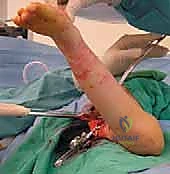
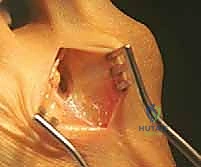
Proximal Tibia Resection With Endoprosthetic Reconstruction
Introduction and Epidemiology
Resection of the proximal tibia for primary bone sarcomas or aggressive benign osseous lesions represents one of the most formidable technical challenges in orthopedic oncology. The procedure typically mandates the wide en bloc removal of one-half to two-thirds of the proximal tibia. This extensive resection inherently includes a portion of all muscular insertions on the proximal tibia, the entire popliteus muscle, and an extra-articular resection of the proximal tibiofibular joint. Concurrently, the common peroneal nerve must be meticulously neurolysed and preserved. Of all anatomic locations necessitating major segmental bone resections and endoprosthetic reconstructions, the proximal tibia is universally recognized as the site where surgical intervention is the most complex, where postoperative complication rates are highest, and where functional outcomes are generally inferior when compared to distal femoral or proximal femoral reconstructions.
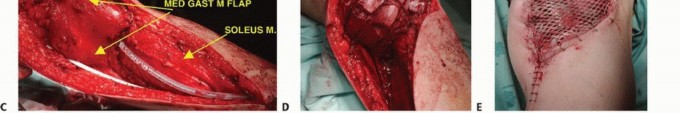
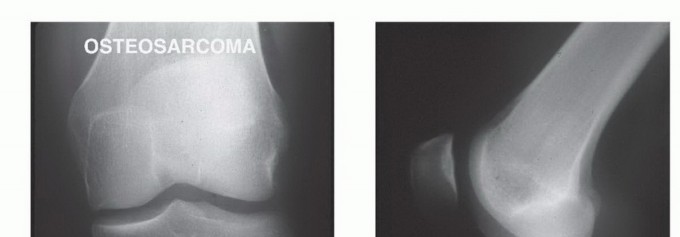
The primary contributors to these elevated complication rates are multifactorial. They include the inherent lack of robust, vascularized muscle coverage along the anteromedial aspect of the tibia, the relatively small caliber and tenuous nature of the trifurcation blood vessels supplying the distal leg, and the absolute oncologic necessity to resect the insertion site of the extensor mechanism (the tibial tubercle) en bloc with the surgical specimen. Primary malignant bone tumors—most notably osteosarcoma, Ewing sarcoma, and chondrosarcoma—frequently arise in the highly active metaphyseal region of the proximal tibia, making it the second most common anatomic site for primary bone sarcomas overall, superseded only by the distal femur.
Evolution of Limb Sparing Surgery
Historically, the profound anatomic and reconstructive difficulties associated with proximal tibial tumors rendered reliable limb-sparing surgery nearly impossible. Consequently, above-knee amputations (AKA) were the definitive and often the sole surgical option for achieving local control of malignant tumors at this site. Over the past four decades, this treatment paradigm has shifted dramatically. This evolution has been propelled by the advent of efficacious neoadjuvant chemotherapy protocols, the development of high-resolution cross-sectional imaging (MRI), and revolutionary advancements in modular endoprosthetic design and biomaterials.
Modern limb-salvage techniques now facilitate a safe, systematic approach to the intricate dissection of the popliteal vessels and the wide resection of the proximal tibia. Reconstructive options have historically included primary arthrodesis, massive osteoarticular allograft replacement, and endoprosthetic reconstruction. In contemporary academic orthopedic oncology, modular rotating-hinge endoprosthetic replacements are strongly preferred. This consensus is driven by the unacceptably high rates of nonunion, allograft fracture, and catastrophic deep periprosthetic infections associated with massive allografts, as well as the profound functional limitations and severe gait deviations inherent to a knee arthrodesis.
Surgical Anatomy and Biomechanics
A profound, three-dimensional understanding of the popliteal fossa, the extensor mechanism, and the proximal leg compartments is mandatory. The margin between a successful limb salvage and a catastrophic complication often rests on millimeter-level precision in these anatomic zones.

Knee Joint and Cruciate Ligaments
The articular compartment of the knee joint is seldom directly invaded by primary metaphyseal tumors of the proximal tibia, as the avascular articular cartilage acts as a relative biologic barrier to tumor propagation. When intra-articular invasion does occur, it is typically the catastrophic result of a pathologic intra-articular fracture, gross contamination from an improperly placed biopsy tract, or direct tumor extension tracking along the synovium or cruciate ligaments. The clinical presence of a hemarthrosis or MRI evidence of joint effusion in the setting of a proximal tibial sarcoma is highly suspicious for intra-articular disease.
Microscopic involvement of the cruciate ligaments is occasionally difficult to definitively ascertain until the time of surgical exploration, although high-resolution, multi-planar MRI remains the most reliable preoperative diagnostic tool. If tumor nodules or abnormal signal intensity are identified within the cruciate ligaments, an extra-articular resection must be executed to achieve negative oncologic margins (R0 resection). An extra-articular resection is defined as the en bloc removal of the proximal tibia, the entire intact joint capsule, the patella, and the distal femoral condyles, necessitating a total knee megaprosthetic reconstruction.
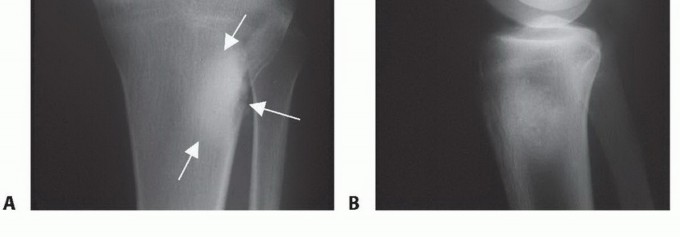
Extensor Mechanism
The extensor mechanism of the knee is the single most critical determinant of postoperative ambulatory function following proximal tibial replacement. The anatomic attachment site of the patellar tendon at the tibial tuberosity must be resected en bloc with the proximal tibia to ensure adequate wide margins, as these tumors frequently extend into the anterior metaphyseal bone directly deep to the tuberosity. Reconstruction of this mechanism is biomechanically essential for a functioning extremity. Failure to achieve a stable, properly tensioned extensor mechanism results in a profound extensor lag, rendering the limb unstable during the stance phase of gait and functionally inferior to a well-fitted above-knee amputation prosthesis.
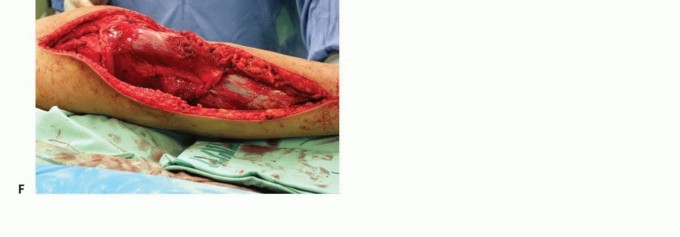
Popliteal Trifurcation
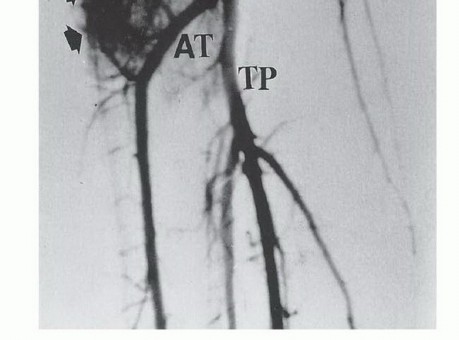
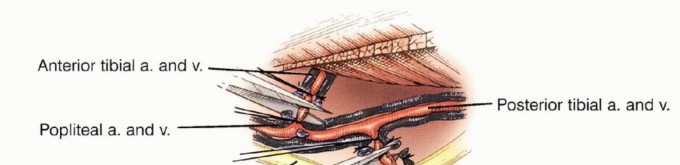
The vascular anatomy immediately posterior to the proximal tibia dictates the technical feasibility of limb salvage. The popliteal artery divides into the anterior tibial artery, the posterior tibial artery, and the peroneal artery at the inferior border of the popliteus muscle. Anatomically, this "trifurcation" is more accurately described as two distinct, sequential bifurcations.
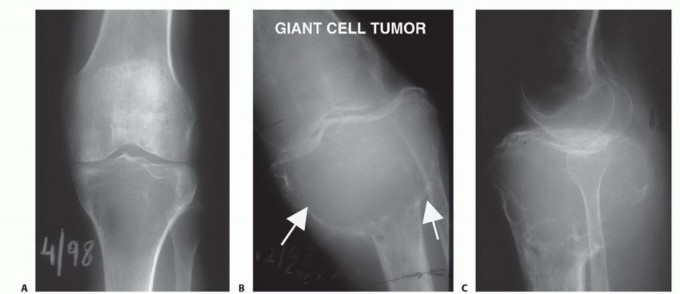
The primary bifurcation occurs where the anterior tibial artery arises from the popliteal artery, which then continues distally as the tibioperoneal trunk. The anterior tibial artery is the first branch, arising precisely at the inferior border of the popliteus muscle and immediately passing anteriorly over the proximal border of the interosseous membrane. The secondary bifurcation occurs where the peroneal artery and the posterior tibial artery diverge from the tibioperoneal trunk. Due to the intimate proximity of the anterior tibial artery to the posterior tibial cortex and its tethering at the interosseous membrane, it is almost universally necessary to ligate and transect the anterior tibial artery at its origin. This maneuver allows the remaining neurovascular bundle to be safely retracted posteriorly, facilitating the oncologic resection of the posterior tibial cortex. Consequently, the posterior tibial and peroneal vessels must be meticulously identified, protected, and preserved to ensure distal limb perfusion and viability.
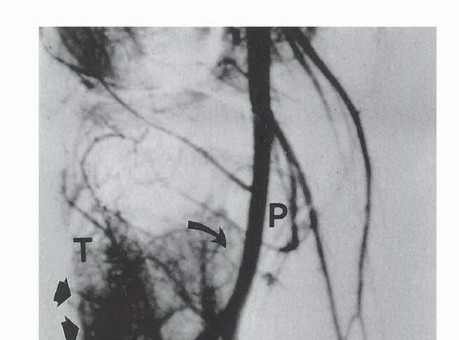
Indications and Contraindications
The decision algorithm for managing complex proximal tibial tumors demands a rigorous multidisciplinary approach, integrating input from orthopedic oncology, medical oncology, musculoskeletal radiology, and pathology. The primary objective is to weigh oncologic safety against anticipated functional outcomes. Limb salvage is considered the standard of care, provided wide (negative) margins can be achieved without compromising the major neurovascular bundle supplying the distal extremity.
| Category | Indications | Contraindications |
|---|---|---|
| Limb-Sparing Surgery (Endoprosthesis) | Primary malignant bone tumors (Osteosarcoma, Ewing sarcoma, Chondrosarcoma) without major neurovascular encasement; Aggressive benign tumors (e.g., Campanacci Grade III Giant Cell Tumor) with massive structural bone destruction; Salvage of failed massive allografts or severe periarticular trauma. | Circumferential encasement of the popliteal artery or tibioperoneal trunk; Direct invasion or encasement of the tibial nerve; Extensive soft tissue contamination from a poorly placed, non-longitudinal biopsy tract; Inability to achieve R0 (negative) margins. |
| Above-Knee Amputation (AKA) | Major neurovascular encasement precluding preservation of a sensate, perfused foot; Massive fungating soft-tissue extensions; Uncontrollable deep periprosthetic infection in a previous limb salvage attempt; Severe baseline peripheral neuropathy or advanced peripheral vascular disease. | Tumors anatomically amenable to wide resection with reliable preservation of the posterior tibial/peroneal vessels and the tibial/common peroneal nerves. |
| Non-Operative Management | Palliative care in patients with overwhelming, widely disseminated metastatic disease and a severely limited life expectancy; Patients physiologically unfit to survive major oncologic surgery due to severe cardiopulmonary comorbidities. | Curable, localized primary bone sarcomas; Impending or actual pathologic fractures in patients with a reasonable life expectancy who would benefit from pain control and mobilization. |
Pre Operative Planning and Patient Positioning
Thorough and exhaustive preoperative planning is the cornerstone of successful limb-sparing surgery. The exact margin of resection, the level of the osteotomy, and the comprehensive reconstructive strategy (including soft tissue coverage) must be entirely formalized before the patient enters the operating theater.
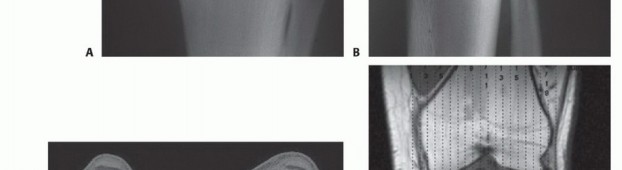
Imaging Modalities
Preoperative evaluation of tumor extent requires a detailed understanding of the cross-sectional anatomy and careful evaluation of multiple imaging modalities.
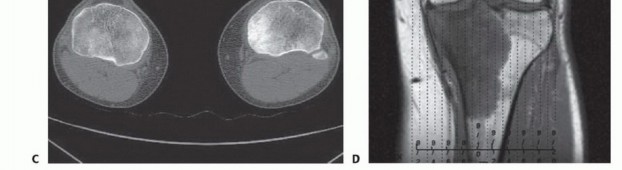
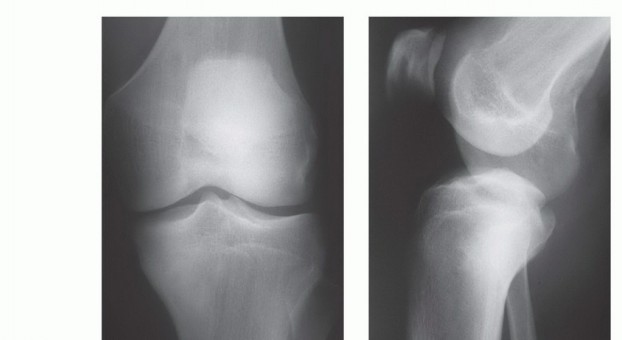
1. Magnetic Resonance Imaging (MRI): The absolute gold standard for evaluating intraosseous tumor extent, identifying skip metastases, and delineating soft tissue extension. T1-weighted longitudinal (coronal and sagittal) images are critical for determining the level of the tibial osteotomy. The osteotomy is typically planned 2 to 3 centimeters distal to the furthest microscopic extent of the marrow replacement/edema to ensure a wide margin. STIR or T2-weighted sequences are essential for evaluating peritumoral edema and potential cruciate ligament or neurovascular involvement.
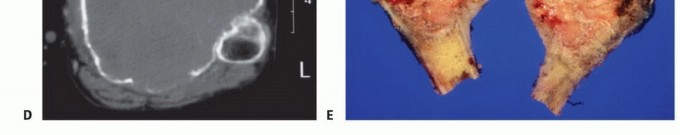
2. Computed Tomography (CT): Provides unparalleled cortical detail and aids in assessing the structural integrity of the tibial plateau, the proximal tibiofibular joint, and the presence of pathologic microfractures. High-resolution CT of the chest is mandatory for systemic staging (pulmonary metastasis screening).
3. Biplane Angiography or CT Angiography (CTA): Highly recommended for mapping the popliteal trifurcation. Because the anterior tibial artery will likely be ligated during the resection, the surgeon must definitively confirm the patency and adequate flow through the posterior tibial and peroneal arteries to prevent postoperative distal limb ischemia.
Patient Positioning and Setup
The patient is positioned supine on a fully radiolucent operating table to allow for unencumbered intraoperative fluoroscopy. A bump is placed under the ipsilateral hip to internally rotate the leg slightly, preventing the natural external rotation of the limb and allowing neutral, ergonomic access to both the medial and lateral aspects of the knee. A sterile pneumatic tourniquet is applied to the proximal thigh but is typically not inflated unless catastrophic, uncontrollable hemorrhage occurs. Continuous visual assessment of distal limb perfusion and venous return is critical during the delicate popliteal dissection. The entire limb, from the iliac crest to the toes, is prepped and draped free. This facilitates full dynamic manipulation of the knee joint and provides unobstructed access for potential autologous vein grafting or local/free flap harvesting.
Detailed Surgical Approach and Technique
The surgical technique for proximal tibial resection is highly demanding, requiring a systematic, phased approach. The surgeon must seamlessly transition between aggressive oncologic resection and meticulous reconstructive microsurgical principles to ensure margins are maintained while preserving the neurovascular structures necessary for a viable, functional limb.
Incision and Biopsy Tract Excision
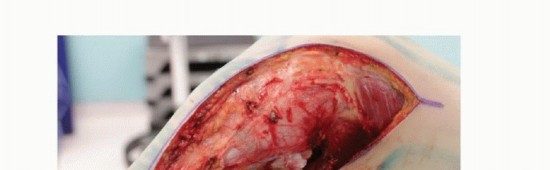
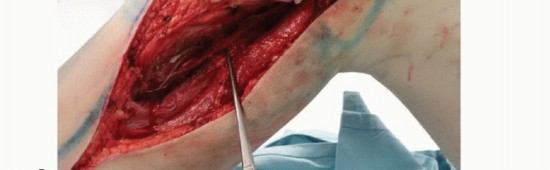
A long, utilitarian anteromedial or midline longitudinal incision is utilized. It is imperative that the previous biopsy tract is incorporated within an ellipse of skin. The biopsy tract must be resected en bloc with the underlying tumor specimen; it is carefully dissected down to the bone and left attached to the anterior tibia to prevent tumor seeding. Full-thickness fasciocutaneous flaps are raised medially and laterally. To maintain the precarious vascularity of these flaps and prevent postoperative marginal necrosis, dissection must proceed deep to the deep fascia wherever oncologically permissible.
Neurovascular Dissection
The deep dissection typically begins laterally to identify, neurolyse, and protect the common peroneal nerve. The nerve is located posterior to the biceps femoris tendon and is traced distally as it winds around the fibular neck. Because the proximal tibiofibular joint is routinely resected en bloc with the tibia, the peroneal nerve must be mobilized extensively. The anterior tibial recurrent artery and the muscular branches supplying the anterior compartment are ligated to allow the nerve to be safely retracted laterally out of the resection field.

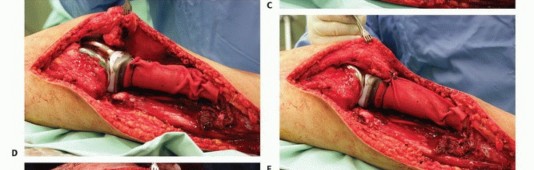
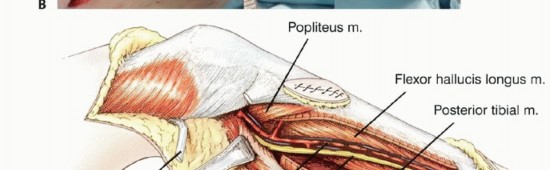
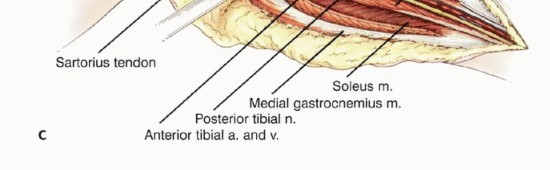
Attention is then turned to the medial aspect of the knee. The pes anserinus is identified and transected, leaving a sufficient cuff for potential soft tissue repair if it is not involved by the tumor. The medial head of the gastrocnemius is retracted posteriorly, exposing the popliteal neurovascular bundle. The popliteal artery and vein are mobilized from the posterior capsule of the knee and the popliteus muscle, utilizing vessel loops for gentle retraction.
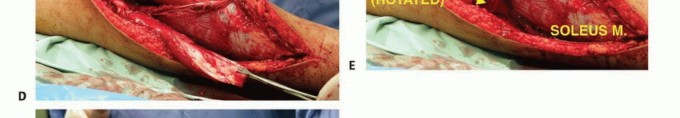
The dissection proceeds distally to carefully expose the popliteal trifurcation. The anterior tibial artery is identified as it dives anteriorly above the proximal border of the interosseous membrane. As noted previously, the anterior tibial artery is double-ligated and transected at its origin. This critical step allows the entire neurovascular bundle to fall posteriorly, completely away from the posterior tibial cortex, thereby facilitating a safe transverse osteotomy and en bloc resection without vascular injury.
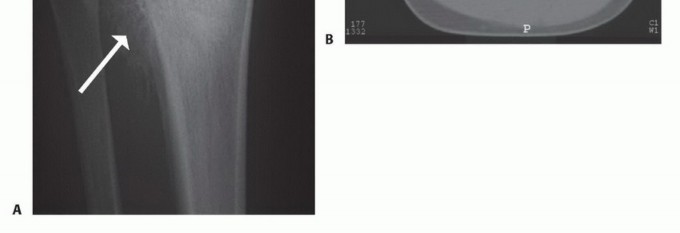
Osteotomy and Tumor Resection
The exact level of the tibial osteotomy is marked using a sterile ruler based on preoperative MRI measurements. A step-cut or transverse osteotomy is performed using a heavy-duty oscillating saw, with the surrounding soft tissues protected by broad retractors. The interosseous membrane is divided longitudinally. The fibula is osteotomized distal to the proximal tibiofibular joint, ensuring the peroneal nerve is completely protected.
The extensor mechanism is transected by dividing the patellar tendon near its insertion. If the articular joint is spared (intra-articular resection), a standard arthrotomy is performed, and the collateral and cruciate ligaments are divided at their tibial insertions. If an extra-articular resection is indicated due to cruciate involvement or joint contamination, the distal femur is osteotomized, and the entire joint capsule is kept completely intact. The specimen is then carefully elevated, dissecting the remaining posterior soft tissue attachments off the popliteus and soleus muscles while keeping the neurovascular bundle under direct, continuous vision.
Prosthetic Reconstruction
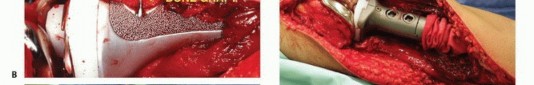
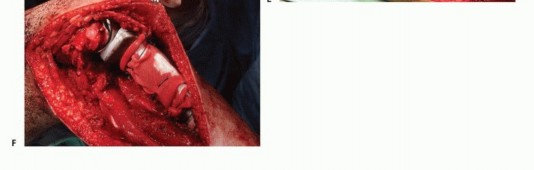
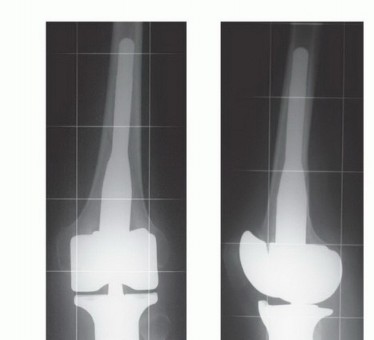
Following the extirpation of the tumor, the tibial and femoral intramedullary canals are sequentially reamed. A rotating hinge knee endoprosthesis is the implant of choice, as it provides intrinsic coronal and sagittal stability in the complete absence of collateral and cruciate ligaments. The modular tibial component is cemented into the remaining distal tibial diaphysis, and the femoral component is cemented into the distal femur. Meticulous attention is paid to the rotational alignment of the tibial tray; external rotation of the tibial component must be optimized to ensure proper tracking of the reconstructed extensor mechanism and to prevent patellar subluxation.
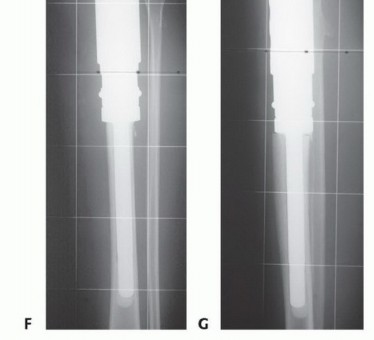
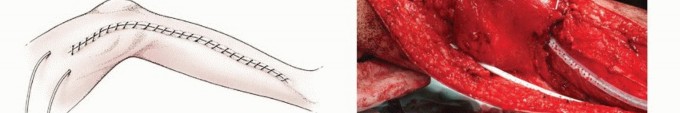
Reconstruction of the extensor mechanism is arguably the most critical biomechanical step of the operation. The remaining native patellar tendon is typically sutured with heavy non-absorbable sutures to a synthetic mesh (such as a Trevira tube or Marlex mesh) that is mechanically secured to the proximal tibial prosthesis.
Soft Tissue Coverage and the Gastrocnemius Flap
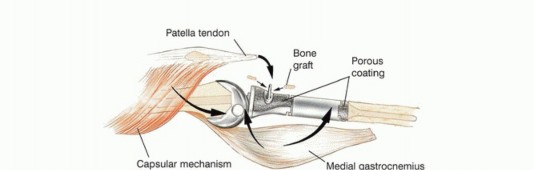
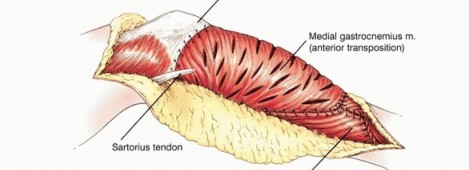
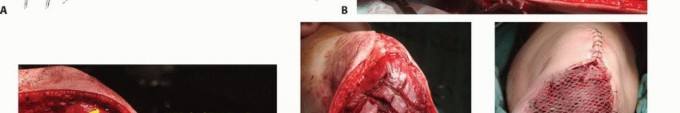
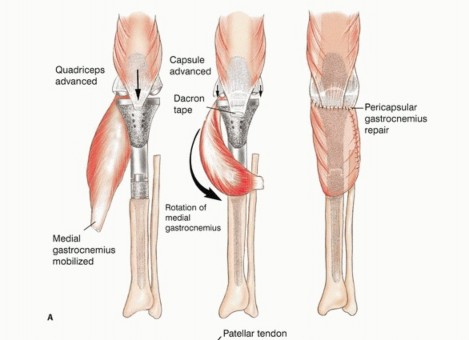
The utilization of a medial gastrocnemius rotational flap is a mandatory, non-negotiable factor in achieving adequate soft tissue coverage over the massive metallic prosthesis and in restoring the biologic function of the extensor mechanism. The absolute lack of native muscle coverage along the anteromedial aspect of the tibia makes catastrophic skin necrosis and subsequent deep prosthetic infection highly probable if a vascularized muscle flap is not utilized.
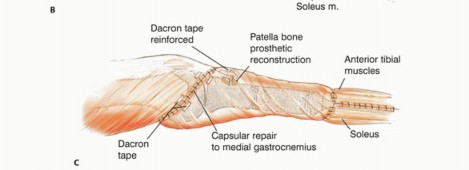
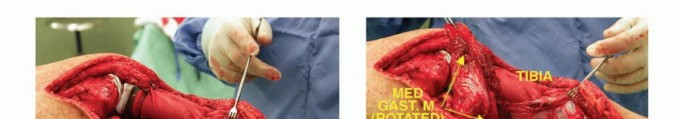
The medial head of the gastrocnemius is carefully detached from its femoral origin, meticulously preserving its primary neurovascular pedicle (the medial sural artery and vein). The muscle belly is rotated anteriorly to completely cover the proximal tibial prosthesis and the synthetic extensor mesh. The patellar tendon and the synthetic mesh are sutured directly into the robust, vascularized fascial surface of the gastrocnemius flap. This technique not only provides a highly vascularized envelope to thwart infection but also biologically augments the extensor mechanism reconstruction, allowing for robust fibrovascular ingrowth and significantly improved long-term mechanical stability.
Complications and Management
The complication profile for proximal tibial megaprosthetic replacements is historically the highest among all major joint endoprostheses utilized in orthopedic oncology. Surgeons must maintain a high index of suspicion and be fully prepared to manage both early wound complications and late catastrophic mechanical failures.
| Complication | Incidence | Etiology and Management Strategies |
|---|---|---|
| Deep Periprosthetic Infection | 12% - 25% | Driven by the tenuous anterior soft tissue envelope, extensive dead space, and prolonged operative times in immunocompromised (post-chemotherapy) patients. Management requires aggressive two-stage revision with articulating antibiotic cement spacers. If functional soft tissue cannot be restored, above-knee amputation is the ultimate, life-saving salvage. |
| Extensor Mechanism Failure | 10% - 20% | Results from mechanical avulsion of the patellar tendon from the prosthesis or failure of the synthetic mesh integration. Presents clinically as a profound, debilitating extensor lag. Treatment involves complex revision of the extensor mechanism repair, often requiring Achilles tendon allograft augmentation and revision of the gastrocnemius flap. |
| Aseptic Loosening |
Clinical & Radiographic Imaging

You Might Also Like