Pediatric Trigger Thumb: An Intraoperative Masterclass on A1 Pulley Release
Key Takeaway
This masterclass details open A1 pulley release for pediatric trigger thumb, guiding fellows through comprehensive anatomy, meticulous preoperative planning, and granular intraoperative execution. Learn critical neurovascular protection, precise incision techniques, and how to confirm complete release. We cover extensive pearls, pitfalls, and postoperative care for optimal outcomes.
Introduction and Epidemiology
Pediatric trigger thumb is a well-recognized orthopedic condition characterized by a mismatch in volume between the flexor pollicis longus tendon and the first annular pulley of the thumb. This volumetric mismatch prevents normal excursion of the tendon, resulting in a fixed flexion contracture or, less commonly, dynamic triggering of the thumb interphalangeal joint. Although historically termed "congenital trigger thumb," this nomenclature is widely considered a misnomer within the contemporary orthopedic literature. Extensive prospective screening of combined cohorts totaling over 14,500 newborns across multiple international centers has consistently failed to identify the condition at birth. Consequently, the term "pediatric trigger thumb" or "acquired trigger thumb of infancy" is more accurate and reflective of its postnatal development.

The condition typically presents between late infancy and five years of age. Unlike adult trigger digits, which are predominantly driven by inflammatory stenosing tenosynovitis, pediatric trigger thumb lacks gross, microscopic, or electron-microscopic evidence of inflammation. The hallmark pathoanatomic feature is a distinct enlargement or nodule within the flexor pollicis longus tendon, eponymously referred to as Notta's node, interacting with a thickened, unyielding first annular pulley.
Pathogenesis and Natural History
The exact pathogenesis of pediatric trigger thumb remains elusive. While adult trigger digits are associated with repetitive microtrauma and inflammatory cascades, pediatric biopsies consistently demonstrate fibrocartilaginous metaplasia without inflammatory infiltrates. Genetic predispositions have been hypothesized, particularly in bilateral presentations, but definitive Mendelian inheritance patterns remain unestablished. Traumatic etiologies are frequently reported by parents; however, these are generally considered recall bias, wherein an incidental minor trauma draws parental attention to a pre-existing fixed flexion contracture.
The natural history of the condition heavily influences management algorithms. Early literature suggested that spontaneous resolution was exceedingly rare, mandating prompt surgical intervention. However, contemporary longitudinal studies demonstrate spontaneous improvement rates ranging from 24% to 63%. It is critical to note that "resolution" in these conservative management cohorts is frequently defined as the restoration of passive interphalangeal joint extension to neutral, rather than the return of normal physiologic hyperextension. Furthermore, achieving this partial resolution requires an average of 48 months of observation. This prolonged timeline and the potential for incomplete resolution must be carefully weighed against the immediate, definitive outcomes provided by surgical release.
Surgical Anatomy and Biomechanics
A profound understanding of the surgical anatomy of the volar thumb is paramount to executing a safe and effective pulley release, particularly given the diminutive size of the pediatric structures and the unforgiving nature of iatrogenic neurovascular injury.

The Flexor Pulley System of the Thumb
The flexor pollicis longus tendon courses through a specialized fibro-osseous canal designed to maintain the tendon's proximity to the axis of rotation of the metacarpophalangeal and interphalangeal joints. This sheath is composed of a series of retinacular pulleys that prevent bowstringing during active flexion.
The most proximal pulley is the first annular pulley. It is a transverse structure originating from the volar plate of the metacarpophalangeal joint and the base of the proximal phalanx. In pediatric trigger thumb, the first annular pulley is the primary site of constriction. Biomechanically, isolated division of the first annular pulley does not alter the moment arm of the flexor pollicis longus tendon sufficiently to cause clinically significant bowstringing or functional deficit.
Distal to the first annular pulley lies the oblique pulley, which originates proximally on the ulnar aspect of the proximal phalanx and courses distally to insert on the radial aspect. The oblique pulley is the critical biomechanical constraint against flexor pollicis longus bowstringing. Iatrogenic transection of the oblique pulley during surgical release leads to a profound loss of mechanical advantage, resulting in flexion weakness and a visible bowstringing deformity. Some anatomical studies identify a distinct second annular pulley analogous to the A2 pulley in the digits, situated between the first annular and oblique pulleys, though its distinct presence is variable.
Neurovascular Topography
The digital nerves of the thumb are intimately associated with the flexor pollicis longus tendon sheath and are at significant risk during surgical dissection.

The radial digital nerve is particularly vulnerable. It courses distally and crosses obliquely over the flexor tendon sheath just proximal to the proximal edge of the first annular pulley. Because the surgical release must ensure complete division of the proximal first annular pulley, the radial digital nerve is directly in the surgical path if dissection is not meticulous. The ulnar digital nerve runs a more parallel course along the ulnar border of the tendon sheath, immediately adjacent to the first annular pulley. While less likely to cross the midline of the surgical field, it remains highly susceptible to injury from aberrant retractor placement or lateral straying of the scalpel.
Indications and Contraindications
The decision to proceed with surgical release of the first annular pulley hinges on patient age, duration of symptoms, severity of the contracture, and the presence of pain or active triggering. Because spontaneous resolution is possible, a period of observation is often warranted for children presenting under the age of one year.

Surgical intervention is definitively indicated for children over the age of two years who present with a fixed, rigid flexion contracture, or for those who have failed a prolonged period of observation. Children presenting with painful, active triggering that limits the functional use of the hand are also prime candidates for early surgical release.
Contraindications are few but critically important. The presence of active local infection precludes elective release. Furthermore, surgeons must meticulously differentiate isolated pediatric trigger thumb from syndromic contractures. Flexion deformities secondary to arthrogryposis multiplex congenita, spasticity from cerebral palsy, or congenital clasped thumb represent complex, multi-level pathology. In these scenarios, isolated first annular pulley release will fail to correct the deformity and is strictly contraindicated as a standalone procedure.
| Clinical Parameter | Non-Operative Management (Observation/Splinting) | Operative Management (A1 Pulley Release) |
|---|---|---|
| Patient Age | < 12 to 18 months | > 18 to 24 months |
| Symptom Duration | Newly diagnosed, short duration | Persistent beyond 6-12 months of observation |
| Deformity Type | Flexible, intermittent triggering | Rigid, fixed flexion contracture |
| Pain/Function | Painless, normal hand use | Painful triggering, avoidance of thumb use |
| Underlying Pathology | Isolated Notta's node | Isolated Notta's node (Rule out CP/Arthrogryposis) |
Pre Operative Planning and Patient Positioning
Preoperative planning relies almost entirely on a thorough clinical examination. Advanced imaging modalities such as magnetic resonance imaging are entirely unwarranted for classic presentations. Ultrasonography can dynamically demonstrate the volumetric mismatch between Notta's node and the first annular pulley but is rarely necessary to establish the diagnosis or alter the surgical plan.

Parental counseling is a critical component of preoperative planning. The surgeon must clearly articulate the goals of the procedure: restoration of interphalangeal joint extension and elimination of triggering. Parents should be advised that the palpable nodule (Notta's node) is not excised during the procedure; rather, the constricting tunnel is opened to accommodate it. The nodule typically remodels and diminishes in size over several months postoperatively.
The procedure is performed under general anesthesia, given the pediatric patient population. The patient is positioned supine with the affected upper extremity extended on a radiolucent hand table. A well-padded pediatric tourniquet is applied to the proximal arm to ensure a bloodless surgical field, which is absolutely mandatory for the safe identification of the diminutive digital nerves. Loupe magnification (minimum 2.5x to 3.5x) is strongly recommended for all stages of the dissection.
Detailed Surgical Approach and Technique
The surgical release of the pediatric first annular pulley demands meticulous tissue handling and precise anatomic recognition. The margin for error regarding neurovascular injury is measured in millimeters.

Incision and Superficial Dissection
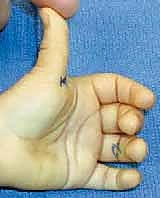
The surgical approach begins with an appropriately placed incision. A transverse incision measuring approximately 1.5 to 2.0 centimeters is placed directly within the metacarpophalangeal flexion crease of the thumb. This transverse orientation provides an excellent cosmetic result and minimizes the risk of longitudinal scar contracture. Alternatively, some surgeons prefer a longitudinal or zig-zag incision over the volar metacarpophalangeal joint, though this is generally reserved for revision cases.
Once the dermis is incised, superficial dissection must proceed with extreme caution. The subcutaneous fat in the pediatric volar thumb is dense and lobulated. Dissection should be performed bluntly using fine tenotomy scissors, spreading longitudinally parallel to the neurovascular bundles.

Deep Dissection and Nerve Protection
As the dissection deepens, the primary objective before exposing the tendon sheath is the definitive identification and protection of the radial and ulnar digital nerves. Small Senn or Ragnell retractors are utilized to gently retract the subcutaneous adipose tissue.
The radial digital nerve must be visualized as it courses obliquely across the proximal aspect of the surgical field. It is often found immediately deep to the dermis at the proximal edge of the transverse incision. Once identified, the nerve is gently mobilized and protected behind the radial retractor. The ulnar digital nerve is similarly identified along the ulnar border of the field and protected. Bipolar electrocautery should be used sparingly and only with direct visualization of the nerve branches.

Pulley Release and Verification
With the neurovascular structures securely retracted, the flexor tendon sheath is exposed. The first annular pulley is identified as a thick, transverse band of fibrous tissue overlying the flexor pollicis longus tendon at the level of the metacarpophalangeal joint.

Using a #15 scalpel blade or fine tenotomy scissors, the first annular pulley is divided longitudinally strictly in the midline. The release must begin at the proximal edge of the pulley, extending distally. As the pulley is divided, the underlying Notta's node will frequently herniate through the defect, confirming the site of constriction.

The distal extent of the release requires careful attention. The surgeon must completely divide the first annular pulley while meticulously preserving the proximal edge of the oblique pulley. The oblique pulley can be identified by the oblique orientation of its fibers, contrasting with the transverse fibers of the first annular pulley.
Once the release is believed to be complete, verification is mandatory. The surgeon passively extends and flexes the interphalangeal joint of the thumb.

Full, unimpeded passive extension to at least neutral, and ideally to symmetric hyperextension, must be achieved. Furthermore, the surgeon should directly observe the excursion of Notta's node during passive motion to ensure it clears both the proximal and distal remnants of the pulley system without catching. If residual catching or an incomplete extension arc remains, the proximal and distal extents of the release must be re-evaluated and extended as necessary.

Following verification, the tourniquet is deflated to achieve meticulous hemostasis. The wound is irrigated with sterile saline. Closure is typically performed using interrupted, absorbable sutures (e.g., 5-0 or 6-0 plain gut or chromic gut) to avoid the need for suture removal in the pediatric patient.
Complications and Management
While surgical release of the first annular pulley is highly successful, complications can occur and are often related to technical errors during dissection or an incomplete understanding of the regional anatomy.

Management of Specific Complications
Digital nerve injury represents the most devastating complication. The radial digital nerve is injured more frequently than the ulnar digital nerve due to its oblique course proximal to the first annular pulley. Injury can range from a transient neuropraxia due to overzealous retraction to complete sharp transection. If a sharp transection is recognized intraoperatively, immediate primary epineural repair utilizing microsurgical techniques and 8-0 or 9-0 nylon is mandatory. Delayed recognition presents as a persistent sensory deficit or the formation of a painful neuroma, which may require subsequent excision and nerve grafting.
Bowstringing of the flexor pollicis longus tendon occurs if the oblique pulley is inadvertently transected during the distal extent of the release. This results in a mechanical disadvantage, presenting clinically as a prominent volar tendon during active flexion and a subjective loss of pinch strength. While mild bowstringing may be tolerated, severe cases require complex pulley reconstruction utilizing extensor retinaculum or palmaris longus autograft to restore the biomechanical fulcrum.
Recurrence of triggering or persistent flexion contracture is almost universally the result of an incomplete proximal or distal release of the first annular pulley. If aggressive postoperative stretching fails to resolve the residual contracture, a revision surgical release is indicated. Revision surgery carries a significantly higher risk of neurovascular injury due to the presence of scar tissue, necessitating an extended incision and meticulous neurolysis prior to addressing the residual pulley.
| Complication | Estimated Incidence | Etiology / Pathoanatomy | Salvage / Management Strategy |
|---|---|---|---|
| Incomplete Release / Recurrence | 1% - 3% | Failure to divide proximal or distal extent of A1 pulley | Revision surgery with extended exposure; aggressive post-op stretching |
| Digital Nerve Injury | < 1% | Transection or traction neuropraxia (Radial > Ulnar) | Intra-op: Primary microsurgical repair. Post-op: Observation for neuropraxia; neuroma excision/grafting if transected |
| FPL Bowstringing | < 1% | Iatrogenic transection of the oblique pulley | Observation if mild/asymptomatic. Pulley reconstruction with autograft if severe weakness |
| Superficial Infection | 1% - 2% | Normal skin flora colonization of surgical site | Oral antibiotics (e.g., Cephalexin); local wound care |
| Incisional Contracture | Rare | Use of longitudinal incision crossing flexion crease | Z-plasty or local tissue rearrangement |
Post Operative Rehabilitation Protocols
The postoperative management following a pediatric trigger thumb release is generally straightforward, reflecting the robust healing potential of the pediatric population.

Immediately postoperatively, a soft, bulky compressive dressing is applied to the hand and thumb. Immobilization with a rigid splint or cast is generally unnecessary and actively discouraged, as early mobilization prevents tendon adhesions. The bulky dressing serves primarily to protect the incision site from local trauma and to absorb any minimal postoperative oozing.
The dressing is typically removed by the parents or in the clinic at approximately one to two weeks postoperatively. At this stage, the wound should be well-healed. Formal physical therapy or occupational therapy is rarely required. Children naturally resume age-appropriate play and functional use of the hand, which provides excellent dynamic rehabilitation. Parents are instructed to encourage activities that involve thumb extension and grasping.
In rare cases where a severe, long-standing flexion contracture was present preoperatively, the child may exhibit a persistent, albeit improved, lack of terminal extension due to secondary capsular contracture of the interphalangeal joint. In these specific instances, a nighttime extension splint may be fabricated and utilized for 6 to 12 weeks to gradually stretch the volar capsule and achieve maximal extension.
Summary of Key Literature and Guidelines
The academic discourse surrounding pediatric trigger thumb has evolved significantly, particularly regarding the natural history and the timing of surgical intervention.
Historically, the condition was viewed as a strict surgical mandate. However, landmark longitudinal studies have fundamentally altered the treatment paradigm. Prospective cohorts have demonstrated that observation is a viable initial strategy, with spontaneous resolution rates approaching 63% over an average follow-up of 48 months. These studies emphasize that while the deformity may improve, the definition of "resolution" often accepts a residual lack of hyperextension, a nuance that must be communicated during shared decision-making with parents.
Conversely, surgical literature consistently demonstrates near-universal success with first annular pulley release. Large retrospective series report success rates exceeding 95%, with minimal complication profiles when performed by appropriately trained surgeons. The consensus among pediatric orthopedic surgeons suggests a stratified approach: conservative observation for infants and toddlers under 18 to 24 months of age, particularly those with flexible deformities, and definitive surgical release for older children, those with rigid contractures, or those who fail a dedicated period of observation.
The debate regarding the exact etiology remains unresolved. The absence of inflammatory markers in pediatric histological specimens firmly separates the condition from adult stenosing tenosynovitis. Future research directions are focused on identifying potential genetic markers and understanding the cellular mechanisms driving the fibrocartilaginous metaplasia characteristic of Notta's node. Despite these etiologic questions, the surgical release of the first annular pulley remains the definitive, highly reliable solution for the correction of pediatric trigger thumb.
Clinical & Radiographic Imaging














You Might Also Like