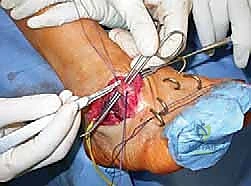
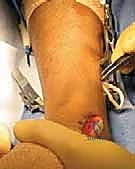
Masterclass: Percutaneous & Intramedullary Reduction for Pediatric Radial Neck Fractures
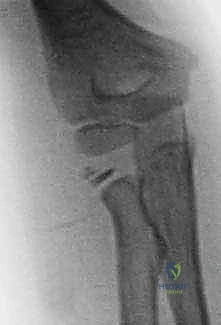
Key Takeaway
Welcome, fellows, to an in-depth masterclass on managing pediatric radial neck fractures using percutaneous joystick and intramedullary Metaizeau techniques. We'll meticulously cover comprehensive anatomy, precise preoperative planning, and granular intraoperative execution. This session emphasizes critical decision-making, neurovascular protection, and advanced reduction maneuvers to achieve optimal outcomes and prevent complications in these challenging injuries.
Introduction and Epidemiology
Radial neck fractures in the pediatric population present a unique biomechanical and therapeutic challenge for the orthopedic surgeon. These injuries typically manifest as transphyseal fractures, predominantly Salter-Harris type II injuries, although Salter-Harris type I fractures are also frequently observed. Unlike adult radial head fractures, pediatric injuries seldom involve the epiphysis (radial head) directly due to the robust cartilaginous envelope protecting the secondary center of ossification. In older children approaching skeletal maturity, the fracture pattern may transition to an entirely metaphyseal location.
Epidemiologically, radial neck fractures represent approximately 14% of all pediatric elbow fractures, with a peak incidence occurring between the ages of 9 and 10 years. The natural history of minimally displaced fractures is generally favorable, but the management of significantly displaced fractures is fraught with complications if not handled with precise surgical technique.
Pathogenesis and Injury Mechanisms
The most common mechanism of injury involves a fall on an outstretched hand (FOOSH) with the elbow in full extension and the forearm in supination. This position locks the radiocapitellar joint, and the resultant axial and valgus forces compress the capitellum directly against the lateral margin of the radial head. This valgus impaction creates a predictable pattern of lateral or posterolateral angulation of the proximal fragment.
Furthermore, radial neck fractures frequently occur in association with other traumatic elbow pathology. A classic associated injury is the posterior dislocation of the elbow. A posteriorly displaced radial neck fracture can occur either during the spontaneous reduction of a posterior elbow dislocation or, iatrogenically, during the manipulative reduction of an unrecognized dislocation. During the reduction maneuver, if the elbow is flexed prematurely, the distal humerus (specifically the lateral condyle) may strike the radial head, effectively knocking it posteriorly off the radial metaphysis.







Surgical Anatomy and Biomechanics
A thorough understanding of the osteology, vascularity, and neuroanatomy of the proximal radius is critical to the safe execution of percutaneous and intramedullary reduction techniques.
Osteology and Ossification
The proximal radial epiphysis (radial head) is entirely cartilaginous at birth. Ossification typically commences by 4 years of age, at which point the radial head and neck begin to assume their definitive adult morphology. The proximal radial physis contributes relatively little to the overall longitudinal growth of the radius (approximately 20-25%), which mitigates the clinical impact of premature physeal closure following trauma. Physeal closure occurs at approximately 14 years of age in females and 17 years of age in males.
Vascular Anatomy of the Proximal Radius
The vascular supply to the proximal radius is tenuous and highly susceptible to iatrogenic disruption. The radial head receives its blood supply primarily from intra-articular vessels that traverse the joint capsule and enter the non-articular portions of the radial head and neck. There is negligible cross-physeal blood flow. Because the vessels run along the periosteum of the radial neck before penetrating the epiphysis, significant displacement of the fracture—or aggressive open surgical dissection—can easily strip these vessels, precipitating avascular necrosis (AVN) of the radial head. This anatomic reality strongly underpins the modern preference for closed, percutaneous, or intramedullary reduction techniques over open reduction.
Neurologic Considerations
The radial nerve and its terminal branches dictate the safe zones for percutaneous pin placement. At the level of the radiocapitellar joint, the radial nerve bifurcates into the superficial radial nerve and the posterior interosseous nerve (PIN). The PIN enters the substance of the supinator muscle at the arcade of Frohse and winds around the anterolateral aspect of the radial neck.
The relationship between the PIN and the radial neck is dynamic and highly dependent on forearm rotation. Supination brings the PIN closer to the anterolateral aspect of the radial neck, placing it at high risk during lateral percutaneous wire insertion. Conversely, pronation of the forearm moves the PIN more medially and anteriorly, safely away from the anterolateral side of the radial neck. Therefore, all lateral percutaneous joystick maneuvers must be performed with the forearm in maximal pronation to avoid devastating iatrogenic PIN palsy.







Indications and Contraindications
The management algorithm for pediatric radial neck fractures is dictated by the degree of angulation, the amount of translation, and the presence of any mechanical block to forearm rotation. The natural history of minimally displaced fractures is excellent, as remodeling potential in the sagittal and coronal planes is robust in young children.
The upper limit of acceptable angulation remains somewhat controversial and is inversely proportional to the patient's age. Generally, angulation of less than 30 degrees is unlikely to cause a clinically significant loss of pronation or supination and can be managed non-operatively. In children under 10 years of age, some authors accept up to 45 degrees of angulation, relying on the remodeling potential of the proximal radial physis. Translation greater than 2 to 3 millimeters typically requires reduction.
Judet Classification System
The Judet classification is frequently utilized to guide treatment:
* Type I: Non-displaced fractures.
* Type II: Angulation less than 30 degrees.
* Type III: Angulation between 30 and 60 degrees.
* Type IV: Angulation greater than 60 degrees or complete translation.
| Clinical Scenario | Operative Indications | Non-Operative Indications |
|---|---|---|
| Angulation | > 30-45 degrees (age-dependent) | < 30 degrees |
| Translation | > 3 mm translation | < 2-3 mm translation |
| Range of Motion | Mechanical block to pronation/supination | Full, unrestricted rotation (examined under anesthesia if needed) |
| Associated Injuries | Polytrauma, floating elbow, compartment syndrome | Isolated injury without neurovascular compromise |
| Judet Classification | Type III, Type IV | Type I, Type II |
Contraindications to percutaneous or intramedullary techniques include active local infection, established nonunion, or fractures presenting late (typically >7-10 days) where early callus formation precludes closed or percutaneous manipulation.







Pre Operative Planning and Patient Positioning
Meticulous preoperative planning and optimal operating room setup are fundamental to the success of percutaneous and intramedullary techniques.
Imaging Protocols
Standard anteroposterior (AP) and lateral radiographs of the elbow are mandatory. Because the radial neck is often obscured by the proximal ulna on standard views, a radiocapitellar (Greenspan) view can be highly beneficial. This view is obtained with the patient's arm in neutral rotation and the X-ray beam angled 45 degrees cephalad, projecting the radial head free of the coronoid process. Contralateral elbow radiographs should be obtained to establish the patient's baseline proximal radial anatomy and physeal appearance.
Operating Room Setup
The patient is positioned supine on the operating table. A radiolucent arm board or hand table is utilized. General anesthesia is required to ensure complete muscle relaxation, which is critical for closed reduction maneuvers. A sterile tourniquet is applied to the proximal arm but is often not inflated unless an open reduction becomes necessary, as the percutaneous techniques involve minimal blood loss.
The C-arm fluoroscope is brought in parallel or perpendicular to the arm board, depending on surgeon preference and room configuration. The monitor must be placed directly in the surgeon's line of sight. The ability to obtain true AP, lateral, and oblique views seamlessly without moving the fracture is essential.







Detailed Surgical Approach and Technique
The surgical management of displaced radial neck fractures follows a stepwise escalation of invasiveness: closed reduction, percutaneous joystick reduction, intramedullary (Metaizeau) reduction, and, only as a last resort, open reduction.
Closed Reduction Techniques
Before proceeding to percutaneous methods, a closed reduction maneuver (the Patterson technique) should be attempted. The elbow is extended, and a varus stress is applied to open the lateral radiocapitellar joint space. The surgeon applies direct digital pressure over the displaced radial head while simultaneously pronating and supinating the forearm. If fluoroscopy confirms acceptable alignment (<30 degrees angulation), the elbow is immobilized, and no hardware is required. If closed reduction fails, percutaneous or intramedullary techniques are indicated.
Percutaneous Joystick Technique
The percutaneous joystick technique utilizes a Kirschner wire (K-wire) as a lever to manipulate the proximal fragment.
- Preparation and Pronation: The forearm is placed in maximal pronation to draw the posterior interosseous nerve (PIN) medially and anteriorly, protecting it from the lateral entry point.
- Wire Insertion: Under fluoroscopic guidance, a 1.5 mm or 2.0 mm K-wire is inserted percutaneously from the lateral aspect of the elbow. The wire is driven into the displaced radial head fragment. Care must be taken not to penetrate the articular surface or to advance the wire so far that it exits the medial cortex, which would tether the fragment.
- Joystick Maneuver: Once secure purchase in the radial head is achieved, the K-wire is used as a joystick. The surgeon levers the radial head distally and medially to correct the valgus and posterior displacement, aligning it with the radial shaft.
- Metaphyseal Push: Alternatively, a second K-wire or a freer elevator introduced through a stab incision can be used to push the radial metaphysis laterally to meet the head.
- Fixation: Once reduced, the fracture can be stabilized by advancing the joystick wire across the fracture site into the medial cortex of the radial shaft. Alternatively, a separate transcapitellar wire can be used for temporary fixation, though this is generally avoided due to the risk of intra-articular wire breakage.
Intramedullary Reduction Metaizeau Technique
Described by Metaizeau in 1993, the retrograde intramedullary technique is considered the gold standard for displaced radial neck fractures that fail closed reduction. It avoids the PIN entirely and preserves the delicate extraosseous blood supply to the radial head.
- Entry Point Preparation: A 1-2 cm longitudinal incision is made over the lateral aspect of the distal radius, approximately 2-3 cm proximal to the radiocarpal joint, avoiding the superficial radial nerve.
- Cortical Window: The periosteum is incised, and a small cortical window is created using an awl or a drill bit. The entry angle should be oblique to facilitate passage of the wire up the medullary canal.
- Wire Selection and Bending: A titanium elastic nail (TEN) or a smooth K-wire (typically 1.5 mm to 2.0 mm, depending on the canal diameter) is selected. The distal 5-10 mm of the wire is pre-bent to an angle of 15 to 30 degrees.
- Retrograde Passage: The wire is mounted on a T-handle or power drill and advanced retrograde up the radial shaft under fluoroscopic guidance.
- Crossing the Fracture: As the wire reaches the fracture site, the bend is oriented to point toward the displaced radial head. The wire is carefully advanced across the fracture site and driven into the subchondral bone of the radial head.
- The Reduction Maneuver: Once the tip of the wire is firmly seated in the radial head, the entire wire is rotated 180 degrees around its longitudinal axis. The pre-bent tip sweeps the radial head from its displaced, angulated position back into anatomic alignment with the radial shaft.
- Final Seating and Cutting: The reduction is confirmed on orthogonal fluoroscopic views. The wire is then tapped further into the subchondral bone to secure the reduction. The distal end of the wire is cut and either buried beneath the skin or left protruding slightly for easy removal in the clinic.







Complications and Management
The management of pediatric radial neck fractures carries a high risk of complications, particularly if open reduction is performed. The surgeon must be prepared to identify and manage these issues promptly.
Avascular Necrosis (AVN)
AVN of the radial head is the most devastating complication, characterized by sclerosis, fragmentation, and eventual collapse of the epiphysis. It results from the disruption of the tenuous retrograde blood supply. The incidence is exponentially higher following open reduction (up to 70% in some historical series) compared to closed or percutaneous techniques. Management is largely conservative, focusing on maintaining range of motion, as revascularization can occur over several years. Radial head excision is absolutely contraindicated in the growing child due to resultant proximal radial migration and severe cubitus valgus.
Premature Physeal Closure
Premature closure of the proximal radial physis is common, occurring in up to 30% of cases. However, because the proximal physis contributes only a small percentage to the overall length of the radius, this complication is rarely clinically significant unless it occurs in a very young child, which may lead to a positive ulnar variance.
Neurologic Injury
Injury to the posterior interosseous nerve (PIN) is a well-documented risk of the percutaneous joystick technique and open approaches. It
Clinical & Radiographic Imaging






















































You Might Also Like