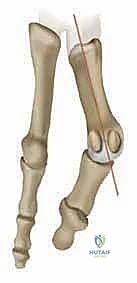
Calcaneonavicular Coalition Resection: An Adult Surgical Masterclass with EDB Interposition
Key Takeaway
This masterclass guides orthopaedic fellows through calcaneonavicular coalition resection in adult patients. We cover comprehensive anatomy, meticulous preoperative planning, and a step-by-step intraoperative execution of the Ollier approach with extensor digitorum brevis interposition. Emphasis is placed on neurovascular protection, precise osteotomy, and managing potential complications for optimal outcomes.
Alright fellows, gather 'round. Today, we're addressing a fascinating, albeit often challenging, condition: the symptomatic calcaneonavicular coalition in an adult patient. While frequently identified in adolescents, a subset of adults presents with significant pain and dysfunction, often after a traumatic event. Our goal is to meticulously resect this abnormal bony bridge and restore hindfoot mechanics, alleviating pain and improving function. This isn't just about removing bone; it's about understanding the intricate anatomy, respecting soft tissues, and preventing recurrence.
Understanding the Calcaneonavicular Coalition: Anatomy and Pathogenesis
Before we make an incision, let's review the fundamental principles. A tarsal coalition is an abnormal fusion between two adjacent tarsal bones, a developmental anomaly stemming from a failure of segmentation of the primitive mesenchyme. Unlike other tarsal coalitions, which often involve joint surfaces, the calcaneonavicular coalition forms between two bones that normally do not articulate with each other.
Specifically, this coalition typically occurs between the anterior process of the calcaneus and the inferolateral aspect of the navicular. Histologically, these coalitions can be fibrous, cartilaginous, or osseous, often progressing through these stages as the patient matures. In adults, we typically encounter a more ossified, rigid bridge.
Clinical Presentation and Natural History
Adult patients with symptomatic calcaneonavicular coalitions commonly present with hindfoot or midfoot pain, recurrent ankle sprains, and difficulty ambulating on uneven surfaces. Unlike the often insidious onset in adolescents, symptoms in adults can be abrupt, frequently coinciding with a specific traumatic event like a severe ankle sprain, which may "tip" a previously asymptomatic coalition into a painful state.
The natural history is one of progressive disability. As the coalition ossifies, the lack of subtalar range of motion imposes increased stresses on the remaining mobile tarsal joints, potentially leading to degenerative arthritic changes elsewhere in the foot. You might also see a planovalgus foot deformity, or, less commonly, a cavovarus deformity, due to the biomechanical alterations. Tenderness directly over the coalition and pain with attempted hindfoot inversion or eversion are classic physical examination findings.
Preoperative Planning: The Blueprint for Success
Effective preoperative planning is paramount. It allows us to anticipate challenges, define our surgical strategy, and ensure we have all the necessary tools at hand.
Diagnostic Imaging Review
We start by thoroughly reviewing all available imaging.
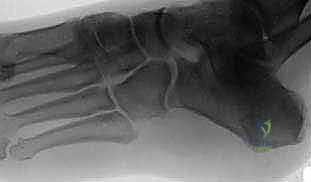
* Plain Radiographs: These are our first line. We obtain AP, lateral, 45-degree oblique, and axial views of the foot.
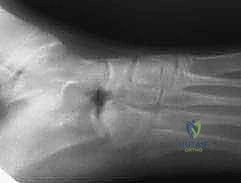
* The 45-degree oblique view is the workhorse for identifying a calcaneonavicular coalition. You might see a discrete bony bridge, or, more subtly, an extended, narrow beak of bone projecting from the anterior process of the calcaneus towards the navicular – this is the classic "anteater sign."
* Axial View: Crucial for ruling out a concomitant talocalcaneal coalition, which would significantly alter our surgical plan.
* Computed Tomography (CT) Scans: Absolutely essential in all adult patients preoperatively. CT provides a detailed 3D roadmap of the coalition, allowing us to:
* Precisely delineate the extent and morphology of the bony bridge.
* Rule out any concomitant talocalcaneal coalitions, which are often missed on plain films.
* Evaluate for degenerative changes in adjacent joints (e.g., subtalar, talonavicular, calcaneocuboid). Significant degenerative changes might contraindicate simple resection and necessitate a primary arthrodesis.
* Magnetic Resonance Imaging (MRI): While useful for identifying fibrous or cartilaginous coalitions, it's generally not necessary for the workup of most adult calcaneonavicular coalitions, which are typically ossified. However, if there's suspicion of soft tissue pathology or other occult lesions, an MRI can be helpful.
Differential Diagnosis
Always keep a broad differential in mind:
* Talocalcaneal (subtalar) coalition
* Trauma or fracture of the hindfoot
* Arthritis (primary osteoarthrosis, post-traumatic arthritis, or inflammatory arthritis)
* Flatfoot secondary to posterior tibial tendon insufficiency
* Chronic ankle instability
Nonoperative Management
Remember, fellows, surgery is reserved for patients who fail an adequate trial of nonoperative management. This typically includes:
* Nonsteroidal anti-inflammatory medications (NSAIDs)
* Custom orthotics that support the medial longitudinal arch, such as a UCBL brace, to limit hindfoot motion.
* If initial measures fail, immobilization in a fiberglass short leg walking cast for 4 to 6 weeks.
Only symptomatic coalitions recalcitrant to these conservative measures, and in feet displaying no significant degenerative changes, are candidates for surgical resection.
Patient Positioning and Pre-Surgical Setup
Now, let's get our patient ready.
Prophylactic Antibiotics
Thirty to ninety minutes before we make our incision, the patient receives an appropriate intravenous antibiotic. This is standard practice to minimize the risk of surgical site infection.
Operating Room Setup
- OR Table: We'll be using a standard operating table.
- Patient Position: The patient is placed supine. This allows for excellent access to the lateral aspect of the foot.
- Bump Placement: Crucially, we place a small bump under the ipsilateral sacrum. This maneuver helps to internally rotate the foot, presenting the lateral aspect of the hindfoot more effectively to us, improving our ergonomic access and visualization.
- Tourniquet: A pneumatic tourniquet is placed around the upper thigh. This will allow us to create a bloodless field, which is essential for identifying delicate neurovascular structures and for precise osteotomy.
- Prep and Drape: The extremity is prepped and draped in a standard, sterile fashion, ensuring a wide sterile field that extends well above the ankle.
Fluoroscopy Setup
We'll need a C-arm in the room, positioned to allow for immediate AP and lateral views of the foot. This will be critical for confirming the adequacy of our resection. Ensure the C-arm can be brought in and out easily without compromising the sterile field.
Comprehensive Surgical Anatomy: A Refresher
Let's quickly review the critical anatomy we'll encounter during our approach.
- Osteology:
- Calcaneus: Specifically, its anterior process, which forms the posterior component of the coalition.
- Navicular: The inferolateral aspect, forming the anterior component.
- Talus: Superior to the calcaneus, forming the subtalar joint. We must avoid violating this joint.
- Cuboid: Lateral to the navicular, articulating with the anterior calcaneus.
- Muscular Intervals & Soft Tissues:
- Extensor Digitorum Brevis (EDB) Muscle: This muscle originates from the anterior aspect of the calcaneus and inserts into the toes. It lies directly in our surgical field. We will be elevating this as a distally based flap and later using it for interposition.
- Peroneal Tendons: The peroneus longus and brevis tendons run along the lateral malleolus and then along the lateral aspect of the calcaneus, deep to the EDB. We must identify and protect them.
- Extensor Digitorum Longus (EDL) Tendons: These tendons run dorsally, lateral to which our incision will extend.
- Neurovascular Structures: This is where we must be most vigilant.
- Sural Nerve: This purely sensory nerve runs superficially along the posterolateral aspect of the ankle and foot. It's highly susceptible to injury during lateral approaches.
- Dorsal Intermediate Cutaneous Branch of the Superficial Peroneal Nerve: This branch also provides sensation to the dorsum of the foot and can be in our field.
- Small Cutaneous Vessels: Numerous small vessels will be encountered in the subcutaneous layer. Pre-emptive cauterization is key to maintaining a clear field.
Surgical Warning: Nerve injury is a significant complication. Always identify and protect the sural nerve and superficial peroneal nerve branches. Blunt dissection and careful retraction are your allies.
Step-by-Step Intraoperative Execution: The Masterclass
Alright, fellows, let's begin. Tourniquet is inflated, the field is sterile, and we're ready to proceed.
1. Incision and Initial Exposure
We'll use a standard Ollier incision. This is a curvilinear incision centered directly over the dorsal aspect of the coalition.
- Landmarks: It extends along a transverse Langer line, plantarly to the peroneal tendon sheath and dorsally to the most lateral of the extensor digitorum longus tendons. We want it to be about 4-5 cm in length, but adjust based on the patient's anatomy and the extent of the coalition.
- Execution: Make a precise incision through the skin.
- Subcutaneous Dissection: Now, carefully deepen the incision through the subcutaneous tissues.
- Pre-emptive Cauterization: As we proceed, pre-emptively cauterize any crossing vessels to minimize bleeding and maintain a clear view.
- Nerve Identification and Protection: This is critical. Use careful, blunt dissection to identify and protect the sural cutaneous nerve and the dorsal intermediate branch of the superficial peroneal nerve. Gently retract them superiorly or inferiorly, away from our working area.
- Peroneal Tendons: Continue dissecting deep, and you'll visualize the peroneal tendons (peroneus longus and brevis) running along the lateral aspect of the calcaneus. These also need to be identified and protected, usually retracted inferiorly.
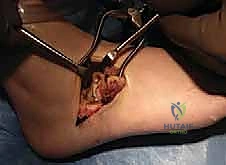
2. Extensor Digitorum Brevis (EDB) Flap Elevation
Once the nerves and tendons are safely retracted, our next key structure is the EDB muscle.
- Visualization: The extensor digitorum brevis muscle is visualized in the depths of the wound, originating from the anterior calcaneus.
- Flap Elevation: Using a scalpel and a Cobb elevator, carefully elevate the EDB as a distally based flap.
- Crucial Technique: Take great care to preserve the overlying fascia. This fascia is vital; it will significantly increase the suture-holding capacity of our flap later, preventing pull-out.
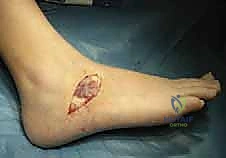
- Suture Placement: Once the origin of the brevis is adequately elevated, we'll grasp it with a modified Mason-Allen stitch using a 0-Vicryl suture. This will allow us to manipulate and later interpose the flap.
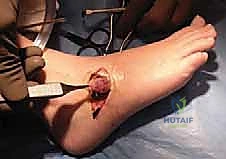
- Coalition Visualization: As we retract the EDB flap distally, the calcaneonavicular coalition should now be easily identified, lying beneath the muscle belly.
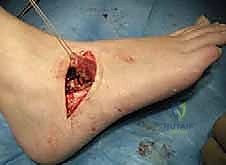
3. Resection of the Calcaneonavicular Coalition
With the coalition clearly visible, we proceed with its resection. Our goal is to remove the entire abnormal bridge, creating a sufficiently wide gap to prevent recurrence.
- Initial Osteotomy: After confirming adequate visualization, take a straight osteotome. We aim to remove a 1-cm block of bone, ensuring it includes the entire coalition.
- Parallel Cuts: This is a critical technical point. Make your osteotome cuts parallel to each other.
-
Surgical Pitfall: If your cuts converge, you'll remove a trapezoidal block, leaving an inadequate medial excision. This can lead to recurrent pain due to residual coalition or early re-ossification. Keep those cuts parallel to create a rectangular void.
-
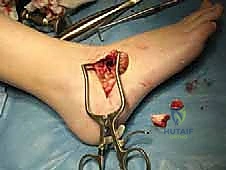
- Completion of Resection: Once the bone block is free, carefully extract it.
- Debridement: Use a rongeur to clear any remaining fibrous or cartilaginous soft tissue within the resection site. We want clean, bleeding bone edges.
- Fluoroscopic Confirmation: Now, bring in the C-arm. Obtain AP and lateral radiographs to confirm the adequacy of the resection. We are looking for a clear, wide gap between the calcaneus and navicular, ensuring no residual coalition.
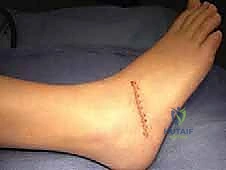
* > **Surgical Pearl:** If there's any doubt about the resection, go back in. An inadequate resection is a primary cause of recurrence.
4. Interposition of the Extensor Digitorum Brevis Flap
To prevent recurrence, we must interpose a soft tissue barrier. The EDB flap is ideal for this.
- Flap Passage: Take the two limbs of the previously placed Vicryl suture attached to the EDB flap. Using a free Keith needle, pass these two limbs through the void created by the coalition resection.
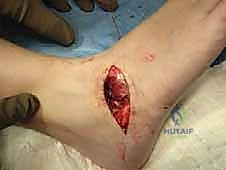
- Exit Point: The tips of the Keith needles should pass just dorsal to the glabrous skin of the medial arch. Be careful not to damage the skin excessively.
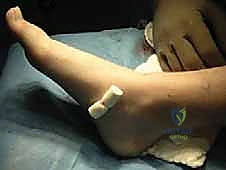
- Securing the Flap: Once the sutures are passed, tie the two limbs of the Vicryl suture over a soft dental bolster (no button). This provides gentle, even pressure, holding the EDB flap firmly within the resection void.

- Alternative Interposition: If for some reason the EDB flap is not viable or sufficient, alternative methods include covering the raw bony surfaces with bone wax, or filling the void with Gelfoam or an autologous fat graft. Then, the brevis can be reattached to its origin. However, the EDB flap is generally preferred due to its robust nature and biological barrier effect.
5. Wound Closure and Dressing
We're nearing the end of the procedure.
- Irrigation and Hemostasis: Thoroughly irrigate the wound with sterile saline to remove any bone dust or debris. Then, release the tourniquet. We must achieve meticulous hemostasis before closing to prevent hematoma formation, which can increase infection risk and cause pain.
- Deep Closure: Close the deep subcutaneous layer using 2-0 Vicryl sutures.
- Skin Closure: For the skin, we'll use 4-0 nylon horizontal mattress sutures. These provide good eversion and strength.
- Dressing: Apply a nonadherent dressing directly over the incision, followed by sterile gauze, sterile cast padding, and finally, a short leg fiberglass walking cast. This cast provides immediate immobilization and protection.
Pearls and Pitfalls: Navigating the Challenges
Let's consolidate some critical points, fellows. These are the lessons learned from experience.
- Preoperative Imaging Review: Always review CT or MRI scans for concomitant coalitions or significant degenerative changes. Missing these can lead to surgical failure.
- Osteotome Cuts: Always make parallel osteotome cuts. A convergent, trapezoidal resection will inevitably lead to an inadequate medial excision and likely recurrence. Aim for a 1 cm rectangular block.
- EDB Flap Preservation: Preserve the fascia overlying the extensor digitorum brevis. This is crucial for the holding power of your Vicryl stitch and the long-term viability of your interpositional graft.
- Deformity Correction: In the face of a significant pes planus deformity, consider adding a lateral column lengthening procedure (e.g., Evans osteotomy) at the same time. Simply resecting the coalition might not adequately address the underlying biomechanical issues if a severe flatfoot is present. This is a judgment call based on the patient's overall foot alignment and symptoms.
- Neurovascular Protection: The sural nerve and superficial peroneal nerve branches are highly vulnerable. Always identify, visualize, and protect them with careful blunt dissection and gentle retraction.
- Inadequate Resection: This is the most common reason for recurrence. Be aggressive but precise. Use fluoroscopy to confirm a wide, clear gap.
Postoperative Care and Rehabilitation
Our job isn't done until the patient is successfully rehabilitated.
Immediate Postoperative Period
- Weight Bearing: The patient is allowed to weight bear as tolerated in the cast on postoperative day 1. This early mobilization, within the protection of the cast, helps with pain management and reduces the risk of stiffness.
- Pain Management: Ensure adequate pain control with a multimodal approach.
- DVT Prophylaxis: Standard DVT prophylaxis protocols should be followed.
Follow-up and Cast Removal
- 3 Weeks Postoperatively: The patient returns to the clinic.
- We will remove the short leg cast, the skin sutures, and the dental bolster stitch.
- At this point, the patient is transitioned into a walking boot.
- Physical Therapy Initiation: Immediately following cast removal, physical therapy is initiated. The focus will be on:
- Ankle and hindfoot range-of-motion (ROM) exercises: Gentle, progressive exercises to restore motion.
- Strengthening: Gradually introduce strengthening exercises for the foot and ankle musculature.
- Gait Training: Re-education on proper gait mechanics.
Long-Term Rehabilitation
- Boot Weaning: The patient will typically remain in the walking boot for another 3-4 weeks, gradually weaning out of it as pain allows and strength improves.
- Return to Activity: Full return to activity is gradual, usually taking 3-6 months, depending on the individual and the demands of their lifestyle.
Complications and Outcomes
Even with meticulous technique, complications can occur. It's crucial to be aware of them and know how to manage them.
Potential Complications
- Superficial or Deep Infection:
- Management: Superficial infections may respond to oral antibiotics and local wound care. Deep infections often require surgical debridement, intravenous antibiotics, and potentially hardware removal if an arthrodesis was performed. Prophylactic antibiotics and strict sterile technique are our best prevention.
- Wound Dehiscence:
- Management: Minor dehiscence can be managed with local wound care. Significant dehiscence may require secondary closure or skin grafting. Ensure tension-free closure and proper postoperative wound care.
- Recurrence of the Coalition: This is a major concern, particularly if the resection was inadequate or if interposition was not performed.
- Management: If symptomatic, recurrence may necessitate revision surgery, potentially with a wider resection and robust interposition, or even a primary arthrodesis (e.g., triple arthrodesis) if significant degenerative changes have developed. Mitchell and Gibson's work highlighted a high recurrence rate (nearly two-thirds) in patients who underwent simple resection without EDB interposition, emphasizing its importance.
- Nerve Damage: Injury to the sural or superficial peroneal nerves can lead to chronic neuropathic pain, numbness, or paresthesias.
- Management: Initial management is conservative, with nerve blocks, NSAIDs, and neuropathic pain medications. If severe and persistent, nerve repair or neurolysis may be considered, though outcomes can be variable. Prevention through careful identification and protection is key.
- Inadequate Resection: As discussed, this leads to persistent symptoms and recurrence.
- Management: Revision surgery with more aggressive and precise resection.
- Reflex Sympathetic Dystrophy (RSD) / Complex Regional Pain Syndrome (CRPS): A rare but debilitating complication characterized by chronic pain, swelling, and autonomic dysfunction.
- Management: Early recognition and aggressive multidisciplinary treatment involving pain management specialists, physical therapy, and sometimes stellate ganglion blocks or other interventions.
Outcomes
In the absence of significant degenerative changes that may necessitate an appropriate arthrodesis, resection of a calcaneonavicular coalition with EDB interposition can be a highly successful procedure in symptomatic adults or adolescents. Patients typically experience significant pain relief, improved hindfoot motion, and enhanced functional capacity, allowing them to ambulate on uneven surfaces with greater ease and confidence.
This procedure, when performed meticulously, offers a viable pathway to restoring function and alleviating chronic pain for these challenging patients. Always remember, fellows, attention to detail, comprehensive anatomical knowledge, and careful execution are the hallmarks of a successful outcome. Any questions?
REFERENCES
-
Cohen BE, Davis WH, Anderson RB. Success of calcaneonavicular coalition resection in the adult population. Foot Ankle Int 1996;17: 569–572.
-
Cooperman DR, Janke BE, Gilmore A, et al. A three-dimensional study of calcaneonavicular tarsal coalitions. J Pediatr Orthop 2001; 21:648–651.
-
Ehrlich MG, Elmer EB. Tarsal coalition. In: Jahss M, ed. Disorders of the Foot and Ankle, ed
-
Philadelphia: Saunders, 1991:921–938.
-
Gonzalez P, Kumar SJ. Calcaneonavicular coalition treated by resection and interposition of the extensor digitorum brevis muscle. J Bone Joint Surg Am 1990;72A:71–77.
-
Jayakumar S, Cowell HR. Rigid flatfoot. Clin Orthop Relat Res 1977;122:77–84.
-
Kulik SA, Clanton TO. Foot fellow’s review: tarsal coalition. Foot Ankle Int 1996;17:286–296.
-
Mitchell GP, Gibson JMC. Excision of calcaneonavicular bar for painful spasmodic flatfoot. J Bone Joint Surg Br 1967;49B:281–287.
-
Moyes ST, Crawford EJP, Aichroth PM. The interposition of extensor digitorum brevis in the resection of calcaneonavicular bars. J Pediatr Orthop 1994;14:387–388.
-
Swiontkowski MF, Scranton PE, Hansen S. Tarsal coalitions: longterm results of surgical treatment. J Pediatr Orthop 1983;3:287–292.
-
Vincent KA. Tarsal coalition and painful flatfoot. J Am Acad Orthop Surg 1998;6:274–281.
-
Cohen et al reviewed results of calcaneonavicular coalition resection in 12 adult patients. Subjective relief was attained in 10 patients and the average increase in total subtalar range of motion was 10 degrees. 1
-
In a group of 48 child and adolescent patients, Gonzalez and Kumar achieved 77% good to excellent results following calcaneonavicular coalition resection with interposition of the extensor digitorum brevis. The results did not deteriorate with time in those patients followed up for more than 10 years. 4
-
The importance of using an interpositional material has been reinforced in several publications.
-
No recurrences of a calcaneonavicular coalition were noted by Moyes et al on oblique radiographs when an extensor digitorum brevis interposition was performed. However, in this same study, three of seven patients who underwent resection without interposition displayed radiographic evidence of a recurrence. 8
-
Swiontkowski et al used an interpositional material (fat or muscle) in 38 of 39 feet undergoing calcaneonavicular coalition resection and found no radiographic recurrences. 9

You Might Also Like