Full Question & Answer Text (for Search Engines)
Question 1:
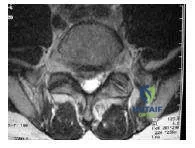
A 10-year-old girl injured her neck (Slide) after falling and hitting her head. Recommended treatment includes:
Options:
- Anterior fusion C 6-T1 with plate fixation
- Posterior fusion C 6-T1 with plate fixation
- Anterior and posterior fusion C 6-T1 with plate fixation
- Halo vest immobilization
- Cervicothoracic orthosis
Correct Answer: Cervicothoracic orthosis
Explanation:
The patient has an anterior compression fracture of C 7, which can be treated by cervicothoracic orthosis. Halo vest immobilization improves control of the head and upper cervical spine but is unnecessary treatment in this patients case. Although an anterior operation is an optional treatment for an anterior compression fracture, it is also unnecessary in this patientâ s case.
Question 2:
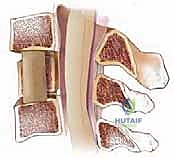
Which of the following conditions is represented in the radiograph (Slide):
Options:
- Spina bifida of the first lumbar vertebra
- Diastematomyelia
- Burst fracture
- Chance fracture
- Flexion-rotation injury
Correct Answer: Chance fracture
Explanation:
This radiograph demonstrates a chance fracture. The posterior elements of the spine are separated, as indicated by the transverse fracture of the transverse processes, pedicles, and lamina. There is no significant element of rotation of the spine.
Question 3:
A 15-year-old girl experienced an injury of L1 during a sledding accident (Slide). Her neurologic examination is normal. The best treatment is:
Options:
- Thoracolumbosacral orthosis
- Hyperextension cast
- Reduction and posterior fusion of T12-L1 with pedicle screws
- C orpectomy of T12 and anteroposterior instrumented fusion
- Reduction and posterior fusion of T12-L2 with pedicle screws
Correct Answer: Reduction and posterior fusion of T12-L1 with pedicle screws
Explanation:
This patient has a C hance fracture of L1, which is indicated by the compression of the anterior portion of L1 and the distraction of the posterior portion of L1. A hyperextension cast will not treat the patientâ s C hance fracture completely. Operative treatment is needed to remove residual kyphosis at the thoracolumbar junction. Posterior column compression will also likely reduce the presence of residual kyphosis. Posterior fusion of T12- L2 with pedicle screws results in the best angular correction for a patient with a C hance fracture of L1. T12-L1 with hooks is an optional treatment for patients with a C hance fracture of L1 because residual kyphosis may persist even if the inferior lamina of L1 is intact.
Question 4:
Which of the following conditions is represented in this radiograph (Slide) of a childs neck:
Options:
- Osteoid osteoma of C 1
- Jeffersonâ s fracture
- Rotatory subluxation
- Hangman fracture
- Os odontoideum
Correct Answer: Rotatory subluxation
Explanation:
This radiograph indicates a rotatory subluxation of a childâ s neck. Alteration of the cortical ring of the anterior atlas is present and superimposed on the lateral mass of atlas. Increased distance between the anterior atlas and axis is the result of rotation.
Question 5:
Which of the following conditions is represented by this computed tomography scan of a cervical spine (Slide):
Options:
- Jeffersonâ s fracture
- Osteoid osteoma
- Odontoid fracture
- Rotatory subluxation
- Chiaris malformation
Correct Answer: Rotatory subluxation
Explanation:
Partial superimposition of C1 on C2 is present in this radiograph. C2 is the portion in the center of the frame. C1 and C 2 would normally be on different cuts of a scan but are superimposed because the atlas overlaps the axis as it falls forward. If an imaginary line is drawn between the vertebral foramena of C 1 and across the body of C 2, an angle will form representing the degree of malrotation, which is approximately 30°.
Question 6:
Which of the following conditions is not commonly associated with C hance fractures in children:
Options:
- Renal trauma
- Intestinal contusion
- Dural tear
- Neurologic injury
- Multilevel spine trauma
Correct Answer: Multilevel spine trauma
Explanation:
Chance fractures in children are often associated with blunt contusions to abdominal structures. Blunt contusions to abdominal structures cause renal and intestinal trauma and distraction of the spinal cord and may be associated with dural tearing or neurologic injury. Neurologic injuries occur in fewer than half of children with Chance fractures that have blunt contusions to abdominal structures. Although spinal fractures caused by falls or axial loads can result in multilevel spinal injuries, multilevel spinal injuries do not commonly result from Chance fractures.
Question 7:
The lesion indicated in this computed tomography (Slide) most likely represents:
Options:
- Brodieâ s abscess
- Eosinophilic granuloma
- Osteosarcoma
- Osteoid osteoma
- Osteoma
Correct Answer: Osteoid osteoma
Explanation:
This patient has an osteoid osteoma with pain in the lumbar spine where the lesion is located. The patientâ s osteoid osteoma shows hot on a photon emission computed tomography scan and is relieved by nonsteroidal anti- inflammatory agents. Most patients with osteoid osteoma with lesions have them in the posterior region of their vertebrae.
Question 8:
Which of the following conditions is represented by this radiograph (Slide) of an infantâ s elbow:
Options:
- Salter I fracture of distal humerus
- Elbow dislocation
- Type 2 Monteggiaâ s fracture dislocation
- Septic elbow
- Proximal radioulnar synostosis
Correct Answer: Proximal radioulnar synostosis
Explanation:
This patient has a proximal radioulnar synostosis. Patients with proximal radioulnar synostosis often have dysplasia of the proximal ulna, maldirection of the proximal radius, and cortical continuity of the ulna and radius.
Question 9:
Which of the following conditions is represented by this radiograph (Slide):
Options:
- Developmental dysplasia of the hip
- Juvenile rheumatoid arthritis
- Hemophilic arthropathy
- Legg-Calv-Perthes disease
- Rickets
Correct Answer: Developmental dysplasia of the hip
Explanation:
This patient has early fragmentation, epiphyseal flattening, metaphyseal lucency and widening, and sclerosis typical of patients with Legg-C alvé- Perthes disease in the early stages. In patients with juvenile rheumatoid arthritis, osteopenia and joint space narrowing are present, whereas in patients with developmental dysplasia, the acetabulum is shallow. C orrect Answer: Legg-Calv-Perthes disease
Question 10:
Which of the following designations best describes this radiograph (Slide):
Options:
- Herring antibody
- Herring body
- Stulberg 4
- C atterall 1
- 30% epiphyseal extrusion
Correct Answer: Herring body
Explanation:
This patient has Herring body involvement of the hip. As a result, this patient has less than a 50% loss of lateral column height and is in the early fragmentation phase. This patient has a Catterall involvement of at least 3. The Stulberg classification is used to rate a patientâ s hip after it has healed.
Question 11:
In which stage of Legg-Calva-Perthes disease is this patient:
Options:
- Initial
- Fragmentation
- Reossification
- Healed
- Degenerative
Correct Answer: Fragmentation
Explanation:
This patient is in the end of the fragmentation phase of Legg-Calv-Perthes disease. Note the extreme flattening of the head and the lateral fragmentation.
Question 12:
All of the following conditions are indicated by this radiograph (Slide) of a patient with Legg- Calv-Perthes disease except:
Options:
- Coxa magna
- Coxa brevis
- Trochanteric overgowth
- Coxa vara
- Coxa plana
Correct Answer: Coxa vara
Explanation:
The hip of this patient with Legg-C alvé-Perthes disease has undergone epiphyseal flattening and premature (primarily lateral) physeal arrest. The femoral head has regrown with an enlarged width. The radiograph shows elements of coxa magna, coxa brevis, trochanteric overgrowth, and coxa plana. Coxa vara is not present.
Question 13:
A 5-year-old girl is evaluated for Legg-Calva-Perthes disease. She is in the fragmentation phase, and rotation is 10° internal and 15° external. Her epiphyseal extrusion index is 15%. Recommended treatment includes:
Options:
- Femoral osteotomy
- Iliac osteotomy
- Traction
- Shelf procedure
- Observation
Correct Answer: Observation
Explanation:
The patients restricted range of motion is normal for a patient in the fragmentation phase of Legg-Calva-Perthe disease. The patiens degree of epiphyseal extrusion is not extreme. Observation is the most appropriate course of treatment.
Question 14:
What is the risk of hip arthroplasty for 50-year-old patients with Legg-C alva-Perthes disease:
Options:
Correct Answer: 50%
Explanation:
Long-term study has shown that 50% of 50-year-old patients with Legg-C alva-Perthes disease will have degenerative changes in their hips significant enough to make them candidates for hip arthroplasty.
Question 15:
Which of the following descriptions reflects all transverse-plane factors affecting the position of the patientâ s foot during gait:
Options:
- Thigh-foot angle
- Transmalleolar axis
- Foot progression angle
- Heel bisector
- Femoral anteversion
Correct Answer: Foot progression angle
Explanation:
The foot-progression angle is a reflection of all transverse-plane factors affecting the position of the patientâ s foot during gait.
Question 16:
In which of the following conditions is a Trendelenburgâ s gait unlikely to occur:
Options:
- L4 myelomningocele
- Legg-Calva-Perthes disease
- Untreated developmental dysplasia of the hip
- Polio- L5
- Osgood-Schlatter disease
Correct Answer: Osgood-Schlatter disease
Explanation:
Patients with complications that cause pain around their hips or that decrease the abductor strength of their hips may develop a Trendelenburgs gait.
Question 17:
In which muscle does Elys test detect spasticity or contracture:
Options:
- Biceps femoris
- Rectus femoris
- Gastrocnemius
- Soleus
- Semimembranosus
Correct Answer: Rectus femoris
Explanation:
Elys test is performed while the patient is prone and his or her hip is at maximal extension. Elys test is positive if flexion of the patients knee causes the patientâ s hip to flex. A positive Elys test indicates spasticity or contracture of the rectus femoris.
Question 18:
Stahelis test is designed to detect hip flexion contracture. Which of the following tests also detects hip flexion contracture:
Options:
- Silfvers test
- Oberâ s test
- Thomas test
- Jacks test
- Trendelenburgâ s test
Correct Answer: Thomas test
Explanation:
Staheliâ s test and the Thomas test are designed to detect hip flexion contracture. Staheliâ s test is performed with a patient in the prone position. The lumbar lordosis is eliminated by flexing a patientâ s hips, and then gradually extending the affected hip. The Thomas test is performed with a patient in the supine position. The lumbar lordosis is minimized by flexing a patientâ s hips forward, allowing the affected hip to go into extension.
Question 19:
Which of the following conditions has the highest rate of bilaterality:
Options:
- Slipped capital femoral epiphysis
- Legg-C alvé-Perthes disease
- Developmental dysplasia of the hip
- Discoid lateral meniscus
- Fibular hemimelia
Correct Answer: Slipped capital femoral epiphysis
Explanation:
Slipped capital femoral epiphysis has a bilaterality rate of 25% to 40%. Legg-Calva-Perthes disease, developmental dysplasia of the hip, discoid lateral meniscus, and fibular hemimelia have bilateral rates of less than 20%.
Question 20:
In which pattern does the most common presentation of Trevorâ s disease occur:
Options:
- Generalized involvement of all extremities
- Distal medial areas of one lower extremity
- Proximal lateral areas of both lower extremities
- Distal medial areas of both upper extremities
- Proximal lateral areas of one upper extremity
Correct Answer: Distal medial areas of one lower extremity
Explanation:
Trevors disease, also known as dysplasia epiphysialis hemimelia, refers to epiphyseal osteochondromas. Epiphyseal osteochondromas are usually few in number and are more common on the distal and medial portions of the epiphysis of one lower extremity.

 The patient has an anterior compression fracture of C 7, which can be treated by cervicothoracic orthosis. Halo vest immobilization improves control of the head and upper cervical spine but is unnecessary treatment in this patients case. Although an anterior operation is an optional treatment for an anterior compression fracture, it is also unnecessary in this patientâ s case.
The patient has an anterior compression fracture of C 7, which can be treated by cervicothoracic orthosis. Halo vest immobilization improves control of the head and upper cervical spine but is unnecessary treatment in this patients case. Although an anterior operation is an optional treatment for an anterior compression fracture, it is also unnecessary in this patientâ s case.