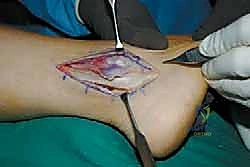
Mastering Deltoid Ligament Reconstruction: An Intraoperative Guide
Key Takeaway
This masterclass guides orthopaedic fellows through deltoid ligament reconstruction for chronic insufficiency, primarily in stage IV AAFD. We cover essential anatomy, meticulous preoperative planning, exact patient positioning, and a step-by-step minimally invasive allograft technique. Critical intraoperative pearls, potential pitfalls, and comprehensive postoperative protocols are emphasized, ensuring optimal outcomes for complex medial ankle instability.
Introduction and Epidemiology
Deltoid ligament deficiency is present when both the deep and superficial components of the medial collateral ligament complex of the ankle are ruptured or structurally insufficient. While acute disruptions frequently occur in the setting of supination-external rotation (SER) ankle fractures, chronic deltoid ligament insufficiency is most commonly encountered as a late-stage manifestation of adult acquired flatfoot deformity (AAFD), recently reclassified as progressive collapsing foot deformity (PCFD).

The transition from Stage III to Stage IV AAFD marks a critical biomechanical failure. As the posterior tibial tendon (PTT) becomes deficient, the dynamic ability to invert the hindfoot is lost. Consequently, the mechanical axis of the lower extremity shifts medially relative to the foot. As the hindfoot deformity progresses into severe, rigid valgus, eccentric tension increases exponentially on the medial ankle soft tissues. The medial collateral ligament complex ultimately fails to resist these loads, leading to progressive attenuation, elongation, and eventual incompetence.

Progression to Stage IV AAFD is defined by the moment the deltoid ligament becomes functionally incompetent, allowing the valgus vector from the preexisting hindfoot deformity to cause the talus to tilt into valgus within the ankle mortise. This talar tilt fundamentally alters tibiotalar contact mechanics, accelerating asymmetric cartilage wear and leading to end-stage ankle arthropathy if left untreated. Deltoid ligament reconstruction in this setting aims to restore the anatomic restraints of the medial ankle, realign the tibiotalar joint, and prevent the progression to obligate tibiotalar arthrodesis.
Surgical Anatomy and Biomechanics
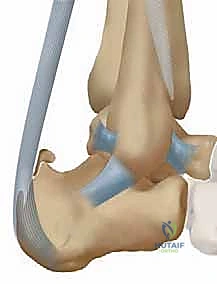
The deltoid ligament complex is a robust, multiunit structure providing critical static support and restraint for the tibiotalar joint, subtalar joint, spring ligament complex, and talonavicular joint. The complex is broadly divided into deep and superficial components, each with distinct anatomic origins, insertions, and biomechanical roles.
Superficial Deltoid Ligament Complex
The superficial layer primarily resists hindfoot eversion and valgus tilting of the talus. It originates from the anterior colliculus of the medial malleolus and fans out distally. According to the detailed anatomic studies by Pankovich and Shivaram, the superficial layer comprises three distinct bands:
1. Tibionavicular Ligament: The most anterior component, inserting onto the dorsal and medial aspects of the navicular tuberosity. It blends intimately with the superomedial calcaneonavicular (spring) ligament.
2. Tibiocalcaneal Ligament: Descends vertically to insert onto the sustentaculum tali of the calcaneus.
3. Superficial Tibiotalar Ligament: The most posterior component of the superficial layer, inserting onto the medial tubercle of the posterior process of the talus.

Deep Deltoid Ligament Complex
The deep portion of the complex is the primary restraint to external rotation and lateral translation of the talus within the mortise. It originates from the intercollicular groove and the posterior colliculus of the medial malleolus.
1. Anterior Tibiotalar Ligament (ATTL): Consists of short, stout fibers that are intra-articular but extrasynovial.
2. Posterior Tibiotalar Ligament (PTTL): The thickest and strongest component of the entire deltoid complex, inserting onto the medial face of the talar body near the center of rotation of the tibiotalar joint.

Pathomechanics of Insufficiency
In the setting of PCFD, the superficial deltoid ligament typically attenuates first due to chronic hindfoot valgus. Once the superficial restraints fail, the deep deltoid ligament is subjected to abnormal external rotation and lateral translation forces. The subsequent failure of the deep deltoid allows the talus to tilt into valgus and translate laterally, clinically manifesting as Stage IV AAFD. Restoration of both the deep and superficial components is therefore biomechanically imperative when undertaking anatomic reconstruction.

Clinical Presentation and Evaluation
Patients with Stage IV AAFD present with profound medial column collapse and severe hindfoot valgus. Due to the chronic nature of PTT involvement, inversion strength is absent. The patient cannot actively bring the forefoot across the midline or perform a single-limb heel rise.
Because of the decreased working length of the triceps surae resulting from chronic hindfoot valgus, a severe equinus contracture is universally present. The Silfverskiöld test is mandatory to differentiate between isolated gastrocnemius contracture and combined Achilles tendon contracture, dictating the choice of posterior lengthening procedure.

Clinically, the medial malleolus may appear prominent, and patients often report medial ankle pain secondary to deltoid attenuation and medial gutter impingement, or lateral pain due to subfibular impingement as the calcaneus abducts and abuts the lateral malleolus.
Indications and Contraindications
Deltoid ligament reconstruction is specifically indicated for flexible Stage IV AAFD (Stage IVa), where the tibiotalar joint can be passively reduced to a neutral alignment and significant osteoarthritic changes have not yet developed. It is rarely performed in isolation; it must be coupled with extra-articular osteotomies and tendon transfers to correct the underlying structural deformity that led to the ligamentous failure.

Rigid deformities with fixed talar tilt (Stage IVb) or significant tibiotalar arthritis are absolute contraindications for joint-sparing reconstruction and require tibiotalocalcaneal (TTC) arthrodesis.
| Parameter | Operative Indications (Joint-Sparing) | Non-Operative or Arthrodesis Indications |
|---|---|---|
| Tibiotalar Alignment | Reducible talar tilt on weight-bearing views | Fixed, rigid talar tilt |
| Joint Cartilage | Preserved tibiotalar joint space | Bone-on-bone arthritis (Requires Arthrodesis) |
| Hindfoot Flexibility | Supple subtalar joint (allows correction) | Rigid subtalar joint (Requires Triple/Subtalar Fusion) |
| Patient Physiology | Adequate vascularity, non-diabetic/controlled | Charcot neuroarthropathy, active infection |
| Soft Tissue Envelope | Intact medial skin without ulceration | Medial ulceration, severe venous stasis |
Pre Operative Planning and Patient Positioning
Imaging Protocol
Standard weight-bearing radiographs of the foot and ankle are the cornerstone of preoperative planning.
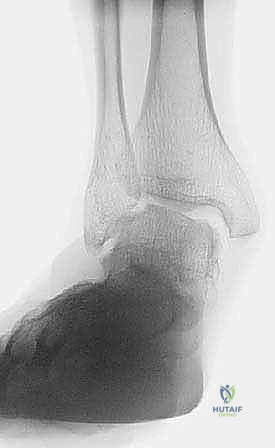
* Anteroposterior (AP) Ankle: Evaluates the degree of talar tilt and lateral translation of the talus. The medial clear space will be widened.
* Lateral Foot: Demonstrates talonavicular uncoverage, lowering of the calcaneal pitch, and Meary's angle disruption.
* Hindfoot Alignment View: Quantifies the degree of hindfoot valgus offset.

Advanced imaging is highly recommended. Magnetic Resonance Imaging (MRI) is utilized to assess the structural integrity of the PTT, spring ligament, and deltoid complex, as well as to evaluate for focal chondral defects in the tibiotalar joint. Weight-bearing Computed Tomography (WBCT) is increasingly utilized to provide a three-dimensional assessment of peritalar subluxation, bone stock for tunnel placement, and subtle osteoarthritic changes.

Patient Positioning
The patient is positioned supine on the operating table. A bump is placed under the ipsilateral hip to internally rotate the leg until the patella points directly toward the ceiling, neutralizing the natural external rotation of the lower extremity. This provides orthogonal access to the medial ankle.

A well-padded thigh tourniquet is applied. The limb is prepped and draped in standard sterile fashion. A sterile bump or triangle may be placed under the calf to allow the heel to hang free, facilitating intraoperative fluoroscopy and manipulation of the hindfoot.
Detailed Surgical Approach and Technique
Deltoid ligament reconstruction requires meticulous dissection and precise isometric tunnel placement. The procedure is almost universally performed in conjunction with a medializing calcaneal osteotomy (MCO), flexor digitorum longus (FDL) transfer, and posterior lengthening (gastrocnemius recession or Achilles lengthening). The deltoid reconstruction is typically performed after the bony correction of the hindfoot has been provisionally or definitively fixed, as restoring the mechanical axis removes the deforming valgus force from the medial repair.

Incision and Superficial Dissection
A curvilinear incision is made over the medial aspect of the ankle, beginning approximately 4 cm proximal to the tip of the medial malleolus, extending distally along the course of the PTT, and curving toward the navicular tuberosity.
Careful subcutaneous dissection is required to identify and protect the saphenous nerve and great saphenous vein, which typically cross the operative field in the proximal aspect of the incision. The flexor retinaculum is incised, and the PTT is inspected. In Stage IV AAFD, the PTT is often severely degenerated or completely ruptured. The tendon is debrided or excised as necessary, preparing the bed for the subsequent FDL transfer.

Deep Dissection and Joint Inspection
The remnants of the superficial deltoid ligament are incised longitudinally to expose the medial malleolus and the medial aspect of the talus. An anteromedial arthrotomy is performed to inspect the tibiotalar joint. The surgeon must confirm that the articular cartilage is viable and that the talus can be concentrically reduced within the mortise without excessive force. Any medial gutter osteophytes that may block reduction are excised.

Graft Selection and Preparation
Reconstruction can be performed using autograft (e.g., plantaris, split tibialis anterior, or harvested semitendinosus) or allograft (e.g., semitendinosus or peroneus longus). Recent advancements also support the use of synthetic suture tape augmentation (internal bracing) either alone or in conjunction with a tendon graft to provide immediate mechanical strength and protect the biologic graft during incorporation.
The selected graft is sized, and the ends are whipstitched with high-strength non-absorbable suture. A graft diameter of 4.5 to 5.5 mm is typically sufficient.

Bone Tunnel Preparation
The success of the reconstruction relies on anatomic tunnel placement to recreate the vectors of the deep and superficial deltoid components.
- Medial Malleolar Tunnels: Two blind-ended tunnels or a single transosseous tunnel are created in the medial malleolus. For a two-tunnel technique, the anterior tunnel is placed in the anterior colliculus (recreating the superficial deltoid origin), and the posterior tunnel is placed in the intercollicular groove (recreating the deep deltoid origin).
- Talar Tunnel: A guide pin is directed from the anatomic insertion of the deep deltoid on the medial talar body, aiming laterally and slightly anteriorly to avoid penetrating the posterior subtalar joint. A 4.5 mm or 5.0 mm reamer is used to create a blind tunnel approximately 15-20 mm deep.
- Calcaneal Tunnel: To reconstruct the tibiocalcaneal band of the superficial deltoid, a tunnel is drilled into the sustentaculum tali. The trajectory must be carefully monitored under fluoroscopy to avoid violating the subtalar joint articular surface.

Graft Passage and Fixation
The graft is first secured in the talar tunnel using a biocomposite interference screw. This anchors the deep deltoid reconstruction. The graft is then passed proximally into the posterior medial malleolar tunnel, tensioned, and secured with a second interference screw.

The remaining limb of the graft is then routed distally from the anterior medial malleolar tunnel down to the sustentaculum tali tunnel to recreate the superficial deltoid.
Critical Tensioning Step: The graft must be tensioned with the ankle in neutral dorsiflexion and the hindfoot held in slight varus (approximately 5 degrees) to ensure the talus is fully reduced within the mortise. Fixation in the calcaneus is achieved with a final interference screw or suture anchor.

Intraoperative fluoroscopy is utilized to confirm concentric reduction of the tibiotalar joint, resolution of the talar tilt, and appropriate hardware placement without intra-articular penetration.
Complications and Management
Surgical management of Stage IV AAFD via deltoid reconstruction is complex and carries a significant complication profile. Precise execution of concomitant bony procedures is required to protect the ligamentous reconstruction from failure.

Common Complications
- Recurrent Deformity: The most common mode of failure is recurrent talar tilt and hindfoot valgus. This typically occurs if the underlying bony deformity (e.g., severe forefoot abduction or inadequate medialization of the calcaneus) is undercorrected, placing excessive stress on the graft.
- Ankle Stiffness: Over-tensioning the graft, particularly the deep deltoid component, can lead to restricted tibiotalar motion, specifically a loss of plantarflexion and external rotation.
- Nerve Injury: The saphenous nerve is highly vulnerable during the medial approach. Neuroma formation can lead to debilitating chronic medial ankle pain.
- Hardware Prominence: Interference screws or suture anchors in the medial malleolus can cause soft tissue irritation due to the thin subcutaneous envelope in this region.

Complication Incidence and Salvage Strategies
| Complication | Estimated Incidence | Prevention Strategy | Salvage Management |
|---|---|---|---|
| Recurrent Talar Tilt / Valgus | 10 - 15% | Ensure adequate bony correction (MCO, Cotton); use robust graft | Revision to Tibiotalocalcaneal (TTC) Arthrodesis |
| Ankle Stiffness | 15 - 20% | Tension graft in neutral dorsiflexion, avoid over-constraining | Aggressive physical therapy; rarely arthroscopic debridement |
| Saphenous Nerve Injury | 5 - 10% | Meticulous superficial dissection; avoid aggressive retraction | Gabapentinoids; targeted nerve block; surgical neurectomy |
| Hardware Prominence | 5 - 8% | Countersink screws completely; use low-profile anchors | Hardware removal after graft incorporation (post 6 months) |
| Nonunion of Osteotomies | 2 - 5% | Rigid internal fixation; optimize host biology (smoking cessation) | Revision internal fixation with bone grafting |
Post Operative Rehabilitation Protocols
The postoperative rehabilitation protocol must balance the need for soft tissue healing and graft incorporation with the prevention of debilitating ankle stiffness.
Phase 1: Maximum Protection (Weeks 0 - 6)
- Weight Bearing: Strictly Non-Weight Bearing (NWB).
- Immobilization: The patient is placed in a well-padded short leg splint in neutral dorsiflexion and slight varus for the first 2 weeks. At the first postoperative visit, sutures are removed, and the patient is transitioned to a fiberglass short leg cast or a locked Controlled Ankle Motion (CAM) boot.
- Goals: Edema control, wound healing, protection of the graft and osteotomies.
Phase 2: Progressive Loading (Weeks 6 - 10)
- Weight Bearing: Initiate progressive partial weight-bearing in the CAM boot, advancing to full weight-bearing as tolerated by week 8-10.
- Immobilization: CAM boot at all times when weight-bearing.
- Physical Therapy: Begin active and active-assisted range of motion (ROM) out of the boot. Focus on sagittal plane motion (dorsiflexion/plantarflexion). Avoid aggressive passive eversion or external rotation that could stretch the reconstruction.
Phase 3: Strengthening and Weaning (Weeks 10 - 16)
- Weight Bearing: Full weight-bearing.
- Immobilization: Transition from the CAM boot to a supportive athletic shoe with a custom medial posting orthotic or an articulated ankle-foot orthosis (AFO) to support the medial column.
- Physical Therapy: Initiate closed-chain strengthening, proprioceptive training, and gentle isometric strengthening of the FDL transfer.
Phase 4: Return to Activity (Months 4 - 6+)
- Patients may gradually return to low-impact activities (cycling, swimming). High-impact activities and sports involving rapid changes of direction are generally discouraged to ensure the long-term longevity of the joint-sparing reconstruction. Maximal medical improvement is typically achieved between 9 and 12 months postoperatively.
Summary of Key Literature and Guidelines
The paradigm of treating Stage IV AAFD has shifted significantly over the last two decades. Historically, talar tilt in the setting of PTTD was considered an absolute indication for tibiotalocalcaneal (TTC) arthrodesis.
Pioneering work by Hintermann and colleagues demonstrated that the deltoid ligament could be anatomically reconstructed using tendon allografts, effectively restoring the medial restraints of the ankle. Their long-term cohort studies indicated that if the tibiotalar articular cartilage is preserved, joint-sparing reconstruction combined with aggressive extra-articular osteotomies yields superior functional outcomes and preserves physiologic gait mechanics compared to pan-talar or TTC fusions.
Current consensus guidelines from the American Orthopaedic Foot & Ankle Society (AOFAS) and the newly proposed Progressive Collapsing Foot Deformity (PCFD) classification system emphasize the
Clinical & Radiographic Imaging



















You Might Also Like