Medial Epicondylitis Release: An Intraoperative Masterclass in Flexor-Pronator Debridement and Ulnar Nerve Management
Key Takeaway
Join us in the OR for an in-depth masterclass on open medial epicondylitis release. We'll meticulously debride the flexor-pronator origin, address concurrent ulnar nerve pathology, and prepare the epicondyle for optimal healing. Learn crucial anatomical landmarks, avoid common pitfalls, and ensure excellent patient outcomes with precise technique and comprehensive postoperative care.
Introduction and Epidemiology
Medial epicondylitis involves profound tendinosis at the origin of the flexor-pronator mass. It is commonly referred to in lay terminology as golfer's elbow, although there is a significantly stronger epidemiological association with racquet sports, overhead throwing, and repetitive manual labor. The condition represents a degenerative tendinopathy rather than an acute inflammatory process, characterized by angiofibroblastic hyperplasia within the tendon origin.

While lateral epicondylitis is far more prevalent, medial epicondylitis accounts for approximately 10% to 20% of all epicondylitis cases. The peak incidence occurs in patients between the fourth and sixth decades of life, with an equal prevalence among male and female patients. The dominant extremity is affected in over 75% of presentations. Most patients improve with conservative treatment; however, a greater percentage of patients with medial epicondylitis ultimately progress to surgical intervention when compared to patients with lateral epicondylitis. This higher rate of surgical conversion is often attributed to the complex interplay between the flexor-pronator mass, the ulnar nerve, and the medial collateral ligament complex, which can complicate nonoperative recovery.

Pathogenesis and Clinical Evaluation
Epicondylitis results from repetitive microtrauma followed by an incomplete and aborted reparative response. This cascade results in tendinosis, a pathologic state in which the degenerative tendon cannot heal itself effectively. Histologically, this is identified as angiofibroblastic tendinosis, characterized by disorganized collagen architecture, mucoid ground substance accumulation, and a distinct lack of acute inflammatory cells (prostaglandins and macrophages).
Medial epicondylitis can frequently be seen in conjunction with medial collateral ligament instability. In this biomechanical scenario, myotendinous overload occurs as the flexor-pronator mass attempts to dynamically stabilize the ulnohumeral joint against valgus stress. Consequently, ulnar neuropathy often presents as part of a triad of medial elbow pathology (tendinosis, ligamentous laxity, and neuritis).
Patient History and Physical Findings
Patients commonly complain of proximal medial forearm pain rather than strictly localized elbow pain. At times, the regional anatomic alterations are significant enough to cause secondary irritation or compression of the ulnar nerve as it enters the two heads of the flexor carpi ulnaris, causing distinct ulnar nerve symptoms such as local irritability, distal numbness, and tingling in the ring and small fingers.
Onset usually is insidious, but the patient may occasionally recall a specific inciting event. Medial epicondylitis can be present simultaneously with lateral epicondylitis, necessitating a comprehensive bilateral elbow examination. Standardized examination methods include the following key maneuvers. Palpation of the anterior aspect of the medial epicondyle for tenderness is a nearly universal finding in medial epicondylitis. Resisted pronation is highly sensitive for medial epicondylitis, as it directly loads the humeral head of the pronator teres.

A decreased range of motion suggests intra-articular pathology such as radiocapitellar or ulnohumeral arthritis, or potentially a loose body, rather than isolated tendinopathy. If resisted wrist flexion reproduces symptoms, it strongly supports a diagnosis of medial epicondylitis, specifically implicating the flexor carpi radialis. Provocative nerve testing is mandatory. The surgeon should tap the ulnar nerve in the cubital tunnel and along its path into the flexor carpi ulnaris (Tinel's sign). The presence of a tingling sensation locally prompts further neurodiagnostic investigation. Additionally, the elbow flexion test should be performed. Flex the patient's elbow maximally, then compress the ulnar nerve just proximal to the cubital tunnel. The presence of hand numbness or tingling confirms ulnar nerve hyperirritability.

Imaging and Other Diagnostic Studies
While the diagnosis of medial epicondylitis is primarily clinical, imaging and adjunctive studies are critical for ruling out concomitant pathology and surgical planning. Plain radiographs (anteroposterior, lateral, and oblique views) may show calcifications at the flexor-pronator origin in chronic cases. Traction osteophytes at the sublime tubercle or medial epicondyle may indicate chronic valgus overload.
Magnetic resonance imaging will reliably demonstrate increased intratendon signal on T2-weighted sequences, indicative of mucoid degeneration and microtearing. Most scans will also show increased intratendon signal and tendon thickening on T1-weighted sequences. A small percentage of patients may show increased T2 signal in the medial epicondyle itself, representing bone marrow edema, or anconeus edema. Periosteal reaction is not commonly seen on magnetic resonance imaging and should raise suspicion for alternative diagnoses.

Electrophysiologic testing, including electromyography and nerve conduction studies, is warranted if patients have persistent ulnar nerve symptoms. However, it is imperative to recognize that with mild ulnar neuropathy or purely dynamic compression, these tests have a very low sensitivity and may yield false-negative results.
Differential Diagnosis
The differential diagnosis for medial elbow pain is broad and must be systematically evaluated. Pronator syndrome involves median nerve compression in the proximal forearm and can mimic the proximal forearm aching of epicondylitis, though it typically presents with median nerve sensory changes. Medial collateral ligament injury must be ruled out via the moving valgus stress test and milking maneuver. Ulnar neuropathy at the cubital tunnel can present independently or concomitantly. Ulnohumeral arthritis often presents with mechanical symptoms and loss of terminal extension. Cervical radiculopathy (specifically C8-T1) can refer pain to the medial elbow and forearm. Finally, malingering or secondary gain issues should be considered in complex workers' compensation cases unresponsive to standard modalities.

Surgical Anatomy and Biomechanics
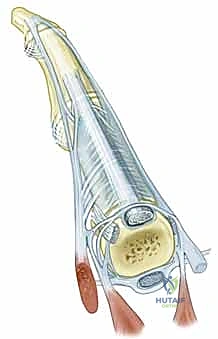
A precise understanding of medial elbow anatomy is paramount to successful surgical intervention and the avoidance of iatrogenic complications. The common flexor-pronator origin is primarily located on the anterior aspect of the medial epicondyle.
The common flexor-pronator origin includes the humeral head of the pronator teres, the flexor carpi radialis, the flexor carpi ulnaris, and a small portion of the flexor digitorum superficialis. The palmaris longus also shares the origin, although this is not likely to be clinically relevant in the pathogenesis of the disease. The most common tendon insertions affected by angiofibroblastic degeneration are the pronator teres and the flexor carpi radialis; however, any tendon insertion of the common flexor-pronator origin can be involved.

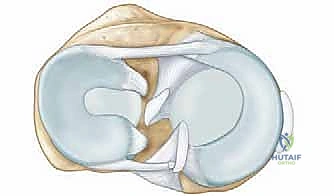
Medial Collateral Ligament Complex
The anterior bundle of the medial collateral ligament is the primary restraint to valgus stress at the elbow. It originates on the anteroinferior surface of the medial epicondyle, deep to the flexor-pronator mass, and inserts onto the sublime tubercle of the proximal ulna. During surgical debridement of the flexor-pronator origin, the surgeon must remain meticulously aware of the anterior bundle's footprint to prevent iatrogenic destabilization of the elbow. The flexor-pronator musculature acts as an active, dynamic secondary stabilizer to valgus stress, which explains why tendinopathy frequently coexists with subtle ligamentous insufficiency.
Neurovascular Anatomy
The medial antebrachial cutaneous nerve provides sensation to the medial forearm. Its anterior and posterior branches cross the operative field and are highly susceptible to injury during the surgical approach. Neuroma formation of the medial antebrachial cutaneous nerve is a devastating complication that can yield worse outcomes than the primary tendinopathy. The ulnar nerve passes posterior to the medial epicondyle through the cubital tunnel, roofed by Osborne's ligament, and enters the forearm between the two heads of the flexor carpi ulnaris.

Indications and Contraindications
Appropriate initial treatment involves nonoperative management, which includes avoidance of painful activities and symptomatic relief with nonsteroidal anti-inflammatory drugs and cryotherapy. Daytime wrist bracing for exertional activities can offload the flexor origin. Physical or occupational therapy is critical to supervise and instruct on eccentric stretching and strengthening protocols for patients not otherwise inclined to comply with those instructions.
Although corticosteroid injection at the medial epicondyle can provide short-term relief, repeated injections are associated with tendon atrophy, hypopigmentation, and an increased risk of subsequent tendon rupture. Biologic adjuncts, such as leukocyte-rich platelet-rich plasma, have shown superior long-term efficacy in regenerating the tendinopathic tissue compared to corticosteroids.

Surgical management is indicated when exhaustive nonoperative measures fail.
| Clinical Scenario | Management Strategy | Rationale and Evidence Base |
|---|---|---|
| Acute onset medial elbow pain without mechanical symptoms | Non-Operative | High rate of spontaneous resolution; physical therapy and NSAIDs are first-line. |
| Persistent pain > 6 months despite comprehensive conservative care | Operative (Open Debridement) | Angiofibroblastic tissue is incapable of self-repair; surgical excision is required to stimulate a healing response. |
| Concomitant ulnar neuropathy failing conservative management | Operative (Debridement + Ulnar Nerve Decompression/Transposition) | Structural compression or dynamic irritation necessitates neurolysis or transposition to prevent irreversible axonal loss. |
| Coexisting symptomatic MCL insufficiency | Operative (Debridement + MCL Reconstruction) | Debridement alone in the setting of valgus instability will fail due to persistent dynamic overload on the repaired tendon. |
| Cervical radiculopathy mimicking epicondylitis | Contraindicated for Elbow Surgery | Source of pain is proximal; elbow intervention will yield no symptomatic improvement. |
Pre Operative Planning and Patient Positioning
Preoperative planning requires a meticulous review of advanced imaging to localize the exact epicenter of tendinosis, which dictates the surgical trajectory. If magnetic resonance imaging demonstrates significant mucoid degeneration extending deep into the flexor digitorum superficialis, the surgical exposure must be adequately planned to address this deeper pathology. Furthermore, the surgeon must decide preoperatively whether the ulnar nerve requires in situ decompression, subcutaneous transposition, or submuscular transposition based on the presence of subluxation and the severity of preoperative electromyographic findings.

The patient is positioned supine on the operating table with the operative extremity extended onto a radiolucent hand table. A non-sterile tourniquet is applied high on the brachium. The shoulder is abducted and externally rotated, allowing the medial aspect of the elbow to face the surgeon. The elbow can be flexed to 90 degrees to relax the neurovascular structures and bring the medial epicondyle into prominent relief. Bony landmarks, including the medial epicondyle, the olecranon, and the course of the ulnar nerve, are marked with a sterile surgical pen prior to exsanguination and tourniquet inflation.

Detailed Surgical Approach and Technique
The open surgical treatment of medial epicondylitis involves a systematic progression of exposure, pathological tissue excision, biological stimulation, and robust repair.
Incision and Superficial Dissection
A 5 to 7 centimeter longitudinal incision is made centered just anterior to the medial epicondyle. Subcutaneous dissection is performed with meticulous hemostasis. The surgeon must remain highly vigilant for the branches of the medial antebrachial cutaneous nerve. These branches typically cross the operative field from proximal-anterior to distal-posterior. They must be identified, mobilized gently with vessel loops, and protected throughout the procedure. Retraction of these cutaneous nerves should be minimized to prevent traction neuropraxia.

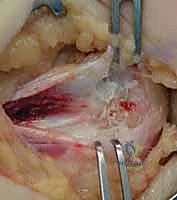
Deep Dissection and Identification of Pathology
The common flexor-pronator fascia is identified. A longitudinal incision is made in the fascia, typically in line with the interval between the pronator teres and the flexor carpi radialis, as this is the most common site of pathology. The normal tendon appears glistening and white, whereas the pathological angiofibroblastic tissue appears gray, dull, friable, and edematous.
Using sharp dissection, the degenerative tissue is meticulously excised. The surgeon must delineate the borders of the healthy tendon to ensure complete removal of the tendinotic mass. It is critical during this deep excision to avoid violating the anterior bundle of the medial collateral ligament, which lies immediately deep to the flexor-pronator origin. The ligament can be protected by maintaining the forearm in pronation and avoiding deep dissection posterior to the mid-axis of the medial epicondyle.

Cortical Decortication and Biological Stimulation
Once the pathological tissue is entirely excised, the anterior aspect of the medial epicondyle is exposed. The cortical bone is mechanically prepared to stimulate a localized healing response. This is achieved by lightly decorticating the footprint using a rongeur or a high-speed burr until punctate bleeding is visualized from the subchondral bone. Alternatively, multiple small drill holes or microfracture awl perforations can be made into the epicondyle to allow bone marrow elements, rich in mesenchymal stem cells and growth factors, to populate the repair site.

Ulnar Nerve Management
If the patient demonstrated preoperative ulnar neuropathy, the ulnar nerve is addressed at this stage. For in situ decompression, Osborne's fascia and the arcuate ligament of the flexor carpi ulnaris are divided. If the nerve subluxates anteriorly over the epicondyle during elbow flexion, or if there is significant tension, an anterior transposition is performed. The nerve is circumferentially mobilized, taking care to preserve the longitudinal intrinsic blood supply, and moved anterior to the epicondyle into a subcutaneous or subfascial pocket. A fascial sling may be created from the flexor-pronator fascia to prevent posterior subluxation back into the cubital tunnel.

Tendon Repair and Closure
The remaining healthy margins of the flexor-pronator mass are then firmly reattached to the decorticated medial epicondyle. This can be accomplished using transosseous tunnels or, more commonly in contemporary practice, via double-loaded suture anchors placed securely into the epicondyle. A locked running suture or a modified Mason-Allen technique is utilized to grasp the tendon edge and tie it down securely to the bone footprint.
The overlying fascial interval is closed with absorbable sutures to ensure a watertight seal and restore the anatomical tension of the flexor-pronator complex. The subcutaneous tissues are closed in layers, and the skin is approximated with a subcuticular closure. A sterile compressive dressing and a posterior plaster splint are applied with the elbow immobilized at 90 degrees of flexion and the forearm in neutral rotation.
Complications and Management
Surgical intervention for medial epicondylitis is generally successful, but complications can significantly compromise clinical outcomes. Meticulous surgical technique is the primary defense against these adverse events.
| Complication | Estimated Incidence | Etiology and Pathomechanism | Salvage Strategy and Management |
|---|---|---|---|
| Medial Antebrachial Cutaneous Nerve Neuroma | 2% - 5% | Iatrogenic transection or aggressive traction during superficial exposure. | Initial management with gabapentinoids and localized blocks. Refractory cases require surgical excision of the neuroma and proximal burying of the nerve stump into muscle. |
| Ulnar Neuritis / Injury | 1% - 3% | Iatrogenic injury during deep dissection, or secondary compression from postoperative hematoma or scar tissue. | Immediate decompression if acute hematoma is present. Late presentations require neurolysis and anterior submuscular transposition. |
| Iatrogenic Medial Collateral Ligament Injury | < 1% | Overzealous deep debridement of the flexor-pronator origin violating the underlying anterior bundle. | Acute recognition requires primary repair. Delayed presentation with valgus instability necessitates formal MCL reconstruction using autograft (palmaris longus). |
| Recurrent Tendinopathy | 5% - 10% | Incomplete excision of angiofibroblastic tissue or premature return to high-demand activities. | Prolonged conservative therapy, biologic injections (PRP), and potentially revision open debridement if structural failure is confirmed on MRI. |
| Postoperative Elbow Stiffness | 3% - 7% | Prolonged immobilization or excessive scar tissue formation. | Aggressive physical therapy, dynamic splinting. Arthroscopic or open capsular release is reserved for refractory contractures > 6 months. |

Post Operative Rehabilitation Protocols
The postoperative rehabilitation protocol must balance the need for tissue protection with the prevention of elbow stiffness.
Phase I Immediate Postoperative Phase
From day 0 to day 14, the primary goals are pain control, edema reduction, and protection of the repair. The patient remains in the posterior splint at 90 degrees of elbow flexion. Active range of motion of the shoulder and digits is encouraged immediately to prevent distal edema and proximal stiffness.
Phase II Intermediate Motion Phase
At 2 weeks postoperatively, the splint and sutures are removed. The patient is transitioned to a hinged elbow brace. Passive and active-assisted range of motion for elbow flexion and extension is initiated. However, active resisted forearm pronation and wrist flexion are strictly prohibited to prevent tensioning the repaired flexor-pronator origin. Isotonic exercises for the biceps, triceps, and shoulder musculature can begin.
Phase III Strengthening Phase
Between 6 and 8 weeks postoperatively, clinical healing of the tendon to the epicondyle is generally sufficient to begin progressive loading. Isometrics for wrist flexion and forearm pronation are introduced, gradually advancing to concentric and eventually eccentric strengthening protocols. Eccentric loading is paramount for realigning the collagen matrix and restoring the tensile strength of the tendon.
Phase IV Return to Sport and Labor
Return to heavy manual labor or overhead racquet sports is typically permitted between 4 and 6 months postoperatively. This is contingent upon the patient achieving full, painless range of motion and demonstrating at least 90% grip and forearm strength compared to the contralateral unaffected extremity. Interval throwing or swinging programs are highly recommended to ensure a graded return to peak mechanical loads.
Summary of Key Literature and Guidelines
The foundational understanding of epicondylitis pathophysiology was established by Nirschl and Pettrone, who first characterized the histology of angiofibroblastic hyperplasia, fundamentally shifting the paradigm away from acute inflammatory "itis" toward degenerative "osis." Their work established the biological rationale for surgical excision of the diseased tissue rather than simple fascial release.
Recent systematic reviews comparing open, percutaneous, and arthroscopic techniques for medial epicondylitis continue to support the open approach as the gold standard. While arthroscopic techniques have gained significant traction for lateral epicondylitis, the proximity of the ulnar nerve and the medial antebrachial cutaneous nerve makes arthroscopic debridement on the medial side technically demanding and fraught with a higher risk of neurological complications.
Current clinical practice guidelines emphasize a mandatory minimum of 6 months of comprehensive nonoperative management before considering surgical intervention. When patient selection is rigorous and surgical technique meticulously preserves the medial collateral ligament and regional neurovasculature, open debridement and repair yields good to excellent outcomes in 85% to 90% of patients, with durable long-term relief of pain and restoration of functional grip strength.
Clinical & Radiographic Imaging
















You Might Also Like