Introduction and Historical Context of Femoral Resection
The proximal and mid-femur represent frequent anatomic sites for the manifestation of primary bone sarcomas and metastatic osseous lesions. Historically, patients presenting with extensive malignant tumors of the femur were relegated to high-risk groups for limb-sparing procedures. The prevailing surgical dogma dictated that the requisite massive bone and soft tissue resections would inevitably yield unacceptable postoperative functional deficits. Furthermore, the deleterious consequences of adjuvant chemotherapy and radiation therapy on wound healing and local tissue integrity heavily influenced surgical decision-making. Consequently, radical ablative procedures—specifically hip disarticulation and hemipelvectomy—were the standard of care for large lesions of the proximal or mid-femur. These ablative procedures, while achieving local oncologic control, were universally associated with catastrophic functional, aesthetic, and psychological morbidity.
Evolution to Limb-Sparing Surgery
The contemporary orthopedic oncology paradigm has shifted dramatically toward limb salvage. Enhanced survivorship of patients with musculoskeletal malignancies, driven by advanced neoadjuvant and adjuvant chemotherapeutic regimens, has necessitated surgical solutions that prioritize both oncologic clearance and functional restoration. Concurrently, leaps in bioengineering, materials science, and refined surgical techniques have made limb-sparing procedures highly viable.
Today, proximal and total femur resections with endoprosthetic reconstruction represent reliable, standard-of-care surgical options. These procedures provide excellent local tumor control while preserving a functional extremity. Beyond primary bone sarcomas and metastatic bone disease, the indications for massive endoprosthetic reconstruction have expanded to encompass complex non-oncologic scenarios. These include catastrophic failure of internal fixation, severe periprosthetic fractures (e.g., Vancouver B3/C) with profound osteolysis, failed total hip arthroplasty with massive segmental bone loss, chronic recalcitrant osteomyelitis, metabolic bone diseases, and complex congenital skeletal defects.
Advances in Modular Prostheses
Historically, skeletal reconstruction methods included resection arthrodesis, massive osteoarticular allografts, and allograft-prosthetic composites. Osteoarticular allografts, heavily utilized in the 1970s and 1980s, aimed to restore native joint anatomy by matching donor bone to the recipient. However, they were plagued by high complication rates, including deep infection, nonunion at the host-allograft junction, joint instability, allograft fracture, and subchondral collapse, ultimately leading to high failure rates.
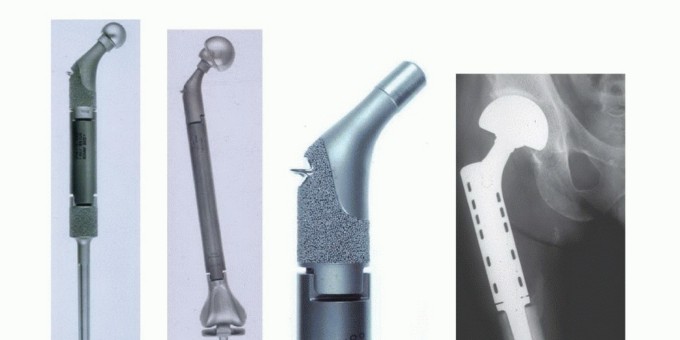
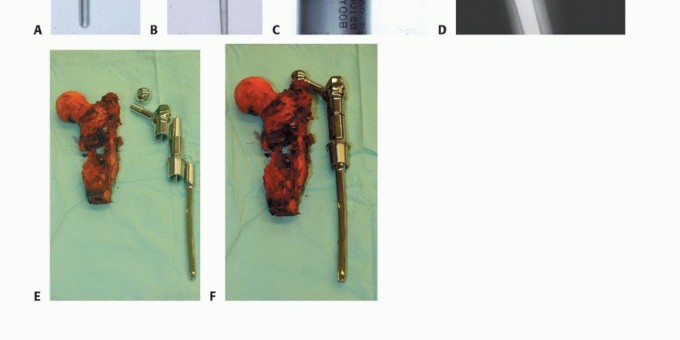
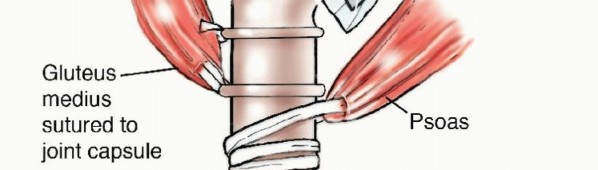
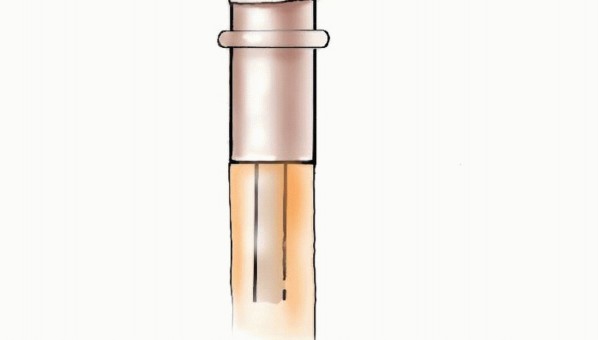
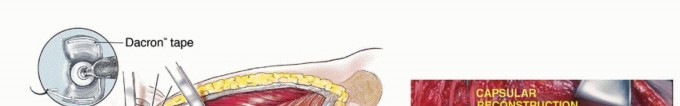
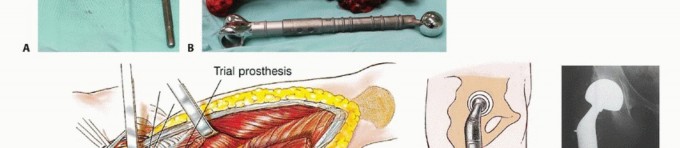
The introduction of modular endoprostheses in the mid-1980s revolutionized the reconstruction of massive skeletal defects. Modularity affords the surgeon intraoperative flexibility to precisely measure the osseous defect following tumor resection and assemble a customized construct. These interchangeable systems consist of articulating segments, body segments of varying lengths, and intramedullary stems of different diameters and lengths. Modern design features incorporate extensive porous coatings (often titanium or hydroxyapatite) on the extracortical portions to promote osteointegration and soft tissue ingrowth. Additionally, metallic loops and dedicated trochanteric claws facilitate the critical reattachment of the abductor mechanism.
Surgical Anatomy and Biomechanics
A profound understanding of the regional anatomy is paramount for achieving negative oncologic margins while preserving critical neurovascular structures and optimizing biomechanical reconstruction.
Hip Joint and Capsular Considerations
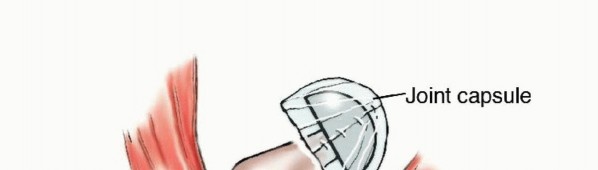
The intracapsular location of the femoral neck creates a unique biologic environment. Tumors of the proximal femur can theoretically spread into the hip joint, adjacent synovium, joint capsule, and ligamentum teres. The ligamentum teres, in particular, serves as a potential anatomic conduit for transarticular skip metastases to the acetabulum. Fortunately, direct intra-articular involvement remains rare in the absence of a pathologic fracture.
In most proximal femoral resections, the hip capsule can be meticulously preserved, allowing for an intra-articular resection of the femur. However, if preoperative imaging demonstrates capsular invasion, acetabular extension, or if the biopsy tract is contaminated, an extra-articular resection of the hip joint (en bloc resection of the proximal femur with the intact capsule and acetabular articular surface) must be executed to adhere to oncologic principles.
Trochanters and Muscle Reattachment
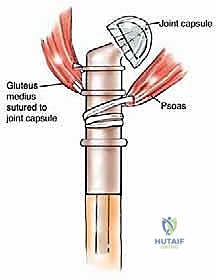
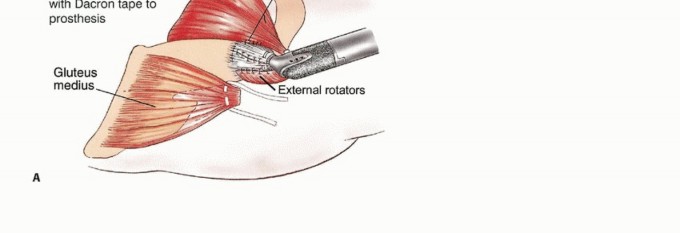
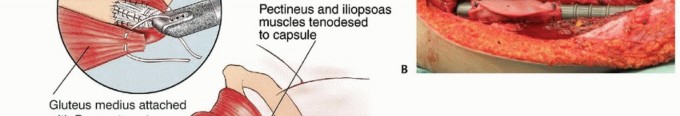
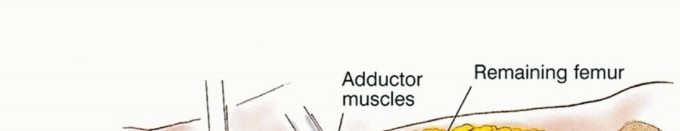
The greater trochanter serves as the critical insertion site for the hip abductors (gluteus medius and minimus). During en bloc resection, the greater trochanter is typically removed with the surgical specimen. The abductor tendon stump must be meticulously tagged with heavy non-absorbable sutures for later reattachment to the prosthesis.
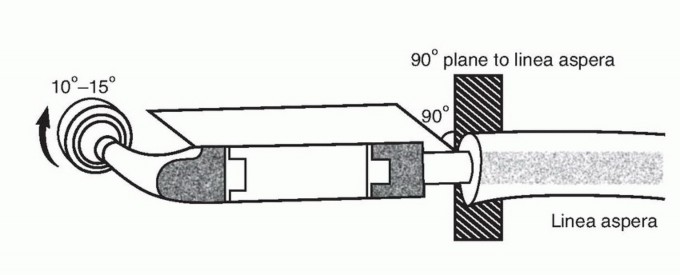
Similarly, the lesser trochanter, the insertion site for the iliopsoas muscle, is resected. The psoas tendon must be identified, tagged, and preserved. The biomechanical success of the reconstruction relies heavily on the balanced reattachment of the abductors laterally and the psoas medially to the prosthesis, which restores a functional force couple and provides dynamic stability to the prosthetic hip joint.
Femoral Vascular Considerations
The femoral artery courses distally within the anterior thigh, entering the sartorial (Hunter's) canal and transitioning into the popliteal artery as it passes through the adductor hiatus. The profunda femoris artery, branching laterally and posteriorly from the common femoral artery approximately 4 cm distal to the inguinal ligament, is a critical structure during proximal femoral resections.
Large extraosseous tumor components extending medially may necessitate the en bloc ligation and resection of the profunda femoris. In pediatric or adolescent patients with pristine vasculature, ligation of the profunda femoris is generally well-tolerated without ischemic compromise. However, in adult populations, mandatory preoperative angiography is required. Ligation of the profunda femoris in a patient with an occluded superficial femoral artery (SFA) will precipitate acute limb ischemia, inevitably leading to amputation.
Knee Joint Tumor Invasion
For diaphyseal tumors extending distally, the knee joint is rarely invaded directly unless facilitated by a pathologic fracture, an improperly placed biopsy tract, or direct extension along the cruciate ligaments. The presence of a hemarthrosis is highly suspicious for intra-articular disease. In such clinical scenarios, an intra-articular resection of the knee joint—entailing en bloc resection of the distal femur with the knee joint capsule, cruciate ligaments, and the articular surface of the proximal tibia—is oncologically mandated.
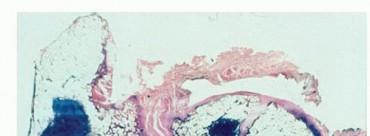
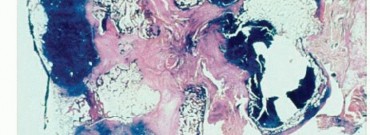
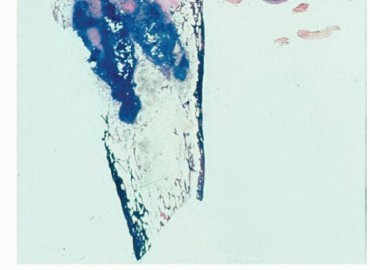
Indications and Contraindications for Femoral Resection
The decision to proceed with massive endoprosthetic reconstruction is dictated by the pathology, the extent of bone loss, and the patient's overall physiologic status.
Proximal versus Total Femur Resection Criteria
Proximal Femur Resection is indicated for metaphyseal-diaphyseal lesions that:
1. Extend distally beyond the lesser trochanter.
2. Induce extensive cortical destruction precluding standard osteosynthesis or standard arthroplasty.
3. Allow for the preservation of at least 3 to 4 cm of healthy distal femoral diaphysis to accommodate the intramedullary stem of the prosthesis.
Total Femur Resection is an extreme limb-salvage procedure indicated for extensive diaphyseal lesions that:
1. Extend proximally to the lesser trochanter and distally to the distal diaphyseal-metaphyseal junction.
2. Cause massive, uncontained bone destruction or represent multi-focal skip lesions within the same bone.
Non-oncologic indications have expanded significantly. These include catastrophic failure of proximal femoral internal fixation, severe acute periprosthetic fractures in the setting of profound osteopenia or osteolysis, failed total hip arthroplasty with segmental bone loss extending below the lesser trochanter, and debilitating chronic osteomyelitis where eradication requires complete segmental resection.
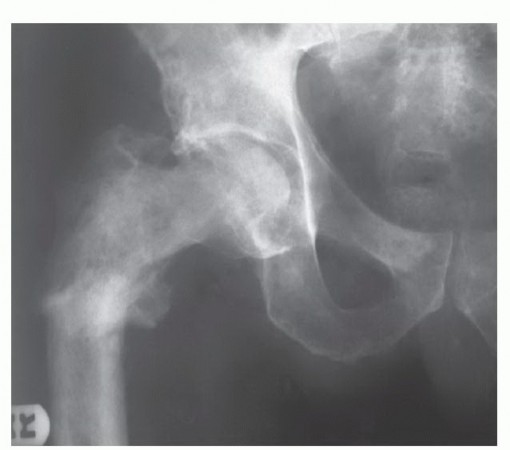
Preoperative Planning and Imaging Studies
Given the magnitude of proximal and total femur resections, meticulous preoperative planning is non-negotiable. The surgeon must precisely define the extent of bone resection, the dimensions of the requisite modular components, and the feasibility of soft tissue coverage.
Essential Imaging Modalities
A comprehensive imaging protocol is mandatory. This includes orthogonal plain radiography, Computed Tomography (CT), and Magnetic Resonance Imaging (MRI) of the entire femur, hip, and knee joints.
* Plain Radiography and CT: Utilized to define the geometry of cortical destruction, assess bone stock for prosthetic fixation, and measure the medullary canal diameter.
* MRI: The gold standard for evaluating the intramedullary extent of the tumor, assessing extraosseous soft tissue mass, determining the proximity to the neurovascular bundle (femoral and sciatic nerves, femoral vessels), and ruling out skip metastases within the femoral canal or transarticular spread into the acetabulum.
Angiography and Preoperative Embolization
Angiography of the iliofemoral axis is critical when evaluating large proximal femoral tumors. Vascular displacement is frequent with medial extraosseous extension. The profunda femoris is particularly susceptible to encasement. If ligation is anticipated, SFA patency must be confirmed.
Preoperative embolization is an invaluable adjunct, particularly for hypervascular metastatic lesions (e.g., renal cell carcinoma, thyroid carcinoma). Embolization performed 24 to 48 hours prior to surgery significantly diminishes intraoperative blood loss, mitigating the risk of catastrophic exsanguination during surgical exposure and tumor mobilization.

Detailed Surgical Approach and Technique
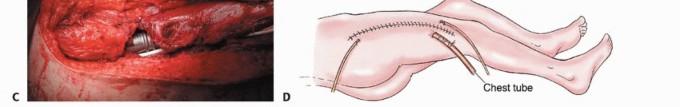
Limb-sparing surgery involving massive endoprosthetic replacement is executed in three distinct phases: oncologic tumor resection, endoprosthetic reconstruction, and meticulous soft tissue reconstruction.
Patient Positioning and Incision
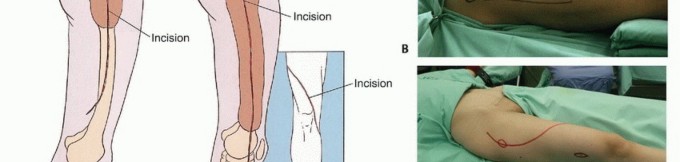
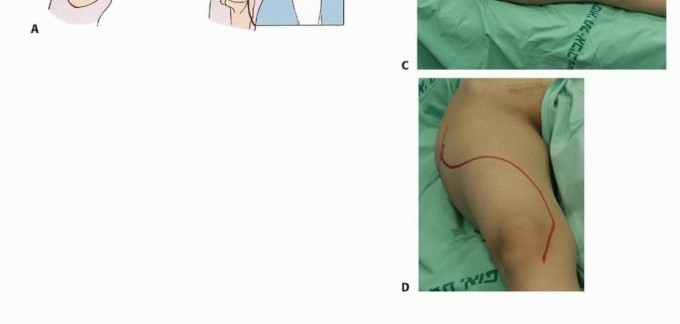
The patient is positioned in the lateral decubitus position. A standard extensile lateral approach is utilized. The incision begins 3 to 4 cm proximal to the greater trochanter, extending distally along the lateral thigh. For total femur resections, the incision is extended distally to the anterolateral aspect of the patellar tendon and tibial tuberosity.
If the tumor exhibits massive medial soft tissue extension, an ilioinguinal extension may be required proximally to gain control of the external iliac/common femoral vessels. Distally, if the tumor extends toward the popliteal fossa, a medially curved incision may be necessary to facilitate delicate dissection of the popliteal vessels.
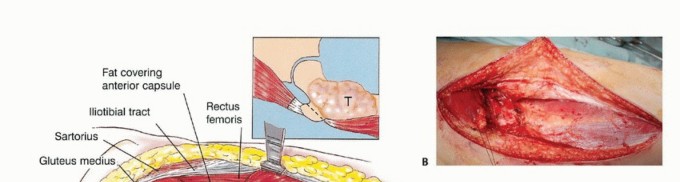
Gluteus Medius and Maximus Detachment
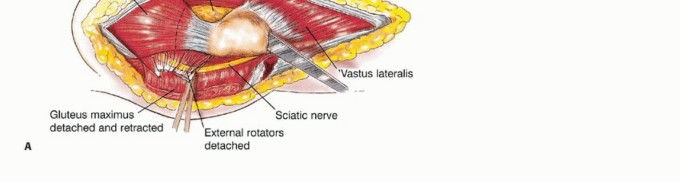
The iliotibial band is incised longitudinally. The gluteus maximus is identified, and its femoral insertion is partially detached to allow posterior reflection. This maneuver exposes the retrogluteal space, external rotators, sciatic nerve, abductors, and the posterior hip capsule. The first perforating artery, intimately associated with the gluteal insertion, must be identified and ligated.
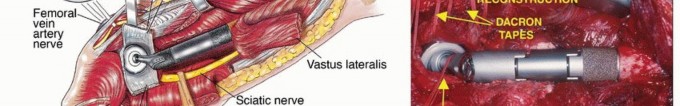
The sciatic nerve, lying directly posterior to the short external rotators, must be identified early. In the presence of a large primary bone sarcoma, the external rotators are often displaced posteriorly, acting as a biologic barrier protecting the nerve. Consequently, the sciatic nerve may be anatomically distorted; it must be neurolysed and mobilized safely out of the resection bed.
If the greater trochanter is free of tumor, a trochanteric osteotomy may be performed to preserve the abductor insertion. If involved, the abductors (gluteus medius and minimus) are transected through their tendinous insertions and tagged for later reconstruction.
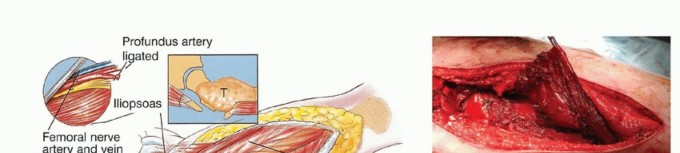
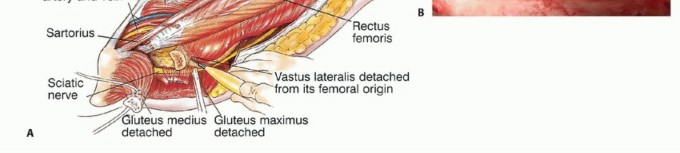
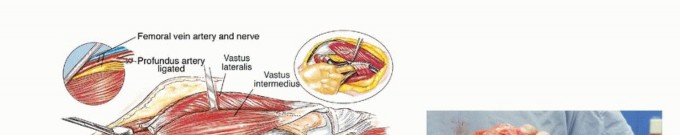
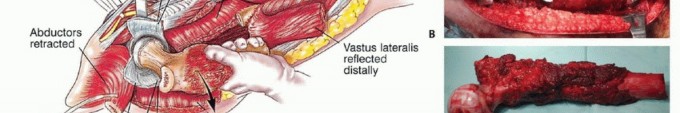
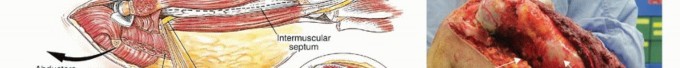
Vastus Lateralis Reflection
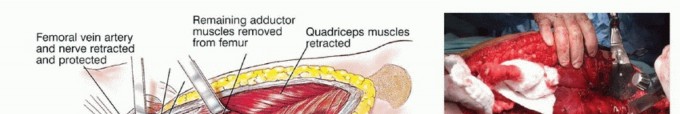
The vastus lateralis is elevated from its origin at the vastus ridge and reflected anteriorly and distally. The posterior perforating vessels from the profunda femoris are systematically identified and ligated. Preservation of the vastus lateralis muscle belly is critical, as it provides the primary soft tissue coverage for the metallic prosthesis and is advanced proximally during closure to reinforce the abductor mechanism. Care must be taken to protect its main neurovascular pedicle (descending branch of the lateral circumflex femoral artery and branches of the femoral nerve), which courses obliquely along the deep fascia of the rectus femoris.
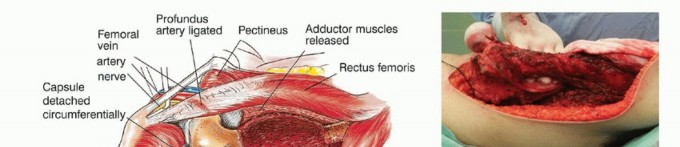
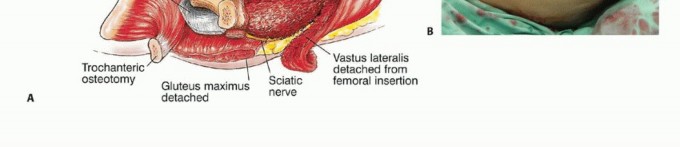
Detachment of Posterior Hip Musculature and Capsule
The short external rotators are detached en bloc approximately 1 cm from their insertion on the proximal femur. If the hip capsule is oncologically safe, it is preserved to aid in postoperative hip stability. The capsule is incised longitudinally along its anterolateral aspect and detached circumferentially from the femoral neck. The hip is then dislocated anterolaterally. Extreme caution is exercised to avoid an iatrogenic femoral neck fracture during dislocation, which could contaminate the surgical field with tumor cells.
For total femur resections requiring an anterolateral knee arthrotomy, the cruciate ligaments, collateral ligaments, and menisci are resected en bloc with
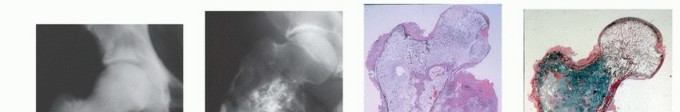
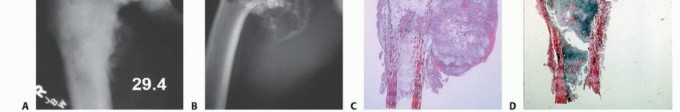
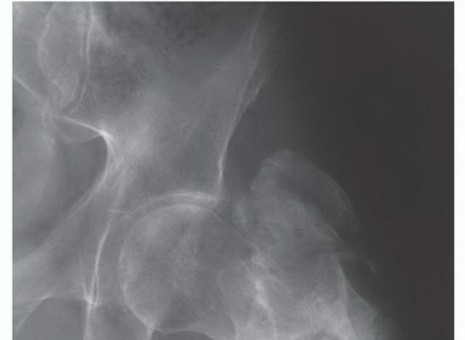
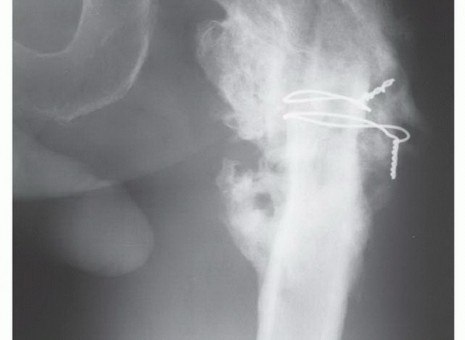
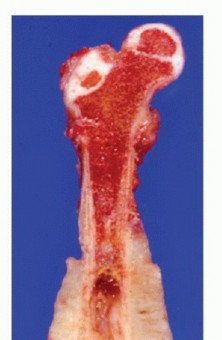
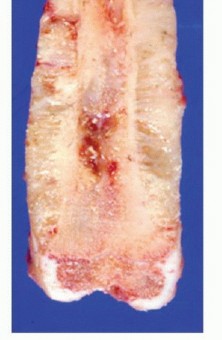
Clinical & Radiographic Imaging
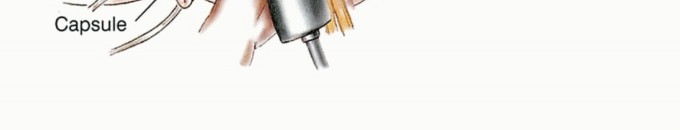
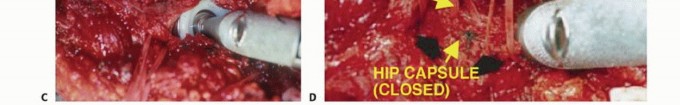

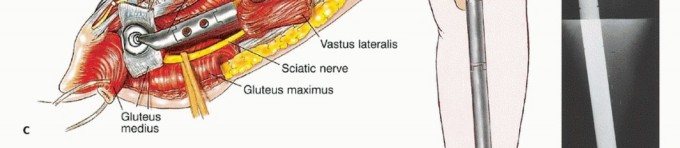



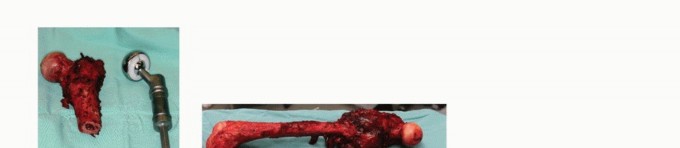



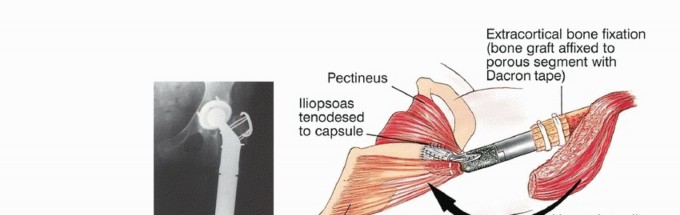


References
- Bickels J, Meller I, Henshaw RM, et al. Reconstruction of hip joint stability after proximal and total femur resections. Clin Orthop Relat Res 2000;(375):218-230. 2. Enneking WF, Shirley PD. Resection-arthrodesis for malignant and potentially malignant lesions about the knee using an intramedullary rod and local bone graft. J Bone Joint Surg 1977;59(2):223-236. 3. Freedman EL, Eckardt JJ. A modular endoprosthetic system for tumor and non-tumor reconstructions: preliminary experience. Orthopedics 1997;20:27-36. 4. Friesecke C, Plutat J, Block A. Revision arthroplasty with the use of a total femur prosthesis. J Bone Joint Surg 2005;87(12):2693-2701. 5. Hejna MJ, Gitelis S. Allograft prosthetic composite reconstruction for bone tumors. Semin Surg Oncol 1997;13:18-24. 6. Mankin HJ, Gebhardt MC, Jennings LC, et al. Long-term results of allograft replacement in the management of bone tumors. Clin Orthop Relat Res 1996;(324):86-97. 7. Ottolenghi CE. Massive osteoarticular bone grafts. Transplant of the whole femur. J Bone Joint Surg 1966;48(4):646-659. 8. Zehr RJ, Enneking WF, Scarborough MT. Allograft-prosthetic composite versus megaprosthesis in proximal femoral reconstruction. Clin Orthop Relat Res 1996;(322):207-223.
Detailed Chapters & Topics
Dive deeper into specialized chapters regarding proximal-and-total-femur-resection-with-endoprosthetic-reconstruction
