Pectoralis Major Transfer for Long Thoracic Nerve Palsy: An Intraoperative Masterclass
Key Takeaway
Join us in the OR for a detailed masterclass on pectoralis major transfer for long thoracic nerve palsy. We'll meticulously cover comprehensive anatomy, precise patient positioning, step-by-step surgical execution from incision to fixation, and critical pearls to manage scapular winging. Understand graft choices, tensioning, and rehabilitation for optimal outcomes in patients with persistent symptomatic serratus anterior dysfunction.
Introduction and Epidemiology
Long thoracic nerve palsy leads to classical medial scapular winging because of weakness of the serratus anterior muscle. Lesions of the long thoracic nerve can range from mild paresis to complete paralysis, leading to varying degrees of shoulder dysfunction and debilitating pain. Other types of winging include trapezius lateral winging (typically secondary to spinal accessory nerve injury) and rhomboid winging (associated with dorsal scapular nerve injury).
The serratus anterior muscle functions to stabilize the scapula against the chest wall, thus providing a fulcrum for the humerus to push against while moving the arm in space. Without this stable fulcrum, shoulder elevation is profoundly weakened, which leads to an inability to use the arm in forward activities. Forward elevation of the shoulder is most severely affected, followed by shoulder abduction. Patients often present with fatigue, periscapular spasm, and secondary impingement symptoms due to the loss of synchronous scapulothoracic rhythm.
Epidemiologically, long thoracic nerve palsy is most frequently observed following closed trauma, traction injuries, or viral illnesses such as Parsonage-Turner syndrome (neuralgic amyotrophy). Iatrogenic injuries also account for a significant proportion of cases, particularly following axillary lymph node dissection, first rib resection for thoracic outlet syndrome, or lateral chest wall interventions. Most traumatic or idiopathic neurapraxic injuries will resolve spontaneously with conservative management, but recovery can take up to 24 months. For patients who fail to demonstrate clinical or electromyographic improvement after 12 to 18 months, surgical intervention via pectoralis major transfer is indicated to restore scapular mechanics and upper extremity function.

Pathogenesis of Scapular Winging
Scapular winging may be due to primary, secondary, or voluntary causes. Primary scapular winging can be divided into neurologic, bony, and soft tissue types. Neurologic primary winging is the most common and is directly related to denervation of the periscapular musculature. Secondary winging occurs as a compensatory mechanism for glenohumeral pathology, such as adhesive capsulitis or rotator cuff arthropathy, where the scapula moves abnormally to compensate for limited glenohumeral motion. Voluntary winging is a rare psychiatric or behavioral manifestation.
In the context of long thoracic nerve palsy, the pathogenesis is rooted in the loss of the serratus anterior's mechanical tethering of the medial scapular border to the thoracic cage. When this tether is lost, the unopposed pull of the pectoralis minor and the remaining functional periscapular muscles results in the characteristic medial and superior translation of the scapula.

Surgical Anatomy and Biomechanics
Serratus Anterior and Long Thoracic Nerve Anatomy
The serratus anterior is a large broad muscle that covers the lateral aspect of the thorax. It has digitations that take origin from the upper nine ribs, pass deep to the scapula, and insert on the medial aspect of the scapula. The muscle is anatomically and functionally divided into three distinct divisions.
The first division consists of one slip and takes origin from the first two ribs. This division runs slightly upward and inserts on the superior angle of the scapula. The second division is made up of three slips from the second, third, and fourth ribs and inserts on the anterior surface of the medial border of the scapula. The third division, which consists of the inferior five slips from ribs five through nine, inserts on the inferior angle of the scapula. Because this division has the longest course, it possesses the longest lever arm and generates the most power for scapular upward rotation and protraction.

The serratus anterior muscle is innervated exclusively by the long thoracic nerve, which arises from the ventral rami of cervical roots C5, C6, and C7. The C5 and C6 roots pass through the scalenus medius muscle and merge before they receive a branch from C7. The nerve enters the axillary sheath at the level of the first rib and travels posteriorly in the axilla. It then passes over a prominence in the second rib and descends along the lateral chest wall where it enters the serratus anterior fascia and then the muscle itself.
The total length of the nerve is approximately 24 cm, and there are several possible points of injury along its course. Proximally, as well as distally along the chest wall, the nerve is highly susceptible to injury because of its superficial location. Furthermore, the nerve is tethered in the axillary sheath, which places it on stretch with forward elevation and contralateral lateral flexion of the cervical spine. Cadaveric examinations have illustrated a fascial sling with the potential to cause nerve bowstringing with abduction and external rotation. This fascial band extends from the inferior aspect of the brachial plexus to just superior to the middle scalene muscle.

Pectoralis Major Anatomy
The pectoralis major is a powerful, fan-shaped muscle situated on the anterior chest wall. It is composed of three primary segments based on their origin: the clavicular head, the sternocostal head, and the abdominal head. The sternocostal head, which originates from the anterior surface of the sternum and the cartilages of the upper six ribs, is the most robust portion of the muscle.
For the surgical management of medial scapular winging, the sternocostal head is typically isolated and transferred. The innervation to the sternocostal head is provided by the medial pectoral nerve (C8, T1), which enters the deep surface of the muscle, and the lateral pectoral nerve (C5, C6, C7). Preserving these neurovascular pedicles during mobilization is critical for the viability and function of the transfer.

Biomechanics of Scapulothoracic Motion
The serratus anterior protracts and upwardly rotates the scapula. Its direction of pull brings the inferomedial border of the scapula anteriorly. The inferior border of the scapula is pulled forward with forward elevation of the arm. This causes the glenoid to tip posteriorly and superiorly, allowing full forward elevation without impingement of the rotator cuff against the coracoacromial arch.
With weakness or paralysis of the serratus anterior muscle, the scapula translates superiorly and medially, and the inferior border rotates medially and dorsally. This disruption of the normal force couple between the serratus anterior and the trapezius severely limits the ability to elevate the arm past 90 degrees. The rationale for the pectoralis major transfer is to replicate the vector of the third division of the serratus anterior. By routing the sternal head of the pectoralis major to the inferior angle of the scapula, the surgeon restores the anterior and lateral pull required to stabilize the scapula against the thoracic wall and re-establish the fulcrum necessary for glenohumeral elevation.

Indications and Contraindications
Patient selection is paramount for achieving successful outcomes following pectoralis major transfer. The procedure is generally reserved for patients who have sustained a permanent or refractory long thoracic nerve injury and have failed exhaustive non-operative management. A minimum of 12 to 18 months of observation and physical therapy is recommended before surgical intervention, as spontaneous reinnervation can occur up to two years post-injury.

| Category | Specific Criteria |
|---|---|
| Operative Indications | Chronic long thoracic nerve palsy (> 12-18 months duration) without clinical or electromyographic improvement. |
| Severe, debilitating shoulder pain and fatigue secondary to periscapular muscle spasm and altered kinematics. | |
| Profound weakness in forward elevation and abduction directly attributable to loss of scapular stabilization. | |
| Failure of comprehensive conservative management (physical therapy, bracing, NSAIDs). | |
| Non-Operative Indications | Acute or subacute long thoracic nerve palsy (< 12 months duration). |
| Mild to moderate winging with acceptable functional compensation and minimal pain. | |
| Patients with high surgical risk or those unable to comply with strict postoperative rehabilitation protocols. | |
| Contraindications | Concomitant trapezius paralysis (spinal accessory nerve palsy), which requires a different reconstructive approach (e.g., Eden-Lange procedure). |
| Stiff shoulder or severe adhesive capsulitis (glenohumeral motion must be restored prior to tendon transfer). | |
| Generalized myopathy or progressive neuromuscular disease affecting the donor muscle. | |
| Medial pectoral nerve palsy or prior resection of the pectoralis major muscle. |
Pre Operative Planning and Patient Positioning
Clinical Evaluation and Diagnostics
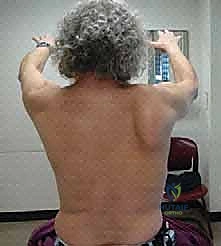
A meticulous clinical examination is required to differentiate medial winging from lateral winging. The classic "wall push test" involves the patient standing arm's length from a wall and pushing against it with both hands at shoulder height. In long thoracic nerve palsy, the medial border and inferior angle of the scapula will prominently lift off the thoracic wall.
Electromyography (EMG) and nerve conduction studies (NCS) are mandatory to confirm the diagnosis, localize the lesion, and rule out concurrent cervical radiculopathy, brachial plexopathy, or other peripheral nerve injuries. Sequential EMGs over a 12-month period are useful to document the absence of reinnervation potentials, thereby justifying surgical intervention. Advanced imaging, including MRI of the cervical spine and brachial plexus, may be indicated to rule out compressive lesions. MRI of the shoulder is also recommended to ensure the rotator cuff and glenohumeral joint are structurally intact, as occult pathology here will compromise the outcome of the transfer.

Patient Positioning and Setup
Proper patient positioning is critical to allow simultaneous access to the anterior chest wall (for pectoralis major harvest) and the posterior thorax (for scapular fixation). The lateral decubitus position is most commonly utilized. The patient is placed in the lateral decubitus position on a beanbag with the operative extremity facing upward.

The entire forequarter, including the anterior chest to the sternum, the axilla, the entire arm, and the posterior thorax to the spinous processes, must be prepped and draped free. This allows the arm to be manipulated intraoperatively to assess graft tension and scapular tracking. An axillary roll is placed under the contralateral axilla, and all bony prominences are meticulously padded. A sterile tourniquet is not used. Intravenous antibiotics are administered prior to incision.

Detailed Surgical Approach and Technique
Graft Selection and Preparation
Because the sternocostal head of the pectoralis major does not have sufficient length to reach the inferior angle of the scapula directly, an extension graft is required. Autologous fascia lata is the historical gold standard, providing excellent tensile strength and biological incorporation. However, the use of structural allografts, such as Achilles tendon, semitendinosus, or tensor fascia lata allografts, has become increasingly popular to avoid donor site morbidity. When using an Achilles allograft, the calcaneal bone block is removed, and the broad aponeurotic expansion is utilized to interface with the pectoralis major muscle belly.

Anterior Dissection and Pectoralis Major Harvest
The anterior incision is made along the anterior axillary fold, extending obliquely toward the sternum following the inferior border of the pectoralis major. The subcutaneous tissues are divided, and the deltopectoral fascia is identified. The interval between the clavicular and sternocostal heads of the pectoralis major is bluntly developed.

The sternocostal head is mobilized from its humeral insertion. Care must be taken to protect the long head of the biceps tendon and the coracobrachialis. The insertion of the sternocostal head is sharply detached from the humerus, tagging the tendinous stump with heavy non-absorbable traction sutures.
The muscle belly is then carefully elevated off the underlying pectoralis minor and chest wall. The neurovascular pedicle (medial and lateral pectoral nerves and the pectoral branch of the thoracoacromial artery) enters the deep surface of the muscle. Dissection must stop well medial to this pedicle to prevent denervation or devascularization of the transfer. Once mobilized, the prepared fascial graft is securely interwoven into the tendinous stump and muscle belly of the sternocostal head using a Pulvertaft weave or a robust modified Mason-Allen technique with heavy non-absorbable sutures.

Posterior Dissection and Scapular Preparation
A second incision is made vertically along the posterior axillary line, curving slightly medial toward the inferior angle of the scapula. Dissection is carried down through the subcutaneous tissues to expose the latissimus dorsi and the inferior angle of the scapula.

The latissimus dorsi is identified and mobilized. The optimal routing for the transfer is deep to the latissimus dorsi. This submuscular routing prevents unsightly bowstringing of the graft across the axilla and provides a more anatomical vector that closely mimics the native serratus anterior. A large blunt clamp or tunneler is passed from the posterior incision, deep to the latissimus dorsi, into the axilla to communicate with the anterior incision.

The inferior angle of the scapula is then prepared. The periosteum is elevated, and the bone is decorticated with a burr to create a bleeding bed that will promote graft-to-bone healing. Two or three transosseous drill holes are created through the inferior pole of the scapula. Alternatively, robust cortical suture anchors can be placed into the inferior angle, though transosseous fixation remains the biomechanical standard in many academic centers.

Graft Routing and Scapular Fixation
The traction sutures attached to the extension graft are passed through the sub-latissimus tunnel and retrieved in the posterior wound. The graft is pulled through, ensuring there are no twists and that the muscle belly of the pectoralis major glides smoothly into the axilla without tethering.

Setting the appropriate tension is the most critical step of the procedure. The patient's arm is placed in approximately 30 to 45 degrees of abduction and neutral rotation. An assistant applies a strong lateral and anterior force to the scapula, protracting it and holding it firmly against the chest wall in its anatomic position.
With the scapula reduced, the extension graft is pulled taut over the decorticated inferior angle. The heavy non-absorbable sutures are passed through the transosseous drill holes and tied securely. Additional sutures are used to sew the edges of the graft to the surrounding periosteum and the residual fascial stump of the serratus anterior to reinforce the repair. Once fixation is complete, the arm is gently moved to confirm that the scapula tracks smoothly and that the repair is stable under physiological tension.

The wounds are thoroughly irrigated. Closed suction drains are typically placed in both the anterior axillary space and the posterior scapular space to prevent hematoma formation. The subcutaneous tissues are closed in layers, and the skin is approximated with subcuticular sutures or staples. The patient is immediately placed into a specialized shoulder abduction brace before leaving the operating room.

Complications and Management
Surgical intervention for long thoracic nerve palsy is complex, and patients must be counseled regarding potential complications. The most devastating complication is failure of the transfer, which can occur due to graft rupture, pull-out from the scapula, or denervation of the donor muscle during harvest.
| Complication | Incidence / Risk Factors | Management and Salvage Strategies |
|---|---|---|
| Graft Rupture or Pull-out | 5-10%. Often due to non-compliance with postoperative immobilization or aggressive early physical therapy. | Revision surgery with robust allograft augmentation. If revision tendon transfer fails, scapulothoracic arthrodesis is the ultimate salvage procedure. |
| Neurovascular Injury | < 5%. Injury to the medial/lateral pectoral nerves during harvest leads to donor muscle atrophy. | Prevention is key via meticulous dissection. If denervation occurs, alternative transfers (e.g., split pectoralis minor or Eden- |
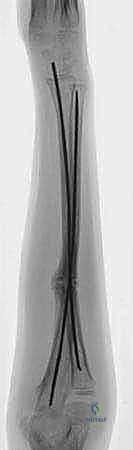
Clinical & Radiographic Imaging



















You Might Also Like