Full Question & Answer Text (for Search Engines)
Question 1:
An 18-year-old man comes to the office with a grade IV isthmic spondylolisthesis and severe left lower extremity discomfort. Which imaging study would best help identify the site of potential nerve root compression:
Options:
- Computed tomography scan
- Magnetic resonance imaging (MRI) scan
- Plain myelography
- Bone scan
- Positron emission tomography (PET)
Correct Answer: Magnetic resonance imaging (MRI) scan
Explanation:
An MRI scan would be the imaging study of choice to best identify the site of nerve root compression because it provides parasagittal views that can help determine the degree of narrowing of the neural foramina. Plain myelography may not accurately identify lateral recess compression. A C T scan would produce images perpendicular to the plane of nerve root compression. Bone scan and PET scan would be of little or no help in identifying nerve root compression.
Question 2:
Some of the more common risk factors that could predispose a person to developing low back pain are listed below. Which risk factor has not been implicated:
Options:
- Occupations requiring the use of jackhammers
- Being above normal bodyweight
- Cigarette or other tobacco consumption
- Female gender
- Occupations requiring the frequent operation of motor vehicles
Correct Answer: Female gender
Explanation:
Being female has not been implicated as a risk factor in the development of low back pain. Occupations that require heavy lifting, the use of jackhammers, and operating motor vehicles, as well as the usage of tobacco products and being overweight have all been associated with a higher incidence of developing low back pain.
Question 3:
When considering surgical intervention in the management of low back pain, it is crucial to try and identify the possible offending agent or pain generator. Based on awake anatomical stimulation studies, what percentage of patients should report significant discomfort when a nerve root is either compressed or stretched in an attempt to elicit pain:
Options:
Correct Answer: 99%
Explanation:
Studies have reported on diskectomies in awake patients performed under local anesthesia. Anatomic spinal structures were stimulated prior to additional local anesthesia placed into these deeper areas and patients were asked to report any pain. Compression or stretching of nerve roots caused significant pain 100% of the time. Stimulation of the posterior dura caused significant pain only 1% of the time.
Question 4:
Which disorder does not represent a rheumatologic/inflammatory condition associated with causing low back pain:
Options:
- Rheumatoid arthritis
- Reiter syndrome
- Psoriatic arthritis
- Ankylosing spondylitis
- Osteoarthritis
Correct Answer: Osteoarthritis
Explanation:
Although osteoarthritis is the most common arthritic disorder associated with low back pain, it is not a rheumatologic condition. Rheumatoid arthritis, Reiter syndrome, psoriatic arthritis, and ankylosing spondylitis are all rheumatologic or inflammatory conditions associated with the development of low back pain.
Question 5:
A 57-year-old man with known lung cancer and metastatic disease complains of increasing low back pain. How often is the lumbar spine involved when a patient has known spinal metastasis:
Options:
Correct Answer: 5%
Explanation:
In 85 % of patients with metastatic disease to the spine, the lumbar region vertebral body is involved. If operable, the vertebral body lesion can be managed via an anterior approach with a corpectomy, as opposed to a posterior approach with laminectomy and removal of all involved posterior elements (if they are involved).
Question 6:
A 32-year-old man develops left lower extremity discomfort following a basketball game. A magnetic resonance image of the lumbar spine reveals a posterolateral disk herniation at the level of L4/L5. All of the following conditions could be associated with this except:
Options:
- Decreased strength in the hip abductors
- Decreased strength in the extensor hallucis longus muscle
- Numbness in the lateral aspect of the leg
- Decreased strength in plantarflexion of the foot
- Pain in the dorsum of the foot
Correct Answer: Decreased strength in the hip abductors
Explanation:
Decreased strength in the hip abductors and in the extensor hallucis longus muscle along with numbness in the lateral aspect of the leg and pain in the dorsum of the foot can all be associated with a herniation at the L4/L5 level affecting the L5 nerve root. Decreased strength in plantarflexion of the foot is present when the S1 nerve root is involved, such as with a disk herniation at the L5/S1 level.C orrect Answer: Decreased strength in plantarflexion of the foot
Question 7:
A 43-year-old man develops pain radiating down his left leg from a far- lateral disk herniation at the L5/S1 level. Which is the most likely nerve root contributing to his discomfort:
Options:
Correct Answer: L5
Explanation:
Typically, for a posterolateral disk herniation, the traversing or more distal nerve root is often involved. With a far-lateral disk herniation (as in this case), the exiting nerve root is usually involved. In this case, it would be the L5 nerve root.
Question 8:
Which orthopedic test, designed to apply tension to the spinal cord producing pain, involves having the patient lie supine while the examiner flexes the patient's head to his chest:
Options:
- Kernig sign
- Hoover test
- Milgram test
- Naffziger test
- Gaenslen test
Correct Answer: Kernig sign
Explanation:
The Kernig test involves the patient lying supine while the examiner forcibly flexes the head to the chest applying tension to the spinal cord. The test is positive if pain is elicited and indicates meningeal irritation in conditions such as meningitis. The Hoover test can help identify a patient who is malingering. This test involves having the patient lie supine with the examiner's hands placed under both of the patient's heels. The patient is asked to lift the affected leg. If a true effort is made, the examiner should feel downward pressure in the patient's opposite foot as he attempts to lift the affected leg. If no downward pressure is felt, the patient purposely may not be trying and might be malingering. The Milgram test may be used in conditions with suspected intrathecal pathology. While lying supine, the patient is asked to perform bilateral straight leg lifts. If the patient can sustain his feet 2 inches off the ground for more 30 seconds, intrathecal pathology is less likely. The Naffziger test is designed to increase intrathecal pressure and thus pain by compressing the jugular veins. The Gaenslen test is used to determine sacroiliac joint pathology.
Question 9:
A 52-year-old man sustained an L1 burst fracture after falling from a ladder 3 weeks ago. He was found neurologically intact after initial examination. He has been treated with conservative management since the accident, but he now complains of an inability to void along with numbness and tingling in both of his legs. Computed tomography scan shows worsening conus compression. On physical examination, you discover that he has weak anal sphincter tone. Your next step in the treatment of this patient should be:
Options:
- Anterior decompression and fusion with grafting with or without instrumentation
- High-dose steroids
- Laminectomy
- Posterior fusion with instrumentation
- C ontinue conservative management with follow-up in 1 month
Correct Answer: Anterior decompression and fusion with grafting with or without instrumentation
Explanation:
This patient has deteriorating neurological findings involving the cauda equina; therefore, surgical decompression is indicated. An anterior approach will directly decompress the neural structures. Performing a laminectomy alone is actually contraindicated as it may increase potential spinal instability. A posterior approach to achieve a fusion with instrumentation may not fully decompress the neural structures, although this is somewhat controversial.
Question 10:
A 27-year-old man comes in for examination. He complains of worsening pain in his lower back. He states that the pain started 4 days ago after lifting a heavy box. The patient's neurological exam is completely nonfocal. The initial management of this patient should include:
Options:
- Computed tomography scan of the lumbar spine with contrast
- Epidural steroid injection
- Magnetic resonance image of the lumber spine
- Bed rest of short duration along with nonsteroidal anti-inflammatory medications
- Computed tomography scan of the lumbar spine without contrast
Correct Answer: Bed rest of short duration along with nonsteroidal anti-inflammatory medications
Explanation:
This patient's neurological exam is normal and his injury was recent; this is most likely a soft tissue injury to his low back. Due to the patient's age and the fact that this is most likely not a serious injury, an initial conservative approach would be most appropriate. Epidural steroids or a selective nerve root block would be indicated if this patient developed worsening low back complaints or radicular pain in association with his low back pain.
Question 11:
When trying to distinguish sciatic radicular pain from pain following a hamstring strain, it is important to know that pain from a hamstring strain usually only involves the posterior aspect of thigh. Sciatic nerve pain may also be associated with:
Options:
- Pain radiating down the leg and into the foot
- Low back pain
- Pain in the opposite leg
- Pain radiating down the leg and into the foot, and pain in the opposite leg
- Pain radiating down the leg and into the foot, pain in the opposite leg, and low back pain
Correct Answer: Pain radiating down the leg and into the foot
Explanation:
Sciatic pain can involve all of the above complaints including radicular pain extending down the leg, low back pain, and pain into the opposite leg.
Question 12:
A 42-year-old man sustained a twisting injury to his low back 5 months ago. Since the injury, he has persistent low back pain that radiates into his right thigh and down to his posterior calf. The patient underwent a magnetic resonance imaging of his lumbar spine revealing a small posterolateral lumbar disk herniation at the L4L5 level. Over the past month, the patient states that his leg pain has been getting progressively better and has almost disappeared over the past week with the use of nonsteroidal anti- inflammatory medications and occasional bed rest. The next step in the management of this patient should be:
Options:
- A lumbar computed tomography scan
- Repeat magnetic resonance image
- Surgical excision of the herniated disk
- C ontinued conservative management
- Epidural steroid injection
Correct Answer: C ontinued conservative management
Explanation:
The patient has shown continued improvement of his symptoms including the leg pain with conservative treatment. Epidural steroids would be indicated if this patient had continued or worsening leg pain and/or low back pain.
Question 13:
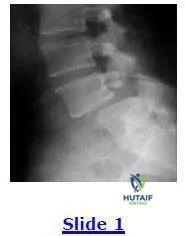
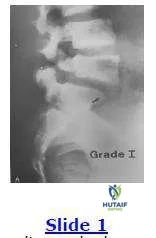
This radiograph shows a grade I spondylolisthesis of L5 on S1. This is due to a defect in what anatomical area:
Options:
- Superior articular process
- Inferior articular process
- Pars interarticularis
- Pedicle
- Lamina
Correct Answer: Pars interarticularis
Explanation:
The anatomical region involved in a spondylolisthesis is the pars interarticularis that is located between the superior and inferior articular processes and is a high stress area of relatively thinner bone.
Question 14:
A 16-year-old football lineman develops unrelenting low back pain for the past 3 months. Based on the magnetic resonance image shown, the next step in the management of this patient is:
Options:
- Fusion in situ
- Epidural injection therapy
- Excision of a herniated disk
- Restriction of the exacerbating activity
- Observation
Correct Answer: Fusion in situ
Explanation:
This patient has a grade I-II spondylolisthesis of L5 on S1. The initial management should include restriction of physical activity. Once the symptoms abate, the athlete can return to the sport. If symptoms return, other interventions are indicated including possible brace wear.C orrect Answer: Restriction of the exacerbating activity
Question 15:
A 50-year-old woman with 3 months of low back pain recently discovers a hard, painless lump in her breast. Due to the back discomfort, she undergoes plain radiography and subsequently a computed tomography scan (below). The most likely diagnosis is:
Options:
- Osteomyelitis
- Osteoid osteoma
- Fracture
- Herniated nucleus pulposis
- Metastatic disease
Correct Answer: Metastatic disease
Explanation:
The computed tomography scan reveals a destructive lesion involving the vertebral body extending into the pedicle in a patient with a suspected breast malignancy. This is a metastatic lesion until proven otherwise. This patient needs a thorough evaluation of her breast lesion, as well as her spine lesion, including biopsies. An osteoid osteoma is seen in a younger population and is seen on a computed tomography scan as a sclerotic round lesion.
Question 16:
A 45-year-old construction worker with long standing low back pain now notices bilateral thigh and lower extremity discomfort for the past 6 months. He has undergone conservative treatment with little success including injection therapy. He cannot perform his work duties. Based on the lateral radiograph shown below, the next step in the management of the patient should consist of:
Options:
- Laminectomy
- C ontinued conservative treatment
- Posterolateral fusion in situ without instrumentation
- Diskectomy
- Decompression and posterolateral fusion in situ with instrumentation.
Correct Answer: Posterolateral fusion in situ without instrumentation
Explanation:
This patient has an isthmic L4L5 spondylolisthesis with accompanied neuroforaminal stenosis. He already failed conservative management and would benefit from operative intervention. This should consist of a decompressive procedure to alleviate his lower extremity symptomatology along with a fusion procedure of the L4-L5 level due to the listhesis. If he undergoes a laminectomy alone, he may develop increased low back pain in the future.
Question 17:
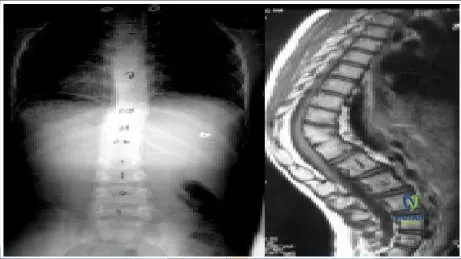
A 35-year-old woman presents with severe back pain. Radiographic evaluation reveals a thoracic curve of 70° and a loss of thoracic kyphosis. Surgery is recommended to correct the deformity. Which of the following tests must be ordered as part of the preoperative evaluation:
Options:
- Electrocardiogram (ECG)
- Pulmonary function tests
- Electromyelogram (EMG)
- Chest radiograph
- Somatosensory evoked potentials (SSEP)
Correct Answer: Pulmonary function tests
Explanation:
Thoracic curves greater than 65° may affect pulmonary function, especially when they are combined with thoracic lordosis. This patient displays a thoracic curve of 70° and a loss of the normal thoracic kyphosis; therefore, pulmonary function tests are part of the routine evaluation.
Question 18:
A calcified thoracic disk in the spinal canal is pathognomonic for:
Options:
- Scheuermann disease
- Ankylosing spondylitis
- Thoracic disk herniation
- Vertebral wedging
- Infection
Correct Answer: Thoracic disk herniation
Explanation:
Plain radiographs of the spine are helpful in the diagnosis of disk herniation only if they demonstrate disk calcification. However, the calcified disk is not always the disk that is herniated, but it suggests the diagnosis. Detection of a calcified disk on radiograph in the canal is pathognomonic of herniation.
Question 19:
Surgical treatment of thoracic disk herniation by a laminectomy is contraindicated because this procedure is associated with which of the following:
Options:
- Incomplete relief of symptoms
- High incidence of neurologic damage
- Destabilization of the spine
- High incidence of recurrence
- High incidence of post-laminectomy kyphosis
Correct Answer: High incidence of neurologic damage
Explanation:
There is a high incidence of spinal cord injury associated with thoracic disks removed by laminectomy. The advent of alternative procedures, such as costotransversectomy and transthoracic decompression, has led to a decrease in spinal cord injury admissions. Also, patients who do not improve after laminectomy are less likely to be helped by later anterior decompression.
Question 20:
The most common presenting symptom of a patient with a thoracic disk herniation is:
Options:
- Anterior band-like chest pain
- Intrascapular pain
- Epigastric pain
- Lower extremity pain
- Lower extremity weakness
Correct Answer: Anterior band-like chest pain
Explanation:
Brown et al reported on a series of 55 patients initially treated with conservative management. Anterior band-like chest pain occurred in 67% of his patients. Lower extremity complaints accounted for 20% and ranged from weakness (16%) to parasthesias (4%).
 The anatomical region involved in a spondylolisthesis is the pars interarticularis that is located between the superior and inferior articular processes and is a high stress area of relatively thinner bone.
The anatomical region involved in a spondylolisthesis is the pars interarticularis that is located between the superior and inferior articular processes and is a high stress area of relatively thinner bone.