Full Question & Answer Text (for Search Engines)
Question 1:
A patient with a fracture dislocation of the spine has a sensory level at the xiphoid process. Which of the following nerve root levels indicates this finding:
Options:
Correct Answer: T7
Explanation:
The skin over the xiphoid process area is innervated by the T7 nerve root. In addition to knowing the innervation of selected muscles and the deep tendon reflexes, the clinician should also know the sensory levels to localize pathologic processes. T4 Nipple line T7 Xiphoid process T10 Umbilicus T12 Groin
Question 2:
A patient with a fracture dislocation of the spine has a sensory level at the umbilicus. Which of the following nerve root levels indicates this finding:
Options:
Correct Answer: T10
Explanation:
The skin of the umbilicus is innervated by the T10 nerve root.br> In addition to knowing the innervation of selected muscles and the deep tendon reflexes, the clinician should also know the sensory levels to localize pathologic processes. T4 Nipple line T7 Xiphoid process T10 Umbilicus T12 Groin
Question 3:
Which of the following statements regarding the presentation of thoracic disk herniations is false:
Options:
- Pain is the principal symptom.
- Radicular pain may be present.
- Mechanical axial back pain may be present.
- Myelopathic pain may be present.
- Bowel and bladder symptoms occur in more than 50% of affected patients.
Correct Answer: Bowel and bladder symptoms occur in more than 50% of affected patients.
Explanation:
Patients with thoracic disk herniations may present with mechanical axial back pain, radicular pain, or myelopathy, but pain is the principal symptom. Bowel and bladder symptoms occur in 10% to 20% of affected patients.
Question 4:
Which of the following statements regarding the treatment of thoracic disk herniations is true:
Options:
- The majority of patients can be treated nonoperatively.
- Surgical decompression is necessary in most cases.
- Laminectomy is the surgical procedure of choice.
- The anterior transthoracic approach is used for T1-T4 lesions.
- C ostotransversectomy is used for large central calcified herniations.
Correct Answer: The majority of patients can be treated nonoperatively.
Explanation:
The majority (75%) of patients with thoracic disk herniations may be managed nonoperatively. Surgical procedures must adequately decompress the involved nerve root. Posterior approach by laminectomy is usually not adequate, and costotransversectomy is not effective for large central calcified herniations (an anterior approach is preferred). The anterior transthoracic approach is effective for T5-T12 lateral and anterior disk herniations.
Question 5:
Which of the following is the only accepted pharmacological agent for the acute treatment of a spinal cord injury:
Options:
- GM-1 ganglioside
- Tirilazad (lipid peroxidation inhibitor)
- Nimodipine (calcium channel blocker)
- Naloxone (opoid antagonist)
- Methylprednisolone
Correct Answer: Methylprednisolone
Explanation:
Methylprednisolone is currently the only accepted pharmacologic agent for the treatment of spinal cord injury. The North American Spinal C ord Injury Studies (NASC IS) found significant motor and sensory improvement in patients who were treated within 8 hours of injury with a methylprednisolone bolus of 30 mg/kg, followed by an infusion of 5.4 mg per hour for 24 hours. Other agents have been studied in animal experiments but have not been promising in clinical trials.
Question 6:
A 45-year-old man has neck pain following a motor vehicle accident. His neurologic examination is normal. His plain radiographs are shown (Slide). The most likely diagnosis is:
Options:
- C ervical strain (whiplash-type injury)
- C ompression fracture of C 5
- Unilateral facet dislocation
- Bilateral facet dislocation
- Spinous process fracture
Correct Answer: Unilateral facet dislocation
Explanation:
The lateral radiograph shows translation and kyphosis at the level of injury. The facets of C4 do not superimpose on each to create a "double sail" sign. This patient has a unilateral facet dislocation. With unilateral facet dislocations, there is usually 3 mm to 4 mm of forward translation and 5° to 7° of angulation.
Question 7:
A 35-year-old man has neck pain following a motor vehicle accident. His axial computed tomography scan is shown (Slide). The most likely diagnosis is:
Options:
- C 4 compression fracture
- C lay shovelers fracture
- Bilateral facet dislocation
- Unilateral facet dislocation
- Pseudosubluxation of C 4 on C 5
Correct Answer: Unilateral facet dislocation
Explanation:
The axial computed tomography scan of C 4-C 5 shows a unilateral facet dislocation. Notice that the superior facet of C 5 lies posterior to the inferior facet of C 4. This relationship should be the exact opposite. Also, notice that C 4 is rotated on the body of C 5 and translated forward.
Question 8:
A 40-year-old woman has severe neck pain following a motor vehicle accident. Her plain lateral radiograph of the spine is shown (Slide). A sagittal magnetic resonance scan is shown (Slide). The most likely diagnosis is:
Options:
- Pseudosubluxation of C 5 on C 6
- C ompression fracture of C 5
- Unilateral facet dislocation
- Bilateral facet dislocation
- Degenerative sponylolisthesis C 5 on C 6
Correct Answer: Bilateral facet dislocation
Explanation:
There is significant subluxation of C 5 on C 6 on the plain radiograph. The facets of C 5 and C 6 have lost their normal relationship. This patient has a bilateral facet dislocation. There is compression and significant changes within the spinal cord. This patient should be treated with reduction and fusion.
Question 9:
A 40-year-old woman has severe neck pain following a motor vehicle accident. Her plain lateral radiograph of the spine is shown (Slide). A sagittal magnetic resonance is shown (Slide). The most appropriate treatment would be:
Options:
- Observation
- Neck collar and physical therapy
- Reduction and collar immobilization
- Reduction and halo immobilization
- Reduction and fusion
Correct Answer: Reduction and collar immobilization
Explanation:
There is significant subluxation of C 5 on C 6 on the plain radiograph. The facets of C 5 and C 6 have lost their normal relationship. This patient has a bilateral facet dislocation. There is compression and significant changes within the spinal cord. This patient should be treated with reduction and fusion. This is a ligamentous injury so reduction and immobilization will not result in satisfactory healing.
Question 10:
In which of the following nerve roots is compression neuropathy common in cervical spondylosis:
Options:
- C 3 and C 4
- C 4 and C 5
- C 5 and C 6
- C 6 and C 7
- C 7 and C 8
Correct Answer: C 6 and C 7
Explanation:
The nerve roots that are most commonly affected in cervical spondylosis are C6 and C7, secondary to degenerative changes in the C 5-C 6 and C 6-C 7 nerve roots. Patients may have specific dermatomal pain or pain that is diffuse and poorly localized.
Question 11:
Which of the following sensory areas is affected by compression of the C 6 nerve root:
Options:
- Lateral forearm into the radial side of the hand
- Base of neck, medial shoulder
- Posterior neck, occiput
- Ulnar side of the forearm and hand
- Posterolateral forearm into the middle finger of the hand
Correct Answer: Lateral forearm into the radial side of the hand
Explanation:
It is important to remember the sensory dermatome when examining patients who have neck and upper extremity pain: C3 Posterior neck, occiput C4 Base of neck, medial shoulder C5 Base of neck to shoulder and upper arm C6 Lateral forearm into the radial side of the hand C7 Posterolateral forearm into the middle finger of the hand C8 Ulnar side of the forearm and hand
Question 12:
Which of the following sensory areas is affected by compression of the C 7 nerve root:
Options:
- Base of neck, medial shoulder
- Base of neck to shoulder and upper arm
- Lateral forearm into the radial side of the hand
- Posterolateral forearm into the middle finger of the hand
- Ulnar side of the forearm and hand
Correct Answer: Lateral forearm into the radial side of the hand
Explanation:
It is important to remember the sensory dermatome when examining patients who have neck and upper extremity pain: C3 Posterior neck, occiput C4 Base of neck, medial shoulder C5 Base of neck to shoulder and upper arm C6 Lateral forearm into the radial side of the hand C7 Posterolateral forearm into the middle finger of the hand C8 Ulnar side of the forearm and hand
Question 13:
A patient comes into your office with neck and arm pain. The patientâ s plain radiograph is shown (Slide). Which of the following signs is most likely to be found on physical examination:
Options:
- Triceps muscle weakness
- Deltoid muscle weakness
- Finger flexion weakness
- Numbness on the lateral forearm into the radial side of the hand
- Numbness on the ulnar side of the forearm and hand
Correct Answer: Numbness on the lateral forearm into the radial side of the hand
Explanation:
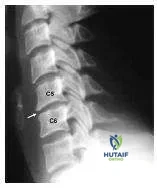
The lateral radiograph shows narrowing of the C 5-C 6 intervertebral disk space with osteophytes arising anteriorly and posteriorly. This degenerative process results in facet joint hypertrophy, osteophytes in the uncovertebral joints, and hypertrophy of the ligamentum flavum. The C 6 nerve root is compressed resulting in numbness on the lateral forearm into the radial side of the hand. Elbow and wrist extension may be affected, and the biceps tendon reflex may be diminished or absent. It is important to remember the sensory dermatome when examining patients who have neck and upper extremity pain: C3 Posterior neck, occiput C4 Base of neck, medial shoulder
C5 Base of neck to shoulder and upper arm C6 Lateral forearm into the radial side of the hand C7 Posterolateral forearm into the middle finger of the hand C8 Ulnar side of the forearm and hand
Question 14:
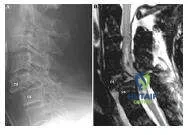
A 45-year-old woman has pain in her right upper extremity and neck. The plain film is is presented (Slide 1) as well as an axial post myelogram CT images (Slide 2, A & B). Her pain has not responded to nonsteroidal anti- inflammatory drugs or physical therapy. Which of the following is the most appropriate treatment:
Options:
- Needle aspiration of the C 4-C 5 intervertebral space
- 6-week course of antibiotics and bracing
- Needle biopsy of C 4 or C 5
- Mammography and technetium bone scan
- Anterior cervical diskectomy
Correct Answer: Anterior cervical diskectomy
Explanation:
The axial post myelogram CT image shows a disk herniation, and the sagittal view shows prominent osteophytes. There is no evidence of an infection or a neoplasm. This patient is a candidate for anterior disckectomy and fusion.
Question 15:
Plain radiographs of the lumbosacral spine are useful for:
Options:
- Detecting marrow changes
- Far lateral herniated intervertebral disks
- Distinction between disk material and the dural sac
- Lateral recess stenosis
- Instability patterns
Correct Answer: Instability patterns
Explanation:
Plain radiographs are useful for assessing the alignment of the spine, bone destruction by tumors and infections, and instability patterns. The radiographs also will show degenerative intervertebral disks. Plain radiographs are not sensitive for detecting marrow changes, herniated disks, and neural compression secondary to degenerative changes.
Question 16:
Computerized tomography scans are efficacious for detecting which of the following conditions:
Options:
- Marrow changes
- Lytic lesion suspected on Plain L spine film
- Intrathecal abnormalities
- Instability patterns
- Intervertebral disk hydration
Correct Answer: Lytic lesion suspected on Plain L spine film
Explanation:
Computerized tomography scans are excellent for assessing bone structure, especially in patients with metastatic bone disease and primary bone tumors of the spine. C omputerized tomography is useful for distinguishing between bone and soft tissue compression in neural compressive disorders.
Question 17:
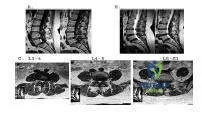
A 35-year-old construction worker has left leg pain and difficulty walking. His examination is normal except for decreased sensation to the lateral border of the left foot, the inability to walk on the toes of the left foot, and a positive stretch test producing left heel and lateral foot pain. A magnetic resonance image shows a large posterolateral herniated nucleus pulposus on the left side at L5-S1. The gait abnormality is most likely due to:
Options:
- Cauda equina syndrome
- L5 radiculopathy and gastrocsoleus muscle complex denervation
- L5 radiculopathy and extensor hallucis longus weakness
- S1 radiculopathy and gastrocsoleus muscle complex denervation
- S2 denervation and extensor hallucis longus weakness
Correct Answer: S1 radiculopathy and gastrocsoleus muscle complex denervation
Explanation:
In the lumbar spine, direct posterior and posterolateral disk herniations typically compress the traversing nerve root. In this patient, the herniated disk at the L5-S1 level compresses the shoulder of the S1 nerve root as it comes off the dural sac. The S1 nerve root supplies sensation to the posterior calf and lateral border of the foot, and motor chiefly to the gastrocsoleus muscle complex.
Question 18:
Which of the following types of neural dysfunction is present with a cervical fracture-dislocation, resulting in a Brown-Sequard neurological injury:
Options:
- Ipsilateral loss of pain, temperature recognition, and contralateral loss of motor function
- Ipsilateral loss of motor and contralateral loss of pain/temperature
- Bilateral loss of pain/temperature and unilateral loss of motor
- Bilateral loss of motor and unilateral loss of pain/temperature
- Bilateral upper extremity loss of motor and unilateral lower extremity loss of pain/temperature
Correct Answer: Ipsilateral loss of pain, temperature recognition, and contralateral loss of motor function
Explanation:
A Brown-Sequard injury causes damage to half of the spinal cord. Brown- Sequard injuries produce ipsilateral proprioceptive and motor loss and contralateral loss of sensitivity to pain and temperature. Proprioceptive sensory fibers enter the spinal cord, travel in the dorsal columns and lateral and ventral spinothalmic tracts, and decussate high in the thalamus. Motor efferent nerves cross in the medulla and travel down in the lateral corticospinal tracts.Spinthalamic fibers enter and decussate in the spinal cord. Hence, cord hemi-section produces contralateral pain and temperature (spinothalamic) loss, and ipsilateral motor (corticospinal) and, proprioceptive (dorsal columns) deficit. Often due to penetrating injuries, Brown-Sequard injuries have the best prognosis of the cord injury complexes.
Question 19:
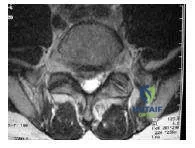
The axial computed tomography scan depicts a patient with spinal stenosis (Slide). The primary source of neural compression is impingement on the traversing nerve root by the:
Options:
- Superior facet of the level below
- Inferior facet of the level above
- Redundant ligamentum flavum
- Overgrown medial pedicle
- Herniated nucleus pulposus
Correct Answer: Superior facet of the level below
Explanation:
Spinal stenosis involves narrowing of the spinal canal by a combination of factors. Degeneration of the disk with dehydration allows loss of disk height and bulging posteriorly into the canal. The ligamentum flavum becomes redundant at the segment due to loss of the disk height and buckling of the ligament. C hief among the sources of compression, however, is the overgrowth of the facet joint, which acts to autostabilize the motion segment. The facets are oriented in an oblique plane, depending on the level involved. The superior facet of the subjacent vertebral body lies anterior and lateral to its counterpart from the level above, forming a shingle configuration. The superior articular process, therefore, lies adjacent to the shoulder of the traversing nerve root and is a significant source of lateral recess stenosis.
Question 20:
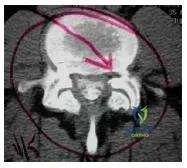
The type of disk herniation shown (Slide) at the L5-S1 level is most likely to cause:
Options:
- Quadriceps weakness and numbness of the medial thigh
- Diminished sensation to the anteromedial calf
- Weakness of the tibialis anterior
- Weakness of the gastrocsoleus complex
- Extensor hallucis longus weakness
Correct Answer: Weakness of the tibialis anterior
Explanation:
This slide shows a posterolateral disk herniation on the right. Posterolateral disk herniations cause compression of the traversing S1 nerve root at this level. Sensation affected is the posterior calf and lateral border of the foot, while motor innervation is to the gastroc soleus complex. With far lateral disk herniations, the exiting nerve root is compressed and symptoms may be seen referred to the level above.
 C5 Base of neck to shoulder and upper arm C6 Lateral forearm into the radial side of the hand C7 Posterolateral forearm into the middle finger of the hand C8 Ulnar side of the forearm and hand
C5 Base of neck to shoulder and upper arm C6 Lateral forearm into the radial side of the hand C7 Posterolateral forearm into the middle finger of the hand C8 Ulnar side of the forearm and hand