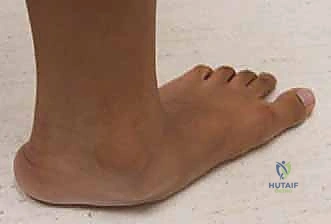
Bridge Plating for High-Energy Distal Radius Fractures: An Intraoperative Masterclass
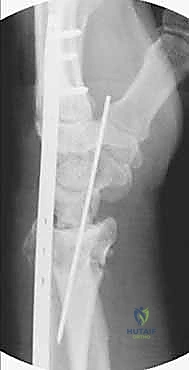
Key Takeaway
This masterclass guides fellows through bridge plating high-energy distal radius fractures. We cover detailed surgical anatomy, meticulous preoperative planning, and a step-by-step intraoperative execution, emphasizing indirect reduction and plate insertion techniques. Crucial pearls on avoiding neurovascular injury, managing intra-articular fragments, and assessing DRUJ stability are discussed. Postoperative care and complication management ensure comprehensive understanding for optimal patient outcomes.
Introduction and Epidemiology
High-energy fractures of the distal aspect of the radius with extensive comminution of the articular surface and extension into the diaphysis represent a major treatment challenge in orthopedic trauma. Standard volar or dorsal locking plates and conventional osteosynthesis techniques may be inadequate for the management of such complex fracture patterns. Before the introduction of the bridge plating technique, also known as internal distraction plating, treatment of these severe injuries was primarily limited to cast immobilization or external fixation with or without Kirschner wire augmentation. Both of these historical methods are associated with unacceptably high complication rates, including pin tract infections, loss of reduction, pin loosening, and complex regional pain syndrome.

The advent of bridge plating fundamentally altered the management of these challenging fractures. By functioning as an "internal external fixator," a spanning plate utilizes the principles of ligamentotaxis to maintain radial length, alignment, and rotation while bypassing the zone of severe comminution. This technique is particularly critical for two distinct subsets of patients: those with high-energy wrist injuries featuring fracture extension into the radial diaphysis, and polytraumatized patients who require immediate load-bearing through the injured extremity to assist with mobilization, crutch ambulation, and intensive nursing care.
Epidemiologically, these high-energy fractures typically present in a bimodal distribution, though the severe comminution necessitating bridge plating is most frequently observed in younger patients involved in motor vehicle collisions, falls from significant heights, or industrial accidents. The natural history of comminuted distal radius fractures treated by closed methods is poor; the end results reliably resemble the prereduction radiographs more than any subsequent imaging during treatment, even when the initial reduction successfully restores wrist anatomy. Functional outcome scores in patients without anatomic or near-anatomic reduction are demonstrably inferior, leading to chronic pain, stiffness, weak grip strength, and carpal instability. Long-term consequences include degenerative radiocarpal and midcarpal arthritis in up to 50 percent of patients with even minimal articular displacement in the young adult population. Consequently, surgical intervention utilizing spanning techniques ensures more consistent correction of displacement and maintenance of reduction.
Surgical Anatomy and Biomechanics
A profound understanding of the osseous and ligamentous anatomy of the distal radius and carpus is mandatory for the successful application of a bridge plate. The articular surface of the distal radius is tilted 21 degrees in the anteroposterior plane (radial inclination) and 5 to 11 degrees in the lateral plane (volar tilt). Normal radial height averages 11 to 12 millimeters relative to the distal ulna.

The dorsal cortex surface of the radius thickens to form the tubercle of Lister, which serves as a critical surgical landmark and acts as a pulley for the extensor pollicis longus tendon. A central ridge divides the articular surface of the radius into a scaphoid facet and a lunate facet. Because of the differential areas of bone thickness and trabecular density, fractures tend to occur in the relatively weaker metaphyseal bone and propagate intra-articularly between the scaphoid and lunate facets. The degree, direction, and magnitude of applied load may cause coronal or sagittal splits within the lunate or scaphoid facets, frequently creating independent volar and dorsal ulnar corner fragments that dictate the stability of the distal radioulnar joint.

Biomechanically, bridge plating relies on the concept of stress shielding and ligamentotaxis. Unlike standard volar locking plates that directly buttress the subchondral bone and require intact cortical contact for load sharing, a spanning plate bypasses the metaphyseal defect entirely. The plate is fixed proximally to the intact radial diaphysis and distally to the stable metacarpal shaft (typically the second or third metacarpal). Longitudinal traction applied during plate fixation tensions the strong volar radiocarpal ligaments (such as the radioscaphocapitate and long radiolunate ligaments), which indirectly reduces the articular fragments.
This construct effectively neutralizes axial loading, bending, and torsional forces. In the polytrauma patient, the spanning plate acts as a robust load-bearing device. Biomechanical studies have demonstrated that a 3.5mm dorsal spanning plate provides superior resistance to axial compression compared to external fixation, allowing patients to safely bear weight through the wrist for platform crutch or walker use without catastrophic loss of reduction or hardware failure.
Indications and Contraindications
The decision to utilize a bridge plate rather than standard non-spanning internal fixation hinges on the degree of metaphyseal comminution, the presence of diaphyseal extension, and the patient's overall physiologic and trauma status.

Primary indications include highly comminuted intra-articular fractures where standard screw purchase in the distal fragments is impossible, fractures with significant diaphyseal extension that preclude the use of standard distal radius plates, and severe radiocarpal fracture-dislocations with extensive ligamentous instability. Furthermore, polytrauma patients with concurrent lower extremity injuries who require upper extremity weight-bearing for mobilization are prime candidates for this robust fixation method.
Contraindications are generally relative but require careful consideration. Active local infection is an absolute contraindication. Pre-existing severe radiocarpal arthritis may make the procedure less desirable unless a subsequent total wrist arthrodesis is already planned. Fractures that can be adequately reduced and stably fixed with a standard volar or dorsal non-spanning plate should be treated as such to avoid the necessity of a secondary surgery for plate removal and to allow immediate post-operative wrist mobilization.
| Clinical Scenario | Operative Strategy | Rationale and Considerations |
|---|---|---|
| High-Energy Comminution with Diaphyseal Extension | Bridge Plating | Bypasses zone of injury; standard plates lack proximal fixation length. |
| Polytrauma Requiring Upper Extremity Weight Bearing | Bridge Plating | Construct provides sufficient biomechanical stability for crutch/walker use. |
| Simple Intra-articular Fracture with Adequate Bone Stock | Standard Volar Locking Plate | Allows immediate wrist ROM; avoids secondary removal surgery. |
| Severe Open Fracture with Gross Contamination | External Fixation | Minimizes deep hardware placement in contaminated field; allows soft tissue management. |
| Elderly Patient with Low-Demand Wrist | Standard Plate or Closed Reduction | Bridge plating may lead to unacceptable stiffness in this demographic. |
Pre Operative Planning and Patient Positioning
Thorough preoperative evaluation is essential for successful bridge plating. A complete history must detail the mechanism of injury, as axial loading forces typically produce the high-energy fracture patterns requiring this technique. Physical examination must rigorously evaluate the soft tissue envelope to rule out open fractures and assess for signs of impending compartment syndrome. Median nerve dysfunction from acute carpal tunnel syndrome is common in severely displaced fractures and must be clearly documented; prophylactic or therapeutic carpal tunnel release may be indicated concurrently.

Good-quality pre- and postreduction wrist radiographs (posteroanterior, lateral, and oblique views) must be obtained to assess the fracture pattern, measure radial height and inclination, and rule out associated injuries to the carpus or distal radioulnar joint. Computed tomography scans are highly recommended and often considered mandatory to assess complex intra-articular distal radius fractures. Axial, coronal, and sagittal reconstructions assist in identifying specific fragment locations, such as a depressed central die-punch fragment or a malrotated volar lunate facet, which may require limited open reduction or percutaneous pinning prior to the application of the spanning plate.

For patient positioning, the patient is placed supine on the operating table with the affected extremity extended on a radiolucent hand table. A pneumatic tourniquet is applied to the proximal arm. The C-arm fluoroscopy unit is positioned parallel to the arm board, entering from the distal or lateral aspect to allow unhindered anteroposterior and lateral visualization of the entire radius, carpus, and metacarpals. Prophylactic intravenous antibiotics are administered prior to tourniquet inflation. The surgeon must ensure that appropriate implants, typically 2.4mm or 3.5mm dorsal spanning plates, are available in various lengths.
Detailed Surgical Approach and Technique
The application of a bridge plate demands meticulous soft tissue handling and a precise understanding of the extensor compartments of the wrist to prevent iatrogenic tendon injury. The dorsal spanning technique utilizing the second or third metacarpal is the most widely accepted method.

Proximal Incision and Radial Dissection
A longitudinal incision is made over the dorsal aspect of the distal radial diaphysis, typically centered over Lister's tubercle and extending proximally. The superficial branch of the radial nerve and the lateral antebrachial cutaneous nerve must be identified and protected during the superficial dissection. The extensor retinaculum is exposed, and the third extensor compartment is opened longitudinally. The extensor pollicis longus tendon is identified, mobilized, and transposed radially or ulnarly.
Preparation of the Extensor Compartments
To create a safe pathway for the spanning plate, subperiosteal elevation of the second extensor compartment (containing the extensor carpi radialis longus and brevis) and the fourth extensor compartment (containing the extensor digitorum communis and extensor indicis proprius) is performed. The plate will ultimately reside on the floor of these compartments, directly against the dorsal cortex of the radius, deep to the extensor tendons. This submuscular and sub-retinacular placement is critical to minimize tendon attrition and rupture.

Distal Incision and Metacarpal Exposure
A second longitudinal incision is made dorsally over the shaft of the chosen metacarpal—either the second or the third. The choice between the second and third metacarpal depends on surgeon preference and fracture morphology. Using the third metacarpal provides a more central mechanical axis and aligns well with Lister's tubercle, whereas the second metacarpal avoids the extensor carpi radialis brevis insertion and may be technically easier to access. The dorsal interosseous fascia is incised, and the extensor tendons are retracted to expose the bare area of the metacarpal diaphysis.
Articular Reduction and Provisional Fixation
Before the spanning plate is secured, the articular surface must be addressed. Longitudinal traction is applied to utilize ligamentotaxis. If CT imaging identified depressed articular fragments, a limited arthrotomy or percutaneous joysticks (Kirschner wires) may be used to elevate and reduce the joint surface. Bone graft or orthobiologics can be packed into metaphyseal voids to support the articular reduction. Provisional fixation with independent K-wires or headless compression screws is often necessary to secure the articular block before the spanning plate locks the wrist in distraction.

Plate Insertion and Proximal Fixation
A specialized spanning plate (often pre-contoured with a slight dorsal bend to accommodate the carpus and wrist extension) is introduced through the proximal incision and advanced distally deep to the extensor retinaculum, emerging in the distal metacarpal incision. Alternatively, it can be passed from distal to proximal. Fluoroscopy is used to confirm the plate is centered on the radial diaphysis and the metacarpal shaft.

The plate is first secured to the proximal radial diaphysis using non-locking or locking cortical screws, ensuring at least three bicortical screws (six cortices) are placed for adequate proximal purchase.
Distal Fixation and Final Construct Tensioning
Once proximal fixation is achieved, longitudinal traction is applied to the digits to restore radial length and correct volar tilt. The wrist is typically positioned in neutral to slight extension (10 to 15 degrees). While maintaining this reduction and traction, the plate is secured to the metacarpal shaft using bicortical screws. Fluoroscopy must confirm the restoration of the radiocarpal and midcarpal joint spaces, ensuring the wrist is not over-distracted, which can lead to severe postoperative stiffness and complex regional pain syndrome. The extensor retinaculum is left open over the transposed extensor pollicis longus, and the wounds are meticulously closed in layers.

Complications and Management
While bridge plating provides robust fixation for complex fractures, it is associated with a specific profile of complications. The most significant complications arise from the hardware's interaction with the dorsal soft tissue envelope and the prolonged immobilization of the radiocarpal joint.
Extensor tendon irritation or rupture is a known complication, particularly involving the extensor pollicis longus or the extensor digitorum communis. This typically occurs if the plate is not adequately seated beneath the extensor retinaculum or if distal screws are excessively long, prominent, or impinging on the tendons. Meticulous surgical technique, proper plate sizing, and subperiosteal placement are the primary preventative measures.
Hardware failure, including plate breakage or screw pullout, is rare but can occur in noncompliant patients or polytrauma patients who overload the construct before adequate callus formation.
Complex regional pain syndrome and severe postoperative stiffness are risks inherent to prolonged wrist immobilization. Over-distraction of the carpus during plate application significantly increases the risk of these complications. The surgeon must carefully evaluate intraoperative fluoroscopy to ensure the radiocarpal joint space is symmetric and not widened compared to the uninjured contralateral side.

| Complication | Estimated Incidence | Pathophysiology and Risk Factors | Management and Salvage Strategies |
|---|---|---|---|
| Extensor Tendon Rupture | 2% - 5% | Hardware prominence; inadequate sub-retinacular placement; EPL attrition. | Tendon transfer (e.g., EIP to EPL); hardware removal; tenolysis. |
| Complex Regional Pain Syndrome | 5% - 10% | Over-distraction of radiocarpal joint; severe initial trauma; median nerve injury. | Aggressive occupational therapy; gabapentinoids; stellate ganglion blocks. |
| Hardware Failure | < 2% | Premature excessive weight-bearing; inadequate screw purchase in osteopenic bone. | Revision ORIF; conversion to external fixation; bone grafting. |
| Nonunion or Delayed Union | 1% - 3% | Severe devascularization of metaphyseal fragments; large un-grafted bone voids. | Plate retention; autologous bone grafting; consideration of shortening osteotomy. |
| Post-Traumatic Arthritis | 20% - 50% | Initial articular cartilage damage; failure to anatomically reduce articular step-offs. | Conservative management (NSAIDs, bracing); partial or total wrist fusion. |
Post Operative Rehabilitation Protocols
The postoperative rehabilitation protocol for a patient with a bridge plate differs significantly from that of standard volar plating due to the intentional immobilization of the radiocarpal and midcarpal joints.
In the immediate postoperative phase (0 to 2 weeks), the focus is on edema control, wound healing, and immediate mobilization of the un-immobilized joints. Patients are instructed to perform aggressive active range of motion exercises for the fingers, thumb, elbow, and shoulder. Preventing metacarpophalangeal joint stiffness is paramount, as the distal plate fixation on the metacarpal can tether the extensor mechanism if adhesions form.
During the intermediate phase (2 to 12 weeks), the plate remains in situ. For polytrauma patients, weight-bearing through the upper extremity using platform walkers or crutches is permitted as dictated by their concurrent lower extremity injuries. Occupational therapy continues to focus on composite fist formation and independent digit motion.

Unlike standard internal fixation implants, the bridge plate is a temporary device that mandates surgical removal to restore wrist kinematics. Plate removal is typically scheduled between 12 and 16 weeks postoperatively, contingent upon radiographic evidence of clinical union across the metaphyseal defect. Following hardware removal, a rigorous rehabilitation protocol is initiated to restore wrist flexion, extension, pronation, and supination. Patients often experience significant initial stiffness, and maximal medical improvement regarding range of motion may not be achieved until 6 to 12 months following plate removal.
Summary of Key Literature and Guidelines
The evolution of bridge plating is well-documented in orthopedic literature, shifting the paradigm for high-energy distal radius fractures. The use of internal distraction plating for distal radius fractures was originally introduced and popularized by Burke and colleagues, who recognized the limitations of external fixation in maintaining length and alignment without the high incidence of pin tract morbidity.
Subsequent landmark studies, such as those by Ruch et al., demonstrated the biomechanical superiority and favorable clinical outcomes of dorsal spanning plates in highly comminuted intra-articular fractures. Their work highlighted that internal distraction provides a stable environment for metaphyseal healing while allowing immediate digit mobilization.
Hanel and colleagues further expanded the indications by demonstrating the safety and efficacy of bridge plating in the polytraumatized patient. Their retrospective reviews confirmed that the spanning construct could withstand the cyclical loading associated with crutch ambulation without hardware failure or loss of reduction, a critical advantage over standard osteosynthesis.
Lafontaine et al. established the classic criteria for instability in distal radius fractures (dorsal angulation >20 degrees, dorsal comminution, intra-articular radiocarpal extension, associated ulnar fracture, and patient age >60 years). Modern guidelines dictate that fractures meeting three or more of these criteria, particularly when associated with diaphyseal extension or high-energy axial loads, are highly unstable and strongly warrant consideration for bridge plating to prevent the inevitable collapse associated with lesser forms of fixation.
Current academic consensus and trauma guidelines support the use of bridge plating as an indispensable tool in the orthopedic surgeon's armamentarium. While it requires a secondary procedure for hardware removal, the reliable restoration of radial anatomy, the prevention of catastrophic collapse in highly comminuted patterns, and the facilitation of early rehabilitation in polytrauma patients solidify its role as the definitive key to managing challenging distal radius fractures.
Clinical & Radiographic Imaging













You Might Also Like