Full Question & Answer Text (for Search Engines)
Question 1:
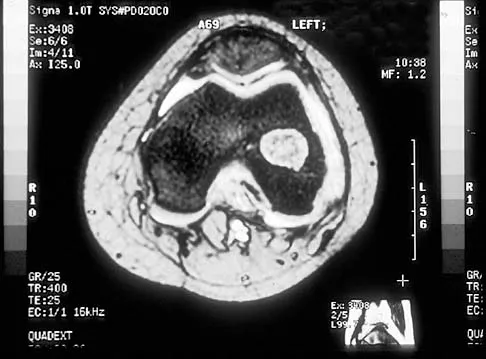
A 32-year-old male recreational tennis player presents with a 4-week history of progressive activity-related elbow pain in his dominant upper extremity. C linical examination demonstrates marked tenderness at the lateral epicondyle and pain at the lateral epicondyle with resisted wrist extension. No instability is detected on clinical examination. The next step in management is:
Options:
- Routine radiography
- Magnetic resonance imaging
- Activity modification, nonsteroidal anti-inflammatory agents, and physical therapy
- Open surgical excision of pathological tissue
- Arthroscopic surgical excision of pathological tissue
Correct Answer: Activity modification, nonsteroidal anti-inflammatory agents, and physical therapy
Explanation:
This patient has lateral epicondylitis. A recent radiographic analysis of lateral epicondylitis showed that radiographs taken at initial presentation did not alter the initial management. Most patients with lateral epicondylitis respond to nonoperative treatment. Surgical treatment should only be considered after failure of a prolonged course (at least 6 months) of nonoperative treatment.
Question 2:
During diagnostic elbow arthroscopy, which of the following nerves is at the greatest risk for injury:
Options:
- Ulnar nerve
- Median nerve
- Radial nerve
- Posterior interosseous nerve
- Anterior interosseous nerve
Correct Answer: Radial nerve
Explanation:
The radial nerve is at the greatest risk for injury during elbow arthroscopy. Injury usually occurs during creation of the anterolateral portal.
Question 3:
Which of the following elbow arthroscopic portals is correctly matched to the nerve at risk during portal creation:
Options:
- Anteromedial portal â ulnar nerve
- Anteromedial portal â radial nerve
- Posterior portal â ulnar nerve
- Anterolateral portal â median nerve
- Posterior portal â radial nerve
Correct Answer: Anteromedial portal â ulnar nerve
Explanation:
Incorrect placement of the anterolateral portal places the radial nerve at risk. Incorrect placement of the anteromedial portal places the median and ulnar nerves at risk. The posterior portal is not associated with neural injury.
Question 4:
Which of the following statements is true regarding the use of a two-incision technique vs a single-incision technique for distal biceps repair:
Options:
- The two-incision technique is associated with increased risk of neural injury, while the single-incision technique is associated with an increased risk of heterotopic ossification.
- The two-incision technique is associated with increased risk of heterotopic ossification, while the single-incision technique is associated with an increased risk of nerve injury.
- The two-incision technique is associated with increased risk of neural injury, while the risk of heterotopic ossification is the same for both procedures.
- The two-incision technique is associated with increased risk of heterotopic ossification, while the risk of nerve injury is the same for both procedures.
- The risk of nerve injury and heterotopic ossification is the same for both procedures.
Correct Answer: The two-incision technique is associated with increased risk of neural injury, while the single-incision technique is associated with an increased risk of heterotopic ossification.
Explanation:
Successful treatment of distal biceps tendon tears include dual- and single- incision techniques. The two-incision technique is associated with increased risk of heterotopic ossification, whereas the single-incision technique is associated with an increased risk of nerve injury.
Question 5:
Approximately what percentage of supination strength is lost with an unrepaired distal biceps tendon rupture:
Options:
Correct Answer: 40%
Explanation:
The biceps provides approximately 40% of supination strength to the forearm.
Question 6:
The anterior cruciate ligament is composed of which of the following bundles:
Options:
- Anterolateral, posteromedial
- Anteromedial, posterolateral
- Mediolateral, posteromedial
- Anterior, posterior
- Medial, lateral
Correct Answer: Anteromedial, posterolateral
Explanation:
The anterior cruciate ligament consists of two bundles. The anteromedial bundle is tight in flexion, and the posterolateral bundle is tight in extension.
Question 7:
The anterior cruciate ligament (AC L) provides what percent of the stability to anterior tibial translation with the knee flexed 30°:
Options:
Correct Answer: 85%
Explanation:
The AC L functions as the primary stabilizer to anterior tibial translation providing more than 85% of stability with the knee in 30° of flexion.
Question 8:
Which of the following positions of knee flexion produces the greatest strain in the anterior cruciate ligament with anterior loading of the tibia:
Options:
- 30° (Lachman test)
- 45°
- 55°
- 75°
- 90° (anterior drawer test)
Correct Answer: 30° (Lachman test)
Explanation:
Clinical and biomechanical studies show that anterior loading of the tibia in 30° of knee flexion produces greater strain and elongation of the normal anteromedial bundle than loading in 90° of knee flexion.
Question 9:
Anterior cruciate ligament (AC L) injuries are almost _______ in women than in their male counterparts in collegiate basketball players:
Options:
- Four times less common
- One and a half times more common
- Eight times more common
- Equal in prevalence
- Half as common
Correct Answer: Eight times more common
Explanation:
Female collegiate basketball players are almost eight times as likely to sustain AC L injuries as their male counterparts.
Question 10:
Which of the following is not considered an intrinsic risk factor for anterior cruciate ligament (AC L) injury:
Options:
- Narrow notch width index
- Altered neuromuscular control
- All of the above
- Increased laxity
- Male gender
Correct Answer: Male gender
Explanation:
Intrinsic risk factors for AC L injury include a narrow notch width index, a weak or small native AC L, knee joint anteroposterior laxity, malalignment of the lower extremity, pelvic position, navicular drop, and subtalar joint pronation. Male gender is not a risk factor for AC L injury.
Question 11:
Anterior cruciate ligament (AC L) injury is most commonly the result of:
Options:
- A valgus load as a result of contact
- A hyperextension as a result of contact
- A varus load as a result of contact
- A noncontact injury
- Penetrating trauma
Correct Answer: A noncontact injury
Explanation:
An AC L injury is commonly the result of a noncontact mechanism. Two common mechanisms that have been described include a valgus force to a flexed knee with the leg in external rotation and knee hyperextension with the leg internally rotated.
Question 12:
The incidence of meniscal injury with a concomitant AC L tear is reported to be nearly ____, with the _____ meniscus more commonly injured in the acute setting:
Options:
- 30%, medial
- 70%, medial
- 30%, lateral
- 50%, lateral
- 70%, lateral
Correct Answer: 70%, lateral
Explanation:
The incidence of meniscal tear after acute anterior cruciate ligament (AC L) injury is reported to be approximately 70%. The lateral meniscus is more often injured in the acute setting, and the medial meniscus is more often injured in the chronically AC L-deficient knee.
Question 13:
The healing rate of meniscal repairs in association with acute anterior cruciate ligament (AC L) reconstruction is_______ that reported for isolated meniscal repairs:
Options:
- Higher than
- Lower than
- Equal to
- Meniscal repairs are not recommended in this situation
- Unknown
Correct Answer: Higher than
Explanation:
The results with respect to healing of meniscal repairs in the association of an acute AC L injury are reported to be better than in other situations (92% vs 67%).
Question 14:
The typical locations for bone contusions as viewed on magnetic resonance imaging after anterior cruciate ligament (AC L) injury are the:
Options:
- Medial femoral condyle and medial tibial plateau
- Anterior third of the lateral femoral condyle and posterolateral tibia
- Middle third of the lateral femoral condyle and posterolateral tibia
- Posterior third of the lateral femoral condyle and posterolateral tibia
- Patellofemoral compartment
Correct Answer: Middle third of the lateral femoral condyle and posterolateral tibia
Explanation:
The typical locations for bone contusions after an AC L injury are the middle third of the lateral femoral condyle and the posterolateral tibia.
Question 15:
The sensitivity of the Lachman test is reported to be up to:
Options:
Correct Answer: 98%
Explanation:
Physical examination of the knee includes performing a Lachman test, which has a reported sensitivity of up to 98%.
Question 16:
The optimal timing for performing anterior cruciate ligament reconstruction after an acute injury is:
Options:
- Within 24 hours
- Within the first 3 weeks
- After 4 to 6 weeks
- After return of full knee range of motion
- Timing has not been shown to effect outcomes
Correct Answer: After return of full knee range of motion
Explanation:
Shelbourne noted a decrease in the incidence of postoperative stiffness to less than 1% and faster return of strength when surgery is performed after obtaining full knee range of motion including hyperextension of the knee.
Question 17:
The most common technical errors when performing anterior cruciate ligament reconstruction are:
Options:
- Excessively anterior tunnels
- Intraoperative fracture
- Iatrogenic posterior cruciate ligament injury
- Excessively posterior tunnels
- Excessively medial tunnels
Correct Answer: Excessively anterior tunnels
Explanation:
The most common technical errors involve excessively anterior placement of the tunnels. Anterior tibial tunnel and femoral tunnel placement can result in graft impingement, inability to fully extend the knee, and eventual failure. Excessively anterior femoral tunnel placement can also result in capturing the knee with difficulty in gaining full flexion and eventual stretching or rupture of the graft with attempts at gaining full flexion.
Question 18:
All of the following is used to identify the appropriate position for anterior cruciate ligament (AC L) tibial tunnel placement except:
Options:
- Inner rim of the anterior horn and lateral meniscus
- 7 mm anterior to the posterior cruciate ligament (PC L)
- Medial tibial spine
- AC L stump/footprint
- Inner rim of the anterior horn of the medial meniscus
Correct Answer: Inner rim of the anterior horn and lateral meniscus
Explanation:
Tibial tunnel misplacement can be avoided by using the appropriate landmarks (inner rim of the anterior horn of the lateral meniscus, referencing off of the PC L, the medial tibial spine, and the ACL stump).
Question 19:
Adequate bone plug length for interference screw fixation during bone- tendon-bone anterior cruciate ligament reconstruction is:
Options:
- At least 5 mm in length
- At least 10 mm in length
- At least 15 mm in length
- No less than 20 mm in length
- Bone plug length is not related to fixation strength.
Correct Answer: At least 10 mm in length
Explanation:
Graft fixation is the weak point in the early postoperative period. Researchers have reported that the optimal bone plug length is at least 1 cm. Bone plugs of shorter lengths have decreased peak load to failure, but bone plugs of greater length did not have significantly increased peak loads to failure.
Question 20:
Anterior knee pain was noted in all of the following situations except:
Options:
- Anterior cruciate ligament (AC L) reconstruction with bone-tendon-bone autograft
- AC L reconstruction with hamstrings
- After nonoperative treatment of the AC L injury
- In meniscal tears treated nonoperatively
- Following acute patellar dislocation
Correct Answer: In meniscal tears treated nonoperatively
Explanation:
Anterior knee pain was reported after patellar tendon and hamstring AC L reconstruction. Although some reports show increased pain with kneeling after patellar tendon AC L reconstruction, it is important to note the development of anterior knee pain in patients with AC L injuries treated nonoperatively. Anterior knee pain after AC L injury with or without reconstruction is not well understood and is likely multifactorial in nature.