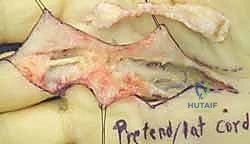
Dupuytren's Disease Fasciectomy: A Masterclass in Palmar and Digital Reconstruction
Key Takeaway
Welcome, fellows, to an immersive operative masterclass on Dupuytren's disease. We'll meticulously dissect the complex palmar anatomy, execute precise fasciectomy techniques, and navigate critical neurovascular structures. This session emphasizes real-time decision-making, meticulous dissection, and advanced strategies for managing contractures and preventing recurrence, ensuring optimal patient outcomes. Prepare to scrub in and master this challenging condition.
Understanding Dupuytren's Disease: A Unique Fibroproliferative Disorder
Welcome, fellows, to the operating theater. Today, we're tackling Dupuytren's disease (DD), a condition that, while seemingly straightforward, demands our utmost respect and a deep understanding of hand anatomy. This isn't just another inflammatory or neoplastic disorder; it’s a unique fibroproliferative process affecting the palmar fascial complex, leading to progressive contracture. While it shares some characteristics with normal wound healing, the relentless proliferation and abnormal collagen deposition are truly astonishing.
The Pathogenesis of Contracture: From Nodule to Cord
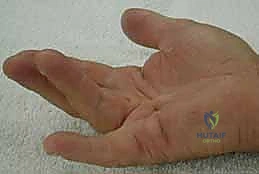
In DD, normal fascial bands transform into pathological cords. The hallmark of this disease is the presence of Dupuytren nodules and cords. Typically, a nodule appears first, often in the palm, followed by the development of cords. These cords, involving the palmar, palmodigital, or digital regions, progressively shorten, leading to the characteristic flexion deformities of the MCP and PIP joints.
- Pretendinous Cord: The most common cord, arising from the pretendinous band. It primarily causes MCP joint flexion deformity and can extend distally, contributing to digital cords. Occasionally, it bifurcates, forming a "commissural Y cord" extending into adjacent digits.

Figure: Pretendinous cord and nodule in the palm, causing MCP flexion contracture.
* Central Cord: An extension of the pretendinous cord into the digit.
* Lateral Cord: Originates from the lateral digital sheet, attaching to skin or the flexor tendon sheath near Grayson's ligament. It primarily causes PIP joint contracture but can also affect the DIP joint.
* Spiral Cord: A critical cord, most often seen in the small finger. It's composed of the pretendinous band, spiral band, lateral digital sheet, and Grayson ligament. Its relationship with the neurovascular bundle is crucial: initially superficial in the palm, it dives deep to the neurovascular bundle distal to the MCP joint, then runs lateral, and finally becomes superficial again as it involves Grayson's ligament. As it contracts, the neurovascular bundle spirals around the cord, making it highly vulnerable.
* Natatory Cord: Develops from the natatory ligament (NL), converting the normal U-shaped web space into a V-shape, leading to contracture of the second, third, and fourth web spaces.
* Abductor Digiti Minimi Cord: Also known as an isolated digital cord, originating from the abductor digiti minimi tendon or adjacent muscle fascia. It courses superficial to the neurovascular bundle, potentially displacing it medially. It inserts on the ulnar side of the middle phalanx, or sometimes the radial side or distal phalanx, causing PIP or DIP contracture.
* Commissural Cords:
* Distal Commissural Cord: Arises from the diseased distal commissural ligament (radial extension of the NL).
* Proximal Commissural Cord: Originates from the proximal commissural ligament (radial extension of the TLPA).
Both cause first web space contracture.
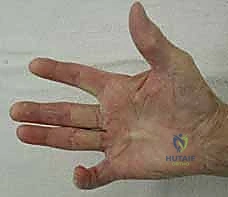
Figure: Two pretendinous cords with MCP and PIP contracture of the small finger, and a small proximal commissural cord in the first web space.
* Vertical Cords (Diseased Septa of Legueu and Juvara): These are short, thick cords connected to the pretendinous cord, extending deeply between the neurovascular bundle and the flexor tendon fibrous sheath.
* Grapow Vertical Bands: Become microcords, leading to skin thickening and pitting, often an early sign.
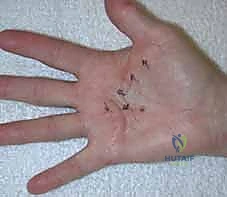
Figure: Diffuse Dupuytren palmar fascial disease with nodular thickening throughout the palm.
Comprehensive Surgical Anatomy: Navigating the Palmar Fascial Complex
Fellows, before we make any incision, a thorough understanding of the palmar fascial complex is paramount. This intricate network is where Dupuytren's disease wreaks havoc, and it's also where we'll be operating, millimeters away from vital neurovascular structures.
The Palmar Fascial Complex Components
The palmar fascial complex includes the radial, ulnar, and central aponeuroses, palmodigital fascia, and digital fascia.
- Radial Aponeurosis:
- Thenar fascia: An extension of the central aponeurosis.
- Thumb pretendinous band: Often small or absent, but can form a cord causing thumb MCP flexion deformity.
- Distal and proximal commissural ligaments: Give rise to the respective commissural cords causing first web space contracture.
- Ulnar Aponeurosis:
- Hypothenar muscle fascia: Extension of the central aponeurosis.
- Pretendinous band to the small finger: Consistently substantial, a common site for cord formation.
- Abductor digiti minimi confluence: Origin for the abductor digiti minimi cord.
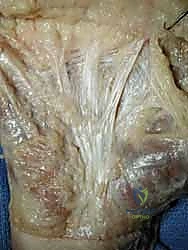
- Central Aponeurosis: This is the core of DD activity. It's triangular with a proximal apex.
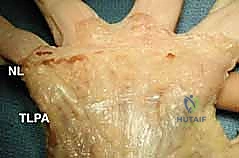
Figure: The central aponeurosis, triangular with a proximal apex, is the core of Dupuytren disease activity.
* Longitudinal fibers: Fan out as pretendinous bands to the central three digits. Each band bifurcates distally into three layers:
* Superficial layer: Inserts into the dermis, responsible for skin pits.
* Middle layer: Continues as the spiral band into the digit.
* Deep layer: Passes vertically dorsally towards the flexor tendon and its digital sheath.
* Transverse fibers: Form the natatory ligament (NL) in the distal palm and the transverse ligament of the palmar aponeurosis (TLPA) proximally, parallel to the NL.
* The TLPA lies deep to the pretendinous bands and gives origin to the septa of Legueu and Juvara.
* The NL's proximal fibers are transverse, but distal fibers form a U-shape, continuing longitudinally as the lateral digital sheet.
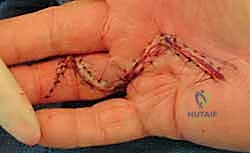
Figure: The transverse fibers forming the natatory ligament (NL) in the distal palm and the transverse ligament of the palmar aponeurosis (TLPA) proximally.
* Vertical fibers: Include the strong vertical bands of Grapow and the septa of Legueu and Juvara. These eight septa form seven fibro-osseous compartments: four flexor septal canals (containing flexor tendons) and three web space canals (containing common digital nerves, arteries, and lumbrical muscles).
* These septa insert into a soft tissue confluence comprising the A1 pulley, palmar plate, sagittal band, and inter-palmar plate ligament (IPPL).
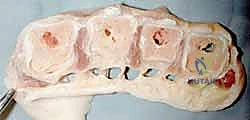
Figure: Septum of Legueu and Juvara in relation to the interpalmar plate ligament.
* They continue distally, deep to the neurovascular bundle and NL, emerging distally to contribute to the lateral digital sheet.
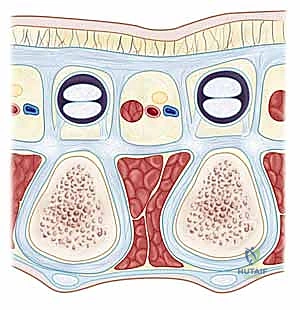
Figure: Three interpalmar plate ligaments (radial, central, ulnar) forming the floor of the three web space canals.
* Palmodigital Fascia: Encompasses terminal fibers of pretendinous bands, spiral bands, and the beginning of the lateral digital sheet.
* Digital Fascia: Surrounds the neurovascular bundle in the digit, including:
* Grayson ligament (palmar): Involved in the spiral cord, becoming superficial to the neurovascular bundle distally.
* Cleland ligaments (dorsal): Dorsal to the neurovascular bundle.
* Gosset lateral digital sheet (laterally): Has deep and superficial contributions from the spiral band and NL.
* Check-rein ligaments (medially and dorsally): Also known as Thomaine retrovascular fascia.
Neurovascular Relationships: The Critical Danger Zone
The neurovascular bundles are the most critical structures at risk during Dupuytren's surgery.
* Distorted Anatomy: As the cords contract, the neurovascular bundles, normally running lateral to the flexor tendons, become distorted. The spiral cord, in particular, wraps around the neurovascular bundle, displacing it medially and centrally. What was once superficial can become deep, and what was lateral can be pulled centrally.
* Protection: Always assume the neurovascular bundle is not in its expected anatomical position. Meticulous, sharp dissection, especially in the digital rays, is imperative.
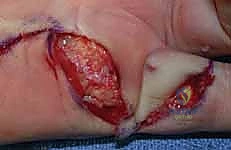
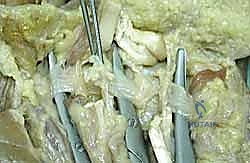
Figure: Intraoperative view highlighting the intricate relationship between diseased cords and neurovascular structures.
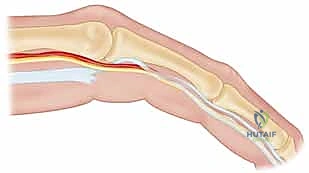
Figure: Careful dissection revealing a neurovascular bundle displaced by a contracting Dupuytren's cord.
Preoperative Planning and Patient Positioning
Fellows, proper planning and positioning are the foundation for a successful outcome in Dupuytren's surgery.
Indications for Surgical Intervention
Surgery is indicated for symptomatic and severe DD.
* MCP Joint Contracture: Greater than 30 degrees.
* PIP Joint Contracture: Greater than 15 degrees.
* Presence of a well-developed cord that interferes with hand function.
* Dermofasciectomy: Procedure of choice for recurrent or aggressive disease, especially with marked skin adherence.
Preoperative Templating & Imaging
While not always requiring extensive imaging, we must carefully assess the extent of the disease.
* Clinical Assessment: Palpate all cords, assess joint contractures (using a goniometer), and check for skin tethering. Document the exact location and severity.
* Fluoroscopy: Not typically used for Dupuytren's fasciectomy unless there's a need to assess bony involvement or for specific joint releases, which is rare. Our focus here is soft tissue.
Patient Positioning
- Supine Position: The patient is positioned supine on the operating table.
- Hand Table: The affected hand is placed on a specialized hand table, ensuring it is stable and allows for full manipulation and access.
- Shoulder Abduction: The shoulder is abducted to 90 degrees, allowing for comfortable positioning of the arm and hand, preventing nerve compression, particularly of the brachial plexus.
- Pneumatic Tourniquet: A padded pneumatic tourniquet is applied as proximally as possible on the upper arm.
- Exsanguination: The upper extremity is exsanguinated using an Esmarch bandage to achieve a bloodless field.
- Inflation: The tourniquet is then inflated to 250 mm Hg (or 100 mmHg above systolic blood pressure), providing excellent visibility, which is crucial for identifying delicate neurovascular structures.
- Anesthesia: Local, regional (e.g., axillary block), or general anesthesia can be used, depending on the extent of the procedure and patient comorbidities. For extensive cases, general anesthesia or a regional block with sedation is often preferred.
Intraoperative Execution: A Step-by-Step Masterclass
Now, let's scrub in. We'll proceed with a partial fasciectomy, the most widely used technique, focusing on meticulous dissection and complete cord excision while preserving normal tissue.
Approach and Incisions
The choice of incision is critical for optimal exposure and minimizing skin complications.
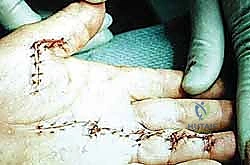
- Brunner Zigzag Incision: This is the most commonly used incision. It provides excellent exposure to the underlying cords while allowing for lengthening of the skin during closure, reducing the risk of contracture and skin necrosis.
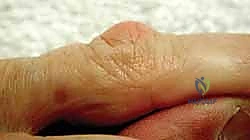
Figure: The Brunner zigzag incision, commonly used for Dupuytren's fasciectomy.
* Execution: Carefully plan the zigzag angles to avoid sharp corners that can necrose. The apices of the flaps should be blunt.
* Midline Longitudinal Incision with Multiple Z-plasties: An alternative for extensive palmar disease, particularly when primary closure is challenging. The Z-plasties help lengthen the skin and prevent scar contracture.
Figure: Midline longitudinal incision closed with multiple Z-plasties.
* Transverse Palmar Incisions: Can be used for the "open palm" method or for very extensive palmar fascial complex disease where primary closure is not anticipated or desired. This method has advantages in terms of less pain and better motion, but prolonged wound healing is a disadvantage.
Meticulous Dissection and Cord Excision (Partial Fasciectomy)
Our goal is selective excision of diseased tissue while preserving normal fascia. This requires patience and precision.
- Skin Incision: Using a #15 blade, make the planned incision through the skin and subcutaneous tissue. Maintain perpendicularity to the skin to avoid beveling.
- Skin Flap Elevation: Carefully elevate the skin flaps. Use fine skin hooks for retraction, ensuring not to traumatize the skin edges, as Dupuytren's skin is often thin and adherent.
Figure: Intraoperative view of Dupuytren's cords exposed beneath elevated skin flaps.
3. Initial Cord Transection: Begin by identifying a prominent cord. Often, the pretendinous cord is the most accessible. We'll start proximally in the palm.
* Probing and Release: Use a fine blunt probe or a small curved hemostat to gently lift the cord away from deeper structures. Once isolated, carefully transect the cord. This initial release often allows the digit to extend partially, providing better access to more distal structures.
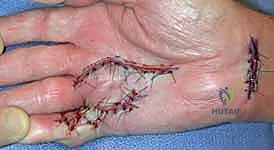
Figure: Initial transection of a Dupuytren's cord, allowing for partial digital extension.
4. Neurovascular Bundle Identification and Protection: This is the most critical step.
* Locate the Neurovascular Bundles: Start proximally where the bundles are typically lateral to the flexor tendons and more superficial. Follow them distally.
* Dissect Around the Cord: Always dissect around the diseased cord, never directly through it, until the neurovascular bundle is positively identified and protected. The spiral cord, in particular, will have the neurovascular bundle wrapped around it.
* Magnification: Use loupes (2.5x to 3.5x magnification) for all deep dissection to clearly visualize the nerves and vessels.
* Fine Instruments: Employ fine dissecting scissors (e.g., tenotomy scissors) and fine forceps (e.g., Adson with teeth) for precise control.
* Blunt Dissection: Use a fine blunt dissector or a small nerve hook to gently tease the neurovascular bundle away from the cord.
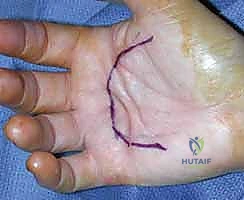
Figure: Meticulous dissection to identify and protect the neurovascular bundle, which is often displaced by the contracting cord.
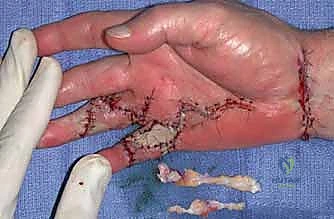
Figure: Intraoperative view demonstrating the careful separation of a digital nerve from an adherent Dupuytren's cord.
> **SURGICAL WARNING:** The neurovascular bundle can be intimately adherent to the diseased cord. *Never* pull on the cord without first ensuring the bundle is free. Gentle traction on the digit can help identify cords, but *never* on the neurovascular structures. Always assume the nerve is displaced.
- Excision of Specific Cords:
- Pretendinous Cords: Excise these from their origin in the central aponeurosis to their distal insertion into the dermis or into the digital cords.
- Spiral Cords: Once the neurovascular bundle is completely freed, the spiral cord can be excised. Ensure complete release of all components (pretendinous band, spiral band, lateral digital sheet, Grayson ligament).
- Lateral Cords: Dissect these from the lateral digital sheet, carefully separating them from the neurovascular bundle.
- Natatory Cords: Release these in the web space. This often involves transecting the U-shaped fibers to restore the web space.
- Vertical Cords (Septa of Legueu and Juvara): These are deeper and require careful dissection between the neurovascular bundle and flexor tendon sheath.
- Abductor Digiti Minimi Cord: Follow its course superficial to the neurovascular bundle, carefully releasing any adherence or displacement of the bundle.
- Commissural Cords: Release these in the first web space to address thumb abduction contracture.
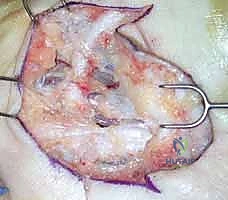
Figure: Excision of a complex Dupuytren's cord system, demonstrating the extent of tissue removal.
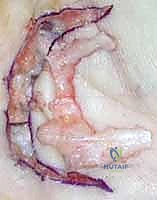
Figure: Post-excision view, showing the cleared surgical field and preserved neurovascular structures.
6. Assess Joint Extension: After all visible cords are excised, passively extend the affected digits and assess the range of motion.
* PIP Joint Check-Rein Ligament Release: If a PIP joint contracture of 40 degrees or more persists after conventional fasciectomy, a check-rein ligament release is indicated. These ligaments are deep to the neurovascular bundles, extending from the flexor tendon sheath to the proximal phalanx. Carefully identify and release these structures using a small periosteal elevator or fine scissors, taking care not to damage the underlying flexor tendons or the neurovascular bundles.
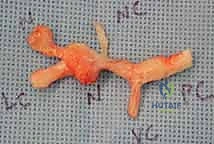
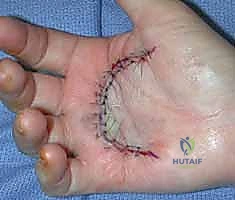
Figure: Intraoperative image demonstrating the release of a PIP joint check-rein ligament to improve extension.
Dermofasciectomy
For recurrent or aggressive disease, especially with marked skin adherence, dermofasciectomy is the procedure of choice.
* Excision of Skin and Diseased Tissue: This involves excising not only the diseased fascia but also the overlying skin.
* Skin Grafting: The resulting skin defect is then covered with a full-thickness skin graft, typically harvested from the groin or inner arm. Secure the graft with sutures and a tie-over dressing.
Extensive Fasciectomy
Indicated for broad involvement of the palmar fascial complex, including the NL and TLPA.
* Wide Excision: A generous fasciectomy of most of the palmar fascial complex is performed.
* Closure: The skin can sometimes be closed primarily. If a defect remains, it can be skin grafted or left open (similar to the open palm method).
Wound Closure
- Hemostasis: Ensure meticulous hemostasis. Release the tourniquet and address any bleeding points with bipolar cautery.
- Irrigation: Lavage the wound with saline.
- Skin Closure:
- Primary Closure: For Brunner incisions, close the skin flaps carefully with fine non-absorbable sutures (e.g., 4-0 or 5-0 nylon), ensuring eversion of the skin edges.
- Local Rotation Flaps: If there are areas of exposed flexor tendons or neuro
Additional Intraoperative Imaging & Surgical Steps
REFERENCES
-
Badalamente M, Hurst L. Enzyme injection as nonsurgical treatment of Dupuytren disease. J Hand Surg Am 2000;25A:629–636.
-
Bilderback K, Rayan G. Dupuytren’s cord involving the septa of Legueu and Juvara: a case report. J Hand Surg Am 2002;27A:344–346.
-
Bilderback K, Rayan G. The septa of Legueu and Juvara: an anatomic study. J Hand Surg Am 2004;29A:494–499.
-
Boyer M, Gelberman R Complications of the operative treatment of Dupuytren disease. Hand Clin 1999;15:161–166.
-
Brenner P, Rayan G. Dupuytren’s Disease: A Concept of Surgical Treatment. Vienna: Springer, 2002.
-
Elliot D. The early history of Dupuytren disease. Hand Clin 1999; 15:1–19.
You Might Also Like