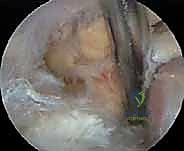
Arthroscopic Synovectomy: An Intraoperative Masterclass in Knee Joint Preservation
Key Takeaway
Master arthroscopic synovectomy with this expert guide. Learn patient selection, detailed knee anatomy, precise portal placement, and meticulous synovial resection. Understand neurovascular risks, optimize visualization, and manage post-operative care. Essential for fellows tackling chronic knee synovitis, including conditions like rheumatoid arthritis and PVNS, ensuring comprehensive joint preservation.
Welcome, fellows, to the operating theater. Today, we're performing an arthroscopic synovectomy – a critical procedure for patients suffering from chronic, debilitating synovitis of the knee. This isn't just about removing inflamed tissue; it's about preserving joint function, alleviating pain, and potentially slowing the progression of arthrosis in a complex patient population. Let's delve into the intricacies, from patient selection to the final stitch.
Understanding the Pathological Knee: Patient Selection and Diagnostic Acumen
Before we even consider surgery, a thorough understanding of the patient's condition is paramount. Synovitis, by definition, is inflammation of the synovial membrane, a specialized mesenchymal lining that normally provides nutrients to articular cartilage and produces lubricating fluid for smooth joint gliding. In pathological states, this lining undergoes hyperplasia, often with a mononuclear infiltration, leading to redundant synovial folds and villi.
Patient History and Physical Examination
Our patient today presents with a long history of chronic knee pain, recurrent swelling, warmth, stiffness, and mechanical symptoms. This is a classic presentation. We've exhausted medical management – oral anti-inflammatories, intra-articular corticosteroid injections, and gentle physical therapy – and the patient continues to experience significant functional impairment. This is our clear indication for surgical intervention.
During your consultation, always elicit a full personal and family history of rheumatologic and hematologic disorders. Ask about involvement of other joints, previous episodes of knee swelling, and systemic symptoms. Conditions like rheumatoid arthritis (RA), pigmented villonodular synovitis (PVNS), synovial osteochondromatosis, psoriatic arthritis, lupus arthrosis, gout, synovial hemangiomas, hemophilic synovitis, and post-traumatic synovitis are all on our differential.
Surgical Warning: Rheumatoid Arthritis Systemic Implications
In patients with rheumatoid arthritis, remember that the disease is often not limited to the musculoskeletal system. Always evaluate the cervical spine for instability with preoperative flexion and extension radiographs, as intubation can pose a significant risk. Also, inquire about vasculitis, subcutaneous nodules, and pericarditis.
On physical examination, we meticulously assess for effusion, tenderness, warmth, palpable mass, and synovial thickening. We document the range of motion (ROM), noting any loss of flexion or extension, which might indicate arthrofibrosis. Crucially, we perform a comprehensive ligamentous examination:
* Lachman test for anterior cruciate ligament (ACL) competence.
* Posterior drawer test for posterior cruciate ligament (PCL) competence.
* Varus stress test for lateral collateral ligament (LCL) competence.
* Valgus stress test for medial collateral ligament (MCL) competence.
Significant malalignment or ligamentous insufficiencies often portend a poorer prognosis for isolated arthroscopic synovectomy and may necessitate a different treatment strategy, given their association with advanced joint destruction.
Diagnostic Studies and Imaging
Joint aspiration is both therapeutic and diagnostic. Synovial fluid analysis should include documentation of fluid color (e.g., brownish in PVNS due to recurrent bleeding), cell count, Gram stain, culture, crystal analysis, and specific markers like rheumatoid factor and complement levels when indicated.
Radiographs are essential to document the extent of joint destruction. We look for characteristic rheumatologic signs such as periarticular erosions and osteopenia in RA, or cystic, sclerotic, or erosive lesions in PVNS and gout. Synovial chondromatosis might present with visible calcified bodies. Remember, advanced degenerative disease is associated with a poorer prognosis after arthroscopy.
Magnetic Resonance Imaging (MRI) is invaluable for assessing the scope of joint involvement before surgery. It helps us differentiate localized from diffuse disease and visualize the extent of synovial hypertrophy. For instance, nodular PVNS can be readily seen as low signal on both T1 and T2 images.
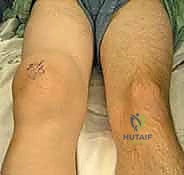
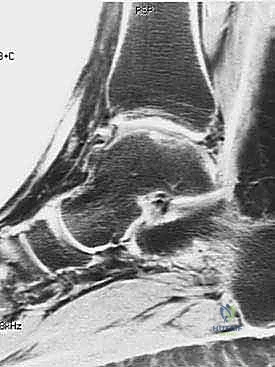
Here, fellows, you see a T2-weighted MRI revealing a large effusion, typical in a patient subsequently diagnosed with rheumatoid arthritis.
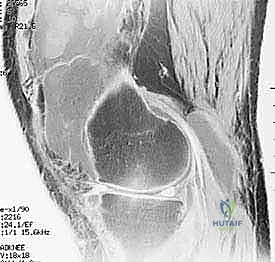
Another view of the T2-weighted MRI, highlighting the extensive synovial involvement.
Preoperative Planning: Setting the Stage for Success
Meticulous preoperative planning is the bedrock of a successful arthroscopic synovectomy.
Anesthesia and Medical Clearance
Given the potential length and complexity of a complete synovectomy, general anesthesia is recommended. An epidural can be a valuable adjunct, providing excellent postoperative pain relief. We ensure appropriate medical clearance for all patients, especially those with systemic conditions, to minimize perioperative complications. For anticipated prolonged cases, a Foley catheter is routinely placed.
Patient Positioning and OR Setup
Let's move to the OR table. The patient is carefully positioned supine on the operating table.
- Table Configuration: We bring the patient to the very edge of the bed, allowing the operative leg to hang freely over the side. The foot of the bed is dropped, and the bed itself is flexed to produce slight hip flexion. This seemingly minor detail is crucial: it decreases the chance of femoral nerve palsy that can be associated with excessive hip extension and leg traction.
- Tourniquet Placement: A well-padded thigh tourniquet is placed high on the operative leg. We will inflate this to 250 to 300 mmHg after exsanguination. Proper padding prevents skin breakdown and nerve compression.
- Contralateral Leg: The contralateral leg is placed securely in a well-padded leg holder, with the hip and knee flexed and the hip in slight abduction. Compressive wrapping or sequential compression stockings are applied to the contralateral leg to aid in venous return and reduce the risk of deep vein thrombosis (DVT), especially given the prolonged nature of these procedures.
- Lateral Post: An arthroscopic lateral post is positioned midthigh on the side of the operative bed. This post acts as a fulcrum, allowing us to apply valgus stress to the knee, which helps open the medial compartment and improve visualization.
> Surgical Warning: Avoiding Leg Holders
> We specifically do not use an arthroscopic leg holder that fixes the operative knee in flexion. This type of holder can prohibit the necessary manipulation and access to the superomedial and superolateral portals, which are critical for a comprehensive synovectomy.
Essential Equipment
Let's ensure we have our full armamentarium ready:
* Arthroscopes: Primarily a 4.5-mm 30-degree arthroscope. Keep a 4.5-mm 70-degree arthroscope available; it can be invaluable for visualizing difficult-to-reach areas, especially in the posterior compartments or behind hypertrophic synovium.
* Shavers: A small suction shaver (e.g., 3.5mm or 4.0mm) is our workhorse for debulking the synovial tissue. Have multiple blades available, including aggressive and soft tissue resectors.
* Electrocautery: An arthroscopic electrocautery device is essential for achieving hemostasis, especially after tourniquet release.
* Arthroscopic Basket Forceps: Useful for excising larger villous structures or loose bodies that the shaver might struggle with.
* Biopsy Trap: A suction canister trap must be set up for collecting synovial tissue biopsies for pathology and microbiology. This is non-negotiable.
Intraoperative Execution: The Arthroscopic Synovectomy Masterclass
Now, let's scrub in.
Portal Placement: Mapping Our Access
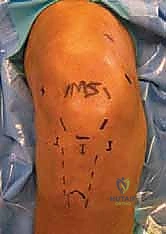
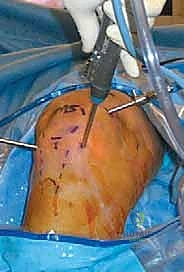
We begin by marking our portals on the skin. A complete synovectomy typically requires five or six portals to ensure thorough access to all compartments.
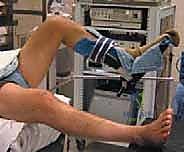
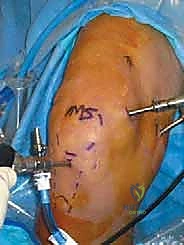
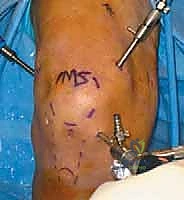
Observe the typical portal markings on this right knee. Accuracy here is crucial for optimal visualization and instrument maneuverability.
Diagnostic Arthroscopy: The Initial Assessment
The first step is a thorough diagnostic arthroscopy.
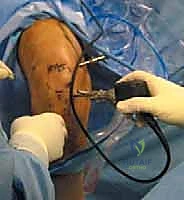
- Exsanguination and Tourniquet Inflation: Nurse, please hand me the Esmarch bandage. We meticulously exsanguinate the operative limb from distal to proximal.
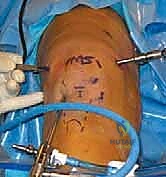
This image shows the limb being exsanguinated with an Esmarch bandage.
Once exsanguinated, we inflate the thigh tourniquet to 250 to 300 mmHg. Note the time.
2. Initial Portal and Fluid Management: We make a small, precise incision in the inferolateral portal – typically just lateral to the patellar tendon, at the level of the inferior pole of the patella. We insert our arthroscopic cannula and blunt trocar.
Next, we establish our outflow in the superomedial portal. This portal is rarely used as a primary viewing or working portal for anterior synovectomy, making it ideal for continuous fluid outflow, which helps maintain clear visualization.
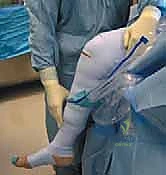
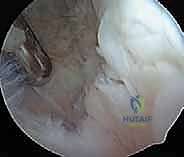
Here, you can see the arthroscopic view revealing the outflow in the superomedial portal, ensuring constant fluid exchange.
3. Systematic Joint Survey: With the arthroscope now in the inferolateral portal, we gently advance it into the suprapatellar pouch with the knee in extension. We perform a systematic diagnostic survey, assessing the articular cartilage, menisci, ligaments, and patellofemoral joint. We're looking for the extent of synovial hypertrophy, any loose bodies, and the overall health of the joint.
4. Establishing the Superolateral Working Portal: Under direct arthroscopic visualization from the inferolateral portal, we establish a superolateral working portal. This is typically placed just superior to the patella, lateral to the quadriceps tendon. We use a spinal needle first to confirm optimal placement, then incise the skin and insert our working cannula.
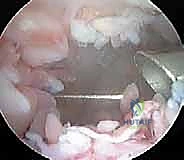
The establishment of the superolateral portal is critical for anterior compartment access.
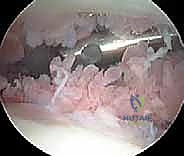
Arthroscopic view confirming the optimal placement of the superolateral working portal under direct visualization.
This image illustrates the superolateral portal being established, ready for instrument insertion.
Synovectomy: Anterior Compartments
Our goal is a near-complete synovectomy, removing all hypertrophied and inflamed synovial tissue while meticulously preserving crucial structures. We will systematically address each compartment.
Suprapatellar Pouch and Lateral Gutter
- Arthroscope in Inferolateral, Shaver in Superolateral: We maintain the arthroscope in the inferolateral portal. Now, we introduce our small suction shaver into the superolateral working portal.
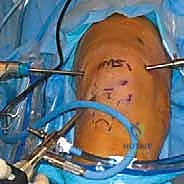
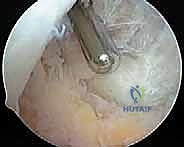
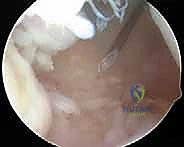
The shaver is placed into the superolateral working portal, ready for action.
With the shaver, we begin our meticulous resection of the suprapatellar pouch synovium. Use a sweeping motion, drawing the hypertrophied tissue into the shaver while maintaining constant visualization.
Next, we direct the shaver laterally to address the lateral gutter. Ensure you reach all recesses, carefully resecting the inflamed tissue along the lateral femoral condyle and capsule.
Observe the partial resection of the lateral gutter synovium under arthroscopic view.
Medial Gutter and Medial Suprapatellar Pouch
- Shaver in Inferomedial Portal: Now, we shift our shaver to the inferomedial portal. This portal is typically placed just medial to the patellar tendon, at the level of the inferior patellar pole.

The shaver is now moved to the inferomedial portal, giving us access to the medial compartment.
From this position, we meticulously excise the synovium from the medial gutter and the medial aspect of the suprapatellar pouch. Use gentle, controlled movements, ensuring not to damage the medial meniscus or articular cartilage.
This arthroscopic view demonstrates the precise resection of medial synovium.
Retropatellar Space, Inferolateral and Inferomedial Gutters
- Arthroscope in Superolateral, Shaver in Inferolateral: To optimize our view of the retropatellar space and the inferior gutters, we now move the arthroscope to the superolateral portal.
We then place the shaver into the inferolateral portal. This configuration enables efficient synovial resection from the inferolateral gutter and the often-overlooked retropatellar space. Maneuver the patella to expose all facets and recesses.
With the scope superolateral and shaver inferolateral, we can now address the retropatellar and inferolateral regions effectively.
2. Shaver in Inferomedial Portal (Completion): To complete the synovectomy of the retropatellar space and the inferomedial gutter, we reposition the shaver into the inferomedial portal while the arthroscope remains in the superolateral portal.
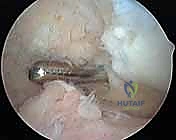
This image shows the shaver completing the resection of the retropatellar space and inferomedial gutter.
Intercondylar Notch
- Arthroscope in Inferolateral, Shaver in Inferomedial: We return the arthroscope to the inferolateral portal, and keep the shaver in the inferomedial portal.
The arthroscope is back in the inferolateral portal, with the shaver in the inferomedial portal, setting up for the notch.
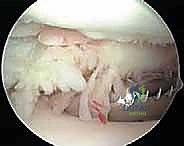
From this vantage point, we carefully perform resection of synovium in the intercondylar notch and around the cruciate ligaments. This creates adequate working space and allows for visualization of the posterior compartments.
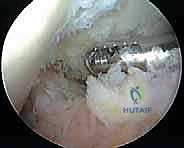
Arthroscopic photograph showing the resection of synovium in the notch.
> Surgical Warning: Cruciate Ligament Preservation
> This area demands extreme precision. Care must be taken to distinguish hypertrophied synovium from the cruciate ligaments themselves. Inadvertent damage to the ACL or PCL can have devastating consequences. Use a gentle, feathering technique with the shaver, or a basket forceps for larger villi near the ligaments.
<a href="/media/hutaif_opertive/hutaif-ch32-arthroscopic-sy-p313-c1
Additional Intraoperative Imaging & Surgical Steps


REFERENCES
-
One study of 96 rheumatoid arthritic knees found significant decreases in pain and synovitis at an average of 4 years after arthroscopic synovectomy. 11
-
Comin JA, Rodriguez-Merchan EC. Arthroscopic synovectomy in the management of painful localized post-traumatic synovitis of the knee joint. Arthroscopy 1997;13:606–608.
-
Fiacco U, Cozzi L, Rigon C, et al. Arthroscopic synovectomy in rheumatoid and psoriatic knee joint synovitis: long-term outcome. Br J Rheumatol 1996;35:463–470.
-
Gilbert MS, Radomisli TE. Therapeutic options in the management of hemophilic synovitis. Clin Orthop Relat Res 1997;343:88–92.
-
Johansson JE, Ajjoub S, Coughlin LP, et al. Pigmented villonodular synovitis of joints. Clin Orthop Relat Res 1982;163:159–166.
-
Klein W, Jensen KU. Arthroscopic synovectomy of the knee joint: indication, technique and follow-up results. Arthroscopy 1988;4: 63–71.
-
Lee BI, Yoo JE, Lee SH, et al. Localized pigmented villonodular synovitis of the knee: arthroscopic treatment. Arthroscopy 1998;14: 764–768.
-
Matsui N, Taneda Y, Ohta H, et al. Arthroscopic versus open synovectomy in the rheumatoid knee. Int Orthop 1989;13:17–20.
-
Moskovich R, Parisien JS. Localized pigmented villonodular synovitis of the knee. Clin Orthop Relat Res 1991;271:218–224.
-
Oglivie-Harris DJ, McLean J, Zarnett ME. Pigmented villonodular synovitis of the knee. J Bone Joint Surg Am 1992;74A:119–123.
-
Ogilvie-Harris DJ, Weisleder L. Arthroscopic synovectomy of the knee: is it helpful? Arthroscopy 1995;11:91–95.
-
Ogilvie-Harris DJ, Basinski A. Arthroscopic synovectomy of the knee for rheumatoid arthritis. Arthroscopy 1991;7:91.
-
Roch-Bras F, Daures JP, Legouffe MC, et al. Treatment of chronic knee synovitis with arthroscopic synovectomy: long-term results. Rheumatology 2002;29:1171–1175.
-
Shibata T, Shiraoka K, Takubo N. Comparison between arthroscopic and open synovectomy for the knee in rheumatoid arthritis. Arch Orthop Trauma Surg 1986;105:257–262.
-
Wiedel JD. Arthroscopic synovectomy of the knee in hemophilia: 10 to 15 year follow-up. Clin Orthop Relat Res 1996;328:46–53.
-
Zvijac JE, Lau AC, Hechtman KS, et al. Arthroscopic treatment of pigmented villonodular synovitis of the knee. Arthroscopy 1999;15: 613–617.
-
Along with the use of rheumatoid medications, arthroscopic synovectomy can reduce inflammation and help preserve range of motion. 2
-
Success rates in the relief of pain and swelling have been as high as 80% in the treatment of rheumatoid arthritis. 10
-
Arthroscopic synovectomy has been used successfully in the treatment of PVNS.
-
In the past, open synovectomies led to stiffness and pain after the procedure. In a series of 18 patients with diffuse PVNS, one third of the patients had a recurrence after open synovectomy, and in most patients the knee was manipulated in an attempt to decrease stiffness. 4
-
Recurrence rates with arthroscopic synovectomy of PVNS have been as low as 11%, with improved range of motion. 9
-
Localized PVNS has responded best to arthroscopic treatment.
-
Multiple series have reported no recurrences at follow-up after excision of the lesion. 8,9,15
-
The procedure allows improved visualization of lesions and facilitates the discovery of small, localized forms of PVNS.
-
Hemophilic synovitis, also associated with aggressive joint destruction, has responded well symptomatically to arthroscopic synovectomy.
-
Unlike most forms of synovitis, this usually requires a short period of hospitalization because of the underlying systemic disorder.
-
The procedure has been effective in reducing recurrent hemarthrosis and maintaining range of motion.

You Might Also Like