Mastering the Lapidus Procedure: A Comprehensive Intraoperative Guide
Key Takeaway
This masterclass guides fellows through the Lapidus procedure for hallux valgus with first TMT hypermobility. We meticulously cover patient selection, detailed surgical anatomy, precise intraoperative steps including joint preparation and stabilization, and critical pearls to ensure successful arthrodesis. Emphasis is placed on neurovascular protection, accurate deformity correction, and comprehensive postoperative management, preparing you for complex forefoot reconstruction.
Introduction and Epidemiology
Paul W. Lapidus originally described a comprehensive procedure for the correction of hallux valgus in 1934. This seminal procedure was founded on the fundamental biomechanical premise that hallux valgus is a secondary phenomenon to metatarsus primus varus arising from first tarsometatarsal joint hypermobility and a medially oriented first tarsometatarsal articulation. The original Lapidus procedure entailed the excision of the lateral aspect of the medial cuneiform and first tarsometatarsal arthrodesis, coupled with a distal first metatarsophalangeal capsulorrhaphy.

Over the subsequent decades, many modifications of the original Lapidus procedure have been introduced. Modern iterations primarily advocate for rigid internal fixation as a means for the maintenance of reduction, achieving lower nonunion rates, and facilitating earlier healing and mobilization. The prevalence of hallux valgus is significant, affecting nearly 23% of adults aged 18 to 65 years and up to 35% of adults over the age of 65. Within this demographic, the subset of patients presenting with concomitant first tarsometatarsal instability or hypermobility represents a unique surgical challenge that cannot be adequately addressed with distal or diaphyseal osteotomies alone.

Understanding the epidemiology of first ray hypermobility is complicated by the historical debate regarding its definition and measurement. However, it is well documented that generalized ligamentous laxity, often seen in conditions such as Ehlers-Danlos or Marfan syndrome, significantly increases the risk of severe, recurrent hallux valgus. Even in the absence of syndromic laxity, hypermobility of the first ray is a common anatomic variant that predisposes individuals to progressive forefoot deformity.

Surgical Anatomy and Biomechanics
The primary goal of reconstructive foot surgery is to obtain a plantigrade position with normal underlying mechanical alignment. This alignment is critical to allow for optimal weight bearing, shock absorption, accommodation to uneven terrain, and the generation of power for an efficient, painless gait cycle.

Foot Column Mechanics and Weight Distribution
Weight should be evenly distributed across the six primary weight-bearing surfaces of the foot, which consist of the paired sesamoids underlying the first metatarsal head, the lesser metatarsal heads, and the calcaneal tuberosity. The foot is functionally divided into medial and lateral columns. The lateral column of the foot is designed for mobility to accommodate uneven surfaces during the contact phase of gait. Conversely, the medial column, which includes the first tarsometatarsal joint, is inherently more rigid to allow efficient power generation for terminal stance and push-off.

First Tarsometatarsal Joint Anatomy
The first tarsometatarsal joint is a complex, kidney-shaped articulation between the base of the first metatarsal and the medial cuneiform. It is typically 30 mm in the dorsoplantar plane and half as wide in the mediolateral plane. The joint capsule is reinforced by strong dorsal and plantar ligaments. The plantar ligaments are particularly robust, providing primary resistance against dorsal subluxation of the first metatarsal during weight-bearing. The interosseous Lisfranc ligament complex, originating from the lateral aspect of the medial cuneiform and inserting onto the medial base of the second metatarsal, further stabilizes the medial column to the middle column.

Pathogenesis of Hypermobility
Debate exists within the orthopedic literature regarding whether first tarsometatarsal hypermobility is a primary or secondary phenomenon. Patients develop first tarsometatarsal hypermobility potentially in both the axial and sagittal planes. Axial instability presents as metatarsus primus varus and resultant hallux valgus. Sagittal instability presents as a dorsiflexed first metatarsal with a predisposition to dorsolateral peritalar subluxation. Furthermore, many patients have a medially oriented first tarsometatarsal joint facet and a tendency toward metatarsus primus varus.
Equinus is often an underlying pathologic feature predisposing the midfoot to increased repetitive tension and subsequent longitudinal collapse and instability. The restricted ankle dorsiflexion forces compensatory midfoot breakdown, particularly at the tarsometatarsal and naviculocuneiform joints, exacerbating first ray elevation and subsequent transfer loading to the lesser metatarsals.

Indications and Contraindications
Symptomatic hallux valgus associated with metatarsus primus varus, underlying first tarsometatarsal hypermobility, and equinus presents with progressive deformity and pain. In the face of underlying pathologic first tarsometatarsal hypermobility or equinus, the hallux valgus deformity will inevitably progress over time in both symptomatology and degree of deformity. Consequently, it is imperative to treat any underlying pathology concomitantly with the treatment of the hallux valgus deformity.

The decision to proceed with a Lapidus procedure hinges on careful patient selection, taking into account the degree of deformity, the presence of hypermobility, and patient comorbidities.
| Parameter | Operative Indications | Non Operative Indications and Contraindications |
|---|---|---|
| Deformity Severity | Severe hallux valgus (IMA > 15 degrees, HVA > 40 degrees) | Mild to moderate deformity without hypermobility |
| Joint Stability | First TMT hypermobility or clinical instability | Stable first TMT joint (consider distal/shaft osteotomy) |
| Recurrence | Recurrent hallux valgus after previous osteotomy | First-time mild presentation amenable to shoe modification |
| Ligamentous Status | Generalized ligamentous laxity (e.g., Ehlers-Danlos) | Normal ligamentous tension with isolated distal deformity |
| Patient Factors | High-demand patient requiring medial column stability | Active infection, severe peripheral vascular disease, Charcot neuroarthropathy (relative), non-compliant patient |
| Skeletal Maturity | Closed physes | Open physes (absolute contraindication) |

The classic indication for the Lapidus procedure is a patient with a severe hallux valgus deformity and clinical evidence of first ray hypermobility. Additionally, patients with degenerative joint disease of the first tarsometatarsal joint alongside hallux valgus are ideal candidates, as the arthrodesis addresses both the deformity and the arthritic pain simultaneously.

Pre Operative Planning and Patient Positioning
Thorough preoperative evaluation is paramount to the success of the Lapidus procedure. This involves a detailed physical examination and a comprehensive radiographic assessment.

Clinical Examination and Radiographic Assessment
Physical examination methods must include an assessment of first tarsometatarsal hypermobility. The examiner rests the index and middle finger of one hand over the dorsal aspect of the first tarsometatarsal joint to monitor motion. The thumb of that hand rests under the lesser metatarsals. The other hand grasps the first metatarsal between the thumb and fingers and translates it dorsally and plantarly. Minimal motion should be palpated at this joint in a normal foot. Excessive motion or translation (greater than 9 mm) is pathologic and indicative of first tarsometatarsal hypermobility and instability. Occasionally, intercuneiform instability is also noted and must be addressed.
The Silfverskiöld test is utilized to evaluate for equinus. The examiner corrects the hindfoot to a neutral subtalar position and checks dorsiflexion range of motion both with the knee in full extension and flexed greater than 25 degrees. An inability to obtain 5 degrees of dorsiflexion with the knee in straight extension that improves with flexion is indicative of isolated gastrocnemius equinus. An inability to obtain 10 degrees of dorsiflexion in both knee extension and flexion is indicative of combined soleus and gastrocnemius equinus.
First metatarsophalangeal range of motion must also be assessed. The examiner assesses flexion and extension of the first metatarsophalangeal joint and repeats the test with the first metatarsal held in a corrected position to ensure that the joint remains congruous and mobile once the metatarsus primus varus is reduced.

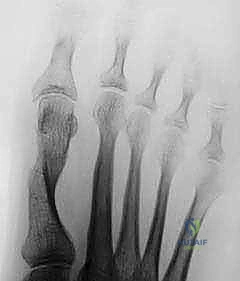
Radiographic evaluation requires standard weight-bearing anteroposterior, lateral, and sesamoid axial views of the foot. The intermetatarsal angle, hallux valgus angle, and distal metatarsal articular angle should be measured. A first intermetatarsal angle greater than 15 degrees and a hallux valgus angle greater than 40 degrees are typical thresholds for a Lapidus procedure. The lateral radiograph is scrutinized for dorsal elevation of the first metatarsal (sagittal breach) and Meary's angle intersection.

Patient Positioning and Operating Room Setup
The patient is positioned supine on the operating table. A bump is placed under the ipsilateral hip to internally rotate the lower extremity to a neutral position, ensuring the patella is facing directly anteriorly. This allows clear access to both the medial and lateral aspects of the foot. A well-padded thigh or calf tourniquet is applied to provide a bloodless surgical field. Fluoroscopy should be positioned to enter from the contralateral side of the table, allowing for unobstructed anteroposterior, oblique, and lateral intraoperative imaging.
Detailed Surgical Approach and Technique
The modern Lapidus procedure involves a meticulous sequence of soft tissue balancing, joint preparation, multiplanar deformity correction, and rigid internal fixation.

Incision and Soft Tissue Dissection
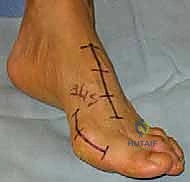
The procedure typically begins with the distal soft tissue release. A dorsal first web space incision is made to access the lateral aspect of the first metatarsophalangeal joint. The adductor hallucis tendon is identified and released from its insertion on the base of the proximal phalanx and the fibular sesamoid. The deep transverse metatarsal ligament is transected, and a lateral capsulotomy is performed to allow for derotation and reduction of the sesamoid apparatus.

Attention is then directed to the first tarsometatarsal joint. A dorsomedial longitudinal incision is utilized, extending from the mid-shaft of the first metatarsal to the navicular. Careful superficial dissection is required to identify and protect the medial dorsal cutaneous nerve and the saphenous nerve branches. The extensor hallucis longus tendon is retracted laterally, and the tibialis anterior tendon is identified and protected medially.

A longitudinal capsulotomy is performed over the first tarsometatarsal joint. Subperiosteal flaps are elevated dorsally and plantarly to expose the articulation fully. A lamina spreader or Hintermann retractor is inserted into the joint to distract the surfaces and provide visualization of the deep plantar and lateral joint margins.

Joint Preparation and Deformity Correction
Meticulous joint preparation is critical to achieving a high union rate. The articular cartilage of the base of the first metatarsal and the distal aspect of the medial cuneiform is removed. This can be accomplished using a combination of sharp osteotomes, curettes, and a high-speed burr, or via parallel planar saw cuts. If saw cuts are utilized, minimal bone resection is paramount to prevent excessive shortening of the first ray. The subchondral bone plate should be breached via fenestration (using a 2.0 mm drill bit) or fish-scaling with a small osteotome to expose cancellous bone and promote osteogenesis.

Correction of the deformity must occur in three planes. The first metatarsal is translated laterally to reduce the intermetatarsal angle, plantarflexed to correct the sagittal elevation and restore the medial longitudinal arch, and derotated (supinated) to correct the frontal plane pronation of the first ray. This triplanar correction is the hallmark of a successful Lapidus arthrodesis.

Reduction and Rigid Internal Fixation
Once the optimal multiplanar reduction is achieved, it is provisionally held with smooth Kirschner wires. Intraoperative fluoroscopy is utilized to confirm the reduction of the intermetatarsal angle, the restoration of the sagittal alignment, and the anatomic position of the sesamoids.

Rigid internal fixation is then applied. Historically, crossed 3.5 mm or 4.0 mm cortical screws were the gold standard. The "home run" screw is typically placed from the dorsal-distal aspect of the first metatarsal, directed plantarly and proximally into the medial cuneiform. A second screw is placed from the dorsal-proximal medial cuneiform into the plantar-distal first metatarsal.

Modern advancements frequently utilize anatomically contoured locking plates applied to the dorsal, medial, or plantar aspect of the joint, often in conjunction with an interfragmentary compression screw. Plantar plating provides superior biomechanical stability by acting on the tension side of the joint, neutralizing the dorsal bending moments experienced during weight-bearing. Following fixation, the medial eminence of the first metatarsal head is resected, and a medial capsulorrhaphy is performed to maintain the hallux in a rectus position.
Complications and Management
Despite excellent outcomes in properly selected patients, the Lapidus procedure carries a specific complication profile that surgeons must be prepared to manage.

Nonunion historically represented the most significant complication, with early literature reporting rates as high as 10% to 15%. However, with the advent of rigid locking plate technology and meticulous joint preparation techniques, modern nonunion rates have decreased to less than 5%.

Malunion, particularly in dorsiflexion, is a devastating complication. Dorsal elevation of the first ray removes the load-bearing capacity of the medial column, leading to severe transfer metatarsalgia and lesser metatarsal overload, often culminating in lesser metatarsal stress fractures or plantar plate tears.

| Complication | Incidence | Prevention and Salvage Strategies |
|---|---|---|
| Nonunion / Delayed Union | 2% to 5% | Prevention: Meticulous cartilage removal, subchondral fenestration, rigid compression. Salvage: Revision arthrodesis with autogenous bone grafting and robust locking plate fixation. |
| Dorsiflexion Malunion | 1% to 3% | Prevention: Intraoperative lateral fluoroscopy; deliberate plantarflexion of the 1st metatarsal during pinning. Salvage: Plantarflexion opening wedge osteotomy of the medial cuneiform or metatarsal base. |
| Shortening of the First Ray | Common (1-3 mm) | Prevention: Joint preparation with curettes rather than aggressive saw cuts. Salvage: Structural interposition bone graft if shortening causes severe transfer metatarsalgia. |
| Hardware Prominence | 5% to 10% | Prevention: Use of low-profile plates; avoiding prominent dorsal screw heads. Salvage: Hardware removal after radiographic confirmation of solid fusion (typically >6 months). |
| Recurrence of Deformity | 2% to 4% | Prevention: Complete lateral release; addressing frontal plane rotation; ensuring rigid TMT fusion. Salvage: Revision Lapidus or proximal osteotomy, depending on the site of failure. |
| Nerve Injury (MDCN) | 1% to 2% | Prevention: Careful blunt dissection in the subcutaneous tissues over the TMT joint. Salvage: Neuroma excision and burying the stump into muscle or bone if conservative measures fail. |

Post Operative Rehabilitation Protocols
The postoperative rehabilitation protocol must balance the need for early mobilization to prevent stiffness with the necessity of protecting the arthrodesis site to ensure bony union.

Historically, patients were maintained strictly non-weight-bearing in a short leg cast for six to eight weeks.
Clinical & Radiographic Imaging































You Might Also Like