OITE & ABOS Orthopedic Board Prep: Adult Reconstruction, Extremities & Deformity MCQs Part 90
Key Takeaway
This page offers Part 90 of a comprehensive board review for orthopedic surgeons and residents. It contains 100 high-yield, verified MCQs mirroring OITE and AAOS exam formats, focusing on key topics like Arthroplasty. Use study or exam modes for effective preparation and certification.
OITE & ABOS Orthopedic Board Prep: Adult Reconstruction, Extremities & Deformity MCQs Part 90
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
A 65-year-old male presents with groin pain 5 years after a primary metal-on-polyethylene total hip arthroplasty. Laboratory analysis shows elevated serum cobalt levels and normal chromium levels. Hip aspiration is negative for infection. What is the most likely source of the elevated metal ions?
Explanation
Question 2
During a total knee arthroplasty, which of the following component malpositions is most likely to result in lateral patellar tracking and potential subluxation?
Explanation
Question 3
According to consensus criteria, which of the following is the most appropriate indication for debridement, antibiotics, and implant retention (DAIR) in a patient with a periprosthetic joint infection following TKA?
Explanation
Question 4
A 45-year-old active male presents with medial compartment osteoarthritis of the knee and 8 degrees of varus alignment. A medial opening wedge high tibial osteotomy (HTO) is planned. To maintain the native posterior tibial slope during the osteotomy, the surgeon should:
Explanation
Question 5
In reverse total shoulder arthroplasty, placing the glenosphere with an inferior tilt rather than neutral or superior tilt achieves which of the following biomechanical advantages?

Explanation
Question 6
A 55-year-old woman undergoes a primary THA using a ceramic-on-ceramic bearing. Two years later, she complains of an audible squeaking sound from her hip during walking, without associated pain. Radiographs show well-fixed components. Which of the following is most strongly associated with the development of squeaking in ceramic-on-ceramic THA?
Explanation
Question 7
During a cruciate-retaining TKA, the surgeon notes that the knee is well balanced in extension but is tight in flexion, demonstrating restricted flexion and anterior liftoff of the tibial trial tray. Which of the following is the most appropriate next step to balance the knee?
Explanation
Question 8
A 72-year-old female presents after a fall with a spiral fracture around her cementless THA stem. The stem has subsided 1.5 cm compared to previous radiographs. Bone stock is deemed adequate. According to the Vancouver classification, what is the most appropriate management?
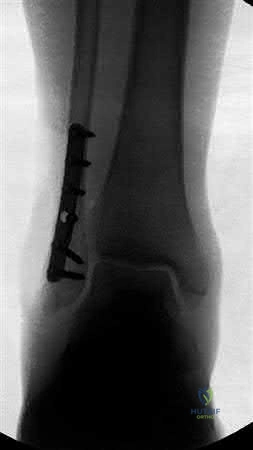
Explanation
Question 9
In a revision total hip arthroplasty for a patient with massive acetabular bone loss, what radiographic finding best differentiates a pelvic discontinuity from a severe but continuous defect?
Explanation
Question 10
To optimize stability and minimize impingement in THA, the concept of combined anteversion is often utilized. If the acetabular cup is placed in 15 degrees of anteversion, what is the ideal target for femoral stem anteversion to achieve a standard combined anteversion of 35-40 degrees?
Explanation
Question 11
A 68-year-old man who underwent primary TKA 4 years ago presents with an inability to actively extend his knee following a fall. Clinical exam reveals a palpable gap at the superior pole of the patella. What is the most reliable surgical option for reconstruction of this chronic extensor mechanism disruption?
Explanation
Question 12
A patient is scheduled for a TKA. Radiographs show a healed midshaft femur fracture with a 15-degree coronal plane varus deformity. If an intra-articular bone resection is performed strictly perpendicular to the mechanical axis of the femur to correct alignment, what is the most likely consequence?
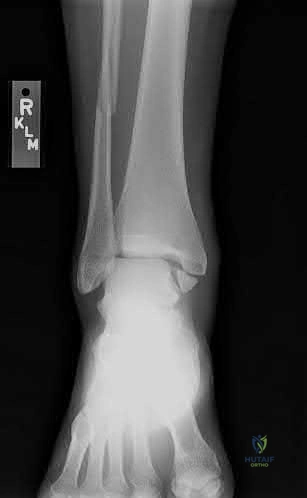
Explanation
Question 13
During a direct anterior approach for total hip arthroplasty, the superficial internervous plane utilized is between muscles innervated by which of the following nerves?
Explanation
Question 14
A 58-year-old woman presents with persistent, unexplained pain and swelling in her knee 2 years after a primary TKA. Joint aspiration is negative for infection. A synovial biopsy demonstrates a perivascular lymphocytic infiltrate with macrophages containing metal wear debris. Which of the following is the most likely diagnosis?
Explanation
Question 15
Which of the following is an absolute indication for using a rotating-hinge prosthesis rather than a constrained condylar knee (CCK) during a revision TKA?
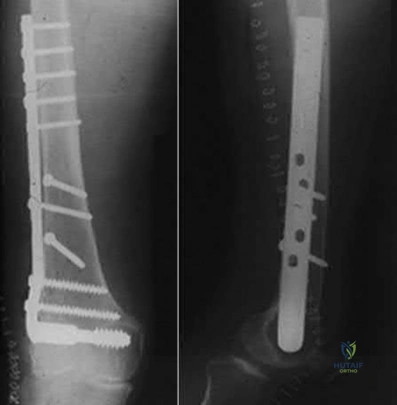
Explanation
Question 16
A 65-year-old male with a B2 glenoid (posterior wear, retroversion of 20 degrees) is undergoing anatomic total shoulder arthroplasty. What is the maximum amount of retroversion correction that should be attempted with eccentric anterior reaming alone before unacceptably compromising glenoid vault bone stock?
Explanation
Question 17
Metal-on-metal hip resurfacing is considered as an alternative to THA in select young, active patients. Which of the following is a recognized absolute contraindication for this procedure?
Explanation
Question 18
A 70-year-old female with long-standing ankylosing spondylitis and a completely fused lumbar spine is undergoing a primary THA. How does her lack of spino-pelvic mobility dictate the optimal intraoperative positioning of her acetabular component to prevent dislocation?
Explanation
Question 19
A patient develops severe true patella baja following a previous high tibial osteotomy and now requires a TKA. During the procedure, the patella cannot be safely everted. What is the most appropriate surgical maneuver to improve exposure and prevent patellar tendon avulsion?

Explanation
Question 20
In the native knee, femoral rollback (the posterior translation of the contact point of the femur on the tibia during flexion) is primarily driven by the tension of which of the following ligaments?
Explanation
Question 21
A patient undergoes primary total knee arthroplasty. During trialing, the knee is perfectly balanced and stable in extension, but it is unacceptably tight in flexion. Which of the following is the most appropriate surgical step to achieve a balanced gap without altering extension?
Explanation
Question 22
Which of the following surgical factors is most strongly associated with the postoperative complication of 'squeaking' in a ceramic-on-ceramic total hip arthroplasty?
Explanation
Question 23
A 62-year-old male presents with new-onset cardiomyopathy, peripheral neuropathy, and visual field changes 6 years after a revision total hip arthroplasty. Aspiration of the hip yields clear fluid with a low white blood cell count. Which of the following implant configurations is most likely responsible for his systemic symptoms?
Explanation
Question 24
According to classic and contemporary criteria, which of the following is considered an absolute contraindication to a medial unicompartmental knee arthroplasty (UKA)?
Explanation
Question 25
A 68-year-old female presents with a painful catching sensation and an audible 'clunk' at 35 degrees of flexion as she extends her knee actively. She underwent a primary posterior-stabilized TKA 14 months ago. What is the underlying pathomechanics of this condition?
Explanation
Question 26
During a medial opening wedge high tibial osteotomy (HTO), the surgeon inadvertently distracts the anterior aspect of the osteotomy gap significantly more than the posterior aspect. What biomechanical consequence will this have on the knee?
Explanation
Question 27
A 55-year-old male undergoes a primary THA via a direct anterior approach. Postoperatively, he notes a burning pain and numbness isolated to the anterolateral aspect of his operative thigh. Strength is fully intact. Injury to which nerve is the most likely cause?
Explanation
Question 28
According to the 2018 International Consensus Meeting (ICM) criteria, which of the following findings is sufficient on its own to confirm the diagnosis of a periprosthetic joint infection?
Explanation
Question 29
A 70-year-old female undergoes TKA for a severe, rigid 20-degree valgus deformity. In the recovery room, she is unable to dorsiflex her ankle or extend her toes, and has numbness in the first web space of her foot. What is the most appropriate initial management step?
Explanation
Question 30
A 76-year-old female presents with a third episode of posterior dislocation following a primary THA. Radiographs show well-fixed, correctly positioned components. Intraoperatively, her abductor musculature is found to be completely avulsed, retracted, and irreparable. Which of the following is the most appropriate definitive management?
Explanation
Question 31
During a primary total knee arthroplasty, the trial components are placed, and the knee is found to be stable in full extension but tight in 90 degrees of flexion. Which of the following modifications is the most appropriate surgical step to balance the knee?
Explanation
Question 32
A 72-year-old female sustains a periprosthetic femur fracture around a cementless THA.
Radiographs show a fracture at the level of the stem tip with evidence of stem subsidence, though the surrounding diaphyseal cortical thickness is well-preserved (>3 mm). What is the standard of care for this patient?

Explanation
Question 33
A 55-year-old male is undergoing a total knee arthroplasty 10 years after a medial opening wedge high tibial osteotomy (HTO). What specific anatomic alterations are most likely present that will complicate the arthroplasty?
Explanation
Question 34
A 65-year-old male with long-standing ankylosing spondylitis and a fully fused lumbar spine in a flattened (loss of lordosis) position requires a THA. How should the acetabular component position be adjusted to minimize the risk of posterior dislocation?
Explanation
Question 35
A 62-year-old male with long-standing ankylosing spondylitis is planned for a primary total hip arthroplasty (THA). Radiographs show a completely fused lumbar spine to the sacrum. How does this spinopelvic stiffness affect optimal acetabular cup positioning compared to a patient with normal spinopelvic mobility?
Explanation
Question 36
During a primary total knee arthroplasty (TKA) for a severe varus deformity, the medial compartment remains significantly tight in both flexion and extension after appropriate bone cuts and thorough osteophyte removal. Which of the following is the most appropriate next step in soft tissue release?
Explanation
Question 37
A 68-year-old female presents with progressive groin pain 6 years after a metal-on-polyethylene THA utilizing a modular titanium stem and cobalt-chrome head. Aspiration yields fluid with 2,500 WBC/uL (80% lymphocytes) and negative cultures. Serum cobalt is markedly elevated. What is the most appropriate definitive management?
Explanation
Question 38
Which of the following best describes the primary objective of caliper-measured kinematic alignment in total knee arthroplasty?
Explanation
Question 39
A 45-year-old active male underwent a primary THA. Two years postoperatively, he complains of an audible squeaking noise with walking and bending, but denies pain. Radiographs show well-fixed, well-positioned components. Which bearing surface combination is most classically associated with this complication?
Explanation
Question 40
A 65-year-old female complains of a painful catch and pop in her knee when extending from a flexed position, one year after a posterior-stabilized TKA. What is the most likely etiology of this classic symptom?
Explanation
Question 41
When correcting a complex multi-planar lower extremity deformity using a hexapod circular external fixator, what mathematically defines the origin from which all spatial corrections are generated by the software?
Explanation
Question 42
A 72-year-old female sustains a periprosthetic femur fracture around a cemented polished taper stem. Radiographs reveal a comminuted fracture around the tip of the stem. The stem is loose, and there is severe proximal femoral bone loss preventing adequate diaphyseal fixation. How is this classified and most appropriately managed?
Explanation
Question 43
Historically, catastrophic subsurface oxidation and subsequent delamination of total knee arthroplasty polyethylene inserts were most strongly associated with which of the following manufacturing processes?
Explanation
Question 44
A 70-year-old male presents with inability to actively extend his knee 3 years following a primary TKA. Examination reveals a palpable gap at the patellar tendon. What is the most reliable reconstructive option for this chronic, massive disruption?
Explanation
Question 45
Which of the following surgical modifications most significantly decreases the risk of postoperative dislocation in primary total hip arthroplasty?
Explanation
Question 46
In a 6-year-old child with late-onset infantile Blount's disease, radiographs show a severe depression of the medial tibial plateau and a medial physeal bar. What is the most appropriate surgical management?
Explanation
Question 47
During preoperative templating for a total hip arthroplasty, the surgeon notes a 15 mm functional leg length discrepancy (affected side short) and a 10 mm anatomic true leg length discrepancy (affected side short). To avoid symptomatic over-lengthening postoperatively, the surgeon should aim to restore:
Explanation
Question 48
A 60-year-old female scheduled for primary TKA reports a severe blistering skin reaction to inexpensive jewelry. Patch testing confirms a severe nickel allergy. Which of the following femoral component materials is most appropriate to prevent a hypersensitivity reaction?
Explanation
Question 49
A 74-year-old female presents for revision THA. Radiographs demonstrate an inferiorly migrated acetabular component, a transverse radiolucent line across the posterior column, and an ilioischial line break. Intraoperatively, the superior and inferior hemi-pelves move independently. Which of the following is the most appropriate reconstructive technique?
Explanation
Question 50
When planning a corrective osteotomy for a diaphyseal angular deformity, placing the osteotomy and the hinge exactly at the Center of Rotation of Angulation (CORA) will mathematically result in:
Explanation
Question 51
A 68-year-old female presents with recurrent episodes of anterior hip dislocation following a primary total hip arthroplasty. Her dislocations typically occur when she extends and externally rotates her hip while walking. Which of the following component malpositions is the most likely cause of this specific instability pattern?
Explanation
None
