Orthopedic Board Review MCQs: Ankle & Foot | Part 94
Key Takeaway
This page presents Part 94 of a comprehensive OITE & ABOS Orthopedic Surgery Board Review series. It features 50 high-yield multiple-choice questions designed for orthopedic residents and surgeons preparing for board certification exams. Utilize interactive study and exam modes to enhance your exam readiness.
Orthopedic Board Review MCQs: Ankle & Foot | Part 94
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
A 32-year-old male is involved in a motor vehicle collision and sustains a talar neck fracture. Radiographs show a displaced talar neck fracture with subluxation of the subtalar joint, but the ankle joint remains reduced. What is the expected rate of avascular necrosis (AVN) of the talar body for this specific injury pattern, and which blood supply is most commonly disrupted first?
Explanation
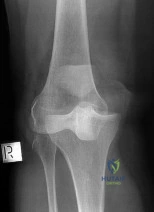
Question 2
A 24-year-old football player presents with midfoot pain after a plant-and-twist injury. Weight-bearing radiographs demonstrate widening of the space between the medial and middle cuneiforms. A pure ligamentous Lisfranc injury is suspected. Which of the following best describes the normal anatomy of the Lisfranc ligament?
Explanation
Question 3
A 50-year-old woman complains of a painful bunion. Radiographs reveal a hallux valgus angle (HVA) of 35 degrees, an intermetatarsal angle (IMA) of 16 degrees, and a distal metatarsal articular angle (DMAA) of 20 degrees. Clinical examination demonstrates hypermobility of the first tarsometatarsal (TMT) joint. Which of the following procedures is most appropriate to provide lasting correction?
Explanation
Question 4
A 55-year-old overweight woman complains of medial ankle pain and flattening of her arch over the past year. She is unable to perform a single-limb heel rise on the affected side. Weight-bearing radiographs show a flexible flatfoot deformity with normal joint spaces and no subtalar arthritis. What is the most appropriate surgical intervention if conservative management fails?
Explanation
Question 5
A 16-year-old boy presents with progressive bilateral foot deformities and frequent ankle sprains. Examination reveals a cavovarus foot posture, depressed first ray, and a positive Coleman block test. Neurologic exam reveals decreased sensation in the distal lower extremities and diminished reflexes. Which muscle's relative preservation and overpowering of its weak antagonist primarily drives the plantarflexion of the first ray?
Explanation
Question 6
A 42-year-old weekend warrior feels a 'pop' in his posterior ankle while playing tennis. He has a positive Thompson test. Non-operative management is chosen. Which of the following rehabilitation protocols has been shown in high-quality randomized controlled trials to yield re-rupture rates comparable to surgical management?
Explanation
Question 7
A 45-year-old roofer falls from a height and sustains a closed, displaced intra-articular calcaneus fracture. CT scan reveals a Sanders Type III fracture. He is a heavy smoker (2 packs per day). What is the most appropriate definitive management considering his social history?
Explanation
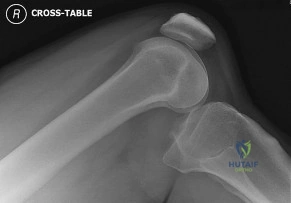
Question 8
A 26-year-old hockey player sustains an external rotation injury to his right ankle. Radiographs show a fibular fracture 5 cm above the joint line and widening of the medial clear space. After ORIF of the fibula, the syndesmosis remains unstable. Which of the following is true regarding syndesmotic fixation?
Explanation
Question 9
A 28-year-old female presents with chronic ankle pain and catching after a severe inversion ankle sprain 1 year ago. MRI demonstrates a 1.2 cm x 1.0 cm osteochondral lesion on the posteromedial talar dome with intact overlying cartilage. After failure of conservative management, what is the most appropriate next step in treatment?
Explanation
Question 10
A 45-year-old man presents with burning pain and tingling in the plantar aspect of his right foot, which worsens with prolonged standing and at night. Tinel's sign is positive over the medial ankle, posterior to the medial malleolus. EMG/NCS confirms compression of the posterior tibial nerve. Which of the following structures forms the roof of the tarsal tunnel?
Explanation
Question 11
A 21-year-old collegiate wide receiver hyperextends his great toe during a game on artificial turf. He has significant pain, swelling, and ecchymosis at the first MTP joint, and is unable to push off. MRI reveals a complete tear of the plantar plate and capsuloligamentous complex with proximal retraction of the sesamoids. What is the most appropriate management?
Explanation
Question 12
A 15-year-old female dancer complains of pain in her forefoot, specifically over the second metatarsal head. Radiographs show flattening, sclerosis, and fragmentation of the second metatarsal head. Which of the following conservative treatments is most appropriate initially?
Explanation
Question 13
A 24-year-old skier presents with lateral ankle pain and a snapping sensation over the lateral malleolus after a fall where his ankle was forcibly dorsiflexed. Physical exam reveals apprehension and a palpable pop over the lateral malleolus with resisted dorsiflexion and eversion. Which structure is most likely injured?
Explanation
Question 14
A 30-year-old male sustains a twisting injury to his foot. Radiographs demonstrate a transverse fracture of the fifth metatarsal at the metaphyseal-diaphyseal junction, extending into the intermetatarsal articulation (between the 4th and 5th metatarsals). What anatomical feature puts this specific area at high risk for nonunion?
Explanation
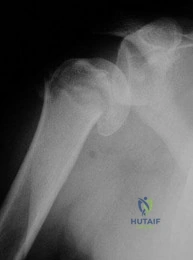
Question 15
A 65-year-old man with post-traumatic end-stage ankle osteoarthritis is evaluated for a total ankle arthroplasty (TAA). He has an active lifestyle but does not participate in high-impact sports. Which of the following is considered an absolute contraindication to TAA?
Explanation
Question 16
A 22-year-old track athlete presents with an insidious onset of vague dorsal midfoot pain that worsens with sprinting. Examination reveals localized tenderness over the 'N-spot'. Radiographs are negative. MRI confirms a non-displaced stress fracture in the central third of the tarsal navicular. What is the recommended initial treatment?
Explanation
Question 17
A 60-year-old woman with longstanding, poorly controlled rheumatoid arthritis presents with a severe forefoot deformity characterized by hallux valgus and dorsal subluxation of the lesser MTP joints with painful plantar callosities. Which of the following surgical strategies is considered the classic and most reliable procedure for this severe rheumatoid forefoot deformity?
Explanation
Question 18
A 12-year-old boy presents with frequent ankle sprains and a rigid, painful flatfoot. Clinical examination shows a lack of subtalar motion and peroneal spasticity. Oblique radiographs of the foot demonstrate an osseous bridge between the anterior process of the calcaneus and the navicular. Which of the following is the most appropriate initial operative management if conservative measures have failed?
Explanation
Question 19
A 40-year-old construction worker falls from a ladder and sustains a high-energy, comminuted distal tibia intra-articular fracture (AO/OTA 43-C3) with severe soft tissue swelling, fracture blisters, and shortening. What is the standard of care for the initial management of this injury?
Explanation
Question 20
A 55-year-old man presents with chronic, severe posterior heel pain. Examination reveals a prominent Haglund's deformity and tenderness at the Achilles tendon insertion. Radiographs show a large calcaneal spur within the tendon insertion. He has failed physical therapy and NSAIDs over the past 12 months. Surgery is planned. If more than 50% of the Achilles tendon insertion must be detached to resect the calcification and exostosis, what additional procedure is most strongly recommended?
Explanation
Question 21
During open repair of an acute Achilles tendon rupture, care must be taken to repair the paratenon. What is the primary function of the paratenon in this region?
Explanation
Question 22
A 62-year-old male presents with dorsal foot pain and limited dorsiflexion of the first metatarsophalangeal (MTP) joint. Radiographs show a dorsal osteophyte with more than 50% joint space narrowing, but the plantar half of the joint space is relatively preserved (Coughlin and Shurnas Grade 2). He has failed conservative management. What is the most appropriate surgical intervention?
Explanation
Question 23
A 55-year-old female presents with progressive flattening of her left foot, medial pain, and inability to perform a single heel raise. Examination reveals hindfoot valgus that is passively correctable and forefoot abduction. In addition to posterior tibial tendon insufficiency, tearing of which of the following structures is most highly associated with the development of the forefoot abduction seen in this stage?
Explanation
Question 24
A 30-year-old male sustains a high-energy injury to his foot and is diagnosed with a Hawkins type III talar neck fracture. Which of the following best describes this injury and its associated risk of avascular necrosis (AVN)?
Explanation
Question 25
The Lisfranc ligament is critical for midfoot stability. Which of the following accurately describes the anatomic attachments of the Lisfranc ligament?
Explanation
Question 26
A 40-year-old roofer falls 15 feet, sustaining a displaced, intra-articular calcaneus fracture (Sanders Type II). He is planned for open reduction and internal fixation via an extensile lateral approach. To minimize the risk of wound complications, which of the following principles must be adhered to during the approach?
Explanation
Question 27
A 60-year-old patient with poorly controlled diabetes mellitus presents with a red, hot, swollen foot. Radiographs demonstrate periarticular fragmentation, subluxation, and bony debris around the midfoot. According to the Eichenholtz classification, what stage of Charcot arthropathy is this, and what is the most appropriate initial treatment?
Explanation
Question 28
During evaluation of an external rotation ankle injury, disruption of the distal tibiofibular syndesmosis is suspected. Which of the following ligaments provides the greatest resistance to lateral translation of the fibula relative to the tibia?
Explanation
Question 29
A 22-year-old collegiate basketball player sustains a fracture of the proximal fifth metatarsal. Radiographs show a transverse fracture at the metaphyseal-diaphyseal junction without distal extension beyond the fourth-fifth intermetatarsal articulation. What is the primary anatomic reason this specific fracture is at high risk for nonunion?

Explanation
Question 30
A 14-year-old boy presents with frequent ankle sprains and rigid flatfeet. On examination, he has decreased subtalar motion and peroneal spasticity. Radiographs demonstrate the 'C-sign' on the lateral view. Which type of tarsal coalition does this finding most strongly suggest?
Explanation
Question 31
Chronic plantar fasciitis often involves degenerative changes rather than purely inflammatory ones. The pathologic changes are most commonly located at the origin of which of the following structures?
Explanation
Question 32
A 45-year-old woman is being evaluated for hallux valgus surgery. Her weight-bearing AP foot radiograph reveals a Hallux Valgus Angle (HVA) of 35 degrees and an Intermetatarsal Angle (IMA) of 16 degrees. The metatarsophalangeal joint is subluxated but reducible. Which of the following surgical procedures is most appropriate?
Explanation
Question 33
A 50-year-old woman complains of burning pain in her forefoot that radiates into her toes, typically worsening when wearing tight shoes. Compressing the metatarsal heads together while applying plantar pressure to the interspace elicits a palpable click and reproduces her pain. What is this clinical test called?
Explanation
Question 34
A 65-year-old man presents with a 'slapping' foot gait and weakness in ankle dorsiflexion following a stumble. He denies significant pain but notes a mass over the anterior ankle. On examination, he has weak active dorsiflexion, but can still extend his toes. Which of the following is true regarding this condition?
Explanation
Question 35
An acute dislocation of the peroneal tendons usually involves forced dorsiflexion of the everted foot with strong reflex contraction of the peroneal muscles. Which structure is primarily injured or avulsed in this mechanism?
Explanation
Question 36
A 45-year-old male sustains a high-energy, closed tibial pilon fracture. The soft tissues are significantly swollen with fracture blisters present. What is the currently recommended protocol for managing this injury to minimize soft tissue complications?

Explanation
Question 37
A football player injures his great toe on artificial turf during a forced hyperextension mechanism. He has severe pain and swelling at the first MTP joint. 'Turf toe' represents an injury to which of the following structures?
Explanation
Question 38
A 20-year-old track athlete presents with insidious onset, vague midfoot pain that worsens with sprinting. A CT scan confirms a nondisplaced stress fracture in the central third of the tarsal navicular. What is the most appropriate initial management?
Explanation
Question 39
Based on classic literature, which of the following best describes the typical location, morphology, and etiology of osteochondral lesions of the talus?
Explanation
Question 40
A 60-year-old female with severe, long-standing rheumatoid arthritis presents with debilitating forefoot pain. She has severe hallux valgus, lesser toe clawing, and dorsal dislocation of the lesser MTP joints. The metatarsal heads are prominent on the plantar aspect. What is the gold-standard surgical procedure for this severe rheumatoid forefoot deformity?
Explanation
Question 41
A 55-year-old female presents with a progressively collapsing arch and medial ankle pain. Examination reveals a positive 'too many toes' sign and the inability to perform a single-leg heel rise. Radiographs demonstrate a talonavicular uncoverage angle of 35 degrees and >40% uncovering of the talonavicular joint. What is the most appropriate surgical management for this stage of adult acquired flatfoot deformity?
Explanation
Question 42
A 52-year-old male with poorly controlled diabetes presents with a swollen, erythematous, and warm left foot without a history of trauma. Pedal pulses are bounding. Radiographs demonstrate fragmentation of the tarsometatarsal joints with bone debris and early subluxation. What is the most appropriate initial step in management?
Explanation
Question 43
A 16-year-old male presents with bilateral progressive cavovarus foot deformities. A Coleman block test normalizes hindfoot alignment. Neurological examination reveals depressed deep tendon reflexes. The pathogenesis of this deformity in Charcot-Marie-Tooth disease is primarily driven by which of the following muscle imbalances?
Explanation
Question 44
A 22-year-old elite track athlete develops focal midfoot pain over the dorsal 'N spot'. A CT scan confirms a non-displaced stress fracture of the central third of the tarsal navicular. The high risk of nonunion in this specific anatomic location is secondary to a vascular watershed zone formed between which two arteries?
Explanation
Question 45
A 52-year-old female presents with progressive medial ankle pain and a severe flatfoot deformity. Clinical examination demonstrates a positive single-leg heel rise test on the affected side but she can perform a double-leg heel rise. Weight-bearing radiographs reveal >30% uncovering of the talonavicular joint and a talonavicular angle of 25 degrees. The hindfoot deformity is flexible. Which of the following surgical strategies is most appropriate for this stage of deformity?
Explanation
Question 46
A 14-year-old boy presents with recurrent ankle sprains and rigid flatfeet. A lateral weight-bearing radiograph demonstrates a prominent 'C-sign' and a talar beak.
Based on the most likely diagnosis, which specific anatomical structure is most commonly involved in this pathology?

Explanation
Question 47
A 68-year-old male is considering surgical intervention for end-stage ankle osteoarthritis. He has a history of well-controlled diabetes and hypertension. Which of the following conditions is considered an absolute contraindication for a primary total ankle arthroplasty (TAA)?
Explanation
Question 48
Based on recent Level I evidence comparing operative and non-operative management of acute Achilles tendon ruptures using early functional rehabilitation protocols, which of the following statements is most accurate?
Explanation
Question 49
A 45-year-old male sustains a displaced intra-articular calcaneus fracture.
The surgeon decides to proceed with an extensile lateral approach. To minimize the risk of apical tip necrosis of the lateral soft tissue flap, the surgeon must preserve the primary blood supply to this angiosome. Which artery is responsible for this blood supply?

Explanation
Question 50
A 26-year-old female presents with progressive bilateral cavovarus foot deformity. A Coleman block test is performed. When her heel and lateral column are placed on the block while the first metatarsal is allowed to plantarflex freely, the hindfoot varus corrects to a neutral position. What is the primary initial step in the surgical reconstruction of this deformity?
Explanation
Question 51
A 19-year-old collegiate basketball player sustains a Zone 2 fracture of the proximal fifth metatarsal (Jones fracture). Why do these specific fractures have a disproportionately high rate of delayed union and nonunion?
Explanation
Question 52
When performing a minimally invasive repair for an acute Achilles tendon rupture, the sural nerve is at highest risk of iatrogenic injury. At what approximate distance proximal to the calcaneal tuberosity insertion does the sural nerve cross the lateral border of the Achilles tendon?
Explanation
Question 53
A 55-year-old diabetic patient presents with a swollen, erythematous, and warm unilateral foot without systemic signs of infection. Radiographs show periarticular fragmentation, subluxation, and bony debris around the midfoot. According to the Eichenholtz classification, what is the most appropriate initial management?
Explanation
Question 54
A 62-year-old female presents with flatfoot deformity. Examination reveals a flexible hindfoot valgus, but she is unable to perform a single-leg heel raise. Radiographs demonstrate significant forefoot abduction with a talonavicular uncoverage angle of 40 degrees. Which surgical intervention is most appropriate?
Explanation
Question 55
A 22-year-old track athlete presents with insidious onset of vague dorsal midfoot pain. Examination reveals focal tenderness at the "N-spot". CT scan confirms an incomplete stress fracture in the central third of the tarsal navicular. What anatomic factor primarily contributes to the high risk of nonunion in this specific region?
Explanation
Question 56
When utilizing the extensile lateral approach for open reduction and internal fixation of a displaced intra-articular calcaneus fracture, preserving the blood supply to the lateral soft tissue flap is critical. Which artery provides the primary vascular supply to the apex of this flap?
Explanation
Question 57
A 28-year-old male presents with persistent anterolateral ankle pain 1 year after an ankle sprain. MRI demonstrates an osteochondral lesion of the talus (OCL) measuring 1.8 cm x 1.6 cm without massive subchondral cyst formation. He has failed non-operative management. What is the most appropriate surgical treatment?
Explanation
Question 58
A 25-year-old professional basketball player sustains an acute fracture at the metaphyseal-diaphyseal junction of the fifth metatarsal. To facilitate the fastest and safest return to elite-level play, what is the recommended treatment?
Explanation
Question 59
A patient with Charcot-Marie-Tooth disease presents with a symptomatic cavovarus foot. A Coleman block test is performed, and the hindfoot varus corrects to a neutral alignment when the first metatarsal is allowed to plantarflex off the block. What does this indicate, and what surgical step is essential?
Explanation
Question 60
A 21-year-old collegiate football player sustains a severe hyperextension injury to his first metatarsophalangeal (MTP) joint. MRI confirms a complete disruption of the plantar plate complex with proximal retraction of the sesamoids. What is the most appropriate management?
Explanation
Question 61
A 14-year-old female dancer presents with pain and swelling over the second metatarsophalangeal joint. Radiographs show flattening, sclerosis, and early fragmentation of the second metatarsal head. What is the primary underlying pathophysiology of this condition?
Explanation
Question 62
A 65-year-old male with severe post-traumatic ankle osteoarthritis is evaluated for a total ankle arthroplasty (TAA). Which of the following conditions is generally considered an absolute contraindication for a primary TAA?
Explanation
Question 63
A 30-year-old male falls from a ladder and sustains an isolated lateral subtalar dislocation. Closed reduction in the emergency department under conscious sedation is unsuccessful. What anatomical structure is most likely blocking the reduction?
Explanation
None
