Introduction and Epidemiology
Hallux rigidus is defined as degenerative osteoarthritis of the first metatarsophalangeal joint. It represents the most common arthritic condition of the foot and the second most common pathology affecting the first ray, superseded only by hallux valgus. The condition is characterized by progressive loss of sagittal plane motion, particularly dorsiflexion, accompanied by periarticular osteophyte formation and debilitating pain.
The amount of arthritis can range from focal areas of cartilage injury or osteophyte formation without joint space narrowing to ankylosis with complete loss of the joint space. In the classic classification system proposed by Hattrup and Johnson, the radiographic progression is categorized as follows: grade I is osteophyte formation without joint space narrowing, grade II is narrowing of the joint space, and grade III is loss of visible joint space. This has been further expanded by the Coughlin and Shurnas clinical and radiographic grading system, which incorporates objective range of motion deficits and subjective clinical findings to guide surgical decision-making.
Epidemiologically, hallux rigidus affects approximately 2.5% of the population over the age of 50, with a higher prevalence in females. Bilateral involvement is observed in up to 80% of patients with primary osteoarthritis of the first metatarsophalangeal joint. While arthrodesis remains the gold standard for end-stage disease, metatarsophalangeal joint hemiarthroplasty has emerged as a joint-sparing alternative for appropriately selected patients who demand motion preservation.
Surgical Anatomy and Biomechanics
A thorough understanding of the first metatarsophalangeal joint anatomy is paramount for successful surgical intervention. The joint consists of the articulation of the first metatarsal head with the hallux proximal phalanx and the medial and lateral sesamoids. The metatarsal head is convex and asymmetric, being wider plantarly than dorsally, which inherently confers stability during weight-bearing.

The flexor hallucis brevis contains the two sesamoids within its medial and lateral heads and inserts on the plantar base of the hallux proximal phalanx. The sesamoids function as a fulcrum to increase the mechanical advantage of the intrinsic plantar musculature while protecting the flexor hallucis longus tendon.

The flexor hallucis longus runs between the medial and lateral sesamoids and inserts on the plantar base of the hallux distal phalanx. The extensor hallucis longus and the more lateral extensor hallucis brevis insert into the extensor mechanism of the great toe.

The abductor hallucis and adductor hallucis insert on the medial and lateral sesamoids, respectively, along with the plantar base of the hallux proximal phalanx.
Pathogenesis and Biomechanical Dysfunction
Hallux rigidus may be secondary to primary osteoarthritis, systemic inflammatory arthritis, or less commonly septic arthritis. It may also be posttraumatic in nature, developing after a previous intra-articular fracture or significant turf toe injury to the ligamentous structures of the first metatarsophalangeal joint.
Biomechanical factors play a critical role in the pathogenesis. A long, hypermobile, or dorsally elevated first metatarsal (metatarsus primus elevatus) may lead to dorsal impingement of the proximal phalangeal base on the first metatarsal head with first metatarsophalangeal dorsiflexion. During the normal gait cycle, the first metatarsophalangeal joint must dorsiflex approximately 65 to 75 degrees to engage the windlass mechanism, allowing the plantar fascia to tighten and stabilize the longitudinal arch. When dorsal osteophytes form, this motion is mechanically blocked, leading to abnormal load transfer to the lateral metatarsals and subsequent transfer metatarsalgia.
Natural History
The extent of arthritis often progresses with time, leading to increased osteophyte formation and joint space narrowing. This may occur with or without joint-sparing surgical intervention. The progressive impingement exacerbates cartilage wear, eventually leading to global joint destruction and ankylosis.
Indications and Contraindications
Patient selection is the most critical variable in the success of metatarsophalangeal joint hemiarthroplasty. The procedure is generally reserved for patients with advanced hallux rigidus (Hattrup and Johnson Grade III, or Coughlin and Shurnas Grade 3) who strongly desire to maintain joint motion and refuse arthrodesis.
It is imperative to differentiate between patients who are candidates for joint-sparing procedures (cheilectomy) versus those requiring arthroplasty or arthrodesis. Hemiarthroplasty typically involves replacing the base of the proximal phalanx with a metallic implant, though modern variations include synthetic cartilage implants placed into the metatarsal head.
| Clinical Scenario | Operative Indication | Non-Operative Indication |
|---|---|---|
| Hattrup & Johnson Grade I | Cheilectomy | Rigid shoe insert, NSAIDs, Mortons extension |
| Hattrup & Johnson Grade II | Cheilectomy with or without Moberg osteotomy | Intra-articular corticosteroid injections, rocker-bottom shoes |
| Hattrup & Johnson Grade III | MTP Hemiarthroplasty or MTP Arthrodesis | Activity modification, custom orthotics |
| Hattrup & Johnson Grade IV | MTP Arthrodesis | Carbon fiber footplate, aggressive shoe modification |
| Inflammatory Arthropathy | MTP Arthrodesis (Hemiarthroplasty is contraindicated) | Rheumatologic medical management |
| Severe Hallux Valgus | Corrective Osteotomy + Arthrodesis | Wide toe-box footwear |
Contraindications for hemiarthroplasty include active infection, inadequate bone stock (severe osteopenia or avascular necrosis), systemic inflammatory arthropathies (e.g., rheumatoid arthritis), significant malalignment (uncorrected hallux valgus or varus), and profound neuromuscular disorders.
Pre Operative Planning and Patient Positioning
Patient History and Physical Findings
Patients often complain of pain and stiffness in their first metatarsophalangeal joint. Symptoms may be exacerbated by shoes with a restrictive toe box and by walking barefoot or in shoes with a flexible forefoot.
On examination, there may be a prominent first metatarsal head, a swollen first metatarsophalangeal joint, and tender osteophytes of the metatarsal head and phalangeal base. First metatarsophalangeal joint motion may be limited and painful. Dorsiflexion range of motion should also be assessed with the patient bearing weight or with dorsal translation applied to the first metatarsal head to simulate weight-bearing to assess for functional hallux rigidus.
In mild to moderate hallux rigidus (Hattrup and Johnson grade I and II), pain is principally with maximum joint dorsiflexion or plantarflexion secondary to dorsal osteophytes causing bone impingement or soft tissue tenting, respectively. With severe arthritis (Hattrup and Johnson grade III), there is usually pain throughout the entire arc of motion and a positive grind test, in which midrange of motion with axial compression applied to the first metatarsophalangeal joint is painful.
Imaging and Diagnostic Studies
Anteroposterior, lateral, oblique, and sesamoid views of the foot should be obtained to assess the extent of arthritis in the first metatarsophalangeal joint and in the adjacent first tarsometatarsal and hallux interphalangeal joints.

An assessment is also made for any concurrent hallux valgus or hallux varus deformity, osteopenia, avascular necrosis, or cystic changes within the metatarsal head or proximal phalanx. Severe cystic degeneration may compromise implant fixation and necessitate bone grafting or default to an arthrodesis.
Patient Positioning
The patient is placed in the supine position on the operating table. A calf tourniquet or ankle block tourniquet is applied to ensure a bloodless surgical field. A bump may be placed under the ipsilateral hip to correct for natural external rotation of the lower extremity, ensuring the foot rests strictly neutral, pointing directly toward the ceiling. Prophylactic intravenous antibiotics are administered prior to tourniquet inflation.
Detailed Surgical Approach and Technique
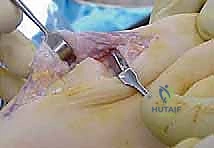
Incision and Dissection
A dorsal longitudinal incision is utilized, measuring approximately 5 to 6 centimeters, centered over the first metatarsophalangeal joint. The incision extends from the midshaft of the first metatarsal to the midshaft of the proximal phalanx.
Careful blunt dissection is performed through the subcutaneous tissues. The medial dorsal cutaneous nerve, a branch of the superficial peroneal nerve, frequently crosses the surgical field obliquely from proximal-lateral to distal-medial. This nerve must be identified and gently retracted to prevent painful postoperative neuromas. The extensor hallucis longus tendon is identified and mobilized. The extensor retinaculum is incised, and the extensor hallucis longus is retracted laterally, while the extensor hallucis brevis can be retracted laterally or transected depending on exposure needs.
Capsulotomy and Joint Exposure
A longitudinal or inverted T-shaped capsulotomy is performed. The capsule and periosteum are elevated off the dorsal aspect of the metatarsal head and the base of the proximal phalanx via sharp dissection. Medial and lateral collateral ligaments are released off the base of the proximal phalanx to allow for adequate plantarflexion and exposure of the articular surfaces.

Osteophyte Resection and Joint Preparation
The initial step of joint preparation involves a thorough cheilectomy. A sagittal saw or osteotome is used to resect the dorsal osteophyte of the first metatarsal head. Typically, the dorsal 25% to 30% of the metatarsal head is removed in a plane parallel to the plantar aspect of the foot. Medial and lateral osteophytes are also excised to restore the normal contour of the metatarsal head and decompress the joint space.
Attention is then turned to the proximal phalanx. The base of the proximal phalanx is exposed by plantarflexing the hallux. Using a sagittal saw, a minimal resection of the articular base of the proximal phalanx is performed, ensuring the cut is perpendicular to the long axis of the phalanx. It is critical to avoid excessive bone resection to preserve the insertions of the intrinsic musculature (flexor hallucis brevis, abductor hallucis, and adductor hallucis) at the plantar base of the phalanx.
Implant Trialing and Fixation
For a phalangeal-based metallic hemiarthroplasty, the medullary canal of the proximal phalanx is sequentially broached or reamed according to the specific implant system's instrumentation.

Trial components are inserted to assess sizing, stability, and range of motion. The ideal implant should cover the cortical margins of the resected phalangeal base without overhanging, which could cause soft tissue irritation or impingement.
Once the appropriate size is determined, the definitive implant is impacted into the proximal phalanx. The joint is reduced, and the surgeon must confirm that there is no pistoning of the implant and that the joint tracks smoothly without subluxation. Dorsiflexion should be assessed to ensure the dorsal impingement has been adequately relieved.
Closure
The joint capsule is meticulously repaired using absorbable suture (e.g., 2-0 or 3-0 Vicryl). A secure capsular closure is vital to prevent postoperative subluxation or dislocation of the implant. The extensor retinaculum is reapproximated to prevent bowstringing of the extensor hallucis longus. The subcutaneous tissue and skin are closed in a layered fashion. A sterile, bulky compressive dressing is applied.
Complications and Management
Metatarsophalangeal joint hemiarthroplasty carries a unique set of complications compared to arthrodesis, primarily related to implant longevity and biomechanical failure. Patient counseling regarding these risks is mandatory.
| Complication | Estimated Incidence | Etiology and Pathomechanics | Salvage Strategy |
|---|---|---|---|
| Aseptic Loosening / Subsidence | 10% - 25% | Poor bone stock, excessive resection, repetitive microtrauma | Conversion to MTP Arthrodesis (often requires structural interpositional bone graft) |
| Persistent Pain | 15% - 20% | Progression of sesamoid arthritis, undersized implant, impingement | Corticosteroid injection, orthotics, conversion to Arthrodesis |
| Transfer Metatarsalgia | 5% - 10% | Iatrogenic shortening of the first ray, loss of windlass mechanism | Metatarsal pads, custom orthotics, lesser metatarsal osteotomies (Weil) |
| Deep Infection | < 2% | Surgical site contamination, hematogenous spread | Implant removal, antibiotic spacer, staged Arthrodesis |
| Nerve Injury (Neuroma) | 2% - 5% | Iatrogenic injury to the medial dorsal cutaneous nerve | Gabapentinoids, targeted nerve block, surgical excision of neuroma |

Management of Implant Failure
The most challenging complication is aseptic loosening or subsidence of the implant. When a hemiarthroplasty fails, the standard salvage procedure is conversion to a first metatarsophalangeal joint arthrodesis. Because the initial hemiarthroplasty required bone resection, and subsequent subsidence often creates cavitary defects, primary arthrodesis is rarely possible without significant shortening of the first ray.
To restore the length of the first ray and maintain the biomechanical integrity of the forefoot, an interpositional structural bone graft (typically an autograft from the iliac crest or a structural allograft) is required. The graft is contoured to fit the defect and stabilized with a robust dorsal plate and interfragmentary screws.
Post Operative Rehabilitation Protocols
The postoperative rehabilitation protocol is designed to protect the capsular repair while encouraging early range of motion to prevent arthrofibrosis.
Phase I: Immediate Postoperative (Weeks 0 to 2)
The patient is placed in a rigid postoperative shoe or a controlled ankle motion boot. Weight-bearing is typically restricted to heel-touch or flat-foot weight-bearing to minimize axial loading on the newly implanted prosthesis. Elevation and strict adherence to edema control protocols are emphasized. Sutures are removed at approximately 10 to 14 days postoperatively.
Phase II: Early Rehabilitation (Weeks 2 to 6)
Once the incision is healed, aggressive range of motion exercises are initiated. This includes active and passive dorsiflexion and plantarflexion of the first metatarsophalangeal joint. Patients are instructed to manually distract the joint slightly during motion exercises to minimize shear forces across the implant interface. The patient may transition to a stiff-soled athletic shoe with a wide toe box as swelling permits.
Phase III: Return to Activity (Weeks 6 and Beyond)
Full weight-bearing in normal footwear is permitted. Strengthening exercises for the intrinsic foot musculature and the flexor hallucis longus are incorporated. High-impact activities (e.g., running, jumping) are generally discouraged indefinitely to prolong the survivorship of the implant, though low-impact activities such as cycling and swimming are highly encouraged.
Summary of Key Literature and Guidelines
The debate between metatarsophalangeal joint hemiarthroplasty and arthrodesis remains a prominent topic in orthopedic literature. Arthrodesis is universally recognized as the gold standard for stage III and IV hallux rigidus due to its predictable pain relief, functional improvement, and low long-term revision rates.
However, hemiarthroplasty remains a viable option for patients who prioritize motion. Historical silastic implants demonstrated unacceptably high rates of foreign body reaction, particulate synovitis, and implant fracture, leading to their general abandonment. Modern metallic phalangeal-based implants have shown improved survivorship, though studies indicate a revision rate of approximately 10% to 15% at ten-year follow-up.
Recent literature has also heavily evaluated synthetic polyvinyl alcohol hydrogel implants (e.g., Cartiva) placed in the metatarsal head. Early prospective randomized trials suggested equivalency to arthrodesis in pain relief with the added benefit of motion preservation. However, subsequent independent, retrospective cohort studies have demonstrated concerning rates of early implant subsidence and failure, prompting many academic surgeons to approach synthetic cartilage implants with caution.
Current guidelines from foot and ankle societies suggest that while arthrodesis provides the most reliable long-term outcome, hemiarthroplasty may be offered to appropriately counseled patients with realistic expectations regarding the potential need for future salvage procedures. Rigorous preoperative radiographic evaluation and meticulous surgical technique remain the cornerstones of optimizing outcomes in metatarsophalangeal joint hemiarthroplasty.
Clinical & Radiographic Imaging







Detailed Chapters & Topics
Dive deeper into specialized chapters regarding first-metatarsophalangeal-joint-hemiarthroplasty
