Orthopedic Board Prep MCQs: Shoulder, Elbow, Arthroplasty & Trauma Part 84
Key Takeaway
This interactive quiz, Part 84, provides 50 high-yield MCQs for OITE & AAOS Orthopedic Board Review. Designed for orthopedic residents and surgeons, it offers practice with clinical scenarios in study or exam modes, complete with detailed explanations. Ideal for board exam preparation.
Orthopedic Board Prep MCQs: Shoulder, Elbow, Arthroplasty & Trauma Part 84
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
In reverse total shoulder arthroplasty, moving the center of rotation medially and inferiorly alters the biomechanics of the deltoid. Which of the following best describes this effect?
Explanation
Question 2
A 45-year-old male sustains a terrible triad injury to the elbow. During surgical management, which of the following sequences of repair provides the most biomechanically sound restoration of stability?
Explanation
Question 3
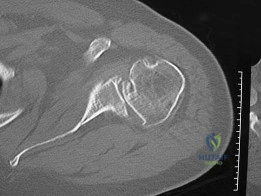
In the evaluation of a proximal humerus fracture, which of the following radiographic findings is the most reliable predictor of subsequent avascular necrosis of the humeral head?
Explanation

Question 4
A 62-year-old man presents with vague shoulder pain 18 months after a total shoulder arthroplasty. Inflammatory markers (ESR, CRP) are normal. Aspiration yields no growth at 3 days. What is the optimal approach to diagnose a suspected Cutibacterium acnes (C. acnes) infection?
Explanation
Question 5
During an anatomic coracoclavicular (CC) ligament reconstruction for a chronic Type V AC joint separation, the surgeon aims to reconstruct both the conoid and trapezoid ligaments. To accurately replicate their anatomic insertions on the clavicle, where should the tunnels be placed relative to the distal end of the clavicle?
Explanation
Question 6
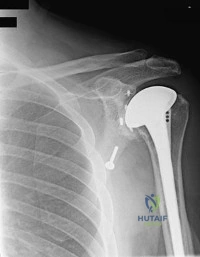
A 78-year-old female with severe rheumatoid arthritis sustains a comminuted intra-articular distal humerus fracture (OTA type 13-C3). Which of the following is an established advantage of performing a total elbow arthroplasty (TEA) compared to open reduction and internal fixation (ORIF) in this specific patient population?
Explanation
Question 7
Which of the following component positioning strategies is most effective at reducing the incidence of scapular notching in reverse total shoulder arthroplasty?
Explanation
Question 8
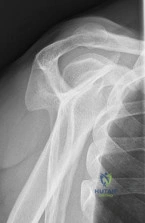
A 25-year-old competitive cyclist sustains a Type IIB distal clavicle fracture (Neer classification). Which of the following best describes the pathomechanics and optimal treatment of this injury?
Explanation
Question 9
A patient presents with a history of recurrent elbow clicking and a sense of instability when pushing up from a chair. A lateral pivot-shift test of the elbow is positive. This condition is primarily caused by insufficiency of which of the following structures?
Explanation
Question 10
A 65-year-old female is scheduled for a total shoulder arthroplasty for primary osteoarthritis. Preoperative CT reveals a Walch B2 glenoid. What does a B2 glenoid signify, and what is a common surgical strategy for addressing it in anatomic TSA?
Explanation
Question 11
A 72-year-old male presents with inability to actively elevate his right arm past 45 degrees, despite having full passive range of motion. MRI demonstrates a massive, retracted tear of the supraspinatus and infraspinatus with Goutallier grade 4 fatty infiltration. The subscapularis and teres minor are intact. What is the most appropriate definitive surgical intervention?
Explanation

Question 12
When performing a two-incision repair for a distal biceps tendon rupture (modified Morrey approach), which of the following nerves is at the greatest risk of injury during the creation of the posterior bone tunnel in the radial tuberosity?
Explanation
Question 13
A 32-year-old male sustains a closed, spiral fracture of the distal third of the humerus (Holstein-Lewis fracture). On examination in the emergency department, he is noted to have a dense radial nerve palsy. What is the most appropriate initial management?
Explanation
Question 14
A 24-year-old rugby player undergoes a Latarjet procedure for recurrent anterior shoulder instability with 25% glenoid bone loss. Which of the following is the most frequent long-term complication associated with this procedure?
Explanation

Question 15
In the management of extra-articular scapular body and neck fractures, which of the following is generally accepted as an absolute indication for open reduction and internal fixation (ORIF)?
Explanation
Question 16
A 35-year-old female falls on an outstretched hand and sustains a shear fracture of the capitellum that includes a large portion of the trochlea (McKee modification of Bryan and Morrey Type 4). Which of the following surgical approaches provides the most optimal exposure for fixation of this specific fracture pattern?
Explanation
Question 17
Which of the following intraoperative techniques is most strongly recommended to minimize the risk of postoperative ulnar neuropathy during a total elbow arthroplasty for a patient with rheumatoid arthritis?
Explanation
Question 18
A 70-year-old female presents with sudden, sharp shoulder pain 6 months after an uncomplicated reverse total shoulder arthroplasty (rTSA). Radiographs reveal a new stress fracture of the acromion base (Levy Type II). What biomechanical factor of the rTSA construct most significantly contributed to this complication?
Explanation
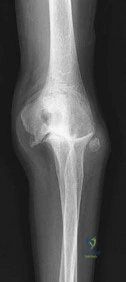
Question 19
A 28-year-old male develops severe elbow stiffness 3 months following open reduction and internal fixation of a terrible triad injury. Radiographs show mature heterotopic ossification (HO) bridging the radioulnar joint. He is scheduled for excision of the HO and capsular release. What is the optimal postoperative prophylaxis to prevent recurrence of HO in this patient?
Explanation
Question 20
When performing open reduction and internal fixation (ORIF) of a valgus-impacted 4-part proximal humerus fracture, which structural element is critical to maintain or repair to prevent postoperative varus collapse?
Explanation
Question 21
In a patient undergoing total elbow arthroplasty for a severely comminuted, osteoporotic distal humerus fracture, what is the most common early postoperative nerve-related complication?
Explanation
Question 22
To minimize the risk of scapular notching in reverse total shoulder arthroplasty (RTSA), how should the glenosphere baseplate optimally be positioned?
Explanation
Question 23
A 40-year-old male presents with a severely comminuted, non-reconstructable radial head fracture after a fall from a height. He also complains of severe ipsilateral wrist pain. Radiographs reveal a shortened radius and disruption of the distal radioulnar joint (Essex-Lopresti injury). What is the most appropriate management?
Explanation
Question 24
In the surgical management of a 'terrible triad' injury of the elbow (elbow dislocation, radial head fracture, coronoid fracture), what is the recommended order of reconstruction to methodically restore joint stability?
Explanation
Question 25
Which of the following radiographic findings in a proximal humerus fracture is the strongest predictor for the development of avascular necrosis (AVN) of the humeral head according to the Hertel criteria?

Explanation
Question 26
A 25-year-old cyclist sustains a midshaft clavicle fracture. Which of the following is considered an absolute indication for operative fixation?
Explanation
Question 27
Operative management of a scapular body and neck fracture is typically indicated if the glenoid medialization exceeds which of the following thresholds?
Explanation
Question 28
A 32-year-old bodybuilder feels a pop in his anterior axilla while performing a heavy bench press. Examination reveals loss of the anterior axillary fold and weakness with internal rotation. MRI confirms a rupture of the pectoralis major tendon at its insertion. What is the anatomic insertion site of the pectoralis major?
Explanation
Question 29
A 65-year-old female sustains a comminuted fracture of the olecranon extending distal to the coronoid process. What is the most appropriate fixation construct?
Explanation
Question 30
According to the Hamada classification for rotator cuff arthropathy, a shoulder radiograph showing acetabularization of the coracoacromial arch and femoralization of the humeral head without glenohumeral arthritis is classified as:

Explanation
Question 31
An 18-year-old athlete undergoes arthroscopic anterior stabilization for recurrent anterior shoulder instability. Intraoperatively, he is found to have an 'off-track' engaging Hill-Sachs lesion. Which of the following procedures should be added to the Bankart repair?
Explanation
Question 32
A patient develops severe heterotopic ossification (HO) following a distal humerus fracture, resulting in profound elbow stiffness. What is the most appropriate timing for surgical excision of the HO?
Explanation
Question 33
A 45-year-old male feels a pop in his elbow while lifting a heavy box. On examination, the examiner's finger cannot hook beneath the tendon in the antecubital fossa from the lateral side. What structure is evaluated by this 'hook test'?

Explanation
Question 34
A 20-year-old male is involved in a high-speed MVA and sustains a posterior sternoclavicular joint dislocation. He is hemodynamically stable but complains of dysphagia and mild dyspnea. A closed reduction is planned in the operating room. Which surgical specialty must be immediately available during this procedure?
Explanation
Question 35
A 35-year-old male sustains a closed, spiral fracture of the distal third of the humeral shaft (Holstein-Lewis fracture). He presents with an isolated radial nerve palsy noted immediately after the injury. What is the most appropriate initial management?
Explanation
Question 36
A 'floating shoulder' is typically defined as a double disruption of the superior shoulder suspensory complex (SSSC). Which of the following injury combinations classically constitutes a floating shoulder?
Explanation
Question 37
When treating an intra-articular distal humerus fracture, an olecranon osteotomy approach provides excellent visualization of the articular surface. Which of the following osteotomies is preferred to facilitate subsequent reduction and promote reliable bone healing?
Explanation
Question 38
In anatomic total shoulder arthroplasty for primary osteoarthritis, a biconcave glenoid with significant posterior wear (Walch B2) is encountered. Failure to correct this excessive retroversion during glenoid component placement strongly increases the risk of which complication?
Explanation
Question 39
Posterolateral rotatory instability (PLRI) of the elbow, which classically presents with a positive pivot-shift test and apprehension when pushing up from a chair, is primarily caused by a deficiency of which ligamentous structure?
Explanation
Question 40
A 30-year-old female sustains a shear fracture of the capitellum extending into the trochlea. During open reduction and internal fixation via a lateral approach, the surgeon decides to use the Kocher approach to visualize the capitellum while minimizing risk to the LUCL. The Kocher approach utilizes the internervous plane between which two muscles?
Explanation
Question 41
In reverse total shoulder arthroplasty, which of the following baseplate and glenosphere configurations is most effective in preventing scapular notching?
Explanation
Question 42
To minimize scapular notching in Reverse Total Shoulder Arthroplasty (RSA), what is the optimal positioning of the glenoid baseplate?
Explanation
Question 43
A 78-year-old female with severe rheumatoid arthritis sustains a comminuted intra-articular distal humerus fracture. She is managed with a Total Elbow Arthroplasty (TEA). Which implant design is most appropriate for this patient?
Explanation
Question 44
During a single-incision anterior approach for distal biceps tendon repair, which nerve is at greatest risk of iatrogenic injury if retractors are placed too vigorously on the lateral aspect of the wound?
Explanation
Question 45
Which of the following factors is most strongly predictive of nonunion in nonoperatively managed midshaft clavicle fractures?
Explanation
Question 46
When evaluating a patient with recurrent anterior shoulder instability, which imaging modality is considered the gold standard for quantifying anterior glenoid bone loss?
Explanation
Question 47
After open reduction and internal fixation of a proximal humerus fracture using a fixed-angle locking plate, what is the most common cause of late intra-articular screw penetration?
Explanation
Question 48
A 35-year-old male sustains a posterior elbow dislocation with an associated Regan-Morrey Type III coronoid fracture. What is the primary biomechanical consequence of failing to fix this specific coronoid fragment?
Explanation
Question 49
A 65-year-old male presents with primary glenohumeral osteoarthritis. A preoperative CT scan identifies a Walch B2 glenoid. What defines this specific glenoid morphology?
Explanation
Question 50
Which of the following is considered an absolute indication for operative fixation of a scapular fracture?
Explanation
Question 51
A 6-year-old child sustains a Bado Type I Monteggia fracture equivalent. Closed reduction normalizes the ulnar alignment, but the radial head remains anteriorly dislocated. What is the most likely interposing structure preventing reduction?
Explanation
Question 52
A 60-year-old male presents with insidious shoulder pain and stiffness 2 years after an anatomic total shoulder arthroplasty. Aspiration yields fluid that grows Cutibacterium acnes after 10 days. Which of the following best describes this organism?
Explanation
Question 53
What is the most common long-term complication leading to revision following linked Total Elbow Arthroplasty (TEA) for rheumatoid arthritis?
Explanation
Question 54
During tension band wiring of a transverse olecranon fracture, what is the biomechanical principle achieved by the figure-of-eight wire?
Explanation
Question 55
A 25-year-old male sustains a closed transverse fracture of the middle third of the humeral shaft resulting from a high-energy fall. He presents with a complete radial nerve palsy. What is the most appropriate initial management?
Explanation
Question 56
When performing an olecranon osteotomy for exposure of a complex distal humerus fracture, what type of osteotomy provides the best stability and surface area for subsequent repair?
Explanation
Question 57
Which of the following patients is the most classic and appropriate candidate for a primary Reverse Total Shoulder Arthroplasty (RSA)?
Explanation
Question 58
In the Rockwood classification of acromioclavicular (AC) joint injuries, what defines a Type V injury?
Explanation
Question 59
During ORIF of a comminuted radial head fracture, the "safe zone" for hardware placement is utilized to prevent impingement. Which anatomical landmarks define this safe zone?
Explanation
Question 60
A 72-year-old female sustains a minimally displaced 3-part proximal humerus fracture involving the greater tuberosity. She elects for non-operative management. What is the most common complication she should be counseled about?
Explanation
Question 61
A 45-year-old tennis player presents with refractory lateral epicondylitis despite 12 months of conservative treatment. Surgical debridement is planned. Which tendon is the primary pathological structure targeted during this procedure?
Explanation
Question 62
In reverse total shoulder arthroplasty (RTSA), scapular notching is a recognized complication. Which of the following surgical techniques or implant designs is most effective in minimizing the incidence of inferior scapular notching?
Explanation
None
