Advanced Orthopedic Pathology: Skeletal Dysplasia, Tabes Dorsalis, Septic Arthritis | Part 3

Key Takeaway
Skeletal dysplasia spinal and joint pathology encompasses a range of complex conditions reviewed for orthopedic board exams. Key areas include managing spinal deformities (kyphosis, scoliosis, atlantoaxial instability) in achondroplasia and other dysplasias, understanding neuropathic arthropathy (Charcot joint) in Tabes Dorsalis, and diagnosing/treating acute and chronic bacterial arthritis. These cases highlight critical orthopedic and neurological considerations.
Question 1
A 35-year-old male with known achondroplasia presents with progressive bilateral lower extremity weakness, numbness, and claudication-like symptoms. Physical exam reveals hyperreflexia and a positive Babinski sign. Radiographs show short pedicles and reduced interpedicular distance in the lumbar spine.
View Answer & Explanation
Correct Answer: C
Rationale: Progressive neurological deficits, such as weakness and hyperreflexia, in the setting of symptomatic lumbar spinal stenosis in achondroplasia are a clear indication for surgical decompression via lumbar laminectomy. Conservative measures are typically ineffective due to the fixed anatomical narrowing. Spinal fusion is generally not indicated unless there is associated instability or severe deformity requiring correction.
Question 2
A 1-year-old infant with achondroplasia is noted to have a flexible thoracolumbar kyphosis measuring 55 degrees. The child is not yet walking independently. Physical examination confirms the flexibility of the curve.
View Answer & Explanation
Correct Answer: E
Rationale: In non-ambulatory infants with achondroplasia, a flexible thoracolumbar kyphosis is common. The most appropriate initial management is close observation and avoidance of unsupported sitting, which can exacerbate the deformity. Encouraging prone positioning can also be beneficial. Bracing is generally not effective for flexible curves in this age group and can hinder motor development. Surgical fusion is reserved for rigid, progressive curves, or those with neurological compromise.
Question 3
A 5-year-old boy with a known diagnosis of Spondyloepiphyseal Dysplasia Congenita (SEDC) presents for a pre-operative evaluation for bilateral hip osteotomies. Lateral cervical radiographs reveal significant odontoid hypoplasia and an atlanto-dens interval (ADI) of 7 mm in flexion. He is asymptomatic neurologically.
View Answer & Explanation
Correct Answer: C
Rationale: Odontoid hypoplasia and atlantoaxial instability are common and severe in SEDC, posing a significant risk of spinal cord injury during intubation or positioning for general anesthesia. Even if asymptomatic, an ADI of 7mm indicates significant instability. Cervical spine stabilization (e.g., halo vest or surgical fusion) is often required before other major surgeries to prevent catastrophic neurological injury. While respiratory complications and intubation difficulties can occur in some dysplasias, atlantoaxial instability is the most critical spinal concern in SEDC.
Question 4
A 6-month-old infant with diastrophic dysplasia is brought to the clinic due to a progressively worsening cervical kyphosis. Physical examination reveals a stiff neck and limited range of motion. Radiographs confirm a severe cervical kyphosis with anterior wedging of vertebral bodies at C3-C4.
View Answer & Explanation
Correct Answer: C
Rationale: Progressive cervical kyphosis in diastrophic dysplasia can lead to myelopathy. In infants, halo-vest immobilization is often attempted first to correct the deformity and allow for potential spontaneous fusion. If the kyphosis is rigid, progressive, or associated with neurological symptoms, surgical fusion (typically posterior) may be necessary. Close observation or a soft collar would be insufficient for a progressively worsening severe kyphosis.
Question 5
A 10-year-old boy with Morquio syndrome (MPS IV) presents with gait disturbance and upper extremity paresthesias. Neurological exam reveals hyperreflexia and clonus. Lateral cervical radiographs show severe odontoid hypoplasia and an atlanto-dens interval (ADI) of 9 mm in flexion.
View Answer & Explanation
Correct Answer: C
Rationale: Symptomatic atlantoaxial instability with myelopathy (gait disturbance, paresthesias, hyperreflexia, clonus) in Morquio syndrome requires surgical stabilization. Given the odontoid hypoplasia and significant ADI, a posterior atlantoaxial fusion is the definitive treatment to prevent irreversible spinal cord damage. Conservative measures are inadequate for symptomatic instability.
Question 6
A 7-year-old girl with pseudoachondroplasia presents with progressive thoracolumbar scoliosis measuring 45 degrees and a compensatory lumbar lordosis. She has generalized ligamentous laxity. Radiographs show platyspondyly and irregular endplates. Her parents note that her facial features are normal.
View Answer & Explanation
Correct Answer: B
Rationale: Pseudoachondroplasia is characterized by normal facial features and head size, which is a key distinguishing feature from achondroplasia (which has characteristic midface hypoplasia and frontal bossing). While both have spinal involvement, the type and severity differ. Pseudoachondroplasia often presents with more severe kyphoscoliosis and ligamentous laxity, but not the same degree of spinal stenosis as achondroplasia.
Question 7
A 3-year-old child presents with disproportionate short stature, a "pear-shaped" trunk, and severe joint contractures. Radiographs show generalized platyspondyly and dumbbell-shaped long bones. He also has a progressive kyphoscoliosis. Further review of his spine radiographs reveals specific vertebral anomalies.
View Answer & Explanation
Correct Answer: C
Rationale: Coronal clefts in vertebral bodies are a classic and highly characteristic radiographic feature of Kniest dysplasia, especially in infancy and early childhood. This finding, along with platyspondyly, dumbbell-shaped long bones, and severe joint contractures, points strongly to Kniest dysplasia.
Question 8
A newborn is diagnosed with metatropic dysplasia based on clinical findings of short limbs, a long trunk, and a prominent coccyx. Radiographs show severe platyspondyly and dumbbell-shaped long bones. The parents are counseled about potential future complications.
View Answer & Explanation
Correct Answer: C
Rationale: Metatropic dysplasia is characterized by severe and progressive kyphoscoliosis, which often leads to significant respiratory compromise and may require early surgical intervention. While other spinal issues can occur, severe kyphoscoliosis is a hallmark and major management challenge.
Question 9
A 6-year-old boy presents with short stature, a waddling gait, and a history of recurrent ear infections. Radiographs show generalized platyspondyly, irregular vertebral endplates, and metaphyseal irregularities in the long bones. He has a mild thoracolumbar kyphosis.
View Answer & Explanation
Correct Answer: C
Rationale: Generalized platyspondyly (flattened vertebral bodies) is a hallmark radiographic feature seen across many types of Spondyloepimetaphyseal Dysplasia (SEMD), contributing to short stature and spinal deformities. The other options are either less common, not characteristic, or specific to other conditions.
Question 10
A 4-year-old boy with achondroplasia is scheduled for a bilateral lower extremity lengthening procedure. Pre-operative assessment reveals no neurological deficits, but a history of obstructive sleep apnea and a relatively large head with midface hypoplasia.
View Answer & Explanation
Correct Answer: B
Rationale: Patients with achondroplasia often have craniofacial features such as midface hypoplasia, relative macroglossia, and a small foramen magnum, which can lead to a difficult airway, obstructive sleep apnea, and potential for cervicomedullary compression. These are critical anesthetic considerations. While atlantoaxial instability can occur in some dysplasias, it is less common in achondroplasia compared to conditions like SEDC or MPS.
Question 11
A 15-year-old male presents with progressive back pain and increasing difficulty with physical activity. He has disproportionate short stature with a short trunk. Radiographs show severe platyspondyly, particularly in the lumbar spine, and a rigid thoracolumbar kyphoscoliosis. He has no history of neurological symptoms. His mother and sister are unaffected, but his maternal uncle had similar features.
View Answer & Explanation
Correct Answer: C
Question 11
A 6-year-old boy presents with progressive short stature and a waddling gait. Physical examination reveals a prominent thoracolumbar kyphosis, limited elbow extension, and genu varum. Radiographs show platyspondyly, particularly in the lumbar spine, with anterior wedging, and a hypoplastic odontoid process. Epiphyseal changes are noted in the hips and knees. Genetic testing confirms a mutation in the *COL2A1* gene.
View Answer & Explanation
Correct Answer: C
Rationale: Spondyloepiphyseal dysplasia congenita (SEDc) is characterized by severe short stature, platyspondyly, a hypoplastic odontoid process leading to atlantoaxial instability, and epiphyseal dysplasia. The *COL2A1* gene mutation is diagnostic. Thoracolumbar kyphosis is a common spinal manifestation. Kniest dysplasia (D) also involves *COL2A1* but typically presents with more severe joint contractures, a "Swiss cheese" appearance of epiphyses, and a distinctive facial appearance, though spinal involvement is similar. Achondroplasia (A) is caused by *FGFR3* mutation and presents with rhizomelic dwarfism, prominent forehead, and lumbar lordosis/thoracolumbar kyphosis but not significant platyspondyly or odontoid hypoplasia to this degree. Diastrophic dysplasia (B) is caused by *SLC26A2* mutation and presents with hitchhiker's thumb, clubfoot, and ear deformities, in addition to spinal deformities. Pseudoachondroplasia (E) is caused by *COMP* mutation, has normal facial features, and significant epiphyseal involvement but less severe platyspondyly and no odontoid hypoplasia.
Question 12
A 3-year-old girl with known achondroplasia presents for routine follow-up. Her parents report she has recently started having difficulty with fine motor skills and occasional tripping. On examination, she has hyperreflexia in the lower extremities and clonus. Her head circumference is at the 95th percentile. Radiographs of the spine show a normal alignment, but a previous MRI at 1 year of age showed mild foramen magnum stenosis.
View Answer & Explanation
Correct Answer: D
Rationale: The symptoms of hyperreflexia, clonus, and fine motor difficulties in a child with achondroplasia, especially with a history of foramen magnum stenosis, are highly suggestive of cervicomedullary compression. Foramen magnum stenosis is a critical complication in achondroplasia, often requiring surgical decompression. Progressive thoracolumbar kyphosis (A) is common in achondroplasia but typically presents with gait disturbance or pain, not upper motor neuron signs in the upper extremities. Lumbar spinal stenosis (B) is also common in achondroplasia but usually manifests later in life with neurogenic claudication or radicular symptoms in the lower extremities. Atlantoaxial instability (C) is rare in achondroplasia. Diastematomyelia (E) is a congenital spinal anomaly not typically associated with achondroplasia.
Question 13
A 10-year-old boy with a history of Hurler syndrome (MPS I) presents with increasing neck pain and gait unsteadiness. Physical examination reveals a short neck, limited neck rotation, and hyperreflexia in all four extremities. Radiographs show a gibbus deformity at the thoracolumbar junction and significant odontoid hypoplasia. An MRI confirms spinal cord compression at the C1-C2 level.
View Answer & Explanation
Correct Answer: B
Rationale: Odontoid hypoplasia leading to atlantoaxial instability and spinal cord compression is a common and severe complication in mucopolysaccharidoses, particularly Hurler syndrome. Given the neurological deficits (hyperreflexia, gait unsteadiness) and confirmed cord compression, surgical stabilization and decompression are indicated. Posterior cervical fusion, typically C1-C2 or C1-C3, is the standard treatment for atlantoaxial instability with neurological compromise in MPS patients. Observation (A) is inappropriate with neurological deficits. Anterior cervical discectomy and fusion (C) is not indicated for atlantoaxial instability due to odontoid hypoplasia. Laminectomy without fusion (D) would decompress but not stabilize, potentially worsening instability. Halo immobilization (E) may be used pre-operatively or for non-surgical cases without neurological deficits, but not as definitive treatment for symptomatic instability.
Question 14
A 14-year-old girl with diastrophic dysplasia presents with severe progressive scoliosis (70-degree thoracolumbar curve) and increasing back pain. She also has characteristic "hitchhiker's thumbs," clubfeet, and cauliflower ears. Her pulmonary function tests show restrictive lung disease. Non-operative management with bracing has failed to control the curve progression.
View Answer & Explanation
Correct Answer: B
Rationale: For severe, progressive scoliosis in adolescents with skeletal dysplasias like diastrophic dysplasia, who have failed bracing, posterior spinal fusion with instrumentation is the standard surgical treatment. Diastrophic dysplasia often presents with stiff, angular curves that are challenging to correct. Anterior vertebral body tethering (A) is typically reserved for younger patients with flexible curves and significant growth remaining. Vertebral column resection (C) is a highly invasive procedure reserved for severe, rigid, congenital deformities or those with significant sagittal imbalance, usually after failed initial fusion or for very complex cases. Growing rod surgery (D) is for very young children with significant growth potential to allow for continued spinal growth while controlling the curve. Spinal osteotomy without fusion (E) would not provide long-term stability or correction.
Question 15
A 5-year-old boy with achondroplasia is noted to have a severe, rigid thoracolumbar kyphosis measuring 65 degrees. He is ambulatory but uses a walker for stability. Radiographs show anterior wedging of several vertebral bodies at the apex of the kyphosis. There are no neurological deficits. His parents are concerned about progression and potential neurological compromise.
View Answer & Explanation
Correct Answer: B
Rationale: In young children with achondroplasia and a progressive thoracolumbar kyphosis without neurological deficits, bracing (thoracolumbar orthosis) is the initial treatment of choice. The goal is to prevent progression and allow for remodeling of the vertebral bodies. Surgical intervention is typically reserved for curves that are progressive despite bracing, rigid curves exceeding 60 degrees in older children, or those with neurological compromise. Observation (A) alone is insufficient for a 65-degree rigid kyphosis. Posterior spinal fusion (C) or combined anterior/posterior fusion (D) would be considered for larger, rigid curves or those with neurological deficits, usually in older children. Vertebral body tethering (E) is not typically used for kyphosis in achondroplasia.
Question 16
A 2-year-old girl is diagnosed with Kniest dysplasia. Her parents are counseled regarding potential orthopedic complications. Which of the following spinal findings is most characteristic and requires close monitoring in this condition?
View Answer & Explanation
Correct Answer: C
Rationale: Kniest dysplasia, like SED congenita, is a type II collagenopathy (*COL2A1* mutation) and is frequently associated with odontoid hypoplasia, leading to atlantoaxial instability. This can result in spinal cord compression and requires careful monitoring. Severe lumbar hyperlordosis (A) is more characteristic of achondroplasia. Progressive cervical kyphosis (B) can occur in diastrophic dysplasia but is less common or severe in Kniest. Early onset idiopathic-like scoliosis (D) can occur in many dysplasias but atlantoaxial instability is a more specific and critical concern for Kniest. Sacral agenesis (E) is a distinct congenital anomaly not typically associated with Kniest dysplasia.
Question 17
A 45-year-old man with a history of achondroplasia presents with bilateral lower extremity weakness, numbness, and neurogenic claudication. He reports symptoms worsening over the past year, limiting his walking distance to less than one block. Physical examination reveals diminished sensation in a stocking-glove distribution and 3/5 strength in ankle dorsiflexion bilaterally. Radiographs show severe narrowing of the lumbar spinal canal, particularly at L3-L5.
View Answer & Explanation
Correct Answer: C
Rationale: Lumbar spinal stenosis is a common and debilitating complication in adults with achondroplasia due to short pedicles, thickened facets, and ligamentum flavum hypertrophy. Given the progressive neurological deficits (weakness, numbness) and severe neurogenic claudication, surgical decompression via lumbar laminectomy is the definitive treatment. Epidural steroid injections (A) and physical therapy (B) may provide temporary symptomatic relief but are unlikely to address severe, progressive neurological deficits caused by structural compression. Anterior lumbar interbody fusion (D) is primarily for instability or discogenic pain, not for multi-level central canal stenosis. Spinal cord stimulator implantation (E) is for chronic neuropathic pain, not for direct mechanical compression causing weakness.
Question 18
A 7-year-old boy with Morquio syndrome (MPS IVA) is being evaluated for spinal involvement. He has a characteristic short trunk, pectus carinatum, and genu valgum. Radiographs show universal platyspondyly with central anterior beaking of the vertebral bodies, and a severely hypoplastic odontoid. What is the most significant spinal complication to anticipate and monitor for in this patient?
View Answer & Explanation
Correct Answer: C
Rationale: Morquio syndrome is well-known for severe odontoid hypoplasia, leading to significant atlantoaxial instability and a high risk of cervical myelopathy. This is the most critical spinal complication requiring close monitoring and often surgical intervention. While thoracolumbar kyphosis (B) can occur in MPS disorders, it is less universally severe and less immediately life-threatening than atlantoaxial instability in Morquio syndrome. Progressive lumbar lordosis (A) is not a primary concern. Severe adolescent idiopathic scoliosis (D) is a distinct entity. Sacral agenesis (E) is a congenital malformation unrelated to Morquio syndrome.
Question 19
A 12-year-old girl with pseudoachondroplasia presents with increasing back pain and a progressive scoliosis. She has normal facial features but significant short stature and waddling gait. Radiographs show mild platyspondyly, irregular and flattened epiphyses, and a 55-degree thoracolumbar scoliosis. Her parents report no neurological symptoms.
View Answer & Explanation
Correct Answer: B
Rationale: Pseudoachondroplasia is caused by mutations in the *COMP* gene. While scoliosis can be progressive, a 55-degree curve in an adolescent without neurological symptoms would typically be managed initially with bracing, similar to idiopathic scoliosis, to attempt to prevent further progression. Surgical fusion (C) is usually considered for curves exceeding 45-50 degrees that are progressive despite bracing, or for larger curves. Genetic counseling for *FGFR3* mutation (A) is incorrect as *FGFR3* is associated with achondroplasia. Atlantoaxial instability (D) is not a primary feature of pseudoachondroplasia. MRI of the brain for hydrocephalus (E) is more relevant for achondroplasia.
Question 20
A 1-year-old infant is diagnosed with metatropic dysplasia. The parents are concerned about the child's future mobility and spinal health. Which of the following is a characteristic spinal deformity often seen in metatropic dysplasia that can be severe and progressive?
View Answer & Explanation
Correct Answer: C
Rationale: Metatropic dysplasia is characterized by severe platyspondyly and progressive kyphoscoliosis, which can be very severe and lead to respiratory compromise. The name "metatropic" refers to the changing body proportions, often with a long trunk in infancy that later appears short due to severe spinal deformity. Isolated lumbar lordosis (A) is not characteristic. Progressive cervical kyphosis (B) can occur but severe kyphoscoliosis is more prominent. Sacral agenesis (D) is a distinct congenital anomaly. Fixed atlantoaxial subluxation (E) is less common than the severe kyphoscoliosis.
Question 21
A 2-year-old boy with achondroplasia presents with a 40-degree thoracolumbar kyphosis. He is not yet walking independently. Radiographs show anterior wedging of the vertebral bodies at the apex of the kyphosis. There are no neurological deficits. What is the most appropriate initial management?
View Answer & Explanation
Correct Answer: A
Rationale: In young, non-ambulatory children with achondroplasia and a flexible thoracolumbar kyphosis, observation and encouraging prone positioning (tummy time) are often sufficient. The kyphosis often resolves or improves spontaneously with ambulation. Bracing (B) is typically reserved for progressive curves or those that persist after ambulation. Surgical intervention (C, D) is for severe, rigid, or neurologically compromising curves. Genetic counseling (E) is important but not a treatment for the kyphosis itself.
Question 22
A 15-year-old boy with Spondyloepiphyseal Dysplasia Tarda (SEDT) presents with chronic low back pain and increasing stiffness. He has a short trunk, barrel chest, and waddling gait. Radiographs show universal platyspondyly with posterior scalloping of the vertebral bodies, and degenerative changes in the lumbar spine. What is the genetic basis for SEDT?
View Answer & Explanation
Correct Answer: D
Rationale: Spondyloepiphyseal Dysplasia Tarda (SEDT) is an X-linked recessive disorder caused by mutations in the *COL2A1* gene. This explains why it primarily affects males and presents later in childhood or adolescence. Spondyloepiphyseal Dysplasia Congenita (SEDc) is an autosomal dominant form of *COL2A1* mutation (A). *SLC26A2* (B) is associated with diastrophic dysplasia. *TRPV4* (C) is associated with metatropic dysplasia and some forms of SED. *FGFR3* (E) is associated with achondroplasia.
Question 23
A 6-year-old girl with a known diagnosis of Mucopolysaccharidosis type IV (Morquio syndrome) is scheduled for a posterior cervical fusion due to atlantoaxial instability and myelopathy. Pre-operative assessment is crucial due to potential anesthetic risks. Which of the following is a primary concern during intubation for this patient?
View Answer & Explanation
Correct Answer: B
Rationale: Patients with Morquio syndrome, and other MPS disorders, often have a short neck, limited neck extension, and potential for atlantoaxial instability. These factors make intubation extremely challenging and carry a high risk of cervical spinal cord injury if not handled with extreme care (e.g., fiberoptic intubation). Malignant hyperthermia (A) is not specifically associated with MPS. Hypoglycemia (C) is not a primary concern. Severe bradycardia (D) is not a direct intubation risk, though spinal cord compression can cause autonomic dysfunction. Aspiration pneumonia (E) is a general risk but not the primary concern related to intubation difficulty and spinal instability.
Question 24
A 3-year-old boy with achondroplasia presents with a 50-degree thoracolumbar kyphosis. He is ambulatory. Radiographs show a flexible curve with no significant anterior wedging. What is the most appropriate management strategy?
View Answer & Explanation
Correct Answer: B
Rationale: For an ambulatory child with achondroplasia and a flexible thoracolumbar kyphosis of 50 degrees, bracing with a thoracolumbar orthosis is the recommended treatment. The brace helps to prevent progression and encourage remodeling of the vertebral bodies. Immediate surgical fusion (A) is too aggressive for a flexible curve without neurological deficits. Observation with prone positioning (C) is more appropriate for non-ambulatory infants or very mild curves. Genetic counseling (D) is part of overall care but not a treatment for the kyphosis. Anterior vertebral body tethering (E) is not typically used for kyphosis in achondroplasia.
Question 25
A 16-year-old male with multiple epiphyseal dysplasia (MED) presents with chronic hip and knee pain, and mild scoliosis (30 degrees). He has a waddling gait and mild short stature. Radiographs show flattened and irregular epiphyses, particularly in the hips, and mild platyspondyly. What is the most common long-term orthopedic complication in patients with MED?
View Answer & Explanation
Correct Answer: C
Rationale: Multiple epiphyseal dysplasia (MED) is characterized by abnormal epiphyseal development, leading to premature and severe osteoarthritis, particularly in weight-bearing joints like the hips and knees. While scoliosis and mild platyspondyly can occur, severe spinal cord compression (A) and atlantoaxial instability (B) are not typical primary features of MED, unlike SED or MPS. Recurrent fractures (D) are more common in osteogenesis imperfecta. Severe limb length discrepancy (E) is not a hallmark of MED, which primarily affects epiphyseal growth symmetrically.
Question 26
A 7-year-old boy with a history of Spondyloepiphyseal Dysplasia Congenita (SEDc) is being evaluated for increasing gait disturbance and clumsiness. He has a known hypoplastic odontoid. Physical examination reveals hyperreflexia in the lower extremities and a positive Babinski sign. An MRI confirms severe spinal cord compression at the C1-C2 level.
View Answer & Explanation
Correct Answer: C
Rationale: In SEDc, odontoid hypoplasia leads to atlantoaxial instability, and with neurological signs (hyperreflexia, Babinski, gait disturbance) and confirmed cord compression, surgical stabilization and decompression are urgently indicated. Posterior cervical fusion, typically C1-C2 or C1-C3, is the standard treatment. Cervical collar immobilization (A) or physical therapy (B) are insufficient for symptomatic instability with myelopathy. Anterior cervical discectomy and fusion (D) is not appropriate for atlantoaxial instability. Observation (E) is contraindicated given the progressive neurological deficits.
Question 27
A 9-year-old girl with diastrophic dysplasia presents with a rigid, progressive cervical kyphosis measuring 40 degrees. She has a short neck and limited range of motion. There are no neurological deficits. What is the most appropriate initial management for this cervical deformity?
View Answer & Explanation
Correct Answer: B
Rationale: Cervical kyphosis is a known complication of diastrophic dysplasia. For a rigid, progressive curve without neurological deficits, a cervical orthosis (brace) is the initial treatment to attempt to prevent further progression. Observation (A) is insufficient for a progressive, rigid 40-degree curve. Halo immobilization (C) is typically used for unstable fractures or as a pre-operative/post-operative adjunct, not as a primary treatment for a progressive kyphosis without instability. Surgical fusion (D, E) would be considered if the kyphosis progresses despite bracing, becomes severe, or develops neurological compromise.
Question 28
A 25-year-old woman with achondroplasia is considering pregnancy. She has a history of mild lumbar spinal stenosis, managed conservatively. What is the most significant spinal concern during pregnancy and delivery for patients with achondroplasia?
View Answer & Explanation
Correct Answer: B
Rationale: Pregnancy in women with achondroplasia often leads to a significant exacerbation of lumbar spinal stenosis symptoms due to increased lumbar lordosis, weight gain, and hormonal changes causing ligamentous laxity and edema, further compromising the already narrowed spinal canal. This can necessitate surgical decompression during or after pregnancy. Thoracolumbar kyphosis progression (A) is less common in adults. Atlantoaxial instability (C) is rare in achondroplasia. Sacroiliac joint dysfunction (D) can occur in any pregnancy but is not specific to achondroplasia. Increased risk of vertebral compression fractures (E) is not a primary concern in achondroplasia.
Question 29
A 65-year-old male presents with a 2-year history of progressive difficulty with balance, episodes of sharp, shooting pains in his legs, and recent onset of urinary incontinence. Physical examination reveals a wide-based gait and diminished proprioception in his lower extremities. Radiographs of his left knee show significant joint disorganization, subchondral sclerosis, osteophytes, and joint effusions, disproportionate to his reported pain level. Laboratory tests confirm a history of syphilis.
View Answer & Explanation
Correct Answer: D
Rationale: The constellation of progressive ataxia (difficulty with balance, wide-based gait), lancinating lightning-like pain, urinary incontinence, loss of sense of position (diminished proprioception), and neuropathic arthropathy (Charcot joint) in a patient with a history of syphilis is highly characteristic of tabes dorsalis, a tertiary manifestation of syphilis. Rheumatoid arthritis, osteoarthritis, gout, and psoriatic arthritis do not typically present with this specific combination of neurological and joint findings.
Question 30
A 70-year-old female is diagnosed with tabes dorsalis after presenting with a Charcot joint in her ankle, severe ataxia, and optic nerve degeneration. Her medical history indicates a syphilis infection treated over 20 years ago. This condition is primarily characterized by the slowly progressive degeneration of which anatomical structure?
View Answer & Explanation
Correct Answer: C
Rationale: Tabes dorsalis is explicitly described as the "slowly progressive degeneration of the spinal cord" occurring in the tertiary phase of syphilis. While other neurological structures can be affected in syphilis, the defining pathology of tabes dorsalis is spinal cord degeneration. The cerebral cortex, peripheral nerves, cerebellum, and brainstem are not the primary sites of degeneration in tabes dorsalis.
Question 31
A 58-year-old male is diagnosed with tabes dorsalis. He reports a history of an untreated sexually transmitted infection in his early 20s. Based on the typical progression of this condition, approximately how long after the initial infection does tabes dorsalis usually manifest?
View Answer & Explanation
Correct Answer: D
Rationale: The text states that tabes dorsalis occurs in the tertiary phase of syphilis, "a decade or more after originally contracting the infection." This indicates a very long latency period. Options A, B, C, and E represent much shorter timeframes that are inconsistent with the typical presentation of tabes dorsalis.
Question 32
A 68-year-old patient with a known history of tabes dorsalis is being evaluated for new-onset joint pain and swelling in her right hip. Radiographs reveal significant degenerative changes, subluxation, and fragmentation, consistent with a neuropathic joint. What is the approximate prevalence of neuropathic arthropathy (Charcot's joint) in patients with tabes dorsalis?
View Answer & Explanation
Correct Answer: B
Rationale: The provided text explicitly states, "Neuropathic arthropathy is seen in 10–20% of patients with tabes dorsalis." This makes option B the correct answer. The other options are outside the stated prevalence range.
Question 33
A 62-year-old male presents with a history of progressive difficulty walking, described as an unsteady, wide-based gait. He also reports episodes of severe, sudden, sharp pains in his legs. Which of the following neurological features is also commonly associated with tabes dorsalis, in addition to ataxia and lancinating pain?
View Answer & Explanation
Correct Answer: C
Rationale: The text lists "loss of sense of position" as one of the serious features of tabes dorsalis, alongside lancinating lightning-like pain and ataxia. Hyperreflexia and spasticity are typically associated with upper motor neuron lesions, while tabes dorsalis primarily affects the dorsal columns (sensory pathways). Tremors at rest are characteristic of Parkinson's disease, and hemiplegia is a sign of a unilateral cerebral lesion, none of which are features of tabes dorsalis.
Question 34
A 72-year-old female is diagnosed with tabes dorsalis. Her medical history indicates a remote syphilis infection. Tabes dorsalis is a manifestation of which phase of syphilis?
View Answer & Explanation
Correct Answer: D
Rationale: The text explicitly states that "Tabes dorsalis is the slowly progressive degeneration of the spinal cord that occurs in the tertiary phase of syphilis." The other options represent earlier or different forms of syphilis that do not typically present with tabes dorsalis.
Question 35
A 60-year-old male with a history of syphilis presents with progressive vision loss over several years. Ophthalmic examination reveals optic atrophy. This ocular manifestation in tabes dorsalis is a result of:
View Answer & Explanation
Correct Answer: D
Rationale: The text specifically lists "deterioration of the optical nerves leading to blindness" as one of the serious features of tabes dorsalis. The other options are common causes of vision loss but are not the specific mechanism described for tabes dorsalis.
Question 36
A 67-year-old patient with tabes dorsalis complains of severe, sudden, and unpredictable pain episodes in his lower extremities. He describes the pain as "like electric shocks." This characteristic pain is best described as:
View Answer & Explanation
Correct Answer: C
Rationale: The text explicitly mentions "lancinating lightning-like pain" as one of the serious features of tabes dorsalis. This description perfectly matches the patient's report of "electric shocks" and sudden, severe pain. The other options describe different types of pain not specifically characteristic of tabes dorsalis.
Question 37
A 75-year-old male with a history of syphilis presents with a severely disorganized and swollen left ankle joint, consistent with a Charcot arthropathy. He also reports difficulty maintaining balance, especially in the dark. This balance issue is primarily due to the loss of which sensory modality?
View Answer & Explanation
Correct Answer: D
Rationale: The text lists "loss of sense of position" as a serious feature of tabes dorsalis. This proprioceptive loss significantly contributes to ataxia and difficulty with balance, particularly when visual cues are absent (e.g., in the dark). While other sensations might be affected, loss of position sense is specifically highlighted as a cause of ataxia.
Question 38
A 63-year-old patient with a long-standing history of syphilis is being evaluated for progressive neurological symptoms. The degeneration of the spinal cord in tabes dorsalis primarily affects which tracts, leading to the characteristic sensory and proprioceptive deficits?
View Answer & Explanation
Correct Answer: C
Rationale: Although not explicitly named in the provided text, the symptoms described for tabes dorsalis (loss of sense of position, lancinating pain, ataxia) are classic signs of dorsal column degeneration. The term "tabes dorsalis" itself refers to the dorsal (posterior) columns. The corticospinal tracts are motor, spinothalamic tracts carry pain and temperature, lateral funiculi contain various tracts, and ventral horns contain motor neurons. Therefore, dorsal column degeneration is the most accurate answer based on the clinical presentation described.
Question 39
A 69-year-old male presents with a Charcot joint of the shoulder, along with a history of progressive gait instability and episodes of severe, sharp leg pains. He also reports difficulty controlling his bladder. This urinary symptom is specifically referred to as:
View Answer & Explanation
Correct Answer: D
Rationale: The text explicitly lists "urinary incontinence" as one of the serious features of tabes dorsalis. Dysuria (painful urination), polyuria (frequent urination), urinary retention (inability to empty bladder), and nocturia (waking up to urinate at night) are other urinary symptoms, but incontinence is the specific one mentioned in the context of tabes dorsalis.
Question 40
A 70-year-old patient with a history of untreated syphilis from decades ago develops a neuropathic arthropathy in his knee. Which of the following is a characteristic feature of the joint degeneration seen in tabes dorsalis?
View Answer & Explanation
Correct Answer: C
Rationale: Neuropathic arthropathy (Charcot's joint) in tabes dorsalis is characterized by progressive joint destruction that is often painless or disproportionately less painful than the severe damage observed, due to the underlying sensory neuropathy. The text refers to "degeneration of the joints (Charcot’s joint)." Inflammatory synovitis is characteristic of rheumatoid arthritis, symmetrical small joint involvement is also typical of rheumatoid arthritis, osteoporosis with pathological fractures is a general bone pathology, and tophi are characteristic of gout. Rapidly progressive, painless destruction is a hallmark of Charcot arthropathy.
Question 41
A 66-year-old female presents with a Charcot joint in her foot, along with a history of progressive difficulty with coordination and balance. She also reports episodes of severe, shooting pains in her legs. These symptoms are consistent with tabes dorsalis, which is described as having what kind of progression?
View Answer & Explanation
Correct Answer: C
Rationale: The text explicitly states, "Tabes dorsalis is the slowly progressive degeneration of the spinal cord." This indicates a gradual worsening of symptoms over time. Acute onset, rapidly progressive, intermittent, or stuttering progressions are not characteristic of tabes dorsalis.
Question 42
A 71-year-old male is diagnosed with tabes dorsalis, presenting with optic atrophy, ataxia, and a Charcot knee. The underlying infectious agent responsible for this condition is:
View Answer & Explanation
Correct Answer: C
Rationale: The case explicitly states that tabes dorsalis occurs in the tertiary phase of "syphilis." Syphilis is caused by the bacterium *Treponema pallidum*. The other options are causative agents for other conditions (HIV for AIDS, HSV for herpes, Borrelia burgdorferi for Lyme disease, Mycobacterium tuberculosis for tuberculosis) and are not associated with tabes dorsalis.
Question 43
A 68-year-old patient with a known history of tabes dorsalis presents with severe, painless destruction of his right ankle joint, requiring orthopedic intervention. This specific type of joint degeneration is referred to as:
View Answer & Explanation
Correct Answer: C
Rationale: The text explicitly states that a serious feature of tabes dorsalis is "degeneration of the joints (Charcot’s joint)." It also mentions "Neuropathic arthropathy," which is synonymous with Charcot's joint. Septic arthritis is an infection, osteomyelitis is bone infection, avascular necrosis is bone death due to lack of blood supply, and pseudogout is crystal deposition disease; none of these are the specific type of joint degeneration associated with tabes dorsalis.
Question 44
A 60-year-old male with a history of syphilis presents with progressive gait disturbance, lancinating pains, and a Charcot joint in his knee. Which of the following symptoms is LEAST likely to be associated with tabes dorsalis?
View Answer & Explanation
Correct Answer: E
Rationale: The text lists lancinating pain, ataxia, deterioration of optical nerves (leading to blindness), urinary incontinence, and loss of sense of position as serious features of tabes dorsalis. Muscle spasticity is typically associated with upper motor neuron lesions, whereas tabes dorsalis primarily affects the dorsal columns, leading to sensory and proprioceptive deficits, not spasticity.
Question 45
A 73-year-old female with a remote history of syphilis presents with a several-year history of progressive unsteadiness, episodes of sharp, shooting pains in her legs, and recent onset of vision impairment. Examination reveals a wide-based gait, diminished vibratory and position sense, and optic atrophy. Radiographs of her right ankle show severe disorganization and fragmentation. This clinical picture is most consistent with:
View Answer & Explanation
Correct Answer: D
Rationale: The combination of progressive ataxia (unsteadiness, wide-based gait), lancinating pains, optic nerve deterioration (vision impairment, optic atrophy), loss of sense of position (diminished vibratory and position sense), and neuropathic arthropathy (Charcot ankle) in a patient with a history of syphilis is the classic presentation of tabes dorsalis. While diabetic neuropathy can cause Charcot foot, it typically does not present with optic atrophy or lancinating pains in this specific pattern. Multiple sclerosis and ALS have different neurological profiles, and peripheral vascular disease does not explain the neurological and joint findings.
Question 46
A 65-year-old male with tabes dorsalis is being managed for his symptoms. The degeneration of the spinal cord in this condition primarily affects which type of neurological function?
View Answer & Explanation
Correct Answer: C
Rationale: The key features of tabes dorsalis listed in the text, such as lancinating pain, ataxia (due to proprioceptive loss), and loss of sense of position, all point to a primary impact on sensory and proprioceptive pathways within the spinal cord (specifically the dorsal columns). While autonomic functions (like urinary incontinence) are affected, and ataxia involves cerebellar input, the core degeneration is of sensory tracts. Motor and cognitive functions are not primarily affected in tabes dorsalis itself.
Question 47
A 70-year-old patient presents with a Charcot joint of the foot. During the workup, a history of syphilis treated decades ago is uncovered, along with neurological symptoms including ataxia and lancinating pains. The development of tabes dorsalis in this patient indicates that the initial syphilis infection was:
View Answer & Explanation
Correct Answer: D
Rationale: Tabes dorsalis is a manifestation of the tertiary phase of syphilis, occurring a decade or more after the initial infection. Its development indicates that the infection either was not adequately treated, allowing it to progress to the tertiary stage, or that the treatment failed to prevent late neurological sequelae. It does not imply a mild infection, spontaneous resolution, or a false positive diagnosis. Full eradication would prevent tertiary manifestations.
Question 48
A 62-year-old female is diagnosed with tabes dorsalis. Her symptoms include progressive gait disturbance, episodes of severe leg pain, and urinary incontinence. The term "syphilitic myelopathy" in the context of tabes dorsalis refers to:
View Answer & Explanation
Correct Answer: C
Rationale: The title of the case is "Arthropathy in Tabes: Syphilitic Myelopathy," and the text describes tabes dorsalis as "the slowly progressive degeneration of the spinal cord that occurs in the tertiary phase of syphilis." Myelopathy specifically refers to a disorder of the spinal cord. Therefore, "syphilitic myelopathy" directly refers to spinal cord degeneration caused by syphilis. The other options describe different neurological manifestations of syphilis or other conditions.
Question 49
A 65-year-old male presents with a 2-year history of progressive difficulty walking, described as a wide-based, unsteady gait. He also reports intermittent, sharp, shooting pains in his legs that resolve spontaneously. Physical examination reveals diminished proprioception and vibratory sense in the lower extremities. Radiographs of his knees show significant degenerative changes with joint disorganization disproportionate to his reported pain level. His medical history is notable for an untreated sexually transmitted infection decades prior. Which of the following is the most likely underlying diagnosis?
View Answer & Explanation
Correct Answer: D
Rationale: The constellation of progressive ataxia, lancinating lightning-like pains, loss of sense of position (proprioception), and neuropathic arthropathy (Charcot's joint) in a patient with a history suggestive of prior untreated syphilis is highly characteristic of tabes dorsalis, a tertiary manifestation of syphilis. Diabetic neuropathy can cause neuropathic arthropathy and sensory deficits but typically presents with different pain characteristics and less prominent ataxia in this manner. ALS, MS, and Parkinson's disease do not typically present with this specific combination of symptoms, especially the lancinating pains and Charcot's joint.
Question 50
A 72-year-old female presents with severe, sudden, brief, and intense "lightning-like" pains in her lower extremities. These pains are unpredictable and debilitating. She also reports difficulty with balance, especially in the dark. Her neurological examination reveals diminished deep tendon reflexes and impaired sensation to light touch and pinprick. This symptom complex is most consistent with which feature of tabes dorsalis?
View Answer & Explanation
Correct Answer: C
Rationale: The description of "severe, sudden, brief, and intense 'lightning-like' pains" directly corresponds to the characteristic lancinating pains seen in tabes dorsalis. While ataxia, optic nerve degeneration, urinary incontinence, and loss of sense of position are also features of tabes dorsalis, the specific pain description points to lancinating pain. Ataxia would describe the balance difficulty, but not the pain itself.
Question 51
A 58-year-old male presents with a 3-year history of progressive difficulty with coordination and balance, particularly when walking without visual cues. He describes his gait as "clumsy" and often stumbles. On examination, he exhibits a wide-based gait and struggles with tandem walking. This neurological deficit, commonly seen in tabes dorsalis, is best described as:
View Answer & Explanation
Correct Answer: C
Rationale: The patient's symptoms of progressive difficulty with coordination, balance, a wide-based gait, and stumbling, especially without visual cues, are classic manifestations of ataxia. Ataxia in tabes dorsalis results from the degeneration of the dorsal columns, which carry proprioceptive information. Spasticity, tremor, paresis, and dystonia are different types of motor disorders not primarily described by these symptoms.
Question 52
A 68-year-old male with a known history of tabes dorsalis presents with severe, painless destruction of his right ankle joint. Radiographs show extensive joint disorganization, fragmentation of articular surfaces, subluxation, and osteophyte formation. Despite the severe radiographic findings, he reports minimal pain. This specific joint pathology is known as:
View Answer & Explanation
Correct Answer: D
Rationale: The description of severe, painless joint destruction with disorganization, fragmentation, and subluxation in a patient with tabes dorsalis is pathognomonic for Charcot's joint, also known as neuropathic arthropathy. This condition arises due to loss of protective sensation and proprioception, leading to repetitive microtrauma and progressive joint destruction. Osteoarthritis, rheumatoid arthritis, septic arthritis, and gouty arthritis present with different clinical and radiographic features, and typically involve significant pain.
Question 53
A 60-year-old patient diagnosed with tabes dorsalis is being counseled on potential long-term complications. The patient is concerned about developing joint problems. Based on epidemiological data, what is the approximate percentage of patients with tabes dorsalis who develop neuropathic arthropathy?
View Answer & Explanation
Correct Answer: C
Rationale: The provided text states that neuropathic arthropathy is seen in 10–20% of patients with tabes dorsalis. This makes it a significant, though not universal, complication. The other percentages are either too low or too high based on the given information.
Question 54
A 70-year-old male presents with a history of syphilis treated decades ago, now experiencing progressive neurological symptoms including difficulty with balance and urinary retention. MRI of the spine reveals atrophy and signal changes in the posterior columns. This finding is consistent with the primary pathological process of tabes dorsalis, which is:
View Answer & Explanation
Correct Answer: C
Rationale: Tabes dorsalis is characterized by the slowly progressive degeneration of the spinal cord, specifically affecting the dorsal columns (posterior columns). This degeneration leads to the loss of proprioception, vibratory sense, and contributes to ataxia and lancinating pains. Degeneration of anterior horn cells is seen in conditions like ALS, demyelination of corticospinal tracts in MS, and spinal cord compression is a mechanical issue. Inflammation of nerve roots can occur but is not the defining pathology of tabes dorsalis.
Question 55
A 62-year-old patient with a long-standing history of tabes dorsalis reports a gradual decline in vision over the past several years, now significantly impacting daily activities. Ophthalmic examination reveals optic atrophy. This visual impairment is a direct consequence of which feature of tabes dorsalis?
View Answer & Explanation
Correct Answer: C
Rationale: The case text explicitly states that "deterioration of the optical nerves leading to blindness" is one of the serious features of tabes dorsalis. Optic atrophy is the clinical manifestation of this deterioration. Cerebellar dysfunction causes ataxia, peripheral neuropathy affects sensation in extremities, cortical blindness is a brain-based visual impairment, and retinal detachment is a distinct ocular pathology not directly caused by tabes.
Question 56
A 75-year-old male with a history of tabes dorsalis complains of frequent involuntary leakage of urine, particularly when coughing or laughing, and a sensation of incomplete bladder emptying. Urodynamic studies show a neurogenic bladder. This symptom is a recognized feature of tabes dorsalis, specifically:
View Answer & Explanation
Correct Answer: D
Rationale: The case text lists "urinary incontinence" as one of the serious features of tabes dorsalis. While different types of incontinence exist (stress, urge, overflow), the general term "urinary incontinence" encompasses the bladder dysfunction caused by the neurological degeneration in tabes. The neurogenic bladder in tabes often leads to a combination of storage and emptying issues, manifesting as incontinence. Nocturia is frequent nighttime urination, which can be a symptom but not the primary feature described.
Question 57
A 68-year-old patient with suspected tabes dorsalis undergoes a neurological examination. When asked to stand with feet together and eyes closed, the patient sways significantly and loses balance. This finding, known as a positive Romberg sign, indicates a deficit in which sensory modality, a hallmark of tabes dorsalis?
View Answer & Explanation
Correct Answer: D
Rationale: A positive Romberg sign is indicative of impaired proprioception, or "loss of sense of position," which is a key feature of tabes dorsalis due to dorsal column degeneration. Patients rely on visual input to compensate for the lack of proprioceptive feedback, hence the instability when eyes are closed. While vibratory sensation is also affected, the Romberg sign specifically tests proprioception. Pain, temperature, and light touch are carried by different spinal tracts.
Question 58
A 60-year-old male presents with a 15-year history of untreated syphilis. He now complains of episodes of severe, stabbing leg pains, difficulty walking steadily, and recent onset of urinary leakage. Physical examination reveals bilateral knee joint effusions with crepitus and instability, despite minimal reported pain. These findings are most consistent with which stage of syphilis?
View Answer & Explanation
Correct Answer: D
Rationale: Tabes dorsalis, characterized by lancinating pains, ataxia (difficulty walking steadily), urinary incontinence, and neuropathic arthropathy (Charcot's joint), is a manifestation of the tertiary phase of syphilis. This phase typically occurs a decade or more after the initial infection. Primary and secondary syphilis present with earlier, distinct symptoms (chancre, rash, lymphadenopathy). Latent syphilis is asymptomatic, and congenital syphilis occurs in newborns.
Question 59
A 63-year-old patient with a long-standing history of syphilis, now presenting with progressive neurological deficits and joint destruction, is diagnosed with tabes dorsalis. The degeneration of the spinal cord in this condition is described as "slowly progressive." This implies that the onset of symptoms typically occurs:
View Answer & Explanation
Correct Answer: D
Rationale: The case text explicitly states that tabes dorsalis "occurs in the tertiary phase of syphilis, a decade or more aft er originally contracting the infection." This long latency period is characteristic of tertiary syphilis manifestations. The other options represent much shorter timeframes or specific populations not relevant to the typical adult onset of tabes dorsalis.
Question 60
A 70-year-old patient is diagnosed with tabes dorsalis after presenting with a classic constellation of symptoms including lancinating pains, ataxia, and early signs of neuropathic arthropathy. The underlying infectious agent responsible for this condition is:
View Answer & Explanation
Correct Answer: C
Rationale: Tabes dorsalis is a manifestation of tertiary syphilis, which is caused by the bacterium Treponema pallidum. HIV, HSV, Borrelia burgdorferi (Lyme disease), and Mycobacterium tuberculosis (tuberculosis) are all infectious agents that can cause neurological symptoms, but they are not the cause of syphilis or tabes dorsalis.
Question 61
A 66-year-old patient with tabes dorsalis develops severe destruction of the hip joint. Radiographs show extensive bone resorption, fragmentation, and joint instability. The key factor contributing to the progressive joint degeneration in this condition is:
View Answer & Explanation
Correct Answer: C
Rationale: Neuropathic arthropathy (Charcot's joint) in tabes dorsalis is primarily caused by the loss of protective sensation (pain, temperature) and proprioception due to dorsal column degeneration. This leads to repetitive microtrauma, unnoticed injuries, and progressive joint destruction without the patient experiencing the normal protective pain signals. Direct bacterial infection, autoimmune inflammation, primary osteonecrosis, and systemic metabolic disorders are causes of other types of arthropathy but not the primary mechanism for Charcot's in tabes.
Question 62
A 71-year-old male with a history of tabes dorsalis presents with progressive difficulty with fine motor control, particularly when buttoning his shirt or writing. He also reports a sensation of numbness and tingling in his hands. These symptoms are consistent with the degeneration of which specific part of the spinal cord?
View Answer & Explanation
Correct Answer: C
Rationale: The symptoms of difficulty with fine motor control (due to impaired proprioception and vibratory sense) and numbness/tingling are characteristic of dorsal column (posterior column) degeneration. The dorsal columns are responsible for transmitting fine touch, vibratory sense, and proprioception. Lateral corticospinal tracts control voluntary motor movement, spinothalamic tracts transmit pain and temperature, and the ventral horn contains motor neurons.
Question 63
A 69-year-old patient with a confirmed diagnosis of tabes dorsalis is being evaluated for orthopedic complications. Which of the following statements accurately describes the nature of joint involvement in tabes dorsalis?
View Answer & Explanation
Correct Answer: C
Rationale: Neuropathic arthropathy (Charcot's joint) in tabes dorsalis is characterized by slowly progressive, often painless, joint degeneration due to the loss of protective sensation and proprioception. It is not typically acute or painful, nor does it primarily involve symmetrical small joint inflammation or the axial skeleton. The prevalence is 10-20%, not less than 1%.
Question 64
A 73-year-old male with a history of tabes dorsalis presents with a severely disorganized and unstable left knee joint. He reports minimal pain despite significant radiographic evidence of destruction. The orthopedic surgeon explains that the lack of pain perception is a critical factor in the progression of this joint disease. This phenomenon is directly related to the degeneration of which neurological pathway?
View Answer & Explanation
Correct Answer: D
Rationale: While the spinothalamic tracts transmit pain and temperature, the primary degeneration in tabes dorsalis affects the dorsal columns. The dorsal columns are responsible for proprioception and vibratory sense, and their degeneration leads to the loss of protective sensation (including the ability to perceive minor injuries that would normally cause pain and lead to protective behaviors). This lack of protective sensation, combined with impaired proprioception, is the key factor in the development of Charcot's joint. The pyramidal and extrapyramidal tracts are involved in motor control, and cerebellar pathways in coordination.
Question 65
A 60-year-old patient is being evaluated for suspected tabes dorsalis. Which of the following symptoms is LEAST likely to be a direct manifestation of tabes dorsalis, based on the provided clinical description?
View Answer & Explanation
Correct Answer: D
Rationale: The provided text lists lancinating lightning-like pain, ataxia, deterioration of the optical nerves leading to blindness, urinary incontinence, loss of sense of position, and degeneration of the joints (Charcot’s joint) as features of tabes dorsalis. Resting tremor is a characteristic symptom of Parkinson's disease and is not typically associated with tabes dorsalis. While some motor symptoms can occur due to severe sensory loss, a classic resting tremor is not a direct feature.
Question 66
A 65-year-old patient presents with a 15-year history of progressive neurological symptoms, including gait instability, episodes of sharp leg pains, and recent vision changes. He also has significant destruction of his left ankle joint. His medical history indicates a past infection with Treponema pallidum that was never fully treated. This clinical picture represents a manifestation of which phase of syphilis?
View Answer & Explanation
Correct Answer: E
Rationale: Tabes dorsalis, with its characteristic neurological and orthopedic features (gait instability/ataxia, lancinating pains, vision changes, Charcot's joint), is a classic manifestation of tertiary syphilis. This phase typically develops a decade or more after the initial infection, consistent with the 15-year history mentioned. Primary, secondary, and latent syphilis represent earlier stages with different clinical presentations.
Question 67
A 70-year-old patient diagnosed with tabes dorsalis is concerned about the progression of his condition. The physician explains that tabes dorsalis is characterized by "slowly progressive degeneration of the spinal cord." This implies that:
View Answer & Explanation
Correct Answer: C
Rationale: The term "slowly progressive degeneration" indicates that the neurological deficits, including those leading to joint degeneration, develop gradually over an extended period, typically many years. It does not imply sudden onset, spontaneous resolution, or that only joint degeneration progresses. While treatment can halt the progression of the underlying syphilis, it generally cannot fully reverse existing neurological damage.
Question 68
A 7-year-old male presents to the emergency department with acute onset of right knee pain, swelling, and refusal to bear weight. His mother reports he has had a fever for the past 24 hours. Physical examination reveals a warm, erythematous, and exquisitely tender right knee with severely limited range of motion. Laboratory tests show elevated C-reactive protein and white blood cell count.
View Answer & Explanation
Correct Answer: B
Rationale: The provided text states, "In 90% of all cases S. haemolyticus is responsible for the septic arthritis." This makes S. haemolyticus the most likely causative organism according to the given information. While Staphylococcus aureus is generally considered the most common cause of septic arthritis in many contexts, the question specifically asks based on the provided text. The main distractor, Staphylococcus aureus, is a common cause of septic arthritis but is not cited as the predominant organism in the provided text.
Question 69
A 55-year-old female presents with acute pain, swelling, and warmth in her left knee, which developed two days after receiving an intra-articular corticosteroid injection for osteoarthritis. She denies any recent trauma or systemic illness. Physical examination reveals a swollen, tender knee with restricted range of motion. Radiographs are unremarkable for acute changes.
View Answer & Explanation
Correct Answer: D
Rationale: The clinical vignette describes the onset of symptoms following an intra-articular injection. The text explicitly lists "iatrogenic infection (e.g. intraarticular injection)" as one of the ways bacteria may affect joints. The main distractor, hematogenous spread, is a common mode of infection but is less likely given the direct temporal relationship with an intra-articular procedure.
Question 70
A 28-year-old male presents with a 3-day history of severe pain, swelling, and redness in his right knee. He reports a fever of 101.5°F. On examination, the knee is markedly swollen, erythematous, warm to touch, and extremely painful with any attempt at movement. Range of motion is severely limited.
View Answer & Explanation
Correct Answer: A
Rationale: The text describes acute purulent arthritis as presenting with a swollen joint, red skin, and fever. The patient's symptoms of acute onset, severe pain, swelling, redness, warmth, fever, and limited range of motion are all classic signs of acute purulent arthritis. The main distractor, chronic purulent arthritis, is characterized by less common signs of inflammation and a more insidious onset, which does not fit this patient's presentation.
Question 71
A 68-year-old female presents with a 6-month history of persistent right knee pain, swelling, and stiffness. She reports a gradual worsening of symptoms and significant limitation in her daily activities. She denies any recent fever, chills, or skin redness around the knee. Physical examination reveals a swollen, mildly warm right knee with crepitus and a restricted, painful range of motion.
View Answer & Explanation
Correct Answer: B
Rationale: The text states that in chronic purulent arthritis, "the signs of inflammation are less common," while the joint remains swollen, painful, and has limited range of motion. This patient's long-standing symptoms, absence of acute inflammatory signs (fever, redness), and persistent swelling and pain are consistent with chronic purulent arthritis. The main distractor, acute purulent arthritis, would typically present with more pronounced acute inflammatory signs such as fever and erythema, which are absent in this case.
Question 72
A 40-year-old male presents with a swollen, painful left knee and elevated inflammatory markers. Clinical suspicion for bacterial arthritis is high. The orthopedic surgeon plans to perform a procedure to confirm the diagnosis.
View Answer & Explanation
Correct Answer: D
Rationale: The text explicitly states, "Punction and bacterial culture are the method of choice to make a certain diagnosis in bacterial arthritis." This procedure directly identifies the pathogen from the infected joint fluid. The main distractor, blood culture, can be positive in septic arthritis but is not as definitive as direct joint fluid culture for confirming joint infection.
Question 73
During arthrocentesis of a swollen, painful knee, a yellowish, turbid fluid is aspirated. This fluid is sent for analysis to confirm the diagnosis of bacterial arthritis.
View Answer & Explanation
Correct Answer: B
Rationale: The text describes the joint fluid in purulent arthritis as "pus of yellowish color, a necrotic mass with bacteria and white blood cells." This directly indicates that high white blood cell counts are an expected finding. The main distractor, predominantly lymphocytes, would be more characteristic of chronic inflammatory or viral arthritis, not acute bacterial infection.
Question 74
A 3-year-old child is admitted with a diagnosis of acute septic arthritis of the hip. Blood tests are ordered to monitor the inflammatory response.
View Answer & Explanation
Correct Answer: A
Rationale: The text states, "Laboratory tests show elevated C reactive protein levels, high sedimentation rate, high white blood cell counts." Therefore, elevated C-reactive protein levels are an expected finding. The main distractor, low erythrocyte sedimentation rate, contradicts the text which specifies a "high sedimentation rate" in bacterial arthritis.
Question 75
A 6-month-old infant presents with irritability, refusal to move the right lower extremity, and a swollen, warm right hip. Physical examination reveals pain with passive range of motion of the hip. Suspecting bacterial arthritis, the physician considers common sites of involvement.
View Answer & Explanation
Correct Answer: C
Rationale: The text lists "the hip" as one of the most common sites where septic arthritis may occur. The vignette also mentions "newborn's coxitis" as an example of direct affection in metaphyseal osteomyelitis, further highlighting the hip's susceptibility in children. The main distractor, elbow, is not explicitly listed as one of the most common sites in the provided text, although it can be affected.
Question 76
A 72-year-old male with a long history of chronic purulent arthritis of the right knee presents for follow-up. He complains of persistent pain and stiffness. Radiographs of his right knee are obtained.
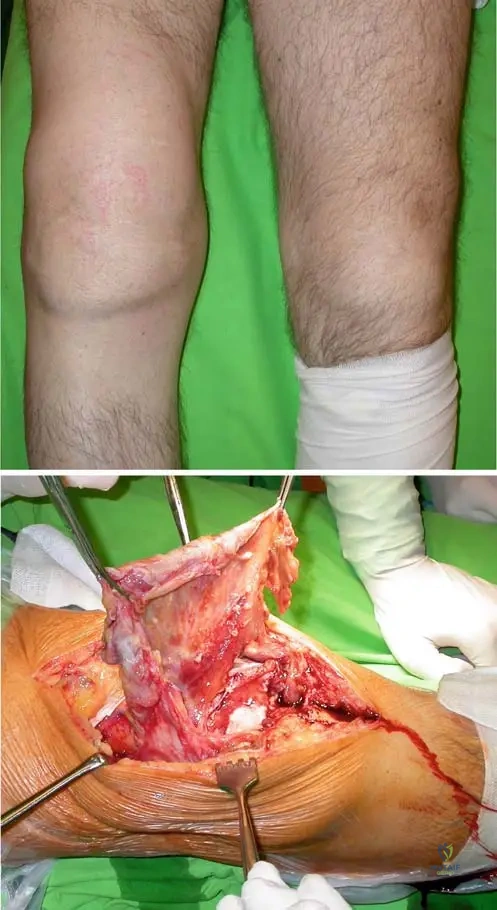
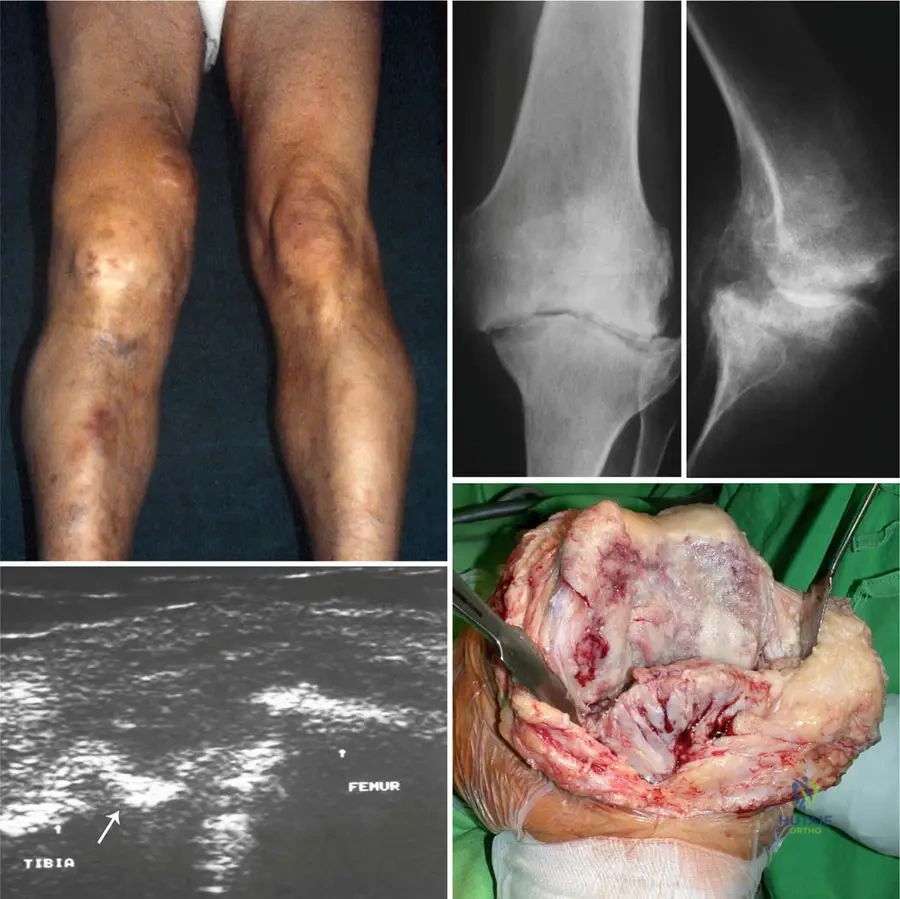
View Answer & Explanation
Correct Answer: B
Rationale: The text states, "AP (b) and lateral (c) view radiographs reveal secondary osteoarthritis of the same patient due to chronic bacterial arthritis: there are secondary osteoarthritic changes, such as subchondral sclerosis, osteophytes, subchondral cyst formation, narrowing of joint space." The images provided show these characteristic changes. The main distractor, primary osteoarthritis, would not be directly attributed to chronic bacterial arthritis as a secondary complication.
Question 77
A 58-year-old patient with chronic purulent arthritis of the knee undergoes ultrasonography to assess the joint's condition.
View Answer & Explanation
Correct Answer: B
Rationale: The text describes ultrasonography in chronic purulent arthritis as "detecting the well visible irregular, rough surface of the medial tibia and femur." This is a specific finding mentioned for this condition. The main distractor, joint effusion with normal cartilage surface, would not reflect the destructive changes expected in chronic purulent arthritis.
Question 78
A 65-year-old patient with a long-standing history of chronic purulent arthritis of the knee undergoes surgical exploration and debridement. The surgeon is assessing the intra-articular structures.
View Answer & Explanation
Correct Answer: B
Rationale: The text describes the intraoperative findings for chronic purulent arthritis as "serious destruction of cartilage surface of the knee, with osteophytes, edematous soft tissues." The main distractor, intact cartilage surface with minimal synovial inflammation, is contrary to the expected severe degenerative changes in chronic purulent arthritis.
Question 79
A 4-year-old child presents with acute onset of right knee pain, refusal to bear weight, and fever. Physical exam reveals a swollen, warm, and exquisitely tender knee with severely limited range of motion. The differential diagnosis includes both septic arthritis and osteomyelitis.
View Answer & Explanation
Correct Answer: C
Rationale: The text states, "The primary bacterial arthritis is most likely in the childhood, and occurs twice as often as osteomyelitis." The main distractor, half as often, directly contradicts the information provided in the text.
Question 80
A 32-year-old construction worker sustains a deep laceration over his right knee joint after falling onto a rusty nail. Despite initial wound care, he develops increasing pain, swelling, and purulent discharge from the wound site, along with fever.
View Answer & Explanation
Correct Answer: C
Rationale: The text lists "penetrating injury" as one of the ways bacteria may affect the joints. The deep laceration from a rusty nail directly into the joint space is a classic example of a penetrating injury leading to infection. The main distractor, hematogenous spread, involves bacteria traveling through the bloodstream from a distant site, which is not the primary mechanism described in this vignette.
Question 81
A 60-year-old patient presents with a chronically swollen and painful right knee with limited range of motion. They report no recent fever or skin redness. Arthrocentesis reveals yellowish pus, and culture confirms bacterial arthritis.
View Answer & Explanation
Correct Answer: E
Rationale: The text explicitly states, "in chronic form the signs of inflammation are less common." This refers to systemic signs like fever and local signs like skin redness. The main distractor, signs of inflammation are more severe, is characteristic of acute bacterial arthritis, not the chronic form described.
Question 82
Arthrocentesis is performed on a patient with suspected bacterial arthritis. The fluid analysis is crucial for diagnosis, and several characteristics are typically assessed.
View Answer & Explanation
Correct Answer: D
Rationale: The text states, "The quality, cell count and color of the articular fluid (pus) are the characteristics" used for diagnosis. While the presence of bacteria is implied by "a necrotic mass with bacteria," viscosity is not mentioned as a specific characteristic for diagnosis in the provided text. The main distractor, presence of bacteria, is a direct component of the "necrotic mass with bacteria" and is the ultimate goal of the culture, making it a critical diagnostic characteristic, even if not explicitly listed in the "quality, cell count, color" triad.
Question 83
A 48-year-old male with a history of intravenous drug use presents with acute onset of right knee pain, swelling, and fever. He has a skin abscess on his forearm. Physical examination reveals a warm, erythematous, and tender right knee with limited range of motion.
View Answer & Explanation
Correct Answer: B
Rationale: The text states, "Septic articular inflammation may occur primarily in the joint, or it is developed secondary due to a septic inflammation in the body elsewhere." The patient's skin abscess (septic inflammation elsewhere) leading to knee infection is a classic example of secondary bacterial arthritis. The main distractor, primary bacterial arthritis, occurs directly in the joint without an obvious distant source, which is not the case here.
Question 84
A 68-year-old patient with a history of chronic bacterial arthritis of the knee presents for follow-up. Radiographs are obtained to assess for secondary changes.


Question 84
A 4-year-old male presents to the emergency department with acute onset of right hip pain, refusal to bear weight, and a fever of 102°F. Physical examination reveals a swollen, warm, and exquisitely tender hip with severely limited range of motion. Arthrocentesis is performed, yielding purulent fluid. Given the high incidence of primary bacterial arthritis in childhood, what is the most likely causative organism responsible for this condition, according to the provided text?
View Answer & Explanation
Correct Answer: B
Rationale: The text explicitly states, "In 90% of all cases S. haemolyticus is responsible for the septic arthritis." This makes it the most likely causative organism in a primary bacterial arthritis case, especially in childhood. Main Distractor: Staphylococcus aureus (A) is a common cause of septic arthritis overall, but the provided text specifically highlights S. haemolyticus as responsible for 90% of cases of septic arthritis, making it the best answer based on the given information.
Question 85
A 55-year-old female presents with a 3-day history of acute left knee pain, swelling, and warmth. She reports a low-grade fever and general malaise. Physical examination reveals an erythematous, swollen knee with significant pain on palpation and severely restricted range of motion. Laboratory tests show elevated C-reactive protein (CRP) and a high white blood cell (WBC) count. What is the method of choice to make a certain diagnosis in bacterial arthritis?
View Answer & Explanation
Correct Answer: D
Rationale: The text clearly states, "Punction and bacterial culture are the method of choice to make a certain diagnosis in bacterial arthritis." This directly addresses the question about definitive diagnosis. Main Distractor: Blood culture (C) can be positive in septic arthritis but is not as definitive as direct culture of the joint fluid, as it may not always identify the pathogen or confirm its presence within the joint. Imaging (A, B) and inflammatory markers (E) are supportive but not diagnostic methods of choice.
Question 86
A 38-year-old male presents with acute onset of pain and swelling in a peripheral joint. The clinician is considering septic arthritis and is reviewing common sites of involvement. Based on the provided clinical context, which of the following joints is *least* commonly mentioned as a site where septic arthritis may occur?
View Answer & Explanation
Correct Answer: D
Rationale: The text lists the most common sites as "the knee, the olecranon bursa, the wrist and finger joints, the hip, the glenohumeral joint and the metatarsophalangeal joint." The temporomandibular joint is not mentioned in this list. Main Distractor: While the olecranon bursa (C) is a bursa rather than a true joint, the text explicitly includes it in the list of common sites for septic arthritis, making it a commonly affected area according to the provided information.
Question 87
A 62-year-old diabetic patient undergoes arthrocentesis for a swollen, painful right knee. The collected articular fluid is sent for analysis. The text describes the characteristics of articular fluid in purulent arthritis. Which of the following findings would be most consistent with purulent arthritis?
View Answer & Explanation
Correct Answer: B
Rationale: The text states, "The joint contains pus of yellowish color, a necrotic mass with bacteria and white blood cells." This directly describes the characteristic findings of articular fluid in purulent arthritis. Main Distractor: Milky, non-viscous fluid with urate crystals (D) describes gout, a crystalline arthritis, which is distinct from bacterial arthritis. While both can cause inflammation, the specific fluid characteristics differ significantly.
Question 88
A 72-year-old male develops acute septic arthritis of the knee three days after receiving an intra-articular corticosteroid injection for osteoarthritis. He presents with increased pain, swelling, warmth, and fever. Based on the provided text, what is the most appropriate classification for the mode of infection in this patient?
View Answer & Explanation
Correct Answer: D
Rationale: The text lists "iatrogenic infection (e.g. intraarticular injection)" as one of the ways bacteria may affect the joints. An infection following an intra-articular injection directly falls under this category. Main Distractor: Hematogenous spread (A) involves bacteria traveling through the bloodstream from a distant site. While possible, the direct temporal and anatomical link to the intra-articular injection makes iatrogenic infection the more specific and accurate classification based on the vignette and text.
Question 89
A 68-year-old female presents with a several-month history of persistent right knee pain, swelling, and limited range of motion, following an inadequately treated acute bacterial arthritis episode. While she has some discomfort, the acute inflammatory signs are less pronounced. According to the text, which of the following clinical signs would be *least* common in this chronic presentation compared to an acute form?
View Answer & Explanation
Correct Answer: D
Rationale: The text states, "in acute form the skin is red, fever may occur, in chronic form the signs of inflammation are less common." Redness of the skin is a classic acute inflammatory sign that would be less prominent in chronic cases. Main Distractor: Joint swelling (A), pain (B), and limited range of motion (C) are described as features of both acute and chronic forms, though the intensity of acute inflammatory signs like redness and fever diminishes in chronic presentations.
Question 90
A 65-year-old male presents with chronic right knee pain and limited range of motion following a history of bacterial arthritis. AP and lateral radiographs are obtained.

Which of the following radiographic findings is *most* characteristic of secondary osteoarthritis due to chronic bacterial arthritis, as described in the text and depicted in the image context?
View Answer & Explanation
Correct Answer: D
Rationale: The text explicitly states that radiographs in secondary osteoarthritis due to chronic bacterial arthritis "reveal secondary osteoarthritic changes, such as subchondral sclerosis, osteophytes, subchondral cyst formation, narrowing of joint space." Subchondral sclerosis is directly listed. Main Distractor: Joint space widening (A) is the opposite of what is expected; joint space narrowing is a characteristic feature of osteoarthritis. Subchondral lucency (B) is not specifically mentioned as a primary characteristic, while subchondral sclerosis (D) is.
Question 91
A pediatrician is reviewing the epidemiology of musculoskeletal infections in children. They are particularly interested in the relative frequency of primary bacterial arthritis compared to osteomyelitis. According to the provided text, what is the relationship between the incidence of primary bacterial arthritis and osteomyelitis in childhood?
View Answer & Explanation
Correct Answer: B
Rationale: The text states, "The primary bacterial arthritis is most likely in the childhood, and occurs twice as often as osteomyelitis." This directly answers the question. Main Distractor: Occurs half as often (A) is the inverse of the correct statement and directly contradicts the information provided in the text.
Question 92
A 70-year-old patient presents with a long history of right knee pain and stiffness. Clinical examination reveals swelling and severely limited range of motion. AP and lateral radiographs are shown, illustrating the effects of chronic purulent arthritis.

Based on the provided image and clinical context, which of the following is a characteristic radiographic finding of secondary osteoarthritis due to chronic bacterial arthritis?
View Answer & Explanation
Correct Answer: C
Rationale: The text explicitly describes radiographic findings in secondary osteoarthritis due to chronic bacterial arthritis as including "subchondral sclerosis, osteophytes, subchondral cyst formation, narrowing of joint space." Subchondral sclerosis is a direct match. Main Distractor: Absence of joint space narrowing (B) is incorrect; joint space narrowing is a hallmark of osteoarthritis, including secondary forms from bacterial arthritis, as stated in the text.
Question 93
A 45-year-old male presents with acute onset of right knee pain, swelling, and fever. Physical examination reveals a warm, erythematous, and tender knee with restricted movement. Blood samples are drawn for laboratory analysis. Which combination of laboratory findings would most strongly support a diagnosis of acute bacterial arthritis, according to the provided text?
View Answer & Explanation
Correct Answer: B
Rationale: The text states, "Laboratory tests show elevated C reactive protein levels, high sedimentation rate, high white blood cell counts." This combination directly matches the correct option. Main Distractor: Normal CRP levels, high ESR, high WBC counts (E) is partially correct but misses the elevated CRP, which is a key indicator of acute inflammation and infection mentioned in the text.
Question 94
A 58-year-old patient with suspected chronic bacterial arthritis of the knee undergoes ultrasonography to assess the joint condition. The image provided illustrates a typical ultrasonographic finding in such a case.

As depicted in the provided image (d) and described in the text, what specific finding would an ultrasonography reveal in chronic bacterial arthritis of the knee?
View Answer & Explanation
Correct Answer: D
Rationale: The text explicitly states, "Ultrasonography (d) detecting the well visible irregular, rough surface of the medial tibia and femur (arrow)." This directly describes the expected ultrasound finding. Main Distractor: Smooth articular cartilage surface (A) is incorrect. Chronic bacterial arthritis leads to articular destruction, resulting in an irregular and rough surface, not a smooth one.
Question 95
A 60-year-old patient with a long-standing history of chronic purulent arthritis of the knee, unresponsive to conservative management, undergoes surgical exploration. The intraoperative picture (e) from the provided context illustrates the findings.

Based on the provided image and description of chronic purulent arthritis, what intraoperative finding would be expected?
View Answer & Explanation
Correct Answer: D
Rationale: The text describes the intraoperative picture (e) as illustrating "serious destruction of cartilage surface of the knee, with osteophytes, edematous soft tissues." Serious destruction of cartilage surface is a direct match. Main Distractor: Intact articular cartilage (A) is incorrect. Chronic purulent arthritis is characterized by significant articular destruction, not preservation of cartilage.
Question 96
A 5-year-old child develops acute septic arthritis of the hip. Investigations confirm the diagnosis, and there is no evidence of a preceding systemic infection or trauma. The infection is believed to have originated directly within the joint. This presentation is best classified as:
View Answer & Explanation
Correct Answer: C
Rationale: The text states, "Septic articular inflammation may occur primarily in the joint, or it is developed secondary due to a septic inflammation in the body elsewhere. The primary bacterial arthritis is most likely in the childhood..." A direct infection in the joint without a preceding systemic source fits the definition of primary bacterial arthritis. Main Distractor: Secondary bacterial arthritis (A) would imply an infection spreading from another site in the body, which is explicitly ruled out in the vignette.
Question 97
Arthrocentesis yields yellowish, turbid fluid from a swollen, painful knee of a 40-year-old male. The fluid is sent for microscopic analysis. Based on the description of purulent arthritis in the provided text, microscopic examination of this fluid would most likely reveal:
View Answer & Explanation
Correct Answer: D
Rationale: The text states, "The joint contains pus of yellowish color, a necrotic mass with bacteria and white blood cells." This directly describes the microscopic composition of the purulent fluid. Main Distractor: Urate crystals (A) are characteristic of gout, a crystalline arthritis, not bacterial arthritis. While both cause inflammation, the specific cellular and crystalline components differ.
Question 98
A patient with a history of recurrent bacterial arthritis in the knee now presents with persistent pain, stiffness, and crepitus. Radiographs show significant degenerative changes, including joint space narrowing and subchondral bone changes. The long-term consequence of chronic bacterial arthritis on the joint, as described in the text, is primarily:
View Answer & Explanation
Correct Answer: C
Rationale: The text explicitly describes the radiographic findings in chronic purulent arthritis as "secondary osteoarthritis... due to chronic bacterial arthritis: there are secondary osteoarthritic changes, such as subchondral sclerosis, osteophytes, subchondral cyst formation, narrowing of joint space." Main Distractor: Joint space widening (A) is incorrect; the text specifies "narrowing of joint space" as a characteristic of secondary osteoarthritis due to chronic bacterial arthritis.
Question 99
A 30-year-old male presents with sudden onset of severe pain, swelling, and warmth in his right knee. He also reports a low-grade fever and feels generally unwell. Physical examination reveals an acutely inflamed joint. Which of the following is a typical acute clinical sign of purulent arthritis, as described in the text?
View Answer & Explanation
Correct Answer: C
Rationale: The text states, "in acute form the skin is red, fever may occur." Redness of the skin is a direct clinical sign of acute inflammation in purulent arthritis. Main Distractor: Absence of pain (A) and normal range of motion (B) are contrary to the description of acute purulent arthritis, where the affected joint is painful and range of motion is significantly decreased.
Question 100
A 5-year-old boy presents with short stature, macrocephaly, and bilateral varus deformity of the knees and legs. Radiographs reveal diffuse osteosclerosis, narrow medullary cavities, and widened metaphyses. His parents report a history of easy bruising and fatigue.
View Answer & Explanation
Correct Answer: B
Rationale: The presentation in early age with severe skeletal manifestations (short stature, varus deformity, macrocephaly, diffuse osteosclerosis) and systemic symptoms like easy bruising (suggesting anemia) is characteristic of the autosomal recessive form of osteopetrosis. The autosomal dominant form typically presents later, in the second decade, and is generally more benign. The main distractor, autosomal dominant, is incorrect because its presentation is typically in the second decade and is less severe.
You Might Also Like