal Excision: As the talus is plantarflexed, a bone hook can be placed into the talar dome to provide traction. The posterior capsule is divided. The most critical and technically demanding step is the subperiosteal dissection of the calcaneus from the heel pad. This must be performed staying strictly on the bone. Straying into the subcutaneous fat of the heel pad will disrupt the fibrous septa that provide structural integrity and, more importantly, risk transecting the terminal branches of the posterior tibial artery, leading to flap necrosis.

The Achilles tendon is identified at its insertion on the calcaneal tuberosity. It is carefully dissected and divided close to the bone. In children, preserving the cartilaginous apophysis of the calcaneus within the heel pad can provide additional volume and cushioning.

Malleolar Modification and Flap Stabilization: Once the foot is removed, the distal tibia is addressed. In adults, the malleoli are resected flush with the tibial plafond to create a broad, flat weight-bearing surface. In pediatric patients with fibular deficiency, the distal tibial physis and the articular cartilage must be preserved to maintain longitudinal growth and prevent terminal overgrowth. The medial malleolus (and lateral, if present) is shaved down just enough to reduce bulbousness without violating the physis.

The posterior tibial nerve is identified, dissected proximally, placed under tension, and transected sharply so that it retracts deep into the muscular compartment, minimizing the risk of a symptomatic neuroma. The heel pad is then folded anteriorly over the distal tibia. To prevent the notorious complication of heel pad migration, the pad must be secured. This is achieved by drilling small holes through the anterior cortex of the distal tibia and suturing the deep fascia of the heel pad directly to the bone.
The Boyd Amputation Technique
The Boyd amputation is technically more demanding due to the requirement of achieving a solid arthrodesis between the calcaneus and the distal tibia, but it provides superior resistance to heel pad migration.

Incision and Initial Dissection: The incision is identical to the Syme amputation. The anterior dissection, ligation of the anterior neurovascular bundle, and division of the extensor tendons proceed similarly.

Talectomy and Calcaneal Preparation: An anterior capsulotomy is performed, and the talus is excised completely. Unlike the Syme, the calcaneus is left within the heel pad. The superior articular surface of the calcaneus is resected using an oscillating saw to create a flat, bleeding cancellous bone surface. In very young children, aggressive resection may damage the calcaneal apophysis; therefore, sharp decortication of the articular cartilage with a scalpel or curette is preferred to expose the subchondral bone while preserving the cartilaginous anlage.

Tibial Preparation and Arthrodesis: The articular cartilage of the distal tibia is similarly decorticated. The calcaneus is then translated anteriorly so that its denuded superior surface opposes the distal tibia. This anterior translation is crucial to align the weight-bearing axis of the tibia directly over the center of the heel pad.
Fixation is typically achieved using two smooth Steinmann pins or heavy Kirschner wires. These can be driven retrograde from the plantar aspect of the heel, through the calcaneus, and into the distal tibia. Intraoperative fluoroscopy is mandatory to confirm appropriate alignment, anterior translation of the calcaneus, and secure hardware placement. The posterior tibial nerve is handled exactly as in the Syme procedure. The wound is closed in layers over a closed suction drain.
Complications and Management
While both Syme and Boyd amputations provide excellent functional outcomes when executed correctly, they are associated with specific complications that require meticulous surgical technique to avoid.

Heel Pad Migration: This is the most common and problematic complication of the Syme amputation. The heel pad typically migrates posteriorly and laterally due to the unopposed pull of the residual Achilles tendon fibers or inadequate initial osseous fixation. When the pad migrates, the distal tibia bears weight on thin, non-glabrous skin, leading to ulceration and pain. Management requires surgical revision to mobilize the heel pad and re-anchor it to the distal tibia, often requiring more robust transosseous sutures or even transition to a Boyd-style arthrodesis if sufficient calcaneal bone is available.
Terminal Bony Overgrowth: This phenomenon is characterized by appositional bone growth at the distal end of the transected diaphysis, resulting in a spiked osseous prominence that pierces the overlying skin. It is highly prevalent in pediatric transtibial amputations but is effectively prevented by the Syme and Boyd techniques, provided the distal tibial physis and cartilage cap are preserved. If overgrowth occurs (usually due to iatrogenic damage to the physis), management involves stump revision, resection of the overgrowth, and capping of the medullary canal (e.g., using an osteochondral graft or synthetic cap).
Wound Dehiscence and Flap Necrosis: This catastrophic complication is almost always secondary to technical error during the subperiosteal dissection of the calcaneus, resulting in damage to the posterior tibial artery. If superficial, it may heal by secondary intention. If full-thickness necrosis occurs, the end-bearing concept is lost, and the patient will require revision to a higher, transtibial amputation level.

Nonunion (Boyd Amputation): Failure of the tibiocalcaneal arthrodesis can lead to a painful, unstable stump. Risk factors include inadequate decortication of the articular surfaces, insufficient anterior translation of the calcaneus, or early hardware failure. Management requires revision arthrodesis with autologous bone grafting and rigid internal fixation.
| Complication | Estimated Incidence | Etiology / Risk Factors | Salvage Strategy |
|---|---|---|---|
| Heel Pad Migration | 10-15% (Syme) | Inadequate fixation, Achilles pull | Revision stabilization, transosseous anchoring |
| Terminal Overgrowth | < 5% (Syme/Boyd) | Damage to distal tibial physis/cartilage | Osseous resection, medullary capping |
| Flap Necrosis | 2-5% | Injury to posterior tibial artery | Debridement, revision to transtibial amputation |
| Symptomatic Neuroma | 5-10% | Inadequate proximal retraction of PT nerve | Excision of neuroma, proximal transposition |
| Nonunion | 5-10% (Boyd) | Inadequate decortication, poor fixation | Revision arthrodesis with bone graft |
Post Operative Rehabilitation Protocols
The immediate postoperative management focuses on wound healing, edema control, and protection of the surgical site. In the operating room, a rigid compressive dressing or a well-padded short leg cast is applied.

For a Syme amputation, the patient is kept strictly non-weight-bearing for the first 3 to 4 weeks to allow the soft tissues to heal and the heel pad to adhere to the distal tibia. Once the incision is fully healed, progressive weight-bearing in a cast or a preparatory prosthesis can begin.
For a Boyd amputation, the non-weight-bearing period is extended to protect the tibiocalcaneal arthrodesis. Patients are typically immobilized in a cast and kept non-weight-bearing for 6 to 8 weeks. Radiographic confirmation of osseous union is required before initiating weight-bearing. The percutaneous pins are usually removed in the clinic at the 4- to 6-week mark.
Prosthetic fitting is a critical phase of rehabilitation. The initial prosthesis is often a "stubby" or a simple preparatory socket that allows the child to begin standing and walking. The definitive Syme or Boyd prosthesis is highly specialized. It typically features a patellar tendon-bearing design combined with distal end-bearing capabilities. Because the Syme/Boyd stump is bulbous distally, the prosthesis often requires an expandable inner socket or a medial window to allow the stump to pass through the narrow shank. Physical therapy is essential to train the child in gait mechanics, balance, and prosthetic management. Given the optimal timing of the surgery (10-18 months), children typically adapt to the prosthesis seamlessly, incorporating it as a natural extension of their limb.
Summary of Key Literature and Guidelines
The foundational literature supporting the use of
Clinical & Radiographic Imaging


























You Might Also Like