OITE & ABOS Orthopedic Board Review: Fracture, Hip, Knee MCQs Part 64
Key Takeaway
This page presents Part 64 of a professional orthopedic board review quiz. Designed for orthopedic residents and surgeons, it features 50 high-yield MCQs, modeled after OITE and AAOS exams, covering fracture, hip, and knee topics. Optimize your board certification preparation with interactive study and exam modes.
OITE & ABOS Orthopedic Board Review: Fracture, Hip, Knee MCQs Part 64
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
Figure 9 shows the AP radiograph of a 65-year-old man who has knee pain and swelling. What is the most likely diagnosis?
Explanation
REFERENCES: Barrack RL, Booth RE Jr, Lonner JH, et al (eds): Orthopaedic Knowledge Update: Hip and Knee Reconstruction 3. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2006, p 188.
Berkow R (ed): The Merck Manual, ed 14. Rathway, NJ, Merck, 1984, pp 910, 1176, 1200.
Question 2
If a surgeon inadvertently burrs through the midlateral wall of C5 during a anterior corpectomy, what structure is at greatest risk for injury?
Explanation
REFERENCES: Pfeifer BA, Freidberg SR, Jewell ER: Repair of injured vertebral artery in anterior cervical procedures. Spine 1994;19:1471-1474.
Gerszten PC, Welch WC, King JT: Quality of life assessment in patients undergoing nucleoplasty-based percutaneous discectomy. J Neurosurg Spine 2006;4:36-42.
Question 3
In patients with displaced radial neck fractures treated with open reduction and internal fixation with a plate and screws, the plate must be limited to what surface of the radius to avoid impingement on the proximal ulna?
Explanation
REFERENCES: Smith GR, Hotchkiss RN: Radial head and neck fractures: Anatomic guidelines for proper placement of internal fixation. J Shoulder Elbow Surg 1996;5:113-117.
Caputo AE, Mazzocca AD, Santoro VM: The nonarticulating portion of the radial head: Anatomic and clinical correlations for internal fixation. J Hand Surg Am 1998;23:1082-1090.
Question 4
A 57-year-old man reports right hip pain that has been progressive for the past several months. The pain is exacerbated by weight-bearing activities and improves somewhat with rest. A radiograph is shown in Figure 10a and a coronal T 1 -weighted MRI scan is shown in Figure 10b. What is the most likely diagnosis?
Explanation
REFERENCES: Resnick D (ed): Diagnosis of Bone and Joint Disorders. Philadelphia, PA,
WB Saunders, 2002, pp 3160-3162.
Sugano N: Osteonecrosis, in Fitzgerald R Jr, Kaufer H, Malkani A (eds): Orthopaedics. Philadelphia, PA, Mosby International, 2002, pp 877-887.
Question 5
The arrow in Figure 11 points toward a finding consistent with which of the following?
Explanation
REFERENCES: McLain R, Weinstein J (eds): Rothman-Simeone: The Spine, ed 4. Philadelphia, PA, WB Saunders, 1999, p 1173.
Koval KJ (ed): Orthopaedic Knowledge Update 7. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2002, p 674.
Question 6
The attachments of the transverse carpal ligament include which of the following structures?
Explanation
REFERENCES: Hollinshead W: Anatomy for Surgeons: The Back and Limbs, ed 3. Philadelphia, PA, Harper and Row, 1982, vol 3, pp 471-472.
Hoppenfeld S, deBoer P: Surgical Exposures in Orthopaedics, ed 2. Philadelphia, PA, Lippincott-Raven, 1994, pp 168-170.
Question 7
A 23-year-old woman falls from a bicycle and sustains a right knee injury. Figures 12a through 12d show radiographs and MRI scans of the knee. What is the most likely diagnosis?
Explanation
REFERENCES: Meyers MH, McKeever FM: Fracture of the intercondylar eminence of the tibia. J Bone Joint Surg Am 1970;52:1677-1684.
Wiss DA, Watson JT: Fractures of the tibial plateau, in Rockwood CA, Green DP, Bucholz RW, et al (eds): Rockwood and Green’s Fractures in Adults. Philadelphia, PA, Lippincott-Raven, 1996, pp 1920-1953.
Lubowitz JH, Elson WS, Guttmann D: Arthroscopic treatment of tibial plateau fractures: Intercondylar eminence avulsion fractures. Arthroscopy 2005;21:86-92.
Question 8
A 25-year-old man has a mass on the medial aspect of the left knee. He reports that the mass has been present for several years, but a recent increase in physical activity has resulted in periodic tenderness. Radiographs are shown in Figures 13a and 13b. What is the most likely diagnosis?
Explanation
REFERENCES: Menendez LR (ed): Orthopaedic Knowledge Update: Musculoskeletal Tumors. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2002, pp 103-111.
Parsons TW: Benign bone tumors, in Fitzgerald R Jr, Kaufer H, Malkani A (eds): Orthopaedics. Philadelphia, PA, Mosby International, 2002, pp 1027-1035.
Question 9
A previously asymptomatic 40-year-old man injures his shoulder in a fall. Examination shows that he is unable to lift the hand away from his back while maximally internally rotated. An axial MRI scan of the shoulder is shown in Figure 14. What is the most likely diagnosis?
Explanation
REFERENCES: Lyons RP, Green A: Subscapularis tendon tears. J Am Acad Orthop Surg 2005;13:353-363.
Warner JJ, Higgins L, Parsons IM, et al: Diagnosis and treatment of anterosuperior rotator cuff tears. J Shoulder Elbow Surg 2001;10:37-46.
Question 10
A patient is treated with volar plating for a distal radius fracture. The CT scan shown in Figure 15 is obtained after union of the fracture because the patient reports ongoing symptoms. The prominent hardware is most likely injuring what tendon?
Explanation
REFERENCES: Benson EC, Decarvalho A, Mikola EA, et al: Two potential causes of EPL rupture after distal radius volar plate fixation. Clin Orthop Relat Res 2006;451:218-222.
Cooney WP, Linscheid RL, Dobyns JH (eds): The Wrist: Diagnosis and Operative Treatment. Philadelphia, PA, Mosby-Year Book, 1998.
Question 11
A 9-year-old child sustains a proximal tibial physeal fracture with a hyperextension mechanism. What structure is at most risk for serious injury?
Explanation
REFERENCE: Beaty JH, Kasser JR: Rockwood and Wilkins Fractures in Children. Philadelphia, PA, JB Lippincott, 2006, p 961.
Question 12
A 25-year-old tennis player has shoulder pain and weakness to external rotation. MRI scans are shown in Figures 16a and 16b. What is the most likely cause of his weakness?
Explanation
REFERENCES: Piatt BE, Hawkins RJ, Fritz RC, et al: Clinical evaluation and treatment of spinoglenoid notch ganglion cysts. J Shoulder Elbow Surg 2002;11:600-604.
Inokuchi W, Ogawa K, Horiuchi Y: Magnetic resonance imaging of suprascapular nerve palsy.
J Shoulder Elbow Surg 1998;7;223-227.
Question 13
The posterior approach to the proximal radius uses what intermuscular interval?
Explanation
REFERENCES: Spinner M: Injuries to the Major Branches of Peripheral Nerves of the Forearm, ed 2. Philadelphia, PA, WB Saunders, 1978, pp 66-77.
Henry AK: Extensile Exposure, ed 3. New York, NY, Churchill Livingstone, 1995.
Question 14
Which of the following statements best describes the anatomic considerations of the popliteal artery posterior to the knee joint?
Explanation
90 degrees of flexion.
REFERENCES: Barrack RL, Booth RE Jr, Lonner JH, et al (eds): Orthopaedic Knowledge Update: Hip and Knee Reconstruction 3. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2006, p 151.
Anderson JE: Grant’s Atlas of Anatomy, ed 7. Baltimore, MD, Lippincott Williams & Wilkins, 1978, pp 4-53.
Question 15
A 62-year-old woman reports diffuse aches and pains of the hip and pelvis. She denies any significant trauma but does have a history of chronic anemia. Figure 17a shows a radiograph of the pelvis, and Figures 17b and 17c show T 2 -weighted MRI scans. What is the most likely diagnosis?
Explanation
REFERENCE: Resnick D (ed): Diagnosis of Bone and Joint Disorders. Philadelphia, PA,
WB Saunders, 2002, pp 2189-2216.
Question 16
What structure is located at the tip of the arrow in Figure 18?
Explanation
REFERENCE: An H: Diagnostic imaging of the spine, in Principles and Techniques of Spine Surgery. Baltimore, MD, Lippincott Williams & Wilkins, 1998, pp 102-125.
Question 17
What structure is located at the tip of the arrow in Figure 18?
Explanation
REFERENCE: An H: Diagnostic imaging of the spine, in Principles and Techniques of Spine Surgery. Baltimore, MD, Lippincott Williams & Wilkins, 1998, pp 102-125.
Question 18
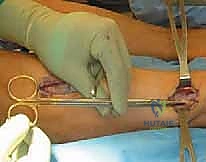
A patient undergoes the procedure shown in Figure 19. An important part of this procedure is preservation of what wrist ligament?
Explanation
REFERENCE: Jebson PJ, Engber WD: Proximal row carpectomy. Tech Hand Up Extrem Surg 1999;3:32-36.
Question 19
A 23-year-old woman reports right knee pain and fullness. The pain is worse with activity but also present at rest. Radiographs are shown in Figures 20a and 20b. What is the most likely diagnosis?
Explanation
REFERENCES: Sanders TG, Parsons TW: Radiographic imaging of musculoskeletal neoplasia. Cancer Control 2001;8:221-231.
Menendez LR (ed): Orthopaedic Knowledge Update: Musculoskeletal Tumors. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2002, pp 175-186.
Question 20
What is the structure indicated by the letter “A” in Figure 21?
Explanation
REFERENCES: Morrey BF: Anatomy of the elbow joint, in Morrey BF (ed): The Elbow and Its Disorders. Philadelphia, PA, WB Saunders, 1993, p 30.
O’Driscoll SW, Bell DF, Morrey BF: Posterolateral rotatory instability of the elbow. J Bone Joint Surg Am 1991;73:440-446.
Question 21
A 16-year-old boy sustains a twisting injury to the left knee while wrestling. MRI scans are shown in Figures 22a through 22c. What is the most likely diagnosis?
Explanation
REFERENCES: Sanders TG, Miller MD: A systematic approach to magnetic resonance imaging interpretation of sports medicine injuries of the knee. Am J Sports Med 2005;33:131-148.
Miller TT: Magnetic resonance imaging of the knee, in Insall JN, Scott WN (eds): Surgery of the Knee, ed 4. Philadelphia, PA, Churchill Livingstone, 2006, vol 1, pp 201-224.
Question 22
A 48-year-old woman reports bilateral thigh pain that is limiting her function as a librarian. A radiograph and a bone scan are shown in Figures 23a and 23b. What is the most likely diagnosis?
Explanation
REFERENCES: Resnick D: Diagnosis of Bone and Joint Disorders, ed 3. Philadelphia, PA,
WB Saunders, 1995, pp 956-957.
Wheeless’ Textbook of Orthopaedics: Acetabular Protrusio. www.wheelessonline.com/ortho/acetabular_protrusio
Question 23
At the level of tibial bone resection in total knee arthroplasty, where does the common peroneal nerve lie?
Explanation
REFERENCES: Clarke HD, Schwartz JB, Math KR, et al: Anatomic risk of peroneal nerve injury with the “pie crust” technique for valgus release in total knee arthroplasty. J Arthroplasty 2004;19:40-44.
Anderson JE: Grant’s Atlas of Anatomy, ed 7. Baltimore, MD, Lippincott Williams & Wilkins, 1978, pp 4-52, 4-53.
Question 24
Figures 24a through 24c show the coronal T 1 -weighted, T 2 -weighted fat-saturated, and T 1 -weighted fat-saturated gadolinium MRI scans of the proximal thigh of a 52-year-old woman who reports a mass in the medial thigh and groin area. She notes that the fullness has grown in size over the course of many months. Based on these findings, what is the most likely diagnosis?
Explanation
REFERENCE: Sanders TG, Parsons TW: Radiographic imaging of musculoskeletal neoplasia. Cancer Control 2001;8:221-231.
Question 25
The arrows in the axial T 1 -weighted MRI scan shown in Figure 25 show which of the following structures?
Explanation
REFERENCES: Gross MS, Gelberman RH: The anatomy of the distal ulnar tunnel. Clin Orthop Relat Res 1985;196:238-247.
Denman EE: The anatomy of the space of Guyon. The Hand 1978;10:69-76.
Question 26
An 82-year-old man has had episodic right thigh pain after undergoing a total hip arthroplasty 10 years ago. Initial postoperative radiographs are shown in Figures 26a and 26b, and current radiographs are shown in Figures 26c and 26d. What is the most likely cause of his pain?
Explanation
REFERENCES: Engh CA, Massin P, Suthers KE: Roentgenographic assessment of biologic fixation of porous-surface femoral components. Clin Orthop Relat Res 1990;257:107-128.
Engh CA, Hooten JP, Zettl-Schaffer KF, et al: Evaluation of bone ingrowth in proximally and extensively porous-coated anatomic medullary locking prostheses retrieved at autopsy. J Bone Joint Surg Am 1995;77:903-910.
Question 27
A 37-year-old patient with type I diabetes mellitus has a flexor tenosynovitis of the thumb flexor tendon sheath following a kitchen knife puncture wound to the volar aspect of the thumb. Left unattended, this infection will likely first spread proximally creating an abscess in which of the following spaces of the palm?
Explanation
REFERENCES: Hollinshead W: Anatomy for Surgeons: The Back and Limbs, ed 3. Philadelphia, PA, Harper and Row, 1982, vol 3, pp 478-479.
Lee D, Ferlic R, Neviaser R: Hand infections, in Berger R, Weiss AP (eds): Hand Surgery. Philadelphia, PA, Lippincott Williams & Wilkins, 2004, pp 1784-1785.
Question 28
What tendon is closest to an appropriately placed anterolateral portal for ankle arthroscopy?
Explanation
REFERENCE: Ogut T, Akgun I, Kesmezacar H, et al: Navigation for ankle arthroscopy: Anatomical study of the anterolateral portal with reference to the superficial peroneal nerve. Surg Radiol Anat 2004;26:268-274.
Question 29
A 52-year-old woman reports nagging shoulder pain that has been present for months and is slowly progressive in nature. The patient also reports nocturnal pain and notes that the pain is not activity related. Figures 27a and 27b show the radiograph and bone scan, and Figures 27c through 27e show T 1 -weighted, T 2 -weighted, and gadolinium MRI scans, respectively. Based on these findings, what is the most likely diagnosis?
Explanation
REFERENCES: Menendez LR (ed): Orthopaedic Knowledge Update: Musculoskeletal Tumors. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2002, pp 187-194.
Resnick D (ed): Diagnosis of Bone and Joint Disorders. Philadelphia, PA, WB Saunders, 2002, pp 3897-3904.
Question 30
Figure 28 shows an arthroscopic view of a right shoulder in the lateral position through a posterior portal. What is the area between structure B (biceps) and SS (subscapularis tendon)?
Explanation
REFERENCES: Selecky MT, Tibone JE, Yang BY, et al: Glenohumeral joint translation after arthroscopic thermal capsuloplasty of the rotator interval. J Shoulder Elbow Surg 2003;12:139-143.
Harryman DT, Sidles JA, Harris SL, et al: The role of the rotator interval capsule in passive motion and stability of the shoulder. J Bone Joint Surg Am 1992;74:53-66.
Question 31
New painful paresthesias near the site of the incision after an ulnar nerve transposition is the result of injury to what nerve?
Explanation
REFERENCE: Dellon AL, Mackinnon SE: Injury to the medial antebrachial cutaneous nerve during cubital tunnel surgery. J Hand Surg Br 1985;10:33-36.
Question 32
A 23-year-old man reports pain on the superior aspect of his right shoulder with repetitive overhead activities and when lying on his right side. Figure 29 shows an axial MRI scan. What is the most likely diagnosis based on the MRI findings?
Explanation
REFERENCES: Kurtz CA, Humble BJ, Rodosky MW, et al: Symptomatic os acromiale. J Am Acad Orthop Surg 2006;14:12-19.
Ortiguera CJ, Buss DD: Surgical management of the symptomatic os acromiale. J Shoulder Elbow Surg 2002;11:521-528.
Question 33
Following a chevron bunionectomy performed through a dorsal approach, a patient has persistent numbness on the dorsal and medial aspect of the hallux. What nerve has most likely been injured?
Explanation
REFERENCE: Miller SD: Dorsomedial cutaneous nerve syndrome: Treatment with nerve transection and burial into bone. Foot Ankle Int 2001;22:198-202.
Question 34
A 74-year-old man reports progressive left hip pain with weight-bearing activities. A radiograph is shown in Figure 30. What is the most likely underlying diagnosis?
Explanation
REFERENCES: Menendez LR (ed): Orthopaedic Knowledge Update: Musculoskeletal Tumors. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2002, pp 211-215.
Resnick D (ed): Diagnosis of Bone and Joint Disorders. Philadelphia, PA, WB Saunders, 2002, pp 1947-2000.
Question 35
The anatomy of the sciatic nerve as it exits the pelvis is best described as exiting through the
Explanation
REFERENCES: Hoppenfeld S, deBoer P: Surgical Exposures in Orthopaedics: The Anatomic Approach. Philadelphia, PA, JB Lippincott, 1984, p 347.
Anderson JE: Grant’s Atlas of Anatomy, ed 7. Baltimore, MD, Lippincott Williams & Wilkins, 1978, pp 4-34, 4-36.
Hollingshead WH: Anatomy for Surgeons: The Back and Limbs, ed 2. Hagerstown, MD, Harper & Row, 1969, pp 607-609.
Question 36
What complication is more likely following excessive medial retraction of the anterior covering structures during the anterolateral (Watson-Jones) approach to the hip?
Explanation
REFERENCES: Hoppenfeld S, deBoer P: Surgical Exposures in Orthopaedics: The Anatomic Approach. Philadelphia, PA, JB Lippincott, 1984, p 325.
Anderson JE: Grant’s Atlas of Anatomy, ed 7. Baltimore, MD, Lippincott Williams & Wilkins, 1978, pp 4-17, 4-18.
Question 37
In the most common condition causing a winged scapula, which of the following nerves is affected?
Explanation
REFERENCES: Kline DG, Hudson AR: Nerve Injuries: Operative Results for Major Nerve Injuries, Entrapments and Tumors. Philadelphia, PA, WB Saunders, 1995.
van Alfen N, van Engelen BG: The clinical spectrum of neuralgic amyotrophy in 246 cases. Brain 2006;129:438-450.
Question 38
A 17-year-old woman seen in the emergency department reports right knee pain and swelling that has progressively worsened over the past several weeks. Radiographs are shown in Figures 31a and 31b. What is the most likely diagnosis?
Explanation
REFERENCES: Sanders TG, Parsons TW: Radiographic imaging of musculoskeletal neoplasia. Cancer Control 2001;8:221-231.
Menendez LR (ed): Orthopaedic Knowledge Update: Musculoskeletal Tumors. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2002, pp 175-186.
Question 39
A 26-year-old man has had hand pain and progressive swelling in the knuckle for the past several months. He denies any trauma to the hand. The ring finger metacarpophalangeal joint is tender, and there is loss of motion in the digit. Figure 32a shows the radiograph and Figures 32b through 32d show the T 1 -weighted, T 2 -weighted, and gadolinium MRI scans, respectively. What is the most likely diagnosis?
Explanation
T2-weighted image and has some gadolinium uptake. There are no cystic components in this lesion. The subchondral location and expansile nature are highly suggestive of giant cell tumor of bone. A lesion with this appearance might also represent an aneurysmal bone cyst, given the amount of expansion present.
REFERENCES: Menendez LR (ed): Orthopaedic Knowledge Update: Musculoskeletal Tumors. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2002, pp 113-118.
Parsons TW: Benign bone tumors, in Fitzgerald R Jr, Kaufer H, Malkani A (eds): Orthopaedics. Philadelphia, PA, Mosby International, 2002, pp 1027-1035.
Question 40
Which of the following best describes the relationship of the median nerve to the flexor carpi radialis tendon just proximal to the carpal canal?
Explanation
REFERENCES: Hoppenfeld S, deBoer P: Surgical Exposures in Orthopaedics, ed 2. Philadelphia, PA, Lippincott-Raven, 1994, pp 118-131.
Henry A: Extensile Exposure, ed 3. Edinburgh, UK, Churchill Livingstone, 1995, pp 100-107.
Question 41
Which of the following muscles has dual innervation?
Explanation
REFERENCE: Mahakkanukrauh P, Somsarp V: Dual innervation of the brachialis muscle.
Clin Anat 2002;15:206-209.
Question 42
Figure 33a shows a line drawing of a normal hemipelvis. The anterior acetabular rim is bold. Figure 33b illustrates a hemipelvis with a crossover sign, which is indicative of what acetabular pathology?
Explanation
REFERENCES: Reynolds D, Lucas J, Klaue K: Retroversion of the acetabulum: A cause of hip pain. J Bone Joint Surg Br 1999;81:281-288.
Espinosa N, Rothenfluh DA, Beck M, et al: Treatment of femoro-acetabular impingement: Preliminary results of labral refixation. J Bone Joint Surg Am 2006;88:925-935.
Question 43
Which of the following structures is most vulnerable during a medial sesamoidectomy of the hallux?
Explanation
REFERENCE: Sarrafian SK: Anatomy of the Foot and Ankle, Descriptive, Topographic, Functional, ed 2. Philadelphia, PA, JB Lippincott, 1993, p 377.
Question 44
What structure is most at risk for injury from a retractor against the tracheoesophageal junction during an anterior approach to the cervical spine?
Explanation
REFERENCES: Ebraheim NA, Lu J, Skie M, et al: Vulnerability of the recurrent laryngeal nerve in the anterior approach to the lower cervical spine. Spine 1997;22:2664-2667.
Kilburg C, Sullivan HG, Mathiason MA: Effect of approach side during anterior cervical discectomy and fusion on the incidence of recurrent laryngeal nerve injury. J Neurosurg Spine 2006;4:273-277.
Question 45
A 40-year-old man has had hip pain with increased activity over the past year. Examination reveals restriction of motion and tenderness with combined hip flexion, adduction, and internal rotation. An AP radiograph is shown in Figure 34. What is the most likely diagnosis?
Explanation
REFERENCES: Beall DP, Sweet CF, Martin HD, et al: Imaging findings of femoraoacetabular impingement syndrome. Skeletal Radiol 2005;34:691-701.
Mardones RM, Gonzalez C, Chen Q, et al: Surgical treatment of femoroacetabular impingement: Evaluation of the effect of the size of the resection. J Bone Joint Surg Am 2006;88:84-91.
Question 46
Figure 35 shows the radiograph of a 44-year-old woman with rheumatoid arthritis who reports neck pain. Below what threshold number is surgical stabilization warranted for the interval shown by the arrow?
Explanation
REFERENCE: Boden SD, Dodge LD, Bohlman HH, et al: Rheumatoid arthritis of the cervical spine: A long-term analysis with predictors of paralysis and recovery. J Bone Joint Surg Am 1993;75:1282-1297.
Question 47
An axillary nerve lesion may cause weakness in the deltoid and the
Explanation
REFERENCE: Hollinshead WH: Anatomy for Surgeons: The Back and Limbs. New York, NY, Harper & Row, 1969.
Question 48
Figure 36 shows an AP radiograph of a 65-year-old man who reports activity-related groin pain. History reveals that he underwent total hip arthroplasty 12 years ago. What is the most likely diagnosis?
Explanation
REFERENCES: Visuri T, Pulkkinen P, Paavolainen P: Malignant tumors at the site of total hip prosthesis: Analytic review of 46 cases. J Arthroplasty 2006;21:311-323.
Bezwada HP, Shah AR, Zambito K, et al: Distal femoral allograft reconstruction for massive osteolytic bone loss in revision total knee arthroplasty. J Arthroplasty 2006;21:242-248.
Kitamura N, Naudie DD, Leung SB, et al: Diagnostic features of pelvic osteolysis on computed tomography: The importance of communication pathways. J Bone Joint Surg Am 2005;87:1542-1550.
Question 49
A 21-year-old man who was injured in a snowboarding accident 18 months ago now reports wrist pain. An MRI scan is shown in Figure 37. Based on the image findings, what is the most likely diagnosis?
Explanation
REFERENCE: Perlik PC, Guilford WB: Magnetic resonance imaging to assess vascularity of scaphoid nonunions. J Hand Surg Am 1991;16:479-484.
Question 50
An 82-year-old woman reports activity-related knee pain. History reveals that she underwent total knee arthroplasty 16 years ago. AP and lateral radiographs and a bone scan are shown in Figures 38a through 38c. What is the most likely diagnosis?
Explanation
well-defined borders. Joint space narrowing medially is consistent with polyethylene wear.
The most likely diagnosis is particle-mediated osteolysis. Metastatic tumors and primary sarcomas adjacent to an arthroplasty are extremely rare. In addition, malignant tumors and infection would more likely reveal a destructive lesion with poorly defined borders and increased uptake on a bone scan. Stress shielding with massive bone loss has not been described in knee arthroplasty literature, although this entity has been observed in fully porous-coated femoral implants in total hip arthroplasty.
REFERENCES: Robinson EJ, Mulliken BD, Bourne RB, et al: Catastrophic osteolysis in total knee replacement: A report of 17 cases. Clin Orthop Relat Res 1995;321:98-105.
Archibeck MJ, Jacobs JJ, Roebuck KA, et al: The basic science of periprosthetic osteolysis. Instr Course Lect 2001;50:185-195.
Bugbee WD, Culpepper WJ, Engh CA Jr, et al: Long-term clinical consequences of stress-shielding after total hip arthroplasty without cement. J Bone Joint Surg Am 1997;79:1007-1012.
Question 51
A 28-year-old male sustains a high-energy Pauwels III (vertical shear) femoral neck fracture. Which of the following fixation constructs provides the highest biomechanical stability against the predominant deforming forces in this fracture pattern?
Explanation
Question 52
A 68-year-old female presents with complaints of instability and knee effusion 6 months after a posterior-stabilized total knee arthroplasty (TKA). Examination reveals a stable knee in full extension and 90 degrees of flexion, but marked laxity at 30 to 45 degrees of flexion. What is the most likely intraoperative technical error that caused this presentation?
Explanation
Question 53
A 55-year-old male undergoes a total hip arthroplasty utilizing a ceramic-on-ceramic bearing surface. Two years postoperatively, he complains of a loud squeaking noise from the hip during specific movements. What is the most significant risk factor for this complication?
Explanation
Question 54
During a posteromedial approach to the tibia for open reduction and internal fixation of a Schatzker IV tibial plateau fracture, the dissection utilizes the interval between the medial head of the gastrocnemius and the pes anserinus. Which of the following structures is at greatest risk of iatrogenic injury during the superficial dissection?
Explanation
Question 55
A 40-year-old male is diagnosed with Ficat Stage II avascular necrosis of the femoral head. If non-operative management fails, preserving the native joint is dependent on the viability of the femoral head's blood supply. What is the primary arterial supply to the weight-bearing dome of the adult femoral head?
Explanation
Question 56
A 22-year-old athlete presents with recurrent instability two years after an anterior cruciate ligament (ACL) reconstruction using a bone-patellar tendon-bone autograft. Imaging shows an intact but non-functional graft. What is the most common technical cause of ACL reconstruction failure?
Explanation
Question 57
A 35-year-old male sustains a Gustilo-Anderson IIIB open tibial shaft fracture following a motorcycle collision. After emergent debridement and external fixation, soft tissue coverage is required. Based on classic orthopedic trauma principles, soft tissue flap coverage should ideally be performed within what timeframe to minimize the risk of deep infection?
Explanation
Question 58
An 80-year-old female falls and sustains a periprosthetic femur fracture around a cemented total hip arthroplasty stem. Radiographs demonstrate a fracture at the tip of the stem. The stem is radiographically loose, but there is excellent surrounding proximal bone stock. How is this fracture classified, and what is the standard treatment?
Explanation
Question 59
During the physical examination of a patient with a traumatic knee injury, the dial test reveals a 15-degree increase in external rotation on the injured side compared to the normal side when tested at 30 degrees of knee flexion. However, at 90 degrees of knee flexion, the external rotation is symmetric bilaterally. What is the correct diagnosis?
Explanation
Question 60
A 45-year-old male undergoes open reduction and internal fixation of a displaced transverse patella fracture using a tension band wiring technique. Which biomechanical principle best explains the efficacy of this fixation method?
Explanation
Question 61
A 24-year-old hockey player presents with groin pain exacerbated by hip flexion and internal rotation. Radiographs reveal a cam-type femoroacetabular impingement (FAI). Which of the following anatomic abnormalities is the primary driver of this specific type of impingement?
Explanation
Question 62
A 16-year-old female suffers an acute, traumatic lateral patellar dislocation. Which of the following soft-tissue structures is the primary restraint to lateral patellar translation at 0 to 20 degrees of knee flexion, and is nearly universally ruptured in this injury?
Explanation
Question 63
In a 30-year-old patient with a displaced femoral neck fracture, which of the following biomechanical factors most significantly increases the risk of nonunion and fixation failure?
Explanation
Question 64
When treating an intertrochanteric femur fracture with a sliding hip screw, maintaining a Tip-Apex Distance (TAD) of less than 25 mm is primarily associated with a decreased risk of which of the following complications?
Explanation
Question 65
During a posterior-stabilized total knee arthroplasty, the surgeon notes that the knee is well-balanced in extension but is overly tight in flexion. Which of the following is the most appropriate step to balance the knee?
Explanation
Question 66
A surgeon performs a total hip arthroplasty via the direct anterior approach. Which of the following internervous planes is utilized during the deep surgical dissection?
Explanation
Question 67
A 68-year-old woman presents with vague, aching thigh pain for 3 months. She has been taking alendronate for 8 years. Radiographs reveal focal lateral cortical thickening of the subtrochanteric femur with a transverse radiolucent line. What is the most appropriate prophylactic surgical management?
Explanation
Question 68
A 25-year-old man sustains a traumatic knee dislocation. Following closed reduction, his Ankle-Brachial Index (ABI) is measured at 0.85. What is the most appropriate next step in management?
Explanation
Question 69
Which of the following is true regarding a Hoffa fracture (coronal shear fracture) of the distal femur?
Explanation
Question 70
A 60-year-old man with a metal-on-metal total hip arthroplasty presents with groin pain and a palpable anterior mass. Aspiration yields thick, sterile fluid. What is the most likely histologic finding of the periarticular tissue?
Explanation
Question 71
During intramedullary nailing of a proximal third tibial shaft fracture, utilizing a standard infrapatellar entry portal most commonly leads to which of the following malalignments?
Explanation
Question 72
A 72-year-old woman presents with acute onset of knee pain and swelling 3 weeks after a primary total knee arthroplasty. Aspiration reveals 65,000 WBCs/mcL with 95% neutrophils. What is the most appropriate surgical treatment?
Explanation
Question 73
A 35-year-old male sustains a posterior hip dislocation in a motor vehicle accident. Which of the following clinical presentations is most characteristic of this injury?
Explanation
Question 74
Which of the following is the most absolute indication for operative fixation of a closed patella fracture?
Explanation
Question 75
A 22-year-old man sustains a closed bilateral femoral shaft fracture. He undergoes reamed intramedullary nailing 12 hours after injury. On post-operative day 2, he develops petechiae, confusion, and hypoxia. What is the primary pathophysiologic mechanism of this syndrome?
Explanation
Question 76
In the management of posterior wall acetabular fractures, which of the following radiographic findings is an absolute indication for open reduction and internal fixation?
Explanation
Question 77
During a medial parapatellar approach for a total knee arthroplasty, taking the arthrotomy too far distally and laterally risks injury to which of the following structures?
Explanation
Question 78
During an ilioinguinal approach to the acetabulum, the surgeon encounters massive bleeding over the superior pubic ramus near the symphysis. This bleeding is most likely originating from an anastomosis between which two vascular systems?
Explanation
Question 79
A 35-year-old male sustains a vertically oriented, displaced femoral neck fracture (Pauwels type III). Which of the following fixation constructs provides the most biomechanically stable fixation against vertical shear forces and varus collapse?
Explanation
Question 80
A 65-year-old woman presents with an audible and palpable "clunk" during active extension of her knee, 1 year after undergoing a posterior-stabilized total knee arthroplasty (TKA). What is the primary cause of this phenomenon?
Explanation
Question 81
A 45-year-old male sustains a high-energy Schatzker IV tibial plateau fracture featuring a displaced posteromedial shear fragment. Which surgical approach is most appropriate for direct visualization and buttress plating of this specific fragment?
Explanation
Question 82
A patient experiences recurrent posterior dislocations following a primary total hip arthroplasty. Radiographs and a CT scan demonstrate the acetabular component is well-fixed but placed in 5 degrees of retroversion. Which of the following is the most appropriate definitive management?
Explanation
Question 83
A 28-year-old male presents with an acutely swollen knee after a severe hyperextension injury. Examination reveals a positive Lachman, positive posterior drawer, and gross varus/valgus instability. His ankle-brachial index (ABI) is measured at 0.85. What is the most appropriate next step in management?
Explanation
Question 84
A 25-year-old male polytrauma patient sustains a comminuted femoral shaft fracture, bilateral flail chest, and severe pulmonary contusions. His serum lactate is 4.5 mmol/L and pH is 7.21 despite initial fluid resuscitation. What is the most appropriate initial management of the femur fracture?
Explanation
Question 85
A 30-year-old male is involved in a motor vehicle collision and sustains a posterior hip dislocation associated with a femoral head fracture and a posterior wall acetabular fracture. According to the Pipkin classification, what type of injury is this?
Explanation
Question 86
Following an anterior cruciate ligament (ACL) reconstruction using a bone-patellar tendon-bone autograft, a patient complains of a significant loss of knee flexion, though full extension is maintained. Which of the following technical errors is the most likely cause of this specific complication?
Explanation
Question 87
When treating a stable intertrochanteric femur fracture with a sliding hip screw, which of the following radiographic parameters is most strongly predictive of lag screw cut-out?
Explanation
Question 88
An 82-year-old female presents with a displaced periprosthetic distal femur fracture (Lewis and Rorabeck Type II) above a well-fixed total knee arthroplasty. Review of operative records confirms the femoral component has a closed intercondylar box design. What is the most appropriate surgical management?
Explanation
None
