Masterclass: Precision Reconstruction of Boutonnière and Swan-Neck Deformities
Key Takeaway
Step into the operating theater for an in-depth masterclass on reconstructing Boutonnière and Swan-Neck deformities. This guide covers comprehensive anatomy, meticulous preoperative planning, real-time intraoperative execution, critical pearls and pitfalls, and comprehensive postoperative management. Fellows will gain a granular understanding of techniques to restore digital function and stability, addressing both post-traumatic and rheumatoid etiologies with precision.
Introduction: Navigating Digital Deformities in the OR
Alright, fellows, gather 'round. Welcome to the operating theater. Today, we're tackling two of the most challenging and functionally debilitating deformities of the hand: the Boutonnière and Swan-Neck deformities. These are not merely cosmetic issues; they represent a profound imbalance within the intricate extrinsic and intrinsic tendon systems of the digit, leading to progressive dysfunction. Our goal today is not just to correct the deformity, but to restore the delicate biomechanical equilibrium of the digit, ensuring optimal long-term function for our patient.
Remember, the root cause often lies in a systemic process like rheumatoid arthritis, a poorly understood inflammatory disease characterized by synovial proliferation, angiogenesis, and lymphocytosis. This leads to cartilage degeneration, synovial expansion, periarticular erosion, and ligamentous laxity, ultimately disrupting the finely tuned extensor and flexor mechanisms. In other cases, trauma can be the culprit. Regardless of etiology, our approach demands precision, a deep understanding of anatomy, and a nuanced appreciation of digital biomechanics.
Preoperative Planning and Patient Positioning: Setting the Stage for Success
Before we even make an incision, meticulous planning is paramount. This isn't just about the patient; it's about the entire surgical team, ensuring we're all on the same page.
Preoperative Assessment and Templating
For both Boutonnière and Swan-Neck deformities, a thorough clinical examination is critical. We assess the flexibility of the deformity, the presence of fixed contractures, and the integrity of the surrounding soft tissues.
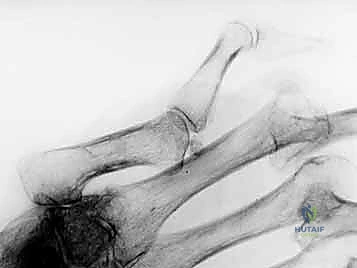
* Radiographs: Standard AP, lateral, and oblique views are essential to evaluate joint alignment, articular destruction, and any associated avulsion fractures. For the thumb, a true lateral view is crucial for assessing MCP and IP joint alignment.
* Fluoroscopy Setup: While not always required for every step, having a C-arm readily available is prudent, especially if we anticipate joint releases, arthroplasties, or internal fixation. We'll position it to allow clear lateral and AP views of the affected digit without repositioning the patient.
* Patient Communication: Discuss realistic outcomes, potential limitations, and the extensive postoperative rehabilitation required.
Patient Positioning and OR Table Setup
Our patient is already supine on the operating table.
1. Arm Board: The affected upper extremity will be positioned on a specialized hand table or arm board, ensuring it's stable, well-padded, and allows for full range of motion assessment intraoperatively. We want the hand to be pronated or supinated as needed, with the digits easily accessible.
2. Tourniquet: A pneumatic tourniquet will be applied to the proximal arm. We'll inflate this to 250 mmHg to ensure a bloodless field, which is absolutely critical for visualizing the delicate structures we're working with.
3. Draping: Standard sterile draping, isolating the hand and forearm, allowing maximum exposure while maintaining sterility. Ensure the drape allows for full range of motion of the digit during intraoperative assessment.
Comprehensive Surgical Anatomy: The Blueprint of the Hand
Before we touch the scalpel, let's review the intricate anatomy we'll encounter. This isn't just theory; it's our roadmap.
Bone and Joint Architecture
- Metacarpophalangeal (MCP) Joint: This is a condyloid joint, offering significant motion, typically from 15 degrees of hyperextension to 90 degrees of flexion. Its stability is highly dependent on the surrounding soft tissues, particularly the collateral ligaments and the sagittal bands. The shape of the metacarpal head creates a "cam effect" for the collateral ligaments, making them taut in flexion and lax in extension.
- Proximal Interphalangeal (PIP) Joint: A hinge joint, inherently more stable than the MCP due to the congruent articulation of the proximal phalanx condyles with the median ridge of the middle phalanx base.
- Volar Plate: A thick, fibrocartilaginous structure originating from the A2 pulley on the proximal phalanx and inserting into the "rough area" at the base of the middle phalanx. It is the primary restraint against PIP joint hyperextension.
- Collateral Ligaments: These are taut throughout the PIP joint's arc of motion, providing crucial lateral stability.

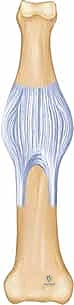
Figure 1A illustrates these critical PIP joint relationships.
* Distal Interphalangeal (DIP) Joint: Stabilized by the collateral ligaments, the terminal extensor tendon insertion, the flexor digitorum profundus (FDP) insertion, and its own volar plate.
Dorsal Restraining Structures and Extensor Mechanism
The dorsal digital extensor apparatus is a complex interplay of extrinsic extensor tendons and intrinsic musculature.
- Extrinsic Extensor Tendon (Ext): At the level of the distal hand, it splits into two lateral slips (LS) and the central tendon slip (CS).
- Sagittal Bands (sb): These originate from the radial and ulnar sides of the MCP joint volar plate and the volar base of the proximal phalanx, inserting into the lateral margins of the extensor tendon over the dorsal MCP joint. They stabilize the extrinsic extensor tendon, preventing lateral subluxation and contributing indirectly to MCP joint extension by preventing bowstringing.
- Interosseous Muscles (IOM): The deep head courses superficial to the sagittal band at the MCP joint level, forming the transverse fibers (T) of the extensor apparatus over the proximal phalanx. These contribute to MCP joint flexion.
- Lumbrical Muscle (L): On the radial aspect, forms the oblique fibers (O) of the extensor apparatus.
- Central Slip (CS): Inserts at the dorsal base of the middle phalanx, primarily extending the PIP joint.
- Lateral Slips (LS): Join with the oblique fibers of the lumbrical tendons (O) to form the conjoined lateral bands (clb).
- Conjoined Lateral Bands (clb): Converge over the middle phalanx to form the terminal tendon (TT), which inserts at the dorsal base of the distal phalanx, extending the DIP joint.
- Triangular Ligament (TL): Stabilizes the two conjoined lateral bands over the dorsal aspect of the middle phalanx, preventing their volar subluxation.
- Transverse Retinacular Ligament (TRL): Composed of volar-dorsally oriented fibers at the PIP joint level, it prevents dorsal subluxation of the conjoined lateral bands.
- Oblique Retinacular Ligament (ORL): A static ligament linking the PIP and DIP joints. It runs from the fibro-osseous gutter (middle third of the proximal phalanx and A2 flexor pulley) to insert into the terminal extensor tendon, passively coupling PIP and DIP joint extension.
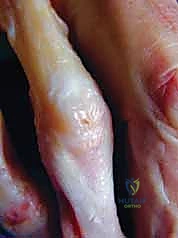
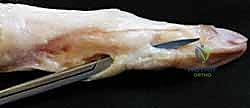
Figure 1B illustrates the dorsal digital extensor apparatus, showing the extrinsic extensor tendon (Ext), sagittal band (sb), lateral slips (LS), central slip (CS), interosseous muscle (IOM), lumbrical (L), transverse fibers (T), and oblique fibers (O).
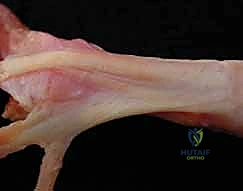
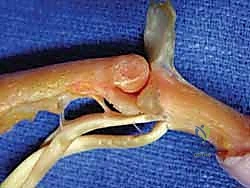
Figure 1C details the trifurcation of the extrinsic extensor tendon into the central slip (CS) and two lateral slips, which form the conjoined lateral bands (clb) with lumbrical contributions, ultimately forming the terminal tendon (TT). Note the triangular ligament (TL).
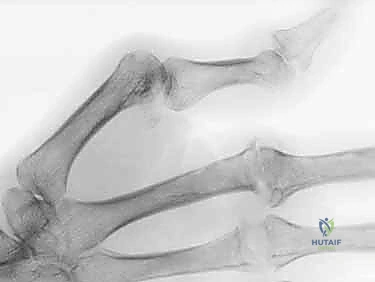
Figure 1D provides a lateral view, highlighting the coalescing lateral slip (LS) and oblique fibers (O) forming the conjoined lateral band (clb), the terminal tendon (TT), and the roles of the transverse retinacular ligament (TRL) and oblique retinacular ligament (ORL).
Flexor Tendon System
- Flexor Digitorum Superficialis (FDS) and Profundus (FDP): At the A1 pulley level, the FDS tendon flattens and bifurcates, allowing the FDP tendon to pass distally to insert at the volar base of the distal phalanx. The FDS slips then rotate laterally and dorsally around the FDP, dividing again. Medial slips rejoin dorsal to the FDP and insert into the distal aspect of the proximal phalanx, while lateral slips continue distally to insert into the base of the middle phalanx.
Neurovascular Risks
- Digital Nerves and Arteries: The dorsal digital nerves and veins are superficial and run along the sides of the extensor mechanism. During dorsal approaches, meticulous dissection is required to protect these structures. The proper digital nerves and arteries run more volarly, but their branches can be encountered during deeper dissection or volar approaches.
- Muscular Intervals: Dorsal approaches typically involve splitting the extensor mechanism longitudinally, or dissecting between the sagittal bands and lateral slips. Volar approaches for FDS tenodesis involve careful identification and isolation of the FDS slip within the flexor sheath, avoiding injury to the FDP and neurovascular bundles.
Pathogenesis of Deformities: Understanding the Imbalance
Boutonnière Deformity
This "buttonhole" deformity involves PIP joint flexion and DIP joint hyperextension, often with MCP joint hyperextension.
* Inciting Pathology: Disruption of the central slip, either from forceful hyperflexion (closed injury, sometimes with an avulsion fracture) or dorsal laceration (open injury).
* Mechanism: Loss of central slip integrity allows the PIP joint to "buttonhole" through the extensor mechanism. The lateral bands, normally dorsal to the PIP joint axis of rotation, subluxate volarly due to attenuation of the triangular ligament. Once volar, these lateral bands become flexors of the PIP joint and, simultaneously, extensors of the DIP joint (via the terminal tendon).
* Progression: Persistent PIP flexion leads to contracture of the volar plate, collateral ligaments, and ORL, resulting in a stiff, fixed deformity.

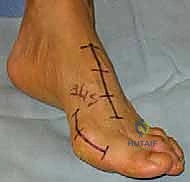
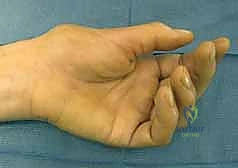
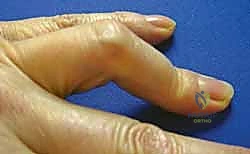
Figure 2A shows a classic Boutonnière deformity of the finger with PIP flexion and DIP hyperextension.
Rheumatoid Boutonnière: Pathologic synovitis of the PIP joint directly attenuates the central slip, triangular ligament, and transverse retinacular ligaments. In the thumb (Type I), MCP joint flexion and IP joint hyperextension are common, often exacerbated by attenuation of the sagittal band, causing the EPL tendon to subluxate volarly and become an MCP flexor.
Swan-Neck Deformity
Characterized by PIP joint hyperextension and DIP joint flexion, often with MCP joint flexion.
* Inciting Pathology: Volar plate insufficiency at the PIP joint is a common cause, allowing unchecked central slip action. This can result from trauma (e.g., recurrent dorsal PIP dislocations) or generalized ligamentous laxity. Avulsion of the terminal tendon can also concentrate extensor forces at the central slip, causing PIP hyperextension.
* Mechanism: The PIP joint hyperextends. Attenuation of the transverse retinacular ligament permits dorsal migration of the lateral bands relative to the PIP joint axis. These dorsally displaced lateral bands become constant hyperextension forces on the PIP joint, while simultaneously increasing the flexion force on the DIP joint.
* Progression: Persistent PIP hyperextension leads to contracture of the extensor apparatus (especially the triangular ligament) and skin, resulting in a stiff, fixed hyperextension contracture.
Rheumatoid Swan-Neck: Pathologic synovitis can affect MCP, PIP, or DIP joints. Chronic PIP synovitis, combined with altered joint mechanics, leads to progressive attenuation of the volar plate, collateral ligaments, and FDS tendon insertion, culminating in PIP hyperextension. Digital flexor tenosynovitis can also contribute by increasing extensor imbalance. In the thumb (Type III), CMC joint synovitis and subluxation cause MCP hyperextension and IP flexion.
Step-by-Step Intraoperative Execution: The Operating Surgeon's Viewpoint
Alright, fellows, let's scrub in. We'll start with a general approach, then delve into specific techniques for each deformity.
General Intraoperative Principles
- Tourniquet Inflation: Nurse, please inflate the tourniquet now. We want a perfectly bloodless field.
- Incision Planning: Always plan your incision to allow adequate exposure, permit future extensile approaches if needed, and minimize scar contracture over the joint. Longitudinal or curvilinear incisions are generally preferred.
- Meticulous Dissection: The hand is a landscape of delicate structures. Sharp dissection, careful hemostasis, and constant awareness of neurovascular bundles are paramount.
Procedure 1: Boutonnière Deformity Reconstruction
For this patient, we are addressing a chronic, flexible Stage II Boutonnière deformity of the long finger, likely post-traumatic, with significant central slip attenuation and volar subluxation of the lateral bands.
A. Surgical Approach and Exposure
- Incision: "Alright, let's begin. I'm making a dorsal curvilinear incision centered over the PIP joint, extending approximately 1.5 cm proximal and distal to the joint line. We'll curve it slightly to avoid a straight-line scar over the joint, which can lead to contracture."
- Rationale: This curvilinear approach provides excellent exposure while minimizing the risk of scar contracture and allowing for skin flap elevation.
- Subcutaneous Dissection: "Now, with a small scalpel, we'll carefully incise the skin. Then, using tenotomy scissors and fine forceps, we'll perform meticulous subcutaneous dissection. Identify and protect the dorsal digital nerves and veins. These are superficial and easily injured. Retract them gently with vessel loops."
- Pearl: Always assume neurovascular structures are just beneath the skin. Blunt dissection and careful retraction are key.
- Extensor Mechanism Exposure: "Once we've cleared the subcutaneous tissue, we'll see the extensor mechanism. Identify the extrinsic extensor tendon proximally. Now, observe the characteristic 'buttonhole' defect: the central slip is attenuated and disrupted, and the lateral bands are displaced volarly, creating that characteristic PIP flexion."
- Warning: > Surgical Warning: Do not mistake the volar plate for the central slip. The central slip is dorsal and inserts into the middle phalanx.
B. Assessment and Preparation
- Joint Assessment: "Let's gently flex and extend the PIP joint. We need to assess the flexibility of the deformity. If there's a fixed flexion contracture, we may need to perform a volar plate release and potentially collateral ligament release later. For now, it feels reasonably flexible, which is good."
- Central Slip Identification: "Identify the remnants of the central slip inserting into the dorsal base of the middle phalanx. In chronic cases like this, it's often frayed and attenuated. Note the triangular ligament, which should stabilize the lateral bands, is also attenuated."
- Lateral Band Assessment: "Observe the lateral bands. See how they've migrated volarly, acting as PIP flexors? Our primary goal is to bring them back dorsally."
C. Central Slip Reconstruction
- Direct Repair (if acute): "If this were an acute injury, we'd perform a direct end-to-end repair of the central slip using non-absorbable sutures. But in this chronic case, direct repair isn't feasible due to tissue loss."
- Reconstruction with Local Tissue (Extensor Hood Flap): "We'll reconstruct the central slip using a local flap from the extensor hood. I'm incising a rectangular flap, based proximally, from the main extensor tendon body, just proximal to the PIP joint. This flap will be approximately 5-7mm wide and long enough to reach the middle phalanx insertion."
- Instrument: "Use a #15 blade for precise incisions."
- Technique: "We'll pass this flap distally and weave it through the remaining central slip tissue or directly anchor it into the dorsal base of the middle phalanx. I'm using a suture anchor here to ensure a robust bony insertion, drilling a small pilot hole with a 1.0mm K-wire, then inserting the anchor."
- Sutures: "Secure the flap with 4-0 non-absorbable sutures (e.g., Ethibond or Fiberwire) in a modified Kessler or Bunnell fashion, ensuring appropriate tension. We want to restore full PIP extension without hyperextension."
- FDS Slip Reconstruction (Alternative): "In some severe cases, where local tissue is insufficient, we might consider using a slip of the FDS tendon. This would involve a separate volar incision to harvest a slip, passing it dorsally, and then anchoring it. However, for this patient, the extensor hood flap is sufficient."
D. Lateral Band Relocation and Stabilization
- Dorsal Relocation: "Now that our central slip is reconstructed, we need to address the lateral bands. Gently elevate them and reposition them dorsally, proximal to the PIP joint axis of rotation. They should now lie dorsal to the joint."
- Triangular Ligament Reefing/Reconstruction: "The attenuated triangular ligament is crucial for maintaining the dorsal position of these lateral bands. I'm going to reef the existing remnants of the triangular ligament by suturing its edges together over the lateral bands using fine 5-0 non-absorbable sutures. This creates a hammock-like sling, preventing future volar subluxation."
- Pearl: Ensure the lateral bands are not overly tightened, as this could restrict PIP flexion. We want stability, not rigidity.
- Warning: > Surgical Warning: Over-tightening the extensor mechanism can lead to a iatrogenic swan-neck deformity. Always assess range of motion.
E. Intraoperative Assessment and Closure
- Range of Motion Check: "Nurse, please release the tourniquet temporarily. Let's check the range of motion. We should now have full, unrestricted PIP extension, with the lateral bands remaining stable dorsally. Flex the PIP joint fully. Good, no restriction. Extend the DIP joint. Excellent, the balance is restored."
- Hemostasis: "Achieve meticulous hemostasis. Any hematoma can lead to adhesions and compromise our repair."
- Wound Closure: "We'll close the wound in layers. First, the subcutaneous tissue with 4-0 absorbable sutures, then the skin with 5-0 non-absorbable nylon sutures in an interrupted fashion. A sterile dressing will be applied, followed by a splint."
Procedure 2: Swan-Neck Deformity Reconstruction
For this patient, we are addressing a flexible Type I Swan-Neck deformity of the index finger, likely due to volar plate laxity and intrinsic tightness. Our primary goal is to prevent PIP hyperextension and restore the balance.
A. Surgical Approach and Exposure
- Incision: "For this flexible swan-neck, our primary focus is the volar plate and potentially an FDS tenodesis. I'll make a volar zigzag incision over the PIP joint, specifically a Bruner-type incision. This provides excellent exposure of the flexor sheath and volar plate while avoiding contracture."
- Rationale: The zigzag incision allows for lengthening without contracture and provides good access to the volar structures.
- Subcutaneous Dissection: "Carefully incise the skin. Now, with tenotomy scissors, dissect through the subcutaneous fat. Identify and protect the proper digital nerves and arteries, which run along the sides of the flexor sheath. Use fine vessel loops for gentle retraction."
- Pearl: The neurovascular bundles are more vulnerable in the web spaces and along the mid-axial line.
- Flexor Sheath Exposure: "Expose the flexor sheath. We'll identify the A2 and A3 pulleys. The A2 pulley is crucial here, as we'll be working around it."
B. Assessment and Preparation
- Joint Assessment: "Gently manipulate the PIP joint. Confirm the hyperextension. We also need to assess the DIP joint flexion. This patient has a flexible deformity, meaning the PIP can be passively flexed, which is a good prognostic sign."
- Volar Plate Assessment: "Examine the volar plate. In this case, it's attenuated and lax, allowing the PIP joint to hyperextend. We need to tighten this."
- FDS Tendon Identification: "Identify the FDS tendon. We'll need one slip for our tenodesis."
C. Volar Plate Plication and FDS Tenodesis
- Volar Plate Plication: "First, let's address the volar plate. I'm going to perform a volar plate plication. We'll make a transverse incision in the central portion of the volar plate, just distal to its origin on the proximal phalanx. Then, we'll overlap the edges and secure them with 4-0 non-absorbable sutures (e.g., Fiberwire) in a mattress fashion. This effectively shortens and tightens the volar plate, acting as a check-rein against hyperextension."
- Instrument: "Use fine dissecting scissors and a small curved hemostat to carefully elevate the volar plate before making the incision."
- Warning: > Surgical Warning: Be extremely cautious not to damage the underlying FDP tendon or the collateral ligaments during volar plate plication.
- FDS Tenodesis (Lateral Slip Transfer): "Now, for the FDS tenodesis. We'll isolate one slip of the FDS tendon, typically the ulnar slip, by dividing it proximally at the level of the A1 pulley and distally at its insertion into the middle phalanx. Ensure you leave the other FDS slip and the FDP intact for continued flexion."
- Instrument: "Use a tendon passer to gently retrieve the isolated FDS slip."
- Technique: "We'll pass this FDS slip dorsally, either through a small window created in the A2 pulley or adjacent fibrous tissue, or around the collateral ligament. The goal is to create a new volar restraint that acts as a dynamic check-rein. I'm going to pass it through a drill hole in the proximal phalanx, just proximal to the PIP joint, from dorsal to volar, and then loop it back on itself."
- Drilling: "Use a 1.5mm drill bit, under constant fluoroscopic guidance, to create a transverse tunnel through the proximal phalanx. Ensure the drill bit exits volarly in a safe zone, away from the flexor tendons."
- Fixation: "Once the FDS slip is passed through the tunnel, we'll tension it to prevent PIP hyperextension while allowing full flexion. Secure it to itself or to the adjacent periosteum with 4-0 non-absorbable sutures. We want the PIP joint to flex to at least 90 degrees but not hyperextend beyond neutral."
- Pearl: Tensioning is critical. Too tight, and you restrict flexion. Too loose, and the deformity recurs. Test it rigorously.
D. Addressing Intrinsic Tightness (if present)
- Intrinsic Release: "If preoperative assessment indicated significant intrinsic tightness contributing to the MCP flexion deformity, we would perform a release of the intrinsic muscles. This involves incising the intrinsic tendons on the radial and ulnar sides of the proximal phalanx, just distal to the MCP joint. This allows the MCP joint to extend more fully."
- Warning: > Surgical Warning: Be careful not to inadvertently injure the collateral ligaments or the neurovascular bundles during intrinsic release.
E. Intraoperative Assessment and Closure
- Range of Motion Check: "Nurse, release the tourniquet. Let's check the range of motion. The PIP joint should now be stable, preventing hyperextension, and should still be able to flex to at least 90 degrees. The DIP joint flexion should also be improved as the extensor forces are now balanced."
- Hemostasis: "Achieve meticulous hemostasis."
- Wound Closure: "Close the skin with 5-0 non-absorbable nylon sutures in an interrupted fashion. Apply a sterile dressing and a dorsal blocking splint to protect our repair."
Extensive Pearls and Pitfalls: Navigating the Minefield
Fellows, surgery is rarely straightforward. Anticipating and managing complications is a hallmark of a master surgeon.
Pearls
- Bloodless Field: Absolutely essential
Additional Intraoperative Imaging & Surgical Steps
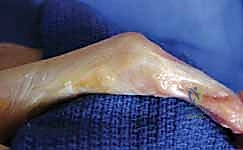
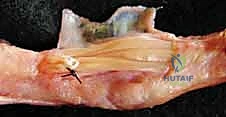
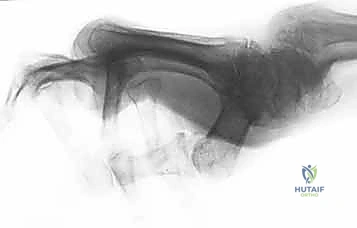
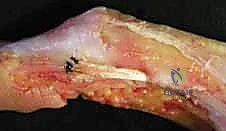
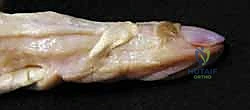
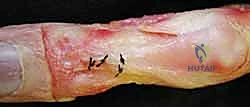
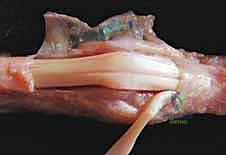
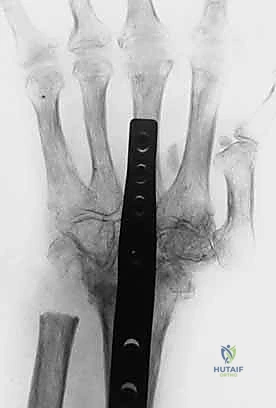
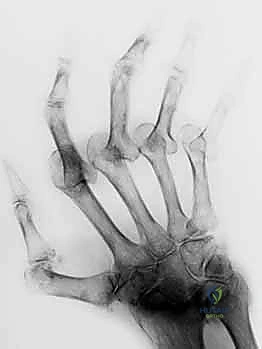
REFERENCES
-
Aiche A, Barsky AJ, Weiner DL. Prevention of boutonniere deformity. Plast Reconst Surg 1970;46:164–167.
-
Arnett FC, Edworthy SM, Bloch DA, et al. The American Rheumatism Association 1987 revised criteria for classification of rheumatoid arthritis. Arthritis Rheum 1988;31:315–324.
- Boyer MI, Gelberman RH. Operative correction of swan-neck and boutonniere deformities in the rheumatoid hand. J Am Acad Orthop Surg 1999;7:92–100.
-
Burton RI, Melchior JA. Extensor tendons: late reconstruction. In: Green DP, Hotchkiss RN, Pederson WC, eds. Green’s Operative Hand Surgery, 4th ed. New York: Churchill Livingstone, 1999: 215–221.
-
Carducci T. Potential boutonniere deformity: its recognition and treatment. Orthopaedic Review 1981;10:121–123.
-
Cook SD, Beckenbaugh RD, Redondo J, et al. Long-term follow-up of pyrolytic carbon metacarpophalangeal implants. J Bone Joint Surg Am 1999;81A:635–648.
-
Coons MS, Green SM. Boutonniere deformity. Hand Clin 1995;11: 387–402.
-
Curtis R. Sublimis tenodesis. In: Edmonson AS, Crenshaw AH, eds. Campbell’s Operative Orthopaedics, 6th ed. St. Louis: CV Mosby, 1980:319.
-
Eberhardt K, Johnson PM, Rydgren L. The occurrence and significance of hand deformities in early rheumatoid arthritis. Br J Rheumatol 1991;30:211–213.
-
Ferlic DC. Boutonniere deformities in rheumatoid arthritis. Hand Clin 1989;5:215–222.
-
Figgie MP, Inglis AE, Sobel M, et al. Metacarpal phalangeal joint arthroplasty of the rheumatoid thumb. J Hand Surg Am 1990;15A: 210–216.
-
Flatt AE. The Care of the Arthritic Hand. St. Louis: Quality Medical Publishing, 1995:263–264.
-
Gainor BJ, Hummel GL. Correction of rheumatoid swan-neck deformity by lateral band mobilization. J Hand Surg Am 1985;10A: 370–377.
-
Harris ED Jr. Rheumatoid arthritis: pathophysiology and implications for therapy. N Engl J Med 1990;18:1277–1289.
-
Kiefhaber TR, Strickland JW. Soft tissue reconstruction for rheumatoid swan-neck and boutonniere deformities: long-term results. J Hand Surg Am 1993;18A:984–989.
-
Kleinman WB, Peterson DP. Oblique retinacular ligament reconstruction for chronic mallet finger deformity. J Hand Surg Am 1984;9A: 399–404.
-
Littler JW, Eatron RG. Redistribution of forces in correction of boutonniere deformity. J Bone Joint Surg Am 1967;49A:1267–1274.
-
Lovett WL, McCalla MA. Management and rehabilitation of extensor tendon injuries. Orthop Clin North Am 1983;14:811–826.
-
Mannerfelt LG, Norman O. Attrition ruptures of flexor tendons in rheumatoid arthritis caused by bony spurs in the carpal tunnel: a clinical and radiological study. J Bone Joint Surg Br 1969;51B: 270–277.
-
Mannerfelt LG, Oetker R, Ostlunel B, et al. Rupture of the extensor pollicis longus tendon after Colles’ fracture and by rheumatoid arthritis. J Hand Surg Br 1990;15B:49–50.
-
Massengill JB. The boutonniere deformity. Hand Clin 1992;8: 787–801.
-
Matev I. Transposition of the lateral slips of the aponeurosis in treatment of long-standing “boutonniere deformity” of the fingers. Br J Plast Surg 1964;17:281–286.
- Meadows SE, Schneider LH, Sherwyn JH. Treatment of the chronic boutonniere deformity by extensor tenotomy. Hand Clin 1995;11: 441–447.
-
Nalebuff EA. The rheumatoid swan-neck deformity. Hand Clin 1989;5:203–214.
-
Nalebuff EA. The rheumatoid thumb. Clin Rheum Dis 1984;10: 589–607.
-
Nalebuff EA. Diagnosis, classification and management of rheumatoid thumb deformities. Bull Hosp Joint Dis 1968;29:119–137.
-
Nalebuff EA, Millender LH. Surgical treatment of the boutonniere deformity in rheumatoid arthritis. Orthop Clin North Am 1975;6:753–763.
-
O’Brien ET. Surgical principles and planning for the rheumatoid hand and wrist. Clin Plast Surg 1996;23:407–420.
-
Ratliff AHC. Deformities of the thumb in rheumatoid arthritis. Hand 1971;3:138–143.
-
Rizio L, Belsky MR. Finger deformities in rheumatoid arthritis. In: Ruby LK, Cassidy C, eds. Rheumatoid Arthritis of the Hand and Wrist. Hand Clin 1996;12:531–540.
-
Rubin J, Bozentha DJ, Bora FW. Diagnosis of closed central-slip injuries. J Hand Surg Br 1996;21B:614–616.
-
Snow JW. Use of a retrograde tendon flap in repairing a severed extensor at the PIP joint area. Plast Reconstr Surg 1973;51:555–558.
-
Stein AB, Terrono AL. The rheumatoid thumb. In: Ruby LK, Cassidy C, eds. Rheumatoid Arthritis of the Hand and Wrist. Hand Clin 1996;12:541–550.
-
Strickland JW, Boyer M. Swan neck deformity. In: Strickland JW, ed. The Hand. Master Techniques in Orthopaedic Surgery series. Philadelphia: Lippincott-Raven, 1998:459–470.
-
Swanson AB, Maupin BK, Gajjar NV, et al. Flexible implant arthroplasty in the proximal interphalangeal joint in the hand. J Hand Surg Am 1985;10A:796–805.
-
Takigawa S, Meletiou S, Sauerbier M, et al. Long-term assessment of Swanson implant arthroplasty in the proximal interphalangeal joint of the hand. J Hand Surg Am 2004;29A:785–795.
-
Terrono A, Millender L. Surgical treatment of the boutonniere rheumatoid thumb deformity. Hand Clin 1989;5:239–248.
-
Terrono A, Millender L, Nalebuff E. Boutonniere rheumatoid thumb deformity. J Hand Surg Am 1990;15A:999–1003.
-
Thompson JS, Littler JW, Upton J. The spiral oblique retinacular ligament (SORL). J Hand Surg Am 1978;3A:482–487.
-
Toledano B, Terrono A, Millender L. Reconstruction of the rheumatoid thumb. Hand Clin 1992;8:121–129.
-
Tonkin MA, Gianoutsos MP, Ryan D, et al. Synovectomy, joint release and lateral band translocation for stiff swan neck deformity. Hand Surg 1996;1:69–74.
-
Tonkin MA, Hughes J, Smith KL. Lateral band translocation for swan-neck deformity. J Hand Surg Am 1992;17A:260–267.
-
Towfigh H, Gruber P. Surgical treatment of the boutonniere deformity. Oper Orthop Traumatol 2005;17:66–78.
-
Urbaniak JR, Hayes MG. Chronic boutonniere deformity: an anatomic reconstruction. J Hand Surg Am 1981;6A:379–383.
-
Zancolli E. Structural and Dynamic Bases of Hand Surgery, 2nd ed. Philadelphia: JB Lippincott, 1979.