Full Question & Answer Text (for Search Engines)
Question 1:
How common are spinal infections following penetrating injury to the spine:
Options:
Correct Answer: 2%
Explanation:
One study found that 5 of 239 patients with gunshot or stab wounds developed meningitis, paravertebral abscess, vertebral osteomyelitis, or epidural abscess.
Question 2:
Risk factors implicated in postoperative wound infection following lumbar spine surgery include all of the following except:
Options:
- Use of instrumentation
- Presence of spina bifida occulta
- History of smoking
- Longer operative duration
- Obesity
Correct Answer: Presence of spina bifida occulta
Explanation:
Instrumented cases, preoperative history of smoking or obesity, and longer operating room duration have all been identified as possible risk factors for surgical site infection. Additionally, patient age may be a risk factor or may be associated with a risk factor like medical comorbidity or nutritional depletion.
Question 3:
In the face of vertebral infection and progressive deformity, surgical reconstruction should:
Options:
- Never use instrumentation
- Never use allograft bone
- Always be approached posteriorly
- Always involve an aggressive debridement
- Always follow extensive antibiotic treatment until the infection is eradicated
Correct Answer: Always involve an aggressive debridement
Explanation:
Surgical reconstruction in the face of spinal infection may be indicated should progressive neurological deficit or deformity occur. Such reconstruction may be successful if an aggressive debridement of all infectious foci is done, even if instrumentation or allograft is used. The optimal approach is dictated by the location of the infection and the type and degree of deformity (and is often anterior or anterior-posterior).
Question 4:
The spinal surgical procedure associated with the highest rate of surgical site infection is:
Options:
- Neuromuscular scoliosis fusion
- Lumbar spondylolisthesis fusion
- Reduction and fusion of traumatic cervical facet fracture-dislocation
- Lumbar stenosis decompression and fusion
- Cervical laminectomy, foraminotomy, and arthrodesis
Correct Answer: Neuromuscular scoliosis fusion
Explanation:
Postoperative infection rates reach 11% for neuromuscular disease indications. For muscular dystrophy scoliosis surgery, the rate may be as high as 23%, for cerebral palsy 18%, and for myelomeningocele 11%.
Question 5:
Which of the following comprises the middle column in the Denis three- column model of the thoracolumbar spine:
Options:
- Posterior longitudinal ligament, spinal canal, pedicles, and facet joints
- Facet joints, intertransverse membrane, and ligamentum flavum
- Vertebral body, posterior longitudinal ligament, and disk
- Posterior half of the vertebral body, posterior half of the disk, and posterior longitudinal ligament
- Interspinous ligament, supraspinous ligament, and ligamentum flavum
Correct Answer: Posterior longitudinal ligament, spinal canal, pedicles, and facet joints
Explanation:
The middle column is composed of the posterior half of the vertebral body, posterior half of the disk, and posterior longitudinal ligament. The middle column, according to Denis, is important to determine the stability of a thoracolumbar fracture. There is the potential for instability when the middle column is disrupted.
Question 6:
Which type of biomechanical force(s) acts on the anterior portion of the thoracolumbar junction (T12-L2) at rest in a standing position:
Options:
- C ompression
- C ompression and shear
- C ompression and tension
- Tension
- Shear and torsion
Correct Answer: C ompression
Explanation:
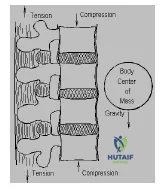
The thoracolumbar junction is normally a straight portion of the spine (no lordosis or kyphosis) and the vertebral bodies are subject to compressive forces at rest when the patient is in a standing position. The posterior
osteoligamentous structures are subject to tension along with the paraspinous muscles that help to maintain an upright posture.
Question 7:
Which of the following statements is true regarding the bulbocavernosus reflex:
Options:
- This reflex is a sign of a spinal cord injury.
- This reflex is mediated by the S3 and S4 segments of the spinal cord.
- This reflex may be elicited by pulling on an indwelling catheter that causes a contraction of the cremaster muscle.
- This reflex often means that a spinal cord injury is complete.
- This reflex is mediated by the S3 and S4 segments of the spinal cord, and this reflex often means that a spinal cord injury is complete.
Correct Answer: This reflex is a sign of a spinal cord injury.
Explanation:
The bulbocavernosus reflex is mediated by the S3 and S4 regions of the spinal cord. This reflex is elicited by pulling on an indwelling catheter or squeezing the glans penis or clitoris and observing contraction of the anal sphincter. The bulbocavernosus reflex may be absent soon after a spinal cord injury due to spinal shock, but it often returns in 24 to 48 hours and indicates the end of spinal shock. A better sense of prognosis of a spinal cord injury is possible after spinal shock has ended.
Question 8:
According to the Frankel grading scale for a neurologic injury, what is meant by Frankel C :
Options:
- There is an antigravity motor function in some distal muscles below the level of the spinal cord injury.
- There is an antigravity muscle function in the muscles 1 or 2 root levels below the spinal cord injury.
- There is muscle function, but not with adequate power to overcome gravity in some muscles below the level of the spinal cord injury.
- There is muscle function, but not with adequate power to overcome gravity in the muscles 1 or 2 root levels below the spinal cord injury.
- The patient has a chance for further neurologic recovery.
Correct Answer: There is muscle function, but not with adequate power to overcome gravity in some muscles below the level of the spinal cord injury.
Explanation:
The Frankel grading scale is used to communicate the extent of neurologic injury in the setting of a spinal cord injury. The A category indicates that there is no motor or sensory function below the level of the injury. The B category indicates that there is only sensory function below the level of the injury. The C category indicates that there is muscle function, but not with adequate power to overcome gravity in some muscles below the level of the spinal cord injury. The D category indicates that there is motor function with at least antigravity power below the level of the injury. The E category indicates that the muscle function below the level of the injury is normal in power. One can see some motor function for 1-2 root levels below the level of a spinal cord injury that is due to root escapeâ and should not be confused with distal motor sparing.
Question 9:
Which type of thoracolumbar fracture is associated with the highest incidence of intra-abdominal visceral trauma:
Options:
- Burst fracture
- C ompression fracture
- Flexion-distraction injury
- Fracture dislocation
- Pathologic fracture
Correct Answer: Flexion-distraction injury
Explanation:
The flexion-distraction injury was originally termed the â seatbelt injuryâ or in the case of a fracture proceeding through bone, a Chance fracture.â This injury is usually the result of a severe flexion force to the lumbar spine with flexion moment anterior to the spine (e.g., at a lap belt). Due to the severe energy dissipation at the level of the flexion moment, there is a high incidence of intra-abdominal visceral trauma.
Question 10:
Which type of treatment would be most appropriate for a young, healthy patient with an incomplete spinal cord injury (ASIA C ) 5 days following a T12 burst fracture with 30% canal compromise:
Options:
- Bed rest, followed by hyperextension casting
- Posterior distractive instrumentation and fusion
- Posterior fusion in situ
- Anterior T12 corpectomy and strut grafting
- Anterior T12 corpectomy, strut grafting, and instrumentation
Correct Answer: Anterior T12 corpectomy and strut grafting
Explanation:
Surgery is indicated in patients with an incomplete spinal cord injury with spinal cord compression. Although some indirect decompression may be achieved early following the injury using posterior distractive instrumentation, the level of decompression is often better using an anterior approach (especially several days following the fracture). Following anterior decompression, either anterior instrumentation or posterior instrumentation is indicated to stabilize the construct and allow early mobilization.
Question 11:
Which of the following is the best indication for a laminectomy in a patient who has sustained a thoracolumbar burst fracture with a neurologic deficit:
Options:
- Spinal cord compression
- A lamina fracture is present on a computerized tomography scan
- A small epidural hematoma is present on a magnetic resonance image
- Greater than 30° of kyphosis on a lateral radiograph
- Greater than 50% canal compromise on a computerized tomography scan
Correct Answer: A lamina fracture is present on a computerized tomography scan
Explanation:
A laminectomy is never indicated as the sole method of treatment for a thoracolumbar burst fracture. Laminectomy creates additional instability at the level of the fracture and does not effectively decompress the spinal cord, which is compressed anteriorly from the retropulsed bony fragment. When lamina fractures are present on a computerized tomography scan, there is a significant incidence of dural tears and entrapped nerve tissue within the lamina fracture. Surgeons should consider performing a laminectomy in addition to other methods of achieving anterior decompression and stabilization of a burst fracture with a lamina fracture.
Question 12:
Which recommendations for the pharmacologic treatment of spinal cord injuries resulted from the NASC IS-II trials:
Options:
- Treat all patients with a spinal cord injury with methylprednisolone 30 mg/kg over 1 hr followed by a maintenance rate of 5.4 mg/kg/hr for 23 hours.
- Treat only patients who present within the first 8 hours of a spinal cord injury with methylprednisolone 30 mg/kg over 1 hr followed by a maintenance rate of 5.4 mg/kg/hr for 23 hours.
- Treat all patients with a spinal cord injury with decadron 10 mg/kg bolus followed by 1 mg/kg/hr for 23 hours.
- Treat only patients who present within the first 8 hours of a spinal cord injury with decadron 10 mg/kg bolus followed by 1 mg/kg/hr for 23 hours.
- Treat only patients who present with complete spinal cord injuries within the first 8 hours of a spinal cord injury with methylprednisolone 30 mg/kg over 1 hr followed by a maintenance rate of 5.4 mg/kg/hr for 23 hours.
Correct Answer: Treat only patients who present within the first 8 hours of a spinal cord injury with methylprednisolone 30 mg/kg over 1 hr followed by a maintenance rate of 5.4 mg/kg/hr for 23 hours.
Explanation:
The NASC IS-II recommendations are to treat patients who present with an incomplete spinal cord injury within 8 hours of the injury with methylprednisolone 30 mg/kg over 1 hour followed by a maintenance rate of 5.4 mg/kg/hr for 23 hours. Because it is difficult to tell which patients have a complete or incomplete spinal cord injury in this time frame due to spinal shock, it has generally been accepted to treat all patients with spinal cord injuries with this treatment protocol as long as they present within the first 8 hours of the injury.
Question 13:
Which of the following statements is true regarding neurogenic shock:
Options:
- Neurogenic shock is due to severe blood loss associated with a spinal cord injury.
- Neurogenic shock can be diagnosed when there is hypotension and tachycardia.
- Neurogenic shock is due to increased parasympathetic tone.
- Neurogenic shock is best treated with judicious use of fluids and vasopressors.
- Neurogenic shock is a sign of an incomplete spinal cord injury.
Correct Answer: Neurogenic shock is due to severe blood loss associated with a spinal cord injury.
Explanation:
Neurogenic shock is present when there is a spinal cord injury interrupting sympathetic tone to the heart and blood vessels, and it is heralded by bradycardia and hypotension. It is important to maintain a reasonable blood pressure to prevent further damage to the spinal cord due to ischemia. In the absence of significant blood loss from another source, neurogenic shock must be treated with vasopressor medication and atropine. Severe neurogenic shock may require cardiac pacing. Fluids must be used carefully as overzealous use of fluid resuscitation can result in pulmonary edema.
Question 14:
Which is the best indication for surgical treatment of a patient with a thoracolumbar burst fracture:
Options:
- 60% canal compromise by a retropulsed bony fragment
- 25° of kyphosis on the lateral radiograph
- A fracture of the lamina present on a computerized tomography scan
- An incomplete neurologic deficit
- A polytrauma patient
Correct Answer: An incomplete neurologic deficit
Explanation:
The exact indications for surgery vs nonoperative management of thoracolumbar burst fractures remains controversial. The best indication is an incomplete neurologic deficit with spinal cord compression. Other considerations include the degree of deformity (greater than 30° is generally considered appropriate to consider surgery) and the other injuries. Although much has been written about canal compromise, in the absence of a neurologic deficit it is not clear that surgery is always indicated due to canal compromise alone. Large canal fragments have been shown to resorb with conservative treatment.
Question 15:
Which of the following patients is not at increased risk for isthmic spondylolisthesis:
Options:
- Football lineman
- Gymnast
- Eskimo
- Nonambulatory patient
- Weight lifter
Correct Answer: Nonambulatory patient
Explanation:
Isthmic spondylolisthesis is most common in white men and least common in black women. It is thought to arise from repetitive hyperextension of the lumbar spine causing a stress fracture of the pars intra-articularis. Sports such as weight lifting, gymnastics, football, and javelin throwing have a particularly high incidence of this condition. Isthmic spondylolisthesis is never present at birth and is rare in nonambulatory patients.
Question 16:
Which patient is at the lowest risk for progression of spondylolisthesis:
Options:
- A 45-year-old man with grade II isthmic spondylolisthesis at L5-S1.
- A 5-year-old girl with grade I dysplastic spondylolisthesis at L5-S1.
- A 25-year-old man with a grade I isthmic spondylolisthesis at L4-5.
- A 16-year-old boy with Grade III isthmic spondylolisthesis at L5-S1.
- A 12-year-old girl with Grade II isthmic spondylolisthesis at L5-S1.
Correct Answer: A 45-year-old man with grade II isthmic spondylolisthesis at L5-S1.
Explanation:
Young age, dysplastic spondylolisthesis, and spondylolisthesis above L5-S1 are all risk factors for progression. Adults with isthmic spondylolisthesis at L5-S1 (85% of cases) are at a low risk for progression of the slippage.
Question 17:
What is the most common source of neurologic compression in a patient with lumbar spinal stenosis due to degenerative changes in the lumbar spine:
Options:
- Disk
- Inferior articular process
- Superior articular process
- Pars intrarticularis
- Lamina
Correct Answer: Superior articular process
Explanation:
Degenerative spinal stenosis is the most common variety of spinal stenosis and usually manifests compression of the thecal sac in the lateral recess of the canal (defined as the area of the spinal canal between the facet joints and the intervertebral disk). The primary cause of stenosis is hypertrophy of the facet joint with compression from the superior articular process. This must be relieved for a patient to achieve an adequate decompression.
Question 18:
Which of the following cervical spine nerve roots may cause paralysis of the diaphragm if injured during an anterior approach:
Options:
Correct Answer: C 4
Explanation:
The C 4 cervical spine nerve root provides the primary innervation of the diaphragm.
Question 19:
The deltoid muscle may become paralyzed as a result of injury to which of the following cervical spine nerve roots:
Options:
Correct Answer: C 5
Explanation:
The deltoid muscle is almost entirely innervated by the C 5 cervical spine nerve root.
Question 20:
The biceps reflex is diminished by compression of which of the following cervical spine nerve roots:
Options:
Correct Answer: C 5
Explanation:
Although there is a small contribution from the C 6 cervical spine nerve root, the biceps reflex is primarily derived from the C 5 cervical spine nerve root.
 osteoligamentous structures are subject to tension along with the paraspinous muscles that help to maintain an upright posture.
osteoligamentous structures are subject to tension along with the paraspinous muscles that help to maintain an upright posture.