Pediatric Orthopaedic Masterclass: Advanced Techniques & Anatomical Precision
Key Takeaway
Welcome, fellows, to an immersive intraoperative masterclass in pediatric orthopaedics. We'll navigate complex anatomical landscapes and refine surgical techniques for diverse conditions, from hip dysplasia and long bone osteotomies to intricate foot and hand reconstructions. Our focus: meticulous dissection, precise instrument handling, and proactive complication management, ensuring optimal outcomes for our young patients. Prepare for a deep dive into critical surgical anatomy and advanced procedural execution.
Introduction to Pediatric Orthopaedic Surgical Principles
Alright, fellows, gather 'round. Welcome to the operating theater. Today, we're not just performing one specific surgery; rather, we're going to embark on an intensive masterclass, dissecting critical principles and advanced techniques across various pediatric orthopaedic domains. Think of this as a rapid-fire tour of complex anatomy and precise execution, drawing from scenarios you’ll encounter in hip preservation, long bone deformity correction, foot and ankle reconstruction, hand surgery, and even intricate spinal approaches. My goal is to imbue you with the mindset of a master surgeon – one who anticipates, executes with precision, and mitigates complications before they arise. Let's scrub in.
Preoperative Planning: The Blueprint for Success
Before we even consider an incision, meticulous preoperative planning is paramount, especially in our pediatric population where growth potential and unique anatomical variations dictate our approach.
- Imaging Review: Beyond standard radiographs, we often utilize CT scans with 3D reconstructions for complex deformities, particularly in hip dysplasia, severe foot deformities, or spinal anomalies. MRI helps delineate soft tissue structures, growth plates, and neurovascular bundles.
- Templating: For procedures involving hardware (e.g., K-wires, Fassier-Duval nails, osteotomy fixation), precise templating on radiographs ensures correct size and trajectory, minimizing intraoperative guesswork. We'll pre-plan K-wire entry points and trajectories, especially for epiphyseal fixation or guide wire placement in proximal femur cases.
- Fluoroscopy Setup: For almost all our cases today, fluoroscopy will be our indispensable intraoperative guide. We'll ensure the C-arm is positioned for optimal orthogonal views without impinging on the sterile field. For hip cases, this means AP and lateral views of the proximal femur and pelvis. For foot corrections, weight-bearing simulations can be invaluable.
- Patient Positioning: This is not a trivial step. It dictates our access, prevents iatrogenic injury, and optimizes fluoroscopic imaging. We'll discuss specific positioning for each segment of our masterclass.
Module 1: Proximal Femur and Hip Preservation Techniques
Let's begin with the hip, a common site of significant pathology in pediatrics, from developmental dysplasia to avascular necrosis. Today, we'll focus on techniques for guide wire placement and considerations for reconstructive procedures like shelf arthroplasty.
Patient Positioning and Surgical Approach for Hip Access
For hip procedures, we typically position the patient supine on a radiolucent table, often with a bump under the ipsilateral hip to facilitate access and allow for full range of motion. The affected leg is draped free to allow for intraoperative manipulation and fluoroscopic imaging.
Comprehensive Surgical Anatomy: Anterior Hip Approach
For procedures requiring access to the anterior hip capsule, such as a shelf arthroplasty or open reduction, a thorough understanding of the anterior hip anatomy is non-negotiable.
- Superficial Landmarks: The anterior superior iliac spine (ASIS) and pubic tubercle are key. The inguinal ligament stretches between them.
- Muscular Intervals:
- Sartorius: Originates from the ASIS, runs inferomedially.
- Tensor Fasciae Latae (TFL): Originates from the ASIS and outer lip of the iliac crest, runs distally to the IT band.
- Rectus Femoris: Has two heads – a direct head from the ASIS and an indirect (reflected) head from the ilium just superior to the acetabulum. This reflected head is often a barrier to capsular access.
- Iliopsoas Muscle: Formed by the iliacus and psoas major, it passes deep to the inguinal ligament. The Psoas tendon inserts onto the lesser trochanter. This muscle group is a primary hip flexor and can be a source of impingement or contracture in certain hip pathologies.
- Neurovascular Structures (Femoral Triangle):
- Femoral Nerve: Lies most lateral, typically within the iliopsoas groove.
- Femoral Artery: Central, palpable pulse.
- Femoral Vein: Medial to the artery.
- Femoral Sheath: Encloses the artery and vein, and lymphatics, but not the femoral nerve.
- Hip Capsule: A strong fibrous capsule enclosing the joint, reinforced by ligaments.
Intraoperative Execution: Hip Guide Wire Placement and Shelf Arthroplasty Principles
Let's imagine we're placing a guide wire for a slipped capital femoral epiphysis (SCFE) or a femoral head osteotomy, and then we'll transition to a shelf arthroplasty.
-
Incision and Superficial Dissection (for Hip Capsule Access):
- We'll make an anterior Smith-Petersen type incision, extending from the ASIS distally, typically between the sartorius and tensor fasciae latae.
- Carefully incise the skin and subcutaneous tissue. Identify and ligate any superficial bleeders.
- Identify the interval: Retract the sartorius medially and the TFL laterally. This exposes the rectus femoris.
- Addressing the Rectus Femoris: To gain optimal access to the hip capsule, we often need to release the origin of the reflected head of rectus femoris. Use a monopolar cautery or scalpel to carefully divide this tendinous attachment from its origin on the ilium, just superior to the acetabulum. This allows the rectus femoris to be retracted distally, significantly improving exposure.
-
Capsular Exposure and K-wire Placement:
- Once the rectus femoris is mobilized, the anterior hip capsule is exposed.
- K-wire Insertion (from tip of trochanter to center of femoral head):
- For a guide wire, say for SCFE, we will make a small stab incision over the lateral aspect of the greater trochanter, aiming for the physis or the center of the femoral head.
- Fluoroscopic guidance is absolutely critical here. We'll obtain true AP and lateral views of the hip.
- Technique: Insert a 2.0 mm or 2.5 mm K-wire. The entry point is typically just distal to the vastus lateralis ridge on the lateral femoral cortex. Angle the wire superiorly and medially.
- Drill under constant fluoroscopic guidance. Advance the K-wire slowly, watching its trajectory in both planes. We want it to be centered in the femoral neck and terminate just short of the articular cartilage of the femoral head.
- Sclerotic bone: In cases of chronic SCFE or avascular necrosis, you might encounter sclerotic bone. This is denser, harder bone. Use a sharper K-wire tip and apply steady, consistent pressure. Do not force it, as this can lead to bending or breakage. If resistance is too high, consider pre-drilling with a small drill bit, but always under fluoroscopic control.
- Cartilage: Ensure the K-wire does not penetrate the articular cartilage. This can cause chondrolysis and long-term joint damage. The K-wire should be subchondral.
- Bone Bump: If you encounter a bone bump (e.g., an osteophyte or prominent bone) that impedes your trajectory, a small osteotome or a Kerrison rongeur can be used to carefully remove it, again, with caution to protect surrounding structures.
- Principles of Shelf Arthroplasty (for Hip Dysplasia):
- This is a reconstructive procedure to improve acetabular coverage of the femoral head.
- Exposure: After adequate exposure of the hip capsule and superior acetabular rim, we identify the displaced ilium.
- Capsulotomy: A capsulotomy is performed to visualize the femoral head and acetabulum.
- Creating the Shelf: A trough is created in the ilium superior to the acetabulum. This is where the bone graft will be placed. The graft, often autogenous from the iliac crest or allograft, is shaped to create a new, extended acetabular roof.
- Fixation: The bone graft is placed on top of the shelf. It is then meticulously secured. We use sutures of the shelf to capsule to help stabilize the graft and reinforce the capsular integrity, creating a buttress. The sutures are placed through drill holes in the graft and then through the anterior hip capsule, pulling the capsule over the graft.
Pearls and Pitfalls: Hip Procedures
- Neurovascular Injury: Always be mindful of the femoral nerve, artery, and vein, especially during initial incision and deep dissection. Retract structures gently.
- K-wire Skiving: A K-wire can skive off hard cortical bone. Start with a sharp tip and ensure a stable purchase.
- Growth Plate Injury: In pediatric patients, avoid damaging the physis with K-wires unless it's the intended target (e.g., SCFE fixation).
- Intra-articular Penetration: Verify K-wire position in multiple fluoroscopic views. If doubt exists, consider an arthrogram or pulling back slightly.
- Inadequate Coverage (Shelf Arthroplasty): Ensure the bone graft provides sufficient coverage. If not, revision or alternative procedures may be necessary.
Postoperative Management: Hip
- Weight-Bearing: Often restricted or protected weight-bearing (e.g., toe-touch) for 6-12 weeks, depending on the stability of fixation and the procedure performed (e.g., K-wire fixation vs. shelf arthroplasty).
- Range of Motion (ROM): Gradual, protected ROM exercises are initiated, avoiding extremes of motion that could stress the repair.
- DVT Prophylaxis: Age and procedure-dependent, but always considered.
Module 2: Long Bone Osteotomies and Nailing (Osteogenesis Imperfecta Context)
Now, let's pivot to long bone deformity correction, particularly relevant in conditions like Osteogenesis Imperfecta (OI), where multiple percutaneous osteotomies and Fassier-Duval telescoping nailing are common. While the raw text doesn't detail the nailing, it mentions osteotomies and K-wires, which are fundamental.
Preoperative Planning & Patient Positioning
- Planning: Detailed templating of osteotomy sites and nail length/diameter is crucial. We mark planned osteotomy levels on the skin preoperatively.
- Positioning: The patient is typically supine or prone, depending on the bone, on a radiolucent table allowing full access for fluoroscopy. The limb is prepped and draped free.
Intraoperative Execution: Percutaneous Osteotomies
The concept of "Cut 1, Cut 2, Cut 3" from the raw image refers to planned osteotomy sites, likely for deformity correction or to facilitate intramedullary nailing. These are often performed percutaneously to minimize soft tissue stripping.
- Incision: Small stab incisions (e.g., 1-2 cm) are made over the planned osteotomy sites.
- Soft Tissue Protection: Use hemostats or small retractors to protect nerves and vessels. A periosteal elevator can be used to create a small window in the periosteum.
- Osteotomy:
- Technique: A small osteotome, Gigli saw, or specialized percutaneous osteotomy device is used.
- Fluoroscopic Guidance: Absolutely essential. Confirm the osteotomy level and ensure it's complete without damaging the opposite cortex or adjacent structures.
- Controlled Fracture: For some deformities, a controlled greenstick fracture or complete osteotomy is performed to allow for realignment.
- K-wire as a Guide: K-wires can be temporarily inserted across the osteotomy site to maintain alignment while other osteotomies are performed or the nail is inserted.
Pearls and Pitfalls: Long Bone Osteotomies
- Neurovascular Injury: Be acutely aware of the course of major nerves and vessels, especially when performing percutaneous osteotomies. For example, in the tibia, the anterior tibial artery and deep peroneal nerve are at risk anteriorly, and the posterior tibial artery and tibial nerve posteriorly.
- Incomplete Osteotomy: Can lead to uncontrolled fracture patterns during reduction or nailing. Verify completeness with fluoroscopy.
- Soft Tissue Impingement: Ensure no soft tissues are caught within the osteotomy site during reduction.
- Malalignment: Repeated fluoroscopic checks in AP and lateral planes are needed to confirm correct alignment after osteotomies and before definitive fixation.
Postoperative Management: Long Bones
- Weight-Bearing: Typically non-weight bearing or protected weight-bearing for 6-12 weeks, depending on the stability of fixation and bone healing.
- Bracing/Casting: External immobilization (casts or orthoses) may be used in conjunction with intramedullary nails, especially in OI patients, to protect the limb and facilitate healing.
- Physical Therapy: Gradual ROM and strengthening exercises once stability is achieved.
Module 3: Elbow Fracture and Arthroscopy Principles
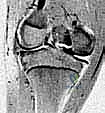
Let's shift our focus superiorly to the elbow. The image shows a brachialis muscle, fracture, brachial artery, median nerve, 90º flexion, arthroscope, and K-wire. This suggests an elbow fracture, potentially managed with arthroscopy and K-wire fixation.
Preoperative Planning & Patient Positioning
- Planning: Detailed imaging (X-rays, CT) to characterize the fracture pattern.
- Positioning: Patient supine, arm abducted on a hand table, or prone with arm suspended. For arthroscopy, the arm is often suspended in a traction tower or held by an assistant at 90º of elbow flexion to open the joint space.
Comprehensive Surgical Anatomy: Anterior Elbow
- Brachialis Muscle: Originates from the anterior surface of the humerus, inserts onto the coronoid process and ulnar tuberosity. It's a primary elbow flexor.
- Brachial Artery: Runs anterior to the elbow joint, deep to the biceps aponeurosis. It's the major arterial supply to the forearm.
- Median Nerve: Runs parallel to the brachial artery, medial to it at the elbow, passing through the cubital fossa. It innervates most forearm flexors and some hand muscles.
- Radial Nerve: Lies more laterally, dividing into superficial and deep branches.
- Ulnar Nerve: Runs posterior to the medial epicondyle in the cubital tunnel.
Intraoperative Execution: Elbow Arthroscopy and K-wire Fixation Principles
Imagine we're dealing with an intra-articular elbow fracture, perhaps a capitellar fracture, where arthroscopy can aid reduction and K-wire fixation.
- Arthroscopic Portals:
- Standard portals include anterolateral, anteromedial, posterolateral, and direct posterior.
- Fluid Management: Maintain constant irrigation to distend the joint and clear debris.
- Visualization: Use the arthroscope to inspect the joint, identify the fracture, and remove any loose bodies or hematoma.
- Fracture Reduction:
- Using arthroscopic instruments (probes, graspers), meticulously reduce the fracture fragments.
- The 90º elbow flexion helps to stabilize the joint and open the posterior compartment for visualization and instrument access.
- K-wire Fixation:
- Once reduced, a K-wire is inserted percutaneously under fluoroscopic and/or arthroscopic guidance to temporarily or definitively fix the fracture.
- Technique: The K-wire is drilled across the fracture line, ensuring stable purchase in both fragments. Avoid penetrating the articular surface or damaging neurovascular structures.
- Brachial artery and Median nerve: These are critical anterior structures. Any K-wire insertion from the anterior aspect must be done with extreme caution, often requiring open visualization or careful blunt dissection to protect these structures.
Pearls and Pitfalls: Elbow Procedures
- Neurovascular Injury: The brachial artery and median nerve are highly vulnerable, especially during anterior approaches or K-wire insertion. Always use blunt dissection and careful retraction.
- Stiffness: The elbow is prone to stiffness. Early, controlled motion is key postoperatively.
- Infection: Arthroscopy minimizes incision size but carries a risk of infection.
- Incomplete Reduction: Arthroscopy can aid visualization, but complex fractures may still require open reduction for optimal alignment.
Postoperative Management: Elbow
- Immobilization: Short-term splinting or casting for pain control and initial stability (e.g., 2-4 weeks).
- Range of Motion: Early, protected ROM exercises are initiated to prevent stiffness, often supervised by a physical therapist.
- K-wire Removal: Typically performed in the clinic once radiographic union is evident.
Module 4: Foot and Ankle Reconstruction
Let's move distally to the foot and ankle, where complex deformities often require precise osteotomies and tendon transfers. The image highlights the medial malleolus, lateral malleolus, distal incision, gastrocnemius muscle, sural nerve, superior peroneal nerve, soleus muscle, tibialis posterior tendon (split), peroneus brevis tendon, Cut 1, Cut 2, Cut 3, Meary's angle 25°, Calcaneal pitch angle 26°. This suggests procedures for flatfoot or cavus foot correction.
Preoperative Planning & Patient Positioning
- Planning: Weight-bearing radiographs are essential to measure angles like Meary's angle (normal 0-10°) and Calcaneal pitch angle (normal 20-30°). A Meary's angle of 25° and a Calcaneal pitch angle of 26° suggest a degree of flatfoot deformity or a foot with altered arch. CT scans help assess bony deformities.
- Positioning: Patient prone for posterior ankle/calf access, or supine with a bump under the hip for medial/lateral ankle access. A tourniquet is typically used.
Comprehensive Surgical Anatomy: Ankle and Calf
- Posterior Calf:
- Gastrocnemius Muscle: Superficial, two heads, originates from femoral condyles, inserts via Achilles tendon.
- Soleus Muscle: Deep to gastrocnemius, originates from tibia/fibula, inserts via Achilles tendon.
- Conjoined Tendon: Refers to the Achilles tendon, formed by gastrocnemius and soleus.
- Sural Nerve: Arises from tibial and common peroneal nerves, runs subcutaneously along the posterior calf, supplies sensation to the lateral foot. It's often retracted with skin during posterior approaches.
- Lateral Ankle:
- Peroneus Brevis Tendon: Inserts onto the base of the 5th metatarsal. Lies deep to the peroneus longus.
- Superior Peroneal Nerve (Superficial Fibular Nerve): Runs superficial to the peroneus muscles, supplies sensation to the dorsum of the foot. It's vulnerable during lateral ankle approaches.
- Lateral Malleolus: Distal fibula.
- Medial Ankle:
- Tibialis Posterior Tendon: Originates from tibia/fibula, passes behind the medial malleolus, inserts onto navicular and cuneiforms. A crucial arch support.
- Medial Malleolus: Distal tibia.
Intraoperative Execution: Foot Reconstruction (Osteotomies & Tendon Transfers)
Let's consider a flatfoot correction, involving osteotomies and potentially tendon work.
-
Incision Planning:
- Distal incision: For posterior ankle access, a longitudinal incision is made along the posterior midline.
- Medial incision: For access to the tibialis posterior tendon or medial osteotomies, a curvilinear incision just posterior to the medial malleolus is made.
- Lateral incision: For access to the peroneus brevis tendon or lateral osteotomies, an incision anterior or inferior to the lateral malleolus is made.
-
Posterior Ankle Dissection:
- Incision through skin and subcutaneous tissue.
- Identify and protect the sural nerve, which is often retracted with skin and subcutaneous fat laterally.
- Incise the deep fascia to expose the gastrocnemius muscle and soleus muscle.
- The tendon of gastrocnemius (Achilles) is identified. If a gastrocnemius recession is needed, the aponeurosis of the gastrocnemius is released.
- The soleus muscle can be retracted or released from its origin to expose deeper structures if needed for posterior osteotomies.
-
Tendon Procedures:
- Tibialis Posterior Tendon (split): In severe flatfoot, the tibialis posterior tendon may be lengthened or augmented. Sometimes, it is split longitudinally, and one half is transferred to a different insertion (e.g., lateral cuneiform) to augment the arch.
- Peroneus Brevis Tendon: This tendon may be lengthened or transferred in certain foot deformities.
-
Osteotomies (Cut 1, Cut 2, Cut 3):
- These cuts represent precise bony resections or realignments to correct the foot angles.
- Calcaneal Osteotomies: Often performed to shift the calcaneus medially (medializing calcaneal osteotomy) to correct hindfoot valgus. This involves a cut through the calcaneus, typically from lateral to medial, under fluoroscopic guidance.
- Midfoot Osteotomies: To correct midfoot collapse or severe Meary's angle. These can be wedge osteotomies (dorsal opening or closing) of the navicular or cuneiforms.
- Forefoot Osteotomies: To address forefoot abduction or adduction.
- Execution: Use a small osteotome or oscillating saw. Ensure cuts are complete and precise.
- Fluoroscopic Guidance: Constantly verify the alignment and completeness of the osteotomies. After the cuts, the foot is manipulated to achieve the desired correction, and provisional K-wires are placed for temporary fixation.
Pearls and Pitfalls: Foot & Ankle
- Neurovascular Injury: The sural nerve, superficial peroneal nerve, posterior tibial neurovascular bundle are all at risk during various approaches. Meticulous dissection and retraction are crucial.
- Over/Under Correction: Precise measurements and intraoperative fluoroscopy are essential to achieve the desired angular correction (e.g., restoring Meary's angle to neutral, adjusting calcaneal pitch angle).
- Nonunion/Malunion: Inadequate fixation or poor bone quality can lead to these complications.
- Tendon Imbalance: Incorrect tensioning or positioning of tendon transfers can lead to new deformities.
Postoperative Management: Foot & Ankle
- Immobilization: Non-weight bearing cast for 6-8 weeks, followed by a walking cast or boot.
- Weight-Bearing: Gradual progression of weight-bearing over several months.
- Physical Therapy: Intensive physical therapy to restore strength, flexibility, and gait mechanics, especially after tendon transfers.
Module 5: Hand Flap Reconstruction
Moving to the upper extremity, let's briefly touch upon hand reconstruction, specifically the principles of flap creation for soft tissue coverage, as indicated by digital midlines, volar flap based on long finger, dorsal flap based on ring finger, DIP, PIP, 1/3 2/3, MCP. This is often seen in syndactyly release or complex trauma.
Preoperative Planning & Patient Positioning
- Planning: Detailed mapping of the defect and potential donor sites. Trace the flap outlines preoperatively.
- Positioning: Patient supine, arm on a hand table, tourniquet applied.
Comprehensive Surgical Anatomy: Hand and Digits
- Digital Midlines: Imaginary lines that divide the volar and dorsal aspects of the digits. Flaps are often designed to cross these lines to prevent scar contracture.
- DIP, PIP, MCP: Distal interphalangeal, proximal interphalangeal, and metacarpophalangeal joints, respectively. Key landmarks for flap design and joint function.
- Volar and Dorsal Skin: Different characteristics; volar skin is thicker, more sensate, and less mobile.
- Neurovascular Bundles: On the radial and ulnar sides of each digit, containing digital nerves and arteries.
Intraoperative Execution: Flap Design and Elevation
Imagine we are releasing a syndactyly between the long and ring fingers, requiring both volar and dorsal flaps.
- Tourniquet Inflation: Exsanguinate the limb and inflate the tourniquet.
- Incision and Flap Design:
- Digital Midlines: The incisions are carefully designed along or slightly off the digital midlines to maximize flap length and prevent contracture.
- **Volar
You Might Also Like