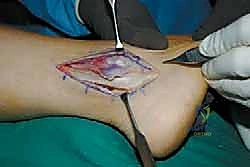
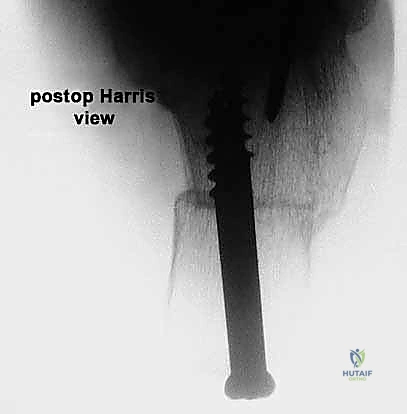
Anatomic Lateral Ankle Ligament Reconstruction: A Masterclass in Plantaris Longus Autograft Technique
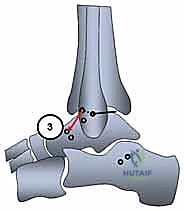
Key Takeaway
Join us in the OR for an immersive masterclass on anatomic lateral ankle ligament reconstruction. We'll meticulously detail the plantaris longus autograft technique, from comprehensive anatomical considerations and precise patient positioning to step-by-step intraoperative execution. Learn critical pearls, pitfalls, and postoperative protocols for optimal outcomes in chronic ankle instability. This guide ensures a thorough understanding of this complex procedure.
Introduction and Epidemiology
Lateral ligament injuries of the ankle are among the most common musculoskeletal pathologies encountered in orthopedic practice, traditionally treated conservatively with favorable outcomes in the majority of cases. However, a significant subset of patients—up to 20% to 30%—will develop chronic ankle instability (CAI) characterized by recurrent ankle sprains, giving way, and persistent pain.

Chronic ankle instability represents a complex interplay of mechanical instability (pathologic laxity) and functional instability (proprioceptive and neuromuscular deficits). Several factors precipitate the progression from an acute sprain to CAI, including inadequate primary immobilization, incomplete ligamentous healing, and repetitive microtrauma that progressively deteriorates localized tissue quality.

The pathogenesis of torn lateral ligaments is inextricably linked to the severity of the initial inversion trauma. The American Medical Association (AMA) standard nomenclature system stratifies these injuries by severity:
* Grade I: Ligament stretched (minimal macroscopic tearing)
* Grade II: Ligament partially torn
* Grade III: Ligament completely torn
Clinically, these are graded by symptom presentation:
* Mild sprain: Minimal functional loss, no limp, minimal swelling, point tenderness.
* Moderate sprain: Moderate functional loss, inability to toe-rise, localized swelling.
* Severe sprain: Diffuse tenderness, profound swelling, requiring ambulatory aids.

With each subsequent ankle sprain, the inherent proprioception of the ankle joint is severely compromised due to the destruction of mechanoreceptors within the ligamentous substance. Epidemiological data indicates that in an uninjured person, an ankle sprain occurs in approximately 1:1,000,000 steps. Following a severe ankle sprain, this risk exponentially increases to 1:1,000 steps. Furthermore, the healing of these ligaments can be biologically compromised by the interposition of synovial fluid between the torn ligament ends and the bony footprint, fundamentally preventing primary tissue bridging.

Surgical intervention is indicated when conservative measures (e.g., structured physical therapy focusing on peroneal strengthening and proprioception) fail. Patients requiring surgical stabilization are broadly divided into two cohorts: those with sufficient tissue quality for a local anatomic repair (e.g., the modified Broström-Gould procedure) and those with inadequate tissue quality necessitating augmentation or anatomic reconstruction. For the latter, the plantaris longus tendon autograft has emerged as a highly efficacious graft choice, offering robust tensile strength without the donor site morbidity associated with peroneal or hamstring harvests.
Surgical Anatomy and Biomechanics
A profound understanding of the lateral ankle ligamentous complex and the plantaris longus anatomy is requisite for executing an anatomic reconstruction. The lateral ankle is primarily stabilized by three distinct ligamentous structures: the anterior talofibular ligament (ATFL), the calcaneofibular ligament (CFL), and the posterior talofibular ligament (PTFL).

Lateral Ligament Complex
The ATFL originates from the anterior margin of the distal fibula and inserts onto the talar body, just anterior to the lateral articular facet. It is a thickening of the joint capsule rather than a distinct extracapsular cord. Biomechanically, the ATFL is the primary restraint to anterior translation of the talus within the mortise, particularly when the ankle is in plantarflexion. It is the weakest of the lateral ligaments and the most frequently injured.

The CFL is an extra-articular, cord-like structure originating from the anterior aspect of the distal fibular tip and inserting onto a small tubercle on the lateral calcaneal surface. It spans both the tibiotalar and subtalar joints. The CFL is the primary restraint to inversion when the ankle is in neutral or dorsiflexion.

The PTFL is the strongest of the three, originating from the malleolar fossa of the fibula and inserting onto the posterior talar tubercle. It is rarely injured except in severe, high-energy trauma or frank dislocations. Additional stability is provided by the osseous architecture; in dorsal extension, the wider anterior dome of the talus becomes locked between the medial and lateral malleoli, conferring maximal mechanical stability.
Plantaris Longus Anatomy
The plantaris muscle originates from the lateral supracondylar ridge of the femur, superior to the lateral head of the gastrocnemius. Its long, slender tendon courses distally and medially between the gastrocnemius and soleus muscles, eventually inserting onto the medial aspect of the calcaneal tuberosity, often blending with the Achilles tendon.

The plantaris tendon is absent in approximately 7% to 20% of the population. When present, it yields a graft of 25 to 35 cm in length, which is exceptionally well-suited for routing through osseous tunnels to reconstruct both the ATFL and CFL simultaneously. Utilizing the plantaris longus preserves the peroneus brevis, thereby maintaining active eversion strength—a critical dynamic stabilizer of the lateral ankle.
Indications and Contraindications
The decision to proceed with an anatomic reconstruction using a plantaris longus autograft, as opposed to a primary Broström repair, hinges on tissue viability, patient anatomy, and physiological demands.

Reconstruction is heavily favored in revision scenarios where a prior local repair has failed. Furthermore, patients with generalized ligamentous laxity (e.g., Ehlers-Danlos syndrome, Marfan syndrome) possess inherently poor collagen cross-linking; a local repair in these patients is highly prone to attenuation and failure. High-demand elite athletes, patients with a high body mass index (BMI), or those with longstanding chronic instability (typically >10 years) where the native ligamentous remnants are completely resorbed or replaced by non-functional scar tissue, are prime candidates for plantaris reconstruction.
Operative vs Non Operative Management
| Management Strategy | Indications | Key Considerations |
|---|---|---|
| Non-Operative | Acute Grade I-III sprains; First-time dislocators without fracture; Low-demand patients; Poor surgical candidates. | Focus on functional rehabilitation, peroneal strengthening, and proprioceptive training (e.g., wobble board). |
| Broström Repair | Chronic instability with adequate native tissue; Failed conservative management; Normal hindfoot alignment. | Gold standard for primary surgical intervention. Often augmented with the extensor retinaculum (Gould modification). |
| Plantaris Reconstruction | Failed prior Broström; Generalized hyperlaxity; Elite athletes; Absent native ligaments; High BMI. | Restores kinematics via anatomic tunnel placement. Preserves peroneal function compared to Evans/Chrisman-Snook procedures. |
Contraindications to reconstruction include severe, end-stage tibiotalar osteoarthritis, active local or systemic infection, and unmanaged Complex Regional Pain Syndrome (CRPS). Crucially, uncorrected hindfoot varus is a strict contraindication to isolated soft-tissue reconstruction. A varus heel drives the mechanical axis laterally, placing insurmountable stress on any lateral ligament reconstruction. In such cases, a lateralizing calcaneal osteotomy must be performed concomitantly.
Pre Operative Planning and Patient Positioning
Thorough preoperative clinical and radiographic evaluation is mandatory to ensure the success of a plantaris longus tendon reconstruction.

Clinical and Radiographic Assessment
Clinical examination must include the anterior drawer test (assessing ATFL integrity) and the talar tilt test (assessing CFL integrity). The Silfverskiöld test is performed to rule out gastrocnemius contracture, which can exacerbate lateral overload.
Standard weight-bearing radiographs (AP, Lateral, Mortise) are obtained to assess for joint space narrowing, osteophytes, and overall alignment. A hindfoot alignment view (Saltzman view) is critical to rule out a varus morphotype. Stress radiography can quantify instability; a talar tilt difference of >10 degrees compared to the contralateral side, or anterior translation >10 mm, is highly suggestive of gross mechanical instability.

Magnetic Resonance Imaging (MRI) without contrast is the gold standard for evaluating the quality of the lateral ligaments. Furthermore, MRI is essential for identifying concomitant intra-articular pathology, such as osteochondral lesions of the talus (OCDs), peroneal tendon tears, or loose bodies, which are present in up to 60% of patients with CAI.
Patient Positioning
The patient is placed in the lateral decubitus position or the supine position with a large bump under the ipsilateral hip to allow for internal rotation of the leg, providing excellent access to the lateral ankle. A thigh tourniquet is applied. The entire limb is prepped and draped to allow access to the posteromedial calf for plantaris harvest and the lateral ankle for the reconstruction.
Detailed Surgical Approach and Technique
The surgical technique for anatomic reconstruction using a plantaris longus autograft requires meticulous attention to anatomic footprints to restore normal joint kinematics without restricting range of motion.
Diagnostic Arthroscopy
Prior to the open procedure, standard anteromedial and anterolateral arthroscopic portals are established. Diagnostic arthroscopy is performed to debride the lateral gutter, remove loose bodies, and address any osteochondral lesions of the talus via microfracture or other cartilage restoration techniques. Synovial hypertrophy, which often impinges in the lateral gutter, is resected.

Plantaris Longus Graft Harvest
The plantaris tendon is typically harvested from the medial aspect of the Achilles tendon insertion. A 2 cm longitudinal incision is made over the posteromedial calcaneus. The plantaris tendon is identified just medial and anterior to the Achilles tendon. It is sharply detached from its insertion and whipstitched. A closed tendon stripper is passed over the tendon, advancing proximally toward the popliteal fossa while maintaining distal tension. Once the muscle belly is reached, the tendon is transected. The graft is then prepared on the back table, cleared of muscle tissue, and tubularized with heavy non-absorbable sutures at both ends.

Lateral Ankle Exposure
A curvilinear incision is made starting posterior to the distal fibula, curving distally and anteriorly toward the sinus tarsi. Care must be taken to identify and protect the superficial peroneal nerve anteriorly and the sural nerve posteriorly. The inferior extensor retinaculum is identified and mobilized for later augmentation.

The joint capsule is incised, and the remnants of the ATFL and CFL are identified. The anatomic footprints on the fibula, talus, and calcaneus are meticulously debrided of soft tissue to expose bleeding cancellous bone, facilitating graft incorporation.
Fibular, Talar, and Calcaneal Tunnel Preparation
Anatomic tunnel placement is the most critical step. Non-anatomic placement alters joint kinematics, leading to stiffness or recurrent instability.

- Fibular Tunnels: Two converging tunnels or a single transosseous tunnel can be utilized. For a two-tunnel technique, the ATFL footprint (anterior border of the distal fibula) and the CFL footprint (distal tip of the fibula) are marked. Drill holes (typically 4.5 mm to 5.0 mm, depending on graft diameter) are created. If a single tunnel is used, it is drilled from the anterior fibula to the distal tip.
- Talar Tunnel: A blind-ending tunnel is drilled at the anatomic footprint of the ATFL on the talar body, aiming posteromedially to avoid penetrating the articular surface of the subtalar or tibiotalar joints.
- Calcaneal Tunnel: A tunnel is drilled at the CFL footprint on the lateral calcaneus, aiming medially and slightly inferiorly.
Graft Passage and Fixation
The prepared plantaris graft is first secured into the talar tunnel using a biocomposite interference screw or a suture anchor.

The graft is then passed beneath the peroneal tendons to accurately replicate the extra-articular course of the native CFL. It is routed into the fibular tunnel(s). Fixation in the fibula is achieved with an interference screw. During fibular fixation, the ankle must be held in neutral dorsiflexion and slight eversion to appropriately tension the ATFL component.

Finally, the remaining tail of the graft is routed into the calcaneal tunnel to reconstruct the CFL. The ankle is held in neutral dorsiflexion and neutral inversion/eversion while the calcaneal interference screw is deployed.
Closure
Following rigid fixation, the construct is tested through a full range of motion to ensure stability and absence of impingement. The inferior extensor retinaculum is mobilized and sutured over the fibula to augment the reconstruction and limit subcutaneous prominence of the graft (Gould modification).

The subcutaneous tissues are closed with absorbable sutures, and the skin is closed with non-absorbable sutures or staples. A sterile dressing and a well-padded short-leg splint in neutral dorsiflexion are applied.
Complications and Management
While anatomic reconstruction yields excellent functional outcomes, the procedure is technically demanding and carries specific risks. Iatrogenic nerve injury remains the most common complication.

Common Surgical Complications
| Complication | Incidence | Etiology | Prevention and Salvage Strategies |
|---|---|---|---|
| Nerve Injury (Sural / SPN) | 5% - 10% | Retraction injury or direct transection during lateral exposure/tunnel drilling. | Meticulous blunt dissection. Avoid excessive retraction. If transected, perform primary repair or bury the proximal stump into muscle to prevent neuroma. |
| Ankle Stiffness | 5% - 8% | Over-tensioning the graft; Non-anatomic tunnel placement (especially fibular tunnels placed too proximally). | Tension the ATFL in neutral dorsiflexion/eversion. Ensure anatomic footprint utilization. Treat with aggressive physiotherapy; rarely requires arthroscopic arthrolysis. |
| Recurrent Instability | 3% - 5% | Failure of graft incorporation; Unrecognized hindfoot varus; Premature return to sport. | Always assess and correct hindfoot varus with a calcaneal osteotomy prior to or during soft tissue reconstruction. Revision requires allograft or synthetic augmentation. |
| Fibular Fracture | < 2% | Tunnels drilled too close together or oversized tunnels in a small fibula. | Maintain at least a 1 cm bone bridge between tunnels. Use appropriately sized drills. If fractured, utilize suture anchor fixation instead of interference screws. |
| Graft Harvest Morbidity | < 1% | Sural nerve irritation at the posteromedial ankle; localized hematoma. | Keep the tendon stripper perfectly aligned with the tendon trajectory. Ensure meticulous hemostasis. |
Post Operative Rehabilitation Protocols
A structured, phased rehabilitation protocol is paramount to allow biological graft incorporation while preventing postoperative stiffness and restoring dynamic neuromuscular control.

Phase I: Protection and Healing (Weeks 0-2)
* The patient is strictly non-weight-bearing (NWB) in a posterior splint or cast.
* The ankle is immobilized in neutral dorsiflexion and slight eversion to minimize tension on the reconstructed ligaments.
* Strict elevation and cryotherapy to manage edema.
Phase II: Controlled Mobilization (Weeks 2-6)
* Sutures are removed at 2 weeks.
* The patient is transitioned to a controlled ankle motion (CAM) boot.
* Weight-bearing is progressively advanced from partial to full weight-bearing as tolerated.
* Active range of motion (ROM) exercises are initiated, focusing strictly on sagittal plane motion (plantarflexion and dorsiflexion). Inversion is strictly prohibited to protect the graft.
Phase III: Strengthening and Proprioception (Weeks 6-12)
* The CAM boot is discontinued, and the patient is transitioned to an ankle lace-up brace for daily activities.
* Aggressive strengthening of the dynamic stabilizers, particularly the peroneus longus and brevis, is initiated.
* Proprioceptive training begins (e.g., single-leg stance, BAPS board, wobble board).
* Closed kinetic chain exercises are advanced.
Phase IV: Return to Sport (Months 3-6)
* Introduction of plyometrics, cutting, and sport-specific drills.
* Clearance for contact sports is typically granted between 4 to 6 months postoperatively, contingent upon symmetrical ROM, >90% strength compared to the contralateral limb, and successful completion of functional hop tests.
Summary of Key Literature and Guidelines
The natural history of untreated chronic ankle instability is well documented in the orthopedic literature. Chronic instability is a definitive risk factor for the development of premature degenerative arthritis of the tibiotalar joint. As demonstrated by Valderrabano et al., there is a significantly increased prevalence of asymmetric, varus-dominant ankle arthritis in patient populations with a history of untreated, recurrent ankle sprains.

Historically, non-anatomic tenodesis procedures (e.g., Evans, Chrisman-Snook, Watson-Jones) were utilized for severe instability. However, long-term follow-up studies have demonstrated that these procedures alter normal hindfoot kinematics, restrict subtalar motion, and inevitably lead to lateral compartment osteoarthritis. Furthermore, they sacrifice the peroneus brevis, weakening active eversion.
Contemporary guidelines strongly advocate for anatomic reconstruction. The utilization of the plantaris longus autograft fulfills these anatomic requirements. Studies evaluating plantaris autografts demonstrate superior load-to-failure rates compared to native ligaments, with functional outcome scores (AOFAS, FAAM) comparable to or exceeding those of hamstring autografts, while entirely avoiding the knee morbidity associated with gracilis or semitendinosus harvest.
In conclusion, plantaris longus tendon reconstruction represents a highly reliable, biomechanically sound surgical strategy for the management of complex chronic ankle instability, provided that meticulous surgical technique is employed and concomitant osseous malalignments are addressed.
Clinical & Radiographic Imaging





















You Might Also Like