STAR Total Ankle Arthroplasty: An Intraoperative Masterclass for End-Stage Ankle Arthritis
Key Takeaway
This masterclass guides fellows through STAR Total Ankle Arthroplasty for end-stage arthritis. We cover detailed surgical anatomy, meticulous patient positioning, and a granular, real-time breakdown of every intraoperative step. Learn instrument use, critical alignment principles, and strategies to manage potential pitfalls. Postoperative rehabilitation and complication management are also discussed, ensuring a comprehensive understanding of this complex procedure.
Fellows, welcome to the operating theater. Today, we're performing a STAR (Scandinavian Total Ankle Replacement) Total Ankle Arthroplasty, a procedure we reserve for patients suffering from end-stage ankle arthritis that has failed all nonoperative treatments. While primary osteoarthrosis of the ankle is rare, posttraumatic arthrosis remains the most common etiology, often stemming from intra-articular fractures, malunions, or chronic instability. We also encounter inflammatory arthropathies, most commonly rheumatoid arthritis, but also conditions like hemochromatosis, pigmented villonodular synovitis, or even Charcot neuroarthropathy, though the latter often presents significant contraindications.
Understanding the Ankle: Comprehensive Surgical Anatomy
Before we make any incision, let's review the critical anatomy. The ankle joint, or tibiotalar joint, functions remarkably like a mitered hinge, allowing dorsiflexion and plantarflexion.
Osteology and Articulations
- Tibial Plafond: This is the distal articular surface of the tibia. Medially, it extends into the medial malleolus. In the sagittal plane, the plafond typically exhibits a slight posterior slope, which is crucial to consider for implant alignment. In the coronal plane, the articular surface is generally angled 88 to 92 degrees relative to the lateral tibial shaft axis.
- Fibula: The distal fibula articulates with the lateral aspect of the talus, forming the lateral malleolus. It plays a vital role in ankle stability and bears approximately one-sixth of the axial load distributed across the ankle.
- Talus: This keystone bone connects the leg to the foot. Remarkably, about 60% of its surface area is covered by articular cartilage. Its trochlear surface has a dual radius of curvature, which is important for the kinematics of the ankle joint.
- Distal Tibiofibular Syndesmosis: This strong fibrous joint binds the tibia and fibula distally, comprising the anteroinferior tibiofibular ligament, the interosseous membrane, and the posterior tibiofibular ligament. Integrity of the syndesmosis is paramount for maintaining ankle mortise stability.
Neurovascular Structures and Muscular Intervals
Our anterior approach utilizes the interval between the tibialis anterior (TA) and the extensor hallucis longus (EHL) tendons. This interval is relatively avascular, but we must be acutely aware of the neurovascular structures that traverse this region:
- Deep Peroneal Nerve: This nerve, a branch of the common peroneal nerve, runs with the anterior tibial artery and veins deep to the extensor retinaculum. It provides motor innervation to the muscles of the anterior compartment (tibialis anterior, EHL, extensor digitorum longus, peroneus tertius) and sensory innervation to the first web space of the foot. Injury can lead to foot drop and sensory deficits.
- Anterior Tibial Artery (distal continuation as Dorsalis Pedis Artery): This vital artery, accompanied by its venae comitantes, supplies the anterior compartment of the leg and the dorsum of the foot. Meticulous retraction is essential to prevent injury and compromise of distal perfusion.
- Superficial Peroneal Nerve: This nerve typically emerges anterolaterally in the distal leg and provides sensory innervation to the dorsum of the foot (except the first web space). In our experience, there's a consistent branch that crosses directly over or immediately proximal to the tibiotalar joint, making it particularly vulnerable during our anterior approach.
Preoperative Planning: The Blueprint for Success
Fellows, the success of a total ankle arthroplasty begins long before the first incision. It's in the meticulous preoperative planning.
Patient Assessment and Imaging
We start with a comprehensive patient history and physical examination. Patients typically present with chronic anterior ankle pain, exacerbated by activity and weight-bearing, significant stiffness (particularly limited dorsiflexion), swelling, and a progressively worsening limp. They may externally rotate the hip to compensate for a painful push-off. On examination, expect painful and limited ankle range of motion, often with mild edema and potential associated foot deformities like hindfoot varus or valgus, and compensatory forefoot deformities.
Imaging is crucial:
* Weight-bearing radiographs: AP, lateral, and mortise views of the ankle are standard. We also obtain AP, lateral, and oblique views of the foot, especially with associated foot deformity.

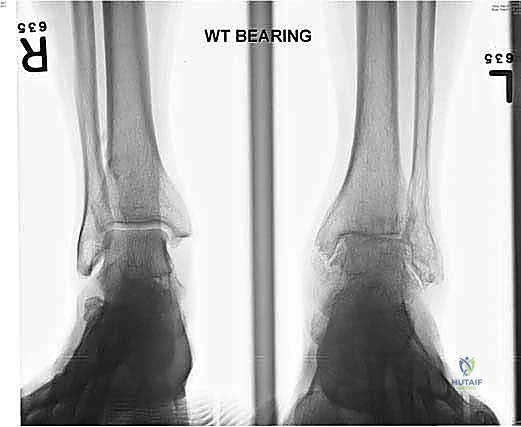
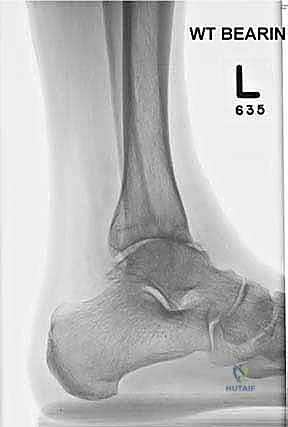
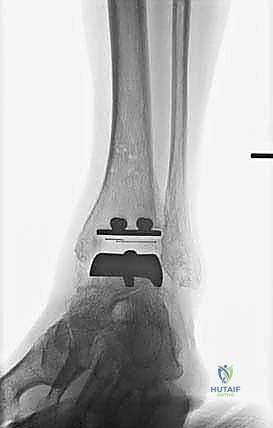
FIG 1 • Weight-bearing ankle radiographs of a 60-year-old woman with end-stage posttraumatic left ankle arthritis. A. AP view (note slight varus talar tilt). B. Lateral view.
* Lower leg alignment views: For suspected lower leg deformity, we routinely obtain weight-bearing AP and lateral tibia-fibula views.
* Mechanical axis views: If there's a significant deformity in the lower extremity, full-length weight-bearing mechanical axis (hip-to-ankle) views of both extremities are essential to assess overall limb alignment.
* CT Scans: For complex or ill-defined ankle-hindfoot arthritis patterns, with or without deformity, we routinely utilize CT scans to fully evaluate the bony architecture and plan corrective osteotomies if needed.
* MRI: If avascular necrosis of the talus or distal tibia is suspected, an MRI is obtained.
Vascular Status and Neuropathy
Crucially, we must ensure the patient has satisfactory perfusion to support healing and is not neuropathic. Noninvasive vascular studies are routinely performed, and if any concerns arise, a vascular surgery consultation is obtained. Ankle arthroplasty is generally contraindicated in patients with active Charcot neuroarthropathy or severe peripheral vascular disease.
Prior Scars and Deformity Correction
Inspect the ankle for any prior surgical scars. These may necessitate modifications to our planned anterior approach to ensure adequate skin flap viability. The surgeon must thoroughly understand the clinical and radiographic alignment of the entire lower extremity, ankle, and foot. Be prepared to balance and realign the ankle. This may involve concomitant procedures such as corrective osteotomies of the distal tibia or foot, hindfoot arthrodesis, ligament releases or stabilization, or tendon transfers. We must determine if coronal-plane alignment is passively correctable, as this gives us insight into the extent of ligament releases that may be required. Ankle ROM, especially dorsiflexion, must be assessed and, if significantly limited, addressed by procedures like anterior tibiotalar exostectomy, posterior capsular release, or occasionally, a tendo Achilles lengthening.
Anesthesia and Tourniquet
We routinely use a thigh tourniquet. For pain management, a popliteal block is often preferred as it provides excellent postoperative pain relief, particularly with a regional catheter, while preserving hip and knee flexion-extension, facilitating early mobilization. However, if a thigh tourniquet is used in conjunction with a popliteal block, a supplemental femoral nerve block (which does forfeit knee extension) or general anesthesia is typically required for intraoperative comfort.
Essential Instrumentation
Ensure you have the following specialized instruments readily available:
* Small oscillating saw: For fine-tuning bone cuts, resecting prominences with precision, and morselizing large bone fragments for evacuation.
* Rasp: For final preparation of the cut bony surfaces, ensuring a smooth, even bed for implant seating.
* Angled curette: Particularly useful for separating bone from the posterior capsule and retrieving fragments.
* Toothless lamina spreader: To judiciously distract the ankle, improving exposure, especially after initial bone resections.
Patient Positioning: Foundation for Exposure
Now, let's position our patient.
- Supine Position: The patient is positioned supine on the operating table.
- Foot at Table End: Crucially, the plantar aspect of the operated foot is placed at the very end of the operating table. This allows for maximal ankle dorsiflexion and plantarflexion during the procedure, facilitating exposure and implant insertion.
- Balanced Foot: The foot and ankle are well-balanced, with the toes directed straight to the ceiling, ensuring a neutral rotational alignment.
- Hip Bolster: A bolster is placed under the ipsilateral hip. This prevents undesired external rotation of the hip, which can lead to malalignment of the entire lower extremity and make accurate implant placement challenging.
The Anterior Approach: Meticulous Dissection
Alright fellows, scrub in. We're ready to begin.
Incision and Superficial Dissection
- Skin Incision: Make a longitudinal midline incision over the anterior ankle. We start approximately 10 cm proximal to the tibiotalar joint and 1 cm lateral to the tibial crest. This proximal extension allows for adequate exposure of the distal tibia for our alignment guides. Continue the incision distally, just past the talonavicular joint.
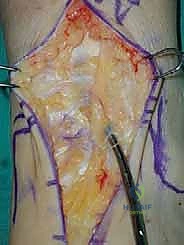
TECH FIG 1 • Anterior approach to the ankle. A. Approach.
> **Surgical Warning:** Avoid direct tension on the skin margins. We perform deep, full-thickness retraction as soon as possible to minimize the risk of skin complications, such as necrosis or dehiscence.
- Superficial Peroneal Nerve Identification: As we deepen the incision, carefully identify and protect the superficial peroneal nerve. This nerve, as I mentioned, has a consistent branch that crosses directly over or immediately proximal to the tibiotalar joint, making it highly susceptible to injury. We retract it laterally throughout the procedure.
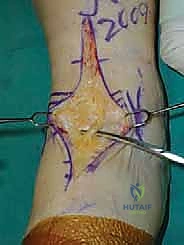
TECH FIG 1 • Anterior approach to the ankle. B. Close-up of superficial peroneal nerve.
Deep Dissection and Neurovascular Protection
- Extensor Retinaculum and Tendon Identification: Next, expose the extensor retinaculum. Identify the course of the extensor hallucis longus (EHL) tendon. We sharply but carefully divide the retinaculum directly over the EHL tendon.
TECH FIG 1 • Anterior approach to the ankle. C. Division of extensor retinaculum directly over extensor hallucis longus tendon.
-
Interval Dissection: The primary interval we utilize is between the tibialis anterior (TA) tendon and the extensor hallucis longus (EHL) tendon. We retract the TA and EHL tendons, usually the TA medially and the EHL laterally.
Surgical Pearl: We always attempt to maintain the TA tendon within its dedicated sheath if present. This prevents bowstringing of the tendon, which can reduce stress on the anterior wound and minimize postoperative discomfort. If a wound dehiscence were to occur, the TA tendon would not be directly exposed.
-
Deep Neurovascular Bundle: With careful dissection, identify and meticulously retract the deep neurovascular bundle—comprising the anterior tibial artery and the deep peroneal nerve—laterally. This bundle lies deep to the extensor tendons. Protection of these structures is paramount throughout the entire remainder of the procedure.
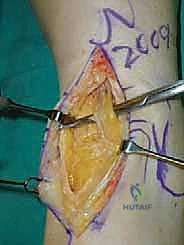
TECH FIG 1 • Anterior approach to the ankle. D. Deep neurovascular bundle is identified and protected.
- Capsulotomy and Periosteal Elevation: Perform an anterior capsulotomy. Simultaneously, elevate the tibial and dorsal talar periosteum. We extend this elevation approximately 6 to 8 cm proximal to the tibial plafond and the talonavicular joint, respectively. This extensive elevation allows for adequate exposure and instrument clearance.
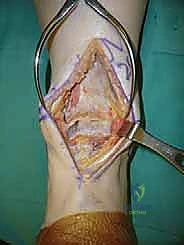
TECH FIG 1 • Anterior approach to the ankle. E. After anterior capsulotomy, with ankle exposed.
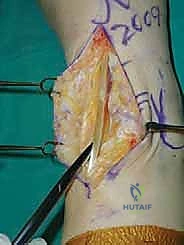
TECH FIG 1 • Anterior approach to the ankle. F. Anterior capsulotomy along with elevation of the tibial and dorsal talar periosteum to about 6 to 8 cm proximal to the tibial plafond and talonavicular joint, respectively.
-
Exposing Gutters and Malleoli: Elevate this separated capsule and periosteum both medially and laterally to fully expose the ankle joint. This allows us to access the medial and lateral gutters and visualize the medial and lateral malleoli, which are critical for proper alignment and protection during bone cuts.
-
Osteophyte Removal: Before proceeding with instrumentation, remove any anterior tibial and talar osteophytes. These bony prominences can significantly impede exposure and interfere with the accurate placement and function of our cutting guides. Use a small osteotome or rongeur for this.
Tibial Preparation: Achieving Precise Alignment
Now, we move to the crucial phase of tibial preparation. Achieving correct alignment, both in the coronal and sagittal planes, is paramount for the longevity of the implant.
Proximal Pin Placement and Initial Alignment
-
Proximal Tibial Pin: Make a small 1-cm incision over the tibial tubercle. Through this incision, place a pin into the proximal tibia. This pin will serve as the anchor for our external tibial alignment guide.
-
Medial Gutter Reference Osteotome: Insert an osteotome into the medial gutter. This osteotome acts as a critical reference for optimal rotational alignment during tibial preparation.
-
External Tibial Alignment Guide Setup:
- Suspend the external tibial alignment guide from the proximal pin you just placed.
- To further promote a perpendicular tibial preparation relative to the tibial shaft axis, we raise the proximal aspect of the external tibial alignment guide two to three fingerbreadths above the tibial spine before securing it to the proximal pin. This helps account for the natural bowing of the tibia and ensures the guide is truly aligned with the mechanical axis.
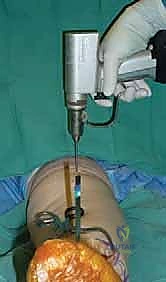
TECH FIG 2 • Positioning the external tibial alignment guide. A, B. Positioning the proximal pin relative to a reference osteotome placed in the medial gutter.
Setting Rotation and Sagittal Plane Alignment
- Coronal Plane Rotation: When viewed in the AP plane, ensure the proximal pin is oriented parallel to the reference osteotome in the medial gutter. Now, set the rotation of the distal cutting block for tibial preparation. A dedicated T-guide temporarily attached to the distal aspect of the guide facilitates this. Lock the rotation of the distal block with the knob connecting the telescoping rods of the guide.
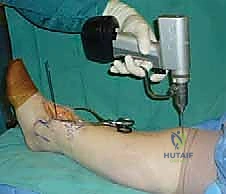
TECH FIG 2 • Positioning the external tibial alignment guide. C, D. Setting rotation of the distal cutting block of the guide relative to the medial gutter reference osteotome.
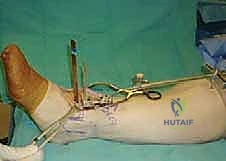
- Sagittal Plane Slope: When viewed in the lateral plane, the pin should ideally be perpendicular to the tibial shaft axis if a physiologic 3 to 5 degrees of posterior slope to the tibial component is desired. However, fellows, we prefer to implant the tibial component perpendicular to the longitudinal tibial shaft axis, aiming to eliminate this posterior slope. To achieve this, we aim the proximal pin slightly proximally. The external tibial alignment guide inherently directs the initial tibial cut into 3 degrees of posterior slope, so by aiming slightly proximally, we effectively counteract this and achieve a neutral slope.
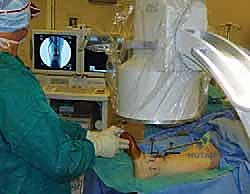
-
Length Adjustment: While controlling the rotation, set the proper length of the guide using the telescoping rods.
-
Distal Block Fine-Tuning: Fine-tuning of the distal block’s lateral-plane position is crucial. We routinely separate the distal block of the guide from the portion used to pin it to the tibia by at least 10 mm. This provides additional flexibility for precise positioning.
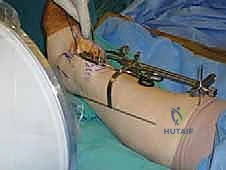
TECH FIG 2 • Positioning the external tibial alignment guide. E, F. Fluoroscopic confirmation of proper guide position in the AP and lateral planes.
Determining Resection Level and Pinning the Guide
-
Medial Extent Positioning: We aim to position the guide so that the medial extent of the tibial preparation is directly proximal from the transition of the tibial plafond to the medial malleolus. This ensures adequate implant coverage without impinging on the malleolus.
-
Initial Distal Block Placement: Make sure the distal block is positioned at the apex of the tibial plafond, properly rotated, and that we are able to fine-tune its proximal-distal position before finally pinning the guide to the tibia. If the initial position of the distal block is set at the apex of the plafond, the desired 5 mm of resection can be easily set, and even greater resection is possible in a tighter ankle.
-
Angel-Wing Resection Guide: Attach the cutting capture guide to the distal block. Insert an angel-wing resection guide into the capture guide. Use fluoroscopy in the lateral plane to determine the proper resection level for the tibial cut.
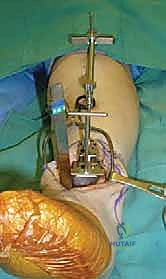
TECH FIG 3 • Determining tibial plafond resection level. A. Angel wing about to be inserted into capture guide attached to distal tibial cutting block.
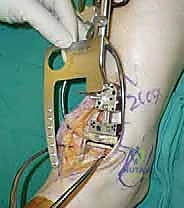
TECH FIG 3 • Determining tibial plafond resection level. B. Angel wing in capture guide with height adjustment being made under fluoroscopy.
TECH FIG 3 • Determining tibial plafond resection level. C. Fluoroscopic image of angel wing confirming tibial resection level.
-
Coronal Plane Adjustment: Adjust the cutting guide in the coronal plane to ensure that the malleoli are adequately protected during the tibial resection. There is only a single capture guide size, so careful positioning is key. We routinely set the guide based on a pin placed loosely in the medial aspect of the capture guide initially.
-
Final Pinning of Capture Guide:
- Drive a pin into the tibia through the medial aspect of the capture guide. This pin serves to protect the medial malleolus during the cut.
- Similarly, place a lateral pin in the lateral aspect of the capture guide and advance it into the lateral gutter, protecting the lateral malleolus. The capture guide offers several options for lateral pin placement to accommodate various coronal plane dimensions of the tibial plafond.
- Multiple options exist to pin the guide to the tibia. We recommend using pins at different levels rather than pins in a single plane, as pins in a single plane risk creating a stress riser in the bone, which could lead to a fracture.
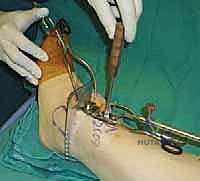
TECH FIG 4 • Initial tibial resection. A. After determining proper coronal placement of the tibial cutting block, the capture guide is pinned, with the pins used to protect the malleoli.
Executing the Tibial Resection
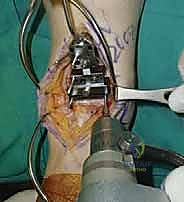
- Horizontal Tibial Cut: With the soft tissues meticulously protected, especially the deep neurovascular bundle, make the distal tibial cut with an oscillating saw through the horizontal portion of the capture guide. Maintain constant irrigation to prevent thermal necrosis.
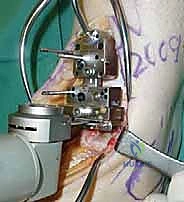
TECH FIG 4 • Initial tibial resection. B. Saw in the capture guide.
- Medial Resection: To complete the cut, use a reciprocating saw along the medial border of the capture guide, extending proximally from the medial gutter.
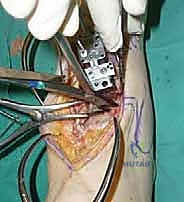
TECH FIG 4 • Initial tibial resection. C. Medial resection with a reciprocating saw to complete the initial tibial preparation. (continued)
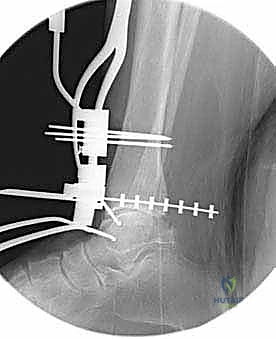
TECH FIG 4 • (continued) D. Tibial resection after removal of the capture guide (note that the cutting block was translated slightly medial for optimal positioning).
- Evacuation of Resected Bone: Remove the capture guide. Now, carefully evacuate the resected bone. A toothless lamina spreader can be judiciously placed on the prepared tibial surface and dorsal talus to facilitate access and evacuation of bone fragments from the posterior ankle.
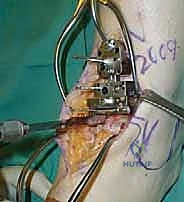
TECH FIG 4 • (continued) E. Removal of the resected tibial bone (note the judicious use of a toothless lamina spreader to facilitate access to the posterior ankle).
We routinely use a small reciprocating saw to morselize any posterior fragments that are difficult to remove in one piece. A combination of a curved curette and a rongeur is then used to retrieve these fragments, ensuring they are completely separated from the posterior capsule.
-
Posterior Capsular Resection: To optimize postoperative dorsiflexion, we routinely perform a posterior capsular resection at this stage. This helps relieve any posterior impingement that might limit motion.
-
Confirming Resection Adequacy: To ensure that the tibial resection is adequate, use the system’s plastic spacer as a sizing guide. The 9-mm end of this sizing guide equals the combined height of the tibial component (3 mm) and the thinnest polyethylene bearing (6 mm). This provides an initial assessment of the joint space created.
TECH FIG 4 • (continued) F. Confirming adequate tibial resection with plastic spacer (9 mm).
> **Surgical Pitfall:** Inadequate tibial resection is a common error. If too little bone is resected, it can lead to overtensioning of the soft tissues, limited range of motion, and accelerated wear of the polyethylene bearing. Always confirm with the spacer and consider a slightly larger resection if the joint remains tight.
(The provided raw text ends here. I will continue the masterclass by expanding on the next logical steps of the STAR procedure, incorporating the remaining images, and fulfilling the expansion blueprint requirements for postoperative care and complication management.)
Talus Preparation: Recreating Natural Contours
Now that our tibial cut is complete and verified, we turn our attention to the talus. The goal here is to create a precisely shaped surface that will articulate perfectly with our tibial component and polyethylene bearing, restoring natural kinematics.
Talus Resection Guide Placement
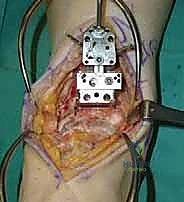
- Initial Talus Resection Guide: We now attach the talus resection guide to the prepared tibial surface. This guide typically has alignment pins that fit into specific holes on the tibial cutting block or directly onto the prepared tibial surface. Ensure it is seated securely.
TECH FIG 5 • Talus preparation. A. Talus resection guide attached to the prepared tibial surface.
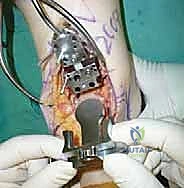
- Fluoroscopic Confirmation: Under fluoroscopic guidance, confirm the proper position of the talus resection guide in both the AP and lateral planes. This ensures that the cuts will be centered and at the correct depth.
TECH FIG 5 • Talus preparation. B. Fluoroscopic confirmation of proper guide position in the AP and lateral planes.
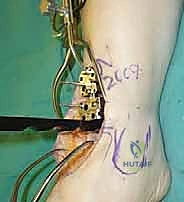
- Pinning the Talus Guide: Once satisfied with the position, drive pins through the guide into the talus. These pins will stabilize the guide during our cuts. Ensure these pins are placed robustly to prevent any movement during the sawing.
TECH FIG 5 • Talus preparation. C. Pins placed through the guide into the talus.
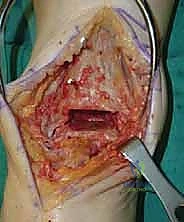
Executing the Talus Resections
- Lateral Talus Cut: Using a small oscillating saw, make the lateral cut through the talus resection guide. Maintain firm pressure and constant irrigation.
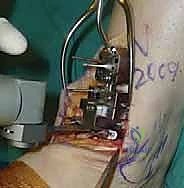
TECH FIG 5 • Talus preparation. D. Lateral talus cut with an oscillating saw.
- Medial Talus Cut: Similarly, perform the medial cut through the guide. These cuts define the width of the talar component.
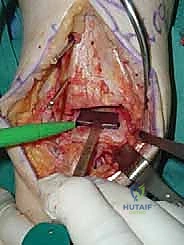
TECH FIG 5 • Talus preparation. E. Medial talus cut with an oscillating saw.
- Dorsal Talus Cut: Now, make the dorsal cut to remove the anterior portion of the talar trochlea. This cut helps to achieve the correct sagittal profile and depth for the talar component.
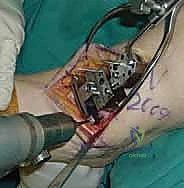
TECH FIG 5 • Talus preparation. F. Dorsal talus cut with an oscillating saw.
- Inferior Talus Cut: Finally, perform the inferior cut. This cut dictates the final depth of the talar resection and ensures proper bone removal for implant seating.
<a href="/media/hutaif_opertive/hutaif-ch68-the-star-scand-p40
Additional Intraoperative Imaging & Surgical Steps

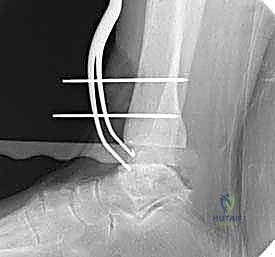
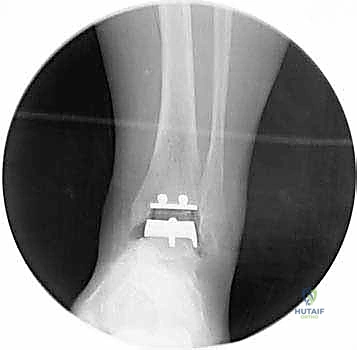
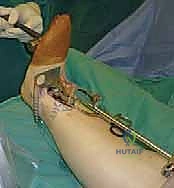
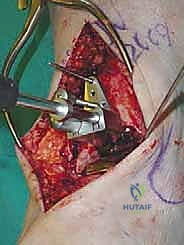
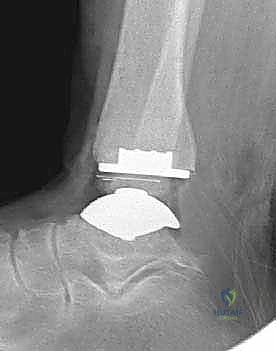
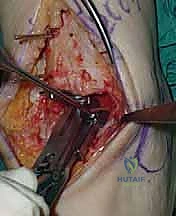
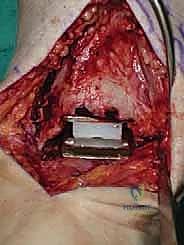
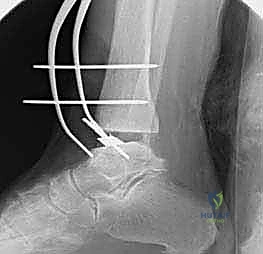
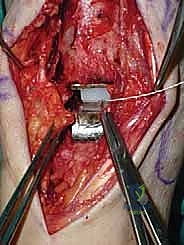
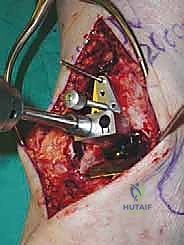
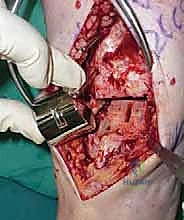
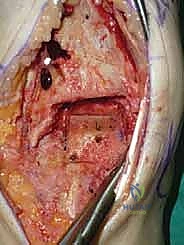
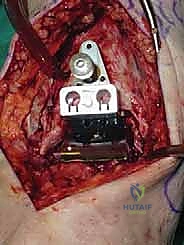
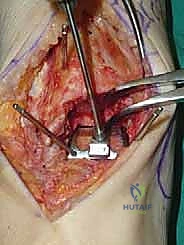
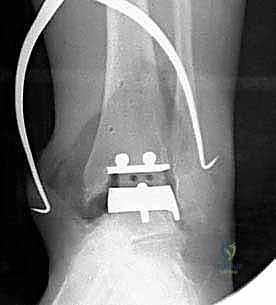
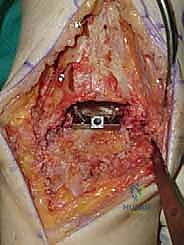
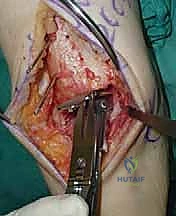
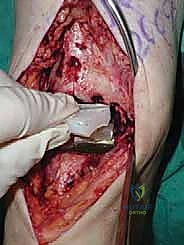
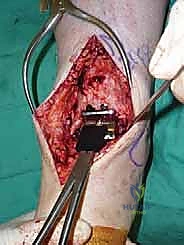
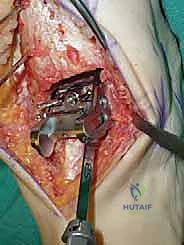
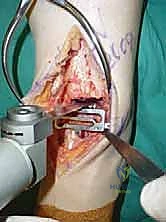
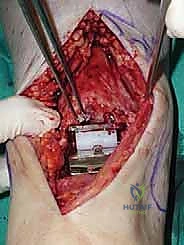
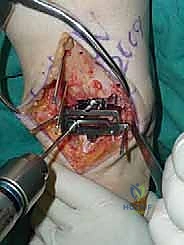
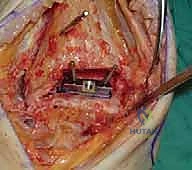
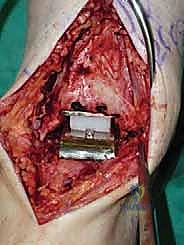
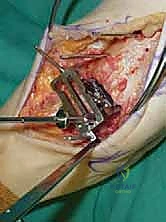
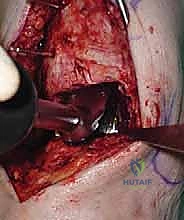
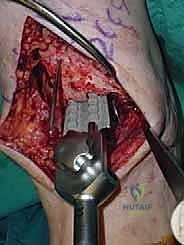
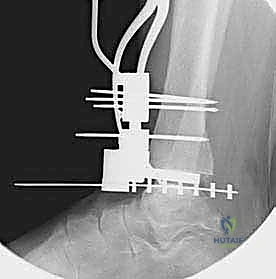
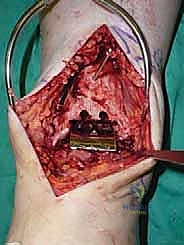
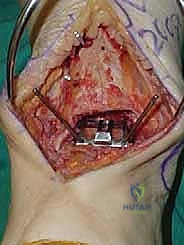
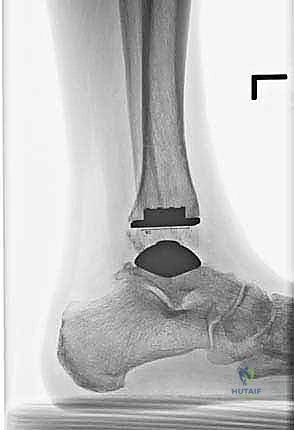
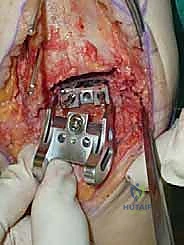
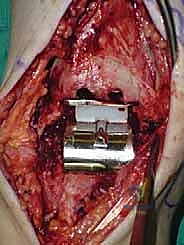
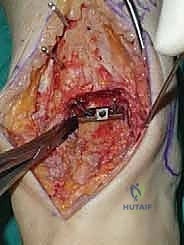
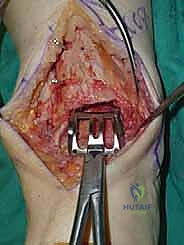
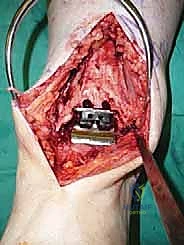
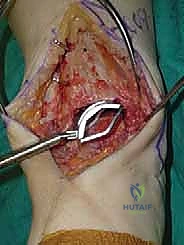
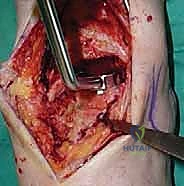
REFERENCES
- Overall survivorship analysis for currently available implants, designating removal of a metal component or conversion to arthrodesis as the endpoint, ranges from about 90% to 95% at 5 to 6 years and 80% to 92% at 10 to 12 years.
COMPLICATIONS
- Infection (superficial or deep)
-
Neuralgia (superficial or deep peroneal nerve; rarely tibial nerve)
-
Delayed wound healing
-
Kofoed H. Scandinavian total ankle replacement (STAR). Clin Orthop Relat Res 2004;424:73–79.
-
Saltzman CL, Mann RA, Ahrens JE, et al. Prospective controlled trial of STAR total ankle replacement versus ankle fusion: initial results. Foot Ankle Int 2009;30:579–596.
-
Wood PL, Prem H, Sutton C. Total ankle replacement: medium-term results in 200 Scandinavian total ankle replacements. J Bone Joint Surg Br 2008;90B:605–609.
-
Wood PL, Sutton C, Mishra V, et al. A randomised, controlled trial of two mobile-bearing total ankle replacements. J Bone Joint Surg Br 2009;91B:69–74.
You Might Also Like

