Orthopedic Board Review MCQs: Knee, Foot & Ankle | Part 86
Key Takeaway
This page offers Part 86 of a comprehensive OITE & AAOS Orthopedic Board Review MCQ bank. Designed for orthopedic residents and surgeons, it features 50 high-yield multiple-choice questions with detailed explanations, clinical scenarios, and two learning modes (study/exam) to help you excel in board certification exams.
Orthopedic Board Review MCQs: Knee, Foot & Ankle | Part 86
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
A 22-year-old female presents with recurrent patellar instability. You plan a medial patellofemoral ligament (MPFL) reconstruction. Intraoperatively, fluoroscopy is used to determine the exact femoral tunnel position. According to Schöttle's criteria, which of the following radiographic landmarks best describes the correct anatomical femoral attachment of the MPFL on a true lateral radiograph?
Explanation
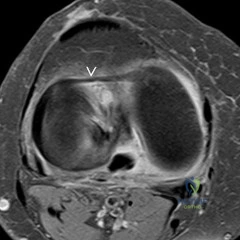
Question 2
A 65-year-old female undergoes primary total knee arthroplasty (TKA) for severe fixed valgus osteoarthritis. During trial reduction, the knee is found to be excessively tight in both flexion and extension on the lateral side. According to the sequential lateral release technique, which specific lateral structure is primarily responsible for balancing the knee in BOTH flexion and extension?
Explanation
Question 3
A 55-year-old woman presents with a progressive flatfoot deformity. Examination reveals a flexible pes planovalgus, an inability to perform a single-leg heel rise, and > 40% uncovering of the talonavicular joint on weight-bearing AP radiographs. What is the most appropriate surgical management for this Stage IIb adult-acquired flatfoot?
Explanation
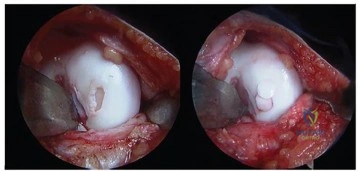
Question 4
A 14-year-old boy sustains an ankle injury while playing soccer. Radiographs reveal a Salter-Harris III fracture of the anterolateral distal tibia. Which ligament's avulsion force is fundamentally responsible for this specific fracture pattern?
Explanation
Question 5
A 25-year-old male presents with a posterolateral corner (PLC) knee injury. During anatomical reconstruction, the surgeon must aim to recreate the primary static stabilizers to restore normal kinematics. What are the three primary static stabilizers of the PLC?
Explanation
Question 6
When evaluating and treating a suspected Lisfranc injury, an understanding of the local anatomy is critical. Which of the following statements regarding the Lisfranc ligament complex is true?
Explanation
Question 7
A 45-year-old avid runner presents with severe posterior heel pain. MRI demonstrates a thickened Achilles tendon with marked intrasubstance degeneration 4 cm proximal to its insertion. There is no Haglund deformity. Six months of eccentric stretching and physical therapy have failed. Which of the following is the most appropriate surgical treatment?
Explanation
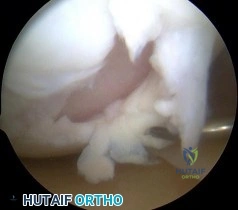
Question 8
A 58-year-old patient with long-standing poorly controlled diabetes presents with a swollen, erythematous, and warm foot. Radiographs demonstrate periarticular fragmentation, subluxation of the tarsometatarsal joints, and bony debris, but no signs of consolidation, fusion, or sclerosis. According to the Eichenholtz classification, what stage of Charcot arthropathy is this, and what is the current standard of care?
Explanation
Question 9
An opening wedge high tibial osteotomy (HTO) is planned for a 45-year-old male laborer with isolated medial compartment osteoarthritis and varus malalignment. What is a common unintended consequence on the sagittal plane biomechanics of the knee if the osteotomy gap is opened equally anteriorly and posteriorly?
Explanation
Question 10
A 50-year-old female presents with an acute onset of medial knee pain after a deep squat. MRI reveals a complete radial tear adjacent to the medial meniscus posterior root attachment. What are the biomechanical consequences of this specific injury if left untreated?
Explanation
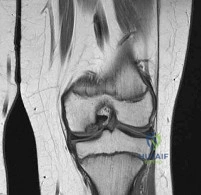
Question 11
A 28-year-old male presents with a progressive cavovarus foot deformity secondary to Charcot-Marie-Tooth disease. A Coleman block test is performed during the clinical examination, and the hindfoot completely corrects to a neutral/valgus position. What does this specific finding imply regarding the nature of the deformity?
Explanation
Question 12
A 26-year-old athlete reports persistent anterolateral ankle pain after sustaining a severe sprain 6 months ago. MRI identifies a 12 mm x 10 mm osteochondral lesion of the anterolateral talar dome. The overlying cartilage is visually intact with no detachment. After a failed 3-month course of conservative management, which of the following is the most appropriate initial surgical intervention?
Explanation
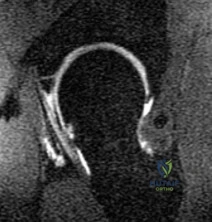
Question 13
During an anterior cruciate ligament (ACL) reconstruction, the surgeon inadvertently places the femoral tunnel too anteriorly (i.e., too 'shallow' or high in the notch on a lateral radiograph) on the lateral femoral condyle. Which of the following kinematic complications will reliably occur as a result of this error?
Explanation
Question 14
A 22-year-old competitive skier presents with lateral ankle pain and an audible 'snapping' sensation behind the lateral malleolus during forced dorsiflexion and eversion. Clinical examination is notable for visible subluxation of the peroneal tendons over the fibula. Which primary anatomical restraint is most likely incompetent in this condition?
Explanation
Question 15
A 34-year-old male sustains a severe knee dislocation (Schenck KD III-M, involving ACL, PCL, and MCL) following a high-speed motorcycle crash. His limb is well-perfused, ABIs are 1.1, and compartment pressures are normal. Assuming no absolute contraindications, what is the most appropriate timing and approach for definitive surgical reconstruction?
Explanation
Question 16
A professional American football player presents with acute, severe pain at the first metatarsophalangeal (MTP) joint after a forced hyperextension injury of the hallux while being tackled. MRI reveals a complete tear of the plantar plate and capsuloligamentous complex with proximal retraction of the sesamoids. What is the grade of this injury, and what is the recommended management for this high-level athlete?
Explanation
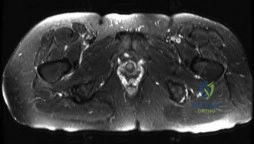
Question 17
Tarsal navicular stress fractures are notoriously difficult to heal and carry a high risk of delayed union or nonunion. This complication is primarily attributed to a watershed zone of relative avascularity located in which specific anatomic portion of the navicular bone?
Explanation
Question 18
A 24-year-old track athlete complains of severe calf cramping, numbness, and paresthesias that reliably occur after 15 minutes of running and resolve rapidly after 10 minutes of rest. Resting and post-exertional compartment pressure testing is within normal limits. Her resting ankle-brachial index (ABI) is normal, but it drops significantly when she performs active, forceful plantarflexion. What is the most likely pathophysiological mechanism of her condition?
Explanation
Question 19
In the surgical management of chronic, neglected Achilles tendon ruptures with a massive gap defect (> 6 cm), a flexor hallucis longus (FHL) tendon transfer is frequently the procedure of choice. What is the primary anatomical advantage of utilizing the FHL tendon over the flexor digitorum longus (FDL) or peroneus brevis for this specific reconstruction?
Explanation
Question 20
Following open reduction and internal fixation of a Weber C fibula fracture, the surgeon intraoperatively evaluates the integrity of the distal tibiofibular syndesmosis. Which of the following radiographic parameters on a standard non-rotated AP and mortise radiograph is considered the most reliable indicator of a well-reduced syndesmosis?
Explanation
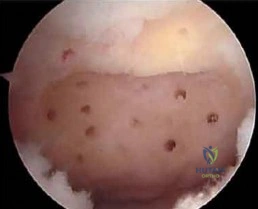
Question 21
A 26-year-old athlete undergoes posterior cruciate ligament (PCL) reconstruction. The surgeon aims to reconstruct the anterolateral (AL) bundle of the PCL. At what knee position is this specific bundle typically the tightest and evaluated for optimal tension during graft fixation?
Explanation
Question 22
A 34-year-old female presents with a progressive cavovarus foot deformity. On examination, a Coleman block test is performed by placing her heel and lateral border of the foot on a block while allowing the first metatarsal to hang free. The hindfoot varus completely corrects. Which of the following is the most appropriate surgical intervention for her deformity?
Explanation
Question 23
During a primary total knee arthroplasty for a severe varus deformity, trial components are placed. The knee is found to be well-balanced in extension but excessively tight medially in flexion. Which of the following medial structures should be released to specifically address the tight medial flexion gap?
Explanation
Question 24
A 22-year-old collegiate basketball player sustains a fracture at the diaphyseal junction of the proximal fifth metatarsal. Radiographs show a transverse fracture line without sclerosis (Zone 3). To minimize the risk of nonunion and allow early return to play, what is the treatment of choice?
Explanation
Question 25
A 28-year-old male sustains a multiligamentous knee injury. On examination, a dial test is performed. There is 15 degrees of increased external rotation at 30 degrees of knee flexion compared to the contralateral side. At 90 degrees of knee flexion, the external rotation is symmetric bilaterally. What injury pattern does this indicate?
Explanation
Question 26
A 55-year-old diabetic patient presents with a warm, swollen, and erythematous left foot and ankle. Radiographs reveal fragmentation, periarticular debris, and joint subluxation at the midfoot. According to the Eichenholtz classification, what stage of Charcot arthropathy is this, and what is the initial management?
Explanation
Question 27
Regarding the anatomy of the anterior cruciate ligament (ACL), which of the following statements correctly describes the biomechanical role of its two distinct bundles?
Explanation
Question 28
A 40-year-old patient underwent open reduction and internal fixation (ORIF) with syndesmotic screw fixation for an unstable ankle fracture. Postoperatively, malreduction of the syndesmosis is suspected. Which imaging modality and specific anatomical relationship provide the most accurate assessment of syndesmotic reduction?
Explanation
Question 29
A surgeon is performing a medial opening wedge high tibial osteotomy (HTO) to treat medial compartment osteoarthritis in a varus knee. To avoid unintentionally increasing the posterior tibial slope (creating a "flexion osteotomy"), what must the ratio of the anterior osteotomy gap to the posterior osteotomy gap approximately be?
Explanation
Question 30
A 45-year-old male presents with dorsal midfoot pain. Examination reveals pain with terminal hallux dorsiflexion but no pain in the mid-range of motion. Radiographs show a dorsal osteophyte on the 1st metatarsal head with relative preservation of the joint space. What is the most appropriate surgical treatment if non-operative management fails?
Explanation
Question 31
A 45-year-old female experiences a sudden "pop" in the back of her knee while ascending stairs, followed by mild effusion and posteromedial pain. MRI reveals a posterior root tear of the medial meniscus with 3 mm of meniscal extrusion. What is the most significant biomechanical consequence of leaving this tear untreated?
Explanation
Question 32
When comparing operative vs. non-operative management (using a functional rehabilitation protocol) for acute Achilles tendon ruptures, high-level evidence demonstrates which of the following regarding complication rates?
Explanation
Question 33
Which of the following component malpositions in a primary total knee arthroplasty (TKA) is most likely to result in lateral patellar subluxation or tracking issues?
Explanation
Question 34
A 30-year-old male falls from a height and sustains a Hawkins Type III talar neck fracture.
What best describes the displacement pattern and the approximate risk of avascular necrosis (AVN) of the talar body?

Explanation
Question 35
A 25-year-old football player sustains a purely ligamentous Lisfranc injury.
Recent prospective randomized trials comparing open reduction internal fixation (ORIF) with primary arthrodesis for this specific injury pattern show which of the following advantages for primary arthrodesis?

Explanation
Question 36
A 12-year-old boy presents with vague knee pain and catching. Radiographs reveal an osteochondritis dissecans (OCD) lesion. What is the most common anatomical location for this lesion in the knee?
Explanation
Question 37
In the pathogenesis of adult-acquired flatfoot deformity (posterior tibial tendon dysfunction), failure of static stabilizers occurs sequentially. Which ligamentous structure is considered the primary static stabilizer of the talonavicular joint and is typically the first to fail?
Explanation
Question 38
A 24-year-old male presents to the emergency department after a high-energy trauma with a grossly dislocated knee (Schenck KD-III). The knee is reduced in the ED. Pulses are palpable, but the Ankle-Brachial Index (ABI) is 0.85. What is the next most appropriate step in management?
Explanation
Question 39
The deltoid ligament complex is crucial for medial ankle stability. Which component of the deltoid ligament is the primary restraint to lateral displacement (talar shift) and external rotation of the talus within the ankle mortise?
Explanation
Question 40
During arthroscopy for an acute anterior cruciate ligament (ACL) rupture, the surgeon evaluates the posterior horn of the medial meniscus. A longitudinal tear at the meniscocapsular junction is identified, which was not visible from the standard anterior portals until the arthroscope was advanced through the intercondylar notch. What is the specific term for this type of lesion?
Explanation
Question 41
A 68-year-old male presents with a feeling of instability 6 months after a primary total knee arthroplasty. Examination reveals the knee is stable in full extension but has 15 degrees of varus/valgus laxity at 90 degrees of flexion. Which of the following technical errors most likely caused this specific instability pattern?
Explanation
Question 42
A 52-year-old female presents with acute medial knee pain after a deep squat. MRI reveals a complete posterior horn medial meniscus root tear with 4 mm of meniscal extrusion. Biomechanically, this injury is most equivalent to which of the following?
Explanation
Question 43
A 34-year-old male sustains a Hawkins Type III talar neck fracture following a motor vehicle collision. At 8 weeks post-ORIF, an AP radiograph of the ankle demonstrates a subchondral radiolucent band in the talar dome. What does this radiographic finding indicate?
Explanation
Question 44
During surgical fixation of a severe acute Lisfranc injury, the surgeon must restore the primary structural stabilizer of the tarsometatarsal articulation. Between which two bones does the true Lisfranc ligament travel?
Explanation
Question 45
A 24-year-old football player sustains a contact knee injury. On examination, the dial test demonstrates 20 degrees of increased external rotation at 30 degrees of knee flexion compared to the contralateral side, but symmetric external rotation at 90 degrees of flexion. Which structure is most likely injured?
Explanation
Question 46
A 28-year-old male undergoes open reduction and internal fixation for a Weber C ankle fracture with syndesmotic disruption. Which of the following intraoperative fluoroscopic parameters is the most reliable indicator of accurate syndesmotic reduction?
Explanation
Question 47
A 70-year-old female complains of an audible and painful "pop" in her knee when rising from a chair, 14 months after a posterior-stabilized total knee arthroplasty (TKA). Examination reveals a palpable catch at roughly 40 degrees of flexion as the knee extends. What is the most likely etiology?
Explanation
Question 48
A 48-year-old female presents with a painful bunion. Weight-bearing radiographs reveal a hallux valgus angle (HVA) of 45 degrees, an intermetatarsal angle (IMA) of 18 degrees, and evidence of hypermobility at the first tarsometatarsal (TMT) joint.
Which surgical intervention is most appropriate?

Explanation
Question 49
A 68-year-old male presents with instability when descending stairs one year after a primary posterior-stabilized total knee arthroplasty (TKA). Clinical examination and stress radiographs demonstrate a well-balanced knee in full extension, but significant laxity is noted at 90 degrees of flexion. Which of the following intraoperative component adjustments would have best prevented this specific complication?
Explanation
Question 50
During open reduction and internal fixation of a severe supination-external rotation ankle fracture, you note widening of the syndesmosis on the Cotton test. You decide to place a syndesmotic position screw. Which of the following ligaments provides the greatest resistance to diastasis of the distal tibiofibular syndesmosis?
Explanation
Question 51
A 45-year-old female presents with a painful bunion. Weight-bearing radiographs reveal a Hallux Valgus Angle (HVA) of 42 degrees and an Intermetatarsal Angle (IMA) of 18 degrees. There is no evidence of first tarsometatarsal hypermobility or midfoot arthritis. What is the most appropriate surgical intervention?
Explanation
Question 52
A 24-year-old soccer player undergoes anterior cruciate ligament (ACL) reconstruction. Postoperatively, the patient complains of the knee 'giving way' when pivoting. Examination reveals a firm endpoint on the Lachman test but a positive pivot shift test. What is the most likely technical error made during the surgery?
Explanation
Question 53
A 30-year-old male sustains a purely ligamentous Lisfranc injury after falling from a horse. The first, second, and third tarsometatarsal (TMT) joints are diastased. Which of the following surgical treatments yields the best long-term functional outcome for this specific injury pattern?
Explanation
Question 54
A 52-year-old female experiences a sudden pop in the back of her knee while squatting. MRI demonstrates an extrusion of the medial meniscus by 4 mm and a radial tear at the posterior root attachment. What is the recommended surgical management to halt the progression of rapidly advancing osteoarthritis?
Explanation
Question 55
A 58-year-old male with poorly controlled type 2 diabetes mellitus presents with a swollen, erythematous, and warm right foot without any open ulcers. Plain radiographs are normal. MRI shows diffuse marrow edema in the midfoot. What is the most appropriate initial management?
Explanation
Question 56
A 21-year-old collegiate basketball player sustains an acute transverse fracture at the metaphyseal-diaphyseal junction of the fifth metatarsal (Zone 2) during a game. To minimize the risk of nonunion and expedite his return to play, what is the treatment of choice?
Explanation
Question 57
A 65-year-old female presents with a painful catching sensation in her anterior knee when moving from flexion to extension, exactly 14 months after undergoing a posterior-stabilized total knee arthroplasty (PS-TKA). What is the most likely etiology of her symptoms?
Explanation
Question 58
When performing a minimally invasive surgical repair of an acute Achilles tendon rupture, care must be taken to avoid injury to the sural nerve. At approximately what distance proximal to the calcaneal insertion does the sural nerve typically cross the lateral border of the Achilles tendon?
Explanation
Question 59
During a knee examination of a trauma patient, the dial test demonstrates 15 degrees of increased external rotation at 30 degrees of knee flexion compared to the contralateral side. However, at 90 degrees of knee flexion, the external rotation is symmetric bilaterally. Which structure is injured?
Explanation
Question 60
A 14-year-old male presents with poorly localized knee pain and intermittent mechanical symptoms. Radiographs reveal an osteochondritis dissecans (OCD) lesion. What is the most common anatomical location for this lesion in the knee?
Explanation
Question 61
A 32-year-old male falls from a height and sustains a Hawkins Type III fracture of the talar neck. What is the approximate rate of avascular necrosis (AVN) of the talar body associated with this specific injury pattern?
Explanation
Question 62
You are performing a medial opening wedge high tibial osteotomy (HTO) on a 40-year-old active male with medial compartment osteoarthritis and varus malalignment. To optimize load distribution and long-term survivorship of the osteotomy, where should the postoperative mechanical axis pass on the tibial plateau (measured from medial to lateral)?
Explanation
Question 63
A 45-year-old runner complains of burning heel pain that radiates into the medial arch of the foot. Examination reveals a positive Tinel's sign posterior to the medial malleolus, and dorsiflexion-eversion exacerbates the symptoms. Which nerve is entrapped in this condition?
Explanation
Question 64
A 35-year-old roofer sustains a severe axial load injury to his heel. Lateral radiographs demonstrate a depressed intra-articular calcaneus fracture. In a normal, uninjured foot, what is the expected range for Böhler's angle?
Explanation
Question 65
During a total knee arthroplasty (TKA), the surgeon inadvertently places both the femoral and tibial components in internal rotation. What is the most likely resulting complication?
Explanation
Question 66
A professional football player suffers a severe hyperdorsiflexion injury to his great toe. MRI shows a complete tear of the plantar plate with proximal retraction of the sesamoids. What grade of 'Turf Toe' is this, and what is the primary indication for surgical intervention in this specific case?
Explanation
Question 67
A 25-year-old male sustains an anterior knee dislocation after a motorcycle accident. The knee is reduced in the emergency department. The patient has palpable, symmetric 2+ dorsalis pedis and posterior tibial pulses. However, the ankle-brachial index (ABI) is measured at 0.85. What is the most appropriate next step in management?
Explanation
Question 68
A 28-year-old skier presents with acute pain behind the lateral malleolus after catching his edge. He reports a snapping sensation on the lateral side of his ankle when dorsiflexing and everting his foot against resistance. Disruption of which anatomical structure is primarily responsible for his symptoms?
Explanation
Question 69
During a posterior stabilized total knee arthroplasty, the surgeon performs a posterior capsular release. The popliteal artery is at highest risk of injury in this region. At the level of the tibial cut, what is the anatomical relationship of the popliteal artery to the posterior capsule and popliteal vein?
Explanation
Question 70
A 24-year-old athlete sustains a hyperplantarflexion injury to the midfoot. Non-weight-bearing radiographs are normal, but weight-bearing views show a 3 mm diastasis between the base of the first and second metatarsals with no fractures. What is the most appropriate management?
Explanation
Question 71
When performing an anterior cruciate ligament (ACL) reconstruction, placing the femoral tunnel using a traditional transtibial technique rather than an independent anteromedial portal technique most commonly results in a tunnel that is:
Explanation
Question 72
A 45-year-old female presents with a painful bunion. Weight-bearing radiographs reveal a hallux valgus angle of 42 degrees, an intermetatarsal angle of 18 degrees, and clinical hypermobility of the first tarsometatarsal joint. Which of the following procedures is most appropriate?
Explanation
Question 73
During a primary cruciate-retaining total knee arthroplasty, the trial reduction reveals that the knee is symmetric and balanced in extension but excessively tight in flexion. Which of the following is the most appropriate intraoperative adjustment?
Explanation
Question 74
A 35-year-old recreational athlete sustains an acute Achilles tendon rupture. He elects for non-operative management utilizing an early functional rehabilitation protocol. Compared to operative management, this non-operative approach is most closely associated with:
Explanation
Question 75
The posterior cruciate ligament (PCL) consists of two main bundles. Which of the following best describes the biomechanical behavior of the anterolateral (AL) bundle?
Explanation
Question 76
A 58-year-old male with poorly controlled diabetes presents with a swollen, warm, and erythematous right foot. Radiographs demonstrate early fragmentation of the midfoot with subluxation and bony debris. According to the Eichenholtz classification, what is the current stage and most appropriate management?
Explanation
Question 77
A 12-year-old male presents with vague knee pain. Radiographs show an osteochondritis dissecans (OCD) lesion on the lateral aspect of the medial femoral condyle. MRI confirms a 1.5 cm lesion with no fluid behind it. The physes are widely open. What is the most appropriate initial management?
Explanation
None
