Full Question & Answer Text (for Search Engines)
Question 1:
A 28-year-old woman complains of pain and numbness in her lower legs bilaterally for approximately 2 months following strenuous moving of furniture. She now states that she has not voided in the past 48 hours and that her abdomen area is markedly distended. What diagnostic test must be performed in order to support the suspected diagnosis:
Options:
- Voiding cystourethrogram
- Magnetic resonance imaging of the lumbosacral spine
- Posteroanterior and lateral plain radiographs of the lumbar spine
- Spinal puncture to rule out infection
- Electromyography of the lower extremities
Correct Answer: Magnetic resonance imaging of the lumbosacral spine
Explanation:
Based on history and physical examination, the suspected diagnosis is cauda equina syndrome. This potential surgical emergency requires immediate spinal imaging. A magnetic resonance imaging of the lumbosacral spine is the most appropriate test.
Question 2:
On physical examination, the umbilicus is a superficial landmark for the bifurcation of the aorta into the common iliac arteries and overlies this disk space:
Options:
- L1/L2
- L2/L3
- L3/L4
- L4/L5
- L5/S1
Correct Answer: L3/L4
Explanation:
The umbilicus is a superficial landmark that often lies over the anterior L3/L4 disk space, which is the location of the aortic bifurcation into the common iliac arteries. Below this arterial division, in lean individuals, one can palpate the anterior bodies of L4, L5, and S1.
Question 3:
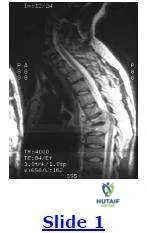
A 35-year-old woman has been complaining of severe unrelenting mid to low back pain for the past 5 months. Conservative management, consisting of bed rest and nonsteroidal anti-inflammatory drugs (NSAIDs), has not decreased the intensity of her symptoms. She immigrated to the United States from Vietnam 6 months ago. Based on the sagittal magnetic resonance image below, the next step in her management is:
Options:
- Antibiotics with gram-positive coverage
- Surgical decompression and reconstruction
- Biopsy of the lesion to obtain a specimen for pathology
- C ontinued conservative management and observation
- Physical therapy for low back strengthening
Correct Answer: Biopsy of the lesion to obtain a specimen for pathology
Explanation:
It is prudent to determine the underlying etiology of this lesion. Tuberculous spondylitis is increasing in frequency and must be suspected in people who emigrate from countries where tuberculosis is endemic. A biopsy of the region must be obtained in order to make the diagnosis of tuberculosis accurately or any other infectious and noninfectious causative agent in order to determine proper management.
Question 4:
What is the most common sequence of steps performed during a midline open disectomy in the treatment and excision of a herniated posterolateral lumbar disk:
Options:
- The paraspinal musculature is stripped from the lamina of the vertebra, the ligamentum flavum is excised, portions of the superior and inferior lamina are removed, the nerve root and dural sac is retracted, and the disk herniation is excised.
- The ligamentum flavum is excised, the paraspinal musculature is stripped from the lamina of the vertebra, portions of the superior and inferior lamina are removed, the nerve root and dural sac is retracted, and the disk herniation is excised.
- The ligamentum flavum is excised, the paraspinal musculature is stripped from the lamina of the vertebra, the nerve root and dural sac is retracted, portions of the superior and inferior lamina are removed, and the disk herniation is excised.
- The paraspinal musculature is stripped from the lamina of the vertebra, the disk herniation is excised, the ligamentum flavum is excised, the nerve root and dural sac is retracted, and portions of the superior and inferior lamina are removed.
- Ligamentum flavum is excised, the disk herniation is excised the paraspinal musculature is stripped from the lamina of the vertebra, the nerve root and dural sac is retracted, and portions of the superior and inferior lamina are removed.
Correct Answer: The paraspinal musculature is stripped from the lamina of the vertebra, the ligamentum flavum is excised, portions of the superior and inferior lamina are removed, the nerve root and dural sac is retracted, and the disk herniation is excised.
Explanation:
The traditional surgery for the excision of a herniated posterolateral lumbar disk is by means of a midline incision. This procedure is then performed in a stepwise fashion: The paraspinal musculature is stripped from the lamina of the vertebra; the ligamentum flavum is then excised; portions of the superior and inferior lamina are removed; and the nerve root and dural sac are identified and carefully retracted. This is followed by excision of the herniated disk material and wound closure.
Question 5:
On physical examination, a patient with a weak extensor hallucis longus muscle might be expected to have a far-lateral disk herniation at what level in the spine:
Options:
- L2/L3
- L3/L4
- L4/L5
- L5/S1
- S1/S2
Correct Answer: L5/S1
Explanation:
A far-lateral disk herniation in the lumbar spine often compromises the more proximal, or exiting, nerve root and not the more distal, or traversing, nerve root most typically affected in a posterolateral disk herniation. Therefore, a far-lateral disk herniation at the L5 - S1 level could irritate the L5 nerve root, which would affect the extensor hallucis longus muscle.
Question 6:
One traditional surgery performed for the treatment of a symptomatic posterolateral lumbar disk herniation is a partial laminectomy and lumbar disk excision by means of a midline incision. What is the long-term (>2 years) success rate for relief of both leg and low back pain, respectively:
Options:
- 80% and 93%
- 93% and 80%
- 93% for both
- 80% for both
- 55% and 65%
Correct Answer: 93% and 80%
Explanation:
The success rate following a partial laminectomy and lumbar disk excision for a posterolateral herniated disk for relief of both leg and low back pain is predictable at 93% and 80%, respectively.
Question 7:
A 38-year-old man injured his neck and spinal cord 6 months ago as a result of a motorcycle accident. He is now a C 6 quadriplegic. He wants to know how his sexual function will be affected by his condition. The patient should be informed that:
Options:
- He should be able to obtain normal erections and ejaculation function.
- No erections or ejaculation function will exist.
- With external stimulation, a reflex erection is possible but normal ejaculation is not.
- Normal erections and ejaculations with low sperm counts are possible.
- He has a low probability of being sterile because precise control of thermal regulation of the testes is usually retained.
Correct Answer: With external stimulation, a reflex erection is possible but normal ejaculation is not.
Explanation:
With this type of spinal cord injury, it is possible to have an erection with external stimulation; however, ejaculation would have to be facilitated by electrical stimulation or vibratory means.
Question 8:
When testing the range of motion in the lumbar spine, which maneuver involves stretching of the interspinous and supraspinous ligaments, ligamentum flavum, and posterior longitudinal ligament while relaxing the anterior longitudinal ligament:
Options:
- Flexion
- Extension
- Lateral bending
- Lateral bending
- None of the above
Correct Answer: Flexion
Explanation:
Flexion of the lumbar spine creates stretching or tension of the posterior spinal structures including the interspinous and supraspinous ligaments, ligamentum flavum, and posterior longitudinal ligament. Flexion also allows relaxation of the anterior longitudinal ligament. This is often elicited by having a patient bend forward in attempt to touch the floor with the fingertips. If the patient cannot touch the floor, the distance from the floor to fingertips is measured in fingerbreadths or inches.
Question 9:
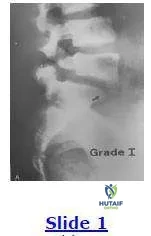
A 22-year-old woman sustained an injury to her low back 1 year ago while playing rugby. She now complains of excruciating low back pain with numbness and tingling into her left buttock. This pain is affecting her daily living activities. The patient underwent 6 months of conservative management consisting of restriction of activities, physical therapy, and anti- inflammatory medication with little relief. Based on the image below, the next appropriate step in the management of this patient is:
Options:
- C ontinued conservative management
- Posterolateral fusion at the L5/S1 level with bone graft
- Laminectomy at the L2/L3 level
- Laminectomy at the L3/L4 level
- Diskectomy at the L3/L4 level
Correct Answer: Posterolateral fusion at the L5/S1 level with bone graft
Explanation:
The patient has an L5/S1 spondylysis with a grade 1 spondylolisthesis. This patient has undergone a sufficient attempt at conservative management with continued unrelenting low back pain. The next most appropriate step in the management of this condition is a posterolateral fusion at the L5/S1 level with autologous bone graft.
Question 10:
When performing a neurological examination, if a surgeon has a patient resist thigh adduction against resistance, the surgeon is testing which nerve(s):
Options:
- Segmental nerves from T1-L1
- Femoral nerve
- Obturator nerve
- Sciatic nerve
- Segmental nerves from L5-S1
Correct Answer: Obturator nerve
Explanation:
The obturator nerve innervates most of the hip adductor group, which consists of neurologic levels L2, L3, and L4.
Question 11:
A 72-year-old man comes to the office complaining of low back and thigh pain that has been progressively getting worse over the years. The pain now bothers him during weather changes. The patient tells you that his pain is worse with standing and walking for long periods. However, leaning forward and sitting alleviates his discomfort. The patient denies any bladder or bowel complaints. This patient most likely has:
Options:
- A herniated lumbar disk
- Cauda equina syndrome
- Lumbar spinal stenosis
- Spinal cord tumor
- Vascular insufficiency
Correct Answer: Lumbar spinal stenosis
Explanation:
This patient is presenting with the hallmark symptoms of lumbar spinal stenosis, which consists of increased back and thigh pain with walking or standing with relief of the symptoms by leaning forward or sitting down. This patient denies any bladder or bowel dysfunction that makes cauda equina syndrome unlikely. Although urinary dysfunction is uncommon in spinal stenosis, it can occur in approximately 3% to 4% of cases.
Question 12:
A positive straight-leg raise sign:
Options:
- Occurs when the obturator nerve is stretched
- Is always associated with a history of trauma or injury
- Is important in predicting a successful outcome if surgery is performed to excise the herniated fragment
- Is a specific test to detect a lumbar disk herniation
- Is not sensitive in detecting a lumbar disk herniation
Correct Answer: Is important in predicting a successful outcome if surgery is performed to excise the herniated fragment
Explanation:
A positive straight-leg raise sign occurs when the sciatic nerve is placed under tension or is stretched reproducing a radiculopathy. It is also suggestive of inflammation around the nerve root, hence it is a good predictor of the successful relief of symptoms from surgical decompression. Additionally, a positive straight-leg raise sign is a relatively sensitive test for detecting a lumbar disk herniation, but it is not specific. Because the sign is not specific, it does not necessarily correspond to trauma or injury.
Question 13:
What physical examination maneuvers listed below check the status of the L4 neurologic level:
Options:
- Sensation on the lateral side of the ankle, the patellar tendon reflex, and plantar eversion
- Sensation on the lateral side of the ankle, the patellar tendon reflex, and plantar inversion
- Sensation on the lateral side of the ankle, the Achilles tendon reflex, and plantar inversion
- Sensation on the medial side of the ankle, the Achilles tendon reflex, and plantar inversion
- Sensation on the medial side of the ankle, the patellar tendon reflex, and plantar inversion
Correct Answer: Sensation on the lateral side of the ankle, the patellar tendon reflex, and plantar eversion
Explanation:
Sensation on the medial side of the ankle, the patellar tendon reflex, and plantar inversion are associated with the L4 neurologic level. Sensation on the lateral side of the ankle and the Achilles tendon reflex are associated with the S1 neurologic level.
Question 14:
In describing idiopathic scoliosis, there are several terms given to curve patterns on radiographs to describe the specific type of spinal deformity present. Which term best describes an area of the spine with a lateral curve that lacks normal flexibility noted radiographically by its failure to demonstrate segmental mobility or correction on supine side-bending radiographs:
Options:
- Primary curve
- C ompensatory curve
- Major curve
- Minor curve
- Structural curve
Correct Answer: Structural curve
Explanation:
The above question is describing a structural (nonflexible) curve. A primary curve is the earliest of several curves that may eventually develop. The term major curve is used to designate the largest structural curve. The minor curve refers to the smallest structural curve and is usually more flexible than the major curve. The compensatory curve is located above or below a major curve to attempt to maintain normal body alignment.
Question 15:
When performing a physical examination, if running the pointed edge of a reflex hammer along the crest of a patient's tibia causes extension of the great toe while the remaining toes splay or plantarflex, this finding would indicate:
Options:
- A Babinski reflex is present
- A Babinski reflex is absent
- A Positive Oppenheim test
- A Negative Oppenheim test
- None of the above
Correct Answer: A Positive Oppenheim test
Explanation:
An Oppenheim test is considered positive when running a pointed object along a patient's tibial crest elicits splaying or plantarflexion of the smaller toes with great toe extension. An Oppenheim test is considered negative when this reaction is not present. A Babinski reflex is present when running a pointed object across the plantar surface of a patient's foot elicits splaying or plantarflexion of the toes with extension of the great toe. A Babinski reflex is considered absent when the toes either do not move or all five toes flex and/or bunch up in response to the stimulus.
Question 16:
When trying to distinguish hamstring tightness/discomfort from sciatic pain/radiculopathy, surgeons can perform a straight-leg raise test on the affected side until the point at which the patient develops discomfort. This is followed by slightly lowering the affected extremity. While holding the patient's leg in this position, what maneuver could be performed in order to help reproduce true sciatic pain:
Options:
- Rotate the patient's foot medially 10°
- Rotate the patient's foot laterally 10°
- Plantarflex the patient's foot
- Dorsiflex the patient's foot
- Perform a Babinski test
Correct Answer: Dorsiflex the patient's foot
Explanation:
Dorsiflexion of the foot, known as Braggard test, adds additional tension or stretch to the sciatic nerve and may help reproduce the sciatic pain/radiculopathy.
Question 17:
Beevor sign is a physical examination maneuver that tests the integrity of the rectus abdominus muscles that are segmentally innervated by the anterior primary divisions of the T5-T12/L1 nerve roots. When performing this test, the patient is asked to perform a partial sit-up. A positive Beevor sign is indicated by:
Options:
- Pain in the abdominal musculature
- Simultaneous raising both lower extremities
- The absence of any deviation of the umbilicus
- The presence of umbilical deviation
- Pain radiating down both lower extremities
Correct Answer: The presence of umbilical deviation
Explanation:
When performing a sit-up, umbilical deviation due to abnormal contraction of the rectus musculature indicates either a partial or complete loss of segmental innervation to a portion of the rectus abdominus and/or paraspinal musculature. It is frequently seen in patients with certain neurological disorders such as meningomyelocele and poliomyelitis.
Question 18:
Which anatomic structure(s) may be the cause of referred pain to the lumbar spine region:
Options:
- The hip
- The rectum
- The pelvis
- Both the hip and the pelvis
- The hip, the pelvis, and the rectum
Correct Answer: The hip
Explanation:
The hip, rectum, and pelvis may refer pain to the lumbar spine region. In order to perform a complete physical examination, a rectal exam is recommended on all patients with pain in the lumbar spine region.
Question 19:
The following nonoperative treatments have not been proven effective in the early acute stage (2 weeks to 3 months) of low back pain:
Options:
- Nonsteroidal anti-inflammatory drugs
- Bed rest
- Anesthetic/corticosteriod injections into the epidural space
- Intrathecal anesthetic/corticosteriod injections
- Intraspinal anesthetic/corticosteriod injections
Correct Answer: Anesthetic/corticosteriod injections into the epidural space
Explanation:
Nonsteroidal anti-inflammatory drugs have been shown effective and are frequently used during the acute phase of low back pain. Their main effect is to alleviate soft tissue inflammation that is often present in the early phase. Patient questionnaires have identified bed rest as among the most frequently prescribed treatments for lower back pain. It has been shown that bed rest results in reduced intradiskal pressure that occurs in the supine position. Anesthetic/corticosteriod injections are widely advocated for the treatment of low back pain and can be administered along nerve roots, into the sacroiliac joints, intervertebral disks, paraspinal soft tissues, and the epidural space or intrathecally for many conditions. However, there is no evidence that intraspinal steroids have an effective role in the acute management of low back pain.
Question 20:
A 32-year-old woman is diagnosed on magnetic resonance imaging with a far-lateral disk herniation at the L3/L4 level causing radiating right lower extremity discomfort across the anterior aspect of her knee with no motor or reflex abnormalities. Which of the following nerve roots is most likely affected:
Options:
Correct Answer: L3
Explanation:
A far-lateral or foraminal disk herniation often affects the exiting or more proximal nerve root. The traversing or more distal nerve root is typically affected from a posterolateral disk herniation. In this case, the patient has a far-lateral disk herniation at the L3/L4 level resulting in L3 nerve root symptomatology.