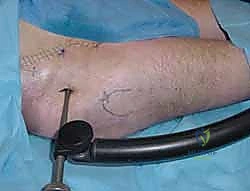
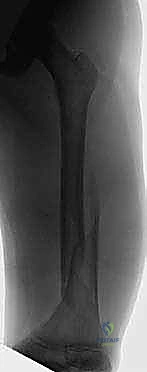
Pediatric Femur Fracture: Closed Reduction & Spica Casting Masterclass
Key Takeaway
Welcome to the OR, fellows. Today, we're tackling pediatric femur fractures with closed reduction and spica casting. This masterclass covers critical anatomy, meticulous preoperative planning, and a step-by-step intraoperative execution. We'll delve into precise patient positioning, reduction maneuvers, and casting techniques for both traditional and walking spicas, emphasizing crucial pearls to avoid complications and ensure optimal outcomes for our young patients.
Introduction and Epidemiology
Femoral shaft fractures in the pediatric population represent a significant orthopedic challenge, occurring with an estimated incidence of 20 per 100,000 children annually. These injuries constitute approximately 2% of all pediatric fractures. The distribution of pediatric femoral shaft fractures is classically bimodal, with peaks occurring in early childhood (toddlers) and mid-to-late adolescence. The etiology and required kinetic energy for fracture vary drastically across this age spectrum, dictating both the clinical index of suspicion for non-accidental trauma and the optimal treatment modality.
In the non-ambulatory infant or very young child presenting with a femoral shaft fracture, non-accidental trauma must be the primary differential consideration. Pathognomonic fracture patterns associated with abuse, such as classic metaphyseal lesions or corner fractures, may be absent; a spiral or transverse diaphyseal fracture in a child who is not yet walking is highly suspicious for abuse and mandates a thorough skeletal survey and pediatric protective services evaluation. Conversely, in a child presenting with a history of recurrent or multiple low-energy fractures, underlying metabolic or genetic osteodystrophies, predominantly osteogenesis imperfecta, must be rigorously evaluated. Osteogenesis imperfecta is frequently misdiagnosed as child abuse in the young demographic, requiring careful assessment of secondary clinical signs such as blue sclerae, dentinogenesis imperfecta, and family history.
In the polytraumatized pediatric patient, the femoral shaft fracture must be contextualized within the Advanced Trauma Life Support framework. The systemic burden of a femur fracture, while less hemodynamically destabilizing in children than in adults, still contributes to the systemic inflammatory response. Consequently, the nature and severity of concomitant head, thoracic, or abdominal injuries must dictate the timing and modality of femur stabilization to optimize overall survivability and functional recovery.
Surgical Anatomy and Biomechanics
The embryological development of the lower extremity begins with the limb bud at approximately four weeks of gestation. The femoral shaft serves as the primary ossification center. Secondary ossification centers emerge sequentially, with the proximal ossification center appearing by six months of age and the distal femoral ossification center visible by seven months. Understanding this timeline is critical for evaluating pediatric radiographs and avoiding the misinterpretation of normal physes or apophyses as traumatic pathology.
The pediatric femur is initially composed of weaker, highly cellular woven bone. Through the process of endochondral ossification and response to physiologic mechanical loading, this woven bone is gradually replaced by highly organized lamellar bone throughout childhood. This structural transition correlates with the exponential increase in the biomechanical force required to fracture the femur as the child ages.
The vascular anatomy of the pediatric femur is robust, supplied by both endosteal and periosteal circulations. The profunda femoris artery gives rise to four distinct perforating arteries that penetrate the femur posteromedially, supplying the endosteal network. While the endosteal circulation provides the majority of the resting blood supply to the intact diaphysis, the hemodynamic dominance shifts dramatically during fracture healing. Following a fracture, the hypervascular periosteal circulation becomes the primary source of osteoprogenitor cells and blood flow, driving the rapid, exuberant callus formation characteristic of pediatric fractures. This robust periosteal response is also the primary driver of the well-documented phenomenon of post-traumatic femoral overgrowth.

Deforming Muscular Forces
The position of the fracture fragments post-injury is reliably dictated by the predictable pull of regional musculature. Understanding these deforming forces is essential for executing a successful closed reduction and applying an effective spica cast mold.
* Proximal Third Fractures: The proximal fragment is driven into flexion by the iliopsoas, abduction by the gluteus medius and minimus, and external rotation by the short external rotators. The distal fragment is pulled proximally and into adduction by the adductor complex.
* Middle Third Fractures: The proximal fragment remains flexed, while the adductor longus and brevis exert a strong medial pull on the distal fragment, typically resulting in a varus deformity with apex lateral angulation.
* Distal Third Fractures: The distal fragment is driven into apex posterior angulation (extension) by the robust pull of the gastrocnemius muscle originating from the posterior femoral condyles, while the adductor magnus contributes to varus malalignment.
Indications and Contraindications
The management of pediatric femur fractures is highly algorithm-driven, primarily based on the patient's age, weight, and fracture morphology. Closed reduction and early spica casting remains the gold standard for children aged 6 months to 4 or 5 years, provided the fracture is isolated and length is relatively maintained. The goal of spica casting is to harness the thick pediatric periosteum and rapid healing potential to achieve union while accepting and managing expected overgrowth.
Contraindications to closed reduction and spica casting include severe polytrauma requiring frequent patient mobilization, massive soft tissue compromise, open fractures requiring serial debridement, and profound head injuries where spasticity may compromise cast immobilization. Additionally, excessive initial shortening (typically greater than 2.5 to 3 cm) that cannot be reduced may necessitate operative intervention to prevent unacceptable leg length discrepancies.
| Parameter | Indications for Closed Reduction and Spica Casting | Indications for Operative Fixation |
|---|---|---|
| Age | 6 months to 5 years | Less than 6 months (Pavlik harness) or Greater than 5 years (Flexible/Rigid Nailing) |
| Weight | Less than 20 kg | Greater than 20 kg |
| Fracture Pattern | Isolated diaphyseal fracture | Polytrauma, open fracture, floating knee |
| Shortening | Less than 2 cm of initial shortening | Greater than 2.5 to 3 cm of irreducible shortening |
| Soft Tissue | Intact soft tissue envelope | Severe soft tissue injury, burns, or impending compartment syndrome |
| Neurologic Status | Normal baseline tone | Severe spasticity or traumatic brain injury |

Pre Operative Planning and Patient Positioning
Thorough preoperative clinical and radiographic evaluation is mandatory. The clinician must meticulously inspect the lower extremity for open wounds, which dramatically alter the treatment algorithm. The thigh typically presents with significant swelling, ecchymosis, and obvious clinical deformity. Shortening is frequently present and must be quantified clinically and radiographically.
A rigorous neurovascular examination is critical. The clinician must palpate the femoral, popliteal, dorsalis pedis, and posterior tibial pulses. Diminished pulses necessitate immediate evaluation with a continuous-wave Doppler and may indicate vascular entrapment or evolving compartment syndrome. Compartments must be palpated for tension. While compartment syndrome of the thigh is rare due to the large volume of the fascial compartments, it can occur, particularly in high-energy crush injuries. Sensation to light touch and motor function (ankle dorsiflexion and plantarflexion) must be documented to rule out sciatic or peroneal nerve neurapraxia.
Orthogonal radiographic views of the entire femur, including the hip and knee joints, are required to rule out ipsilateral femoral neck fractures or physeal injuries.
Anesthesia and Operating Room Setup
Closed reduction and spica casting should be performed under general anesthesia to ensure complete muscle relaxation. Conscious sedation in the emergency department is generally inadequate for overcoming the robust deforming forces of the pediatric thigh musculature and often results in suboptimal reductions and poorly molded casts.
Patient positioning is arguably the most critical step in the procedure. The patient is transferred to a specialized pediatric spica table. The sacrum is supported on a well-padded sacral rest, and the perineum is positioned snugly against the perineal post. The upper torso is supported by the table extension. Bilateral lower extremities are secured in traction boots or wrapped with traction tape.

Detailed Surgical Approach and Technique
The objective of closed reduction and spica casting is to achieve acceptable alignment while anticipating the physiologic overgrowth that occurs in the 18 to 24 months following a pediatric femur fracture. Acceptable radiographic parameters for children aged 2 to 5 years include up to 15 degrees of varus or valgus angulation, 20 degrees of anterior or posterior bowing, and 15 to 20 millimeters of shortening. Rotational malalignment does not remodel reliably and must be anatomically corrected.
Reduction Maneuvers
With the patient positioned on the spica table, longitudinal traction is applied to overcome the shortening and muscular spasm. The amount of traction should be titrated using intraoperative fluoroscopy. The goal is to achieve approximately 1 to 1.5 cm of overriding (shortening) in the acute setting, as this will compensate for the anticipated 1.5 to 2 cm of overgrowth. Distracting the fracture fragments anatomically or leaving them in a distracted position will inevitably lead to an unacceptable leg length discrepancy with the injured leg being longer.
For proximal third fractures, the hip must be flexed and abducted to align the distal fragment with the flexed and abducted proximal fragment. For midshaft fractures, careful attention must be paid to correcting the varus deformity.
Spica Cast Application
Once acceptable alignment is confirmed fluoroscopically, cast application begins.
1. Skin Protection A high-quality stockinette is applied over the torso, extending from the nipple line to the ankles bilaterally. A waterproof, breathable liner (such as Gore-Tex) is highly recommended for the perineal region to minimize urine and feces soiling, which is the leading cause of premature cast failure and skin breakdown.
2. Padding Cast padding is applied generously over bony prominences, specifically the anterior superior iliac spines, the sacrum, the greater trochanters, the patellae, and the heels. Care must be taken not to over-pad the diaphyseal regions, as this will compromise the mechanical hold of the cast and allow loss of reduction.
3. Positioning The classic "90-90" spica cast position involves 90 degrees of hip flexion and 90 degrees of knee flexion. This position relaxes the iliopsoas and gastrocnemius muscles, neutralizing the primary deforming forces. Furthermore, it prevents the child from bearing weight and facilitates seating in specialized car seats and highchairs. The hip is abducted approximately 30 degrees, and external rotation is matched to the contralateral uninjured limb to ensure rotational alignment.
4. Casting Material Fiberglass is preferred over plaster of Paris due to its superior strength-to-weight ratio, radiolucency, and durability. The cast is applied starting from the torso (nipple line) and extended down the injured leg to the transmalleolar region or toes, depending on surgeon preference. The contralateral leg is typically incorporated down to just above the knee (a "one-and-a-half" spica) to lock the pelvis and prevent rotational loss of reduction.
5. Molding While the fiberglass is curing, the surgeon must apply specific, targeted molds. A supracondylar mold is applied to control rotation and length. An anterior bow mold is applied to the thigh to recreate the normal anatomic sagittal contour of the femur and prevent apex anterior angulation. A valgus mold is often necessary to counteract the strong adductor forces that drive the fracture into varus.

Once the cast is cured, the perineal area is trimmed to allow adequate space for diapering and hygiene. The edges are petaled with waterproof tape to prevent skin irritation. Final orthogonal fluoroscopic images are obtained to confirm maintenance of reduction within the cast.

Complications and Management
While closed reduction and spica casting is highly successful, it is not without significant potential complications. Meticulous technique and rigorous postoperative surveillance are required to mitigate these risks.
Loss of Reduction
Loss of reduction is the most common orthopedic complication, occurring in up to 10-15% of cases. It is most frequently caused by the resolution of acute swelling within the cast, allowing the limb to piston or angulate. Serial radiographic monitoring is essential. If unacceptable angulation or shortening occurs within the first two weeks, the cast must be wedged or removed entirely for a repeat closed reduction. Beyond three weeks, the fracture callus is typically too rigid for closed manipulation, and osteotomy or acceptance of the deformity (relying on remodeling potential) must be considered.
Skin Complications
Skin breakdown, maceration, and ulceration occur due to pressure over bony prominences or chemical irritation from trapped urine and feces. The incidence of skin complications can be drastically reduced by utilizing waterproof liners, proper padding techniques, and extensive caregiver education regarding diapering and cast hygiene. Severe ulcers may require cast windowing or premature cast removal and transition to alternative immobilization.
Superior Mesenteric Artery Syndrome
Superior Mesenteric Artery Syndrome (Cast Syndrome) is a rare but potentially life-threatening complication characterized by acute mechanical obstruction of the third portion of the duodenum by the superior mesenteric artery. It is precipitated by the application of a tight body jacket or spica cast, combined with prolonged supine positioning and potential weight loss. Clinical presentation includes intractable vomiting, abdominal distension, and severe discomfort. Immediate management requires univalving or bivalving the abdominal portion of the cast, nasogastric decompression, and intravenous fluid resuscitation.
| Complication | Estimated Incidence | Pathophysiology and Risk Factors | Salvage and Management Strategies |
|---|---|---|---|
| Loss of Reduction | 10% - 15% | Subsidence of swelling, inadequate molding, poor initial reduction. | Early: Cast wedging or repeat closed reduction. Late: Observation for remodeling vs corrective osteotomy. |
| Skin Breakdown | 5% - 10% | Pressure necrosis over prominences, urine/feces maceration. | Prevention via waterproof liners. Treatment via cast windowing, local wound care, or cast change. |
| Leg Length Discrepancy | 5% - 20% | Overgrowth (hyperemia) or unacceptable initial shortening. | Shoe lifts for minor discrepancies. Epiphysiodesis of the longer limb near skeletal maturity for discrepancies > 2 cm. |
| Malunion | 2% - 5% | Failure to maintain reduction, unrecognized rotational deformity. | Spontaneous remodeling for sagittal/coronal plane. Derotational osteotomy for severe rotational malunion. |
| SMA Syndrome | Less than 1% | Duodenal compression by the superior mesenteric artery. | Immediate cast modification (bivalving), NG tube decompression, IV hydration, pediatric surgery consult. |
Post Operative Rehabilitation Protocols
The postoperative phase is heavily reliant on caregiver compliance and education. Prior to discharge, caregivers must be thoroughly instructed on cast hygiene, diapering techniques within the spica, and safe lifting mechanics. Specialized car seats are frequently required, as standard child safety seats cannot accommodate the abducted hip positioning of a spica cast.
Clinical and radiographic follow-up is typically scheduled at 1 week, 3 weeks, and 6 weeks post-reduction. The 1-week and 3-week visits are critical for obtaining anteroposterior and lateral radiographs to ensure maintenance of reduction.
Spica casts are generally removed at 5 to 6 weeks post-injury, depending on the child's age and radiographic evidence of bridging callus on at least three out of four cortices. Upon cast removal, the child will exhibit significant stiffness in the hip and knee, and a temporary limp is universally expected. Physical therapy is rarely indicated in the young pediatric population, as normal play and ambulation will naturally restore full range of motion and strength over the subsequent 4 to 8 weeks. Caregivers should be counseled that the child may refuse to bear weight initially and should be allowed to resume activity at their own pace. High-impact activities and contact sports should be restricted for an additional 4 to 6 weeks following cast removal to prevent refracture.
Summary of Key Literature and Guidelines
The management of pediatric femur fractures is supported by robust clinical practice guidelines. The American Academy of Orthopaedic Surgeons (AAOS) Clinical Practice Guideline for the Treatment of Pediatric Diaphyseal Femur Fractures strongly recommends early spica casting for children aged 6 months to 5 years with isolated fractures and less than 2 cm of shortening.
Historically, treatment involved prolonged periods of skeletal or skin traction followed by spica casting. However, landmark studies over the past two decades have definitively demonstrated that early application of a spica cast (within 24 hours of injury) significantly reduces hospital length of stay, lowers healthcare costs, and provides equivalent or superior clinical outcomes compared to delayed casting after traction.
Furthermore, literature regarding femoral overgrowth dictates the current reduction parameters. Studies tracking leg length discrepancies post-fracture have consistently shown that the injured femur will overgrow by an average of 1.5 to 2.0 cm in the two years following the injury, driven by the hyperemic periosteal response. Therefore, achieving an anatomic, end-to-end reduction is technically a malreduction that will predictably lead to a leg length discrepancy. The evidence-based best practice requires the surgeon to intentionally leave the fracture shortened by 1.5 cm within the cast to allow for this physiologic overgrowth, ensuring equal leg lengths at skeletal maturity.
Clinical & Radiographic Imaging





You Might Also Like